Published online Apr 6, 2024. doi: 10.12998/wjcc.v12.i10.1817
Peer-review started: November 23, 2023
First decision: January 9, 2024
Revised: February 3, 2024
Accepted: March 8, 2024
Article in press: March 8, 2024
Published online: April 6, 2024
Processing time: 130 Days and 22.6 Hours
Carcinosarcoma of the gallbladder is a rare malignant tumor with a very poor prognosis. To date, only approximately 100 patients have been reported in the English literature. The prognosis of this tumor type is poor, the preoperative diagnosis is difficult, and there is a possibility of a misdiagnosis. We present an unsuccessful case of carcinosarcoma of the gallbladder with a preoperative misdiagnosis and rapid early postoperative recurrence. Therefore, we have a deeper understanding of the poor prognosis of gallbladder carcinosarcoma (GBC) patients.
The patient is a 65-year-old male. He was admitted to the hospital because of right upper abdomen distending pain and discomfort for half a month. Abdominal magnetic resonance imaging revealed a polycystic mass in the right lobe of the liver and the fossa of the gallbladder. After admission, the patient was diagnosed with a liver abscess, which was treated by abscess puncture drainage. Obviously, this treatment was unsuccessful. Hepatectomy and cholecystectomy were performed one month after the puncture. Postoperative pathologic examination revealed carcinosarcoma of the gallbladder, and the resected specimen contained two tumor components. One month after surgery, the patient's tumor recurred in situ and started to compress the duodenum, resulting in duodenal obstruction and bleeding. The treatment was not effective. The patient died of gastrointestinal hemorrhage and hypovolemic shock.
Carcinosarcoma of the gallbladder is a rare malignant tumor that is easily misdiagnosed preoperatively and has a poor prognosis.
Core Tip: Herein, we report a patient with carcinosarcoma of the gallbladder who was diagnosed with a liver abscess before surgery due to radiographic polycystic features of the liver. Then, the wrong treatment was administered. After surgical removal of the tumor, the tumor rapidly recurred locally and caused obstruction and bleeding of the digestive tract, leading to the patient’s death. We need to learn some lessons from this case.
- Citation: Dai Y, Meng M, Luo QZ, Liu YJ, Xiao F, Wang CH. Gallbladder carcinosarcoma with a poor prognosis: A case report. World J Clin Cases 2024; 12(10): 1817-1823
- URL: https://www.wjgnet.com/2307-8960/full/v12/i10/1817.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v12.i10.1817
Gallbladder carcinosarcoma is an extremely rare malignant tumor that contains both mesodermal and epithelial tumor components[1]. The clinical presentation of this condition is nonspecific, making it challenging to diagnose preoperatively, and the overall prognosis is unfavorable[2]. In 2023, a patient with highly malignant gallbladder carcinosarcoma was admitted to our department, and unfortunately, the patient’s prognosis was very poor. The details of the case are presented below.
Abdominal pain for two weeks.
In January 2023, we admitted a 65-year-old male patient to our hospital who presented with a history of abdominal pain for two weeks. The patient reported experiencing right upper abdominal pain and discomfort, characterized by intermittent distending pain, along with mild fatigue and weight loss. Notably, the patient denied any symptoms of jaundice, fever, nausea, vomiting, or diarrhea.
The patient denied any history of hepatitis B or gallstones.
The patient denied a family history of similar episodes of illness.
The patient’s body temperature was measured at 36.5 °C, and no obvious signs of jaundice were observed in the skin or sclera. Tenderness was noted in the right upper abdomen, with no evidence of muscle tension or rebound pain. No palpable masses were detected, but a suspicious positive Murphy sign was noted.
The routine blood test results were as follows: WBC 13.9 × 109/L, neutrophils granulocyte percentage 85.5%; RBC 2.86 × 1012/L; Hb 8.0 g/L; PLT 423 × 109/L; CRP 105.71 mg/L; liver function: ALT 23 μ/mL; AST 38 μ/mL; AKP 388 μ/mL; r-GGT 469 μ/mL; TBLD 4.7 μmol/L, ALB 37.5 g/L; tumor marker: CA19-9 59.86 μ/mL; CA125 43.97 μ/mL; CEA 2.13 ng/mL; and AFP 7.4 ng/mL.
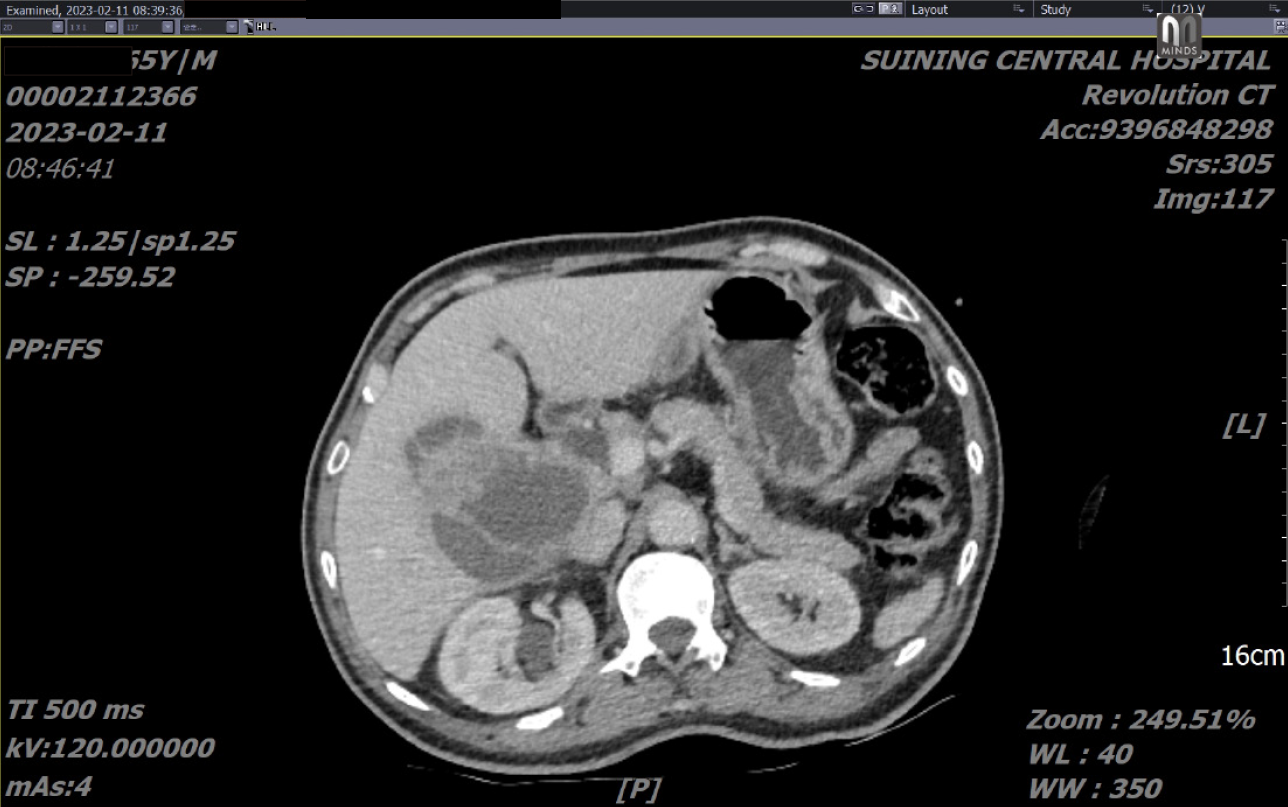
Abdominal computed tomography (CT) revealed clumps with slightly reduced density in the right lobe of the liver and the gallbladder fossa. There was also an area of uneven density, along with localized high-density shadows, with a larger cross-section measuring approximately 10.1 cm × 7.5 cm. An enhanced scan indicated irregular enhancement, suggesting the potential presence of suppurative cholecystitis involving the liver and the formation of a liver abscess (Figure 1).
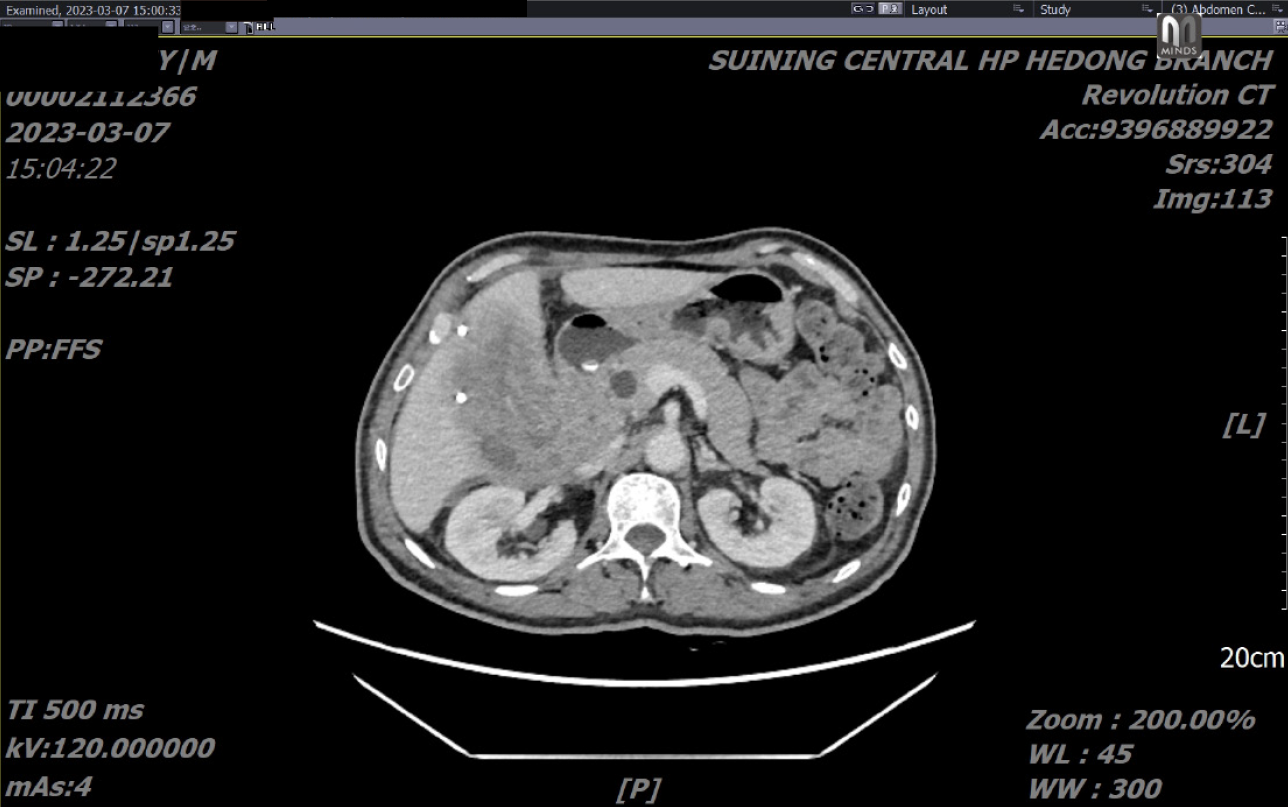
Liver abscess. Followed by abscess puncture drainage guided by color ultrasound. Approximately 100 mL of milky pus was drained, and less drainage followed. One month later, a follow-up abdominal CT scan revealed that the mass consisted mostly of solid tissue, with a small amount of cystic components (Figure 2). A biopsy of the mass was per
The preoperative diagnosis was abdominal soft tissue sarcoma stage IIb (GxT2NxM0, AJCC tumor stage 9th edition). Postoperative pathological diagnosis was "gallbladder carcinoma sarcoma".
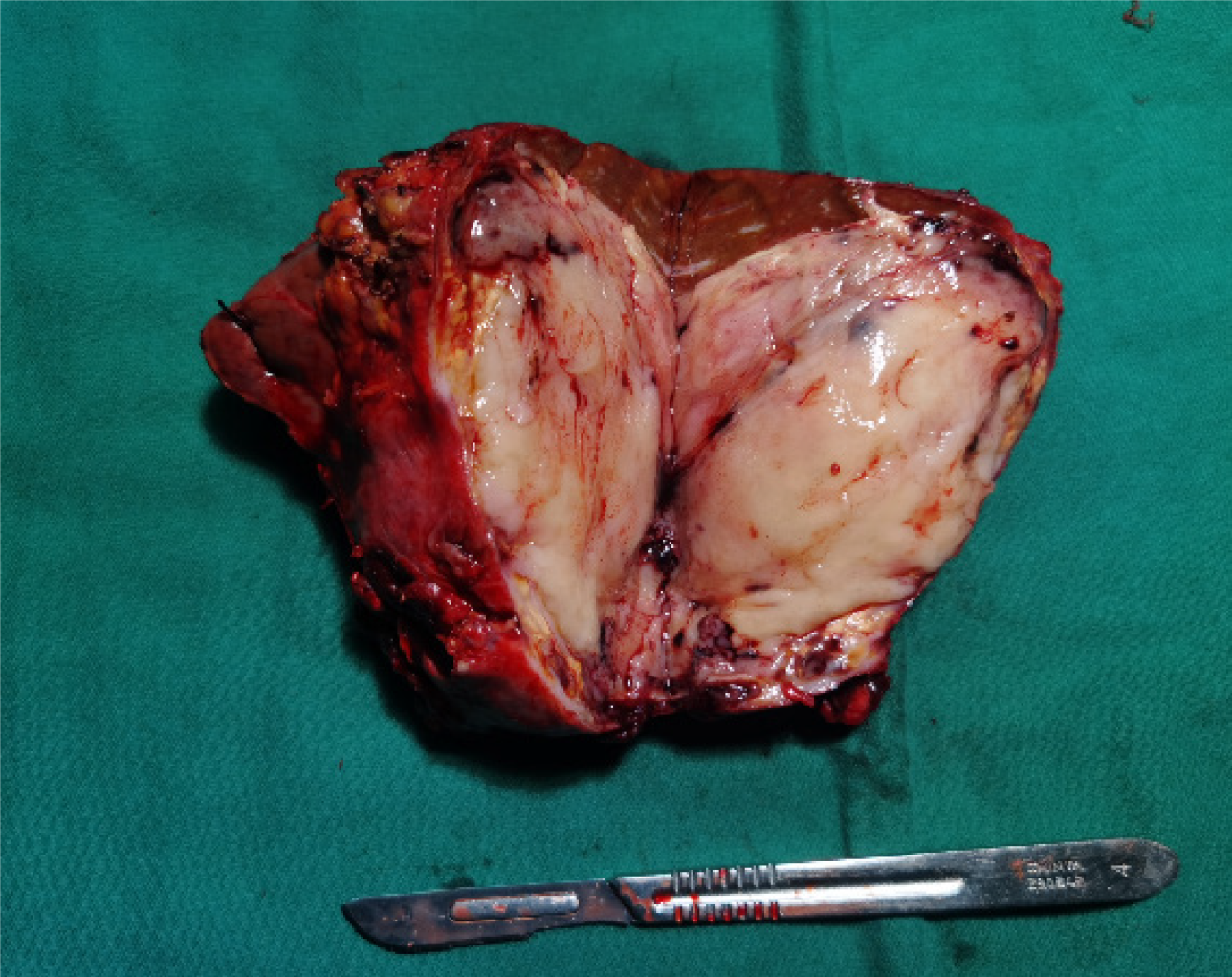
Gallbladder tumor resection was performed under general anesthesia. Intraoperatively, a small amount of light yellow ascites was observed in the abdominal cavity, and the gallbladder was adhered to the surrounding omentum. A palpable soft tissue mass was identified within the gallbladder. The tumor was found to be invading liver segments 5 and 4. Upon removal of the specimen, a section revealed that the gallbladder was filled with soft, fish-like tissue measuring approximately 8 cm × 7 cm × 5 cm. The tumor had invaded the right margin of the liver portal and the right hepatic pedicle. Gallbladder contained new fish-like tissue. Necrosis and bleeding were observed in the lesion (Figure 3).
The findings indicate a malignant gallbladder tumor involving the entire layer and adjacent liver. Extensive necrosis and vascular thrombus are present. Immunohistochemical staining demonstrates positive expression of CK(AE1/AE3) and CK19 in epithelial cells, negative expression of CK7, positive expression of SATB2 in interstitial cells, and positive expression of TLE1 in the lesion (Figure 4).
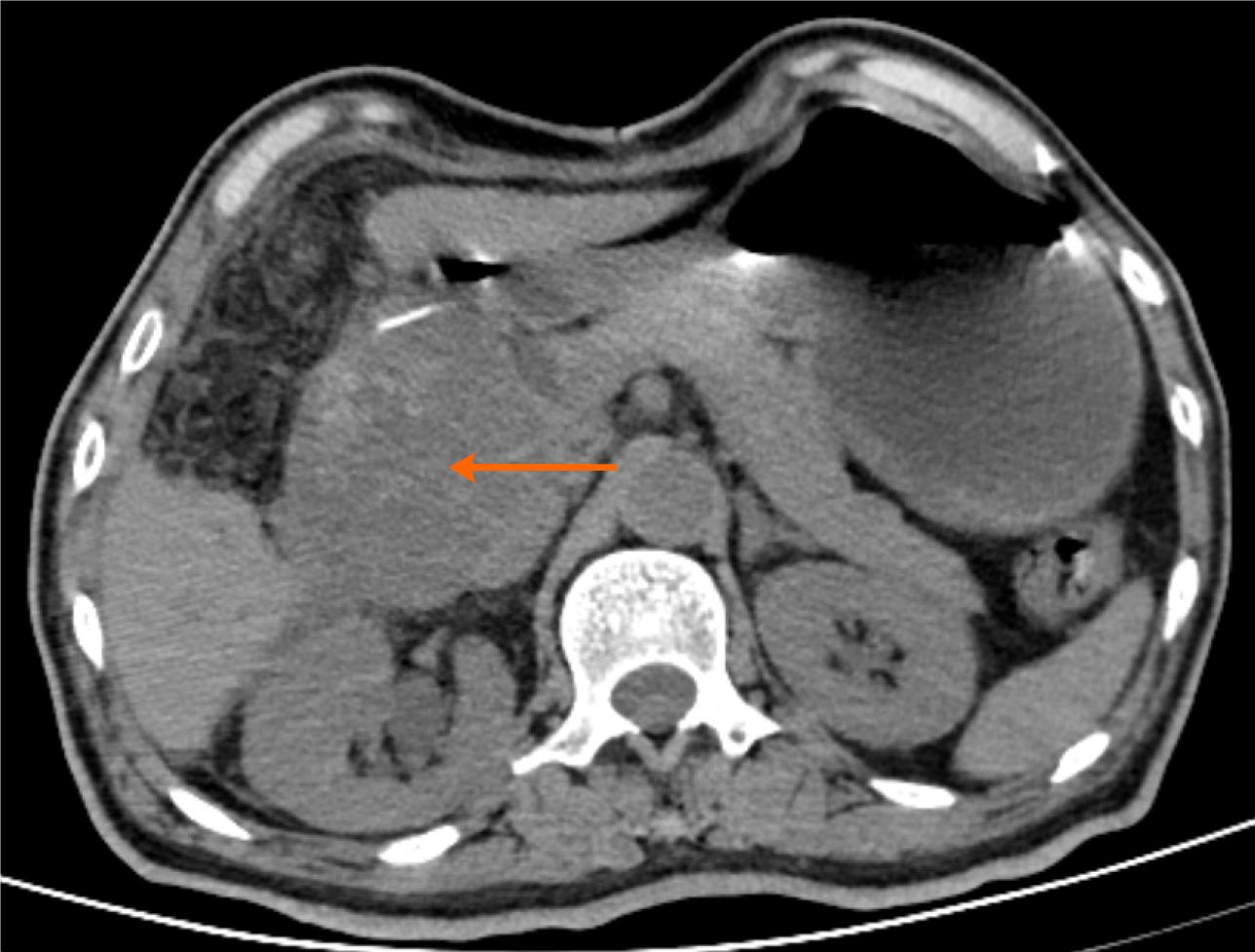
The patient experienced a smooth recovery after surgery. However, one month postsurgery, he was readmitted to the hospital due to recurrent vomiting and abdominal distension. A CT examination of the upper abdomen revealed a 9 cm × 8 cm × 8 cm mass invading the right upper abdomen, causing duodenal obstruction. Local recurrence of gallbladder carcinosarcoma with duodenal invasion was suspected (Figure 5).
To alleviate his gastrointestinal symptoms, a gastric tube was inserted to decompress the gastrointestinal tract, successfully draining approximately 500 mL of gastric fluid per day. Unfortunately, the patient declined further surgical intervention. Within seven days of readmission, a significant amount of blood was drained through the gastric tube, and the patient started to pass bloody stools. An attempted interventional embolization and hemostasis procedure was unsuccessful. Subsequently, there was another significant discharge of bright red blood through the gastric tube the following day, accompanied by the continued presence of blood in the stool. At the request of the patient and his family, no further interventions or blood transfusions were pursued. Tragically, the patient passed away two days later due to gastrointestinal bleeding and resulting hypovolemic shock.
Gallbladder carcinosarcoma is an exceptionally rare malignant tumor of the gallbladder that accounts for only approximately 1.7% of all gallbladder malignancies[1]. Most reported cases in the literature are sporadic, with a total of approximately 100 documented cases. In 1907, Landsteiner[3] reported the first recorded case of gallbladder carcinosarcoma. This tumor is distinguished by the presence of two malignant tumor components: epithelial tumor tissue and stromal sarcoma tissue.
Carcinosarcoma can also occur in other organs, including the uterus, gastrointestinal tract, lungs, pancreas, thyroid, and kidneys. Although the exact cause of this disease is not well understood, a study by Dacic et al[4] suggested that the coexistence of two distinct tumor cell types in carcinosarcoma may be attributed to the varied differentiation pathways of tumor totipotent stem cells.
Gallbladder carcinosarcoma is more frequently diagnosed in women than in men and accounts for approximately 72.4% of cases. The average age of onset was 66 years. The most commonly reported clinical manifestations include abdominal pain (76%), weight loss (29%), nausea and vomiting (25%), fever (17%), jaundice (10%), and abdominal distension (4%). Notably, a significant majority of patients had a prolonged history of gallstones (83%). Abnormal liver function is observed in 47.5% of patients, with CA19-9 (15.5%) being the most commonly elevated tumor marker[5].
In the case of this particular patient, the primary clinical symptoms were mild to moderate distending pain in the right upper abdomen and a slight increase in CA19-9, despite a lack of gallstones being detected.
The reported literature on gallbladder carcinosarcoma shows wide variation in tumor imaging sizes, ranging from 25 cm × 35 cm to 1.5 cm × 1 cm, with an average diameter of approximately 8.1 cm[6]. For the patient in our study, the initial maximum tumor diameter was approximately 9 cm × 8 cm.
Regarding magnetic resonance imaging (MRI) and CT findings, most studies describe solid space-occupying lesions within the gallbladder, with some cases demonstrating invasion of the liver and surrounding organs. Unfortunately, imaging findings often lack specific characteristics that can aid in diagnosis and differentiation. In this particular study, the initial MRI findings showed multiple liver cysts, leading to a misdiagnosis of a liver abscess, which was subsequently treated with puncture drainage. Intriguingly, a similar situation was reported by Khurram[7]. The underlying reasons for this resemblance and whether it reflects any unique tissue biochemical reactions during the growth of gallbladder carcinosarcoma in patients have not been determined. Notably, no similar incidents have been documented in the other cases reported in the literature.
Gallbladder carcinosarcoma exhibits a diverse array of compositions, manifesting in various forms, such as leiomyosarcoma, osteosarcoma, chondrosarcoma, synovial sarcoma, rhabdomyosarcoma, angiosarcoma, fibrosarcoma, etc[8-10]. In the case of this patient, positive expression of TLE1 and SATB2 indicated the presence of synovial sarcoma and osteosarcoma as the two sarcomatous components. On the other hand, the presence of keratin (CK and CK19) primarily serves as the main diagnostic basis for epithelial adenocarcinoma. It is essential for the diagnosis of carcinosarcoma that both tissue components are concurrently present.
Gallbladder carcinosarcoma exhibits biological behavior more akin to that of sarcomas and is characterized by rapid growth and insensitivity to both radiation and chemotherapy. Achieving R0 resection through surgical removal is considered the most promising treatment for ensuring long-term survival. However, the patient outcomes generally remain poor. For instance, in a study of 26 patients with gallbladder carcinosarcoma conducted by Huguet et al[11], only 3 individuals survived beyond one year. Ajiki et al[12] reported in the literature that few patients survive beyond 20 months, regardless of the treatment undertaken. Unfortunately, in the patient who underwent surgical resection, rapid tumor growth, recurrence, and complications arose from organ invasion. These circumstances further underscore the unfavorable prognosis associated with this malignant tumor.
This case report found gallbladder carcinosarcoma is a very rare disease, and its clinical manifestations, laboratory tests and imaging examinations are not specific. As a result, it is easy to be misdiagnosed before operation. Moreover, the prognosis of this disease is extremely poor, and it is prone to relapse even after surgical resection.
Provenance and peer review: Unsolicited article; Externally peer reviewed.
Peer-review model: Single blind
Specialty type: Gastroenterology and hepatology
Country/Territory of origin: China
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): B
Grade C (Good): 0
Grade D (Fair): 0
Grade E (Poor): E
P-Reviewer: Aoki H, Japan; Keeratibharat N, United States S-Editor: Gong ZM L-Editor: A P-Editor: Zhao S
| 1. | Ryś J, Kruczak A, Iliszko M, Babińska M, Wasilewska A, Limon J, Niezabitowski A. Sarcomatoid carcinoma (carcinosarcoma) of the gallbladder. Gen Diagn Pathol. 1998;143:321-325. [PubMed] |
| 2. | Lazcano-Ponce EC, Miquel JF, Muñoz N, Herrero R, Ferrecio C, Wistuba II, Alonso de Ruiz P, Aristi Urista G, Nervi F. Epidemiology and molecular pathology of gallbladder cancer. CA Cancer J Clin. 2001;51:349-364. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 545] [Cited by in RCA: 558] [Article Influence: 23.3] [Reference Citation Analysis (0)] |
| 3. | Landsteiner K. Plattenepithelkarzinom und sarkom der gallenblase in cinem falle von cholelithiasis. Zischr Klin Med. 1907;62:427-433. |
| 4. | Dacic S, Finkelstein SD, Sasatomi E, Swalsky PA, Yousem SA. Molecular pathogenesis of pulmonary carcinosarcoma as determined by microdissection-based allelotyping. Am J Surg Pathol. 2002;26:510-516. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 87] [Cited by in RCA: 77] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 5. | Mansour S, Derkach E, Abergil V, Khuri S. Carcinosarcoma of the Gallbladder: A Rare Tumor. World J Oncol. 2022;13:103-106. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Reference Citation Analysis (0)] |
| 6. | Zhang L, Chen Z, Fukuma M, Lee LY, Wu M. Prognostic significance of race and tumor size in carcinosarcoma of gallbladder: a meta-analysis of 68 cases. Int J Clin Exp Pathol. 2008;1:75-83. [PubMed] |
| 7. | Khurram R, Khamar R, Lunat R, Novelli D, Ozretić L, Chaudhary K. Gallbladder carcinosarcoma masquerading as a hepatic abscess. Radiol Case Rep. 2021;16:152-156. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 5] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 8. | Sodergren MH, Silva MA, Read-Jones SL, Hubscher SG, Mirza DF. Carcinosarcoma of the biliary tract: two case reports and a review of the literature. Eur J Gastroenterol Hepatol. 2005;17:683-685. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 29] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 9. | Gupta S, Kori C, Kumar V. Primary Carcinosarcoma of the Gall Bladder: A Rare Entity. Indian J Surg Oncol. 2016;7:101-105. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 10. | Okabayashi T, Sun ZL, Montgomey RA, Hanazaki K. Surgical outcome of carcinosarcoma of the gall bladder: a review. World J Gastroenterol. 2009;15:4877-4882. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 51] [Cited by in RCA: 47] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 11. | Huguet KL, Hughes CB, Hewitt WR. Gallbladder carcinosarcoma: a case report and literature review. J Gastrointest Surg. 2005;9:818-821. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 30] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 12. | Ajiki T, Nakamura T, Fujino Y, Suzuki Y, Takeyama Y, Ku Y, Kuroda Y, Ohbayashi C. Carcinosarcoma of the gallbladder with chondroid differentiation. J Gastroenterol. 2002;37:966-971. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 33] [Article Influence: 1.4] [Reference Citation Analysis (0)] |