Published online May 26, 2019. doi: 10.12998/wjcc.v7.i10.1234
Peer-review started: January 29, 2019
First decision: March 9, 2019
Revised: March 20, 2019
Accepted: March 26, 2019
Article in press: March 26, 2019
Published online: May 26, 2019
Processing time: 118 Days and 6.2 Hours
This case report discusses a modified approach for maxillary sinus augmentation, in which platelet-rich fibrin, endoscope, simultaneous implant placement, and sinus floor elevation (PESS) were applied for a maxillary sinus floor lift in a 40-year-old patient.
A 40-year-old woman suffered missing upper right first molar. Implant stability quotient and cone-beam computed tomography (CBCT) were used to evaluate the diagnosis. CBCT showed insufficient posterior maxillary bone with a mean residual alveolar bone height of only 3.5 mm. The patient underwent a minimally invasive sinus floor elevation endoscopically. The sinus membrane was elevated in two stages, and a 12-mm implant was placed immediately. At 3 mo postoperatively, the final impressions were accomplished, and a full-ceramic crown was fit-placed. A 6-mo follow-up demonstrated satisfactory aesthetic and functional results.
This is the first report to use an endoscope for maxillary sinus floor lifting in cases with severe and insufficient bone height. This case report demonstrates the advantages of the PESS technique, which include minimal invasiveness with high precision, being applicable in cases with a residual alveolar bone height < 4 mm with a promising result, and a shortened treatment period from 12 to 3 mo.
Core tip: The advantages of the modified approach for maxillary sinus augmentation, in which platelet-rich fibrin, endoscope, simultaneous implant placement, and sinus floor elevation (PESS) are combined, include: (1) Being applicable in cases with a residual alveolar bone height < 4 mm; (2) Shortened treatment period from 12 to 3 mo; and (3) Minimally invasive procedure with high precision.
- Citation: Mudalal M, Sun XL, Li X, Fang J, Qi ML, Wang J, Du LY, Zhou YM. Minimally invasive endoscopic maxillary sinus lifting and immediate implant placement: A case report. World J Clin Cases 2019; 7(10): 1234-1241
- URL: https://www.wjgnet.com/2307-8960/full/v7/i10/1234.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v7.i10.1234
Sufficient bone is an essential requirement in the field of implantology. The maxillary posterior area is a difficult location for implant placement in comparison with the other areas of the mouth[1-3]. The process of maxillary sinus enlargement due to bone loss after maxillary posterior tooth extraction is known as pneumatization of the maxillary sinus. Moreover, this area of maxilla tuberosity has the lowest bone density. Maxillary sinus augmentation is a surgical procedure to increase the vertical height of the alveolar bone followed by immediate or second stage dental implant placement[4]. There are many approaches and bio-materials used for this procedure. Tatum first developed the procedure in 1977, and Boyne and James were the first to publish research regarding this technique in 1980[5].
Traditionally, a residual alveolar bone width of 5 mm would require maxillary sinus augmentation. This was conducted using the lateral window technique that involved a grafting material and simultaneous or delayed implant placement[6]. However, the invasion of microorganisms in the oral cavity often causes infections, leading to a high failure rate[7]. In the early 1990s, an endoscopic technique to lift the sinus membrane was introduced. However, studies on endoscope-controlled sinus elevation showed that lower complication rates were only observed when a residual alveolar bone height in the posterior area of the maxilla was > 4 mm and the mean elevated height was < 4 mm[8,9].
The use of bio-materials as grafts in sinus floor elevation surgeries is gradually gaining grounds with increasing evidence showing that grafted sinus floor elevation showed better Osseo integration than graft-free sinus floor elevation[10]. Commonly used bio-materials included platelet-rich concentrates with anabolic factors that are derived from platelets as well as catabolic factors produced by leukocytes that promote tissue healing. Studies investigating growth factor concentration and release kinetics reported platelet-rich fibrin (PRF) to be superior over other platelet concentrates. PRF contains fibrin, an important adjunct molecule that serves as an ideal delivery vehicle in tissue reengineering, thus giving it a therapeutic advantage over traditional platelet-rich plasma[11,12]. Platelet-rich fibrin + Endoscope + Simultaneous implant placement + Sinus floor elevation (PESS) technique is a promising solution in cases with a < 4 mm residual alveolar crest height[13]. By combining endoscopic-guided trans-crestal sinus floor elevation with PRF and simultaneous dental implant installation, final prosthesis can be fitted within 3 mo, a much shorter period than 12 mo if we followed the traditional treatment.
This aim of this report is to illustrate a modified approach for the enhancement of the atrophic posterior maxilla with dental implants. It also aims to present the minimally invasive option available for the increment of the vertical alveolar bone height for oral rehabilitation surgeries. Moreover, the PESS technique is a promising solution in cases which have a < 4 mm residual alveolar crest height.
A 40-year-old female non-smoker, who was medically fit and had no bruxism, consulted the Department of Oral Implantology with a complaint of a missing upper molar. The tooth was extracted several years ago due to a periodontal problem.
Missing upper molar with adequate dimensions and keratinized gingiva in #16 area were found for further prosthetic restoration.
She had no significant medical history.
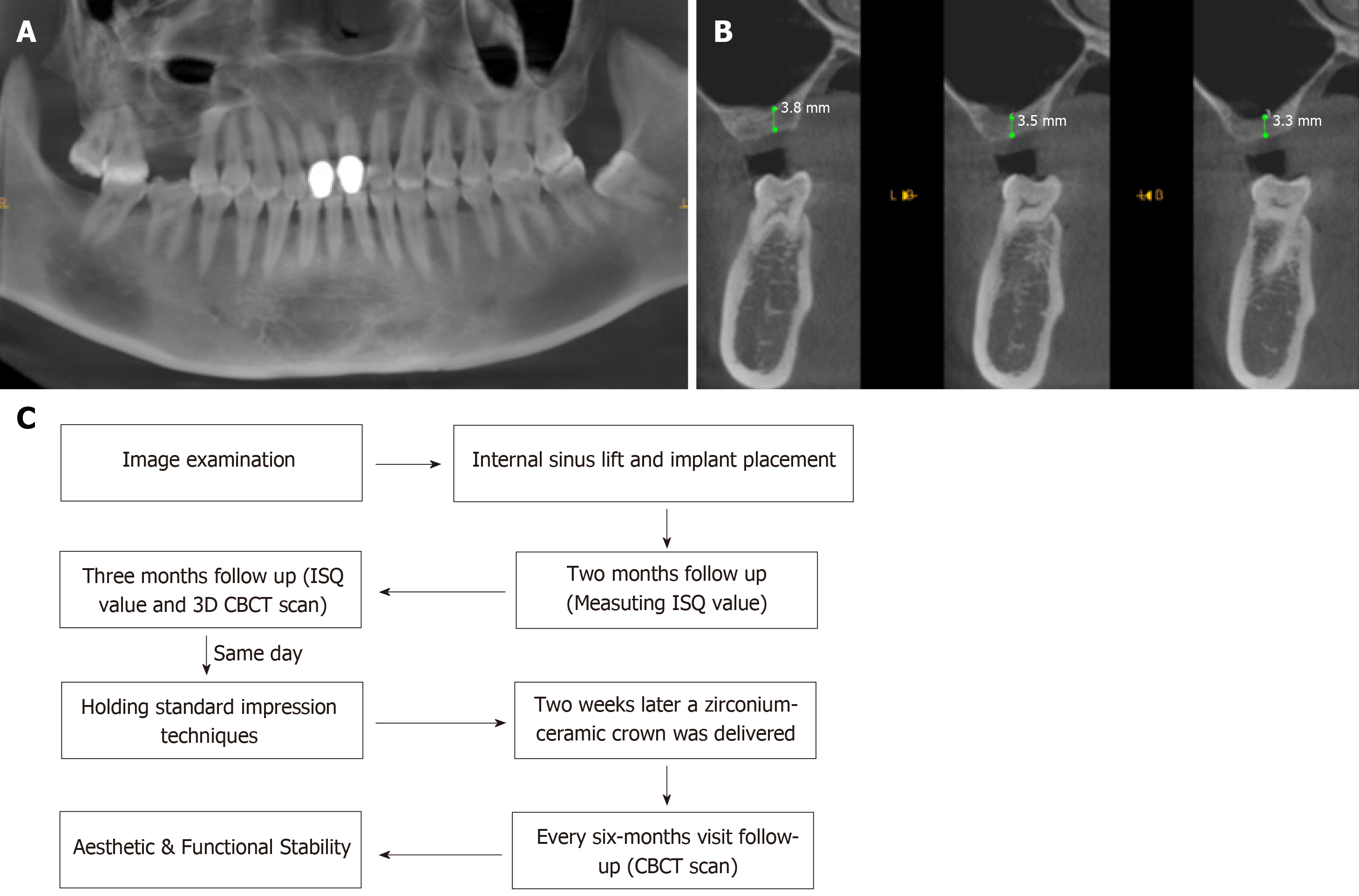
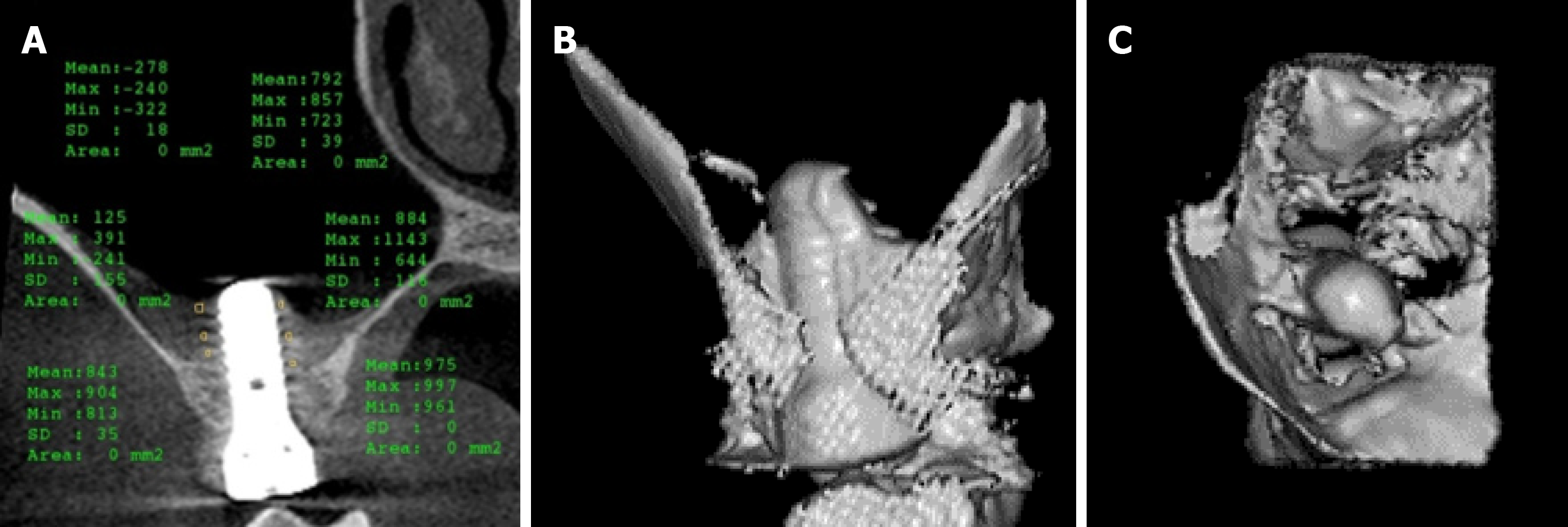
Cone-beam computed tomography (CBCT) showed a severe vertical bone loss with a mean residual bone height (RBH) of 3.53 mm (Figure 1A and B).
The final diagnosis was severe vertical bone loss with an RBH less than 4 mm.
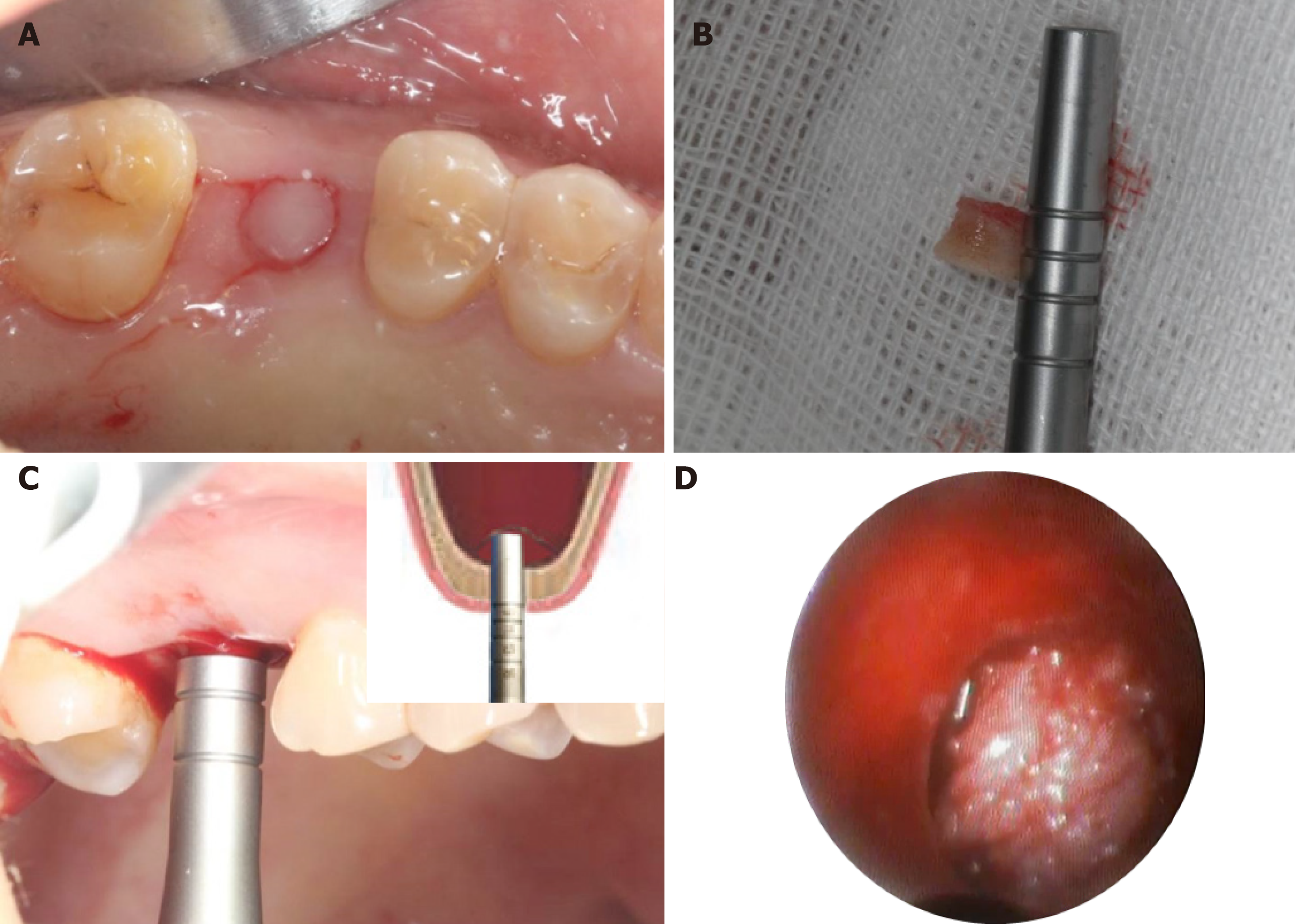
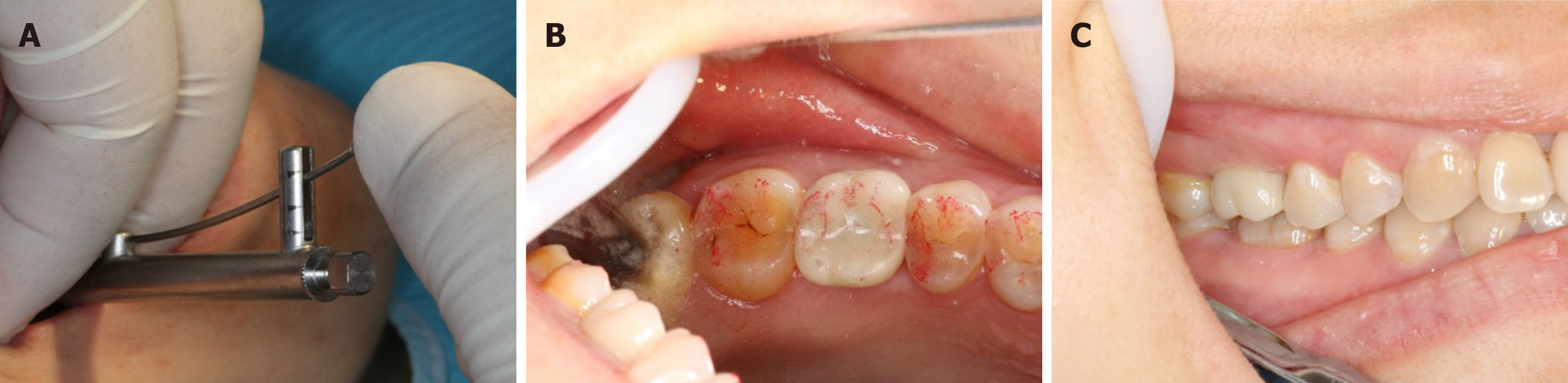
Before the surgery, the patient signed an informed consent form in accordance with the bio-ethical guidelines of the hospital. The treatment plan developed based on the patient’s condition was discussed with the patient and is shown in Figure 1C. The procedure began by patient rinsing her mouth with 0.12% chlorhexidine mouthwash 3 min per time, for 3 times. Articaine with adrenaline 1:100000 was used as local anesthesia. Instead of vertical release incision on the flap and mucoperiosteum, a punch incision was established to gain access to the bone crest using a motor-driven circular tissue bur (29630, Nobel Biocare, Sweden) with the same diameter of the selected implant (Figure 2A and B).
A precise preparation for an implant bed was established with various osteotomes. The pilot drill was used at a speed of 800 rpm in combination with the bur’s width and depth, leaving approximately 1 mm gap from the maxillary sinus floor boundary. This step was done with special care in order not to perforate the Schneiderian membrane, a thin bilaminar mucoperiosteal membrane that lines the maxillary sinuses. After that, the cortical bone of the sinus floor was up-fractured carefully with a rounded and blunted 4.3 mm osteotome (KOHLER, Germany) to elevate the maxillary sinus membrane to a height of 7 mm (Figure 2C). During the elevation procedure, an endoscope (POLYDIAGNOST, Germany) was used to monitor the integrity of the sinus floor membrane (Figure 2D).
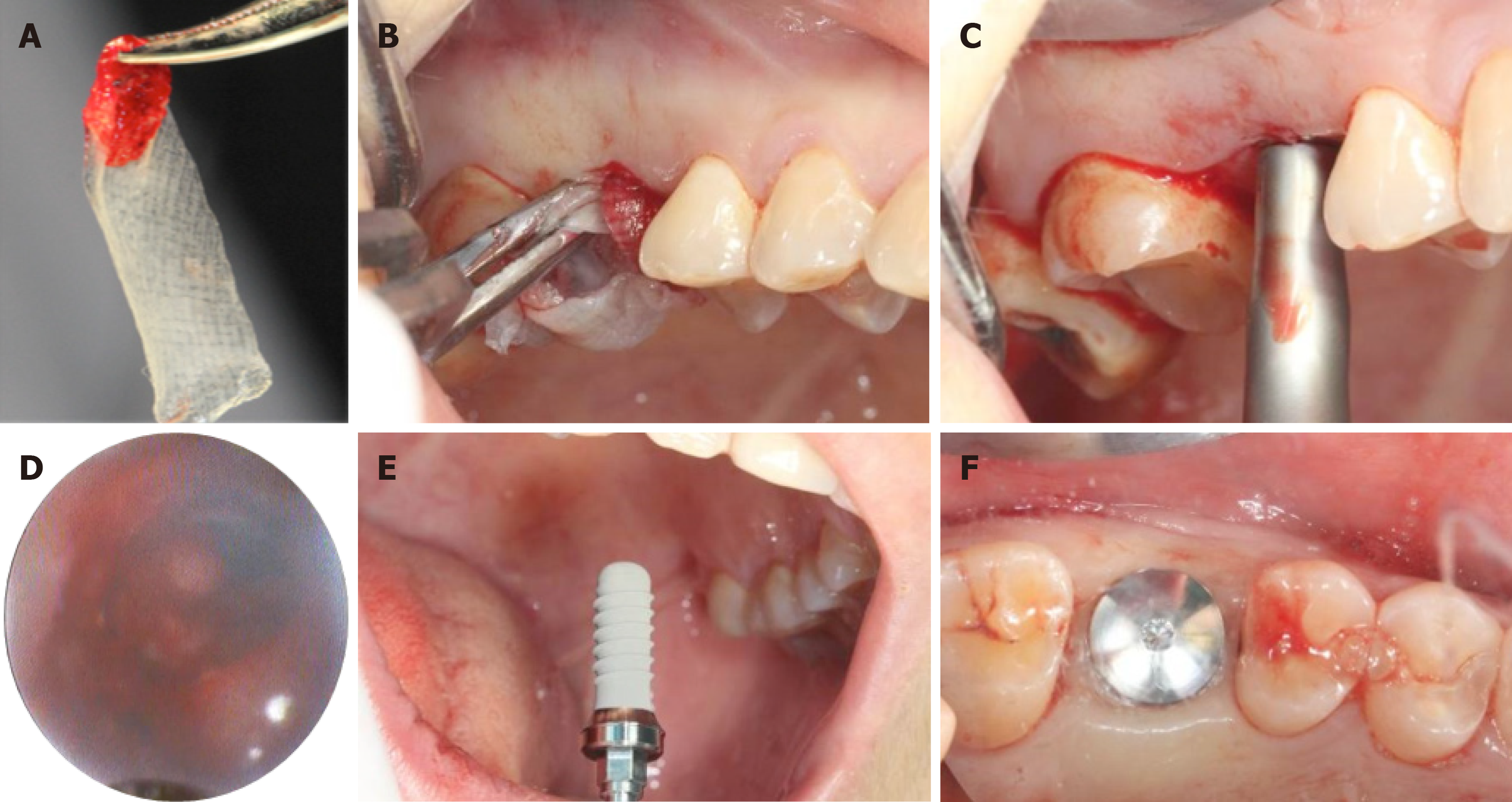
Using the standard protocol, a total of three PRF were established (three whole blood samples were taken in three glass-coated 10 mL plastic tubes without any anticoagulant and immediately centrifuged at 3000 rpm for 10 min). Following that, PRF clots were pressed into the membranes with a sterile dry gauze to fill up the elevated sinus (Figure 3A and B). The maxillary sinus membrane was elevated another time to obtain a total height of 12 mm (Figure 3C). Real-time observation was made endoscopically on the movements of PRF-filled membranes and the maxillary sinus floor membrane during the nasal inspiration and exhalation exercises. It revealed an intact maxillary sinus membrane, in which the entire maxillary sinus and PRF membranes moved together (Figure 3D). Implant installation was implemented properly (⌀ 4.8 mm × 12 mm, Straumann, Switzerland) with a torque of 30 N/cm (Figure 3E), followed by healing cap placement (Figure 3F). All procedures were performed under an assessment with 0.9% saline irrigation and suctioning.
Postoperatively, the patient was prescribed with a 3-d course of antibiotics (oral metronidazole 300 mg TID and amoxicillin 500 mg TID) and 0.12% chlorhexidine mouthwash twice a day for 7 d.
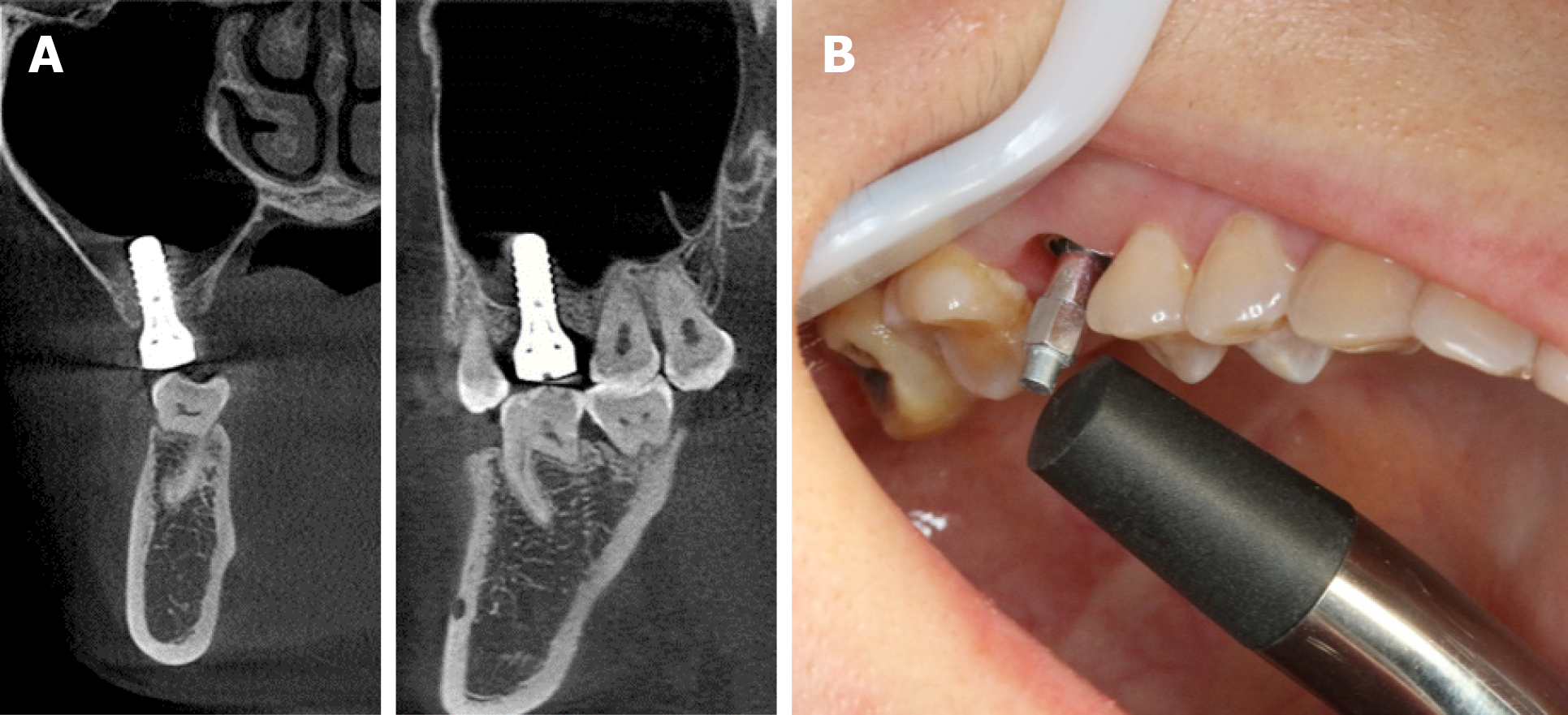
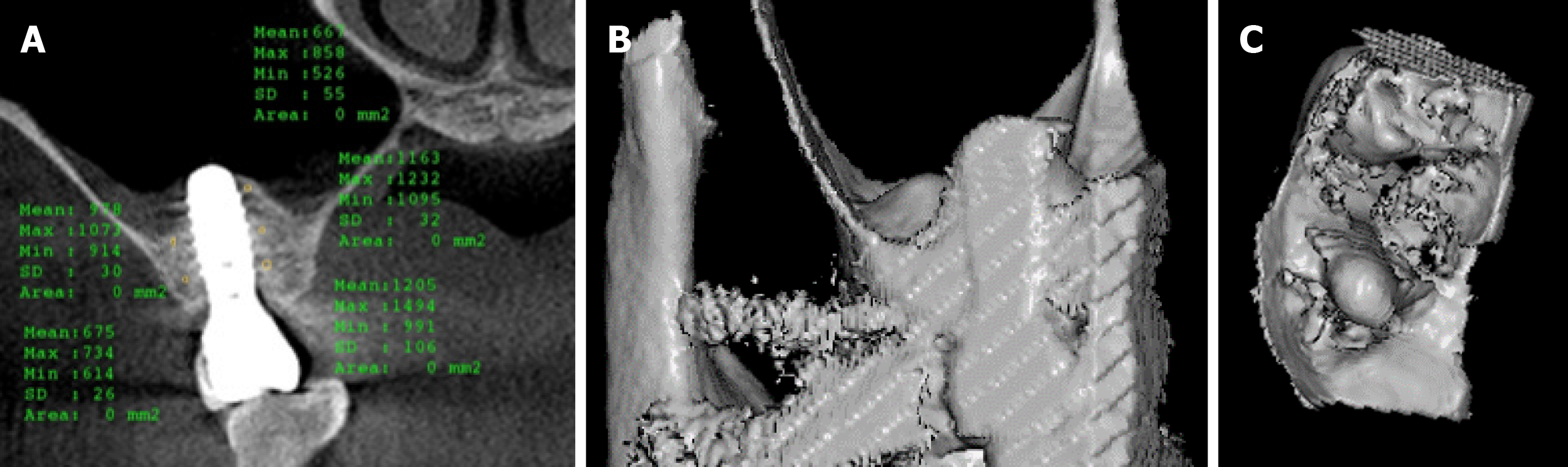
After 2 and 3 mo of the implant placement, CBCT and implant stability quotient (ISQ) measurements were performed using the resonance frequency analysis. The ISQ values were obtained in five directions (mesial, distal, lingual, buccal, and occlusal) of the implant three times. CBCT at 2 mo post-surgery revealed a good level of healing. Results also demonstrated good bone-implant osseointegration during the first 8 wk (Figure 4).
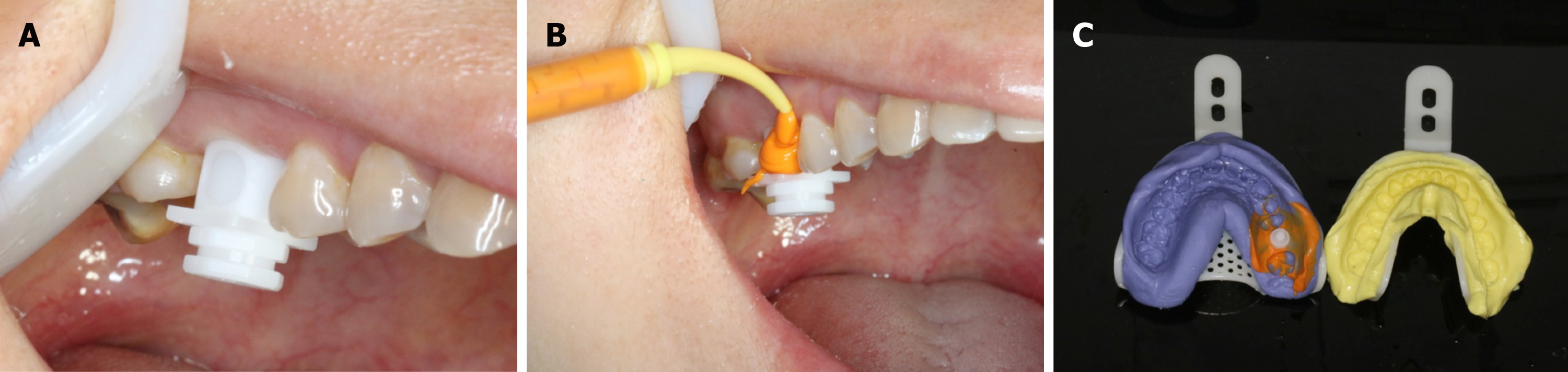
At 3-mo follow-up, the mean ISQ value increased to 67.4 (Figure 5). An impression for the upper arch and a wax-bite registration were made according to standard procedures for implant-level impression techniques (Figure 6). The prosthetic restoration was able to address the main concern of providing proper occlusion, margins, and embrasures during the fabrication process. Two weeks later, a zirconium-ceramic crown was applied, and fine tuning was conducted at the same visit (Figure 7). The final results were highly satisfactory. Six-month follow-up showed that the bone height remained stable. The mean ISQ value was 71.0 (Figure 8).
In patients with insufficient maxilla, it is important to innovate various methods for maxillary sinus floor elevations in order to achieve better clinical results. Moreover, it is vital to compensate any vertical alveolar bone loss to support proper implant placement and to ensure its viability[14,15]. Our case report illustrates a modified approach in a 40-year-old woman in need of a maxillary sinus augmentation.
In order to restore vertical alveolar bone loss, various surgical modalities have been proposed for the insertion of dental implants in the maxillary posterior part, showing a high implant survival rate with a low failure incidence. However, the indication for the any mentioned surgical techniques is not strictly equivalent and the treatment choice should be based on a careful evaluation of the individual case. The residual alveolar bone height and the ability to establish implant stability are fundamental in deciding which augmentation modality should be used to obtain a sufficient bone height for dental implant installation.
Traditionally, lateral window techniques were used to augment the maxillary sinus in cases with an alveolar height < 5 mm. However, this approach often results in postoperative complications such as discomfort, swelling, bleeding, infection, exposure of the covering membrane, and occasionally nasal bleeding[16,17]. As a result, minimally invasive surgical procedures were devised to shorten the treatment period and to optimize the maxillary posterior edentulous area for implantation. In this paper, a modified technique is reported for maxillary sinus floor elevation, achieving a maximum height of 12 mm. The use of endoscope provided a good visualization of the surgical site, thus improving the outcomes of the procedure.
The usage of PRF delivered multiple advantages at different phases. At the initial stage, it was a good cushioning material because of its flexibility. This could decrease the risk of perforation of the Schneider membrane. Due to the blind nature of this procedure, in the unfortunate event that membrane perforation was observed, PRF membrane would also act as an ideal sealant to patch the perforated membrane. In our case, no perforation was monitored during the procedure. Furthermore, PRF is a perfect biomedical additive and could reduce the healing period by half[18].
There were no postoperative complications. Minimally invasive endoscopic techniques are often associated with a high success rate, as shown in our case. CBCT indicated an increase in the bone formation around the implant. The calculated ISQ values represented a significant increase of implant-bone osseointegration. Clinically successful (aesthetically and functionally) crown delivery within 14 wk of surgery represented a great satisfactory result for both the patient and the clinician.
Our case report demonstrated that the PESS technique had promising short and long-term clinical results. It can be used in patients with a residual alveolar bone height < 4 mm. Furthermore, endoscopic-guided trans-crestal sinus floor elevation combined with PRF and simultaneous dental implant installation could be followed by final prosthesis within 3 mo. This represents a perfect solution for similar situations in which traditional treatment would require 12 mo of treatment. In conclusion, minimally invasive endoscopic maxillary sinus lift with immediate implant installation is a reliable approach in oral rehabilitation of atrophic posterior maxilla with an RBH < 4 mm. This case illustrates the advantages of minimally invasive surgical procedures in terms of reduced postoperative discomfort, swelling, and pain as compared to lateral approach techniques, and enhanced healing by adding PRF. This technique can be further expanded in view of the successful outcomes. To the end, endoscopic-guided trans-crestal sinus floor elevation combined with PRF and simultaneous dental implant installation, followed by final prosthesis within 3 mo, is a perfect solution for such a situation which needs 12 mo of treatment if we follow the traditional ways.
Manuscript source: Unsolicited manuscript
Specialty type: Medicine, research and experimental
Country of origin: China
Peer-review report classification
Grade A (Excellent): A
Grade B (Very good): 0
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Mattos B, Munhoz EA S-Editor: Ji FF L-Editor: Wang TQ E-Editor: Wu YXJ
| 1. | Agamy EM, Niedermeier W. Indirect sinus floor elevation for osseointegrated prostheses. A 10-year prospective study. J Oral Implantol. 2010;36:113-121. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 7] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 2. | Esposito M, Grusovin MG, Rees J, Karasoulos D, Felice P, Alissa R, Worthington H, Coulthard P. Effectiveness of sinus lift procedures for dental implant rehabilitation: a Cochrane systematic review. Eur J Oral Implantol. 2010;3:7-26. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 31] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 3. | Lundgren S, Cricchio G, Hallman M, Jungner M, Rasmusson L, Sennerby L. Sinus floor elevation procedures to enable implant placement and integration: techniques, biological aspects and clinical outcomes. Periodontol 2000. 2017;73:103-120. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 67] [Cited by in RCA: 110] [Article Influence: 15.7] [Reference Citation Analysis (0)] |
| 4. | Mohan N, Wolf J, Dym H. Maxillary sinus augmentation. Dent Clin North Am. 2015;59:375-388. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 37] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 5. | Boyne PJ, James RA. Grafting of the maxillary sinus floor with autogenous marrow and bone. J Oral Surg. 1980;38:613-616. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 6. | Fugazzotto PA. Augmentation of the posterior maxilla: a proposed hierarchy of treatment selection. J Periodontol. 2003;74:1682-1691. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 42] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 7. | Petersen PE, Bourgeois D, Bratthall D, Ogawa H. Oral health information systems--towards measuring progress in oral health promotion and disease prevention. Bull World Health Organ. 2005;83:686-693. [PubMed] |
| 8. | Wiltfang J, Schultze-Mosgau S, Merten HA, Kessler P, Ludwig A, Engelke W. Endoscopic and ultrasonographic evaluation of the maxillary sinus after combined sinus floor augmentation and implant insertion. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2000;89:288-291. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 45] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 9. | Engelke W, Deckwer I. Endoscopically controlled sinus floor augmentation. A preliminary report. Clin Oral Implants Res. 1997;8:527-531. [PubMed] |
| 10. | Nedir R, Nurdin N, Khoury P, Perneger T, Hage ME, Bernard JP, Bischof M. Osteotome sinus floor elevation with and without grafting material in the severely atrophic maxilla. A 1-year prospective randomized controlled study. Clin Oral Implants Res. 2013;24:1257-1264. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 31] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 11. | Castillo TN, Pouliot MA, Kim HJ, Dragoo JL. Comparison of growth factor and platelet concentration from commercial platelet-rich plasma separation systems. Am J Sports Med. 2011;39:266-271. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 343] [Cited by in RCA: 330] [Article Influence: 23.6] [Reference Citation Analysis (0)] |
| 12. | Mudalal M, Zhou YM. Biological Additives and Platelet Concentrates for Tissue Engineering on Regenerative Dentistry Basic Science and Concise Review. Asian J Pharm. 2017;11:255-263. |
| 13. | Toscano NJ, Holtzclaw D, Rosen PS. The effect of piezoelectric use on open sinus lift perforation: a retrospective evaluation of 56 consecutively treated cases from private practices. J Periodontol. 2010;81:167-171. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 56] [Cited by in RCA: 42] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 14. | Starch-Jensen T, Aludden H, Hallman M, Dahlin C, Christensen AE, Mordenfeld A. A systematic review and meta-analysis of long-term studies (five or more years) assessing maxillary sinus floor augmentation. Int J Oral Maxillofac Surg. 2018;47:103-116. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 70] [Cited by in RCA: 105] [Article Influence: 13.1] [Reference Citation Analysis (0)] |
| 15. | Ting M, Rice JG, Braid SM, Lee CYS, Suzuki JB. Maxillary Sinus Augmentation for Dental Implant Rehabilitation of the Edentulous Ridge: A Comprehensive Overview of Systematic Reviews. Implant Dent. 2017;26:438-464. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 23] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 16. | Duan DH, Fu JH, Qi W, Du Y, Pan J, Wang HL. Graft-Free Maxillary Sinus Floor Elevation: A Systematic Review and Meta-Analysis. J Periodontol. 2017;88:550-564. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 39] [Cited by in RCA: 39] [Article Influence: 4.9] [Reference Citation Analysis (0)] |
| 17. | Silva LD, de Lima VN, Faverani LP, de Mendonça MR, Okamoto R, Pellizzer EP. Maxillary sinus lift surgery-with or without graft material? A systematic review. Int J Oral Maxillofac Surg. 2016;45:1570-1576. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 65] [Cited by in RCA: 56] [Article Influence: 6.2] [Reference Citation Analysis (0)] |
| 18. | Choukroun J, Diss A, Simonpieri A, Girard MO, Schoeffler C, Dohan SL, Dohan AJ, Mouhyi J, Dohan DM. Platelet-rich fibrin (PRF): a second-generation platelet concentrate. Part V: histologic evaluations of PRF effects on bone allograft maturation in sinus lift. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101:299-303. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 355] [Cited by in RCA: 410] [Article Influence: 21.6] [Reference Citation Analysis (0)] |