Copyright
©The Author(s) 2025.
World J Clin Cases. Oct 16, 2025; 13(29): 110948
Published online Oct 16, 2025. doi: 10.12998/wjcc.v13.i29.110948
Published online Oct 16, 2025. doi: 10.12998/wjcc.v13.i29.110948
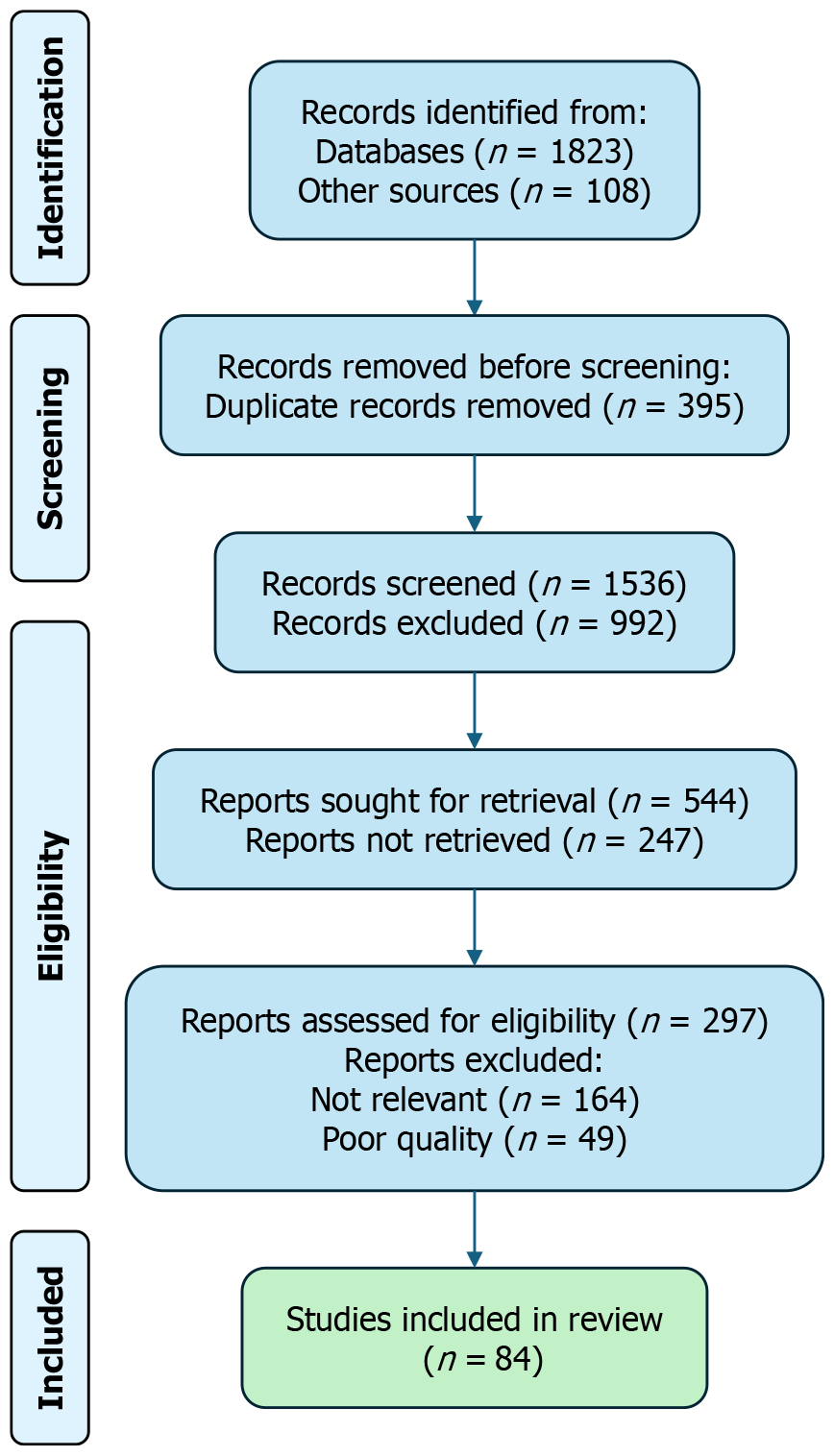
Figure 1 PRISMA 2020 flow diagram of study selection.
PRISMA 2020 flow diagram illustrating the identification, screening, and inclusion process for the studies included in this narrative review.
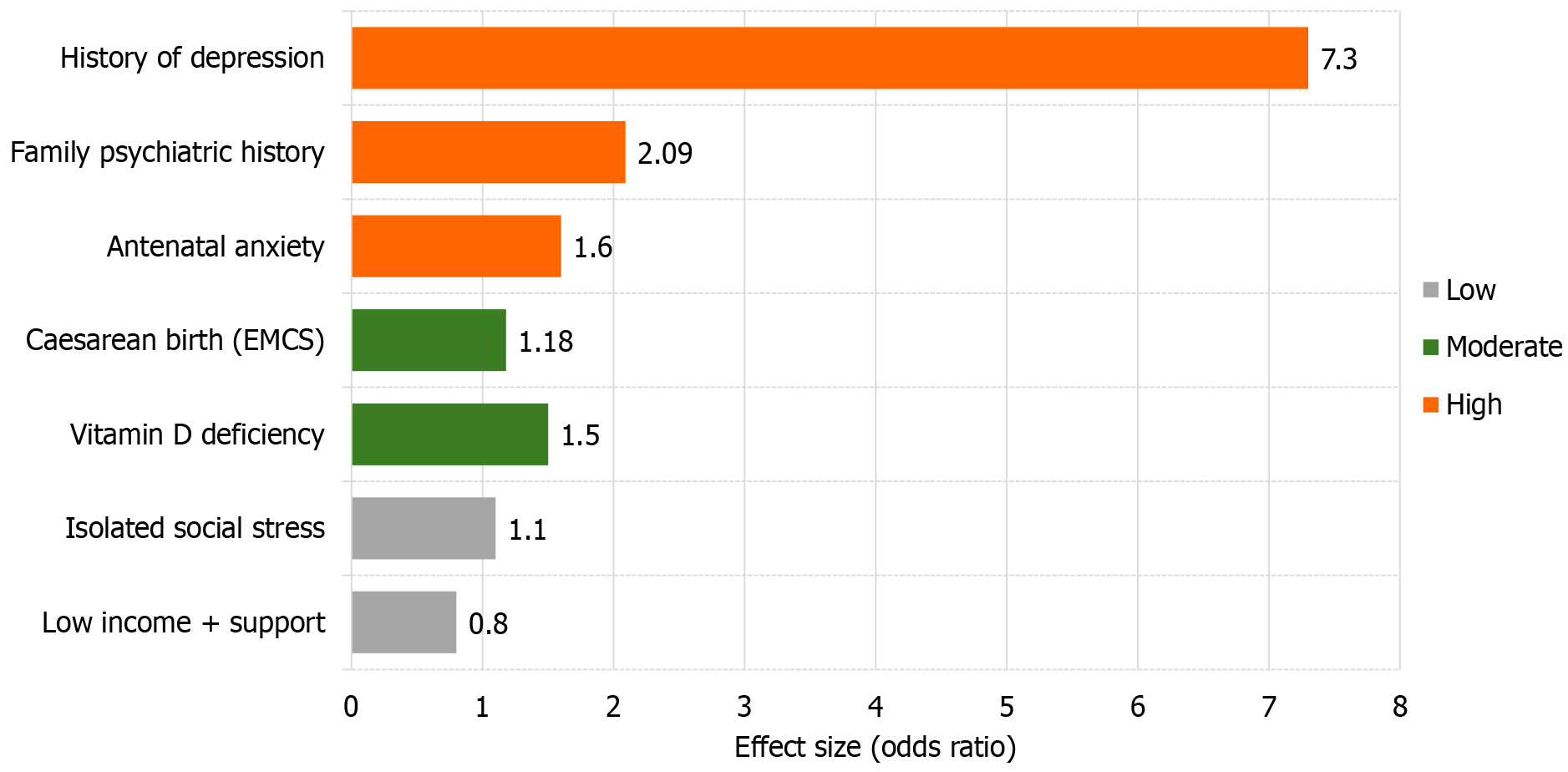
Figure 2 Graded risk factors for postpartum depression based on effect size and evidence strength.
This horizontal bar chart presents key psychosocial and biological risk factors for postpartum depression, categorized by level of supporting evidence (high: Red; moderate: Orange; low: Grey). The x-axis represents effect sizes, quantified as odds ratios (ORs), based on pooled estimates from meta-analyses and systematic reviews. A prior history of depression (OR = 7.3) emerged as the most potent risk factor, followed by family psychiatric history (OR = 2.09) and antenatal anxiety (OR = 1.6), all supported by high-certainty evidence. Moderate-certainty factors include emergency caesarean section (OR = 1.18) and vitamin D deficiency (OR = 1.5). Low-certainty factors, such as isolated social stress and low income with social support, demonstrated weaker and inconsistent associations (ORs < 1.2).
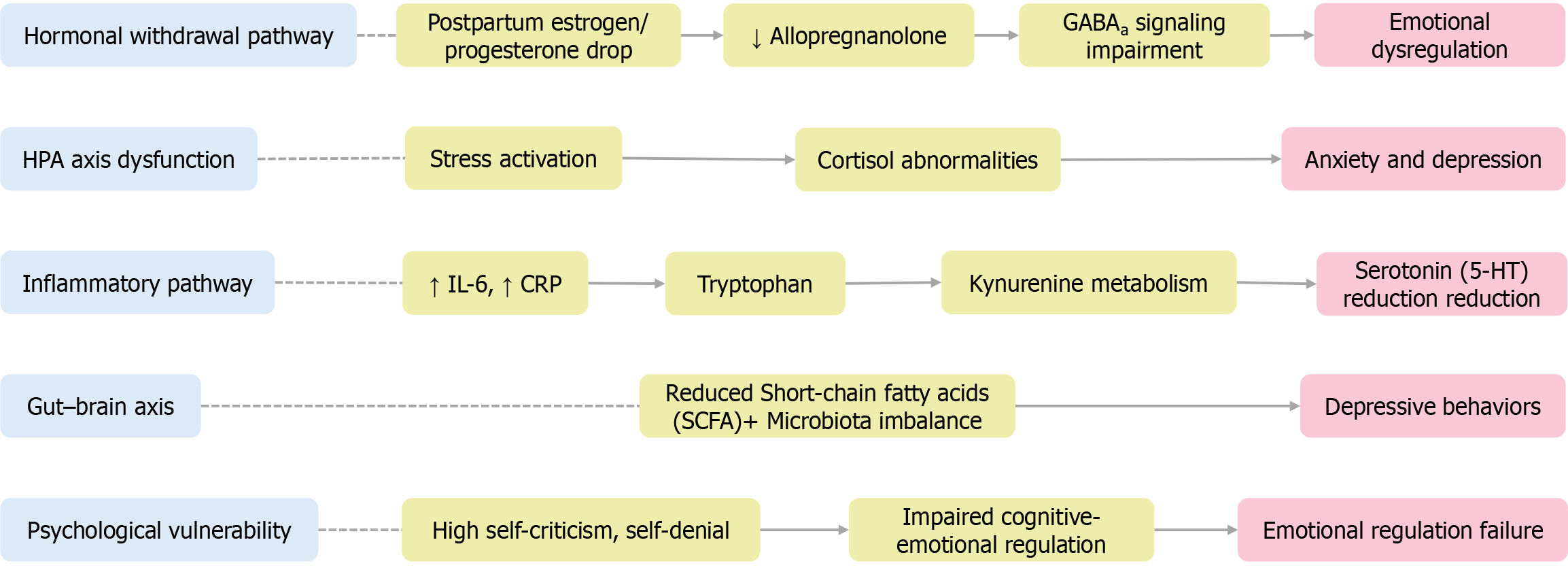
Figure 3 Parallel psychophysiological pathways underlying postpartum depression.
This figure illustrates five interrelated biological and psychological pathways implicated in the pathogenesis of postpartum depression: Hormonal withdrawal, hypothalamic-pituitary-adrenal axis dysregulation, inflammatory activation, gut-brain axis disruption, and psychological vulnerability. The updated hormonal model incorporates recent positron emission tomography/magnetic resonance spectroscopy findings linking postpartum estrogen withdrawal to decreased allopregnanolone levels and impaired GABAa signaling, which contribute to emotional dysregulation. Each pathway interacts with mood, cognition, and behavior through distinct yet interconnected mechanisms in biologically susceptible individuals. CRP: C-reactive protein; IL-6: Interleukin-6; SCFA: Short-chain fatty acid; 5-HT: 5-hydroxytryptamine; GABAa: Gamma-aminobutyric acid type A receptor.
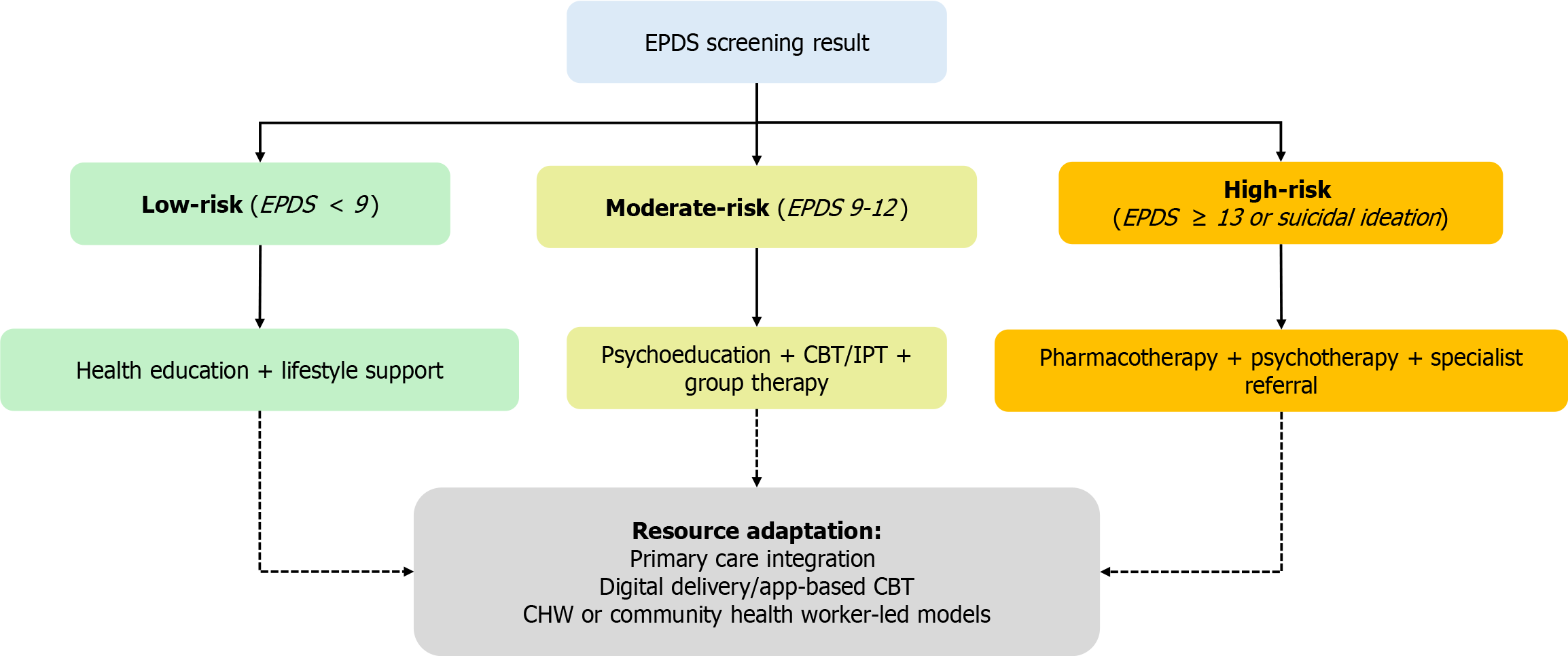
Figure 4 Stepped-care intervention framework for postpartum depression based on Edinburgh Postnatal Depression Scale risk stratification.
This figure presents a stepped-care intervention framework for postpartum depression, guided by risk levels determined through the Edinburgh Postnatal Depression Scale (EPDS). Individuals with low EPDS scores are recommended for basic interventions such as psychoeducation, lifestyle counseling, and informal social support. Those with moderate scores are directed toward more structured treatments including cognitive behavioral therapy, interpersonal therapy, or peer-led programs. For individuals with high EPDS scores, the framework emphasizes timely specialist referral, pharmacological treatment, and integrated psychiatric care. The bottom panel illustrates a range of adaptable delivery modalities applicable across all intervention tiers. These include digital platforms for scalable outreach, integration into primary care systems for streamlined access, and community-health-worker-led models that are especially suitable for low-resource or rural settings. CBT: Cognitive behavioral therapy; EPDS: Edinburgh Postnatal Depression Scale; IPT: Interpersonal therapy; CHW: Community health worker.
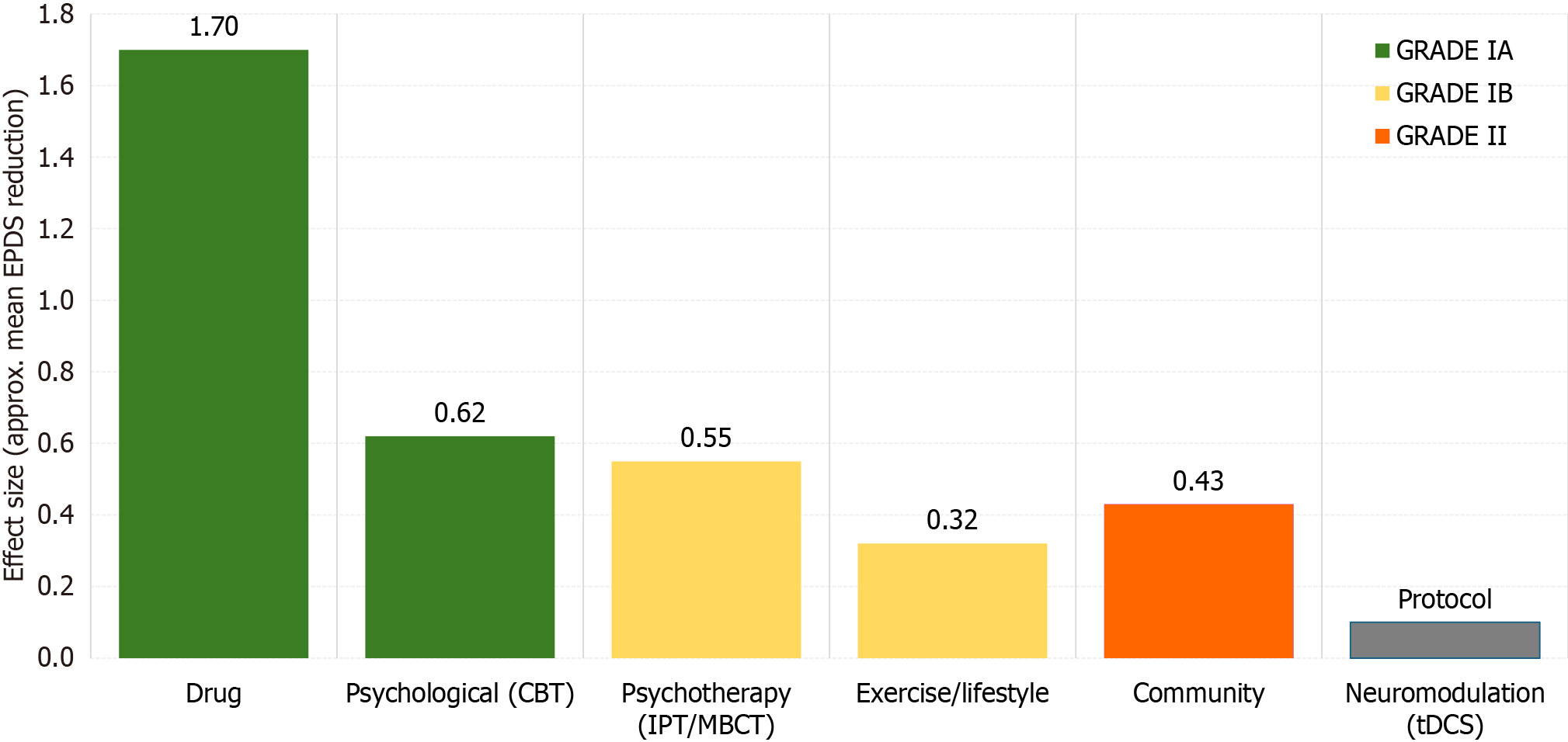
Figure 5 Effectiveness and GRADE evidence of postpartum depression Interventions.
Bar height represents the approximate mean reduction in Edinburgh Postnatal Depression Scale scores based on randomized (controlled) trials or representative meta-analytic estimates. Bar color corresponds to a modified GRADE classification: GRADE IA (green) = ≥ 2 multicenter randomized controlled trials (RCTs) or Phase III trials; GRADE IB (yellow) = ≥ 3 independent RCTs; GRADE II (orange) = systematic reviews where primary trials have sample or design limitations; the gray hatched bar (//) denotes neuromodulation, which is currently in the protocol stage and lacks comparable clinical outcome data. CBT: Cognitive behavioral therapy; EPDS: Edinburgh Postnatal Depression Scale; IPT: Interpersonal therapy; tDCS: Transcranial direct current stimulation.
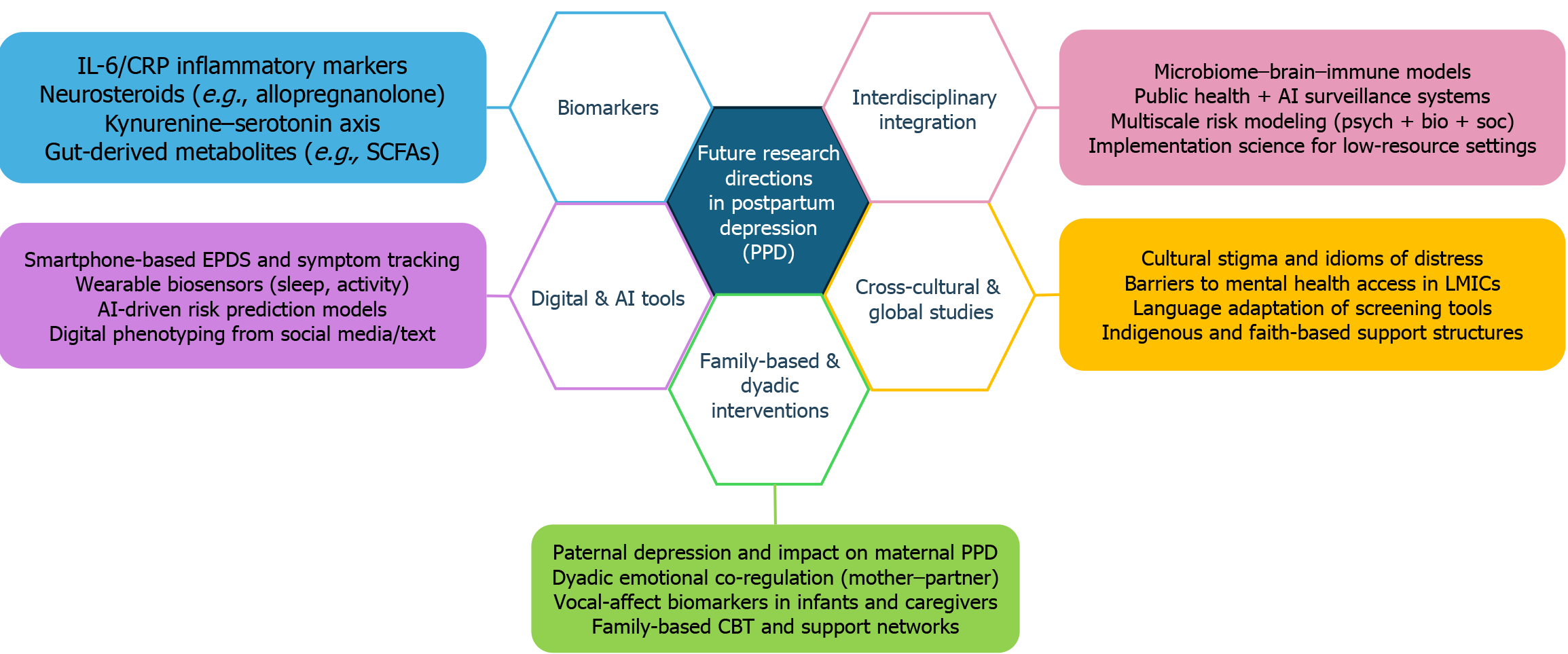
Figure 6 Emerging research frontiers and future directions in postpartum depression.
This figure 6 illustrates five priority research domains for postpartum depression: Biomarkers, digital and artificial intelligence-based screening, family-centered care, cross-cultural adaptation, and interdisciplinary collaboration. Each domain highlights actionable priorities such as immune-inflammatory markers (interleukin-6 and C-reactive protein), smartphone-based Edinburgh Postnatal Depression Scale tools, dyadic emotion regulation, culturally embedded care models, and multisystem frameworks for scalable mental health delivery. AI: Artificial intelligence; CBT: Cognitive behavioral therapy; CRP: C-reactive protein; IL-6: Interleukin-6; SCFAs: Short-chain fatty acids; PPD: Postpartum depression; LMICs: Low- and middle-income countries.
- Citation: Ji QQ, Wang MY. Epidemiology, pathophysiology, and interventions for postpartum depression: Systematic review. World J Clin Cases 2025; 13(29): 110948
- URL: https://www.wjgnet.com/2307-8960/full/v13/i29/110948.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v13.i29.110948