Published online Apr 16, 2021. doi: 10.12998/wjcc.v9.i11.2595
Peer-review started: December 1, 2020
First decision: December 21, 2020
Revised: December 28, 2020
Accepted: February 19, 2021
Article in press: February 19, 2021
Published online: April 16, 2021
Processing time: 121 Days and 21.2 Hours
Currently, open reduction internal fixation is the conventional surgical method for treatment of double ulna and radius fracture. However, open reduction is associated with a high risk of complications. This case of forearm double fracture involved a patient treated using an Acumed intramedullary nail. The patient experienced good follow-up outcomes. The Acumed forearm intramedullary nail enables early functional exercise and hastens healing of the fracture. Few studies have reported on the use of this approach for the treatment of fractures.
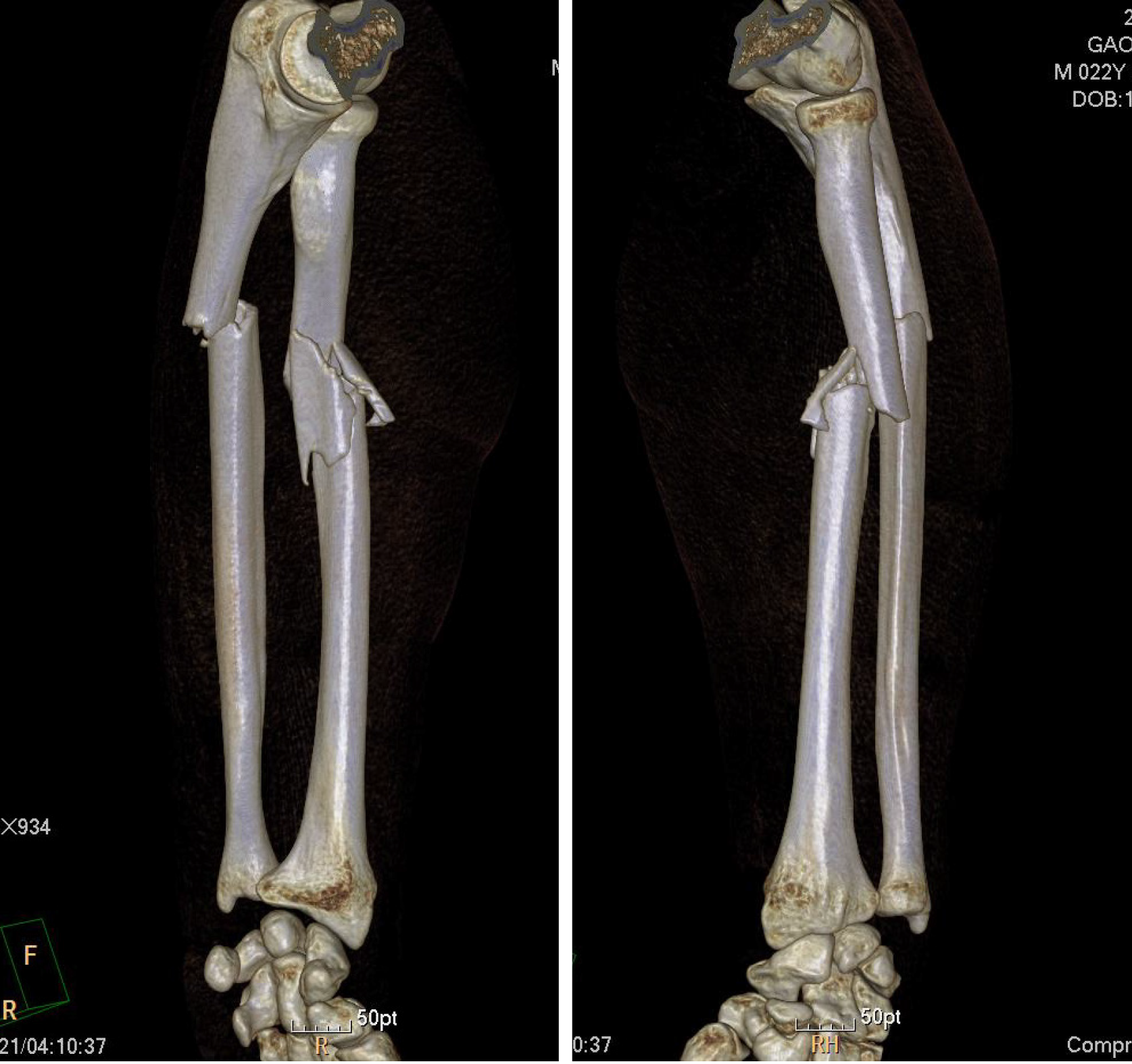
A 23-year-old male patient was admitted to hospital after 5 h of pain, swelling, and limited activity of left forearm caused by a careless fall. Physical examination showed stable basic vital signs, swelling of the left forearm, and severe pain when pressing on the injured part of the forearm. Further, friction was felt at the broken end of the bone; the skin was not punctured. Movement of the left hand was normal, and the left radial artery pulse was normal. Three-dimensional computed tomography examination showed an ulna fracture of the left forearm and comminuted fracture of the radius. The fracture was located in the upper third of the radius, with significant displacement on the fracture side. Clinical diagnosis further confirmed the left radius comminuted fracture and ulna fracture. After analyzing the fracture pattern, age, and other patient characteristics, we chose an Acumed nail for treatment and achieved good follow-up outcomes.
Acumed forearm intramedullary nail for fixation of ulna and radius fracture reduced complication risk and resulted in good follow-up outcomes.
Core Tip: Currently, open reduction internal fixation is the conventional surgical method for treatment of ulna and radius double fracture. However, that approach causes soft tissue damage of blood vessels, the periosteum, and the radial nerve. In addition, performing open reduction and internal fixation using a plate for treatment of double fractures of radius and ulna has side effects and complications. The Acumed forearm rod system was used in this patient for treatment of ulna and radius fracture with minimally invasive surgery; good follow-up outcomes were achieved.
- Citation: Liu JC, Huang BZ, Ding J, Mu XJ, Li YL, Piao CD. Minimally invasive treatment of forearm double fracture in adult using Acumed forearm intramedullary nail: A case report. World J Clin Cases 2021; 9(11): 2595-2601
- URL: https://www.wjgnet.com/2307-8960/full/v9/i11/2595.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v9.i11.2595
Ulna and radius diaphysis fractures are common in young adults and are mainly caused by violent injury. The fracture position can be lateral or overlapping, with angulation and rotational displacement after complete fracture of both diaphyses due to attachment of interosseous membrane and muscle. Forearm is mainly affected by rotation. Poor treatment of the fracture affects the function of the forearm or even the entire upper limb. Guidelines for treating intra-articular fracture are[1] help in choosing the appropriate fixation method to accurately restore limb function. Open reduction provides strong fixation and a high fracture healing rate, and is commonly used for fracture treatment[2]. However, the procedure is associated with complications, such as extensive soft tissue injury, radial nerve injury, refracture after plate removal, and bone nonunion caused by periosteum stripping[3]. The intramedullary nail treatment of forearm double fracture in adults is a minimally invasive procedure and is associated with fewer complications than conventional surgery. Previous studies report clinical use of the method. This study reports a case of forearm double fracture treated using an Acumed intramedullary nail, that achieved good follow-up outcomes.
A 23-year-old male patient was admitted into hospital after 5 h of pain, swelling, and limited activity of the left forearm caused by a careless fall.
The patient presented with swelling of the left forearm, severe pain on pressing the injured area, and friction at the broken end of the bone. The skin at the injured area was not punctured.
The patient was in good health and no history of other diseases.
The patient presented with signs of forearm fracture including, swelling, severe pain on pressing the injured area, and friction at the broken end of the bone. The skin at the site of injury was not punctured. Movement of the left hand was normal, and the left radial artery pulse was normal.
Three-dimensional computed tomography showed an ulna fracture of the left forearm and comminuted fracture of the radius. The fracture was located at the upper third of the radius with significant displacement on the fracture side (Figure 1).
The clinical diagnosis was left radius comminuted fracture and ulna fracture.
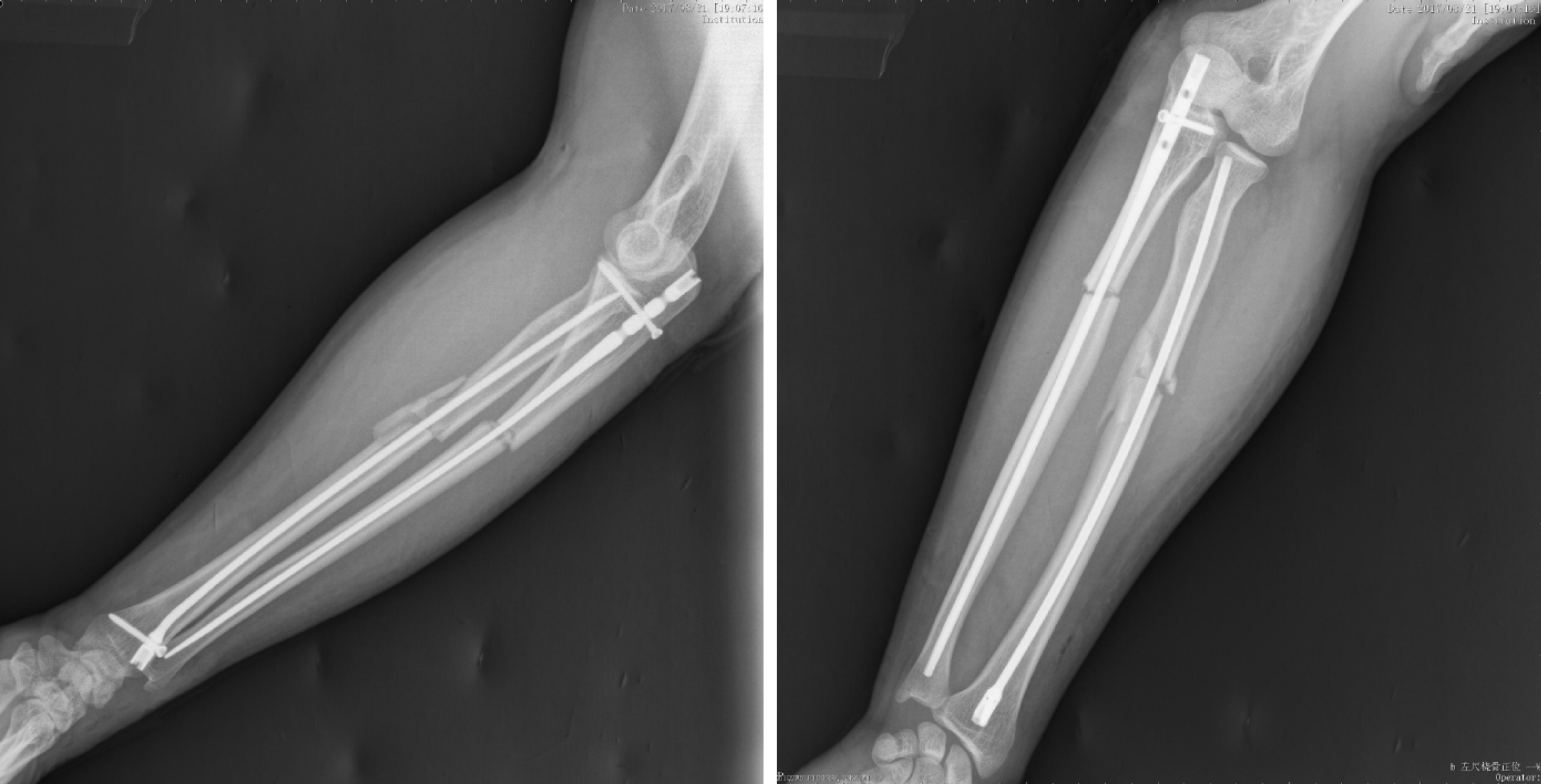
A routine preoperative examination was performed, and no obvious contraindications to surgery were found. Surgical treatment was performed, and an Acumed forearm nail was selected as the implant. The patient was placed in the supine position. The surgical area skin was disinfected after anesthesia. Sterile surgical towels and sheets were laid and disinfected using medical-grade alcohol. An incision of about 1 cm in length) was made on the left olecranon after the left ulna fracture was reduced by traction under elbow flexion. The subcutaneous tissue of the skin and the fascia were cut to expose the vertex of the ulnar olecranon for placement of the nail. A hole was drilled at the insertion point of the ulna olecranon with a reamer, and a guide needle was inserted into the medullary cavity extending to the distal end of the fracture. After the proximal end of the medullary reamer was opened, the medullary cavity was expanded layer by layer by the C arm through fluoroscopy assistance. The guide needle was pulled out, the upper intramedullary needle sight was installed, and a nail of the appropriate size was selected for internal fixation. The nail was inserted into the medullary cavity extending to the distal end of the fracture, and then fixed using a locking screw. Fluoroscopy of the C arm showed that the fracture was in a good position and that the internal fixation was accurate. After counting the instruments and gauze, the surgical area was disinfected and the incision was sutured layer by layer. Another incision was made on the back of the distal radius, approximately 3 cm in length. The subcutaneous tissue of the skin and fascia were cut and the tendon opened to expose the distal radial lister nodules. The lateral distal radial lister nodule was punched. Following the same steps described above, the nail was inserted into the medullary cavity to the proximal radius. Fluoroscopy of the C arm showed that the fracture was in a good position and that the internal fixation was accurate. The nail was then fixed using a locking screw. Passive movement of the left upper limb was observed. No abnormal movement found was found after the procedure. and X-ray examination after surgery showed good positioning of the fracture and good implant position (Figure 2). After counting the surgery devices and gauze, the incision was cleaned and sutured, and the area was covered with sterile gauze. The left upper limb was externally fixed with plaster.
Detumescence medication was administered and the area around the functional position of elbow and wrist joint was fixed with plaster for 4 wk to prevent excessive swelling of the forearm and osteofascial compartment syndrome. The patient underwent gradual rehabilitation exercise after removal of the plaster. In the first 6 wk after surgery, the patient underwent exercise for flexion and extension of the joints of the elbow and wrist. Forearm rotation exercise was performed after week 6.
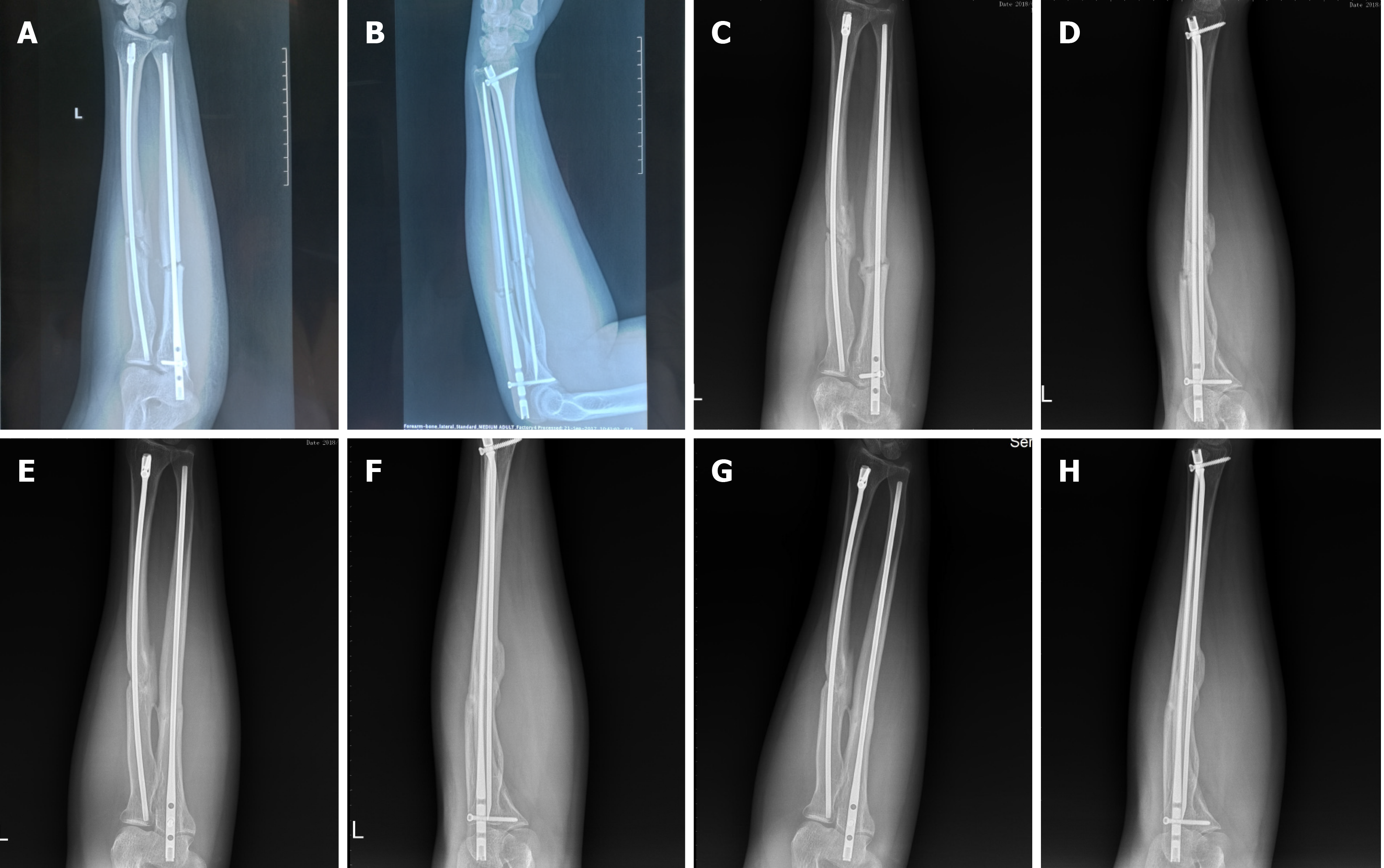
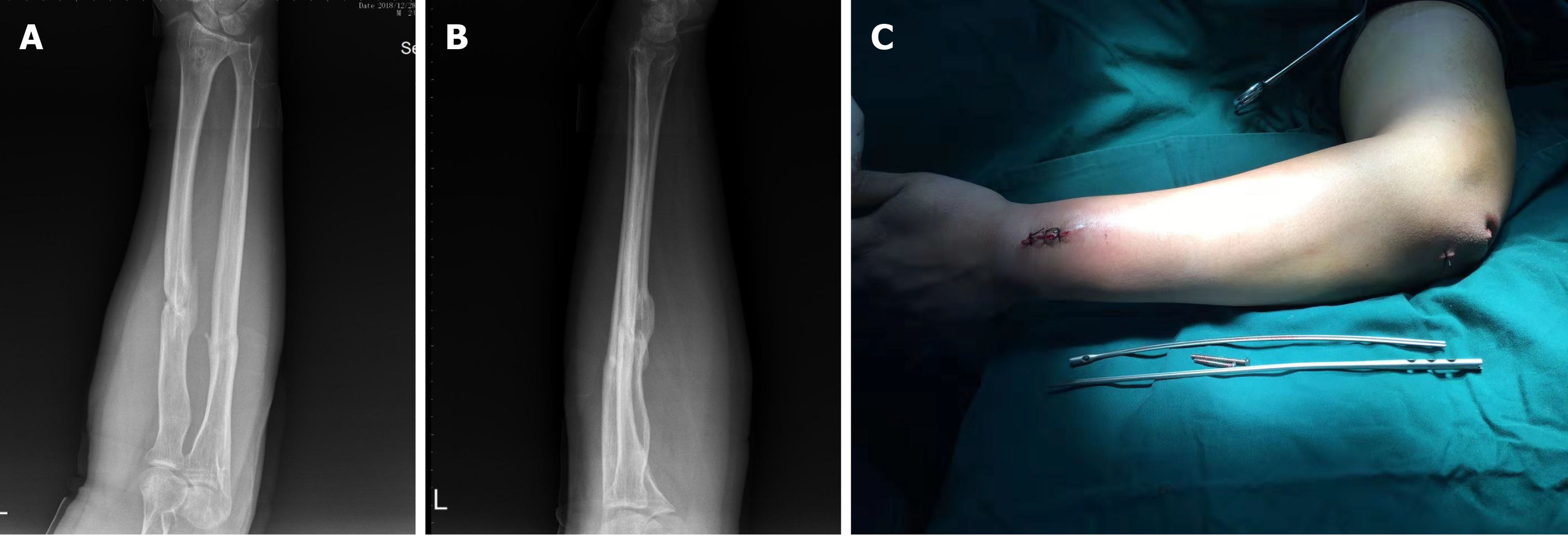
Limb function and imaging examinations were carried out at 1 mo, 3 mo, 6 mo, and 12 mo after surgery, to check for fracture displacement, implant loosening, delayed fracture healing, and fracture nonunion. Function of the fractured limb was evaluated using the disabilities of the arm, shoulder and hand (DASH) score. A score of 0 indicated that upper limb function was completely normal, and a score of 100 indicated that the upper limb function was extremely limited[4]. The DASH scores were 20, 14.2, 5, and 1.7 points (Figure 3). One month after the operation, a small amount of callus formation was seen on X-ray examination. The fracture line was still obvious, but the fracture remained in a good position and showed no signs of displacement. Six months after surgery, the fracture was almost healed. The ulna fracture line could be seen faintly, but the radial line was completely gone, with a small defect on the lateral radial edge. At the last follow-up, the imaging results showed complete fracture healing. As no fracture line was observed and the limb function had recovered well, we carried out the surgery to remove the implant successfully (Figures 4 and 5).
The forearm mainly provides rotation required for movement of the entire upper limb. Poor treatment of fractures of the forearm significantly affects the function of the upper limb. The fracture end is unstable after an ulna and radius double fracture due to the presence of muscle and interosseous membrane. Before the discovery of internal fixation technology, manual reduction and external plaster fixation were the main treatment methods for forearm double fractures. However, those methods are limited by unstable fixation, which may cause fracture malunion or nonunion. Therefore, surgical treatment is preferred over conservative treatment.
Closed reduction Kirschner wire fixation is also used in some situations. Unfortunately, because the Kirschner wire can easily undergo deformation, it is difficult to advance it into the medullary cavity. Moreover, it is difficult to rebuild the diaphyseal rotation alignment due to the unstable internal fixation, which increases the risk of needle withdrawal after surgery. The fixation method also requires a long interval before casting. The aforementioned shortcomings of fixation and the high fracture nonunion rate limit its widespread clinical application[5].
In recent years, elastic intramedullary nail technology has been widely adopted. In the treatment of forearm diaphyseal fractures, elastic intramedullary nail technology is only suitable for young children, with less trauma and fewer complications, and it does not destroy the epiphysis[6]. It is suitable for transverse, short oblique, and simple comminuted fractures. For long oblique or more complex comminuted fractures, it creates tension in the medullary cavity, and hence does not provide a good fixation effect. Its indications are relatively few[7].
A report on 47 forearm fracture patients treated by open reduction internal fixation by Iacobellis et al[8] found that 43 were successfully healed, for a fracture healing rate of 91.5%. Further, a satisfaction rate of 91.4% was attained using the Anderson scoring system. Open reduction internal fixation is widely used and accepted due to the high rate of fracture healing and satisfactory postoperative function[9]. Although open reduction internal fixation has a high fracture healing rate and good postoperative function, the approach is associated with a high risk of complications when used for treatment of forearm fractures. Open reduction provides stable fixation of the fracture area, making it easier to achieve anatomic reduction. On the other hand, it may damage blood vessels, the periosteum, and other soft tissues, thus affecting blood supply to the fracture area. In addition, a large exposed incision is made. Therefore, it is associated with an increased risk of surgical infection. Open reduction internal fixation can cause neurogenic injury of the radical nerve in cases where the fracture occurs in the upper third of the radius. In addition, Yao et al[10] reported an approximately 13% refracture rate after removal of the plate. Furthermore, plate internal fixation for treatment of forearm fractures is associated with postoperative complication rates of up to 25%[11]. Therefore, the effectiveness of open reduction internal fixation for the treatment of forearm fractures is limited. Notably, fixation treatment is characterized by reduced operation time, fewer postoperative complications, small incisions, and reduction in periosteal detachment[12]. However, fractures occurring in the upper third of the radius are associated with a high risk of radial nerve damage and postoperative press-fitting of the radial nerve. In this study, we explored an alternative of open reduction internal fixation using a nail, based on fracture position, age of the patient and better outcomes during follow-up period.
The first case study of treatment of forearm fracture was reported in 1913[14]. However, the initial implants were Rush rods, Kirschner wires, and elastic intramedullary nails, which lack locking and compressing functions. They therefore do not allow rotational and axial stability. Therefore, the duration of healing after using those internal rod systems was approximately 21%[13]. The Acumed forearm nail is more effective than previous approaches as it has interlocking screws at the insertion end to provide axial stability and achieve effective compression at the fracture end. Further, it provides an antirotation function through the paddle structure on the other side, thus improving stability at the fracture side, and promoting healing of the fracture. The Acumed intramedullary nail is effective in forearm and fibula fractures. Bugler et al[15] carried out a study on 105 patients with fibular fracture who were treated with the Acumed intramedullary nail. The method achieved good follow-up outcomes during an 8-year follow-up period after surgery. In this case, an Acumed nail was used to treat a forearm fracture after analysis of the fracture pattern, patient age, and other characteristics.
Fracture characteristics of a patient with forearm fracture were analyzed and Acumed nail was used for fixation of the fracture. The surgical procedure was simple, with minimal bleeding. The study findings show that this invasive operation did not affect the blood supply to the fracture. The procedure did not injure soft tissue and it achieved relatively stable biological internal fixation with good surgical results. Use of the Acumed forearm intramedullary nail is a novel approach for treatment of double forearm fractures.
Manuscript source: Unsolicited manuscript
Specialty type: Neuroimaging
Country/Territory of origin: China
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): B
Grade C (Good): 0
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Philips CA S-Editor: Liu M L-Editor: Filipodia P-Editor: Xing YX
| 1. | He HY, Zhang JZ, Wang XW, Liu Z. [Acumed intramedullary nail for the treatment of adult diaphyseal both-bone forearm fractures]. Zhongguo Gu Shang. 2018;31:803-807. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 2. | Rehman S, Sokunbi G. Intramedullary fixation of forearm fractures. Hand Clin. 2010;26:391-401, vii. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 15] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 3. | Lee SK, Kim KJ, Lee JW, Choy WS. Plate osteosynthesis vs intramedullary nailing for both forearm bones fractures. Eur J Orthop Surg Traumatol. 2014;24:769-776. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 24] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 4. | Hudak PL, Amadio PC, Bombardier C. Development of an upper extremity outcome measure: the DASH (disabilities of the arm, shoulder and hand) [corrected]. Am J Ind Med. 1996;29:602-608. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 46] [Reference Citation Analysis (0)] |
| 5. | SAGE FP, SMITH H. Medullary fixation of forearm fractures. J Bone Joint Surg Am. 1957;39-A:91-98. [PubMed] |
| 6. | Andaloussi S, Amine Oukhouya M, Alaoui O, Atarraf K, Chater L, Afifi MA. [Elastic stable intramedullary nailing (ESIN) in the treatment of both-bone forearm fractures in the child: about 87 cases]. Pan Afr Med J. 2017;27:68. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 7. | Goodbody CM, Lee RJ, Flynn JM, Sankar WN. Titanium Elastic Nailing for Pediatric Tibia Fractures: Do Older, Heavier Kids Do Worse? J Pediatr Orthop. 2016;36:472-477. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 27] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 8. | Iacobellis C, Biz C. Plating in diaphyseal fractures of the forearm. Acta Biomed. 2014;84:202-211. [PubMed] |
| 9. | Köse A, Aydın A, Ezirmik N, Yıldırım ÖS. A comparison of the treatment results of dpen reduction internal fixation and intramedullary nailing in adult forearm diaphyseal fractures. Ulus Travma Acil Cerrahi Derg. 2017;23:235-244. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 5] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 10. | Yao CK, Lin KC, Tarng YW, Chang WN, Renn JH. Removal of forearm plate leads to a high risk of refracture: decision regarding implant removal after fixation of the forearm and analysis of risk factors of refracture. Arch Orthop Trauma Surg. 2014;134:1691-1697. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 34] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 11. | Kuyucu E, Koçyiğit F, Ciftçi L. The importance of patient compliance in nonunion of forearm fracture. Int J Surg Case Rep. 2014;5:598-600. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 7] [Article Influence: 0.6] [Reference Citation Analysis (1)] |
| 12. | Zhao L, Wang B, Bai X, Liu Z, Gao H, Li Y. Plate Fixation Versus Intramedullary Nailing for Both-Bone Forearm Fractures: A Meta-analysis of Randomized Controlled Trials and Cohort Studies. World J Surg. 2017;41:722-733. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 13] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 13. | Dehghan N, Schemitsch EH. Intramedullary nail fixation of non-traditional fractures: Clavicle, forearm, fibula. Injury. 2017;48 Suppl 1:S41-S46. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 14] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 14. | Bartoníček J, Kozánek M, Jupiter JB. History of operative treatment of forearm diaphyseal fractures. J Hand Surg Am. 2014;39:335-342. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 12] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 15. | Bugler KE, Watson CD, Hardie AR, Appleton P, McQueen MM, Court-Brown CM, White TO. The treatment of unstable fractures of the ankle using the Acumed fibular nail: development of a technique. J Bone Joint Surg Br. 2012;94:1107-1112. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 91] [Cited by in RCA: 97] [Article Influence: 7.5] [Reference Citation Analysis (0)] |