Published online Aug 16, 2022. doi: 10.12998/wjcc.v10.i23.8330
Peer-review started: March 5, 2022
First decision: April 28, 2022
Revised: April 30, 2022
Accepted: July 11, 2022
Article in press: July 11, 2022
Published online: August 16, 2022
Processing time: 148 Days and 20.3 Hours
Periosteal chondroma is a very rare benign tumor that develops adjacent to the cortical surface of bone and beneath the periosteal membrane. Periosteal chondroma of the rib is an extremely rare entity.
The patient was a 43-year-old man who had been incidentally found to have a mediastinal mass 1 mo earlier. Plain computed tomography showed a lobulated soft tissue mass on the right side of the T4/5 vertebra that measured about 47 mm × 28 mm in the transverse view and contained diffuse stippled calcification. The mass caused cortical scalloping of the right fourth rib and marginal bone sclerosis. Enhanced computed tomography showed mild enhancement of the mass. Magnetic resonance imaging showed a lobulated mass on the right side of the thoracic vertebra with long TI and T2 signals, mottling, and patchy long T1 and short T2 signals inside. The lesion had a hypointense rim. Enhanced magnetic resonance imaging showed enhancement predominantly at the periphery of the tumor. The tumor was approached through a right posterolateral thoracotomy, and parts of the fourth and fifth ribs were excised with the tumor. Postoperative pathological analysis revealed periosteal chondroma of the rib.
Periosteal chondroma of the rib has a low incidence and typical imaging manifestations. Understanding its imaging features is helpful to ensure a correct preoperative diagnosis.
Core Tip: Periosteal chondroma of the rib is an extremely rare entity. On computed tomography images, this tumor presents as a lobulated soft tissue mass with calcification that causes pressure erosion at the cortical surface. On magnetic resonance imaging, it shows a hyperintense signal on T2-weighted images without involvement of the medullary cavity. The lesion is bordered by a hypointense rim because it consists of fibrous tissue and an intact periosteum with a cartilaginous lobule on the surface.
- Citation: Gao Y, Wang JG, Liu H, Gao CP. Periosteal chondroma of the rib: A case report. World J Clin Cases 2022; 10(23): 8330-8335
- URL: https://www.wjgnet.com/2307-8960/full/v10/i23/8330.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v10.i23.8330
Chondromas are benign tumors composed of mature hyaline cartilage and usually develop at central sites in affected bone. Periosteal chondromas are rare and may occur at several sites, including the scapula and pelvis. A periosteal chondroma arising from a rib is extremely rare. To our knowledge, only 12 cases of periosteal chondroma of the rib have been reported worldwide to date[1]. In this report, we describe a further case of periosteal chondroma of the rib and present a review of the literature.
The patient was a 43-year-old man who had a soft tissue mass in the right paravertebral region discovered incidentally 1 mo earlier.
The patient had no other significant medical history.
There was no personal and family history.
Physical examination on admission revealed no pain or tenderness.
The results of routine blood and urine tests, blood biochemistry, and immune and infection indices were normal.
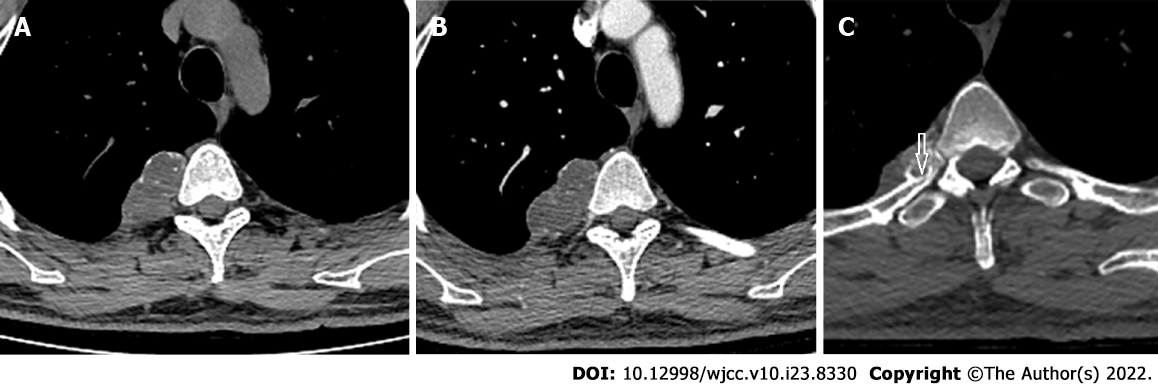
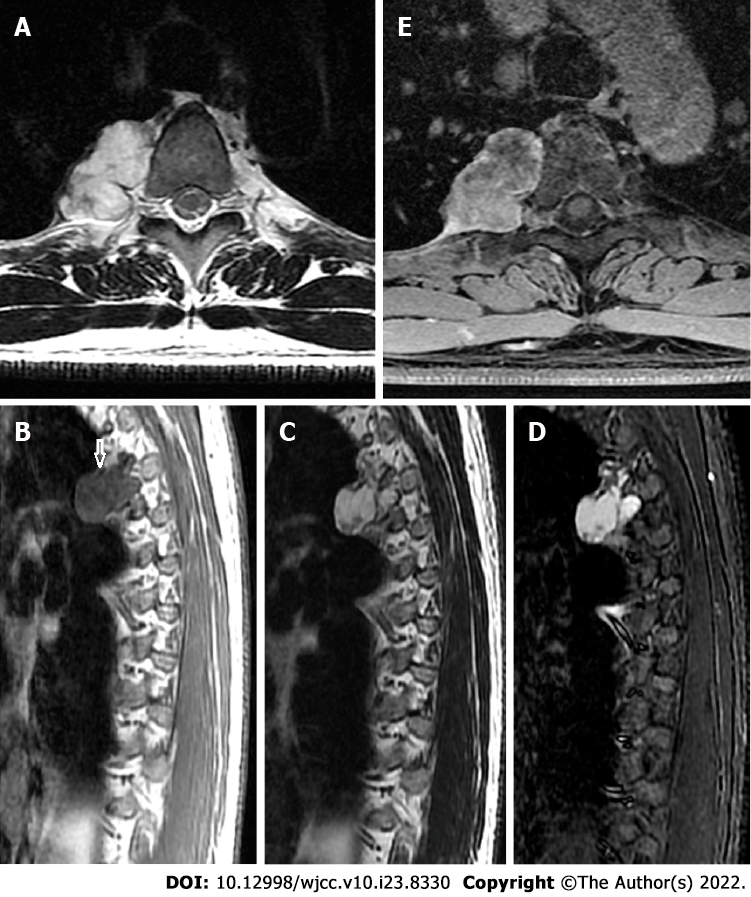
Plain computed tomography (CT) showed a lobulated soft tissue mass on the right side of the T4/5 vertebra that measured about 47 mm × 28 mm in the transverse view and contained diffuse stippled calcification (Figure 1A and B). The mass caused cortical scalloping of the right fourth rib (Figure 1C), rim ossification, and narrowing of the myeloid cavity. Enhanced CT showed mild enhancement of the mass. T1-weighted magnetic resonance imaging (MRI) in the transverse view showed a lobulated tumor on the right side of the thoracic vertebra (Figure 2A). The lesion was bordered by a hypointense rim and showed long Tl and T2 signals in the sagittal view on T1- weighted and T2-weighted images (Figure 2B and C). On short tau inversion recovery imaging, the mass showed high signal intensity and contained mottling and patchy long TI and short T2 abnormal signals (Figure 2D). Enhancement was seen predominantly at the periphery of the lesion on post-enhanced MRI (Figure 2E).
Considering the soft tissue nature of the mass on the right side of T4/5 and the bony destruction of the T4-associated rib, we considered that the mass was a non-neurogenic benign tumor arising from the rib.
The patient underwent surgical treatment. Dissection of adhesions in the upper lobe of the right lung revealed a posterior mediastinal mass (measuring about 5 cm × 3 cm). Part of the mass was removed and rapidly frozen, and pathologic examination of the biopsied tissue showed a mucinous chondroid matrix with scattered cytoplasmic, red-stained epithelioid cells. No obvious cell atypia, mitosis, or necrosis was observed, suggesting a benign mucinous or chondrogenic tumor. The mass was closely associated with the spine and spinal nerves, and the parietal pleura was excised. During the operation, the mass was found to surround the right fourth and fifth sympathetic nerves, which were difficult to separate; therefore, they were excised together with the mass. The mass caused bony destruction requiring removal of part of the bone. The posterior mediastinal mass was completely excised and pathologically examined.
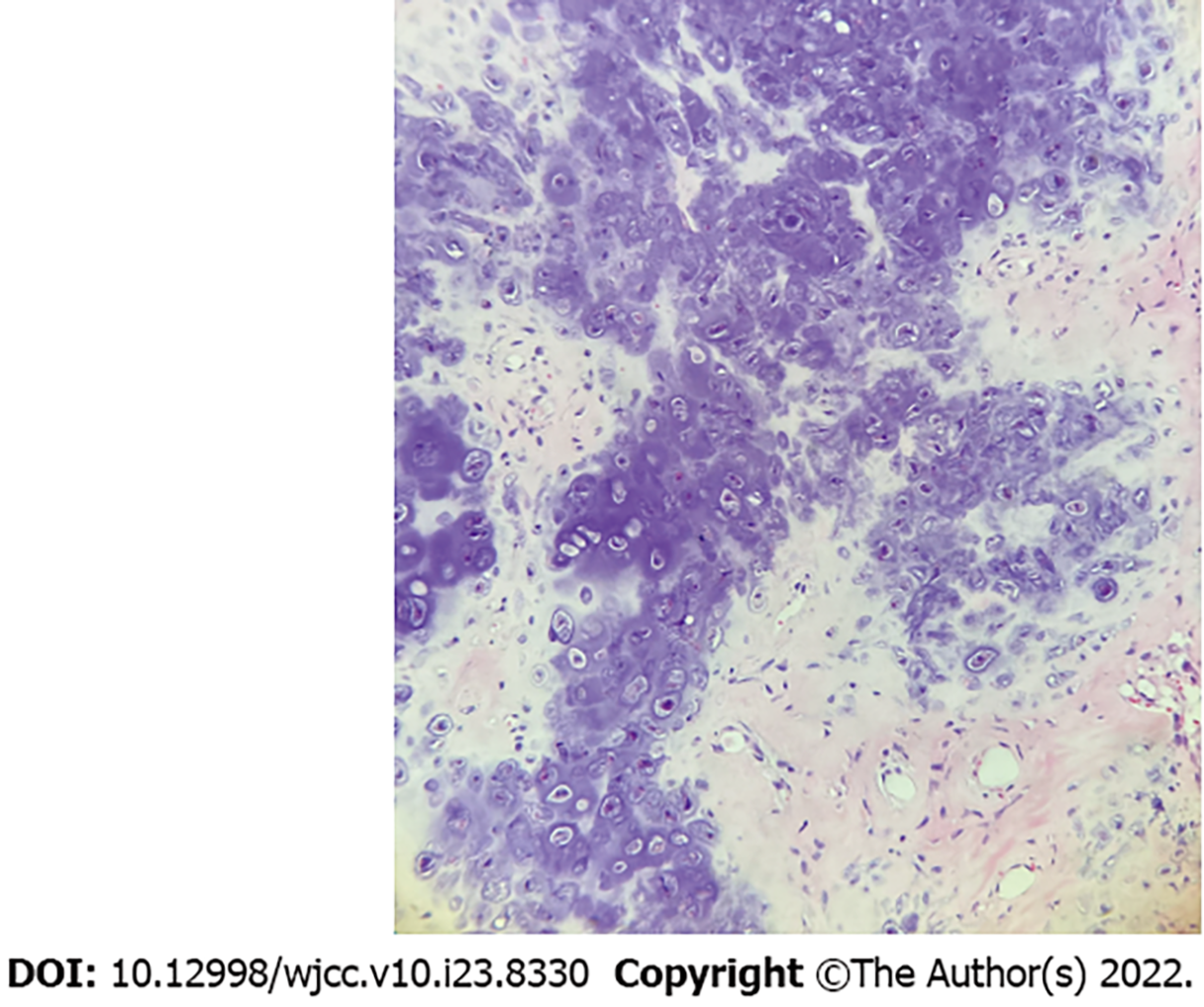
Final pathological examination of the posterior mediastinal mass showed that the tumor tissue consisted of a large amount of highly differentiated transparent cartilage and a mature trabecular bone structure. Most regional chondrocytes were differentiated and mature, consistent with a periosteal chondroma (Figure 3). No sign of recurrence was observed during 6 mo of postoperative follow-up.
Periosteal chondroma was first reported by Lichtenstein et al[2] in 1952. Periosteal chondroma is a slowly growing benign cartilaginous tumor that develops beneath the periosteal membrane. The tumor occurs predominantly in children and young adults with the highest frequency in the second decade of life[1,3,4]. According to Nojima et al[4], periosteal chondromas appear to be rare. A study at the Mayo Clinic found only 46 periosteal chondromas among more than 7000 primary bone tumors and that only 2 of these lesions originated in the rib. In total, only 13 periosteal chondromas of the rib have been reported to date, including our case[1].
The normal periosteum does not contain chondrocytes at the site of this tumor because of the distance from the chondroskeletal junction. Hence, we propose that a totipotent primitive cell located in the periosteum is the histologic origin of this tumor and that mechanical injury induced by previous surgery might contribute to the transformation of this primitive cell into a cartilaginous tumor. All reported cases of periosteal chondroma to date were associated with surgery or trauma[5,6].
CT and MRI reveal the characteristic findings of periosteal chondroma, leading to a correct diagnosis of this tumor. The radiographic abnormalities observed in the present case as well as in a previous report[4] correspond to the findings reported in the literature. On CT images, the lobulated soft tissue mass is seen to cause pressure erosion at the cortical surface of the rib and has a sclerotic rim or a thin cortical shell; these can be regarded as typical radiographic features. Generally, the medullary cavity is not involved[7]. In our case, the lesion arose from the fourth rib of the right side. Stippled calcification within the mass and compressive absorption of the bone cortex are typical manifestations of periosteal chondroma. Enhanced CT in the present case showed mild enhancement of the mass.
The signal characteristics of this lesion are similar to those of enchondroma, namely a well-defined lobulated mass at the bone surface with a hypointense to isointense signal on T1-weighted images and a bright signal with a hypointense border on T2-weighted or short tau inversion recovery images. The high signal intensity of the tumor matrix seen on T2-weighted and short tau inversion recovery images has been attributed to a recension in the highwater content of hyaline cartilage in relation to its mucopolysaccharide component[8]. The hypointense lining could be due to fibrous tissue and an intact periosteum with the cartilaginous lobule on the surface[4].
Sharp margins and a hypointense rim are the typical features of benign bone lesions[9]. Periosteal chondromas are soft tissue masses that show peripheral contrast enhancement on post-enhanced images[4]. The marginal enhancement of the mass is due to the abundance of capillaries in the fibrous tissue surrounding the tumor. This pattern is attributed to the fibrovascular bundles surrounding the car
The differential diagnoses of periosteal chondrosarcoma include paracortical chondrosarcoma and rib hemangioma. Radiographically, paracortical chondrosarcomas typically show popcorn calcification whereas periosteal osteosarcomas show vertical calcified spicules. Low-grade chondrosarcomas may be histologically indistinguishable from chondromas. Hemangioma of the rib presents as a mass with honeycomb-like calcifications and a thin bony cortex with or without cortical destruction on CT images[10]. On MRI, hemangioma appears hypointense on Tl-weighted images and hyperintense on T2-weighted images, and internal enhancement observed on delayed-phase contrast-enhanced MRI is indicative of a rich fibrous stroma or vessels[11].
The most effective treatment for a periosteal chondroma is en bloc resection. Incomplete resection of the tumor can lead to recurrence. Curettage of subcortical bone can reduce the probability of recurrence[5,12].
Periosteal chondroma of the rib appears to have a typical appearance on CT and MRI. On CT images, it presents as a lobulated soft tissue mass causing pressure erosion at the cortical surface without involvement of the medullary cavity. On MRI, it exhibits a hypointense to isointense signal on Tl-weighted imaging, hyperintense signal on T2- weighted imaging, and peripheral contrast enhancement on post-enhanced images. The most effective treatment for a periosteal chondroma is en bloc resection.
Provenance and peer review: Unsolicited article; Externally peer reviewed.
Peer-review model: Single blind
Specialty type: Neuroimaging
Country/Territory of origin: China
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): B
Grade C (Good): C
Grade D (Fair): D
Grade E (Poor): 0
P-Reviewer: Hashimoto K, Japan; Hashimoto K, Japan; Karavaş E, Turkey S-Editor: Wu YXJ L-Editor: Filipodia P-Editor: Wu YXJ
| 1. | Samaddar A, Mishra AK, Katti M, Gangopadhayay A. Successful surgical management of periosteal chondroma of the left second rib: a case report. Indian J Thorac Cardiovasc Surg. 2019;35:101-103. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 2. | Lichtenstein L, Hall JE. Periosteal chondroma; a distinctive benign cartilage tumor. J Bone Joint Surg Am. 1952;24A:691-697. [PubMed] |
| 3. | Lewis MM, Kenan S, Yabut SM, Norman A, Steiner G. Periosteal chondroma. A report of ten cases and review of the literature. Clin Orthop Relat Res. 1990;185-192. [PubMed] |
| 4. | Nojima T, Unni KK, McLeod RA, Pritchard DJ. Periosteal chondroma and periosteal chondrosarcoma. Am J Surg Pathol. 1985;9:666-677. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 104] [Cited by in RCA: 109] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 5. | Morisaki Y, Takagi K, Ishii Y, Furuya T, Ishikawa M, Tanaka S. Periosteal chondroma developing in a rib at the side of a chest wall wound from a previous thoracotomy: report of a case. Surg Today. 1996;26:57-59. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 12] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 6. | Woertler K, Blasius S, Brinkschmidt C, Hillmann A, Link TM, Heindel W. Periosteal chondroma: MR characteristics. J Comput Assist Tomogr. 2001;25:425-430. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 49] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 7. | Inoue S, Fujino S, Kontani K, Sawai S, Tezuka N, Hanaoka J. Periosteal chondroma of the rib: report of two cases. Surg Today. 2001;31:1074-1078. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 11] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 8. | Kransdorf MJ, Meis JM. From the archives of the AFIP. Extraskeletal osseous and cartilaginous tumors of the extremities. Radiographics. 1993;13:853-884. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 201] [Cited by in RCA: 179] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 9. | Zimmer WD, Berquist TH, McLeod RA, Sim FH, Pritchard DJ, Shives TC, Wold LE, May GR. Bone tumors: magnetic resonance imaging vs computed tomography. Radiology. 1985;155:709-718. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 216] [Cited by in RCA: 159] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 10. | Tew K, Constantine S, Lew WY. Intraosseous hemangioma of the rib mimicking an aggressive chest wall tumor. Diagn Interv Radiol. 2011;17:118-121. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 9] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 11. | Tanaka T, Masaoka Y, Sugimoto S, Iguchi T, Hiraki T, Yanai H, Kanazawa S. Cavernous hemangioma of the rib mimicking a chondrosarcoma: Diagnostic value of delayed phase MRI. Diagn Interv Imaging. 2019;100:455-457. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 12. | Ogata T, Miyazaki T, Morino T, Nose M, Yamamoto H. A periosteal chondroma in the lumbar spinal canal. Case report. J Neurosurg Spine. 2007;7:454-458. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 12] [Article Influence: 0.7] [Reference Citation Analysis (0)] |