Published online Apr 6, 2021. doi: 10.12998/wjcc.v9.i10.2170
Peer-review started: December 1, 2020
First decision: December 13, 2020
Revised: December 25, 2020
Accepted: February 12, 2021
Article in press: February 12, 2021
Published online: April 6, 2021
Processing time: 119 Days and 0.6 Hours
The exact risk association of coronavirus disease 2019 (COVID-19) for surgeons is not quantified which may be affected by their risk of exposure and individual factors. The objective of this review is to quantify the risk of COVID-19 among surgeons, and explore whether facemask can minimise the risk of COVID-19 among surgeons. A systematised review was carried out by searching MEDLINE to locate items on severe acute respiratory syndrome coronavirus 2 or COVID-19 in relation to health care workers (HCWs) especially those work in surgical specialities including surgical nurses and intensivists. Additionally, systematic reviews that assessed the effectiveness of facemask against viral respiratory infections, including COVID-19, among HCWs were identified. Data from identified articles were abstracted, synthesised and summarised. Fourteen primary studies that provided data on severe acute respiratory syndrome coronavirus 2 infection or experience among surgeons and 11 systematic reviews that provided evidence of the effectiveness of facemask (and other personal protective equipment) were summarised. Although the risk of COVID-19 could not be quantified precisely among surgeons, about 14% of HCWs including surgeons had COVID-19, there could be variations depending on settings. Facemask was found to be somewhat protective against COVID-19, but the HCWs’ compliance was highly variable ranging from zero to 100%. Echoing surgical societies’ guidelines we continue to recommend facemask use among surgeons to prevent COVID-19.
Core Tip: The risk of coronavirus disease 2019 (COVID-19) among surgeons is unknown. By searching Medline we identified 14 primary studies that provided data on severe acute respiratory syndrome coronavirus infection among surgeons and identified 11 systematic reviews that provided evidence on the role of facemask against respiratory viral infection among health professionals. About 14% of health professionals including surgeons had COVID-19, and facemask was found to be somewhat protective against COVID-19, but the health professionals’ compliance was highly variable ranging from zero to 100%. In line with other guidelines we continue to recommend facemask use among surgeons to prevent COVID-19.
- Citation: Khalil MI, Banik GR, Mansoor S, Alqahtani AS, Rashid H. SARS-CoV-2, surgeons and surgical masks. World J Clin Cases 2021; 9(10): 2170-2180
- URL: https://www.wjgnet.com/2307-8960/full/v9/i10/2170.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v9.i10.2170
Beginning in late December 2019, coronavirus disease 2019 (COVID-19) spread across the globe leading to the largest pandemic of the century affecting (as of January 13, 2021) about 104 million cases with over 2.2 million fatalities[1].
Human to human transmission is believed to primarily occur through respiratory droplets (particles > 5-10 μm in diameter) during coughing and sneezing. Droplet nuclei are also increasingly recognised as a possible mechanism of spread, especially during prolonged exposure to high aerosol concentrations in closed spaces, in procedures like intubation, nebulisation, bone drilling and bronchoscopy[2]. Close contact is necessary for transmission of the disease and pre-symptomatic and asymptomatic individuals can contribute to up to 80% of COVID-19 transmission[3]. The spread, in fact, is primarily limited to household and healthcare settings, and other close contact settings. Across the world, thousands of health care workers (HCWs) have succumbed to the pandemic[4]. In fact, compared with the general community, front-line HCWs have a twelvefold increase in risk of a positive COVID-19 test[5]. HCWs who work in surgical specialities are at special risk of COVID-19 due to their intimate exposure to patients during surgical procedures some of which are aerosol generating. Indeed many initial cases of COVID-19 were among surgeons[4]; the first doctor to notify the emergence of the SARS-CoV-2 and subsequently sadly die of COVID-19, Mr Li Wenliang, was an ophthalmologist at Wuhan Central Hospital[6].
Personal protective equipment (PPE) including facemask, hand hygiene, physical distancing and reducing contact time (< 15 min) are standard measures of preventing COVID-19[2]. For HCWs performing aerosol-generating procedures, well fitted face-piece respirators, for example, N95 or N99 masks are recommended as part of PPE. Among front-line HCWs, reuse or inadequate use of PPE was each associated with a subsequent increased risk of COVID-19[5]. Given the uncertainty regarding the relative contribution of different transmission mechanisms, precautions against airborne transmission are recommended, but SARS-CoV-2 has also been detected in non-respiratory specimens[7].
The exact risk association of COVID-19 for surgeons is not quantified which may be affected by their risk of exposure and individual factors including age and underlying medical conditions.
The objective of this review is to quantify the risk of COVID-19 among surgeons, and explore whether facemasks and other PPE could minimise the risk of COVID-19 among surgeons.
MEDLINE search was conducted to locate items on SARS-CoV-2 or COVID-19 in relation to HCWs especially those working in surgical specialities like general surgeons, ophthalmologists, dentists, surgical nurses, anaesthetists, scrub nurse, and other staff that support operation theatre and surgical wards. Search terms including “exp Coronavirus”, “exp Coronavirus Infections”, “coronavirus.tw.” were combined with terms on surgeon or clinician* or practitioner.tw, health or hospital or clinical or medical, health care worker or HCW or doctor or nurse or allied health or dental or dentist.tw or intensivist or anaesthetist or anesthetist.tw.
All hits were then screened, initially by one reviewer (HR) but subsequently by a second reviewer (MIK), to identify relevant articles, both primary and systematic reviews, for final inclusion on the basis of relevance to our study aim.
The data were abstracted onto an Excel abstraction sheet with the following columns: author name, journal, manuscript title, study year, study type, setting, country, final sample size, HCW-yes/no, surgeon- yes/no, gender distribution (male: female), age of participants, presence of comorbidities, methods applied to establish diagnosis including sample type used, radiological/imaging studies, key results including number of surgeons affected, whether the participants used PPE especially facemask, any beneficial/harmful effect of PPE reported, any limitation of the study acknowledged by authors or identified by us.
This being a systematised review (not a systematic review), it was not deemed necessary to follow Preferred Reporting Items for Systematic Reviews and Meta-Analyses and hence quality assessment was not conducted.
We then identified and summarised systematic reviews that assessed the effectiveness or efficacy of facemask and/or PPE in the prevention of SARS-CoV-2 among HCWs.
We identified 14 original studies (as of November 29, 2020) that potentially include surgical HCWs. The studies included a pooled sample of 116136 HCWs, a large part of those included 100570 HCWs in a Centers for Disease Control (CDC) database and demographic data of 4099 orthopaedic surgeons and 9578 ear, nose and throat surgeons in the United Stated. One study involving elderly neurosurgeons in the United Stated did not provide the number of surgeons in their cohort[8]. Studies were conducted in the United States (n = 5), China (n = 3), the United Kingdom (n = 1), Italy (n = 1), Norway (n = 1), Singapore (n = 1) and Switzerland (n = 1), and one study was conducted in 37 countries across the world. Study settings varied widely from general hospital to tertiary care, and from phone interview to analysis of large national dataset (Table 1).
| Ref. | Study country | Setting | Sample size | Age in years | Male: female | Comorbidity n (%) | Diagnostic TEST | Sample type | Risk of disease | Comment |
| Hunter et al[16] | United Kingdom | Hospital | 1654 | Mean 41.7 | NR | NR | RT-PCR | Combined nose and throat swabs | Of 1654 HCWs tested, SARS-CoV-2 was detected in 240 (14%) | |
| Jella et al[9] | United States | National data pool | 4099 | All were aged ≥ 60 | NR | NR | NR | NR | For the top most states affected by COVID-19, elderly orthopaedic surgeons aged ≥ 60 years comprised up to 48% | |
| Chow et al[12] | United States, Washington | Phone interview of HCWs with COVID-19 | 48 | Median 43 (range 22-79) | 11:37 | 23 (49.7) | Not specified | NR | Among 48 HCWs with COVID-19 interviewed, 31 (64.6%) worked a median of 2 (range: 1-10) d while being symptomatic | Facemask use by HCWs might prevent transmission from asymptomatic cases |
| Liu et al[13] | China | University hospital | 30 | 21-59 | 10:20 | NR | RT-PCR | NR | Of all 30 COVID-19 cases, 8 did not wear masks and 6 others wore irregularly | |
| Hughes et al[46] | United States | CDC data pool | 571,708 with occupational status known | 41 (IQR: 30–53) | 79:21 | 17,838 (44%) had at least one comorbidity | Not specified | NR | Of 571,708 100,570 (22%) were HCWs. Nursing and residential care facilities were the commonest job settings | |
| Jella et al[8] | United States | National data pool | Not mentioned | All were aged ≥ 60 | NR | NR | NR | NR | In the 10 states with the highest number of COVID-19 cases older neurosurgical workforce (≥ 60) accounted for 20.6%-38.9% | |
| Ruthberg et al[10] | United States | National data pool | 9578 | All were aged >60 | NR | NR | NR | NR | Of all, 3081 were (32.2%) ENT surgeons aged > 60 years; the proportion by state ranged from 25.9% to 58.8% | |
| Durante-Mangoni et al[14] | Italy | Regional hospital | 4 (details were known for only 3) | 25-61 (of 3 cases) | 2:1 (no details about the 4th case) | NR | RT-PCR | Nasal/or pharyngeal swab | Four nurses infected. No transmission between HCWs wearing surgical masks and inpatients | Masks were beneficial |
| Jørstad et al[47] | Norway | Regional hospital | 6 | NR | NR | NR | Not specified | NR | Five ophthalmic surgeons and a ward nurse had COVID-19 | |
| Ducournau et al[17] | 37 countries (34) | Questionnaire survey | 47 | NR | NR | NR | Not applicable | NR | 42 of 47 (89.4%) wore surgical mask, 12 of 47 (25.5%) wore N95 mask, 32 of 47 (68.1%) wore goggles | This study is about the compliance of surgeons with PPE |
| Canova et al[15] | Switzerl | Contact racing | 21 | Median 40 (range 18–62) yr | 7:14 | NR | RT-PCR | Nasopharyngeal swab | None wore a face mask | None were positive for virus |
| Guo et al[11] | Wuhan, China | Hospital | 24 cases (and 48 controls) | 36.1 (25-48) | 23:1 | 1 (4.2%) had a comorbidity | RT-PCR and antibody tests | NR | Only 7 (29.2%) wore a facemask or respirator. Wearing respirator or mask all the time was protective (OR: 0.15, 95%CI: 0.04-0.55) | Orthopaedic surgeons are at risk of COVID-19 and masks are beneficial |
| Chan et al[48] | Honkong, China | University hospital | 14 (10 nurses and 4 other staff) | NR | NR | NR | NR | NR | Fourteen neurosurgery staff contracted COVID-19 following exposure to a patient | Full PPE should be worn during high risk procedures |
| Ng et al[18] | Singapore | University hospital | 41 HCWs exposed to an index patient | NR | NR | NR | RT-PCR | Nasopharyngeal swab | None of the exposed HCWs were RT-PCR positive; 85% wore a surgicalmask, and the rest wore N95 masks | Possibly masks and other standard measures are beneficial |
Age of participants ranged from 18 to 62 years, mean or median age was 36-43 years; three studies focused on surgeons aged ≥ 60 years[8-10]. Where data on gender distribution were available, except in one study in China involving orthopaedic surgeons where all but one were male[11], two-thirds to three fourths (66.6% to 77%) of cases were female[12-15]. Attack rate (of those exposed, number of those who had disease) was 14%[16]. Where information were available, the diagnosis was based on reverse transcription-polymerase chain reaction on nasal/pharyngeal/nasopharyngeal samples; this was supplemented by computerised tomography (CT) scan in one study[13] and CT scan plus other laboratory markers along with clinical features for three reverse transcription-polymerase chain reaction negative cases in another study[11].
Use of PPE varied across the studies, an international survey among hand surgeons found 89.4% (42/47) wore surgical mask, 25.5% (6/47) wore N95 mask, and 68.1% (32/47) wore protective glasses[17], but in practice compliance varied from zero in Switzerland[15] to almost 100% in Singapore in the early phase of the pandemic[18]. Wearing respirators or masks all the time was protective [odds ratio (OR: 0.15), 95% confidence interval (95%CI): 0.04-0.55] among orthopaedic surgeons[11], and no transmission between HCWs wearing surgical masks and inpatients was reported in one study[14]. However, despite using facemasks and respirators, COVID-19 transmission occurred among HCWs including surgeons[11,13].
Altogether, 11 systematic reviews were identified that included data involving effectiveness of facemasks against respiratory viruses among HCWs (Table 2). Three systematic reviews[19-21] have found facemasks to be effective mostly with low certainty of evidence from observational studies, another also found facemasks to be effective only in implant surgeons but not in other HCWs[22] another systematic review ruled out the effectiveness of medical masks and cloth masks but affirmed the effectiveness of N95 masks[23]. A systematic review indicated evidence of some effectiveness of cloth masks but that was considerably lower than that of surgical masks and respirators[24], which was buttressed by a focussed systematic review that revealed minimum efficacy of cloth masks compared to medical grade masks[25]. Of two systematic reviews that evaluated the effectiveness of medical masks against respirators, one ruled out any difference[26], but the other affirmed the superiority of N95 masks[27]. Finally, a systematic review of PPE use among surgeons found that whereas protection offered by fluid-repellent surgical mask was short-lasting (about 30 min) the protection offered by FFP2/3 respirators might last up to eight hours[28].
| Ref. | Participants | Intervention(s) | Comparator | Outcome | Comment |
| Jessop et al[28] | Surgeons | PPE including FFP2/3 and simple surgical masks | Nil | Protection using FFP2/3 respirators is reported to last up to 8 h, whereas protection is to last about 30 min for fluid-repellent masks | Narrative synthesis |
| Samaranayake et al[19] | Dentists | PPE: masks and respirators | Nil | Wearing layered, face-fitting masks/respirators and protective-eyewear can limit the spread of infection among HCWs; combined interventions such as a face mask and a face shield are better than individual ones | Mostly on HCWs in general, not just dentists |
| Aggarwal et al[49] | Community dwellers | Facemask and hand washing | Nil | There was no significant reduction in ILI either with facemask alone (pooled effect size: −0.17; [CI95%−0.43–0.10]) or facemask with hand wash (pooled effect size −0.09; [CI95%−0.58 to 0.40]) | |
| Liang et al[20] | Diverse participants including HCWs | Facemask | Nil | Use of masks by HCWs can reduce the risk of respiratory virus infection by 80% (OR: 0.20 (95%CI: −0.11–0.37)] | |
| Marson et al[22] | Surgeons | Facemask | Nil | The pooled effect of not wearing facemasks was a risk factor for infection RR: 0.77 (95%CI: 0.62-0.97), a case-control study demonstrated an OR of 3.34 (95%CI: 1.94-5.74) if facemasks were not worn by implant surgeons | The use of facemasks by implant surgeons may be beneficial |
| Sharma et al[25] | All settings including health care settings | Cloth facemask | Medical grade masks | Cloth facemasks show minimum efficacy in source control than the medical grade mask. The efficacy of cloth face masks filtration varies and depends on material type, and other factors | |
| Santos et al[24] | All settings including health care settings | Cloth facemask | Surgical masks and respirators | Cloth masks presented a considerably lower protection factor [1.9 (95%CI: 1.5-2.3)]; surgical and cloth masks reduced the total number of microbes expelled when coughing wearing a mask, while another study found that neither cloth nor surgical masks effectively filtered the virus expelled through coughing | Cloth masks are not recommendedfor HCWs |
| MacIntyre and Chughtai[23] | Community, HCWs and sick patients | Face masks | Respirators | RCTs in HCWs showed that respirators, if worn continually during a shift, were effective but not if worn intermittently. Medical masks were not effective, and cloth masks even less effective | |
| Chu et al[21] | Health-care and non-health-care settings | Physical distancing, face masks, and eye protection | N95 | Face mask use could result in reduction in risk of infection [aOR: 0.15 (95%CI: 0.07-0.34), RD: -14.3% (95%CI: -15.9 to -10.7)], with stronger association with N95 compared to surgical masks (P = 0.09) | Low certainty of evidence |
| Bartoszko et al[26] | HCWs | Medical masks | N95 | Compared with N95 respirators, the use of medical masks did not increase laboratory-confirmed viral respiratory infection [OR: 1.06 (95%CI: 0.90-1.25)]. Only one trial evaluated coronaviruses separately and found no difference between the two groups (P = 0.49) | Low certainty of evidence but only RCTs are included |
| Chou et al[27] | Health-care and community settings | Surgical, N95, andcloth | N95 or no mask | In health care settings, observational studies found that risk for infection with SARS-CoV-1 probably decreased with mask use and possibly decreased more with N95 mask use. RCTs found, N95 and surgical masks were probably associated with similar risks for ILI and laboratory-confirmed viral infection | Evidence on effectiveness of facemask is stronger in health care than communitysettings |
This narrative mini-review suggests that HCWs including surgeons are at greater risk of COVID-19. Surgeons including ophthalmic, orthopaedic, dental and neurosurgeons are affected by COVID-19 as well as are other staff of surgical team including anaesthetists and scrub nurses across the world.
Based on data from the United Kingdom, we note that roughly about 14% HCWs (that include surgeons) suffer from COVID-19, but this proportion can vary¸ for example 6.4% in the Netherlands, 3.8% to 5.7% in China[29,30], 17.8% in United States, 9% in Italy[30], and 12% HCWs in India had COVID-19[31]. Exceptionally high proportion (29%) of HCWs were affected in Wuhan in the early phase of the pandemic[32]. Variability is understood, and may stem from the HCWs’ exposure risk, their individual risk factors e.g., comorbidities and advanced age, and compliance with preventive measures. To what extent surgeons comprise this could not be ascertained but about 12.5% of COVID-19 transmission occurs in operation theatres[33], however, seeing about 79% of infection occurring among HCWs in general ward, it is likely that many surgical staff contract COVID-19 there[34].
A systematic review shows the incidence of COVID-19 among HCWs in China was much higher than that in general public; for instance in early phase of the pandemic, the pooled incidence in HCWs was 145 per 100000 compared to 42 per 100000 in general population[29]. Although the incidence of COVID-19 was higher among HCWs including surgeons, the incidence of severe or critical disease was lower than among general community. A meta-analysis of studies from China, United States and Italy showed the incidence of severe or critical COVID-19 disease in HCWs to be 9.9% (95%CI: 0.8–18.9) whereas the overall incidence in all COVID-19 patients was 29.4% (95%CI: 18.6–40.2). Similarly, mortality among HCWs was lower compared to the mortality in all patients [0.3% (95%CI: 0.2–0.4) vs 2.3% (95%CI: 2.2–2.4)][29,30,33]. The rate of severe or critical disease was lower despite a higher incidence. This is not fully understood and is a subject of further review but could be due to a number of facts: (1) Relatively younger age of and lower incidence of pre-existing medical conditions among working HCWs[5,35]; (2) Their readier accessibility to health care[30]; and (3) Their awareness of the disease course and knowledge when to seek help[36]. A study in the United States showed only 6% of HCWs were aged ≥ 65 years but approximately 40% of the fatal cases occurred in this age group[37].
Risk factors of COVID-19 among HCWs including surgeons are unqualified hand washing [relative risk (RR): 2.6], suboptimal hand hygiene before contact with patients (RR: 3.1) and suboptimal hand hygiene after contact with patients (RR: 2.4) and improper PPE use (RR: 2.8)[38].
This review shows wearing respirators or masks all of the time is protective [OR: 0.15 (95%CI: 0.04-0.55)][11], however the precise role of facemask and/or other PPE cannot be established because there are instances of no COVID-19 transmission when most (85%) HCWs used facemask as well when no (zero) HCW around an index case used facemask[15,18]. Data from systematic reviews show wearing facemask including by HCWs is effective against COVID-19, but the evidence is of low certainty, i.e. less convincing, primarily because the evidence comes from observational studies. A Cochrane systematic review reports with moderate certainty evidence that wearing a mask probably makes little or no difference to the outcome of laboratory-confirmed influenza compared to not wearing a mask [RR: 0.91 (95%CI: 0.66-1.26)][39]. A large trial conducted in Hajj setting (not included in this minireview) also failed to provide evidence on facemask efficacy against viral respiratory infections[40]. Subsequently, another large trial conducted in Denmark shows COVID-19 infection rate in mask group to be 1.8% compared to 2.1% in control group with the between-group difference of -0.3 percentage point (P = 0.33)[41].
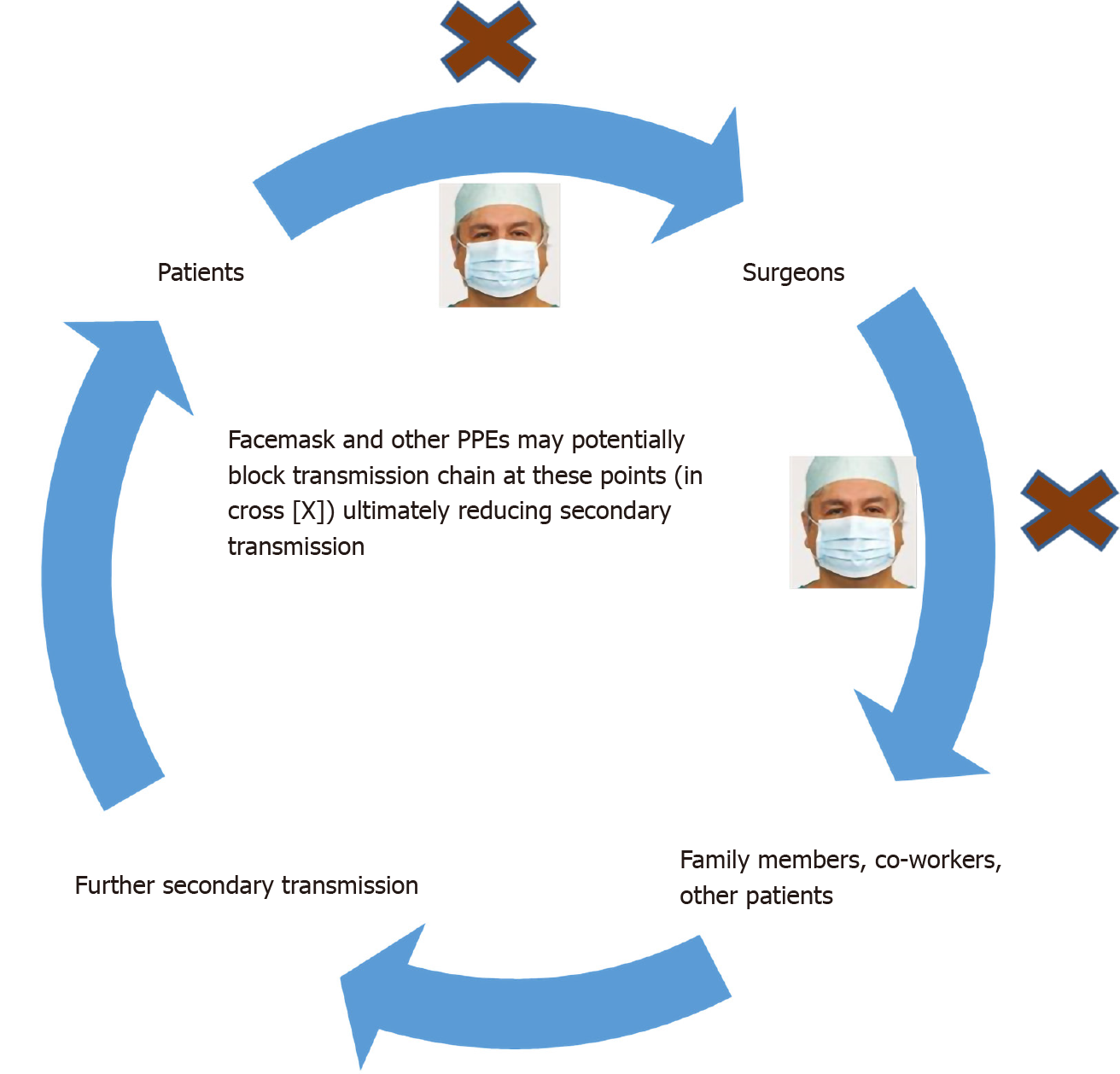
Irrespective of the uncertainty of evidence or having no strong evidence of benefit, facemask and other PPE are recommended by public health bodies (CDC, World Health Organization) and medical societies; since apart from COVID-19 vaccine in the earliest phase of implementation in selected countries, there is, as yet, no other widely available preventive measures to combat COVID-19. In surgeons using a facemask and other shields during a procedure is a traditional practice and can help minimise further secondary transmission of COVID-19 in both healthcare and community settings (Figure 1). Currently, the compliance with PPE use among HCWs ranges from zero to 100%[15,18]. A cross-sectional survey in Asia-Pacific among 263 intensivists showed only 59% intensive care unit staff complied with airborne precautions irrespective of aerosol generation procedures even though 97% claimed to conform to the World Health Organization recommendations for PPE practice[42].
A survey in Thailand involving 833 participants, both HCWs and non-HCWs, shows 454 participants (54.5%) developed adverse skin reactions most commonly acne (39.9%), rash (18.4%), and itching (15.6%)[43]. In many instances HCWs are not trained enough in PPE use and disposal, but the awareness of CDC guidelines on PPE use improves practice[44].
Baldock et al[45] have some advice for orthopaedic staff that include using PPE such as N95 respirator, goggles, face shield, gown, double gloves, and surgical balaclava; be trained in the correct technique of donning and doffing PPE; minimise procedures that lead to aerosolisation, and avoid unnecessary patient-staff contact for example by using dissolvable sutures, clear dressings, split casts[45].
In conclusion, we note that surgeons are at risk of COVID-19, although the precise risk could not be estimated. There is low to moderate evidence from observational studies that facemask and PPE use by HCWs may be beneficial against COVID-19, although these are grossly underutilized[46-49]. Health education trainings can improve practice.
Manuscript source: Invited manuscript
Specialty type: Medicine, research and experimental
Country/Territory of origin: Australia
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): B
Grade C (Good): 0
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Masaki S S-Editor: Zhang L L-Editor: A P-Editor: Ma YJ
| 1. | World Health Organization. WHO Coronavirus Disease (COVID-19) Dashboard. 2021 [cited February 1, 2021]. Available from: https://covid19.who.int. |
| 2. | Chagla Z, Hota S, Khan S, Mertz D; International Hospital and Community Epidemiology Group. Airborne Transmission of COVID-19. Clin Infect Dis. 2020;. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 21] [Cited by in RCA: 16] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 3. | Furukawa NW, Brooks JT, Sobel J. Evidence Supporting Transmission of Severe Acute Respiratory Syndrome Coronavirus 2 While Presymptomatic or Asymptomatic. Emerg Infect Dis. 2020;26. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 328] [Cited by in RCA: 352] [Article Influence: 70.4] [Reference Citation Analysis (0)] |
| 4. | Erdem H, Lucey DR. Healthcare worker infections and deaths due to COVID-19: A survey from 37 nations and a call for WHO to post national data on their website. Int J Infect Dis. 2020;102:239-241. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 108] [Cited by in RCA: 132] [Article Influence: 26.4] [Reference Citation Analysis (0)] |
| 5. | Nguyen LH, Drew DA, Graham MS, Joshi AD, Guo CG, Ma W, Mehta RS, Warner ET, Sikavi DR, Lo CH, Kwon S, Song M, Mucci LA, Stampfer MJ, Willett WC, Eliassen AH, Hart JE, Chavarro JE, Rich-Edwards JW, Davies R, Capdevila J, Lee KA, Lochlainn MN, Varsavsky T, Sudre CH, Cardoso MJ, Wolf J, Spector TD, Ourselin S, Steves CJ, Chan AT; COronavirus Pandemic Epidemiology Consortium. Risk of COVID-19 among front-line health-care workers and the general community: a prospective cohort study. Lancet Public Health. 2020;5:e475-e483. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1446] [Cited by in RCA: 1381] [Article Influence: 276.2] [Reference Citation Analysis (0)] |
| 6. | Petersen E, Hui D, Hamer DH, Blumberg L, Madoff LC, Pollack M, Lee SS, McLellan S, Memish Z, Praharaj I, Wasserman S, Ntoumi F, Azhar EI, Mchugh TD, Kock R, Ippolito G, Zumla A, Koopmans M. Li Wenliang, a face to the frontline healthcare worker. The first doctor to notify the emergence of the SARS-CoV-2, (COVID-19), outbreak. Int J Infect Dis. 2020;93:205-207. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 38] [Cited by in RCA: 42] [Article Influence: 8.4] [Reference Citation Analysis (0)] |
| 7. | Kang M, Wei J, Yuan J, Guo J, Zhang Y, Hang J, Qu Y, Qian H, Zhuang Y, Chen X, Peng X, Shi T, Wang J, Wu J, Song T, He J, Li Y, Zhong N. Probable Evidence of Fecal Aerosol Transmission of SARS-CoV-2 in a High-Rise Building. Ann Intern Med. 2020;173:974-980. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 184] [Cited by in RCA: 141] [Article Influence: 28.2] [Reference Citation Analysis (0)] |
| 8. | Jella TK, Desai A, Jella T, Steinmetz M, Kimmell K, Wright J, Wright CH; Council of State Neurosurgical Societies (CSNS). Geospatial Distribution of Neurosurgeons Age 60 and Older Relative to the Spread of COVID-19. World Neurosurg. 2021;145:e259-e266. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 9. | Jella TK, Acuña AJ, Samuel LT, Jella TK, Mroz TE, Kamath AF. Geospatial Mapping of Orthopaedic Surgeons Age 60 and Over and Confirmed Cases of COVID-19. J Bone Joint Surg Am. 2020;102:1022-1028. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 17] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 10. | Ruthberg JS, Quereshy HA, Jella TK, Kocharyan A, D'Anza B, Maronian N, Otteson TD. Geospatial analysis of COVID-19 and otolaryngologists above age 60. Am J Otolaryngol. 2020;41:102514. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 10] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 11. | Guo X, Wang J, Hu D, Wu L, Gu L, Wang Y, Zhao J, Zeng L, Zhang J, Wu Y. Survey of COVID-19 Disease Among Orthopaedic Surgeons in Wuhan, People's Republic of China. J Bone Joint Surg Am. 2020;102:847-854. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 127] [Cited by in RCA: 135] [Article Influence: 27.0] [Reference Citation Analysis (0)] |
| 12. | Chow EJ, Schwartz NG, Tobolowsky FA, Zacks RLT, Huntington-Frazier M, Reddy SC, Rao AK. Symptom Screening at Illness Onset of Health Care Personnel With SARS-CoV-2 Infection in King County, Washington. JAMA. 2020;323:2087-2089. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 127] [Cited by in RCA: 127] [Article Influence: 25.4] [Reference Citation Analysis (0)] |
| 13. | Liu M, He P, Liu HG, Wang XJ, Li FJ, Chen S, Lin J, Chen P, Liu JH, Li CH. [Clinical characteristics of 30 medical workers infected with new coronavirus pneumonia]. Zhonghua Jie He He Hu Xi Za Zhi. 2020;43:209-214. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 61] [Reference Citation Analysis (0)] |
| 14. | Durante-Mangoni E, Andini R, Bertolino L, Mele F, Bernardo M, Grimaldi M, Cuomo N, Tiberio C, Falco E, Di Spirito A, Raffone M, Russo MG, Atripaldi L, Zampino R. Low rate of severe acute respiratory syndrome coronavirus 2 spread among health-care personnel using ordinary personal protection equipment in a medium-incidence setting. Clin Microbiol Infect. 2020;26:1269-1270. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 16] [Cited by in RCA: 15] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 15. | Canova V, Lederer Schläpfer H, Piso RJ, Droll A, Fenner L, Hoffmann T, Hoffmann M. Transmission risk of SARS-CoV-2 to healthcare workers -observational results of a primary care hospital contact tracing. Swiss Med Wkly. 2020;150:w20257. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 48] [Article Influence: 9.6] [Reference Citation Analysis (0)] |
| 16. | Hunter E, Price DA, Murphy E, van der Loeff IS, Baker KF, Lendrem D, Lendrem C, Schmid ML, Pareja-Cebrian L, Welch A, Payne BAI, Duncan CJA. First experience of COVID-19 screening of health-care workers in England. Lancet. 2020;395:e77-e78. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 240] [Cited by in RCA: 188] [Article Influence: 37.6] [Reference Citation Analysis (0)] |
| 17. | Ducournau F, Arianni M, Awwad S, Baur EM, Beaulieu JY, Bouloudhnine M, Caloia M, Chagar K, Chen Z, Chin AY, Chow EC, Cobb T, David Y, Delgado PJ, Woon Man Fok M, French R, Golubev I, Haugstvedt JR, Ichihara S, Jorquera RA, Koo SCJJ, Lee JY, Lee YK, Lee YJ, Liu B, Kaleli T, Mantovani GR, Mathoulin C, Messina JC, Muccioli C, Nazerani S, Ng CY, Obdeijn MC, Van Overstraeten L, Prasetyono TOH, Ross M, Shih JT, Smith N, Suarez R FA, Chan PT, Tiemdjo H, Wahegaonkar A, Wells MC, Wong WY, Wu F, Yang XF, Yanni D, Yao J, Liverneaux PA. COVID-19: Initial experience of an international group of hand surgeons. Hand Surg Rehabil. 2020;39:159-166. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 46] [Cited by in RCA: 55] [Article Influence: 11.0] [Reference Citation Analysis (0)] |
| 18. | Ng K, Poon BH, Kiat Puar TH, Shan Quah JL, Loh WJ, Wong YJ, Tan TY, Raghuram J. COVID-19 and the Risk to Health Care Workers: A Case Report. Ann Intern Med. 2020;172:766-767. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 417] [Cited by in RCA: 359] [Article Influence: 71.8] [Reference Citation Analysis (0)] |
| 19. | Samaranayake LP, Fakhruddin KS, Ngo HC, Chang JWW, Panduwawala C. The effectiveness and efficacy of respiratory protective equipment (RPE) in dentistry and other health care settings: a systematic review. Acta Odontol Scand. 2020;78:626-639. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 22] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 20. | Liang M, Gao L, Cheng C, Zhou Q, Uy JP, Heiner K, Sun C. Efficacy of face mask in preventing respiratory virus transmission: A systematic review and meta-analysis. Travel Med Infect Dis. 2020;36:101751. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 227] [Cited by in RCA: 279] [Article Influence: 55.8] [Reference Citation Analysis (0)] |
| 21. | Chu DK, Akl EA, Duda S, Solo K, Yaacoub S, Schünemann HJ; COVID-19 Systematic Urgent Review Group Effort (SURGE) study authors. Physical distancing, face masks, and eye protection to prevent person-to-person transmission of SARS-CoV-2 and COVID-19: a systematic review and meta-analysis. Lancet. 2020;395:1973-1987. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2542] [Cited by in RCA: 2386] [Article Influence: 477.2] [Reference Citation Analysis (0)] |
| 22. | Marson BA, Craxford S, Valdes AM, Ollivere BJ. Are facemasks a priority for all staff in theatre to prevent surgical site infections during shortages of supply? Surgeon. 2020;. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 4] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 23. | MacIntyre CR, Chughtai AA. A rapid systematic review of the efficacy of face masks and respirators against coronaviruses and other respiratory transmissible viruses for the community, healthcare workers and sick patients. Int J Nurs Stud. 2020;108:103629. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 165] [Cited by in RCA: 187] [Article Influence: 37.4] [Reference Citation Analysis (0)] |
| 24. | Santos M, Torres D, Cardoso PC, Pandis N, Flores-Mir C, Medeiros R, Normando AD. Are cloth masks a substitute to medical masks in reducing transmission and contamination? Braz Oral Res. 2020;34:e123. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 15] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 25. | Sharma SK, Mishra M, Mudgal SK. Efficacy of cloth face mask in prevention of novel coronavirus infection transmission: A systematic review and meta-analysis. J Educ Health Promot. 2020;9:192. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 59] [Cited by in RCA: 50] [Article Influence: 10.0] [Reference Citation Analysis (0)] |
| 26. | Bartoszko JJ, Farooqi MAM, Alhazzani W, Loeb M. Medical masks vs N95 respirators for preventing COVID-19 in healthcare workers: A systematic review and meta-analysis of randomized trials. Influenza Other Respir Viruses. 2020;14:365-373. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 326] [Cited by in RCA: 292] [Article Influence: 58.4] [Reference Citation Analysis (0)] |
| 27. | Chou R, Dana T, Jungbauer R, Weeks C, McDonagh MS. Masks for Prevention of Respiratory Virus Infections, Including SARS-CoV-2, in Health Care and Community Settings: A Living Rapid Review. Ann Intern Med. 2020;173:542-555. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 101] [Cited by in RCA: 105] [Article Influence: 21.0] [Reference Citation Analysis (0)] |
| 28. | Jessop ZM, Dobbs TD, Ali SR, Combellack E, Clancy R, Ibrahim N, Jovic TH, Kaur AJ, Nijran A, O'Neill TB, Whitaker IS. Personal protective equipment for surgeons during COVID-19 pandemic: systematic review of availability, usage and rationing. Br J Surg. 2020;107:1262-1280. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 102] [Cited by in RCA: 92] [Article Influence: 18.4] [Reference Citation Analysis (0)] |
| 29. | Chou R, Dana T, Buckley DI, Selph S, Fu R, Totten AM. Epidemiology of and Risk Factors for Coronavirus Infection in Health Care Workers: A Living Rapid Review. Ann Intern Med. 2020;173:120-136. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 449] [Cited by in RCA: 422] [Article Influence: 84.4] [Reference Citation Analysis (0)] |
| 30. | Sahu AK, Amrithanand VT, Mathew R, Aggarwal P, Nayer J, Bhoi S. COVID-19 in health care workers - A systematic review and meta-analysis. Am J Emerg Med. 2020;38:1727-1731. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 114] [Cited by in RCA: 139] [Article Influence: 27.8] [Reference Citation Analysis (0)] |
| 31. | Goenka M, Afzalpurkar S, Goenka U, Das SS, Mukherjee M, Jajodia S, Shah BB, Patil VU, Rodge G, Khan U, Bandyopadhyay S. Seroprevalence of COVID-19 Amongst Health Care Workers in a Tertiary Care Hospital of a Metropolitan City from India. J Assoc Physicians India. 2020;68:14-19. [PubMed] |
| 32. | Bielicki JA, Duval X, Gobat N, Goossens H, Koopmans M, Tacconelli E, van der Werf S. Monitoring approaches for health-care workers during the COVID-19 pandemic. Lancet Infect Dis. 2020;20:e261-e267. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 197] [Cited by in RCA: 176] [Article Influence: 35.2] [Reference Citation Analysis (0)] |
| 33. | Zhou Q, Gao Y, Wang X, Liu R, Du P, Wang X, Zhang X, Lu S, Wang Z, Shi Q, Li W, Ma Y, Luo X, Fukuoka T, Ahn HS, Lee MS, Liu E, Chen Y, Luo Z, Yang K; COVID-19 Evidence and Recommendations Working Group. Nosocomial infections among patients with COVID-19, SARS and MERS: a rapid review and meta-analysis. Ann Transl Med. 2020;8:629. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 133] [Cited by in RCA: 136] [Article Influence: 27.2] [Reference Citation Analysis (0)] |
| 34. | Chhabra HS, Bagaraia V, Keny S, Kalidindi KKV, Mallepally A, Dhillon MS, Malhotra R, Rajasekharan S. COVID-19: Current Knowledge and Best Practices for Orthopaedic Surgeons. Indian J Orthop. 2020: 1-15. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 31] [Cited by in RCA: 28] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 35. | McMichael TM, Currie DW, Clark S, Pogosjans S, Kay M, Schwartz NG, Lewis J, Baer A, Kawakami V, Lukoff MD, Ferro J, Brostrom-Smith C, Rea TD, Sayre MR, Riedo FX, Russell D, Hiatt B, Montgomery P, Rao AK, Chow EJ, Tobolowsky F, Hughes MJ, Bardossy AC, Oakley LP, Jacobs JR, Stone ND, Reddy SC, Jernigan JA, Honein MA, Clark TA, Duchin JS; Public Health–Seattle and King County; EvergreenHealth; and CDC COVID-19 Investigation Team. Epidemiology of Covid-19 in a Long-Term Care Facility in King County, Washington. N Engl J Med. 2020;382:2005-2011. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 938] [Cited by in RCA: 926] [Article Influence: 185.2] [Reference Citation Analysis (0)] |
| 36. | Abohamr SI, Aldossari MA, Alaklobi FA, Amer HA, Alzarzour SH, Abdelhamid SW, Aljunaidi O, Badhawi OS, Siddiqui S, Jumaa H, Badwi M, Elsheikh E. Clinical characteristics and in-hospital outcome of medical staff infected with COVID-19 in Saudi Arabia. A retrospective single-center study. Saudi Med J. 2020;41:1336-1343. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 8] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 37. | CDC COVID-19 Response Team. Characteristics of Health Care Personnel with COVID-19 - United States, February 12-April 9, 2020. MMWR Morb Mortal Wkly Rep. 2020;69:477-481. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 522] [Cited by in RCA: 580] [Article Influence: 116.0] [Reference Citation Analysis (0)] |
| 38. | Christopher DJ, Isaac BT, Rupali P, Thangakunam B. Health-care preparedness and health-care worker protection in COVID-19 pandemic. Lung India. 2020;37:238-245. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 30] [Cited by in RCA: 26] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 39. | Jefferson T, Del Mar CB, Dooley L, Ferroni E, Al-Ansary LA, Bawazeer GA, van Driel ML, Jones MA, Thorning S, Beller EM, Clark J, Hoffmann TC, Glasziou PP, Conly JM. Physical interventions to interrupt or reduce the spread of respiratory viruses. Cochrane Database Syst Rev. 2020;11:CD006207. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 83] [Cited by in RCA: 125] [Article Influence: 25.0] [Reference Citation Analysis (0)] |
| 40. | Alfelali M, Haworth EA, Barasheed O, Badahdah AM, Bokhary H, Tashani M, Azeem MI, Kok J, Taylor J, Barnes EH, El Bashir H, Khandaker G, Holmes EC, Dwyer DE, Heron LG, Wilson GJ, Booy R, Rashid H; Hajj Research Team. Facemask against viral respiratory infections among Hajj pilgrims: A challenging cluster-randomized trial. PLoS One. 2020;15:e0240287. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 24] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 41. | Bundgaard H, Bundgaard JS, Raaschou-Pedersen DET, von Buchwald C, Todsen T, Norsk JB, Pries-Heje MM, Vissing CR, Nielsen PB, Winsløw UC, Fogh K, Hasselbalch R, Kristensen JH, Ringgaard A, Porsborg Andersen M, Goecke NB, Trebbien R, Skovgaard K, Benfield T, Ullum H, Torp-Pedersen C, Iversen K. Effectiveness of Adding a Mask Recommendation to Other Public Health Measures to Prevent SARS-CoV-2 Infection in Danish Mask Wearers : A Randomized Controlled Trial. Ann Intern Med. 2020;. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 197] [Cited by in RCA: 233] [Article Influence: 58.3] [Reference Citation Analysis (0)] |
| 42. | Rajamani A, Subramaniam A, Shekar K, Haji J, Luo J, Bihari S, Wong WT, Gullapalli N, Renner M, Alcancia CM, Ramanathan K; SPARTAN Collaborative - Small Projects; Audits; Research Trials – Australia/New Zealand. Personal protective equipment preparedness in Asia-Pacific intensive care units during the coronavirus disease 2019 pandemic: A multinational survey. Aust Crit Care. 2020;. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 17] [Cited by in RCA: 15] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 43. | Techasatian L, Lebsing S, Uppala R, Thaowandee W, Chaiyarit J, Supakunpinyo C, Panombualert S, Mairiang D, Saengnipanthkul S, Wichajarn K, Kiatchoosakun P, Kosalaraksa P. The Effects of the Face Mask on the Skin Underneath: A Prospective Survey During the COVID-19 Pandemic. J Prim Care Community Health. 2020;11:2150132720966167. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 78] [Cited by in RCA: 73] [Article Influence: 14.6] [Reference Citation Analysis (0)] |
| 44. | Cash RE, Rivard MK, Camargo CA Jr, Powell JR, Panchal AR. Emergency medical services personnel awareness and training about personal protective equipment during the COVID-19 pandemic. Prehosp Emerg Care. 2020: 1-11. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 18] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 45. | Baldock TE, Bolam SM, Gao R, Zhu MF, Rosenfeldt MPJ, Young SW, Munro JT, Monk AP. Infection prevention measures for orthopaedic departments during the COVID-2019 pandemic: a review of current evidence. Bone Jt Open. 2020;1:74-79. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 15] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 46. | Hughes MM, Groenewold MR, Lessem SE, Xu K, Ussery EN, Wiegand RE, Qin X, Do T, Thomas D, Tsai S, Davidson A, Latash J, Eckel S, Collins J, Ojo M, McHugh L, Li W, Chen J, Chan J, Wortham JM, Reagan-Steiner S, Lee JT, Reddy SC, Kuhar DT, Burrer SL, Stuckey MJ. Update: Characteristics of Health Care Personnel with COVID-19 - United States, February 12-July 16, 2020. MMWR Morb Mortal Wkly Rep. 2020;69:1364-1368. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 83] [Cited by in RCA: 112] [Article Influence: 22.4] [Reference Citation Analysis (0)] |
| 47. | Jørstad ØK, Moe MC, Eriksen K, Petrovski G, Bragadóttir R. Coronavirus disease 2019 (COVID-19) outbreak at the Department of Ophthalmology, Oslo University Hospital, Norway. Acta Ophthalmol. 2020;98:e388-e389. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 39] [Cited by in RCA: 42] [Article Influence: 8.4] [Reference Citation Analysis (0)] |
| 48. | Chan DYC, Chan DTM, Mak WK, Wong GKC, Poon WS. Letter: Rongeurs, Neurosurgeons, and COVID-19: How Do We Protect Health Care Personnel During Neurosurgical Operations in the Midst of Aerosol-Generation From High-Speed Drills? Neurosurgery. 2020;87:E164-E165. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 11] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 49. | Aggarwal N, Dwarakanathan V, Gautam N, Ray A. Facemasks for prevention of viral respiratory infections in community settings: A systematic review and meta-analysis. Indian J Public Health. 2020;64:S192-S200. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 9] [Article Influence: 1.8] [Reference Citation Analysis (0)] |