Published online Aug 6, 2019. doi: 10.12998/wjcc.v7.i15.2128
Peer-review started: March 28, 2019
First decision: May 31, 2019
Revised: June 24, 2019
Accepted: July 3, 2019
Article in press: July 4, 2019
Published online: August 6, 2019
Processing time: 133 Days and 1.2 Hours
Single coronary artery (SCA) originating from a solitary ostium in the aorta and perfusing the entire myocardium is a very rare congenital anomaly of the coronary artery. Furthermore, a right coronary artery (RCA) arising from the mid segment of the left anterior descending artery (LAD) is an extremely uncommon variation of SCA.
A 76-year-old woman presented a 5-mo history of exertional angina. Selective coronary angiography revealed an SCA, with severe ostial stenosis that originated from the left sinus of Valsalva and bifurcated normally into the LAD and circumflex coronary artery. In addition, an anomalous RCA originated from the mid segment of the LAD as a separate branch. Successful balloon angioplasty and stenting for the SCA ostial stenosis were performed on the patient.
Percutaneous coronary intervention (PCI) of the main trunk for SCA is very similar to PCI of an unprotected left main coronary artery. Although technical difficulties and risks do exist, PCI for severe ostial stenosis of the main trunk is safe and efficacious in selected SCA patients.
Core tip: The right coronary artery arising from the mid segment of the left anterior descending artery is an extremely uncommon variation of single coronary artery (SCA). In this report, a 76 year-old female presented a 5-month history of exertional angina. Selective coronary angiography revealed an SCA, with severe ostial stenosis. Successful balloon angioplasty and stenting for the SCA ostial stenosis were performed on this case. Although technical difficulties and definite risk do exist, percutaneous coronary intervention for severe ostial stenosis of main trunk is safe and efficacious in selected SCA cases.
- Citation: Wu Q, Li ZZ, Yue F, Wei F, Zhang CY. Percutaneous coronary intervention for ostial lesions of the left main stem in a patient with congenital single left coronary artery: A case report. World J Clin Cases 2019; 7(15): 2128-2133
- URL: https://www.wjgnet.com/2307-8960/full/v7/i15/2128.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v7.i15.2128
Single coronary artery (SCA) that originates from a single ostium in the aortic trunk and perfuses the entire myocardium is an extremely rare congenital anomaly of the coronary artery. The incidence of SCA ranges from 0.016% to 0.066% in the patient population undergoing coronary angiography[1-3]. Myocardial perfusion could be affected in patients with different SCA subtypes, such as SCA arising ectopically from the right aortic sinus and passing between the aorta and pulmonary artery before dividing into the left anterior descending artery (LAD) and left circumflex artery, slit-like ostium due to an acute angle of SCA, or those complicated with proximal atherosclerotic stenosis[4-6]. Coronary artery ostioplasty and bypass grafting are recommended as the first-line revascularization therapeutic strategy for these subtypes of SCA which can cause serious, even fatal, consequences[7,8]. In this case report, a patient with SCA, combined with severe ostial lesions of the left main coronary artery (LM) and significant stenosis of the left anterior descending artery (LAD), was successfully treated by percutaneous coronary intervention (PCI).
A 76-year-old woman with a medical history of hypertension and hypercholestero-lemia was admitted with progressive angina over five months.
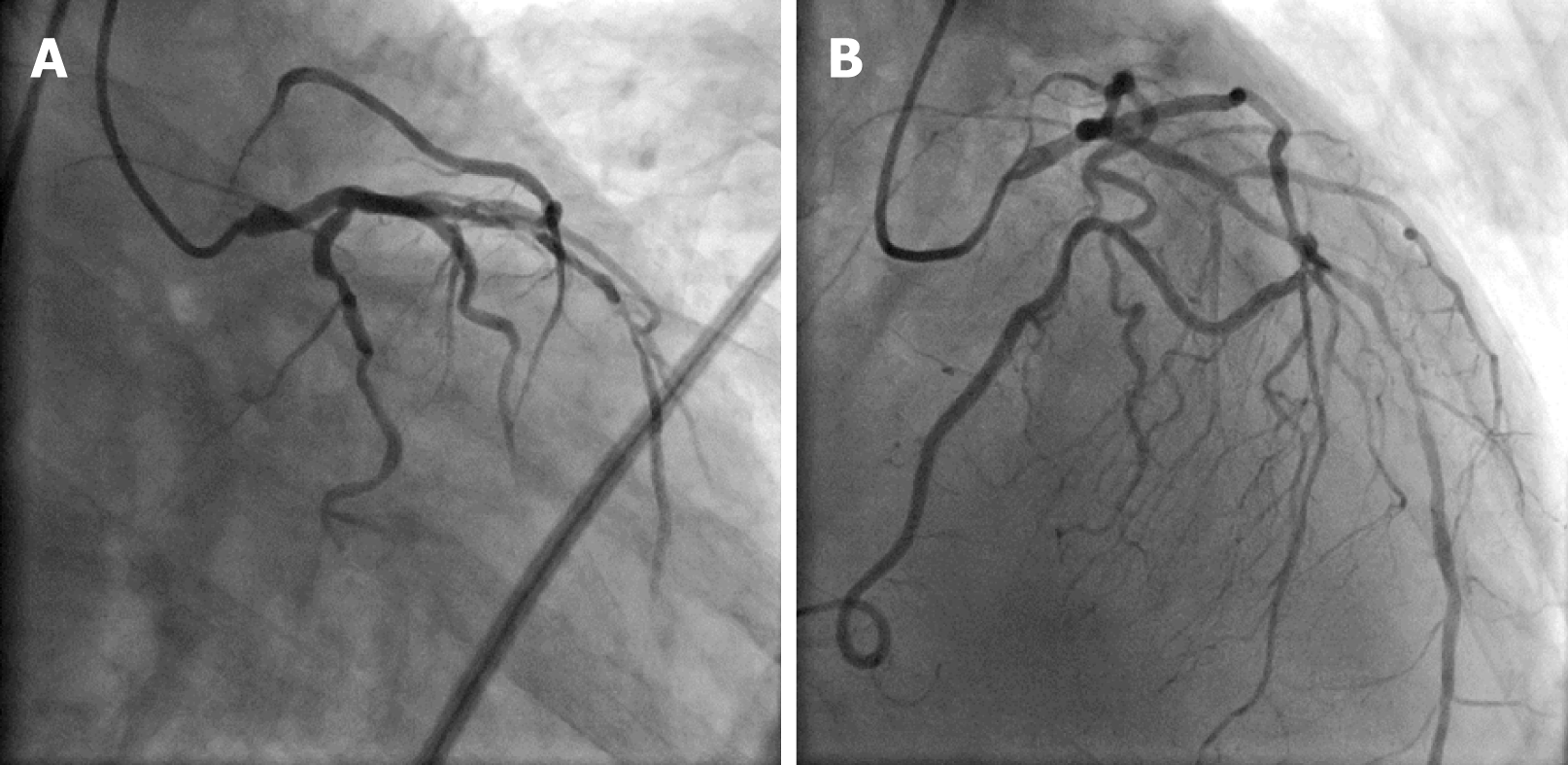
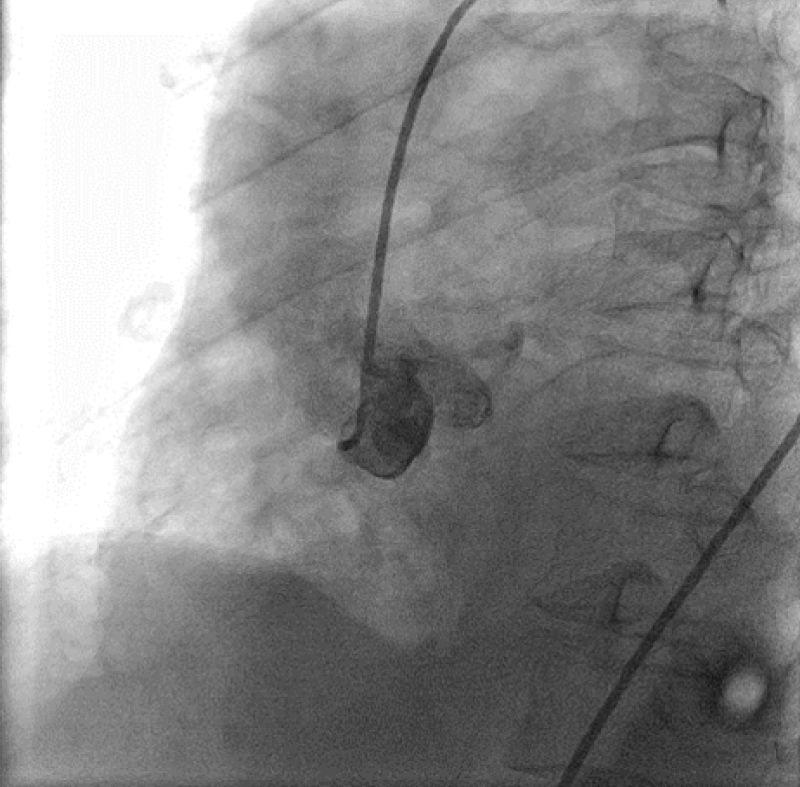
Electrocardiography showed non-specific ST-T abnormalities. The transthoracic echocardiography findings were normal for left ventricular performance without segmental hypokinesis. Diagnostic coronary angiography performed via the transfemoral approach showed that the LM, which normally originates from the left sinus of the Valsalva, had a 95% ostial calcified stenosis and slight shaft lesion. The LM branched into the normal left circumflex artery and the LAD with a diffuse lesion (70%-99%) in its mid segment with delayed distal flow. An anomalous branch without significant lesions arose from the mid-portion of the LAD and perfused the notional area of the right coronary artery (RCA) (Figure 1). The LAD wrapped around the apex, had an extended length, and then supplied to the posterior and inferior wall. Aortography revealed a blunt right and noncoronary sinus without any stumps (Figure 2).
The patient was diagnosed with coronary atherosclerotic heart disease with unstable angina; essential hypertension and hypercholesterolemia; and congenital SCA anomaly with branching of the RCA originating from the LAD, complicated with ostial LM lesions and a mid-segment stenosis of the LAD.
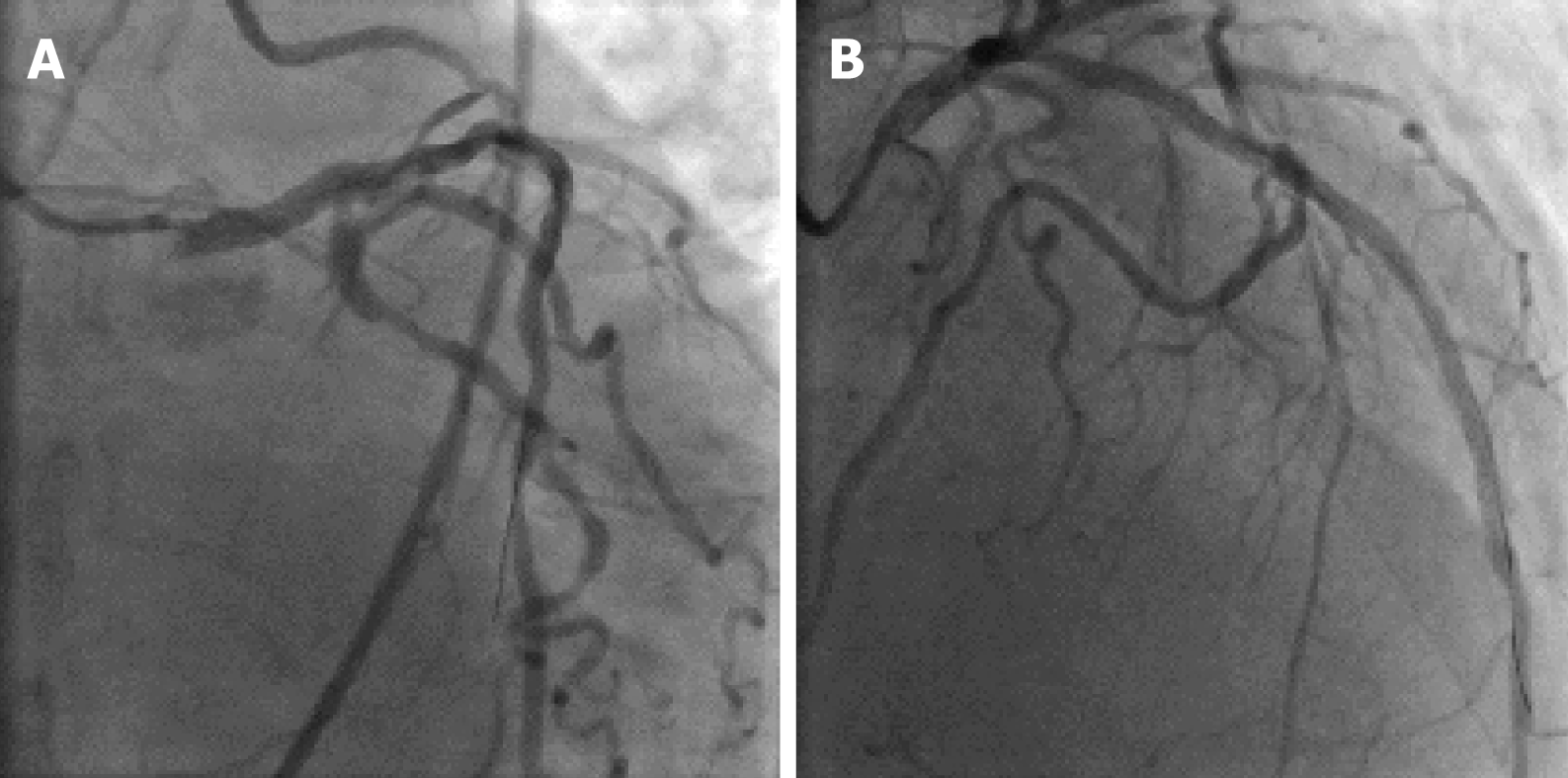
Based on these findings, surgical treatment was advised for the patient. However, she refused coronary artery bypass grafting and instead accepted PCI. A 6F Judkin’s left 4 guiding catheter was used to engage the main trunk and an intra-aortic vacant guide wire was placed to prevent a decrease in blood pressure in the coronary artery. After balloon pre-dilatation of the lesion around the LM and LAD, two sirolimus-eluting stents (2.5 mm × 33 mm and 3.0 mm × 33 mm) were placed at the middle LAD and then a 3.5 mm × 18 mm sirolimus-eluting stent at the ostial and shaft of the single coronary trunk was successfully deployed. Balloon post-dilatations of the entire stented segment were performed per standard procedure. The final angiographic results were satisfactory as demonstrated by thrombolysis in myocardial infarction grade 3 flow (Figure 3). The collaterals from the RCA and left circumflex artery were still visible.
Postoperatively, the patient was treated with guideline-directed medical therapy, which included aspirin, clopidogrel, irbesartan, and atorvastatin. The patient was followed at 6-mo intervals. No myocardial ischemia symptoms, changes in electrocardiography, cardiac dysfunction, or adverse cardiac events were noted during the three-year follow-up period.
SCA is a rare congenital anomaly of the coronary artery and is usually found by coronary angiography or necropsy. An SCA may arise with a single ostium from either the left Valsalva sinus or the right sinus. This causes confusion on where to cannulate another coronary artery ostium upon coronary angiography. Multislice computed tomography and magnetic resonance imaging can also aid in the diagnosis of SCA[4,9,10]. Multislice computed tomography may be superior to conventional selective coronary angiography in confirming and visualizing the origin, course, and termination of the SCA. Magnetic resonance coronary angiography, without radiation and contrast medium, has advantages in providing the spatial position of SCA[11,12].
Lipton et al[13] originally classified these coronary variations based on the site of origin, anatomical distribution, and course of the branches. Type L or R describes SCA that arises from the sinus of Valsalva and divides them into class I-III. Class I denotes SCA following the normal left or right course. In class II, an anomalous artery arises from the proximal part of the normally located opposite coronary artery and crosses at the base of the heart as a large transverse trunk to supply the contralateral coronary artery. Class III represents the LAD and the circumflex artery originating separately from the proximal part of the normal RCA. In classes II and III, based on the relationship between the anomalous coronary artery, the aorta, and the pulmonary artery, the “A” refers to the anomalous artery passing anterior to the pulmonary artery, and “B” refers to it coursing between the aorta and pulmonary artery, while “P” refers to it passing posterior to the large vessels. Yamanaka et al[2] and Shirani et al[14] modified the classification to describe the origin and course of these coronary anomalies. The anomalous origin of the RCA arose from the midportion of LAD in our patient, which is an extremely rare variation of SCA and does not fall under any subtype of Lipton's classification[15,16]. This kind of congenital anomaly generally remains asymptomatic. However, the origin of the anomalies and the course of the coronary artery are heterogeneous variations of clinical presentations and consequences[17].
There has been no consensus regarding the risk for atherosclerosis in patients with SCA. However, the myocardial ischemia symptoms in our patient were caused apparently by atherosclerotic stenosis of the LM and LAD, and not the anomaly itself. Unprotected LM stenosis has been traditionally treated using coronary artery bypass grafting. Improvements in drug-eluting stents and techniques have led to increased use of PCI on unprotected LM[18,19]. Results from randomized clinical trials and registries have confirmed that PCI of the LM lesion is safe and efficacious in selected patients with low or intermediate angiographic risk scores[20,21]. However the PCI procedure for the main trunk ostial lesion of SCA is still a technical challenge for surgeons and may be of high risk. Stenting on the shaft and distal lesions of the LM have been described previously only in three patients[22-24]. However, this report is the first to describe PCI for severe ostial main stem stenosis and SCA with an anomalous origin of the RCA arising from the LAD.
Manuscript source: Unsolicited manuscript
Specialty type: Medicine, research and experimental
Country of origin: China
Peer-review report classification
Grade A (Excellent): 0
Grade B (Very good): B, B
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Castro-Fernandez M, Nagao M, Kruis W S-Editor: Wang JL L-Editor: Wang TQ E-Editor: Xing YX
| 1. | Yildiz A, Okcun B, Peker T, Arslan C, Olcay A, Bulent Vatan M. Prevalence of coronary artery anomalies in 12,457 adult patients who underwent coronary angiography. Clin Cardiol. 2010;33:E60-E64. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 86] [Cited by in RCA: 116] [Article Influence: 8.3] [Reference Citation Analysis (0)] |
| 2. | Yamanaka O, Hobbs RE. Coronary artery anomalies in 126,595 patients undergoing coronary arteriography. Cathet Cardiovasc Diagn. 1990;21:28-40. [PubMed] |
| 3. | Desmet W, Vanhaecke J, Vrolix M, Van de Werf F, Piessens J, Willems J, de Geest H. Isolated single coronary artery: a review of 50,000 consecutive coronary angiographies. Eur Heart J. 1992;13:1637-1640. [PubMed] |
| 4. | Brothers JA, Whitehead KK, Keller MS, Fogel MA, Paridon SM, Weinberg PM, Harris MA. Cardiac MRI and CT: differentiation of normal ostium and intraseptal course from slitlike ostium and interarterial course in anomalous left coronary artery in children. AJR Am J Roentgenol. 2015;204:W104-W109. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 55] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 5. | Kim SY, Seo JB, Do KH, Heo JN, Lee JS, Song JW, Choe YH, Kim TH, Yong HS, Choi SI, Song KS, Lim TH. Coronary artery anomalies: classification and ECG-gated multi-detector row CT findings with angiographic correlation. Radiographics. 2006;26:317-33; discussion 333-4. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 209] [Cited by in RCA: 178] [Article Influence: 9.4] [Reference Citation Analysis (0)] |
| 6. | Basso C, Maron BJ, Corrado D, Thiene G. Clinical profile of congenital coronary artery anomalies with origin from the wrong aortic sinus leading to sudden death in young competitive athletes. J Am Coll Cardiol. 2000;35:1493-1501. [PubMed] |
| 7. | Angelini P, Walmsley RP, Libreros A, Ott DA. Symptomatic anomalous origination of the left coronary artery from the opposite sinus of valsalva. Clinical presentations, diagnosis, and surgical repair. Tex Heart Inst J. 2006;33:171-179. [PubMed] |
| 8. | Anuwatworn A, Karta P, Yee J, Li S, Kumar V, Steffen K. Single Coronary Artery Arising from the Right Sinus of Valsalva and the Role of Coronary Computed Tomography Angiography. S D Med. 2018;71:130-132. [PubMed] |
| 9. | Srinivasan KG, Gaikwad A, Kannan BR, Ritesh K, Ushanandini KP. Congenital coronary artery anomalies: diagnosis with 64 slice multidetector row computed tomography coronary angiography: a single-centre study. J Med Imaging Radiat Oncol. 2008;52:148-154. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 28] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 10. | Aldana-Sepulveda N, Restrepo CS, Kimura-Hayama E. Single coronary artery: spectrum of imaging findings with multidetector CT. J Cardiovasc Comput Tomogr. 2013;7:391-399. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 19] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 11. | Taylor AM, Thorne SA, Rubens MB, Jhooti P, Keegan J, Gatehouse PD, Wiesmann F, Grothues F, Somerville J, Pennell DJ. Coronary artery imaging in grown up congenital heart disease: complementary role of magnetic resonance and x-ray coronary angiography. Circulation. 2000;101:1670-1678. [PubMed] |
| 12. | Clemente A, Del Borrello M, Greco P, Mannella P, Di Gregorio F, Romano S, Morra A. Anomalous origin of the coronary arteries in children: diagnostic role of three-dimensional coronary MR angiography. Clin Imaging. 2010;34:337-343. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 15] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 13. | Lipton MJ, Barry WH, Obrez I, Silverman JF, Wexler L. Isolated single coronary artery: diagnosis, angiographic classification, and clinical significance. Radiology. 1979;130:39-47. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 314] [Cited by in RCA: 340] [Article Influence: 7.4] [Reference Citation Analysis (0)] |
| 14. | Shirani J, Roberts WC. Solitary coronary ostium in the aorta in the absence of other major congenital cardiovascular anomalies. J Am Coll Cardiol. 1993;21:137-143. [PubMed] |
| 15. | Wilson J, Reda H, Gurley JC. Anomalous right coronary artery originating from the left anterior descending artery: case report and review of the literature. Int J Cardiol. 2009;137:195-198. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 26] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 16. | Yurtdaş M, Gülen O. Anomalous origin of the right coronary artery from the left anterior descending artery: review of the literature. Cardiol J. 2012;19:122-129. [PubMed] |
| 17. | Angelini P, Velasco JA, Flamm S. Coronary anomalies: incidence, pathophysiology, and clinical relevance. Circulation. 2002;105:2449-2454. [PubMed] |
| 18. | Yang YY, Wu Q. Two-staged stent-assisted angioplasty treatment strategy for severe left main coronary distal bifurcation stenosis associated with the right coronary chronic total occlusion. Int J Clin Exp Med. 2014;7:4509-4514. [PubMed] |
| 19. | Chen SL, Zhang JJ, Han Y, Kan J, Chen L, Qiu C, Jiang T, Tao L, Zeng H, Li L, Xia Y, Gao C, Santoso T, Paiboon C, Wang Y, Kwan TW, Ye F, Tian N, Liu Z, Lin S, Lu C, Wen S, Hong L, Zhang Q, Sheiban I, Xu Y, Wang L, Rab TS, Li Z, Cheng G, Cui L, Leon MB, Stone GW. Double Kissing Crush Versus Provisional Stenting for Left Main Distal Bifurcation Lesions: DKCRUSH-V Randomized Trial. J Am Coll Cardiol. 2017;70:2605-2617. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 173] [Cited by in RCA: 241] [Article Influence: 30.1] [Reference Citation Analysis (0)] |
| 20. | Xu B, Redfors B, Yang Y, Qiao S, Wu Y, Chen J, Liu H, Chen J, Xu L, Zhao Y, Guan C, Gao R, Généreux P. Impact of Operator Experience and Volume on Outcomes After Left Main Coronary Artery Percutaneous Coronary Intervention. JACC Cardiovasc Interv. 2016;9:2086-2093. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 80] [Cited by in RCA: 97] [Article Influence: 10.8] [Reference Citation Analysis (0)] |
| 21. | Gershlick AH, Kandzari DE, Banning A, Taggart DP, Morice MC, Lembo NJ, Brown WM, Banning AP, Merkely B, Horkay F, van Boven AJ, Boonstra PW, Dressler O, Sabik JF, Serruys PW, Kappetein AP, Stone GW. Outcomes After Left Main Percutaneous Coronary Intervention Versus Coronary Artery Bypass Grafting According to Lesion Site: Results From the EXCEL Trial. JACC Cardiovasc Interv. 2018;11:1224-1233. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 35] [Article Influence: 5.8] [Reference Citation Analysis (0)] |
| 22. | Roffi M, Eberli FR, Wyttenbach R, Gallino A. Percutaneous coronary intervention of the left main trunk in congenitally anomalous single coronary artery. J Invasive Cardiol. 2001;13:808-809. [PubMed] |
| 23. | Stevens GR, Kini AS, Sharma SK. Intervention of stenosed right coronary artery and anomalous left main coronary artery: single main coronary trunk. J Invasive Cardiol. 2008;20:E71-E72. [PubMed] |
| 24. | Kawashima S, Shiraishi J, Hyogo M, Shima T, Sawada T, Kohno Y. Main trunk crossover stenting in a patient with left internal thoracic artery--protected single coronary artery. Cardiovasc Interv Ther. 2015;30:307-310. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.1] [Reference Citation Analysis (0)] |