Published online Jun 15, 2017. doi: 10.4239/wjd.v8.i6.249
Peer-review started: March 10, 2017
First decision: March 29, 2017
Revised: April 24, 2017
Accepted: May 3, 2017
Article in press: May 5, 2017
Published online: June 15, 2017
Processing time: 100 Days and 8.2 Hours
The disorders of gastrointestinal (GI) tract including intestine and colon are common in the patients with diabetes mellitus (DM). DM induced intestinal and colonic structural and biomechanical remodeling in animals and humans. The remodeling is closely related to motor-sensory abnormalities of the intestine and colon which are associated with the symptoms frequently encountered in patients with DM such as diarrhea and constipation. In this review, firstly we review DM-induced histomorphological and biomechanical remodeling of intestine and colon. Secondly we review motor-sensory dysfunction and how they relate to intestinal and colonic abnormalities. Finally the clinical consequences of DM-induced changes in the intestine and colon including diarrhea, constipation, gut microbiota change and colon cancer are discussed. The final goal is to increase the understanding of DM-induced changes in the gut and the subsequent clinical consequences in order to provide the clinicians with a better understanding of the GI disorders in diabetic patients and facilitates treatments tailored to these patients.
Core tip: The disorders of intestine and colon are common in patients with diabetes mellitus (DM). DM induced intestinal and colonic structural and biomechanical remodeling are closely related to motor-sensory abnormalities of gut in DM. These changes due to DM are associated with diarrhea, constipation, gut microbiota modification and colon cancer. Understanding the DM-induced changes in the gut and the clinical consequences provides clinicians with a better understanding of the gastrointestinal disorders in diabetic patients and facilitates the improvement of treatments for these patients.
- Citation: Zhao M, Liao D, Zhao J. Diabetes-induced mechanophysiological changes in the small intestine and colon. World J Diabetes 2017; 8(6): 249-269
- URL: https://www.wjgnet.com/1948-9358/full/v8/i6/249.htm
- DOI: https://dx.doi.org/10.4239/wjd.v8.i6.249
Diabetes mellitus (DM) is a popular metabolic disease which affects many populations worldwide[1]. Complications in different organ systems including the gastrointestinal (GI) tract will occur if the DM is treated inappropriately. NCD Risk Factor Collaboration has demonstrated that the number of adults with DM in the world increased from 108 million in 1980 to 422 million in 2014[1]. Furthermore, huge healthcare expenditures are needed in order to prevent and treat DM and its complications[2].
DM patients often suffer from GI disorders which are recently recognized as one of the most common complications in DM[3]. The whole GI tract can be affected in the DM and common complaints include diarrhea, constipation and fecal incontinence[4]. The symptoms are usually non-specific, but occasionally they may be severe enough to decrease the quality of life. The pathophysiological mechanisms of the symptoms are very complex; they may involve multiple factors and are inadequately explored. However, it is well known that the motor-sensory dysfunctions often seen in the DM patients are closely associated with diabetic autonomic neuropathy (DAN)[5-7]. Furthermore, it has been recently recognized that DAN also includes the disorders of the enteric nervous system (ENS)[7]. It is well known that DM induces histomorphological and biomechanical remodeling of small intestine and colon in type-1 DM patients[5] and in DM animals[8-10]. Such remodeling is closely related to motor-sensory dysfunctions in DM patients[9]. Understanding the mechanisms of DM-induced changes of the intestine and colon is of key importance for the optimization of treatment and for finding new therapeutic approaches.
In this review, we discuss: (1) DM-induced intestinal and colonic histomorphological changes and biomechanical remodeling; (2) intestinal and colonic sensory-motor dysfunction in relation to DM and its relation to the remodeling of intestine and colon; and (3) the clinical consequences of DM-induced changes in intestine and colon including diarrhea, constipation, GM change and colon cancer. It is well known that esophageal and gastric motility disorders are also very common in DM patients; however, these have been reviewed in detail recently (see references[11,12]). Furthermore, as we focus on the topic of DM-induced mechanophysiological changes in the small intestine and colon, the topic of esophageal and gastric disorders in the DM are not included in this review.
Understanding the anatomy and structure of normal intestine and colon is essential in order to gain an insight into the biomechanical properties and the DM-induced remodeling. Intestine and colon are tubular organs. From proximal to distal, the intestine consists of duodenum, jejunum and ileum. The ligament of Treitz marks the anatomical demarcation between duodenum and jejunum, whereas there is no distinct demarcation between jejunum and ileum. A mesentery anchors the jejunum (proximal 40%) and ileum (distal 60%) to the posterior wall of abdomen and allows the intestine to be freely moveable within the peritoneal cavity. The distal end of the intestine is in continuity with colon and the transition is marked by the ileocecal valve which prevents the retrograde flow of colonic contents into the small intestine[13]. The colon is composed of five parts namely cecum, ascending colon, transverse colon, descending colon and sigmoid colon. The external appearance of colon is distinctly different from that of the intestine. The longitudinal layer of muscle fibers forms three discrete bands named tenia, and the formation of sacs filled with adipose tissue on the inner surface gives the colon a segmented appearance characterized by small pouches named haustra.
The histologic characteristics of the intestine and colon shares many similarities. The wall is composed of four layers: Mucosa, submucosa, muscularis, and serosa with the mucosa being the innermost layer. The mucosa consists of sublayers of glandular epithelium, lamina propria, and muscularis mucosae. The glandular epithelium forms cylindrical structures called crypts. The lamina propria serves to support the epithelium and consists of reticular connective tissue with elastin, reticulin, and collagen fibers and cellular components such as lymphocytes, plasma cells, and eosinophilic granulocytes, as well as lymphatics and capillaries. The muscularis mucosae is a thin layer of smooth muscle intertwining the mucosa and submucosa. The submucosa is a fibrous connective tissue layer that contains fibroblasts, mast cells, blood and lymphatic vessels, and extraordinarily an autonomous nerve plexus called the Meissner’s plexus which consists of non-myelinated, postganglionic sympathetic fibers and parasympathetic ganglion cells[14,15]. The muscularis propria beneath the submucosal layer consists of smooth muscle fibers and is responsible for the contractility of the intestines. The muscle fibers are arranged in a helicoidal pattern in two layers, an inner circular layer and an outer longitudinal layer. Between these two muscle layers there is a second autonomous nerve plexus named the myenteric plexus or Auerbach’s plexus[15,16]. Parasympathetic and postganglionic sympathetic fibers in the plexus terminate in parasympathetic ganglion cells; from here, the postganglionic parasympathetic fibers terminate in smooth muscle and influence the intestinal contractility by the release of neurotransmitters. The serosa is the outermost layer of the intestines and consists of connective tissue. Interstitial cells of Cajal (ICC) are present in both the small intestine and the colon and influence the contractility of the smooth muscle fibers. These cells act as pacemaker cells and are located in the myenteric plexus, the muscularis propria and the submucosa[17]. The ICCs express the receptor for tyrosine kinase (c-kit). Thus, immunohistochemical stains that utilize antibodies against c-kit allow the ICCs to be labeled[18].
One important function of both small intestine and colon is the transportation of food by peristaltic contraction. Furthermore, the mixing function by segmental contraction is also important for small intestine in order to establish close contact between the food and mucosa and fully absorb the nutritional contents. Both types of contraction are involved in the force (stress) changes and deformation (strain) in the wall of intestine and colon. Therefore, understanding the normal biomechanical properties is essential for the understanding of the physiological functions of small intestine and colon. Descriptions of biomechanical properties include elasticity such as tension-strain or stress-strain relations, and viscoelasticity such as creep and stress relaxation. Generally the biomechanical properties of small intestine and colon display an exponential behavior and are anisotropic with large axial and location variations[19-40]. The biomechanical characteristics of the normal small intestine and colon can be summarized in Table 1.
| Biomechanical properties | |
| Intestine | Tension-strain or stress-strain curves show an exponential behavior[19-23] |
| The stiffness differs between the duodenal, jejunal and ileal segments[20,21,24] | |
| All segments are stiffest in longitudinal direction[20,21,24] | |
| The opening angle and residual strain shows a large axial variation[25]. The axial variation correlates to the morphometric variation[26] | |
| The serosal residual strains are tensile and the mucosal residual strains are compressive[24,25,27] | |
| The residual strains in longitudinal direction are smaller than those in circumferential direction[24], especially on the mucosal side | |
| The opening angle changes over time for all the small intestine segments. The viscoelastic constant of the rat small intestine is fairly homogenous along its length[28] | |
| The collagen in submucosa layer is important for the passive biomechanical properties[29,30] | |
| The villi are important for the biomechanical properties of the small intestine in circumferential direction[31] | |
| Colon | The rat colon has a tensile strength of around 50 g/mm2 and increases in strength from proximal to distal[33] |
| Quasi-static P-V curves in colon are approximated to a power exponential function and revealed hysteresis, indicative of viscoelasticity[34] | |
| The opening angle vary along the rat colon with the highest values in the beginning of the proximal colon[35]. The residual strain is negative at the inner surface and positive at the outer surface[35] | |
| The stress-strain curves are exponential. All segments were stiffer in longitudinal direction than in the circumferential direction[35] | |
| In human sigmoid colon, the spatial distributions of the biomechanical parameters are non-homogeneous. The circumferential length, strain, pressure and wall stress increase as a function of bag volume[36] | |
| The wall stiffness of human sigmoid colon is reduced in response to butylscopolamine[36] | |
| The phasic and tonic responses to the meal in two colonic regions of human are quantitatively different but qualitatively similar[37] | |
| Smooth muscle cells in the gastrointestinal tract are constantly being deformed due to forces generated by the muscle cells themselves or by the surroundings[38,39] | |
| A mechanical creep behavior in the isolated rat colon smooth muscle cells could be described by a viscoelastic solid model[40] |
The variation of biomechanical properties along and across the wall of intestine and colon have important physiological significance. The residual strain makes the stress distribution through the wall more uniform in the pressurized state[27]. The compression residual stress reduces the stress concentration at the inner wall, thereby offering a better protection of intestine and colon against injury due to contractile activity and against the flow of luminal contents. Furthermore, the different stiffness has been demonstrated in different segments of intestine and colon. For example, the duodenal segment is stiffest whereas the ileum is softest in the small intestine. These may relate to the specialized functions in the proximal and distal locations. Duodenum acts as a capacitative resistor during gastric emptying whereas the transit of distal ileum is slow and acts as a reservoir[32]. The flow patterns of intestine may also relate to biomechanical properties. The stiff duodenal wall will be in favor of a lesser degree of bolus passing whereas the soft ileal wall will be in favor of pooling of luminal content and decreased flow.
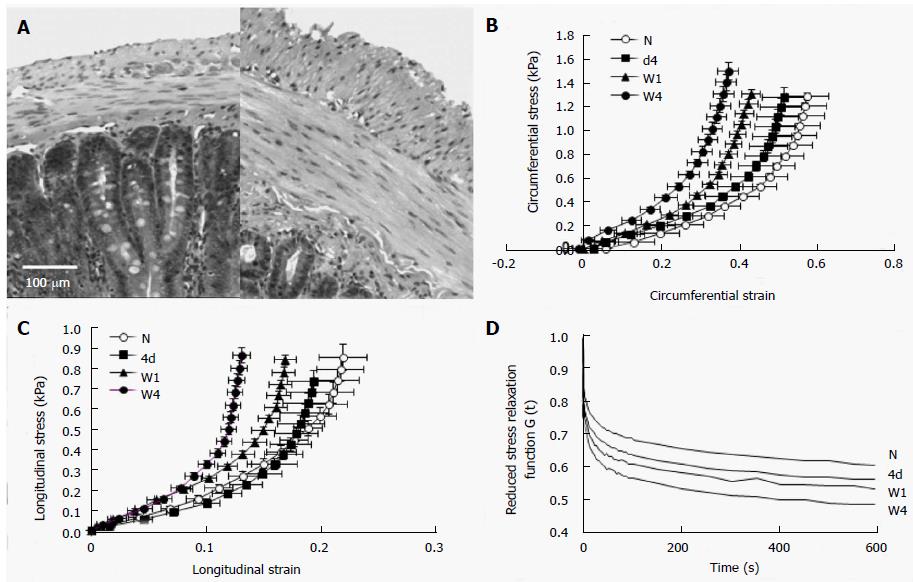
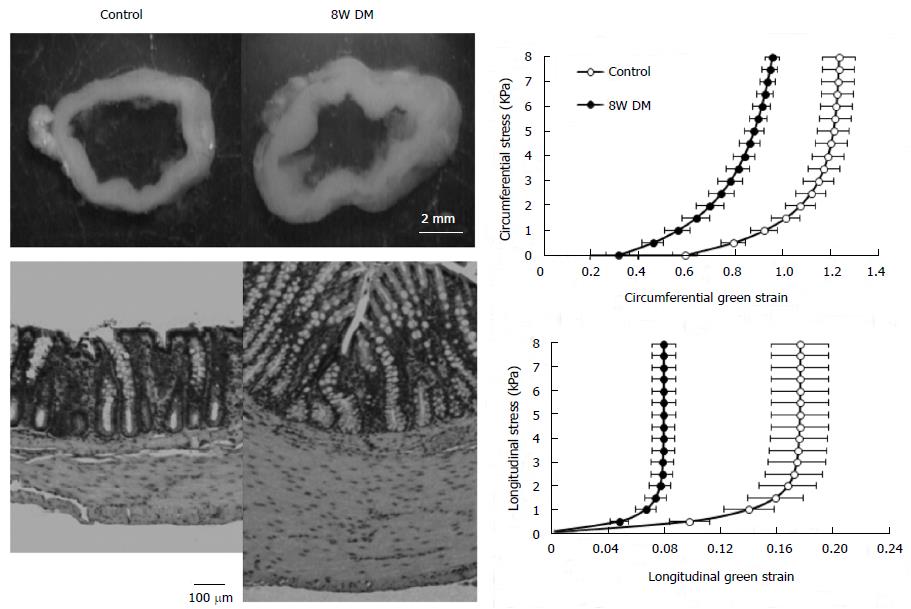
DM-induced histomorphological changes involve different tissue components of the intestinal and colonic wall including epithelia, smooth muscle cell (Figure 1A, Figure 2), neurons, ICC and extracellular matrix (Table 2). Many animal and human studies have demonstrated that DM generally induces changes in the proliferation of different layers[5,8,10,41-51]. Increased expression of advanced glycation end of product (AGE) and AGE receptor (RAGE) has been demonstrated in the DM intestinal and colonic wall[49,51,52]. Furthermore, the number and density of neurons and ICC are changed, and the expressions of some neuropeptides alter as well (Table 2).
| Intestine | Colon | |
| Mucosa | Increased thickness[5,8,47,49]; Damaged tight junctions[260]; Proliferation of villi and crypt[41]; Decreased membrane fluidity[110]; Enhanced transport of glucose, amino acid, bile salts, phosphate, fatty acids, fatty alcohols, and cholesterol[110]; Decreased protein synthesis[261]; Increased expression of the monosaccharide transporters[262,263]; Increased expression of AGE and RAGE[47,49] | Increased thickness[10,49]; Increased thickness of the subepithelial collagen layer[276,277]; Abnormalities of endocrine cells[278]; Increased expression of RAGE[49]; Increased expression of AGE, RAGE, TGF-β1 and TGF-β1 receptor[52] |
| Submucosa | Increased thickness[5,8,47] | Increased thickness[10]; Increased expression of AGE, RAGE, TGF-β1 and TGF-β1 receptor[52] |
| Muscle | Increased thickness[8,47]; Increased expression of AGE and RAGE[49] | Increased thickness[10]; Hypertrophy of smooth muscle cells[51]; Increase type I collagen and expression of AGE[51]; Increased expression of AGE, RAGE, TGF-β1 and TGF-β1 receptor[52] |
| Wall as a whole | Increased thickness[8,47-50]; Increase expression of substance P[264] and neuronal nitric oxide synthase[265]; Dcreased expression of substance P[266], vasoactive intestinal polypeptide[262] and neuronal nitric oxide synthase[267]; Increased RAGE mRNA level[50] | Increased thickness[10,49]; Increase in substance P levels[264] |
| Nerve and ICC | Nuroaxonal dystrophy[48,268]; Decreased myenteric ganglia[269]; Decreased nitrergic neuronal cell number[270]; Decreased density of myenteric neurons[120]; Decreased number of myenteric neurons[271,272]; Increased expression of RAGE[49]; Decreased myosin-V-immunoreactive neurons[273]; Decreased ghrelin cell density[274]; Reduced number of ICC[99,275] | Impairment of nitrergic enteric neurons[111]; Decrease density and size of the myenteric neurons[15]; Decreased nitrergic neuronal cell number[280]; Decreased the numbers of nNOS, CHAT neurons and total neurons[279]; Increased expression of RAGE[49]; Apoptosis of neurons[244]; Decreased ghrelin cell density[274]; Reduced number of ICC[99,110,124,280] and impairment in the ultrastructures of ICC[99] |
In comparison with DM-induced histomorphological remodeling, there are not so many data in relation to the biomechanical remodeling in the small intestine and colon. Data on tension-strain relations has demonstrated that the stiffness of wall in the rat jejunum and ilem increases in DM rats[53]. Lately, the research group of Zhao et al[8,25] and Sha et al[48] did a series of studies investigating the histomorphological and biomechanical remodeling of small intestine in STZ-induced DM rats. They found in diabetic rats that (1) the opening angle and residual strain became smaller in the duodenum and larger in the jejunum and ileum; (2) the stiffness of the intestinal wall increased as function of time of DM development (Figure 1B and C); and (3) the stress of intestinal wall relaxed less(Figure 1D). More recently, remodeling of the jejunal wall in type 2 DM rats (GK rat) has been reported[47]. It was shown that the opening angle and residual strain were reduced and the wall stiffness increased in the circumferential direction. Furthermore, we demonstrated that increasing blood glucose level and the increased AGE/RAGE expression were associated with the remodeling. However, data on biomechanical changes in the diabetic colon is sparse. We have also investigated DM-induced biomechanical and morphometric remodeling in rat colon[10]. It was found in diabetic colon that the opening angle and residual strain became bigger and the stiffness of the colon wall increased with the duration of DM both in the circumferential and longitudinal directions (Figure 2). More recently, the remodeling of the distal colon in DM was studied by Siegman et al[51] in rats. A major finding from the study was the marked decrease in resting compliance and increase in stiffness of the smooth muscle cells of the distal colon in DM rats. Such changes are associated with increased production of type 1 collagen and AGEs.
Hyperphagia: There is study which suggests that hyperphagia is related to DM-induced GI growth[54]. However, other researchers have found that when DM rats and normal rats are fed with same caloric diets, the intestinal mass and DNA synthesis in crypt still increases considerably in diabetic rats[55,56]. This indicates that DM-induced GI growth depends not only on increased nutrient consumption but also on other adaptation factors. It has been demonstrated that there is a close relation between glucagon-like peptide-2 (GLP-2) and DM-induced GI growth[57]. Increasing blood GLP-2 could precede the changes of intestinal mass[57]. Therefore, the increased nutrient in DM-induced GI growth may relate to its role in the stimulation of hormonal release in the GI tract. The nutrient content in the small intestine is greatly increased due to hyperphagia and fast gastric emptying[56] in DM rats. It is well known that the luminal nutrients such as fat and carbohydrate could stimulate physiological L cells[58], therefore the increased luminal nutrients could stimulate GLP-2 secretion and its action on the intestinal epithelium. Furthermore, the balance of the epithelial homeostasis is regulated by cell proliferation and death. It has been shown that apoptosis is inhibited in DM rats which in turn results in the increase of mucosal mass in the small intestine[44].
Non-enzymatic glycation of protein: Hyperglycemia is the most important feature of DM. The increased glucose can induce AGEs formation through non-enzymatic glycation of protein amino groups and by oxidation reaction[59]. The overproduction and accumulation of AGEs in the tissues could alter the structure and function of proteins[60] in the intestinal wall such as collagen. Such changes cause cross-linking of collagen, basement membrane thickening and the loss of matrix elasticity[61-63]. AGEs and corresponding receptors (RAGE) have been demonstrated to be up-regulated in the GI tract both in the experimental type 1[49] and type 2[64] DM rats. Furthermore, there is an association between AGEs and RAGE with DM-induced intestinal and colonic remodeling[47,51]. Two major mechanisms are mainly involved in the link between AGEs and DM-induced GI morphological and biomechanical remodeling. One is a receptor-independent pathway where the AGEs induce changes in the extracellular matrix architecture through the formation of protein cross-links. The other is a receptor-dependent pathway where the AGEs modify cellular functions through the RAGE[65-67].
AGEs and RAGE also play an important role for DAN[68-70]. The expression of AGEs has been demonstrated in the peripheral nerves in DM animals[71] and in the axons and Schwann cells of patients with DM[72]. Increased expression of RAGE in peripheral nerves in DM rats has also been demonstrated[73]. The AGEs-induced changes of proteins could cause structural and functional changes in the peripheral nerves[74]. Modification of major axonal cytoskeletal proteins such as tubulin, neurofilament, and actin by AGEs impairs axonal transport and contributes to the development of atrophy and degeneration of nerve fibers[75,76]. Micro-vessels in peripheral nerves affected by AGEs may also contribute to the damage of peripheral nerves[77]. Therefore, long-term hyperglycemia induced GI tissue nonenzymatic glycation appears to play an important role in the remodeling of GI wall in DM.
DM-induced GI remodeling likely affects the sensory-motor function through the modification of the mechanical environment and structural basis around the motor and sensory nerves in the wall of intestine and colon. DM-induced increase in wall stiffness can change the tension and stress distribution around the mechanosensitive afferents. DM-induced structural and deformational changes can alter the relative position and response rate of the motor-sensory afferents. Furthermore, DAN involves both the sensory nerve supply to the intestine and colon, the ENS and processing in the central nerve system (CNS). Therefore, it is important to explore DM-induced sensory-motor changes in the intestine and colon and its mechanisms.
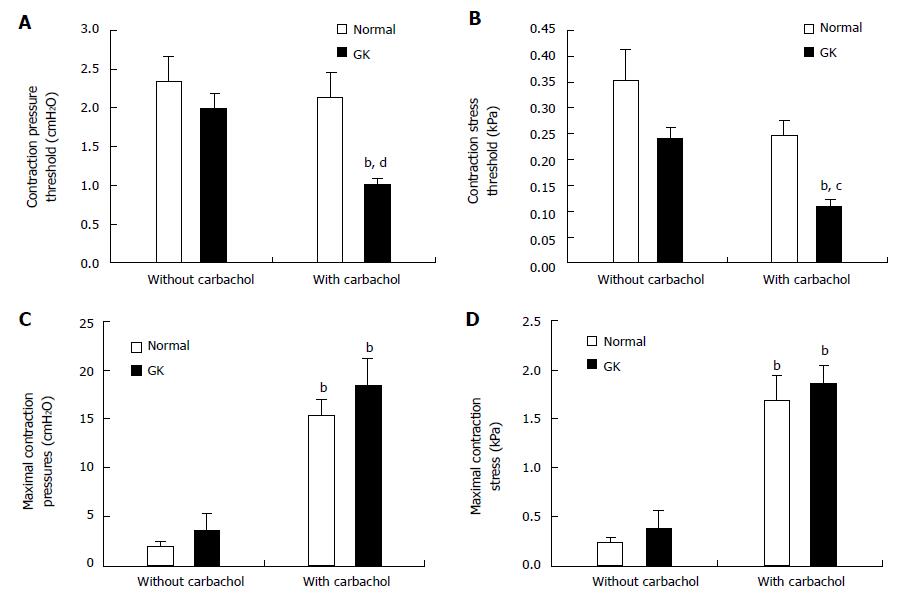
Small intestine (Table 3): Both delayed and rapid transit has been demonstrated in DM animal models[78,79]. It has been found in DM rats that the increase in transit time and decrease in intestinal tone are associated with up-regulated cholinergic activity and low-regulated beta-adrenergic receptor activity[80]. Stress-strain analysis of jejunal contractility in response to flow and ramp distension demonstrated that the jejunal contractility was hypersensitive to stimulations after carbachol application[81,82] in type 2 DM rats (Figure 3). However, the force generated per unit of smooth muscle was decreased in the DM rats, and could be partly compensated by hyperplasia and hypertrophy of the smooth muscle[82]. Furthermore, it was demonstrated that the ileal segment from type-1 DM rats was hypersensitive to distension for contraction induction[83]. However, the contraction force produced by smooth muscle was lowest in DM rats. Increased AGE and RAGE expressions were found to be associated with contractility changes in DM rats.
| Changes | Intestine | Colon |
| Motor | Transit time ↑↓[43,78-80,84,87] Muscle tone ↓[80] Jejunal contractility in response to flow and ramp distension after carbachol application ↑[81] Ileal contractility in response to distension ↑[83] The force generated by the smooth muscle per unit ↓[82,83] Dysmotility DM patients[88,90] Migrating motor complex disorders[89] | Transit time ↑[85,92-99,101,102,106] Contractility ↑↓[104,108,109,111-113] Carbachol induced contractions in muscle ↑↓[100,107,112] Spontaneous contractility ↑↓[100,102] Contraction and relaxation of circular muscle strips from DM were impaired[105] |
| Sensory | Sensitivity of human duodenum to the combination of mechanical, thermal and electrical stimulations ↓[114] Sensitivity of rat jejunum to the mechanical stimulation ↑ | Sensitivity of rat colon to the mechanical stimulation ↑[103,115,116] |
In DM patients, the delay in intestinal transit time has also been demonstrated by using different tests such as breath hydrogen appearance time[84], radiopaque markers[85] and metal-detector[43]. On the contrary, increased intestinal transit time has been found in insulin-dependent DM (IDDM) patients[86]. In patients with long standing IDDM, it has been demonstrated that the duodenal transit is disturbed and the chyme clearance activity is decreased87]. In one study, it has been reported that about 80% of patients with long-standing DM had abnormal motility of the small intestine[88]. The DM-induced dysmotility can occur either in the postprandial or fasting state[89,90]. In noninsulin-dependent DM (NIDDM) patients with diarrhea and DAN, grossly disordered motility such as migrating motor complex disorders has been reported[89]. Although disorders of postprandial motility in small intestine have been reported in DM patients, the findings are inconsistent[90].
Colon (Table 3): Colonic dysmotility is often seen in DM patients[85,91-97] and animal models[97-103]. DM patients with DAN are expected to have delayed transit in the entire gut, this finding is apparent to some extent in the distal colon but not in the proximal colon[92]. Delayed transit is most frequent in male patients with long-term IDDM where the total colonic transit time is prolonged[93]. Even in type II diabetic patients without clinical presentation of neuropathic symptoms, significant elongation of the transit time has been observed in the lower digestive tracts compared to control subjects[85]. Jorge et al[95] found that at 24 h after ingestion, there was no difference in the number of radiopaque particles in the colon between DM patients and controls. However, at 72 h past ingestion, the mean number of radiopaque particles in the colon was significantly higher in DM patients than in healthy controls. Furthermore, The DM patients with constipation had longer colonic transit times than those without constipation[94,96]. Hyperglycemia could inhibit long and short neural reflexes to modulate colonic motility which may contribute to constipation in DM[104]. The postprandial colonic motility is increased in DM patients with mild constipation but not in DM patients with severe constipation, the later may be due to DAN-induced absence of the postprandial gastrocolonic response[91]. Chandrasekharan et al[105] demonstrated that colonic circular muscle strips from DM subjects showed impaired contraction and relaxation responses compared to that of healthy controls. Such changes may be caused by the loss of enteric neurons in the colon due to increased oxidative stress and apoptosis.
Results from animal studies are ambiguous and have shown both delay and enhancement in the colon transit time in DM. Similarly, both reduced and increased colon contractility for whole segment or muscle strips in DM animals are reported. Delayed colonic transit has been found in alloxan-induced DM mice[98], db/db mice[99] and DM rats[101,102]. The prolonged transit time in db/db mice is associated with reduced areas of ICC and the expression of SCF in colon[99]. Insulin-like growth factor 1 (IGF-1) treatment can inhibit the DM-induced colonic smooth muscle cell apoptosis and may be involved in the alleviation of colonic dysmotility in DM rats[102]. However, Domènech et al[106] reported that DM RIP-I/hIFNβ transgenic mice showed an enhanced gut transit associated with gut remodeling including neuroplastic changes and overt myenteric neuropathy. In relation to the contractility, however, carbachol-induced and Ems-induced contractions in the colon muscle were significantly reduced in DM mice[107]. Wang et al[101] showed that endogenous IGF-1 and SCF protein and their mRNA expressions were significantly reduced in the DM colonic muscle tissues. Kim et al[100] demonstrated that spontaneous contractility decreased, carbachol-induced contractility decreased and the number of interstitial cells of Cajal networks was greatly reduced in the proximal colon of DM rats. In addition, the degree of relaxation in response to nitric oxide in the proximal colon of DM rats also appeared to be attenuated. Their results suggest that the decrease of interstitial cells of Cajal network, cholinergic receptors, and neuronal nitric oxide synthase in the proximal colon plays important roles in DM-related dysfunction of colon. Touw et al[108] showed that Type 1 DM is associated with decreased depolarization-induced Ca(2+) influx in colonic smooth muscle, leading to attenuated myosin light chain phosphorylation and impaired colonic contractility. Sung et al[103] showed that the frequency, not the amplitude, of colonic spontaneous contraction in vitro was significantly decreased in DM rats compared to control rats. However, enhanced contractility of the colon in the DM animals has also been reported[109,110]. The increased contractility is associated with loss and injury to ICC in the submucosa and muscle layers[110]. Yoneda et al[111] showed that the colonic peristaltic reflex is enhanced by impairment of enteric nitrergic inhibitory neurons in spontaneous DM rats. Xie et al[112] demonstrated that carbachol-induced contractions of distal colonic strips were greater in DM rats in which β-arrestin2 is involved in the increase of distal colonic contraction in DM rats. Chang et al[113] indicate that the increased contractions of distal colon in DM rats are partly mediated by the IL-6 receptor pathway.
Compared with published studies on motor disorders in DM, only few studies have addressed the sensory function of intestine and colon in the DM (Table 3). In relation to the small intestine, it has been demonstrated in a human study that there was an overall hyposensitivity to the combination of all stimulations including mechanical, thermal and electrical stimulations in the duodenum in the DM patients[114]. Furthermore, it was found that these patients demonstrated a 46% increase in the somatic referred pain areas. This may indicate that central neuronal changes are involved in the sensory changes of gut. Thus, the mechanisms of GI symptoms in long-standing DM patients are likely to involve the interactions between peripheral and central systems[114]. In relation to the colon, Grabauskas et al[115] showed that visceromotor responses to colorectal distension were significantly higher in STZ-induced DM rats 8 wk after the induction of DM. Such visceral hypersensitivity is mediated by abnormal IA current resulting from an increased phosphorylation of MAPK and Kv4.2 in dorsal root ganglion neurons. Similarly Hu et al[116] has also demonstrated that STZ-induced DM rats had colonic hypersensitivity to mechanical stimulation. The hypersensitivity was associated with an enhanced neuronal excitability of primary sensory neurons that showed an up-regulated expression of voltage-gated sodium channels (VGSCs, i.e., NaV1.7 and NaV1.8 subunits). Visceral hypersensitivity is also demonstrated in a rat model of type 2 DM accompanied by weight loss[103].
It is important to understand the mechanism behind the DM-induced sensory-motor changes of gut in order to enhance treatment approaches for the DM patient with gut disorders. As mentioned previously, the histomorphological and biomechanical remodeling could alter the baseline of the mechanosensitive afferents activity and the biomechanical environment around the mechanosensitive afferents. Therefore, DM-induced changes of gut structure and biomechanical properties can induce the changes observed in sensory-motor functions. On the other hand, the sensory-motor changes of the gut may reflect the structural and functional changes of peripheral nerve, ENS and the CNS in patients with DM. It seems that the more severe the neuropathy, the greater the likelihood of the involvement in gut sensory-motor disorders is[9].
More than 30% long-standing DM patients have DAN, therefore DAN is the most prevalent DM complication which is also related to other diabetic complications including GI complications[117]. The sensory nerves and ENS can be affected by peripheral DAN[7,118,119]. There is proof that the nerves in different layers of the GI wall undergo DAN changes and that the parasympathetic fibers in the gut are disrupted in DM patients[114]. Furthermore, ICCs are pacemaker cells in the GI tract distributed along the GI wall[120]. In GI tract, ICCs play an important role for the link between the autonomic nervous system, enteric neurons and smooth muscle cells[121]. Animal studies have demonstrated that the number of ICCs is reduced in different parts of GI tract such as the stomach[99,122], small intestine[99,123] and[99,124] colon. Therefore, the mechanisms of DM-induced sensory-motor function changes extensively involve the autonomic nervous system, ENS and ICCs.
Many factors are related to DAN. As mentioned above, the formation and accumulation of AGEs in peripheral nerves are associated with DAN directly by affecting structural and functional proteins and indirectly by activating receptors for AGEs. In addition to the formation of AGEs, the microvascular complications to DM causing neuropathy include other biochemical pathways. For example, DM can induce oxidative stress which is enhanced by AGE formation and polyol pathway activation[125]. Many data have shown that oxidative stress-induced tissue injury is associated to DAN[77]. Experimental and clinical data provide evidence that C-peptide is related to nerve dysfunction in DM since the C-peptide administration by subcutaneous injections seems to ameliorate nerve dysfunction in DM[126]. Human and animal studies have demonstrated that Na+, K+-ATPase activity is impaired in the cell membrane of many tissues (see details in review)[127]. Thus, the impairment of Na+, K+-ATPase activity also plays an important role in the development of DAN by different pathways[128]. Furthermore, increased polyol pathway in DM has long been regarded as important in DAN[129]. Animal data suggests that glucose shunting through the polyol pathway alters nerve excitability due to the formation of sorbitol[130]. Furthermore, structural alterations of the nerves including thickening of the capillary basal membrane, loss of capillary pericyte coverage and endothelial hyperplasia, all lead to disturbances in capillary flow compromising the exchange of oxygen and glucose[131].
DM-induced sensory and motor dysfunction can affect part of or the entire GI tract, therefore, the perceived symptoms may be associated with one or several parts of the GI tract. In the patients of both IDDM and NIDDM, the GI symptoms are very common and can reach 75%[132-138]. Due to the non-specific nature of GI symptoms in DM patients, differential diagnoses should be considered when clinicians deal with GI symptoms. As DM-induced DAN can affect the enteric nerves supplying the small intestine and colon, abnormal motility, secretion, absorption and transportation can occur as possible outcomes. The clinical manifestation of these can be symptoms such as central abdominal pain, bloating, diarrhea, incontinence and constipation. An overrepresentation of celiac disease has been observed in insulin dependent DM patients, as this is a known etiologic factor of severe diarrhea, celiac disease should be excluded when clearing up the matter of general DM diarrhea[139]. Recent evidence indicates that GM is strongly associated with the development of type 1 and type 2 diabetes[97,140,141]. Furthermore, a close relationship between DM and increased risk of colon cancer has been demonstrated in both women and men[142,143]. DM is considered an independent risk factor for colon and rectal cancer[144].
Chronic diarrhea is a frequent presenting symptom, seen by both general practitioners and gastroenterologists. The differential diagnosis is broad, and diagnostic evaluation may be complicated[145,146]. Diarrhea is an important and often debilitating feature of DM enteropathy occurring in up to 20% of the patients[147]. It has also been reported that chronic diarrhea is more frequent in type I DM patients[148]. The diarrhea is typically painless, may be associated with fecal incontinence and occurs more often at night[149]. Therefore when gastroenterologists are confronted with patients suffering from chronic diarrhea, DM should be considered as a differential diagnosis, especially poorly controlled DM with co-existing DAN.
Many factors may relate to diarrhea in DM patients. These include food composition, intestinal motility disorders, GM changes, excessive loss of bile acids, pancreatic insufficiency and etc.[148,150-152]. Both increasing and decreasing GI transit time in DM patients may cause diarrhea. If the transit time become fast, intra-luminal contents reaching the caecum will increase[153]. If the transit time is slow, there is a risk of bacterial overgrowth. Therefore, both conditions can potentially induce DM diarrhea[154]. The etiology of DM diarrhea is not fully understood and is most likely multifactorial[4,155], involving reversible and irreversible processes. The diarrhea does not always correlate with the duration of DM or glycemic control, therefore DAN is thought to be a main underlying mechanism[156].
The colon likely plays a secondary or permissive role in patients with steatorrhea which could be caused by pancreatic insufficiency, celiac disease, or bacterial overgrowth[157]. However, the colonic dysfunction may be a primary contributor in DM diarrhea where the steatorrhea is absent. Other causes of diarrhea also need to be excluded, such as infectious diarrhea, celiac disease, bile salt diarrhea, and the concomitant use of drugs that may cause diarrhea such as metformin, GLP-1 receptor agonists, dipeptidyl peptidase 4 inhibitors, proton pump inhibitors, and statins[158] as well as functional diarrhea[159].
Constipation may be the most common GI complaint in DM patients[4,96,147,157,160-165]. Constipation also represents the most severe symptomatic problem[132]. The severe constipation may clinically present as obvious abdominal distention, severe nausea and vomiting as well as electrolyte disturbances[157]. Long-term and severe constipation may also cause stercoral ulcerations and perforation.
The etiology of DM constipation is not well understood; however, all factors in the DM patients affecting motor-sensory function of the colon are likely associated with constipation[164]. Among these factors, hyperglycemia is suggested to be the most important one. Inadequate glycemic control and consequent DAN have great influence on the sensory and motor functions of the GI tract[105]. DM angiopathy and vascular complications secondary to chronic hyperglycemia can also cause intestinal ischemia and impair nerve and muscle function resulting in DM gastroenteropathy[166]. Hyperglycemia causes apoptosis of enteric neurons and changes in their chemical code, resulting in motility changes[105]. It is well known that long-term hyperglycemia can induce the formation and accumulation of AGEs which play an important role for DAN[68-70]. ICC, together ENS and smooth muscles, play an important role in the regulation of motility[120]. One study demonstrated that a high dietary saturated fat intake is associated with significant increase in the prevalence of constipation in patients with uncontrolled DM[167]. The long term high dietary saturated fat consumption leading to slower GI motility and constipation may be related to gastrocolic reflux by several mechanisms. In addition, other factors such as stress, inflammation and functional changes in relation to DM may also be associated with constipation in DM patients[164].
The greatest concentration of microorganisms is found in the GI tract, and they consist mostly of bacteria[168]. The GM plays an important role in normal intestinal function and maintenance of the host health[168]. Composition of GM is affected by many factors such as diet, disease state, medications as well as host genetics. Therefore, GM has been associated with immune functions, immune mediated diseases, energy homeostasis and obesity[169,170]. To date, it has become increasingly evident that GM contributes to both type 1 and type 2 DM[140,141,171]. In recent years, many reviews have discussed the impact of GM on the development of obesity and DM[140,171-174]. However, to the best of our knowledge, there are few reviews which discuss how the DM-induced GI changes in turn affect the GM. It is well known that the GM inhabits the gut, therefore the DM-induced intestinal and colonic changes are likely to modify GM composition, in turn, the GM changes may also affect intestinal structure and motility.
As we discussed above in this review, motility disorders are common in diabetic patients[78-97]. There is evidence to suggest that modification of GI transit time can affect the composition of the GM community[175-177]. A close relationship exists between transit time and GM mass[175] and the motility shapes the composition and function of GM[176]. Therefore, the abnormal motility of gut in DM such as decreased or increased transit time can be an independent factor affecting the amount, the composition and the function of GM[178]. The changes of GM may further affect gut function through the brain-gut-axis[179]. The GM can interact with the gut-brain-axis by means of the modulation of afferent sensory nerves to modulate the motility of the intestine[180,181]. The GM can also directly affect the ENS by different molecular pathways[182,183]. Furthermore, the GM can modulate gut motility by nitric oxide generating pathway[184] and by interacting with the vanilloid receptor on capsaicin-sensitive nerve fibers[185].
The DM-induced intestinal histomorphological changes such as mucosa damage may also be related to GM modification and function. The leaky epithelium presumably alleviates the penetration of bacteria through the intestinal epithelium, initiating a pathologic cascade and disturbing the intestinal immunology, which is a critical element in the development of type 1DM[169]. On the other hand, the GM changes may also affect the integrity of intestinal mucosa[186] and smooth muscle functions[187]. The bidirectional interplay between GM and DM-induced intestinal changes contributes to the pathogenesis of GI disorders in DM.
GLP-1 regulates glucose homeostasis by stimulating the secretion of insulin from pancreatic β-cells[188] and plays important roles in metabolism as well as GI motility[188-190]. In relation to DM, GLP-1 acts as a pharmacological agent with definite therapeutic potential in DM treatment, regulating blood glucose by stimulating insulin secretion from insulin-producing β-cells in a blood-glucose dependent manner and inhibiting glucagon secretion from the glucagon-producing α-cells[191,192]. On other hand, it has been demonstrated that GLP-1 is progressively up-regulated in pancreatic islets during type 2 DM development[193]. More recently, the link between GLP-1/GLP-1 receptor (GLP-1R) expression and GI motility mediated by GM has been investigated[194]. They found that the expression of GLP-1R in myenteric neural cells in the GI tract was suppressed and the GI transit time became shorter in Germ-free (GF) mice after transplantation of GM. Therefore, they suggest that the GM accelerates the GI motility while suppressing the expression of GLP-1R in myenteric neural cells throughout the GI tract. There are also other anti-diabetic agents which act in the GI tract such as alpha-glucosidase inhibitors[195] and GLP-1 receptor agonists[196,197]. It is interesting to notice that alpha-glucosidase inhibitors and GLP-1 receptor agonists also affect the GM[198-200]. Alpha-glucosidase inhibitors such as acarbose treatment has been demonstrated to increase the content of gut Bifidobacterium longum and partially restore the imbalance of GM in patients with type 2 DM[198], and the changes in GM are strongly associated with the levels of various metabolic indicators[200]. In contrast, GLP-1 receptor agonists such as liraglutide seem to modulate the composition of the GM[199]. Other therapeutic agents targeting DM such as metformin[201] and antibiotics[202] also affect the GM. Thus, there is an interplay between drugs used for DM and the GM, however, the exact mechanism of the interaction is complex and needs to be investigated more thoroughly.
Type 2 DM mellitus has been reported to increase the risks of a wide spectrum of cancers including colorectal cancer[142-144,203-206]. Colorectal cancer is a significant health problem; it is one of the most common malignancy of the GI tract[207]. Therefore, understanding the association between DM and the risk of colon cancer is crucial.
Although some studies have reported no overall associations between DM and colon cancer risk[208-211], most studies support the finding of an association between DM and colon cancer. Large prospective studies have demonstrated that DM is associated with an increased risk of colon cancer in people investigated[211-217]. Many meta-analysis studies also support a correlation between DM and increased risk of colon cancer[142-144,218-222]. A population-based cohort study investigating the overall sex- and age-specific risks of colorectal cancer in association with DM was done by Chen et al[223]. They showed that DM significantly increased the risk of colorectal cancer, especially in patients aged 45-64 years. A multiethnic Cohort study also found that DM is a risk factor for colorectal cancer[224]. In addition, DM was found to negatively impact the survival outcomes of patients with colon cancer[225].
The mechanisms to explain the association between DM and increased colon cancer risk remain unclear. It has been demonstrated that AGEs and RAGE are up-regulated in the DM GI tract[49,64], and AGEs and RAGE are associated with DM-induced intestinal and colonic histomorphological remodeling[47,51] and DAN[125] which is closely related to motor-sensory disorders[9]. High glucose levels and AGEs increase the proliferation and migration of cultured colon cancer cells[226]. Hyperglycemia and AGEs could also induce oxidative stress and inflammation, which can cause further damage to the cellular components and contribute to malignant cell transformation[227]. Inflammation is a critical component of DM-induced target organ injury and colon cancer initiation and progression[228,229]. The inflammasome regulates the microbiota and the inflammatory response of epithelial cells to the GM[230], and the GM has been shown to be associated with GI malignancy including colonic cancer[231,232]. Recent studies suggest that RAGE signaling plays an important role in colorectal tumor progression[233]. Furthermore, AGEs may promote cancer cell proliferation through the activation of the RAGE signaling[234,235]. Therefore, hyperlipidemia, AGEs, inflammation, extracellular matrix alterations, and altered microbiota may induce GI tissue injury that may favor the development of colonic cancer. It has also been demonstrated that the slower bowel transit time in DM patients could enhance the exposure of the colorectal epithelium to carcinogens such as bile acids, nitrosamines and polycyclic hydrocarbons[236]. The above-mentioned findings show a possible link between DM-induced intestinal mechanophysiological changes and colonic cancer. The potential molecular mechanisms mediating the link between DM and colon-rectal cancer have been reviewed in detail recently[237], however the exact mechanisms need to be explored further. Furthermore, other factors as mentioned below are also likely associated with colon cancer. Metabolic syndrome, characterized by abdominal obesity, hyperglycemia, raised blood pressure, elevated triglyceride levels, and low high-density lipoprotein-cholesterol levels, is often seen in diabetic patients and has been reported to be associated with colon cancer[238-241]. As dietary fibers reduce the risk of metabolic syndrome, dietary fibers may have a role in the prevention of colon cancer in patients with type 2 DM[242]. Chronic hyperinsulinemic state and the elevation of insulin-like growth factor-1 levels may play a crucial role in the proliferation of cells and the occurrence of colon cancer[243] by different molecular mechanisms[244]. Elevated insulin receptor protein expression in colonic tumors has also been proposed as a possible biological mechanism for colonic tumorigenesis as in vivo studies have shown that insulin receptors contribute to cell transformation[245]. Different treatments of DM may also be related to colon cancer in DM patients. Chronic insulin therapy has been reported to be associated with an increased risk of colorectal adenoma[246] and cancer risk[247] among type 2 DM patients. Sulfonylureas stimulate endogenous insulin secretion and have therefore been suggested to be associated with an increased risk of colon cancer[248], however other reports showed that sulfonylurea use was associated with a lower colon cancer risk in DM patients[249]. Data on potential carcinogenic effects of thiazolidinediones are inconsistent, but most studies have found no increased risk of colon cancer[244,250,251] or even reduced risk of colon cancer. Metformin lowers the amount of circulating insulin and there is evidence on Metformin acting as a protective agent against colon cancer[234,252-254], this may be due to a reduction of the formation of precancerous lesions[255,256]. GLP-1-based therapeutic approaches have also been suggested as potential carcinogenic factors[102]. However, animal studies have shown that GLP-1 receptor activation reduced growth and survival in mouse CT26 colon cancer cells[257] and GLP-1 receptor agonists did not accelerate neoplasia in carcinogen treated mice[258]. A recent study also demonstrated that DM medication in general did not impact cancer recurrence or survival[259].
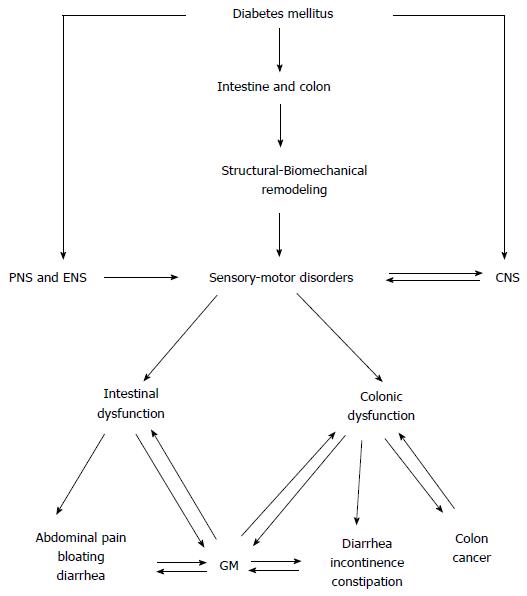
DM-induced intestinal and colon changes are summarized in Figure 4. DM is a chronic disease and is one of the major public health problems worldwide. Disorders of intestine and colon are common in DM. DM is associated with structural changes in the connective tissue matrix and in the muscles in the wall of intestine and colon and further causes biomechanical remodeling. As demonstrated in the text above, many mechanophysiological changes occur in the diabetic intestine and colon such as changed dimensions and changed passive and active tissue properties. Remodeling also occurs in the nerve structure and function. The interplay between these changes is extremely complex and need a scientific base to be explored fully. The changes may to various degrees be part of the mechanisms responsible for the intestinal and colonic sensory-motor disorders causing a variety of symptoms. The complexity is even more difficult to deal with since the symptoms are associated with changes in the central processing of visceral afferent signals from the gut wall. As DM-induced DAN can affect the enteric nerves supplying the intestine and colon, abnormal motility, secretion, absorption and transportation can occur. This presents clinically as symptoms including central abdominal pain, bloating, diarrhea, incontinence and constipation. The DM-induced structural changes and motility disorders of the intestines are associated with GM changes in DM, on the contrary the GM changes may in turn affect intestinal structure and motility. Furthermore, studies suggest an association between DM and increased risk of colon cancer in both women and men, and the link between DM-induced intestinal mechanophysiological changes and colon cancer need to be explored further. Therefore, an insight into DM-induced intestinal and colonic changes and the clinical consequences is important in order to explore better treatment approaches for the gut disorders in diabetic patients.
Manuscript source: Invited manuscript
Specialty type: Endocrinology and metabolism
Country of origin: Denmark
Peer-review report classification
Grade A (Excellent): 0
Grade B (Very good): B, B, B
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P- Reviewer: Cui J, Fatima SS, Hamasaki H, Saisho Y S- Editor: Song XX L- Editor: A E- Editor: Wu HL
| 1. | NCD Risk Factor Collaboration (NCD-RisC). Worldwide trends in diabetes since 1980: a pooled analysis of 751 population-based studies with 4.4 million participants. Lancet. 2016;387:1513-1530. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2594] [Cited by in RCA: 2533] [Article Influence: 281.4] [Reference Citation Analysis (0)] |
| 2. | Seuring T, Archangelidi O, Suhrcke M. The Economic Costs of Type 2 Diabetes: A Global Systematic Review. Pharmacoeconomics. 2015;33:811-831. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 557] [Cited by in RCA: 517] [Article Influence: 51.7] [Reference Citation Analysis (0)] |
| 3. | Horowitz M, Samsom M. Gastrointestinal function in diabetes mellitus. Chichester: John Wiley & Sons, Ltd 2004; . |
| 4. | Shakil A, Church RJ, Rao SS. Gastrointestinal complications of diabetes. Am Fam Physician. 2008;77:1697-1702. [PubMed] |
| 5. | Frokjaer JB, Andersen SD, Ejskjaer N, Funch-Jensen P, Drewes AM, Gregersen H. Impaired contractility and remodeling of the upper gastrointestinal tract in diabetes mellitus type-1. World J Gastroenterol. 2007;13:4881-4890. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 39] [Cited by in RCA: 39] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 6. | Brock C, Søfteland E, Gunterberg V, Frøkjær JB, Lelic D, Brock B, Dimcevski G, Gregersen H, Simrén M, Drewes AM. Diabetic autonomic neuropathy affects symptom generation and brain-gut axis. Diabetes Care. 2013;36:3698-3705. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 44] [Cited by in RCA: 51] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 7. | Yarandi SS, Srinivasan S. Diabetic gastrointestinal motility disorders and the role of enteric nervous system: current status and future directions. Neurogastroenterol Motil. 2014;26:611-624. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 116] [Cited by in RCA: 144] [Article Influence: 13.1] [Reference Citation Analysis (0)] |
| 8. | Zhao J, Yang J, Gregersen H. Biomechanical and morphometric intestinal remodelling during experimental diabetes in rats. Diabetologia. 2003;46:1688-1697. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 62] [Cited by in RCA: 66] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 9. | Zhao J, Frøkjaer JB, Drewes AM, Ejskjaer N. Upper gastrointestinal sensory-motor dysfunction in diabetes mellitus. World J Gastroenterol. 2006;12:2846-2857. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 53] [Cited by in RCA: 52] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 10. | Zhao J, Nakaguchi T, Gregersen H. Biomechanical and histomorphometric colon remodelling in STZ-induced diabetic rats. Dig Dis Sci. 2009;54:1636-1642. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 28] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 11. | Marathe CS, Rayner CK, Jones KL, Horowitz M. Novel insights into the effects of diabetes on gastric motility. Expert Rev Gastroenterol Hepatol. 2016;10:581-593. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 6] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 12. | Zhao J, Gregersen H. Diabetes-induced mechanophysiological changes in the esophagus. Ann N Y Acad Sci. 2016;1380:139-154. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 13] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 13. | Shafik AA, Ahmed IA, Shafik A, Wahdan M, Asaad S, El Neizamy E. Ileocecal junction: anatomic, histologic, radiologic and endoscopic studies with special reference to its antireflux mechanism. Surg Radiol Anat. 2011;33:249-256. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 18] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 14. | Wedel T, Roblick U, Gleiss J, Schiedeck T, Bruch HP, Kühnel W, Krammer HJ. Organization of the enteric nervous system in the human colon demonstrated by wholemount immunohistochemistry with special reference to the submucous plexus. Ann Anat. 1999;181:327-337. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 80] [Cited by in RCA: 80] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 15. | Furness JB, Callaghan BP, Rivera LR, Cho HJ. The enteric nervous system and gastrointestinal innervation: integrated local and central control. Adv Exp Med Biol. 2014;817:39-71. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 419] [Cited by in RCA: 533] [Article Influence: 48.5] [Reference Citation Analysis (1)] |
| 16. | Mandić P, Filipović T, Gasić M, Djukić-Macut N, Filipović M, Bogosavljević I. Quantitative morphometric analysis of the myenteric nervous plexus ganglion structures along the human digestive tract. Vojnosanit Pregl. 2016;73:559-565. [PubMed] |
| 17. | Rumessen JJ. Identification of interstitial cells of Cajal. Significance for studies of human small intestine and colon. Dan Med Bull. 1994;41:275-293. [PubMed] |
| 18. | Streutker CJ, Huizinga JD, Driman DK, Riddell RH. Interstitial cells of Cajal in health and disease. Part I: normal ICC structure and function with associated motility disorders. Histopathology. 2007;50:176-189. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 92] [Cited by in RCA: 101] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 19. | Gregersen H, Orvar K, Christensen J. Biomechanical properties of duodenal wall and duodenal tone during phase I and phase II of the MMC. Am J Physiol. 1992;263:G795-G801. [PubMed] |
| 20. | Storkholm JH, Villadsen GE, Jensen SL, Gregersen H. Passive elastic wall properties in isolated guinea pig small intestine. Dig Dis Sci. 1995;40:976-982. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 20] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 21. | Duch BU, Petersen JA, Vinter-Jensen L, Gregersen H. Elastic properties in the circumferential direction in isolated rat small intestine. Acta Physiol Scand. 1996;157:157-163. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 14] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 22. | Gao C, Arendt-Nielsen L, Liu W, Petersen P, Drewes AM, Gregersen H. Sensory and biomechanical responses to ramp-controlled distension of the human duodenum. Am J Physiol Gastrointest Liver Physiol. 2003;284:G461-G471. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 38] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 23. | Frøkjaer JB, Andersen SD, Drewes AM, Gregersen H. Ultrasound-determined geometric and biomechanical properties of the human duodenum. Dig Dis Sci. 2006;51:1662-1669. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 21] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 24. | Dou Y, Zhao J, Gregersen H. Morphology and stress-strain properties along the small intestine in the rat. J Biomech Eng. 2003;125:266-273. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 32] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 25. | Zhao JB, Sha H, Zhuang FY, Gregersen H. Morphological properties and residual strain along the small intestine in rats. World J Gastroenterol. 2002;8:312-317. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 21] [Cited by in RCA: 23] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 26. | Gabella G, Blundell D. Gap junctions of the muscles of the small and large intestine. Cell Tissue Res. 1981;219:469-488. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 36] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 27. | Gao C, Zhao J, Gregersen H. Histomorphometry and strain distribution in pig duodenum with reference to zero-stress state. Dig Dis Sci. 2000;45:1500-1508. [PubMed] |
| 28. | Smith JB, Zhao JB, Dou YL, Gregersen H. Time-dependent viscoelastic properties along rat small intestine. World J Gastroenterol. 2005;11:4974-4978. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 8] [Cited by in RCA: 10] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 29. | Fackler K, Klein L, Hiltner A. Polarizing light microscopy of intestine and its relationship to mechanical behaviour. J Microsc. 1981;124:305-311. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 25] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 30. | Storkholm JH, Villadsen GE, Jensen SL, Gregersen H. Mechanical properties and collagen content differ between isolated guinea pig duodenum, jejunum, and distal ileum. Dig Dis Sci. 1998;43:2034-2041. [PubMed] |
| 31. | Chen X, Zhao J, Gregersen H. The villi contribute to the mechanics in the guinea pig small intestine. J Biomech. 2008;41:806-812. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 13] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 32. | Schulze-Delrieu K. Intrinsic differences in the filling response of the guinea pig duodenum and ileum. J Lab Clin Med. 1991;117:44-50. [PubMed] |
| 33. | Watters DA, Smith AN, Eastwood MA, Anderson KC, Elton RA. Mechanical properties of the rat colon: the effect of age, sex and different conditions of storage. Q J Exp Physiol. 1985;70:151-162. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 41] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 34. | Bharucha AE, Hubmayr RD, Ferber IJ, Zinsmeister AR. Viscoelastic properties of the human colon. Am J Physiol Gastrointest Liver Physiol. 2001;281:G459-G466. [PubMed] |
| 35. | Gao C, Gregersen H. Biomechanical and morphological properties in rat large intestine. J Biomech. 2000;33:1089-1097. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 35] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 36. | Frøkjaer JB, Liao D, Steffensen E, Dimcevski G, Bergmann A, Drewes AM, Gregersen H. Geometric and mechanosensory properties of the sigmoid colon evaluated with magnetic resonance imaging. Neurogastroenterol Motil. 2007;19:253-262. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 6] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 37. | Ford MJ, Camilleri M, Wiste JA, Hanson RB. Differences in colonic tone and phasic response to a meal in the transverse and sigmoid human colon. Gut. 1995;37:264-269. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 75] [Cited by in RCA: 69] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 38. | Gregersen H. Biomechanics of the Gastrointestinal Tract. London: Springer-Verlag 2002; . |
| 39. | Tanaka H, Hirose M, Osada T, Miwa H, Watanabe S, Sato N. Implications of mechanical stretch on wound repair of gastric smooth muscle cells in vitro. Dig Dis Sci. 2000;45:2470-2477. [PubMed] |
| 40. | Liao D, Sevcencu C, Yoshida K, Gregersen H. Viscoelastic properties of isolated rat colon smooth muscle cells. Cell Biol Int. 2006;30:854-858. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 9] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 41. | Zoubi SA, Mayhew TM, Sparrow RA. The small intestine in experimental diabetes: cellular adaptation in crypts and villi at different longitudinal sites. Virchows Arch. 1995;426:501-507. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 35] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 42. | Verne GN, Sninsky CA. Diabetes and the gastrointestinal tract. Gastroenterol Clin North Am. 1998;27:861-874, vi-vii. [PubMed] |
| 43. | Folwaczny C, Hundegger K, Volger C, Sorodoc J, Kühn M, Tatsch K, Landgraf R, Karbach U. Measurement of transit disorders in different gastrointestinal segments of patients with diabetes mellitus in relation to duration and severity of the disease by use of the metal-detector test. Z Gastroenterol. 1995;33:517-526. [PubMed] |
| 44. | Noda T, Iwakiri R, Fujimoto K, Yoshida T, Utsumi H, Sakata H, Hisatomi A, Aw TY. Suppression of apoptosis is responsible for increased thickness of intestinal mucosa in streptozotocin-induced diabetic rats. Metabolism. 2001;50:259-264. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 24] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 45. | Tormo MA, Martínez IM, Romero de Tejada A, Gil-Exojo I, Campillo JE. Morphological and enzymatic changes of the small intestine in an n0-STZ diabetes rat model. Exp Clin Endocrinol Diabetes. 2002;110:119-123. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 14] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 46. | Adachi T, Mori C, Sakurai K, Shihara N, Tsuda K, Yasuda K. Morphological changes and increased sucrase and isomaltase activity in small intestines of insulin-deficient and type 2 diabetic rats. Endocr J. 2003;50:271-279. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 66] [Cited by in RCA: 68] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 47. | Zhao J, Chen P, Gregersen H. Morpho-mechanical intestinal remodeling in type 2 diabetic GK rats--is it related to advanced glycation end product formation? J Biomech. 2013;46:1128-1134. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 28] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 48. | Sha H, Zhao JB, Zhang ZY, Zhou SP, Tong XL, Zhuang FY, Gregersen H. Effect of Kaiyu Qingwei Jianji on the morphometry and residual strain distribution of small intestine in experimental diabetic rats. World J Gastroenterol. 2006;12:7149-7154. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 4] [Cited by in RCA: 9] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 49. | Chen P, Zhao J, Gregersen H. Up-regulated expression of advanced glycation end-products and their receptor in the small intestine and colon of diabetic rats. Dig Dis Sci. 2012;57:48-57. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 52] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 50. | Liu GF, Zhao JB, Zhen Z, Sha H, Chen PM, Li M, Zhang JC, Yuan MZ, Gao W, Gregersen H. Effect of tangweian jianji on upper gastrointestinal remodeling in streptozotocin-induced diabetic rats. World J Gastroenterol. 2012;18:4875-4884. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 6] [Cited by in RCA: 12] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 51. | Siegman MJ, Eto M, Butler TM. Remodeling of the rat distal colon in diabetes: function and ultrastructure. Am J Physiol Cell Physiol. 2016;310:C151-C160. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 13] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 52. | Sha H, Zhao D, Tong X, Gregersen H, Zhao J. Mechanism Investigation of the Improvement of Chang Run Tong on the Colonic Remodeling in Streptozotocin-Induced Diabetic Rats. J Diabetes Res. 2016;2016:1826281. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 3] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 53. | Jørgensen CS, Ahrensberg JM, Gregersen H, Flyvberg A. Tension-strain relations and morphometry of rat small intestine in experimental diabetes. Dig Dis Sci. 2001;46:960-967. [PubMed] |
| 54. | Jervis EL, Levin RJ. Anatomic adaptation of the alimentary tract of the rat to the hyperphagia of chronic alloxan-diabetes. Nature. 1966;210:391-393. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 77] [Cited by in RCA: 76] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 55. | Miller DL, Hanson W, Schedl HP, Osborne JW. Proliferation rate and transit time of mucosal cells in small intestine of the diabetic rat. Gastroenterology. 1977;73:1326-1332. [PubMed] |
| 56. | Granneman JG, Stricker EM. Food intake and gastric emptying in rats with streptozotocin-induced diabetes. Am J Physiol. 1984;247:R1054-R1061. [PubMed] |
| 57. | Fischer KD, Dhanvantari S, Drucker DJ, Brubaker PL. Intestinal growth is associated with elevated levels of glucagon-like peptide 2 in diabetic rats. Am J Physiol. 1997;273:E815-E820. [PubMed] |
| 58. | Vahl TP, D’Alessio DA. Gut peptides in the treatment of diabetes mellitus. Expert Opin Investig Drugs. 2004;13:177-188. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 23] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 59. | Singh R, Barden A, Mori T, Beilin L. Advanced glycation end-products: a review. Diabetologia. 2001;44:129-146. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1761] [Cited by in RCA: 1791] [Article Influence: 74.6] [Reference Citation Analysis (0)] |
| 60. | Monnier VM, Sell DR, Nagaraj RH, Miyata S, Grandhee S, Odetti P, Ibrahim SA. Maillard reaction-mediated molecular damage to extracellular matrix and other tissue proteins in diabetes, aging, and uremia. Diabetes. 1992;41 Suppl 2:36-41. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 218] [Cited by in RCA: 214] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 61. | Ulrich P, Cerami A. Protein glycation, diabetes, and aging. Recent Prog Horm Res. 2001;56:1-21. [PubMed] |
| 62. | Sánchez SS, Genta SB, Aybar MJ, Honoré SM, Villecco EI, Sánchez Riera AN. Changes in the expression of small intestine extracellular matrix proteins in streptozotocin-induced diabetic rats. Cell Biol Int. 2000;24:881-888. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 19] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 63. | Reddy GK. AGE-related cross-linking of collagen is associated with aortic wall matrix stiffness in the pathogenesis of drug-induced diabetes in rats. Microvasc Res. 2004;68:132-142. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 88] [Cited by in RCA: 95] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 64. | Chen PM, Gregersen H, Zhao JB. Advanced glycation end-product expression is upregulated in the gastrointestinal tract of type 2 diabetic rats. World J Diabetes. 2015;6:662-672. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 18] [Cited by in RCA: 24] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 65. | Bierhaus A, Humpert PM, Morcos M, Wendt T, Chavakis T, Arnold B, Stern DM, Nawroth PP. Understanding RAGE, the receptor for advanced glycation end products. J Mol Med (Berl). 2005;83:876-886. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 863] [Cited by in RCA: 955] [Article Influence: 47.8] [Reference Citation Analysis (0)] |
| 66. | Stern DM, Yan SD, Yan SF, Schmidt AM. Receptor for advanced glycation endproducts (RAGE) and the complications of diabetes. Ageing Res Rev. 2002;1:1-15. [PubMed] |
| 67. | Yamagishi S, Fukami K, Matsui T. Crosstalk between advanced glycation end products (AGEs)-receptor RAGE axis and dipeptidyl peptidase-4-incretin system in diabetic vascular complications. Cardiovasc Diabetol. 2015;14:2. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 87] [Cited by in RCA: 92] [Article Influence: 9.2] [Reference Citation Analysis (0)] |
| 68. | Thornalley PJ. Glycation in diabetic neuropathy: characteristics, consequences, causes, and therapeutic options. Int Rev Neurobiol. 2002;50:37-57. [PubMed] |
| 69. | Sugimoto K, Yasujima M, Yagihashi S. Role of advanced glycation end products in diabetic neuropathy. Curr Pharm Des. 2008;14:953-961. [PubMed] |
| 70. | Singh VP, Bali A, Singh N, Jaggi AS. Advanced glycation end products and diabetic complications. Korean J Physiol Pharmacol. 2014;18:1-14. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 750] [Cited by in RCA: 961] [Article Influence: 87.4] [Reference Citation Analysis (0)] |
| 71. | Wada R, Nishizawa Y, Yagihashi N, Takeuchi M, Ishikawa Y, Yasumura K, Nakano M, Yagihashi S. Effects of OPB-9195, anti-glycation agent, on experimental diabetic neuropathy. Eur J Clin Invest. 2001;31:513-520. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 66] [Cited by in RCA: 66] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 72. | Sugimoto K, Nishizawa Y, Horiuchi S, Yagihashi S. Localization in human diabetic peripheral nerve of N(epsilon)-carboxymethyllysine-protein adducts, an advanced glycation endproduct. Diabetologia. 1997;40:1380-1387. [PubMed] |
| 73. | Wada R, Yagihashi S. Role of advanced glycation end products and their receptors in development of diabetic neuropathy. Ann N Y Acad Sci. 2005;1043:598-604. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 169] [Cited by in RCA: 178] [Article Influence: 8.9] [Reference Citation Analysis (0)] |
| 74. | Sekido H, Suzuki T, Jomori T, Takeuchi M, Yabe-Nishimura C, Yagihashi S. Reduced cell replication and induction of apoptosis by advanced glycation end products in rat Schwann cells. Biochem Biophys Res Commun. 2004;320:241-248. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 65] [Cited by in RCA: 66] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 75. | Vlassara H, Brownlee M, Cerami A. Nonenzymatic glycosylation of peripheral nerve protein in diabetes mellitus. Proc Natl Acad Sci USA. 1981;78:5190-5192. [PubMed] |
| 76. | Williams SK, Howarth NL, Devenny JJ, Bitensky MW. Structural and functional consequences of increased tubulin glycosylation in diabetes mellitus. Proc Natl Acad Sci USA. 1982;79:6546-6550. [PubMed] |
| 77. | Yagihashi S, Mizukami H, Sugimoto K. Mechanism of diabetic neuropathy: Where are we now and where to go? J Diabetes Investig. 2011;2:18-32. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 243] [Cited by in RCA: 320] [Article Influence: 29.1] [Reference Citation Analysis (0)] |
| 78. | El-Salhy M. Gastrointestinal transit in nonobese diabetic mouse: an animal model of human diabetes type 1. J Diabetes Complications. 2001;15:277-284. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 16] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 79. | El-Salhy M. Gastrointestinal transit in an animal model of human diabetes type 2: relationship to gut neuroendocrine peptide contents. Ups J Med Sci. 2002;107:101-110. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 14] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 80. | Anjaneyulu M, Ramarao P. Studies on gastrointestinal tract functional changes in diabetic animals. Methods Find Exp Clin Pharmacol. 2002;24:71-75. [PubMed] |
| 81. | Zhao J, Chen P, Gregersen H. Stress-strain analysis of jejunal contractility in response to flow and ramp distension in type 2 diabetic GK rats: effect of carbachol stimulation. J Biomech. 2013;46:2469-2476. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 8] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 82. | Zhao JB, Chen PM, Gregersen H. Changes of phasic and tonic smooth muscle function of jejunum in type 2 diabetic Goto-Kakizaki rats. World J Diabetes. 2013;4:339-348. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 5] [Cited by in RCA: 3] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 83. | Zhao J, Chen P, Gregersen H. Stress-strain analysis of contractility in the ileum in response to flow and ramp distension in streptozotocin-induced diabetic rats--association with advanced glycation end product formation. J Biomech. 2015;48:1075-1083. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 84. | de Boer SY, Masclee AA, lam WF, Schipper J, Jansen JB, Lamers CB. Hyperglycemia modulates gallbladder motility and small intestinal transit time in man. Dig Dis Sci. 1993;38:2228-2235. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 35] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 85. | Iida M, Ikeda M, Kishimoto M, Tsujino T, Kaneto H, Matsuhisa M, Kajimoto Y, Watarai T, Yamasaki Y, Hori M. Evaluation of gut motility in type II diabetes by the radiopaque marker method. J Gastroenterol Hepatol. 2000;15:381-385. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 36] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 86. | Keshavarzian A, Iber FL, Dangleis MD, Cornish R. Intestinal-transit and lactose intolerance in chronic alcoholics. Am J Clin Nutr. 1986;44:70-76. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 8] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 87. | Nguyen HN, Silny J, Wüller S, Marschall HU, Rau G, Matern S. Abnormal postprandial duodenal chyme transport in patients with long standing insulin dependent diabetes mellitus. Gut. 1997;41:624-631. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 32] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 88. | Camilleri M, Malagelada JR. Abnormal intestinal motility in diabetics with the gastroparesis syndrome. Eur J Clin Invest. 1984;14:420-427. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 242] [Cited by in RCA: 219] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 89. | Dooley CP, el Newihi HM, Zeidler A, Valenzuela JE. Abnormalities of the migrating motor complex in diabetics with autonomic neuropathy and diarrhea. Scand J Gastroenterol. 1988;23:217-223. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 58] [Cited by in RCA: 53] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 90. | Samsom M, Jebbink RJ, Akkermans LM, van Berge-Henegouwen GP, Smout AJ. Abnormalities of antroduodenal motility in type I diabetes. Diabetes Care. 1996;19:21-27. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 48] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 91. | Battle WM, Snape WJ, Alavi A, Cohen S, Braunstein S. Colonic dysfunction in diabetes mellitus. Gastroenterology. 1980;79:1217-1221. [PubMed] |
| 92. | Kawagishi T, Nishizawa Y, Okuno Y, Sekiya K, Morii H. Segmental gut transit in diabetes mellitus: effect of cisapride. Diabetes Res Clin Pract. 1992;17:137-144. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 18] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 93. | Iber FL, Parveen S, Vandrunen M, Sood KB, Reza F, Serlovsky R, Reddy S. Relation of symptoms to impaired stomach, small bowel, and colon motility in long-standing diabetes. Dig Dis Sci. 1993;38:45-50. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 67] [Cited by in RCA: 67] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 94. | Jung HK, Kim DY, Moon IH, Hong YS. Colonic transit time in diabetic patients--comparison with healthy subjects and the effect of autonomic neuropathy. Yonsei Med J. 2003;44:265-272. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 43] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 95. | Jorge JX, Matos HC, Machado JP, Almeida CC. Transit of radiopaque particles through the gastrointestinal tract: comparison between type 2 diabetes patients and healthy individuals. Rev Esp Enferm Dig. 2012;104:118-121. [PubMed] |
| 96. | Bharucha AE, Low P, Camilleri M, Veil E, Burton D, Kudva Y, Shah P, Gehrking T, Zinsmeister AR. A randomised controlled study of the effect of cholinesterase inhibition on colon function in patients with diabetes mellitus and constipation. Gut. 2013;62:708-715. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 69] [Cited by in RCA: 61] [Article Influence: 5.1] [Reference Citation Analysis (0)] |
| 97. | Horváth VJ, Putz Z, Izbéki F, Körei AE, Gerő L, Lengyel C, Kempler P, Várkonyi T. Diabetes-related dysfunction of the small intestine and the colon: focus on motility. Curr Diab Rep. 2015;15:94. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 39] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 98. | Qiu WC, Wang ZG, Lv R, Wang WG, Han XD, Yan J, Wang Y, Zheng Q, Ai KX. Ghrelin improves delayed gastrointestinal transit in alloxan-induced diabetic mice. World J Gastroenterol. 2008;14:2572-2577. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 30] [Cited by in RCA: 30] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 99. | Yamamoto T, Watabe K, Nakahara M, Ogiyama H, Kiyohara T, Tsutsui S, Tamura S, Shinomura Y, Hayashi N. Disturbed gastrointestinal motility and decreased interstitial cells of Cajal in diabetic db/db mice. J Gastroenterol Hepatol. 2008;23:660-667. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 60] [Cited by in RCA: 68] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 100. | Kim SJ, Park JH, Song DK, Park KS, Lee JE, Kim ES, Cho KB, Jang BK, Chung WJ, Hwang JS. Alterations of colonic contractility in long-term diabetic rat model. J Neurogastroenterol Motil. 2011;17:372-380. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 23] [Cited by in RCA: 28] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 101. | Wang Y, Xu XY, Tang YR, Yang WW, Yuan YF, Ning YJ, Yu YJ, Lin L. Effect of endogenous insulin-like growth factor and stem cell factor on diabetic colonic dysmotility. World J Gastroenterol. 2013;19:3324-3331. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 12] [Cited by in RCA: 18] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 102. | Sun M, Wang F, Feng P. Insulin-like growth factor-1 inhibits colonic smooth muscle cell apoptosis in diabetic rats with colonic dysmotility. Regul Pept. 2014;194-195:41-48. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 103. | Sung TS, La JH, Kang TM, Kim TW, Yang IS. Visceral Hypersensitivity and Altered Colonic Motility in Type 2 Diabetic Rat. J Neurogastroenterol Motil. 2015;21:581-588. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 7] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 104. | Sims MA, Hasler WL, Chey WD, Kim MS, Owyang C. Hyperglycemia inhibits mechanoreceptor-mediated gastrocolonic responses and colonic peristaltic reflexes in healthy humans. Gastroenterology. 1995;108:350-359. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 66] [Cited by in RCA: 64] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 105. | Chandrasekharan B, Anitha M, Blatt R, Shahnavaz N, Kooby D, Staley C, Mwangi S, Jones DP, Sitaraman SV, Srinivasan S. Colonic motor dysfunction in human diabetes is associated with enteric neuronal loss and increased oxidative stress. Neurogastroenterol Motil. 2011;23:131-138, e26. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 140] [Cited by in RCA: 141] [Article Influence: 10.1] [Reference Citation Analysis (0)] |
| 106. | Domènech A, Pasquinelli G, De Giorgio R, Gori A, Bosch F, Pumarola M, Jiménez M. Morphofunctional changes underlying intestinal dysmotility in diabetic RIP-I/hIFNβ transgenic mice. Int J Exp Pathol. 2011;92:400-412. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 35] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 107. | Wang CL, Wang X, Yu Y, Cui Y, Liu HM, Lai LH, Guo C, Liu J, Wang R. Type 1 diabetes attenuates the modulatory effects of endomorphins on mouse colonic motility. Neuropeptides. 2008;42:69-77. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 14] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 108. | Touw K, Chakraborty S, Zhang W, Obukhov AG, Tune JD, Gunst SJ, Herring BP. Altered calcium signaling in colonic smooth muscle of type 1 diabetic mice. Am J Physiol Gastrointest Liver Physiol. 2012;302:G66-G76. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 21] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 109. | Forrest A, Parsons M. The enhanced spontaneous activity of the diabetic colon is not the consequence of impaired inhibitory control mechanisms. Auton Autacoid Pharmacol. 2003;23:149-158. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 20] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 110. | Forrest A, Huizinga JD, Wang XY, Liu LW, Parsons M. Increase in stretch-induced rhythmic motor activity in the diabetic rat colon is associated with loss of ICC of the submuscular plexus. Am J Physiol Gastrointest Liver Physiol. 2008;294:G315-G326. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 35] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 111. | Yoneda S, Kadowaki M, Kuramoto H, Fukui H, Takaki M. Enhanced colonic peristalsis by impairment of nitrergic enteric neurons in spontaneously diabetic rats. Auton Neurosci. 2001;92:65-71. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 41] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 112. | Xie DP, Li S, Li L, Chang XW, Xi TF, Yang X, Jin Z, Zeng Y. Beta-arrestin2 is involved in the increase of distal colonic contraction in diabetic rats. Regul Pept. 2013;185:29-33. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 5] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 113. | Chang XW, Qin Y, Jin Z, Xi TF, Yang X, Lu ZH, Tang YP, Cai WT, Chen SJ, Xie DP. Interleukin-6 (IL-6) mediated the increased contraction of distal colon in streptozotocin-induced diabetes in rats via IL-6 receptor pathway. Int J Clin Exp Pathol. 2015;8:4514-4524. [PubMed] |
| 114. | Frøkjaer JB, Andersen SD, Ejskaer N, Funch-Jensen P, Arendt-Nielsen L, Gregersen H, Drewes AM. Gut sensations in diabetic autonomic neuropathy. Pain. 2007;131:320-329. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 47] [Cited by in RCA: 50] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 115. | Grabauskas G, Heldsinger A, Wu X, Xu D, Zhou S, Owyang C. Diabetic visceral hypersensitivity is associated with activation of mitogen-activated kinase in rat dorsal root ganglia. Diabetes. 2011;60:1743-1751. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 25] [Cited by in RCA: 28] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 116. | Hu J, Song ZY, Zhang HH, Qin X, Hu S, Jiang X, Xu GY. Colonic Hypersensitivity and Sensitization of Voltage-gated Sodium Channels in Primary Sensory Neurons in Rats with Diabetes. J Neurogastroenterol Motil. 2016;22:129-140. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 14] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 117. | Drewes AM, Søfteland E, Dimcevski G, Farmer AD, Brock C, Frøkjær JB, Krogh K, Drewes AM. Brain changes in diabetes mellitus patients with gastrointestinal symptoms. World J Diabetes. 2016;7:14-26. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 19] [Cited by in RCA: 19] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 118. | Chandrasekharan B, Srinivasan S. Diabetes and the enteric nervous system. Neurogastroenterol Motil. 2007;19:951-960. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 172] [Cited by in RCA: 112] [Article Influence: 6.2] [Reference Citation Analysis (1)] |
| 119. | Azpiroz F, Malagelada C. Diabetic neuropathy in the gut: pathogenesis and diagnosis. Diabetologia. 2016;59:404-408. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 45] [Cited by in RCA: 48] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 120. | Pasternak A, Szura M, Gil K, Matyja A. Interstitial cells of Cajal - systematic review. Folia Morphol (Warsz). 2016;75:281-286. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 29] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 121. | Ward SM, Sanders KM. Involvement of intramuscular interstitial cells of Cajal in neuroeffector transmission in the gastrointestinal tract. J Physiol. 2006;576:675-682. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 113] [Cited by in RCA: 112] [Article Influence: 5.9] [Reference Citation Analysis (0)] |
| 122. | Wang XY, Huizinga JD, Diamond J, Liu LW. Loss of intramuscular and submuscular interstitial cells of Cajal and associated enteric nerves is related to decreased gastric emptying in streptozotocin-induced diabetes. Neurogastroenterol Motil. 2009;21:1095-1e92. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 65] [Cited by in RCA: 68] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 123. | Lammers WJ, Al-Bloushi HM, Al-Eisaei SA, Al-Dhaheri FA, Stephen B, John R, Dhanasekaran S, Karam SM. Slow wave propagation and plasticity of interstitial cells of Cajal in the small intestine of diabetic rats. Exp Physiol. 2011;96:1039-1048. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 41] [Cited by in RCA: 39] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 124. | Lin L, Xu LM, Zhang W, Ge YB, Tang YR, Zhang HJ, Li XL, Chen JD. Roles of stem cell factor on the depletion of interstitial cells of Cajal in the colon of diabetic mice. Am J Physiol Gastrointest Liver Physiol. 2010;298:G241-G247. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 42] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 125. | Babizhayev MA, Strokov IA, Nosikov VV, Savel’yeva EL, Sitnikov VF, Yegorov YE, Lankin VZ. The Role of Oxidative Stress in Diabetic Neuropathy: Generation of Free Radical Species in the Glycation Reaction and Gene Polymorphisms Encoding Antioxidant Enzymes to Genetic Susceptibility to Diabetic Neuropathy in Population of Type I Diabetic Patients. Cell Biochem Biophys. 2015;71:1425-1443. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 72] [Cited by in RCA: 99] [Article Influence: 11.0] [Reference Citation Analysis (0)] |
| 126. | Wahren J, Ekberg K, Johansson J, Henriksson M, Pramanik A, Johansson BL, Rigler R, Jörnvall H. Role of C-peptide in human physiology. Am J Physiol Endocrinol Metab. 2000;278:E759-E768. [PubMed] |
| 127. | Vague P, Coste TC, Jannot MF, Raccah D, Tsimaratos M. C-peptide, Na+,K(+)-ATPase, and diabetes. Exp Diabesity Res. 2004;5:37-50. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 80] [Cited by in RCA: 90] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 128. | Lattimer SA, Sima AA, Greene DA. In vitro correction of impaired Na+-K+-ATPase in diabetic nerve by protein kinase C agonists. Am J Physiol. 1989;256:E264-E269. [PubMed] |
| 129. | Cameron NE, Eaton SE, Cotter MA, Tesfaye S. Vascular factors and metabolic interactions in the pathogenesis of diabetic neuropathy. Diabetologia. 2001;44:1973-1988. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 452] [Cited by in RCA: 451] [Article Influence: 18.8] [Reference Citation Analysis (0)] |
| 130. | Krishnan AV, Kiernan MC. Altered nerve excitability properties in established diabetic neuropathy. Brain. 2005;128:1178-1187. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 93] [Cited by in RCA: 100] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 131. | Østergaard L, Finnerup NB, Terkelsen AJ, Olesen RA, Drasbek KR, Knudsen L, Jespersen SN, Frystyk J, Charles M, Thomsen RW. The effects of capillary dysfunction on oxygen and glucose extraction in diabetic neuropathy. Diabetologia. 2015;58:666-677. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 51] [Cited by in RCA: 60] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 132. | Ko GT, Chan WB, Chan JC, Tsang LW, Cockram CS. Gastrointestinal symptoms in Chinese patients with Type 2 diabetes mellitus. Diabet Med. 1999;16:670-674. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 75] [Cited by in RCA: 75] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 133. | Maleki D, Locke GR, Camilleri M, Zinsmeister AR, Yawn BP, Leibson C, Melton LJ. Gastrointestinal tract symptoms among persons with diabetes mellitus in the community. Arch Intern Med. 2000;160:2808-2816. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 187] [Cited by in RCA: 169] [Article Influence: 6.8] [Reference Citation Analysis (0)] |
| 134. | Ricci JA, Siddique R, Stewart WF, Sandler RS, Sloan S, Farup CE. Upper gastrointestinal symptoms in a U.S. national sample of adults with diabetes. Scand J Gastroenterol. 2000;35:152-159. [PubMed] |
| 135. | Schvarcz E, Palmér M, Ingberg CM, Aman J, Berne C. Increased prevalence of upper gastrointestinal symptoms in long-term type 1 diabetes mellitus. Diabet Med. 1996;13:478-481. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 136. | Spångéus A, El-Salhy M, Suhr O, Eriksson J, Lithner F. Prevalence of gastrointestinal symptoms in young and middle-aged diabetic patients. Scand J Gastroenterol. 1999;34:1196-1202. [PubMed] |
| 137. | Talley NJ, Young L, Bytzer P, Hammer J, Leemon M, Jones M, Horowitz M. Impact of chronic gastrointestinal symptoms in diabetes mellitus on health-related quality of life. Am J Gastroenterol. 2001;96:71-76. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 142] [Cited by in RCA: 150] [Article Influence: 6.3] [Reference Citation Analysis (0)] |
| 138. | Talley NJ, Howell S, Jones MP, Horowitz M. Predictors of turnover of lower gastrointestinal symptoms in diabetes mellitus. Am J Gastroenterol. 2002;97:3087-3094. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 18] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 139. | Anderson RP. Coeliac disease. Aust Fam Physician. 2005;34:239-242. [PubMed] |
| 140. | Baothman OA, Zamzami MA, Taher I, Abubaker J, Abu-Farha M. The role of Gut Microbiota in the development of obesity and Diabetes. Lipids Health Dis. 2016;15:108. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 266] [Cited by in RCA: 339] [Article Influence: 37.7] [Reference Citation Analysis (0)] |
| 141. | Patterson E, Ryan PM, Cryan JF, Dinan TG, Ross RP, Fitzgerald GF, Stanton C. Gut microbiota, obesity and diabetes. Postgrad Med J. 2016;92:286-300. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 243] [Cited by in RCA: 364] [Article Influence: 40.4] [Reference Citation Analysis (0)] |
| 142. | Deng L, Gui Z, Zhao L, Wang J, Shen L. Diabetes mellitus and the incidence of colorectal cancer: an updated systematic review and meta-analysis. Dig Dis Sci. 2012;57:1576-1585. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 165] [Cited by in RCA: 157] [Article Influence: 12.1] [Reference Citation Analysis (0)] |
| 143. | Wu L, Yu C, Jiang H, Tang J, Huang HL, Gao J, Zhang X. Diabetes mellitus and the occurrence of colorectal cancer: an updated meta-analysis of cohort studies. Diabetes Technol Ther. 2013;15:419-427. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 37] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 144. | Yuhara H, Steinmaus C, Cohen SE, Corley DA, Tei Y, Buffler PA. Is diabetes mellitus an independent risk factor for colon cancer and rectal cancer? Am J Gastroenterol. 2011;106:1911-1921; quiz 1922. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 225] [Cited by in RCA: 275] [Article Influence: 19.6] [Reference Citation Analysis (0)] |
| 145. | Fine KD, Schiller LR. AGA technical review on the evaluation and management of chronic diarrhea. Gastroenterology. 1999;116:1464-1486. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 252] [Cited by in RCA: 195] [Article Influence: 7.5] [Reference Citation Analysis (0)] |
| 146. | Schiller LR. Chronic diarrhea. Gastroenterology. 2004;127:287-293. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 47] [Cited by in RCA: 38] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 147. | Ohlsson B, Melander O, Thorsson O, Olsson R, Ekberg O, Sundkvist G. Oesophageal dysmotility, delayed gastric emptying and autonomic neuropathy correlate to disturbed glucose homeostasis. Diabetologia. 2006;49:2010-2014. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 35] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 148. | Lysy J, Israeli E, Goldin E. The prevalence of chronic diarrhea among diabetic patients. Am J Gastroenterol. 1999;94:2165-2170. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 40] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 149. | Lee TH, Lee JS. Ramosetron might be useful for treating diabetic diarrhea with a rapid small bowel transit time. Korean J Intern Med. 2013;28:106-107. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 13] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 150. | Miller LJ. Small intestinal manifestations of diabetes mellitus. Yale J Biol Med. 1983;56:189-193. [PubMed] |
| 151. | Ogbonnaya KI, Arem R. Diabetic diarrhea. Pathophysiology, diagnosis, and management. Arch Intern Med. 1990;150:262-267. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 19] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 152. | Samsom M, Verhagen MAMT. Intestinal function. Horowitz M, Samsom M (eds) Gastrointestinal function in diabetes mellitus. Chichester: John Wiley & Sons, Ltd 2004; . |
| 153. | Rosa-e-Silva L, Troncon LE, Oliveira RB, Foss MC, Braga FJ, Gallo Júnior L. Rapid distal small bowel transit associated with sympathetic denervation in type I diabetes mellitus. Gut. 1996;39:748-756. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 32] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 154. | Goldstein F, Wirts CW, Kowlessar OD. Diabetic diarrhea and steatorrhea. Microbiologic and clinical observations. Ann Intern Med. 1970;72:215-218. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 62] [Cited by in RCA: 52] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 155. | Gould M, Sellin JH. Diabetic diarrhea. Curr Gastroenterol Rep. 2009;11:354-359. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 20] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 156. | Mashimo H, May RJ, Goyal RK. Diabetic diarrhea. In Joslin’s Diabetes Mellitus. 14th ed. Kahc C, Weir GC, King GL, Jacobson AM, Moses AC, Eds. Philadelphia: Pennsylvania, Lippincott Williams & Wilkins 2005; 1089-1091. |
| 157. | Battle WM, Cohen JD, Snape WJ. Disorders of colonic motility in patients with diabetes mellitus. Yale J Biol Med. 1983;56:277-283. [PubMed] |
| 158. | Maisey A. A Practical Approach to Gastrointestinal Complications of Diabetes. Diabetes Ther. 2016;7:379-386. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 38] [Cited by in RCA: 32] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 159. | Tack J. Functional diarrhea. Gastroenterol Clin North Am. 2012;41:629-637. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 25] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 160. | Bytzer P, Talley NJ, Leemon M, Young LJ, Jones MP, Horowitz M. Prevalence of gastrointestinal symptoms associated with diabetes mellitus: a population-based survey of 15,000 adults. Arch Intern Med. 2001;161:1989-1996. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 486] [Cited by in RCA: 419] [Article Influence: 17.5] [Reference Citation Analysis (0)] |
| 161. | Sun WM, Read NW. Anorectal function. Horowitz M, Samsom M (eds) Gastrointestinal function in diabetes mellitus. Chichester: John Wiley & Sons, Ltd 2004; . |
| 162. | Oh JH, Choi MG, Kang MI, Lee KM, Kim JI, Kim BW, Lee DS, Kim SS, Choi H, Han SW. The prevalence of gastrointestinal symptoms in patients with non-insulin dependent diabetes mellitus. Korean J Intern Med. 2009;24:309-317. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 41] [Cited by in RCA: 41] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 163. | Khoshbaten M, Madad L, Baladast M, Mohammadi M, Aliasgarzadeh A. Gastrointestinal signs and symptoms among persons with diabetes mellitus. Gastroenterol Hepatol Bed Bench. 2011;4:219-223. [PubMed] |
| 164. | Rodrigues ML, Motta ME. Mechanisms and factors associated with gastrointestinal symptoms in patients with diabetes mellitus. J Pediatr (Rio J). 2012;88:17-24. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 30] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 165. | Ihana-Sugiyama N, Nagata N, Yamamoto-Honda R, Izawa E, Kajio H, Shimbo T, Kakei M, Uemura N, Akiyama J, Noda M. Constipation, hard stools, fecal urgency, and incomplete evacuation, but not diarrhea is associated with diabetes and its related factors. World J Gastroenterol. 2016;22:3252-3260. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 22] [Cited by in RCA: 18] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 166. | Rayner CK, Samsom M, Jones KL, Horowitz M. Relationships of upper gastrointestinal motor and sensory function with glycemic control. Diabetes Care. 2001;24:371-381. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 349] [Cited by in RCA: 307] [Article Influence: 12.8] [Reference Citation Analysis (0)] |
| 167. | Taba Taba Vakili S, Nezami BG, Shetty A, Chetty VK, Srinivasan S. Association of high dietary saturated fat intake and uncontrolled diabetes with constipation: evidence from the National Health and Nutrition Examination Survey. Neurogastroenterol Motil. 2015;27:1389-1397. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 40] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 168. | Harmsen HJ, de Goffau MC. The Human Gut Microbiota. Adv Exp Med Biol. 2016;902:95-108. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 58] [Article Influence: 6.4] [Reference Citation Analysis (0)] |
| 169. | Vaarala O, Atkinson MA, Neu J. The “perfect storm” for type 1 diabetes: the complex interplay between intestinal microbiota, gut permeability, and mucosal immunity. Diabetes. 2008;57:2555-2562. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 371] [Cited by in RCA: 366] [Article Influence: 21.5] [Reference Citation Analysis (0)] |
| 170. | Delzenne NM, Cani PD. Interaction between obesity and the gut microbiota: relevance in nutrition. Annu Rev Nutr. 2011;31:15-31. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 302] [Cited by in RCA: 300] [Article Influence: 21.4] [Reference Citation Analysis (0)] |
| 171. | Tai N, Wong FS, Wen L. The role of gut microbiota in the development of type 1, type 2 diabetes mellitus and obesity. Rev Endocr Metab Disord. 2015;16:55-65. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 165] [Cited by in RCA: 186] [Article Influence: 18.6] [Reference Citation Analysis (0)] |
| 172. | Allin KH, Nielsen T, Pedersen O. Mechanisms in endocrinology: Gut microbiota in patients with type 2 diabetes mellitus. Eur J Endocrinol. 2015;172:R167-R177. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 144] [Cited by in RCA: 156] [Article Influence: 15.6] [Reference Citation Analysis (0)] |
| 173. | Blandino G, Inturri R, Lazzara F, Di Rosa M, Malaguarnera L. Impact of gut microbiota on diabetes mellitus. Diabetes Metab. 2016;42:303-315. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 132] [Cited by in RCA: 169] [Article Influence: 18.8] [Reference Citation Analysis (0)] |
| 174. | Knip M, Siljander H. The role of the intestinal microbiota in type 1 diabetes mellitus. Nat Rev Endocrinol. 2016;12:154-167. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 260] [Cited by in RCA: 288] [Article Influence: 32.0] [Reference Citation Analysis (0)] |
| 175. | Stephen AM, Wiggins HS, Cummings JH. Effect of changing transit time on colonic microbial metabolism in man. Gut. 1987;28:601-609. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 135] [Cited by in RCA: 123] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 176. | Kashyap PC, Marcobal A, Ursell LK, Larauche M, Duboc H, Earle KA, Sonnenburg ED, Ferreyra JA, Higginbottom SK, Million M. Complex interactions among diet, gastrointestinal transit, and gut microbiota in humanized mice. Gastroenterology. 2013;144:967-977. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 318] [Cited by in RCA: 343] [Article Influence: 28.6] [Reference Citation Analysis (0)] |
| 177. | Tottey W, Feria-Gervasio D, Gaci N, Laillet B, Pujos E, Martin JF, Sebedio JL, Sion B, Jarrige JF, Alric M. Colonic Transit Time Is a Driven Force of the Gut Microbiota Composition and Metabolism: In Vitro Evidence. J Neurogastroenterol Motil. 2017;23:124-134. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 64] [Cited by in RCA: 90] [Article Influence: 11.3] [Reference Citation Analysis (0)] |
| 178. | Wirth R, Bódi N, Maróti G, Bagyánszki M, Talapka P, Fekete É, Bagi Z, Kovács KL. Regionally distinct alterations in the composition of the gut microbiota in rats with streptozotocin-induced diabetes. PLoS One. 2014;9:e110440. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 46] [Cited by in RCA: 59] [Article Influence: 5.4] [Reference Citation Analysis (0)] |
| 179. | Rhee SH, Pothoulakis C, Mayer EA. Principles and clinical implications of the brain-gut-enteric microbiota axis. Nat Rev Gastroenterol Hepatol. 2009;6:306-314. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 760] [Cited by in RCA: 920] [Article Influence: 57.5] [Reference Citation Analysis (0)] |
| 180. | Barbara G, Stanghellini V, Brandi G, Cremon C, Di Nardo G, De Giorgio R, Corinaldesi R. Interactions between commensal bacteria and gut sensorimotor function in health and disease. Am J Gastroenterol. 2005;100:2560-2568. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 241] [Cited by in RCA: 218] [Article Influence: 10.9] [Reference Citation Analysis (0)] |
| 181. | Kunze WA, Mao YK, Wang B, Huizinga JD, Ma X, Forsythe P, Bienenstock J. Lactobacillus reuteri enhances excitability of colonic AH neurons by inhibiting calcium-dependent potassium channel opening. J Cell Mol Med. 2009;13:2261-2270. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 226] [Cited by in RCA: 248] [Article Influence: 15.5] [Reference Citation Analysis (0)] |
| 182. | Obata Y, Pachnis V. The Effect of Microbiota and the Immune System on the Development and Organization of the Enteric Nervous System. Gastroenterology. 2016;151:836-844. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 130] [Cited by in RCA: 173] [Article Influence: 19.2] [Reference Citation Analysis (0)] |
| 183. | Hyland NP, Cryan JF. Microbe-host interactions: Influence of the gut microbiota on the enteric nervous system. Dev Biol. 2016;417:182-187. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 94] [Cited by in RCA: 130] [Article Influence: 14.4] [Reference Citation Analysis (0)] |
| 184. | Savidge TC. Importance of NO and its related compounds in enteric nervous system regulation of gut homeostasis and disease susceptibility. Curr Opin Pharmacol. 2014;19:54-60. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 14] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 185. | Schicho R, Krueger D, Zeller F, Von Weyhern CW, Frieling T, Kimura H, Ishii I, De Giorgio R, Campi B, Schemann M. Hydrogen sulfide is a novel prosecretory neuromodulator in the Guinea-pig and human colon. Gastroenterology. 2006;131:1542-1552. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 163] [Cited by in RCA: 174] [Article Influence: 9.2] [Reference Citation Analysis (0)] |
| 186. | Malago JJ. Contribution of microbiota to the intestinal physicochemical barrier. Benef Microbes. 2015;6:295-311. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 26] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 187. | Guarino MP, Cicala M, Putignani L, Severi C. Gastrointestinal neuromuscular apparatus: An underestimated target of gut microbiota. World J Gastroenterol. 2016;22:9871-9879. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 25] [Cited by in RCA: 24] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 188. | Holst JJ. The physiology of glucagon-like peptide 1. Physiol Rev. 2007;87:1409-1439. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2055] [Cited by in RCA: 2350] [Article Influence: 130.6] [Reference Citation Analysis (1)] |
| 189. | Thazhath SS, Marathe CS, Wu T, Chang J, Khoo J, Kuo P, Checklin HL, Bound MJ, Rigda RS, Crouch B. The Glucagon-Like Peptide 1 Receptor Agonist Exenatide Inhibits Small Intestinal Motility, Flow, Transit, and Absorption of Glucose in Healthy Subjects and Patients With Type 2 Diabetes: A Randomized Controlled Trial. Diabetes. 2016;65:269-275. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 68] [Cited by in RCA: 62] [Article Influence: 6.9] [Reference Citation Analysis (0)] |
| 190. | Amato A, Cinci L, Rotondo A, Serio R, Faussone-Pellegrini MS, Vannucchi MG, Mulè F. Peripheral motor action of glucagon-like peptide-1 through enteric neuronal receptors. Neurogastroenterol Motil. 2010;22:664-e203. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 86] [Cited by in RCA: 93] [Article Influence: 6.2] [Reference Citation Analysis (0)] |
| 191. | Marathe CS, Rayner CK, Jones KL, Horowitz M. Glucagon-like peptides 1 and 2 in health and disease: a review. Peptides. 2013;44:75-86. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 76] [Cited by in RCA: 71] [Article Influence: 5.9] [Reference Citation Analysis (0)] |
| 192. | Holst JJ, Christensen M, Lund A, de Heer J, Svendsen B, Kielgast U, Knop FK. Regulation of glucagon secretion by incretins. Diabetes Obes Metab. 2011;13 Suppl 1:89-94. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 108] [Cited by in RCA: 115] [Article Influence: 8.2] [Reference Citation Analysis (0)] |
| 193. | O’Malley TJ, Fava GE, Zhang Y, Fonseca VA, Wu H. Progressive change of intra-islet GLP-1 production during diabetes development. Diabetes Metab Res Rev. 2014;30:661-668. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 38] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 194. | Yang M, Fukui H, Eda H, Xu X, Kitayama Y, Hara K, Kodani M, Tomita T, Oshima T, Watari J. Involvement of gut microbiota in association between GLP-1/GLP-1 receptor expression and gastrointestinal motility. Am J Physiol Gastrointest Liver Physiol. 2017;312:G367-G373. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 43] [Article Influence: 5.4] [Reference Citation Analysis (0)] |
| 195. | Joshi SR, Standl E, Tong N, Shah P, Kalra S, Rathod R. Therapeutic potential of α-glucosidase inhibitors in type 2 diabetes mellitus: an evidence-based review. Expert Opin Pharmacother. 2015;16:1959-1981. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 252] [Cited by in RCA: 207] [Article Influence: 20.7] [Reference Citation Analysis (0)] |
| 196. | Bauer PV, Duca FA. Targeting the gastrointestinal tract to treat type 2 diabetes. J Endocrinol. 2016;230:R95-R113. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 18] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 197. | Rayner CK, Jones KL, Wu T, Horowitz M. Gut feelings about diabetes and GLP-1 receptor agonists: lessons to be learnt from studies in functional gastrointestinal disorders. Diabetes Obes Metab. 2017;19:309-312. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 9] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 198. | Su B, Liu H, Li J, Sunli Y, Liu B, Liu D, Zhang P, Meng X. Acarbose treatment affects the serum levels of inflammatory cytokines and the gut content of bifidobacteria in Chinese patients with type 2 diabetes mellitus. J Diabetes. 2015;7:729-739. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 80] [Cited by in RCA: 100] [Article Influence: 10.0] [Reference Citation Analysis (0)] |
| 199. | Wang L, Li P, Tang Z, Yan X, Feng B. Structural modulation of the gut microbiota and the relationship with body weight: compared evaluation of liraglutide and saxagliptin treatment. Sci Rep. 2016;6:33251. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 81] [Cited by in RCA: 112] [Article Influence: 12.4] [Reference Citation Analysis (0)] |
| 200. | Zhang X, Fang Z, Zhang C, Xia H, Jie Z, Han X, Chen Y, Ji L. Effects of Acarbose on the Gut Microbiota of Prediabetic Patients: A Randomized, Double-blind, Controlled Crossover Trial. Diabetes Ther. 2017;8:293-307. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 97] [Cited by in RCA: 136] [Article Influence: 17.0] [Reference Citation Analysis (0)] |
| 201. | Lee H, Ko G. Effect of metformin on metabolic improvement and gut microbiota. Appl Environ Microbiol. 2014;80:5935-5943. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 253] [Cited by in RCA: 292] [Article Influence: 26.5] [Reference Citation Analysis (0)] |
| 202. | Mikkelsen KH, Frost M, Bahl MI, Licht TR, Jensen US, Rosenberg J, Pedersen O, Hansen T, Rehfeld JF, Holst JJ. Effect of Antibiotics on Gut Microbiota, Gut Hormones and Glucose Metabolism. PLoS One. 2015;10:e0142352. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 63] [Cited by in RCA: 78] [Article Influence: 7.8] [Reference Citation Analysis (0)] |
| 203. | Jiang Y, Ben Q, Shen H, Lu W, Zhang Y, Zhu J. Diabetes mellitus and incidence and mortality of colorectal cancer: a systematic review and meta-analysis of cohort studies. Eur J Epidemiol. 2011;26:863-876. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 169] [Cited by in RCA: 159] [Article Influence: 11.4] [Reference Citation Analysis (0)] |
| 204. | Sun L, Yu S. Diabetes mellitus is an independent risk factor for colorectal cancer. Dig Dis Sci. 2012;57:1586-1597. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 52] [Cited by in RCA: 54] [Article Influence: 4.2] [Reference Citation Analysis (0)] |
| 205. | Wu L, Wang Z, Zhu J, Murad AL, Prokop LJ, Murad MH. Nut consumption and risk of cancer and type 2 diabetes: a systematic review and meta-analysis. Nutr Rev. 2015;73:409-425. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 73] [Cited by in RCA: 83] [Article Influence: 9.2] [Reference Citation Analysis (0)] |
| 206. | Guraya SY. Association of type 2 diabetes mellitus and the risk of colorectal cancer: A meta-analysis and systematic review. World J Gastroenterol. 2015;21:6026-6031. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 104] [Cited by in RCA: 118] [Article Influence: 11.8] [Reference Citation Analysis (2)] |
| 207. | Omran S, Ismail AA. Knowledge and beliefs of Jordanians toward colorectal cancer screening. Cancer Nurs. 2010;33:141-148. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 20] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 208. | Marugame T, Lee K, Eguchi H, Oda T, Shinchi K, Kono S. Relation of impaired glucose tolerance and diabetes mellitus to colorectal adenomas in Japan. Cancer Causes Control. 2002;13:917-921. [PubMed] |
| 209. | Misciagna G, De Michele G, Guerra V, Cisternino AM, Di Leo A, Freudenheim JL. Serum fructosamine and colorectal adenomas. Eur J Epidemiol. 2004;19:425-432. [PubMed] |
| 210. | Shonka NA, Anderson JR, Panwalkar AW, Reed EC, Steen PD, Ganti AK. Effect of diabetes mellitus on the epidemiology and outcomes of colon cancer. Med Oncol. 2006;23:515-519. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 211. | Dash C, Palmer JR, Boggs DA, Rosenberg L, Adams-Campbell LL. Type 2 diabetes and the risk of colorectal adenomas: Black Women’s Health Study. Am J Epidemiol. 2014;179:112-119. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 14] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 212. | Bella F, Minicozzi P, Giacomin A, Crocetti E, Federico M, Ponz de Leon M, Fusco M, Tumino R, Mangone L, Giuliani O. Impact of diabetes on overall and cancer-specific mortality in colorectal cancer patients. J Cancer Res Clin Oncol. 2013;139:1303-1310. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 27] [Cited by in RCA: 28] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 213. | Jarvandi S, Davidson NO, Schootman M. Increased risk of colorectal cancer in type 2 diabetes is independent of diet quality. PLoS One. 2013;8:e74616. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 29] [Cited by in RCA: 31] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 214. | Chen H, Wu L, Li Y, Meng J, Lin N, Yang D, Zhu Y, Li X, Li M, Xu Y. Advanced glycation end products increase carbohydrate responsive element binding protein expression and promote cancer cell proliferation. Mol Cell Endocrinol. 2014;395:69-78. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 41] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 215. | Luo J, Lin HC, He K, Hendryx M. Diabetes and prognosis in older persons with colorectal cancer. Br J Cancer. 2014;110:1847-1854. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 25] [Cited by in RCA: 29] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 216. | Vu HT, Ufere N, Yan Y, Wang JS, Early DS, Elwing JE. Diabetes mellitus increases risk for colorectal adenomas in younger patients. World J Gastroenterol. 2014;20:6946-6952. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 24] [Cited by in RCA: 25] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 217. | Woo H, Lee J, Lee J, Park JW, Park S, Kim J, Oh JH, Shin A. Diabetes Mellitus and Site-specific Colorectal Cancer Risk in Korea: A Case-control Study. J Prev Med Public Health. 2016;49:45-52. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 16] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 218. | Luo W, Cao Y, Liao C, Gao F. Diabetes mellitus and the incidence and mortality of colorectal cancer: a meta-analysis of 24 cohort studies. Colorectal Dis. 2012;14:1307-1312. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 42] [Cited by in RCA: 45] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 219. | De Bruijn KM, Arends LR, Hansen BE, Leeflang S, Ruiter R, van Eijck CH. Systematic review and meta-analysis of the association between diabetes mellitus and incidence and mortality in breast and colorectal cancer. Br J Surg. 2013;100:1421-1429. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 132] [Cited by in RCA: 149] [Article Influence: 12.4] [Reference Citation Analysis (0)] |
| 220. | Mills KT, Bellows CF, Hoffman AE, Kelly TN, Gagliardi G. Diabetes mellitus and colorectal cancer prognosis: a meta-analysis. Dis Colon Rectum. 2013;56:1304-1319. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 122] [Cited by in RCA: 152] [Article Influence: 12.7] [Reference Citation Analysis (0)] |
| 221. | Luo S, Li JY, Zhao LN, Yu T, Zhong W, Xia ZS, Shan TD, Ouyang H, Yang HS, Chen QK. Diabetes mellitus increases the risk of colorectal neoplasia: An updated meta-analysis. Clin Res Hepatol Gastroenterol. 2016;40:110-123. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 37] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 222. | Yu F, Guo Y, Wang H, Feng J, Jin Z, Chen Q, Liu Y, He J. Type 2 diabetes mellitus and risk of colorectal adenoma: a meta-analysis of observational studies. BMC Cancer. 2016;16:642. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 25] [Cited by in RCA: 37] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 223. | Chen HF, Chen P, Su YH, Su HF, Li CY. Age- and sex-specific risks of colorectal cancers in diabetic patients. Tohoku J Exp Med. 2012;226:259-265. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 6] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 224. | He J, Stram DO, Kolonel LN, Henderson BE, Le Marchand L, Haiman CA. The association of diabetes with colorectal cancer risk: the Multiethnic Cohort. Br J Cancer. 2010;103:120-126. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 70] [Cited by in RCA: 83] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 225. | Jeon JY, Jeong DH, Park MG, Lee JW, Chu SH, Park JH, Lee MK, Sato K, Ligibel JA, Meyerhardt JA. Impact of diabetes on oncologic outcome of colorectal cancer patients: colon vs. rectal cancer. PLoS One. 2013;8:e55196. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 41] [Cited by in RCA: 45] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 226. | Masur K, Vetter C, Hinz A, Tomas N, Henrich H, Niggemann B, Zänker KS. Diabetogenic glucose and insulin concentrations modulate transcriptome and protein levels involved in tumour cell migration, adhesion and proliferation. Br J Cancer. 2011;104:345-352. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 103] [Cited by in RCA: 115] [Article Influence: 7.7] [Reference Citation Analysis (0)] |
| 227. | Rojas A, Figueroa H, Morales E. Fueling inflammation at tumor microenvironment: the role of multiligand/RAGE axis. Carcinogenesis. 2010;31:334-341. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 116] [Cited by in RCA: 123] [Article Influence: 8.2] [Reference Citation Analysis (0)] |
| 228. | Odegaard JI, Chawla A. Pleiotropic actions of insulin resistance and inflammation in metabolic homeostasis. Science. 2013;339:172-177. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 494] [Cited by in RCA: 499] [Article Influence: 41.6] [Reference Citation Analysis (0)] |
| 229. | Nguyen AV, Wu YY, Lin EY. STAT3 and sphingosine-1-phosphate in inflammation-associated colorectal cancer. World J Gastroenterol. 2014;20:10279-10287. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 46] [Cited by in RCA: 62] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 230. | Hu B, Elinav E, Huber S, Strowig T, Hao L, Hafemann A, Jin C, Wunderlich C, Wunderlich T, Eisenbarth SC. Microbiota-induced activation of epithelial IL-6 signaling links inflammasome-driven inflammation with transmissible cancer. Proc Natl Acad Sci USA. 2013;110:9862-9867. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 220] [Cited by in RCA: 255] [Article Influence: 21.3] [Reference Citation Analysis (0)] |
| 231. | Abreu MT, Peek RM. Gastrointestinal malignancy and the microbiome. Gastroenterology. 2014;146:1534-1546.e3. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 233] [Cited by in RCA: 235] [Article Influence: 21.4] [Reference Citation Analysis (0)] |
| 232. | Baxter NT, Zackular JP, Chen GY, Schloss PD. Structure of the gut microbiome following colonization with human feces determines colonic tumor burden. Microbiome. 2014;2:20. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 210] [Cited by in RCA: 232] [Article Influence: 21.1] [Reference Citation Analysis (0)] |
| 233. | Liang H, Zhong Y, Zhou S, Peng L. Knockdown of RAGE expression inhibits colorectal cancer cell invasion and suppresses angiogenesis in vitro and in vivo. Cancer Lett. 2011;313:91-98. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 48] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 234. | Ishibashi Y, Matsui T, Takeuchi M, Yamagishi S. Metformin inhibits advanced glycation end products (AGEs)-induced growth and VEGF expression in MCF-7 breast cancer cells by suppressing AGEs receptor expression via AMP-activated protein kinase. Horm Metab Res. 2013;45:387-390. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 26] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 235. | Chen KH, Shao YY, Lin ZZ, Yeh YC, Shau WY, Kuo RN, Chen HM, Lai CL, Yeh KH, Cheng AL. Type 2 diabetes mellitus is associated with increased mortality in Chinese patients receiving curative surgery for colon cancer. Oncologist. 2014;19:951-958. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 24] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 236. | Will JC, Galuska DA, Vinicor F, Calle EE. Colorectal cancer: another complication of diabetes mellitus? Am J Epidemiol. 1998;147:816-825. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 197] [Cited by in RCA: 199] [Article Influence: 7.4] [Reference Citation Analysis (0)] |
| 237. | González N, Prieto I, Del Puerto-Nevado L, Portal-Nuñez S, Ardura JA, Corton M, Fernández-Fernández B, Aguilera O, Gomez-Guerrero C, Mas S. 2017 update on the relationship between diabetes and colorectal cancer: epidemiology, potential molecular mechanisms and therapeutic implications. Oncotarget. 2017;8:18456-18485. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 116] [Cited by in RCA: 127] [Article Influence: 15.9] [Reference Citation Analysis (0)] |
| 238. | Forootan M, Tabatabaeefar M, Yahyaei M, Maghsoodi N. Metabolic syndrome and colorectal cancer: a cross-sectional survey. Asian Pac J Cancer Prev. 2012;13:4999-5002. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 14] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 239. | Ishino K, Mutoh M, Totsuka Y, Nakagama H. Metabolic syndrome: a novel high-risk state for colorectal cancer. Cancer Lett. 2013;334:56-61. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 39] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 240. | Ulaganathan V, Kandiah M, Zalilah MS, Faizal JA, Fijeraid H, Normayah K, Gooi BH, Othman R. Colorectal cancer and its association with the metabolic syndrome: a Malaysian multi-centric case-control study. Asian Pac J Cancer Prev. 2012;13:3873-3877. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 14] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 241. | Trabulo D, Ribeiro S, Martins C, Teixeira C, Cardoso C, Mangualde J, Freire R, Gamito É, Alves AL, Augusto F, Oliveira AP, Cremers I. Metabolic syndrome and colorectal neoplasms: An ominous association. World J Gastroenterol. 2015;21:5320-5327. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 28] [Cited by in RCA: 26] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 242. | Kaczmarczyk MM, Miller MJ, Freund GG. The health benefits of dietary fiber: beyond the usual suspects of type 2 diabetes mellitus, cardiovascular disease and colon cancer. Metabolism. 2012;61:1058-1066. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 346] [Cited by in RCA: 331] [Article Influence: 25.5] [Reference Citation Analysis (0)] |
| 243. | Tsugane S, Inoue M. Insulin resistance and cancer: epidemiological evidence. Cancer Sci. 2010;101:1073-1079. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 123] [Cited by in RCA: 124] [Article Influence: 8.3] [Reference Citation Analysis (0)] |
| 244. | Herrigel DJ, Moss RA. Diabetes mellitus as a novel risk factor for gastrointestinal malignancies. Postgrad Med. 2014;126:106-118. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 14] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 245. | Othman EM, Hintzsche H, Stopper H. Signaling steps in the induction of genomic damage by insulin in colon and kidney cells. Free Radic Biol Med. 2014;68:247-257. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 23] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 246. | Chung YW, Han DS, Park KH, Eun CS, Yoo KS, Park CK. Insulin therapy and colorectal adenoma risk among patients with Type 2 diabetes mellitus: a case-control study in Korea. Dis Colon Rectum. 2008;51:593-597. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 58] [Cited by in RCA: 65] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 247. | Yang YX, Hennessy S, Lewis JD. Insulin therapy and colorectal cancer risk among type 2 diabetes mellitus patients. Gastroenterology. 2004;127:1044-1050. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 264] [Cited by in RCA: 268] [Article Influence: 12.8] [Reference Citation Analysis (0)] |
| 248. | Currie CJ, Poole CD, Gale EA. The influence of glucose-lowering therapies on cancer risk in type 2 diabetes. Diabetologia. 2009;52:1766-1777. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 859] [Cited by in RCA: 848] [Article Influence: 53.0] [Reference Citation Analysis (1)] |
| 249. | Chiu CC, Huang CC, Chen YC, Chen TJ, Liang Y, Lin SJ, Chen JW, Leu HB, Chan WL. Increased risk of gastrointestinal malignancy in patients with diabetes mellitus and correlations with anti-diabetes drugs: a nationwide population-based study in Taiwan. Intern Med. 2013;52:939-946. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 36] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 250. | Blanquicett C, Roman J, Hart CM. Thiazolidinediones as anti-cancer agents. Cancer Ther. 2008;6:25-34. [PubMed] |
| 251. | Lewis JD, Capra AM, Achacoso NS, Ferrara A, Levin TR, Quesenberry CP, Habel LA. Thiazolidinedione therapy is not associated with increased colonic neoplasia risk in patients with diabetes mellitus. Gastroenterology. 2008;135:1914-1923, 1923.e1. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 19] [Cited by in RCA: 19] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 252. | Chang CH, Lin JW, Wu LC, Lai MS, Chuang LM, Chan KA. Association of thiazolidinediones with liver cancer and colorectal cancer in type 2 diabetes mellitus. Hepatology. 2012;55:1462-1472. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 139] [Cited by in RCA: 148] [Article Influence: 11.4] [Reference Citation Analysis (0)] |
| 253. | Nie Z, Zhu H, Gu M. Reduced colorectal cancer incidence in type 2 diabetic patients treated with metformin: a meta-analysis. Pharm Biol. 2016;54:2636-2642. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 34] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 254. | Ramjeesingh R, Orr C, Bricks CS, Hopman WM, Hammad N. A retrospective study on the role of diabetes and metformin in colorectal cancer disease survival. Curr Oncol. 2016;23:e116-e122. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 29] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 255. | Cho YH, Ko BM, Kim SH, Myung YS, Choi JH, Han JP, Hong SJ, Jeon SR, Kim HG, Kim JO. Does metformin affect the incidence of colonic polyps and adenomas in patients with type 2 diabetes mellitus? Intest Res. 2014;12:139-145. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 23] [Cited by in RCA: 24] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 256. | Marks AR, Pietrofesa RA, Jensen CD, Zebrowski A, Corley DA, Doubeni CA. Metformin use and risk of colorectal adenoma after polypectomy in patients with type 2 diabetes mellitus. Cancer Epidemiol Biomarkers Prev. 2015;24:1692-1698. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 20] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 257. | Koehler JA, Kain T, Drucker DJ. Glucagon-like peptide-1 receptor activation inhibits growth and augments apoptosis in murine CT26 colon cancer cells. Endocrinology. 2011;152:3362-3372. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 71] [Cited by in RCA: 85] [Article Influence: 6.1] [Reference Citation Analysis (0)] |
| 258. | Kissow H, Hartmann B, Holst JJ, Viby NE, Hansen LS, Rosenkilde MM, Hare KJ, Poulsen SS. Glucagon-like peptide-1 (GLP-1) receptor agonism or DPP-4 inhibition does not accelerate neoplasia in carcinogen treated mice. Regul Pept. 2012;179:91-100. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 70] [Cited by in RCA: 80] [Article Influence: 6.2] [Reference Citation Analysis (0)] |
| 259. | Bae S, Wong HL, Tie J, Desai J, Field K, Kosmider S, Fourlanos S, Jones I, Skinner I, Gibbs P. Impact of Diabetes Status and Medication on Presentation, Treatment, and Outcome of Stage II Colon Cancer Patients. J Cancer Epidemiol. 2015;2015:189132. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 13] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 260. | Min XH, Yu T, Qing Q, Yuan YH, Zhong W, Chen GC, Zhao LN, Deng N, Zhang LF, Chen QK. Abnormal differentiation of intestinal epithelium and intestinal barrier dysfunction in diabetic mice associated with depressed Notch/NICD transduction in Notch/Hes1 signal pathway. Cell Biol Int. 2014;38:1194-1204. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 43] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 261. | Charlton M, Ahlman B, Nair KS. The effect of insulin on human small intestinal mucosal protein synthesis. Gastroenterology. 2000;118:299-306. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 39] [Cited by in RCA: 40] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 262. | Adeghate E, Ponery AS, Sharma AK, El-Sharkawy T, Donáth T. Diabetes mellitus is associated with a decrease in vasoactive intestinal polypeptide content of gastrointestinal tract of rat. Arch Physiol Biochem. 2001;109:246-251. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 17] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 263. | Miró-Queralt M, Guinovart JJ, Planas JM. Sodium tungstate decreases sucrase and Na+/D-glucose cotransporter in the jejunum of diabetic rats. Am J Physiol Gastrointest Liver Physiol. 2008;295:G479-G484. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 8] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 264. | El-Salhy M, Spångéus A. Substance P in the gastrointestinal tract of non-obese diabetic mice. Scand J Gastroenterol. 1998;33:394-400. [PubMed] |
| 265. | Adeghate E, al-Ramadi B, Saleh AM, Vijayarasathy C, Ponery AS, Arafat K, Howarth FC, El-Sharkawy T. Increase in neuronal nitric oxide synthase content of the gastroduodenal tract of diabetic rats. Cell Mol Life Sci. 2003;60:1172-1179. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 37] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 266. | Spångéus A, Forsgren S, El-Salhy M. Effect of diabetic state on co-localization of substance P and serotonin in the gut in animal models. Histol Histopathol. 2001;16:393-398. [PubMed] |
| 267. | Jeyabal PV, Kumar R, Gangula PR, Micci MA, Pasricha PJ. Inhibitors of advanced glycation end-products prevent loss of enteric neuronal nitric oxide synthase in diabetic rats. Neurogastroenterol Motil. 2008;20:253-261. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 31] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 268. | Clark HB, Schmidt RE. Identification of dystrophic sympathetic axons in experimental diabetic autonomic neuropathy. Brain Res. 1984;293:390-395. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 17] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 269. | Spångéus A, el-Salhy M. Myenteric plexus in the gastrointestinal tract of non-obese diabetic mice. Histol Histopathol. 1998;13:989-994. [PubMed] |
| 270. | Izbéki F, Wittman T, Rosztóczy A, Linke N, Bódi N, Fekete E, Bagyánszki M. Immediate insulin treatment prevents gut motility alterations and loss of nitrergic neurons in the ileum and colon of rats with streptozotocin-induced diabetes. Diabetes Res Clin Pract. 2008;80:192-198. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 35] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 271. | Hernandes L, Bazotte RB, Gama P, Miranda-Neto MH. Streptozotocin-induced diabetes duration is important to determine changes in the number and basophily of myenteric neurons. Arq Neuropsiquiatr. 2000;58:1035-1039. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 24] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 272. | Pereira MA, Bagatin MC, Zanoni JN. Effects of the ascorbic acid supplementation on NADH-diaphorase myenteric neurons in the duodenum of diabetic rats. Biocell. 2006;30:295-300. [PubMed] |
| 273. | Tronchini EA, Trevizan AR, Tashima CM, Pereira RV, Zanoni JN. Supplementation with 0.1% and 2% vitamin E in diabetic rats: analysis of myenteric neurons immunostained for myosin-V and nNOS in the jejunum. Arq Gastroenterol. 2012;49:284-290. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 9] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 274. | Rauma J, Spångeus A, El-Salhy M. Ghrelin cell density in the gastrointestinal tracts of animal models of human diabetes. Histol Histopathol. 2006;21:1-5. [PubMed] |
| 275. | Miller SM, Narasimhan RA, Schmalz PF, Soffer EE, Walsh RM, Krishnamurthi V, Pasricha PJ, Szurszewski JH, Farrugia G. Distribution of interstitial cells of Cajal and nitrergic neurons in normal and diabetic human appendix. Neurogastroenterol Motil. 2008;20:349-357. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 35] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 276. | Kandemir O, Utas C, Gönen O, Patiroglu TE, Ozbakir O, Kelestimur F, Yücesoy M. Colonic subepithelial collagenous thickening in diabetic patients. Dis Colon Rectum. 1995;38:1097-1100. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 13] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 277. | Unal A, Guven K, Yurci A, Torun E, Gursoy S, Baskol M, Ozturk F, Arsav V. Is increased colon subepithelial collagen layer thickness in diabetic patients related to collagenous colitis? An immunohistochemical study. Pathol Res Pract. 2008;204:537-544. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 7] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 278. | Spångéus A, El-Salhy M. Large intestinal endocrine cells in non-obese diabetic mice. J Diabetes Complications. 1998;12:321-327. [PubMed] |
| 279. | Du F, Wang L, Qian W, Liu S. Loss of enteric neurons accompanied by decreased expression of GDNF and PI3K/Akt pathway in diabetic rats. Neurogastroenterol Motil. 2009;21:1229-e114. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 41] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 280. | Nakahara M, Isozaki K, Hirota S, Vanderwinden JM, Takakura R, Kinoshita K, Miyagawa J, Chen H, Miyazaki Y, Kiyohara T. Deficiency of KIT-positive cells in the colon of patients with diabetes mellitus. J Gastroenterol Hepatol. 2002;17:666-670. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 70] [Cited by in RCA: 76] [Article Influence: 3.3] [Reference Citation Analysis (0)] |