Published online Oct 6, 2019. doi: 10.12998/wjcc.v7.i19.3126
Peer-review started: March 15, 2019
First decision: July 30, 2019
Revised: August 20, 2019
Accepted: August 25, 2019
Article in press: August 26, 2019
Published online: October 6, 2019
Processing time: 200 Days and 18.2 Hours
Clear cell sarcoma (CCS) of soft tissue is a rare malignant soft tissue sarcoma usually reported to locate at distal end of extremities and rarely at trunk. Herein, we report a case of CCS in pleural cavity.
A 31-year-old male was admitted for an uncertain mass in left pleural cavity in routine physical examination without any symptoms. A VATS surgery was performed to remove the tumor. The pathological finding displayed a cystic mass with 6.5 cm at the longest diameter, dark red in section and cysts could be found locally. A strong expression of S-100, HMB45 and Vimentin was detected in immunohistochemical staining, which was inclined to the diagnosis of the CCS of soft tissue. The patient refused chemotherapy, radiotherapy and targeted therapy because of the personal financial situation. Follow-up computed tomography scans were done at the 90th postoperative day and the 180th postoperative day, and no obvious sign of recurrence was found till now.
CCS of soft tissue also can be found in pleural cavity although in an extremely rare incidence. Radical resection is useful to improve the prognosis.
Core tip: Clear cell sarcoma (CCS) is a rare malignant tumor of soft tissue usually arising from extremities. Now we reported a case of CCS located on the chest cavity, confirmed by the positive stain of HMB-45 and S-100 mark in immunohistochemistry. Radical resection of the tumor was performed and the short-term outcome was good.
- Citation: Chen YT, Yang Z, Li H, Ni CH. Clear cell sarcoma of soft tissue in pleural cavity: A case report. World J Clin Cases 2019; 7(19): 3126-3131
- URL: https://www.wjgnet.com/2307-8960/full/v7/i19/3126.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v7.i19.3126
Clear cell sarcoma (CCS) of soft tissue is a rare malignant soft tissue sarcoma that represents about 1% of all sarcoma[1]. The true origination of CCS is still uncertain, which might be one type of synovial sarcoma because SSC usually arises in association with tendons and aponeuroses and has the same bidirectional differentiation ability as synovial sarcoma. However, on account of sharing similar morphology with malignant melanoma, SSC seems more likely to derive from neural crest cells, which produces melanin typically and has positive HMB-45 and S-100 mark stained in immunohistochemistry[2]. CCS has been usually reported to locate at distal end of extremities and rarely at trunk[3]. According to the literature review, there is no report of CCS in pleural cavity till now.
A 31-year-old male was admitted to our hospital for an uncertain mass in left pleural cavity in routine physical examination without any symptoms.
His past history was unremarkable.
His family history was unremarkable.
Physical examination is normal.
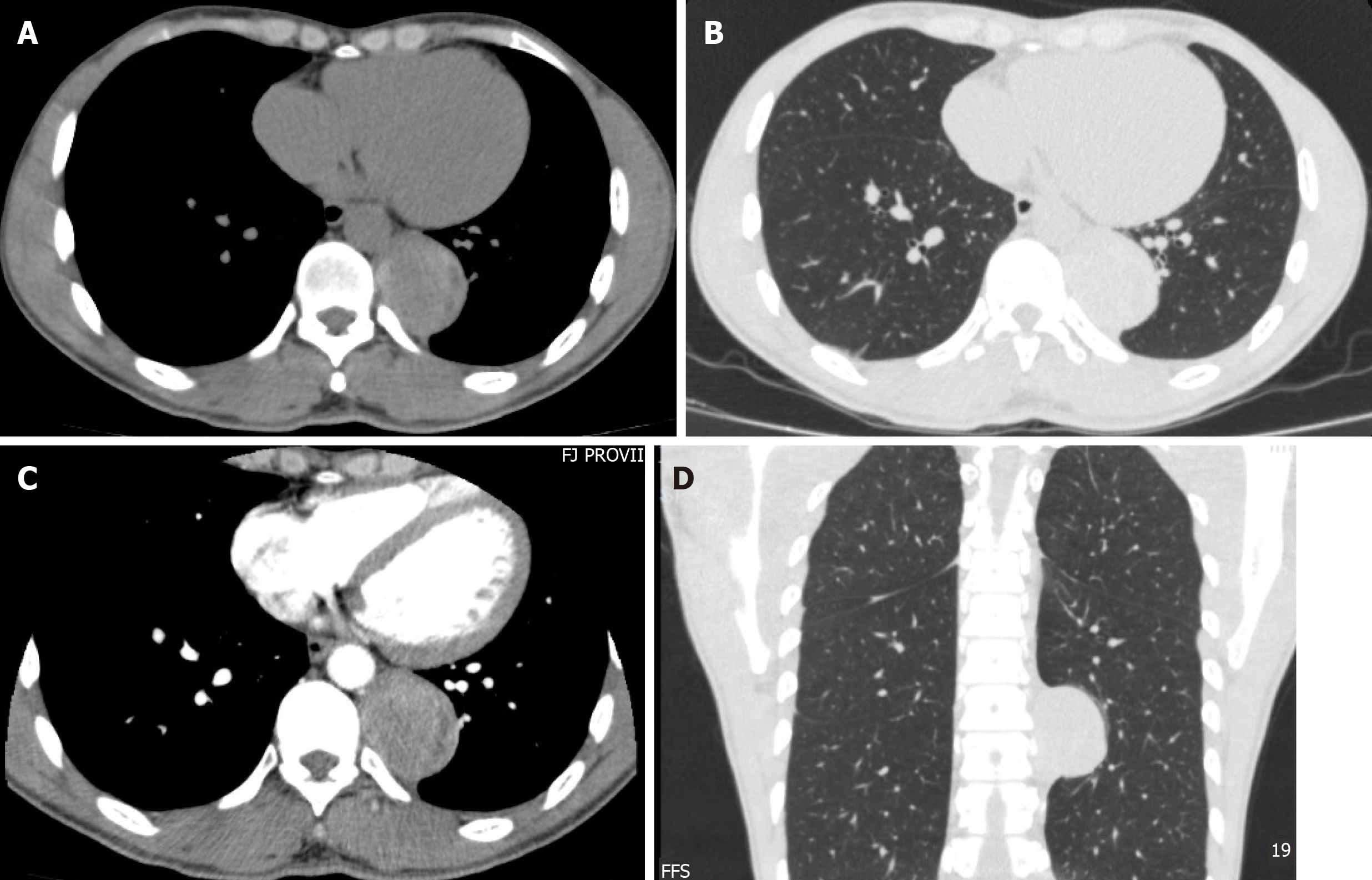
Routine blood parameters were within the normal range. Tumor marker measurement results were as follows: Carcinoembryonic antigen, 0.64 ng/mL; alphafetoprotein, 1.77 ng/mL; CA199, 5.80 U/mL. The enhanced thoracic computed tomography (CT) demonstrated a posterior mediastinal mass about 6 cm diameter in the left pleural cavity, right nearby the 9th and 10th thoracic vertebrae beside the thoracic descending aorta, with an uneven enhancement (Figure 1). A neurologic tumor was suspected as the first diagnosis.
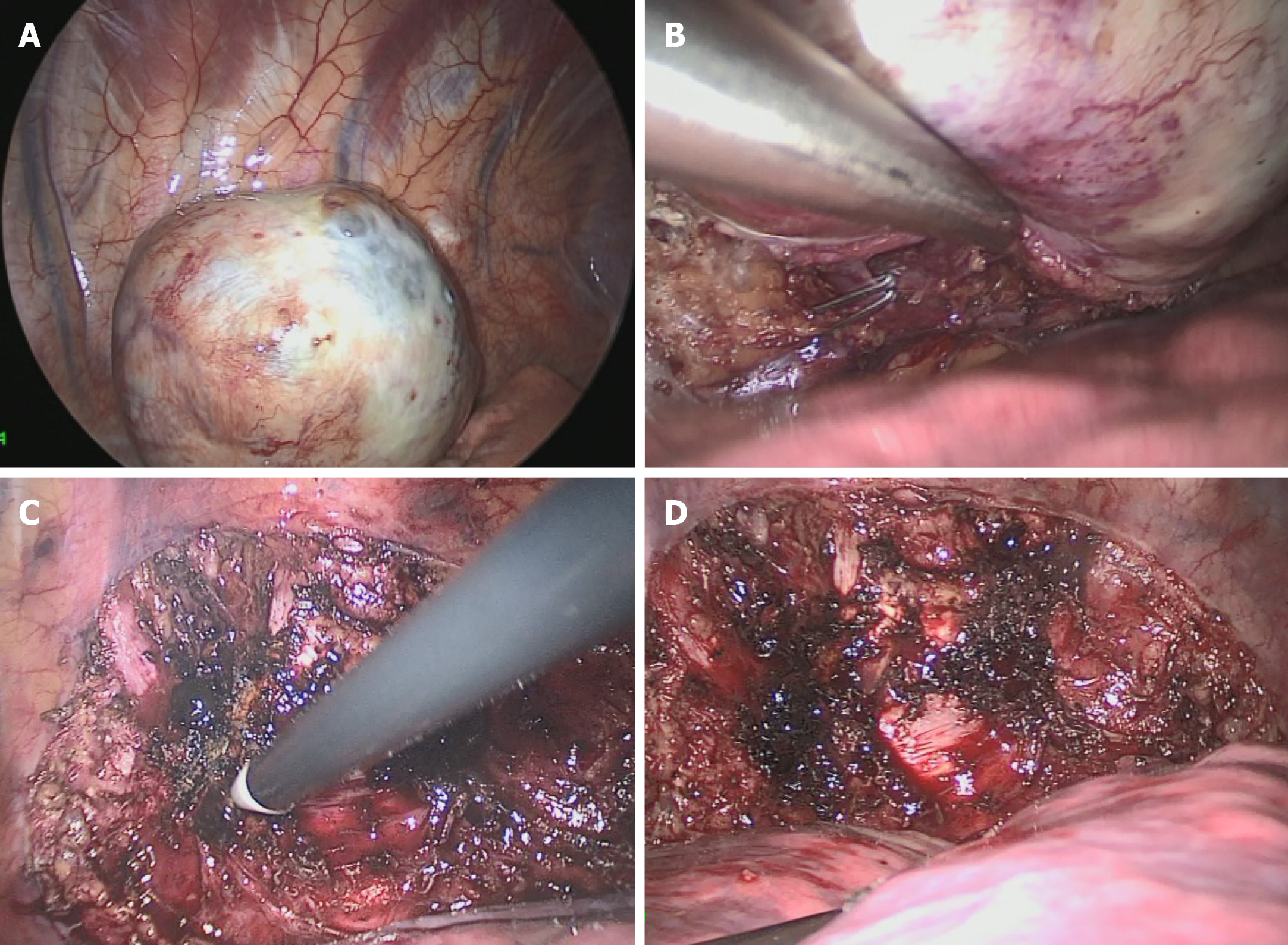
A video-assisted thoracoscopic surgery was performed to remove the mass. During the operation, the patient was placed in a right lateral decubitus position at 70 degree with unilateral ventilation under general anesthesia. Three trocars were placed at 3th, 4th and 8th intercostal space. Under the endoscopy, there was no obvious effusion in the pleural cavity. A spherical mass with broad base was found on the posterior chest wall, just left side by the 9th thoracic vertebra, close to the aorta while no obvious adhesion was found between the tumor and the aorta or vertebra. Careful dissection was done with the electrocautery and the harmonic in turn. A feeding branch from the intercostal artery and a draining vein to the hemiazygos vein were ligated and cut. Finally, the mass was removed under en bloc excision with a relatively clear margin. Furthermore, the base plane on local chest wall was deal with electrocoagulation to ensure no residual tumor (Figure 2). The drain tube was put and the chest wall wound was close routinely. The chest tube was removed on the 1st postoperative day and the patient was discharged on the 5th postoperative day with no events.
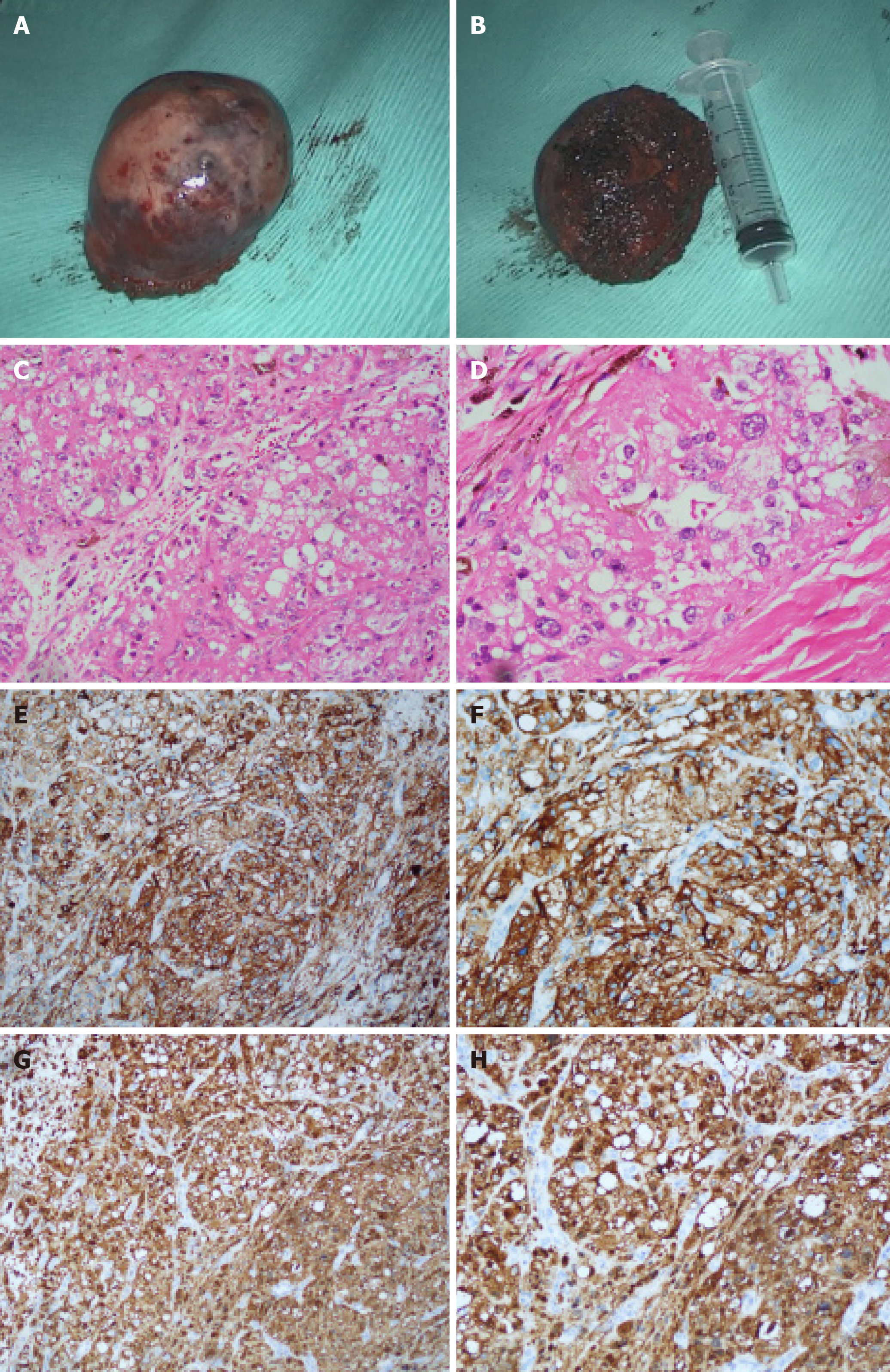
The pathological finding displayed a cystic mass with 6.5 cm at the longest diameter, dark red in section and cysts could be found locally. A strong expression of S-100, HMB45 and Vimentin was detected in immunohistochemical staining (Figure 3), which was inclined to the diagnosis of the CCS of soft tissue[2,3].
A video-assisted thoracoscopic surgery was performed to dissect the tumor. After the surgery, the patient refused the suggestion of all the following treatments such as chemotherapy, radiotherapy and targeted therapy because of the personal financial situation.
Meanwhile, two postoperative follow-up CT scan were done on the 90th postoperative day and the 180th postoperative day, and no obvious sign of recurrence was found till now.
CCS is a rare malignant tumor of soft tissue with uncertain origination, which seems most likely to be diagnosed in adolescents and middle-aged people. The diagnosis of CCS always seems to be a challenge if lack of pathologic immunohistochemical results. Although CCS has the similar morphologic appearance with malignant melanoma, it is possible for pathologists today to distinguish them correctly by the difference of histopathologic and cytogenetic features between them[2]. CCS usually locates in the deep soft tissue or under the deep fascia, in close relation to tendons and aponeuroses at the distal end of extremities, such as foot and knee, rarely at the trunk, with no epidermal involvement[4-9] Differentiation diagnosis from other sarcoma should be made including epithelioid sarcoma, synovial sarcoma, epithelioid malignant peripheral nerve sheath tumor, alveolar soft part sarcoma and so on[3].
Radical resection of the tumor might be the most effective way to treat CCS. Before the operation, magnetic resonance imaging (MRI) of thoracic vertebra is done to exclude the possible invasion of the tumor to the vertebra. The intraoperative exploration also ensures that there is no obvious adhesion between the spine and the tumor. If the vertebra or posterior ribs are invaded by tumor, the nearby vertebra and ribs should be removed with the tumor under en bloc excision and the reconstruction of chest wall should be made.
Adjuvant radiotherapy or chemotherapy might not be necessary for the poor evidence of therapeutic effect on SCC[10]. However, radiation therapy is recommended if there is possible tumor residual after surgery to achieve better outcome[11]. The targeted therapy seems to be a good treatment to SSC with some encouraging evidence on malignant melanoma, but there is still a long way to go[12]. Regular follow-up including CT scan or MRI should be made every 3 mo postoperatively on account of the high risk of early metastases and recurrence of SSC[13].
CCS of soft tissue also can be found in pleural cavity although in an extremely rare incidence. Radical resection is useful to improve the prognosis.
Manuscript source: Unsolicited manuscript
Specialty type: Medicine, Research and Experimental
Country of origin: China
Peer-review report classification
Grade A (Excellent): 0
Grade B (Very good): B
Grade C (Good): C
Grade D (Fair): D
Grade E (Poor): 0
P-Reviewer: Kutlubay Z, Petrucciani N, Simone G S-Editor: Dou Y L-Editor: Filipodia E-Editor: Qi LL
| 1. | Ibrahim RM, Steenstrup Jensen S, Juel J. Clear cell sarcoma-A review. J Orthop. 2018;15:963-966. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 25] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 2. | Yang L, Chen Y, Cui T, Knösel T, Zhang Q, Geier C, Katenkamp D, Petersen I. Identification of biomarkers to distinguish clear cell sarcoma from malignant melanoma. Hum Pathol. 2012;43:1463-1470. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 43] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 3. | James AW, Dry SM. Diagnostically Challenging Epithelioid Soft Tissue Tumors. Surg Pathol Clin. 2015;8:309-329. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 7] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 4. | Kindblom LG, Lodding P, Angervall L. Clear-cell sarcoma of tendons and aponeuroses. An immunohistochemical and electron microscopic analysis indicating neural crest origin. Virchows Arch A Pathol Anat Histopathol. 1983;401:109-128. [PubMed] |
| 5. | Kawai A, Hosono A, Nakayama R, Matsumine A, Matsumoto S, Ueda T, Tsuchiya H, Beppu Y, Morioka H, Yabe H; Japanese Musculoskeletal Oncology Group. Clear cell sarcoma of tendons and aponeuroses: a study of 75 patients. Cancer. 2007;109:109-116. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 91] [Cited by in RCA: 98] [Article Influence: 5.4] [Reference Citation Analysis (0)] |
| 6. | Juel J, Ibrahim RM. A case of clear cell sarcoma-A rare malignancy. Int J Surg Case Rep. 2017;36:151-154. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 7] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 7. | Baus A, Culie D, Duong LT, Ben Lakhdar A, Schaff JB, Janot F, Kolb F. Primary clear cell sarcoma of the tongue and surgical reconstruction: About a rare case report. Ann Chir Plast Esthet. 2019;64:98-105. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 6] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 8. | Zhang X, Hu C, Cai L. A giant clear cell sarcoma on right scapular: A case report. Acta Orthop Traumatol Turc. 2016;50:473-476. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 5] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 9. | Rocco G, de Chiara AR, Fazioli F, Scognamiglio F, La Rocca A, Apice G, Riva C. Primary giant clear cell sarcoma (soft tissue malignant melanoma) of the sternum. Ann Thorac Surg. 2009;87:1927-1928. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 8] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 10. | Hatcher H, Benson C, Ajithkumar T. Systemic Treatments in Soft Tissue Sarcomas. Clin Oncol (R Coll Radiol). 2017;29:507-515. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 12] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 11. | Al-Absi E, Farrokhyar F, Sharma R, Whelan K, Corbett T, Patel M, Ghert M. A systematic review and meta-analysis of oncologic outcomes of pre- versus postoperative radiation in localized resectable soft-tissue sarcoma. Ann Surg Oncol. 2010;17:1367-1374. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 93] [Cited by in RCA: 76] [Article Influence: 5.1] [Reference Citation Analysis (0)] |
| 12. | Stacchiotti S, Marrari A, Dei Tos AP, Casali PG. Targeted therapies in rare sarcomas: IMT, ASPS, SFT, PEComa, and CCS. Hematol Oncol Clin North Am. 2013;27:1049-1061. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 14] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 13. | Bianchi G, Charoenlap C, Cocchi S, Rani N, Campagnoni S, Righi A, Frisoni T, Donati DM. Clear cell sarcoma of soft tissue: a retrospective review and analysis of 31 cases treated at Istituto Ortopedico Rizzoli. Eur J Surg Oncol. 2014;40:505-510. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 48] [Article Influence: 4.4] [Reference Citation Analysis (0)] |