Published online Jun 6, 2021. doi: 10.12998/wjcc.v9.i16.4081
Peer-review started: January 31, 2021
First decision: February 22, 2021
Revised: March 10, 2021
Accepted: March 24, 2021
Article in press: March 24, 2021
Published online: June 6, 2021
Processing time: 103 Days and 2.6 Hours
Glycogen storage disease (GSD) is an autosomal recessive inborn metabolic disorder. Patients with GSD are prone to hypoglycaemia, hyperlactacidemia and bleeding. GSD type 1b (GSD-1b) patients specifically can develop neutropenia, recurrent bacterial infection and inflammatory bowel disease (IBD). Documen
A 20-year-old Chinese lady confirmed by genetic testing to have GSD-1b was initially managed with uncooked cornstarch and granulocyte-colony stimulating factor. With recurrent abdominal symptoms, her condition was treated as clinical “Crohn’s disease” with mesalazine, prednisolone and azathioprine conservatively. Colonoscopy showed a tight stricture at the hepatic flexure. Subsequent computerized tomographic colonography revealed a phlegmon at the ileocaecal region with a suspected coloduodenal fistula. Eventually an exploratory laparotomy was performed and severe colitis at the ascending colon with coloduodenal fistula was confirmed. Right hemicolectomy with primary anastomosis and repair of the duodenum were performed. Surgical management of complications from GSD-1b associated IBD-like colitis has rarely been described. First-line treatment would usually be conservative. Surgical intervention like hemicolectomy is mainly reserved for refractory cases.
Surgical management of coloduodenal fistula in GSD-1b patients is a feasible and safe option when failed conservative management.
Core Tip: Inflammatory bowel disease-like colitis is associated with a few rare genetic disorders or certain drug use. First-line treatment is usually conservative with nutritional support or steroids. Granulocyte-colony stimulating factor or immunosuppressant may be beneficial. Surgical intervention like hemicolectomy is mainly reserved for refractory cases with intestinal obstruction resistant to medical treatment.
- Citation: Lui FCW, Lo OSH. Rare complication of inflammatory bowel disease-like colitis from glycogen storage disease type 1b and its surgical management: A case report . World J Clin Cases 2021; 9(16): 4081-4089
- URL: https://www.wjgnet.com/2307-8960/full/v9/i16/4081.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v9.i16.4081
Glycogen storage disease (GSD) is an autosomal recessive inborn metabolic disorder featured by the defects in the glucose-6-phosphatase (G6Pase) complex. Due to the deficiency of G6Pase activity in the liver, kidneys and intestine, patients are prone to over accumulation of glycogen in these organs and corresponding hypoglycaemia. Secondary metabolic and biochemical changes include hyperlactacidemia, hyperuricaemia and hyperlipidaemia. Hepatomegaly, short stature, truncal obesity, and bleeding tendency due to platelet dysfunction can also occur. Classical clinical presentations specific to GSD type 1b (GSD-1b) patients include neutropenia, neutrophil dysfunction, recurrent bacterial infection and inflammatory bowel disease (IBD)[1,2]. Documentation of the long-term outcomes of surgical management of GSD-1b, especially in Asian patients, has been scarce. Large studies on the topic are also lacking. We herein describe a case of GSD-1b complicated by IBD-like colitis and coloduodenal fistula. The patient was managed successfully with surgical inter
The patient presented to our clinic with recurrent abdominal pain and subtle bowel obstruction.
She presented to our clinic with recurrent abdominal pain, vomiting and passage of loose stool for two years.
The patient, born in mainland China, started developing hepatosplenomegaly, hypoglycaemia and seizure attacks at one month of age. The diagnosis of GSD was suspected in China as blood tests showed lactic acidosis and hyperuricaemia. Her hypoglycemic symptom was managed with frequent meals and dietary modification with uncooked cornstarch (UCCH). During childhood, she developed growth retardation, recurrent abdominal pain and neutropenia [absolute neutrophil count (ANC): 0.95 × 109/L]. Details of her treatment in early childhood in China was lacking as the patient was grown up in rural areas. No definitive workup or diagnosis for IBD was documented. At age 11, she was confirmed by genetic testing to have GSD-1b and given granulocyte-colony stimulating factor (G-CSF) injections for neutropenia.
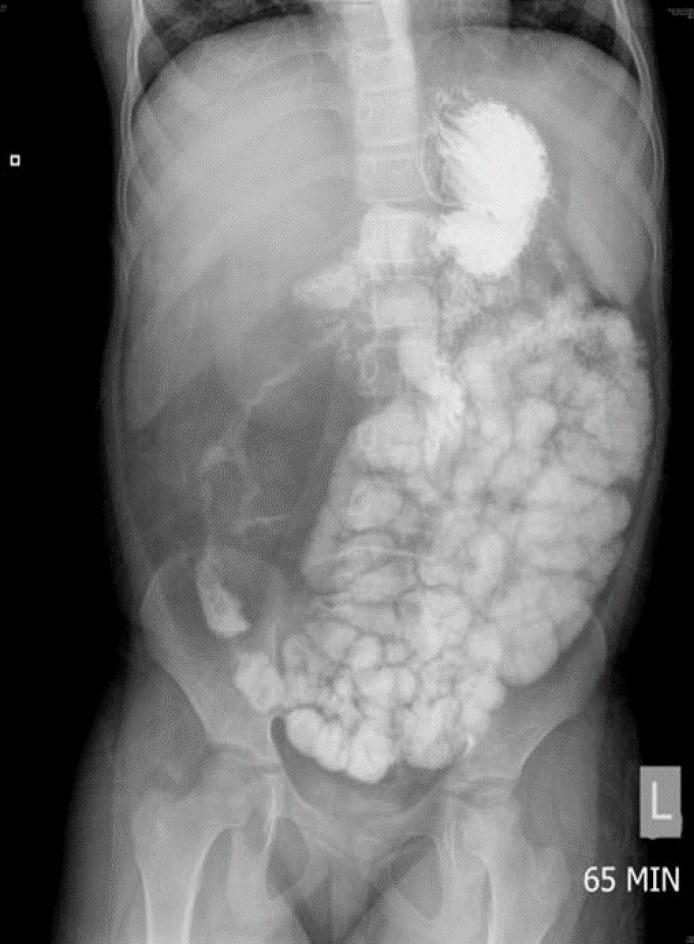
She was firstly seen in Hong Kong at age 12 with chronic diarrhea and associated with perianal fissure. Colonoscopy revealed an ulcer near the hepatic flexure and the histology did not show granulomatous changes. Gastrografin follow-through study did not suggest any small bowel pathology but luminal narrowing in the ascending colon (Figure 1). Contrast computerized tomography (CT) of the abdomen and pelvis noted severe inflammatory changes at the ascending colon and terminal ileum, with enlarged pericolonic lymph nodes. Therefore, her condition was treated clinically as Crohn’s disease with mesalazine, prednisolone and azathioprine. The condition gradually improved and she was followed up at the paediatric metabolic clinic. G-CSF injections were regularly given for her neutropenia. With good compliance with her UCCH diet, she managed to wean off her azathioprine and oral steroid six months later. Follow-up colonoscopy did not show any mucosal lesion while upper endoscopy showed duodenitis only.
There was no family history of glycogen storage disease or IBD.
Physical examination showed soft abdomen but not distended. She had hepatosplenomegaly and hyperactive bowel sound. Per rectal examination showed no stigmata of IBD.
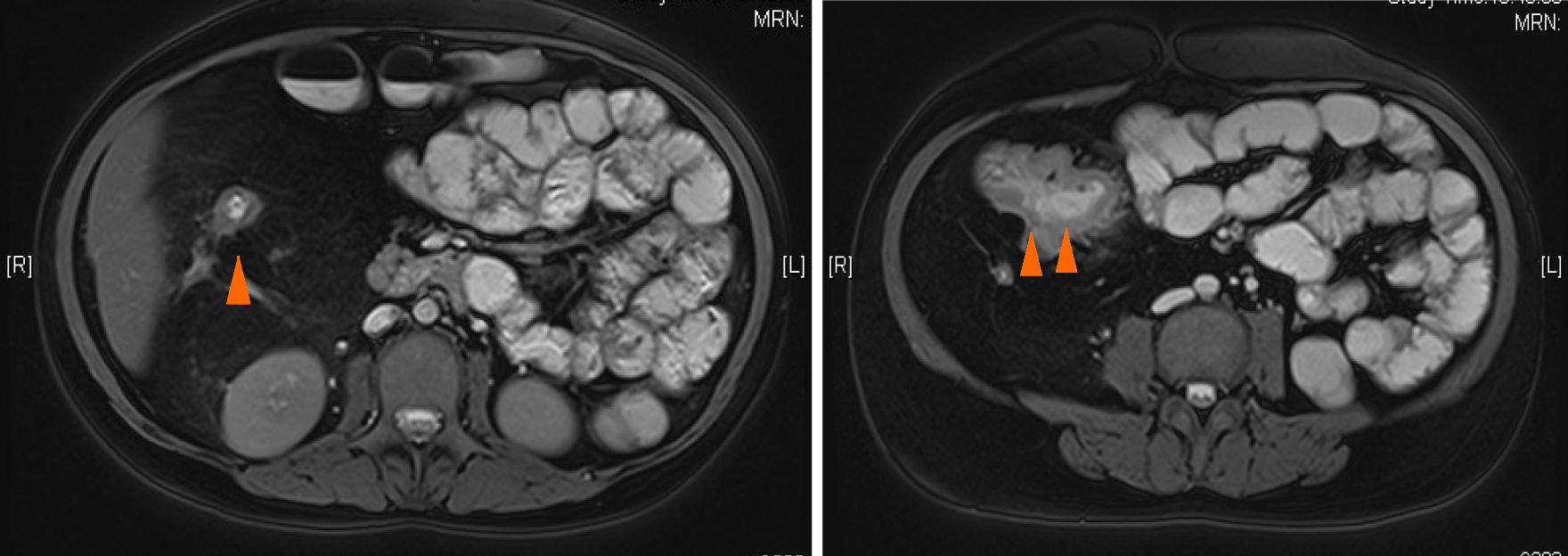
She had neutropenia (ANC: 1.43 × 109/L) and hyperuricaemia (465 μmol/L). Stool calprotectin was found to be significantly elevated (977 μg/g). Magnetic resonance enteroclysis revealed abnormal bowel wall thickening and stricture with hyper-enhancement at the ileocaecal region (Figure 2).
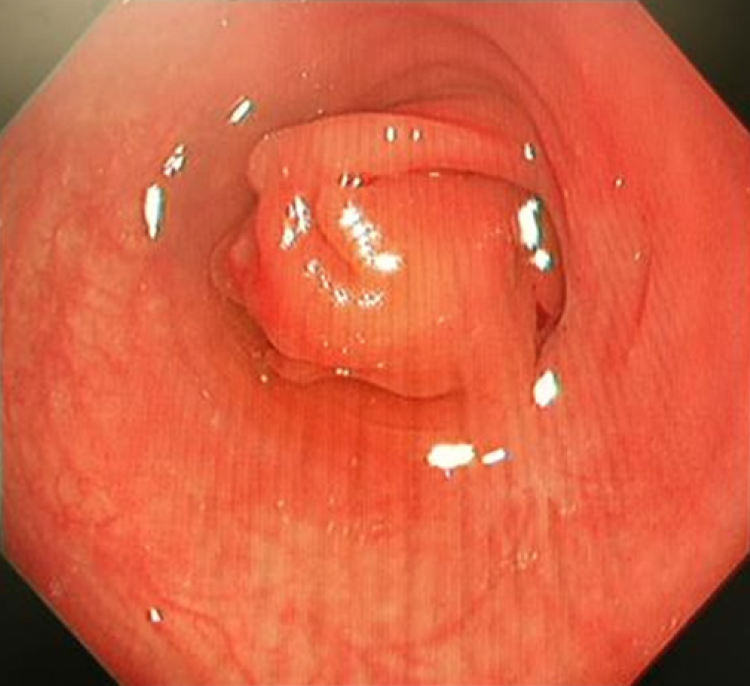
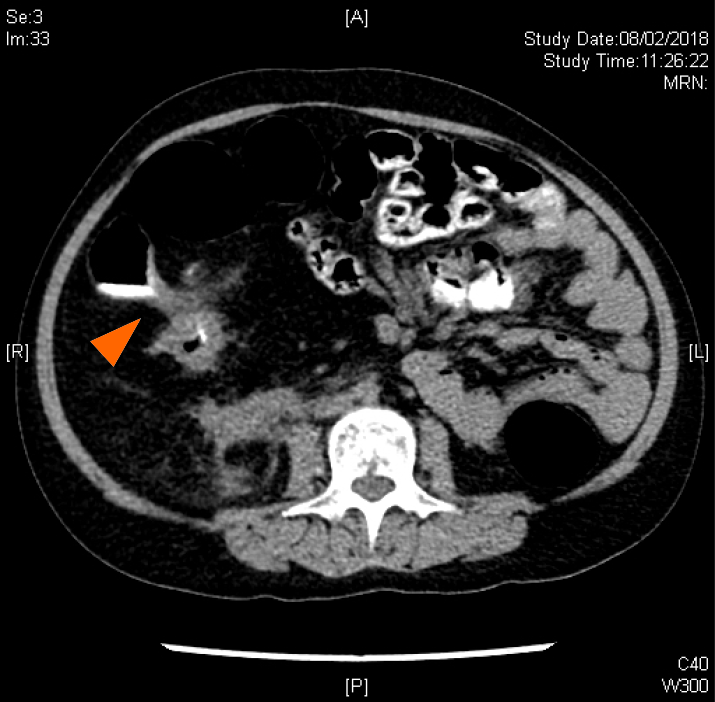
Colonoscopy showed a colonic stricture beyond the hepatic flexure (Figure 3). Biopsy from the stricture revealed mild colitis without cryptitis, granuloma or viral inclusion. Upper endoscopy demonstrated chronic gastritis and duodenitis. CT colonography demonstrated a suspected fistula tract between the caecum and the second and third parts of the duodenum (Figure 4).
G-CSF, iron supplement and allopurinol were recommended for the flare-up of colitis. Compliance with UCCH diet was emphasized. However, the bowel symptom was partially responsive to conservative treatment and the patient was repeatedly admitted for intestinal obstruction in the subsequent 6 mo. At the end, she agreed for exploratory laparotomy because of progressive abdominal pain and vomiting.
GSD-1b disease.
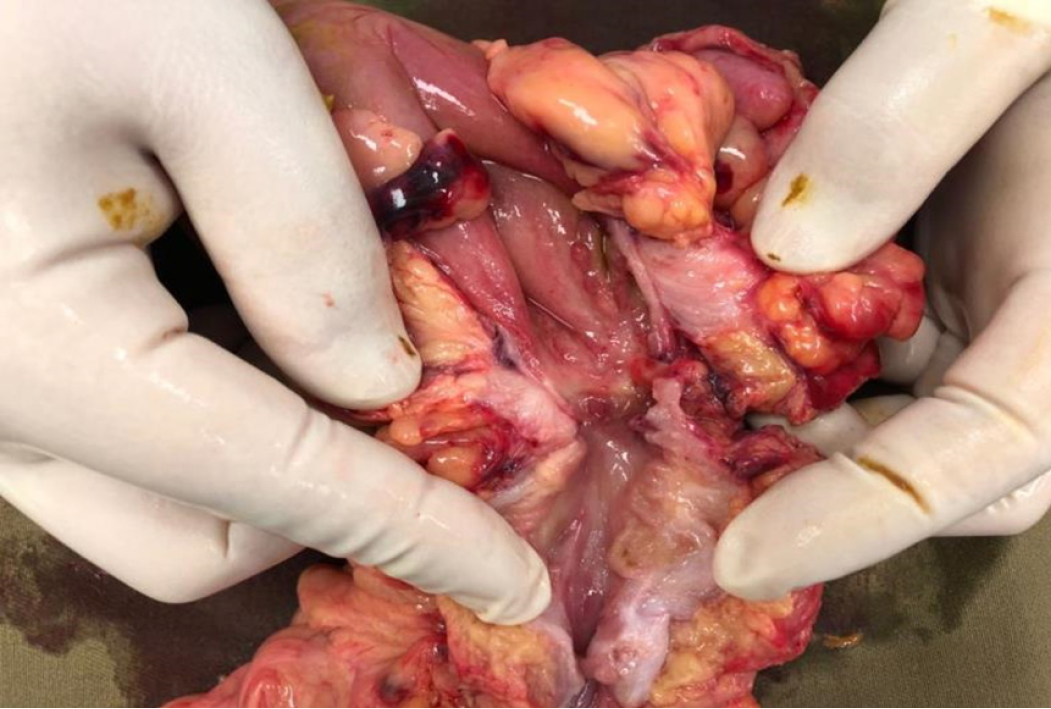
Exploratory laparotomy was performed via a midline incision. A phlegmon was noticed at the ileocaecal region with grossly dilated small bowel adhering to the right colon (Figure 5). The caecum was found lying in the right upper quadrant and a fistulation was seen over the third part of the duodenum. Right hemicolectomy was performed with a side-to-side hand-sewn ileocolic anastomosis. After kocherization of the duodenum, the fibrotic edge of the duodenal fistula tract was trimmed and then primarily closed with 4/0 monofilament absorbable suture in a two-layer continuous manner.
Postoperatively, total parenteral nutrition was continued, and blood lactate level was closely monitored to avoid hypoglycemia and lactic acidosis respectively. Oral diet was started after a normal Gastrografin meal study one week after the operation. The patient was discharged uneventfully three weeks later. Pathology showed transmural fibrosis with colonic stricture and no malignancy or granuloma. During her follow-up, G-CSF was resumed for her neutropenia and she would be seen at an adult metabolic clinic with expertise in managing patients with inborn errors of metabolism.
The medical and surgical management of our patient with a long history of GSD-1b complicated by colitis and resultant coloduodenal fistula was delineated in this review. This is one of the first reported cases in the Asian population with similar pathology.
Classical GSD-1b patients presented at a median age of 4 month, with features including protruding abdomen (83%), growth retardation (25%) and recurrent infection (41%)[3]. Our patient was diagnosed within the first year of life and developed recurrent abdominal pain in primary school years. According to the literature, the average age at first diagnosis of IBD in GSD-1b patients was 8.7 years[2]. As many as 90% of GSD-1b patients with IBD had abdominal pain or intestinal obstructive symptoms, 60% had ileal or colonic stricture, and 50% required surgical resection or endoscopic dilatation.
Although there was no definite pathological evidence of Crohn’s disease such as granuloma formation or crypt abscess, clinically and biochemically our patient exhibited some typical features of Crohn’s disease including relapsing abdominal pain, fever, perianal disease and raised stool calprotectin. A possible differential diagnosis accounting for her symptoms and pathological findings would be chronic IBD-like colitis. IBD-like colitis has been known to be associated with GSD-1b and well described in the literature[4]. It can be associated with features like neutropenia and circumferential ulcers on colonoscopy. The mean age at onset of bowel symptoms was reported to be 12.3 years. Histopathology usually shows nonspecific inflammation without granulomatous lesions, as in the case of our patient. Neutropenia associated with intestinal mucosal inflammation may contribute to the pathogenesis. Treatment, hence, is usually by high-dose G-CSF and sulfasalazine[5,6]. Volz et al[7] gave high-dose G-CSF (30 million IU/d) for five weeks to a young patient with IBD-like colitis and GSD-1b. The neutropenia was successfully corrected, and the C-reactive protein and calprotectin levels were normalized. Repeated colonoscopy, however, revealed progressive stricture and scarring stenosis and the patient eventually required surgical resection. Saltik-Temizel et al[8] reported the case of a 3-year-old girl with GSD-1b and IBD-like colitis successfully treated with G-CSF. It has been speculated that raised platelet count is an early marker of IBD-like colitis, but the exact pathogenesis is unclear. The relationship between platelet count and colitis remains uncertain. In our patient, platelet count was not persistently raised (i.e., 117-538 × 109/L).
Xiao[9] recently reported that two patients with GSD-1b and IBD-like colitis were treated conservatively with G-CSF, partial enteral nutrition and mesalazine and no surgical intervention was required. In a retrospective study[10], nine French patients with mild to severe digestive complications from GSD-1b and IBD-associated colitis were treated with a variable combination of G-CSF, cotrimoxazole, corticosteroids, 5-aminosalicylic acid and infliximab without surgical intervention. The authors suggested that the addition of a polymeric formula enriched in anti-inflammatory cytokine transforming growth factor-beta (Modulen IBD®) might have positive effects on metabolic balance and help to improve digestive symptoms.
Reports of the surgical management of patients with GSD-1b complicated by colitis and coloduodenal fistula are rare and mostly case reports[4,11]. For our patient, we performed primary excision of the coloduodenal fistula followed by primary repair of the duodenal defect. Delayed surgical exploration after repeated colitis episodes and adhesion formation had resulted in the distorted anatomy adjacent to her coloduo
As our patient was at risk of hypoglycemia, particular attention was paid to maximize the perioperative glycemic control, including the use of intravenous dextrose and frequent hemastix monitoring. Optimizing glycemic control not only promotes optimal tissue healing but also can minimize wound complications and infection risks.
Our patient was given G-CSF perioperatively and her neutropenia was fully corrected prior to her emergency operation. She required postoperative blood transfusion but experienced no other major morbidities or surgical site infections. In a report, 98% of GSD-1b patients had neutropenia at some time[4]. Filgrastim, an unglycosylated recombinant G-CSF, has been studied and proved to be efficacious in enhancing neutrophil production and promoting regression of IBD[5,14]. High vigilance and thorough precaution are important in perioperative planning for patients with neutropenia[15]. The decision for the best timing of surgery for our patient therefore necessitated a fine balance between the optimization of her infectious risks and the urgency of her clinical symptoms and rate of disease progression.
Apart from GSD-1b, little evidence or description about the surgical management of IBD-like colitis associated with other etiologies is available in the literature. Common causes of IBD-like colitis are listed in Table 1 and a summary of the studies reviewed is delineated in Table 2 below. Dubeau et al[16] described the etiology of drug-induced IBD-like colitis and medications for the condition but no details of its surgical management. Specifically, IBD-like colitis was also found to be associated with mycophenolic acid (MPA) use in renal transplant recipients[17]. In patients with MPA-related colitis who underwent colonoscopy, the most frequent histologic pattern was non-specific colitis (31.3%), followed by IBD-like colitis (25%) and then other pathologies. Clinically, MPA-related diarrhea resolved after MPA switch, reduction, or discontinuation without the need for operation. Bolton et al[18] recently described a patient with IBD-like colitis secondary to a homozygous variant/mutation in the G6Pase G6PC3 gene. The colitis was refractory to medical therapy. The patient underwent allogenic stem cell transplantation and saw significant improvement in obstructive symptoms and biochemical parameters. Norsa et al[19] described a rare cause of IBD-like colitis, which is congenital chloride diarrhoea, a rare autosomal recessive disease secondary to SLC26A3 gene mutation. Among the twelve patients with IBD or IBD-like colitis, two were treated with 5-aminosalicylate acid, three with immunosuppressants and six with biologics.
| Drug-induced[16,17] |
| Mycophenolic acid |
| Isotretinoin |
| Antibiotics |
| Nonsteroidal antiinflammatory drugs |
| Oral contraceptives |
| Etanercept, ipilimumab, and rituximab |
| Genetic mutations[18,19] |
| Homozygous variant/mutation in the G6Pase G6PC3 gene |
| Congenital chloride diarrhoea (SLC26A3 gene mutation) |
| Primary immunodeficiencies[20,21] |
| Antibody deficiency (common variable immunodeficiency, severe combined immunodeficiency, agammaglobulinemia, etc.) |
| Phagocytes defect (G6PC3 deficiency) |
| Complement deficiency |
| Immune dysregulation |
| Immune deficiency + syndromic features |
| CD4 lymphopenia |
| Author, yr | n | Treatment | Results | Discussion |
| Bolton et al[18], 2020 | 1 | Allogeneic HSCT | HSCT resolves G6PC3-associated immunodeficiency and Crohn’s disease phenotype | |
| Wicker et al[10], 2020 | 9 | G-CSF and cotrimoxazole; polymeric solution enriched in anti-inflammatory cytokine | Modulen IBD®, in addition to G-CSF and anti-bioprophylaxis, improves digestive symptoms | Dietetic treatment improved metabolic balance and clinical symptoms |
| Norsa et al[19], 2019 | 12 (2 patients with IBD-like colitis) | ASA; immuno-suppressant and biologics; ileostomy/colectomy | Treatment included a wide range of conservative treatment and ileostomy with variable success | |
| Xiao[9], 2019 | 2 | PEN, mesalazine, and recombinant human G-CSF | G-CSF increased ANC and improved clinical symptoms | G-CSF lowered the risk of developing IBD-colitis |
| Akkelle et al[20], 2018 | 425 (195 with GI symptoms) | Conventional immunosuppressive treatment, hematopoietic stem cell transplantation, hemicolectomy | Twelve patients (aged 9-16) had immunodeficiency associated IBD-like colitis. | Surgery was indicated if immune-therapy failed |
| de Andrade et al[17], 2014 | 16 | MPA switch, reduction, or discontinuation | IIBD-like colitis found in 25% of patients on MPA who underwent colonoscopy | Symptoms resolved after MPA switch or adjustment without need for surgery |
| Dubeau, et al[16], 2013 | Drugs including isotretinoin, antibiotics, nonsteroidal anti-inflammatory drugs may predispose IBD or IBD-like colitis | Pathogenic mechanisms may include altered immune response or microbiota | ||
| Kamdar et al[21], 2011 | 1 | Steroids and enteral feeding | Primarily conservative treatment usually sufficient without need for surgery |
IBD-like colitis associated with primary immunodeficiencies was studied by Akkelle et al[20]. Multiple genetic causes including glucose-6-phosphatase catalytic subunit 3 deficiency, common variable immunodeficiency and severe combined immunodeficiency were identified. Twelve patients with primary immunodeficiencies had colitis or enteropathy. One patient with recurrent subtotal intestinal obstruction secondary to inflamed stricture in the hepatic flexure underwent hemicolectomy. Another patient with chronic diarrhea, hypoalbuminemia and intestinal obstruction refractory to conventional immunosuppressive treatment also required operative management. IBD-like colitis can also be an unusual presentation in patients with X-linked agammaglobulinemia due to a reduction of B cells, like the case reported by Kamdar et al[21]. Treatment is primarily conservative with steroids and enteral feeding.
IBD-like colitis is associated with a few rare genetic disorders or certain drug use. First-line treatment is usually conservative with nutritional support or steroids. G-CSF or immunosuppressants may be beneficial. Surgical intervention like hemicolectomy is mainly reserved for refractory cases with intestinal obstruction resistant to medical treatment.
Manuscript source: Unsolicited manuscript
Specialty type: Surgery
Country/Territory of origin: China
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): B
Grade C (Good): 0
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Wattanasirichaigoon D S-Editor: Zhang H L-Editor: A P-Editor: Yuan YY
| 1. | Visser G, Rake JP, Fernandes J, Labrune P, Leonard JV, Moses S, Ullrich K, Smit GP. Neutropenia, neutrophil dysfunction, and inflammatory bowel disease in glycogen storage disease type Ib: results of the European Study on Glycogen Storage Disease type I. J Pediatr. 2000;137:187-191. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 168] [Cited by in RCA: 160] [Article Influence: 6.4] [Reference Citation Analysis (0)] |
| 2. | Dieckgraefe BK, Korzenik JR, Husain A, Dieruf L. Association of glycogen storage disease 1b and Crohn disease: results of a North American survey. Eur J Pediatr. 2002;161 Suppl 1:S88-S92. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 40] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 3. | Rake JP, Visser G, Labrune P, Leonard JV, Ullrich K, Smit GP; European Study on Glycogen Storage Disease Type I (ESGSD I). Guidelines for management of glycogen storage disease type I - European Study on Glycogen Storage Disease Type I (ESGSD I). Eur J Pediatr. 2002;161 Suppl 1:S112-S119. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 55] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 4. | Yamaguchi T, Ihara K, Matsumoto T, Tsutsumi Y, Nomura A, Ohga S, Hara T. Inflammatory bowel disease-like colitis in glycogen storage disease type 1b. Inflamm Bowel Dis. 2001;7:128-132. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 49] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 5. | Visser G, Rake JP, Labrune P, Leonard JV, Moses S, Ullrich K, Wendel U, Groenier KH, Smit GP. Granulocyte colony-stimulating factor in glycogen storage disease type 1b. Results of the European Study on Glycogen Storage Disease Type 1. Eur J Pediatr. 2002;161 Suppl 1:S83-S87. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 48] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 6. | Alsultan A, Sokol RJ, Lovell MA, Thurman G, Ambruso DR. Long term G-CSF-induced remission of ulcerative colitis-like inflammatory bowel disease in a patient with glycogen storage disease Ib and evaluation of associated neutrophil function. Pediatr Blood Cancer. 2010;55:1410-1413. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 18] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 7. | Volz MS, Nassir M, Treese C, von Winterfeld M, Plöckinger U, Epple HJ, Siegmund B. Inflammatory bowel disease (IBD)-like disease in a case of a 33-year old man with glycogenosis 1b. BMC Gastroenterol. 2015;15:45. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 8. | Saltik-Temizel IN, Koçak N, Ozen H, Yüce A, Gürakan F, Demir H. Inflammatory bowel disease-like colitis in a young Turkish child with glycogen storage disease type 1b and elevated platelet count. Turk J Pediatr. 2005;47:180-182. [PubMed] |
| 9. | Xiao Y. Two cases of GSD Ib complicated with Crohn-like colitis. J Pediatr Gastr Nutr. 2019;68:642. |
| 10. | Wicker C, Roda C, Perry A, Arnoux JB, Brassier A, Castelle M, Servais A, Donadieu J, Bouchereau J, Pigneur B, Labrune P, Ruemmele FM, de Lonlay P. Infectious and digestive complications in glycogen storage disease type Ib: Study of a French cohort. Mol Genet Metab Rep. 2020;23:100581. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 18] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 11. | El-Hajj II, Abdul-Baki H, El-Zahabi LM, Barada KA. Primary coloduodenal fistula in Crohn’s disease. Dig Dis Sci. 2007;52:59-63. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 11] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 12. | Kamath AS, Iqbal CW, Pham TH, Wolff BG, Chua HK, Donohue JH, Cima RR, Devine RM. Management and outcomes of primary coloduodenal fistulas. J Gastrointest Surg. 2011;15:1706-1711. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 12] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 13. | Gong J, Wei Y, Gu L, Li Y, Guo Z, Sun J, Ding C, Zhu W, Li N, Li J. Outcome of Surgery for Coloduodenal Fistula in Crohn’s Disease. J Gastrointest Surg. 2016;20:976-984. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 14] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 14. | Visser G, Rake JP, Labrune P, Leonard JV, Moses S, Ullrich K, Wendel U, Smit GP; European Study on Glycogen Storage Disease Type I. Consensus guidelines for management of glycogen storage disease type 1b - European Study on Glycogen Storage Disease Type 1. Eur J Pediatr. 2002;161 Suppl 1:S120-S123. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 28] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 15. | Jolissaint JS, Harary M, Saadat LV, Madenci AL, Dieffenbach BV, Al Natour RH, Tavakkoli A. Timing and Outcomes of Abdominal Surgery in Neutropenic Patients. J Gastrointest Surg. 2019;23:643-650. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 14] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 16. | Dubeau MF, Iacucci M, Beck PL, Moran GW, Kaplan GG, Ghosh S, Panaccione R. Drug-induced inflammatory bowel disease and IBD-like conditions. Inflamm Bowel Dis. 2013;19:445-456. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 44] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 17. | de Andrade LG, Rodrigues MA, Romeiro FG, Garcia PD, Contti MM, de Carvalho MF. Clinicopathologic features and outcome of mycophenolate-induced colitis in renal transplant recipients. Clin Transplant. 2014;28:1244-1248. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 16] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 18. | Bolton C, Burch N, Morgan J, Harrison B, Pandey S, Pagnamenta AT; Oxford IBD cohort investigators ; Taylor JC, Taylor JM, Marsh JCW, Potter V, Travis S, Uhlig HH. Remission of Inflammatory Bowel Disease in Glucose-6-Phosphatase 3 Deficiency by Allogeneic Haematopoietic Stem Cell Transplantation. J Crohns Colitis. 2020;14:142-147. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 23] [Cited by in RCA: 21] [Article Influence: 4.2] [Reference Citation Analysis (0)] |
| 19. | Norsa L, Canani RB, Duclaux-Loras R, Bequet E, Koeglmeier J, Russell R, Uhlig H, Koletzko S, Deflandre J, Neil S, Rodrigues A, Heinz-Erian P, Janecke AR, Lachaux A, Kolho KL and Ruemmele F. Congenital Chloride Diarrhea and Inflammatory Bowel Disease: An Emerging Association. J Pediatr Gastr Nutr. 2019;68:577. |
| 20. | Akkelle BS, Tutar E, Volkan B, Sengul OK, Ozen A, Celikel CA, Ertem D. Gastrointestinal Manifestations in Children with Primary Immunodeficiencies: Single Center: 12 Years Experience. Dig Dis. 2019;37:45-52. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 10] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 21. | Kamdar TA, Bass L, Chou P and Fuleihan R. Unusual presentation of an IBD-like colitis in X-linked agammaglobulinemia. Ann Allergy Asthma Immunol. 2011;107:A91. |