Published online May 6, 2019. doi: 10.12998/wjcc.v7.i9.1087
Peer-review started: January 25, 2019
First decision: March 14, 2019
Revised: March 21, 2019
Accepted: March 26, 2019
Article in press: March 26, 2019
Published online: May 6, 2019
Processing time: 102 Days and 4.3 Hours
The Janus kinase 2 (JAK2) V617F mutation is common in patients with breakpoint cluster region-Abelson1 (BCR-ABL1)-negative myeloproliferative neoplasms, including polycythemia vera, essential thrombocythemia and primary myelofibrosis, but is rarely detected in BCR-ABL1-positive chronic myeloid leukemia (CML) patients. Here, we report a CML patient with both a BCR-ABL1 rearrangement and JAK2 V617F mutation.
A 45-year-old Chinese woman was admitted to our department with a history of significant thrombocytosis for 20 d. Color Doppler ultrasound examination showed mild splenomegaly. Bone marrow aspiration revealed a karyotype of 46, XX, t(9;22)(q34;q11.2) in 20/20 metaphases by cytogenetic analysis, rearrangement of BCR-ABL1 (32.31%) by fluorescent polymerase chain reaction (PCR) and mutation of JAK2 V617F (10%) by PCR and Sanger DNA sequencing. The patient was diagnosed with CML and JAK2 V617F mutation. Following treatment with imatinib for 3 mo, the patient had an optimal response and BCR-ABL1 (IS) was 0.143%, while the mutation rate of JAK2 V617F rose to 15%.
Emphasis should be placed on the detection of JAK2 mutation when CML is diagnosed to distinguish JAK2 mutation-positive CML and formulate treatment strategies.
Core tip: The Janus kinase 2 (JAK2) V617F mutation is rare in breakpoint cluster region-Abelson1 (BCR-ABL1)-positive chronic myeloid leukemia (CML). We report a female CML patient with a JAK2 V617F mutation. This rare subset of CML patients often have notable thrombocythemia in addition to more typical CML features. The patient achieved complete hematological response following 2 mo imatinib treatment. After 3 mo of imatinib treatment, the value of BCR-ABL1 (IS) was 0.143%, but the JAK2 V617F mutation rate rose from 10% to 15%.
- Citation: Shi XB, Jiang JF, Jin FX, Cheng W. Coexistence of breakpoint cluster region-Abelson1 rearrangement and Janus kinase 2 V617F mutation in chronic myeloid leukemia: A case report. World J Clin Cases 2019; 7(9): 1087-1092
- URL: https://www.wjgnet.com/2307-8960/full/v7/i9/1087.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v7.i9.1087
Chronic myeloid leukemia (CML) is a hematologic malignant neoplasm with clonal proliferation of hematopoietic cells. The specific molecular biologic feature of typical CML corresponds to a translocation between chromosome 9 and chromosome 22 [t(9;22)(q34;q11)], named the Philadelphia (Ph) chromosome, which leads to breakpoint cluster region-Abelson1 (BCR-ABL1) rearrangement[1]. The Ph chromosome and/or BCR-ABL1 rearrangement are necessary for the diagnosis of typical CML[1]. Janus kinase 2 (JAK2) V617F mutation is an important biomarker in the diagnosis of myeloproliferative neoplasms (MPNs). According to the literature, the mutation rate of JAK2 V617F is 90%-95% in polycythemia vera (PV) and about 60% in both essential thrombocythemia (ET) and primary myelofibrosis (PMF)[2]. However, BCR-ABL1-positive CML with JAK2 V617F mutation is very uncommon. Herein, we present a case of CML with both the BCR-ABL1 rearrangement and JAK2 V617F mutation.
On May 29, 2018, a 45-year-old Chinese woman with a history of marked thrombocytosis for 20 d was admitted to the Department of Hematology and Oncology, Tongling People’s Hospital (Anhui Province, China).
She had been treated with antibiotics for 3 wk for lobar pneumonia in another hospital before admission to our hospital. Peripheral blood count showed a platelet count of 586 × 109/L at the beginning of anti-infective therapy, which increased to 1109 × 109/L when her pneumonia resolved. She attended our department for hematological evaluation.
She had no past history of surgery, anemia or malignant neoplasms and was not taking any medication.
She was married, and her spouse and daughter were both healthy. The family history was unremarkable.
Physical examination showed that the splenic inferior margin was 2 cm under the left arcus costarum.
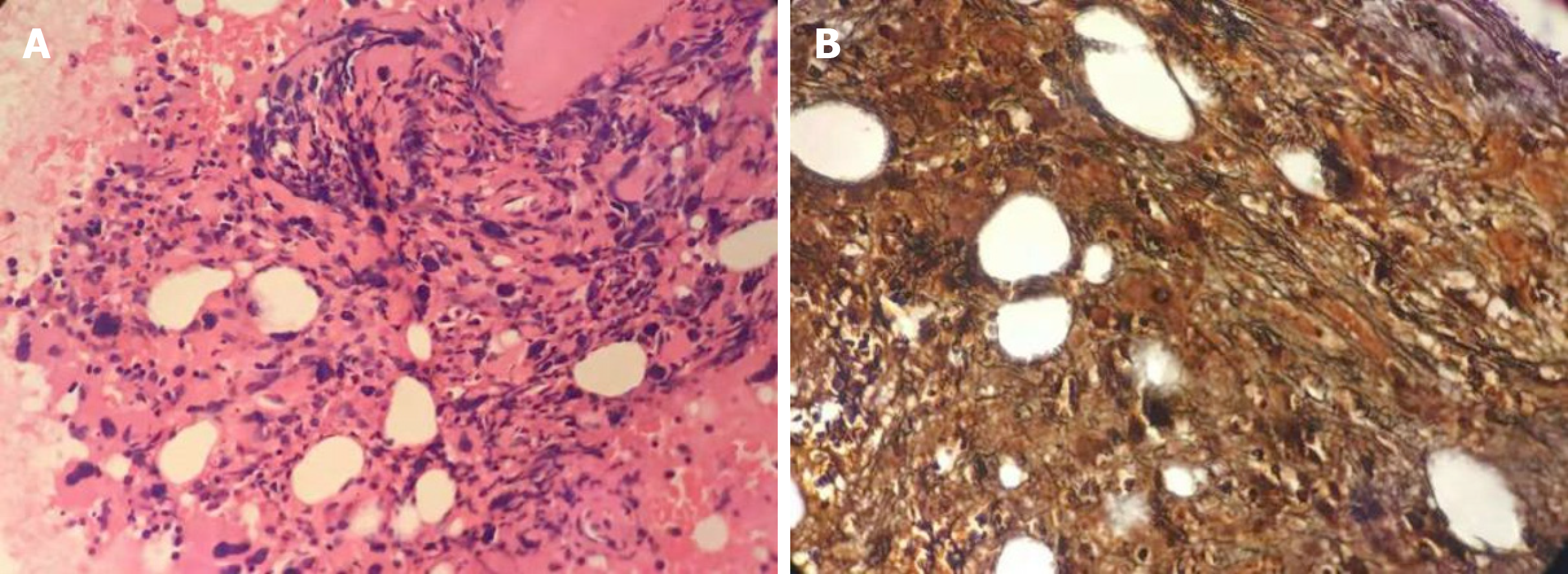
The concentration of lactate dehydrogenase was 364 U/L. Peripheral blood count showed a leukocyte count of 11.46 × 109/L, hemoglobin of 121 g/L, platelet count of 1582 × 109/L and neutrophil count of 7.63 × 109/L. Peripheral blood smear examination showed 2% blasts, 1% myelocytes, 70% mature neutrophils, 3% eosinophils, 7% basophils, 13% lymphocytes and 4% monocytes (Table 1). Bone marrow cytomorphologic examination revealed mild granulocytic hyperplasia of 49%, including 1.5% myelocytes, 5.5% metamyelocytes, 10.5% stab nuclear neutrophils, 22% segmented neutrophils, 1.5% eosinophils, 3% basophils and 5% blasts (Table 1). The leukocyte alkaline phosphatase score was 135 and leukocyte alkaline phosphatase positivity was 92%. Immunophenotyping analysis by flow cytometry revealed 5% blast cells. The reagents applied in flow cytometry mainly consisted of antibodies against CD10, CD19, CD5, CD7, CD13, CD33, HLA-DR, CD38, CD34, CD16, CD11b, CD117, CD36, CD64, CD56, CD14, CD20, CD8, CD3, CD2, CD4, cMPO, cCD22, cCD3, TCRab, TCRgd, CD45RA, CD45RO, CD15,CD11c, CD43 and CD45. Cytogenetic analysis using both the G-banding and R-banding technique demonstrated a karyotype of 46, XX, t(9:22)(q34;q11.2) in 20/20 metaphases examined. The rearrangement of BCR-ABL1 (P210) was detected by fluorescent polymerase chain reaction (commonly known as PCR), and the BCR-ABL1/ABL1 ratio was 32.31%. Moreover, the JAK2 V617F mutation was identified by PCR and Sanger DNA sequencing, and the mutation percentage, which was calculated as [copy-numberJAK2V617F / (copy-numberJAK2V617F + copy-numberwild-type JAK2)], was 10%. Bone marrow biopsy examination showed active proliferation of granulocytic cells and marked hyperplasia of megakaryocytes (Figure 1A). The proliferative megakaryocytes had small cell bodies and decreased karyolobism. Additional immunohistochemistry of bone marrow cells exhibited CD34 (2%+), CD117 (5%+), MPO partial +, CD235a minority +, CD61 + for megakaryocytes and a few scattered CD138 +. Gomori staining was positive (++ - +++) (Figure 1B).
| Cell types | Peripheral blood | Bone marrow |
| Cell counts, % | Cell counts, % | |
| Blast | 2 | 5 |
| Myelocyte | 1 | 1.5 |
| Metamyelocyte | NA | 5.5 |
| Mature neutrophil | 70 | 32.5 |
| Stab nuclear neutrophil | NA | 10.5 |
| Segmented neutrophil | NA | 22 |
| Eosinophil | 3 | 1.5 |
| Basophil | 7 | 3 |
| Lymphocyte | 13 | 10.5 |
| Monocyte | 4 | 1 |
Color Doppler ultrasound examination showed mild splenomegaly.
The patient was diagnosed with CML (chronic phase, Sokal 1.68, high risk) and JAK2 V617F mutation.
Due to severe thrombocytosis, the patient was treated with hydroxyurea (0.5-2.0 g/d), aspirin (0.1 g/d) and platelet separation. On the sixth day of hospitalization, she was administered imatinib (0.4 g/d) due to the detection of the BCR-ABL1 rearrangement. Her platelet count rapidly decreased, and hydroxyurea and aspirin were discontinued successively.
On July 11, 2018, her peripheral blood counts were as follows: leukocytes 3.44 × 109/L, neutrophils 2.11 × 109/L, hemoglobin 117 g/L and platelets 130 × 109/L, and she was discharged from the hospital. After leaving hospital, she continued to take imatinib (0.4 g/d). During regular follow-up, her peripheral blood counts were in the normal reference range, and spleen size returned to normal within 2 mo. After 3 mo of imatinib therapy, bone marrow aspiration was reexamined. Mutation of the ABL1 kinase domain was negative. Chromosomal karyotype was 46, XX in all 20 metaphases by G-banding, while the karyotype of 46, XX, t(9;22)(q34;q11.2) was identified in 1/16 metaphases by R-banding. The BCR-ABL1/ABL1 ratio decreased to 0.216% and BCR-ABL1 (IS) was 0.143%, but the percentage of JAK2 V617F mutation increased to 15%. The patient had an optimal response to imatinib therapy and is continuing to take imatinib.
MPNs are clonal disorders of hematopoietic stem cells, and they can be divided into BCR-ABL1-negative MPN and Ph chromosome and/or BCR-ABL1 positive CML according to the 2016 World Health Organization classification system for hematopoietic and lymphoid tissue tumors. The former mainly includes JAK2/CALR/MPL mutated MPNs (PV, ET and PMF), chronic neutrophilic leukemia, chronic eosinophilic leukemia and unclassified MPN[2]. As an important marker in the diagnosis of JAK2/CALR/MPL mutated MPNs, the JAK2 V617F mutation has often been reported in PV, ET and PMF, but rarely in typical CML.
In recent years, a few studies have reported that BCR-ABL1 rearrangement/Ph chromosome and JAK2 V617F mutation can coexist in CML patients[3-14]. However, some of these studies failed to examine JAK2 status at the time of initial diagnosis of CML, but detected JAK2 V617F mutation with a decrease in BCR-ABL1 translocation level during treatment with tyrosine kinase inhibitors (TKIs)[3-9], while others discovered concomitant BCR-ABL1 rearrangement and JAK2 V617F mutation when CML was diagnosed and before administration of TKIs[5,10-14]. The CML patients with a JAK2 V617F mutation not only had typical CML characteristics but also had notable thrombocythemia[5-7,9-11], and thrombocytosis even persisted in some patients after obtaining a complete cytogenetic response, major molecular response or deep molecular response after TKI therapy[5,7,11]. Most studies indicated that following TKI treatment, the mutation rate of JAK2 V617F increased with a decrease in BCR-ABL1 transcript level in this category of CML patients[7,8,12,13]. Only one study showed that JAK2 V617F mutation gradually decreased and then disappeared, accompanied by a reduction in BCR-ABL1 rearrangement[10]. As reported in the literature, JAK2 V617F mutation affected the curative effect in CML patients, and JAK2 V617F-positive CML patients often had a suboptimal response to TKIs[9,10,13]. Pahore et al[14] demonstrated that 26.7% of 45 CML patients had a JAK2 V617F mutation, and the risk of early disease progression in patients with a JAK2 V617F mutation was significantly higher than that in patients without the JAK2 V617F mutation.
There is no optimal treatment strategy for JAK2 V617F-positive CML patients. As described in published reports, TKIs are preferentially administered in this subset of patients[3-12]. To our knowledge, it is unclear whether such cases can benefit from the JAK2 inhibitor ruxolitinib.
In our patient, bone marrow examination revealed the coexistence of BCR-ABL1 rearrangement and JAK2 V617F mutation before imatinib was administered, and the patient also presented with marked megakaryocytic hyperplasia and myelofibrosis. Following hospitalization, peripheral blood primarily showed a marked increase in platelet count. The patient achieved complete hematological response following 2 mo of imatinib treatment. After 3 mo of imatinib treatment, the proportion of Ph chromosome-positive cells was 6.25% in all metaphases and BCR-ABL1 (IS) was 0.143%, which suggested that the optimum response had been obtained. However, the JAK2 V617F mutation rate rose from 10% to 15%. The marked thrombocytosis observed at diagnosis and identification of the JAK2 V617F mutation level increasing in pace with the decrease in BCR-ABL1 transcript level during imatinib therapy were consistent with previously reported observations[5-9,11-13]. We hypothesize that the coexistence of BCR-ABL1 rearrangement and JAK2 V617F mutation originates from two different clones that grow independently. Although our patient has favorable treatment efficacy at present, the JAK2 V617F mutation level is still increasing and bone marrow fibrosis is still present. Thus, the long-term prognosis of this patient may be poor, and extended follow-up is required.
With the rapid development of molecular biology, a few CML patients with a JAK2 V617F mutation have been reported recently, but such cases are relatively rare. The specific pathogenesis, optimal treatment and prognosis of this special type of CML are currently still ambiguous, and further large-sample studies are urgently needed. Moreover, further research to determine whether the JAK2 mutation is associated with BCR-ABL1 translocation in these patients is required. Attention should be paid to the detection of the JAK2 mutation during the diagnosis and treatment of CML in order to timely identify JAK2 mutation-positive CML patients and guide the formulation of treatment strategies.
CARE Checklist: We have read the CARE Checklist (2016), and this manuscript was prepared and revised according to the CARE Checklist (2016).
Manuscript source: Unsolicited manuscript
Specialty type: Medicine, research and experimental
Country of origin: China
Peer-review report classification
Grade A (Excellent): A
Grade B (Very good): B
Grade C (Good): 0
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Redondo PC, Xavier-Elsas P S-Editor: Gong ZM L-Editor: Filipodia E-Editor: Wu YXJ
| 1. | Jabbour E, Kantarjian H. Chronic myeloid leukemia: 2016 update on diagnosis, therapy, and monitoring. Am J Hematol. 2016;91:252-265. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 110] [Cited by in RCA: 128] [Article Influence: 14.2] [Reference Citation Analysis (0)] |
| 2. | Barbui T, Thiele J, Gisslinger H, Kvasnicka HM, Vannucchi AM, Guglielmelli P, Orazi A, Tefferi A. The 2016 WHO classification and diagnostic criteria for myeloproliferative neoplasms: document summary and in-depth discussion. Blood Cancer J. 2018;8:15. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 252] [Cited by in RCA: 410] [Article Influence: 58.6] [Reference Citation Analysis (0)] |
| 3. | Krämer A, Reiter A, Kruth J, Erben P, Hochhaus A, Müller M, Cross NC, Jones AV, Ho AD, Hensel M. JAK2-V617F mutation in a patient with Philadelphia-chromosome-positive chronic myeloid leukaemia. Lancet Oncol. 2007;8:658-660. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 61] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 4. | Inami M, Inokuchi K, Okabe M, Kosaka F, Mitamura Y, Yamaguchi H, Dan K. Polycythemia associated with the JAK2V617F mutation emerged during treatment of chronic myelogenous leukemia. Leukemia. 2007;21:1103-1104. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 44] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 5. | Darling HS, Kumar R, Kapoor R, Singh J, Verma T. BCR-ABL and JAK2V617F Mutation Co-existence, Rare or Just Unexplored. Indian J Hematol Blood Transfus. 2017;33:633-635. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 6. | Pagnano KB, Delamain MT, Magnus MM, Vassallo J, DE Souza CA, DE Almeida D, Lorand-Metze I. Concomitant essential thrombocythemia with JAK2 V617F mutation in a patient with chronic myeloid leukemia with major molecular response with imatinib and long-term follow-up. Oncol Lett. 2016;12:485-487. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 10] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 7. | Pastore F, Schneider S, Christ O, Hiddemann W, Spiekermann K. Impressive thrombocytosis evolving in a patient with a BCR-ABL positive CML in major molecular response during dasatinib treatment unmasks an additional JAK2V617F. Exp Hematol Oncol. 2013;2:24. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 19] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 8. | Hussein K, Bock O, Seegers A, Flasshove M, Henneke F, Buesche G, Kreipe HH. Myelofibrosis evolving during imatinib treatment of a chronic myeloproliferative disease with coexisting BCR-ABL translocation and JAK2V617F mutation. Blood. 2007;109:4106-4107. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 77] [Cited by in RCA: 76] [Article Influence: 4.2] [Reference Citation Analysis (0)] |
| 9. | Hassan A, Dogara LG, Babadoko AA, Awwalu S, Mamman AI. Coexistence of JAK2 and BCR-ABL mutation in patient with myeloproliferative neoplasm. Niger Med J. 2015;56:74-76. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 18] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 10. | Campiotti L, Appio L, Solbiati F, Ageno W, Venco A. JAK2-V617F mutation and Philadelphia positive chronic myeloid leukemia. Leuk Res. 2009;33:e212-e213. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 20] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 11. | Lewandowski K, Gniot M, Wojtaszewska M, Kanduła Z, Becht R, Paczkowska E, Mędraś E, Wasilewska E, Iwoła M. Coexistence of JAK2 or CALR mutation is a rare but clinically important event in chronic myeloid leukemia patients treated with tyrosine kinase inhibitors. Int J Lab Hematol. 2018;40:366-371. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 11] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 12. | Xu W, Chen B, Tong X. Chronic myeloid leukemia patient with co-occurrence of BCR-ABL junction and JAK2 V617F mutation. Int J Hematol. 2014;99:87-90. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 15] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 13. | De Roeck L, Michaux L, Debackere K, Lierman E, Vandenberghe P, Devos T. Coexisting driver mutations in MPN: clinical and molecular characteristics of a series of 11 patients. Hematology. 2018;23:785-792. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 22] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 14. | Pahore ZA, Shamsi TS, Taj M, Farzana T, Ansari SH, Nadeem M, Ahmad M, Naz A. JAK2V617F mutation in chronic myeloid leukemia predicts early disease progression. J Coll Physicians Surg Pak. 2011;21:472-475. [PubMed] |