Published online Jul 26, 2021. doi: 10.12998/wjcc.v9.i21.6125
Peer-review started: March 25, 2021
First decision: April 29, 2021
Revised: April 30, 2021
Accepted: May 19, 2021
Article in press: May 19, 2021
Published online: July 26, 2021
Processing time: 118 Days and 5.9 Hours
Ligamentum flavum hematoma (LFH) can cause compression of the spinal cord or nerve root, which results in neurological symptoms. We report a case of lumbar radicular pain due to LFH following a traffic accident.
A 59-year-old man complained of left buttock and lateral thigh pain that was dull in nature after a traffic accident 18 d prior to presentation. Magnetic resonance imaging (MRI), taken 17 d after the traffic accident, revealed a mass lesion at the L4-5 Level. These MRI findings suggested subacute LFH. The patient’s pain was not alleviated with conservative treatment, including oral medication and epidural steroid injection. After a partial-hemilaminectomy and removal of LFH, the patient’s pain completely disappeared.
Because early operation for decompression is important for a good outcome, clinicians should be able to determine LFH from MRI results and be aware of the possibility of LFH, especially in patients with a history of trauma.
Core Tip: Magnetic resonance imaging is the method of choice for diagnosis of ligamentum flavum hematoma (LFH). In the acute stage of LFH, the hematoma appears hypointense in T2-weighted images and isointense in T1-weighted images. Between 3 and 7 d of LFH, the methemoglobin causes the hematoma to be hyper
- Citation: Yu D, Lee W, Chang MC. Ligamentum flavum hematoma following a traffic accident: A case report. World J Clin Cases 2021; 9(21): 6125-6129
- URL: https://www.wjgnet.com/2307-8960/full/v9/i21/6125.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v9.i21.6125
Ligamentum flavum hematoma (LFH) is a rare disorder, as the ligamentum flavum is poorly vascularized[1]. LFH can cause compression of the spinal cord or nerve root, which results in neurological symptoms[2-4]. Although the exact mechanism of LFH is not clearly elucidated, the rupture of vessels within the ligamentum flavum or hemorrhage from the facet joint is known to cause LFH[1]. Although some spontaneous LFHs without any significant causes have been reported, LFH is thought to usually result from a back injury or mechanical stress in daily life[5,6].
In the current study, we report a case involving the development of an LFH after a traffic accident.
A 59-year-old man visited the Spine Center at a university hospital with left buttock and lateral thigh pain (dull nature, numeric rating scale = 4), which began immediately after a traffic accident that had occurred 18 d before the visit. The car that the patient was riding in was completely stationary, and another car crashed into the patient’s car from behind. The patient was in the passenger seat next to the driver at the time of the accident.
Conservative treatment with oral medication and transforaminal epidural steroid injection with dexamethasone 40 mg and 1% lidocaine 0.3 mL on the left L4 and L5 was not effective, and the patient’s pain was not endurable.
The patient had no specific history of past illness.
The patient had no specific personal and family history.
Upon physical examination, the straight-leg-raise test was positive at approximately 70 degrees on the left side. Motor and sensory deficits were not present at the bilateral lower extremities, and bilateral knee and ankle jerk reflexes were normal. The patient’s pain was aggravated by walking and standing.
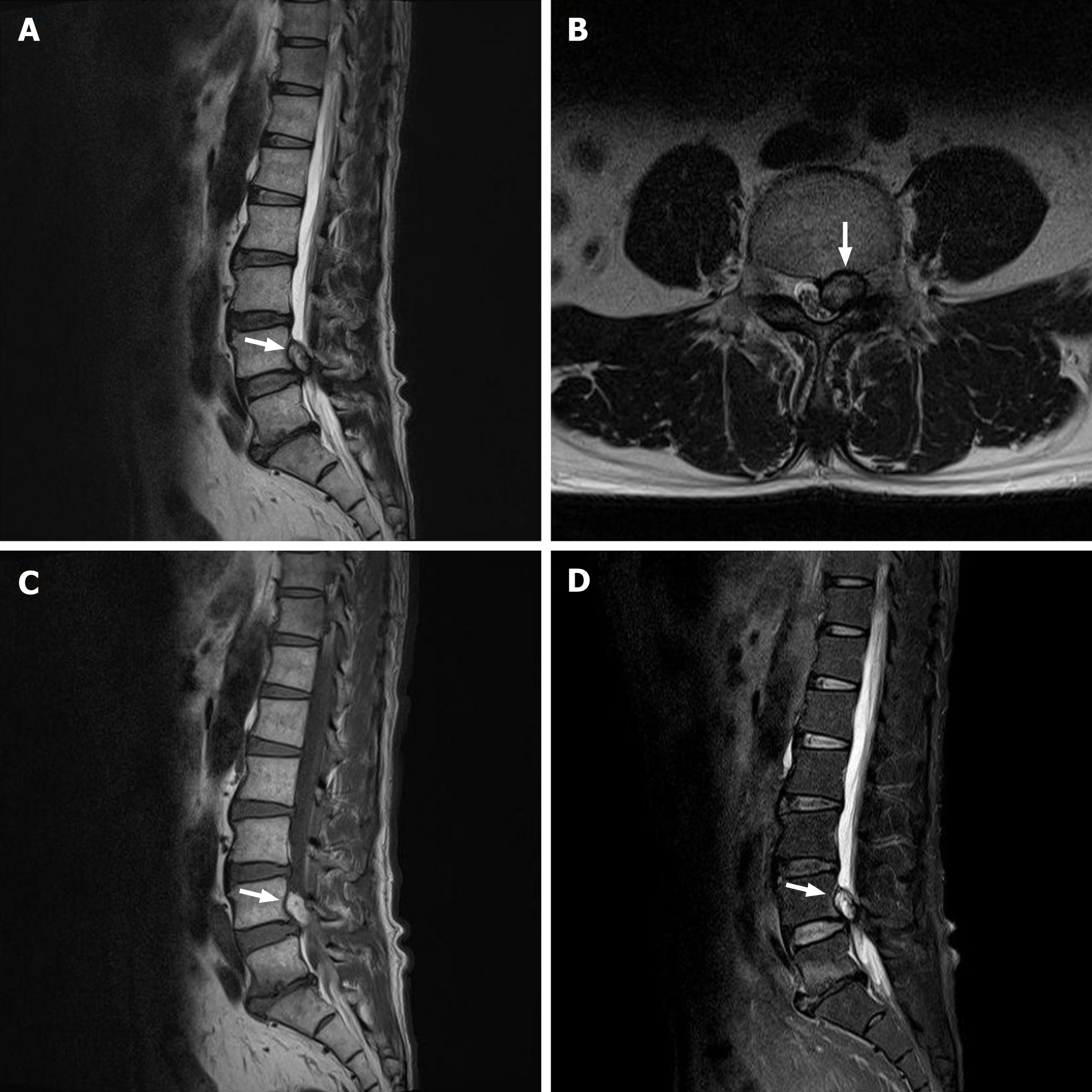
Magnetic resonance imaging (MRI), taken at 17 d after the accident, showed a well-defined epidural mass that originated from the left L4-5 facet joint and was compressing the left L4 and L5 nerve roots at the lateral recess and neural foramen (Figure 1). Imaging showed a T1 signal hyperintensity and lack of fat suppression, suggesting a hematoma of subacute stage. In the T2-weighted image, the mass was mainly hyperintense with some heterogeneity, suggesting extracellular and intracellular methemoglobin due to hemolysis.
Initially, after the diagnosis of an LFH, the patient had received three transforaminal steroid injections at the left L4 and L5 nerve roots. However, pain reduction was not sufficient. Therefore, at 68 d after the traffic accident, the patient underwent a surgical operation. Under general anesthesia, left L4 partial hemilaminectomy was conducted. The ligamentum flavum was identified as a dark brownish mass that was adherent to the dural sac. Moreover, the dural sac was compressed by the ligamentum flaval mass from the dorsolateral side. The LFH was completely removed after careful dissection from the dural sac, and the ligamentum flavum and LFH were completely resected.
Immediately after the surgical operation, the patient’s pain was completely absent.
In this study, we presented an LFH in the lumbar spine following a traffic accident. Our patient’s pain at the buttock and lower extremity seemed to be radicular pain caused by the compression of the spinal nerve root by an LFH. Many previously reported cases of LFH occurred following mild trauma, such as needle injury during a procedure for relief of spinal pain and stretching exercises[5,6,9]. Although LFH can occur at any spine level, LFH occurs most frequently in the lumbar spine, as the largest mechanical loading occurs at the lumbar level[10].
The ligamentum flavum is a thick elastic ligament that resides vertically between the vertebrae[11]. Because of constant tension forces and the few small vessels in the ligamentum flavum, LFH is unlikely to develop[11]. However, when the ligamentum flavum is degenerated and hypertrophied, the vessels in the ligament become thinned, proliferated, and irregular and are therefore susceptible to trauma[12]. On the other hand, in our patient, the hematoma was connected to the facet joint; therefore, the hematoma seems to have resulted from the rupture of vessels within the facet joint.
MRI is the method of choice for diagnosis of LFH. In the acute stage of LFH, the hematoma appears hypointense in T2-weighted images and isointense in T1-weighted images[7,8]. Between 3 and 7 d of LFH, the methemoglobin causes the hematoma to be hyperintense in T1-weighted images. At 1 wk after the onset, the hemolysis of erythrocytes results in the accumulation of extracellular meta-hemoglobin, which appears hyperintense in T1-weighted and T2-weighted images.
For the treatment of symptomatic LFH, laminectomy or partial laminectomy should be conducted[13,14]. When the nerve compression by LFH is massive, the removal of the ligamentum flavum can also be performed together with laminectomy[13,14]. For better treatment outcomes, early decompression is necessary[13,14]. In our case, the patient did not show any significant motor or sensory deficits. Therefore, we initially conducted conservative management for pain reduction. Thereafter, because the patient’s pain had not been controlled, we finally performed the hemilaminectomy.
In the current study, we described a patient with LFH following a traffic accident. LFH in our patient induced lumbar radicular pain that was refractory to conservative treatment. Our case is the first to show the development of an LFH after a traffic accident. Because early treatment is essential for an excellent outcome, clinicians should be able to recognize an LFH on MRI scans and be aware of the possibility of LFH, especially in patients with a history of trauma.
Manuscript source: Unsolicited manuscript
Specialty type: Medicine, research and experimental
Country/Territory of origin: South Korea
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): 0
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Tee YK S-Editor: Gong ZM L-Editor: A P-Editor: Zhang YL
| 1. | Lee HW, Song JH, Chang IB, Choi HC. Spontaneous ligamentum flavum hematoma in the rigid thoracic spine: a case report and review of the literature. J Korean Neurosurg Soc. 2008;44:47-51. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 12] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 2. | Kotani Y, Sudo H, Abumi K, Ito M, Matsubara S, Minami A. Spinal cord compression by hematoma in the cervical ligamentum flavum: a case report. Spine J. 2012;12:e18-e21. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 7] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 3. | Spuck S, Stellmacher F, Wiesmann M, Kranz R. Case reports: a rare cause of radicular complaints: ligamentum flavum hematoma. Clin Orthop Relat Res. 2006;443:337-341. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 17] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 4. | Wild F, Tuettenberg J, Grau A, Weis J, Krauss JK. Ligamentum flavum hematomas of the cervical and thoracic spine. Clin Neurol Neurosurg. 2014;116:24-27. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 6] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 5. | Lee YS, Yi JS, Kim HJ, Kim JO, Choi ES. Epidural block-induced ligamentum flavum hematoma mimicking epidural hematoma in the lumbar spine: a case report. Spine J. 2011;11:e23-e27. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 6. | Liu HP, Chen CL, Chen NF, Liao CY, Ou CY. Ligamentum flavum hematoma due to stretching exercise. Am J Emerg Med 2016; 34: 2058.e3-2058. e6. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 7. | Dorsay TA, Helms CA. MR imaging of epidural hematoma in the lumbar spine. Skeletal Radiol. 2002;31:677-685. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 15] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 8. | Harbury OL, Provenzale JM, Barboriak DP. Vertex epidural hematomas: imaging findings and diagnostic pitfalls. Eur J Radiol. 2000;36:150-157. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 18] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 9. | Salehpour F, Mirzaei F, Rezakhah A, Aeinfar K, Kazemzadeh M, Alavi SAN. Ligamentum Flavum Hematoma Presented with Low Back Pain: A Case Report and Review of the Literature. Int J Spine Surg. 2018;12:337-341. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 10. | Ozdemir B, Kanat A, Batcik OE, Gucer H, Yolas C. Ligamentum flavum hematomas: Why does it mostly occur in old Asian males? J Craniovertebr Junction Spine. 2016;7:7-12. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 18] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 11. | Cruz-Conde R, Berjano P, Buitron Z. Ligamentum flavum hematoma presenting as progressive root compression in the lumbar spine. Spine (Phila Pa 1976). 1995;20:1506-1509. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 42] [Cited by in RCA: 42] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 12. | Minamide A, Yoshida M, Tamaki T, Natsumi K. Ligamentum flavum hematoma in the lumbar spine. J Orthop Sci. 1999;4:376-379. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 39] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 13. | Chen HC, Hsu PW, Lin CY, Tzaan WC. Symptomatic hematoma of cervical ligamentum flavum: case report. Spine (Phila Pa 1976). 2005;30:E489-E491. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 24] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 14. | Yamaguchi S, Hida K, Akino M, Seki T, Yano S, Iwasaki Y. Ligamentum flavum hematoma in the lumbar spine. Neurol Med Chir (Tokyo). 2005;45:272-276. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 28] [Article Influence: 1.4] [Reference Citation Analysis (0)] |