Published online Sep 26, 2023. doi: 10.12998/wjcc.v11.i27.6587
Peer-review started: June 16, 2023
First decision: July 28, 2023
Revised: August 9, 2023
Accepted: August 23, 2023
Article in press: August 23, 2023
Published online: September 26, 2023
Processing time: 96 Days and 6.5 Hours
Foreign bodies in the pulmonary circulation have been documented in the literature and are typically caused by interventional procedures. However, reports of pulmonary artery foreign bodies during femoral vein puncture are rare, and there is no description of this complication from the guidewire surface flows into the pulmonary artery during a pulse ablation in a patient with atrial fibrillation.
We described a case in which a linear foreign body suddenly appeared on fluoroscopy image during pulsed ablation of atrial fibrillation. Multiposition angiography showed that the foreign body was currently lodged in the pul
Mismatches between interventional devices from different manufacturers used for femoral venipuncture may result in pulmonary artery foreign bodies.
Core Tip: A case of pulmonary artery foreign body removal during pulsed atrial fibrillation ablation was reported. This is a rare and serious complication of femoral vein puncture. Therefore, we reported this case in order to avoid a similar situation.
- Citation: Yan R, Lei XY, Li J, Jia LL, Wang HX. Removal of a pulmonary artery foreign body during pulse ablation in a patient with atrial fibrillation: A case report. World J Clin Cases 2023; 11(27): 6587-6591
- URL: https://www.wjgnet.com/2307-8960/full/v11/i27/6587.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v11.i27.6587
Foreign bodies in the pulmonary circulation have been documented in the literature and are typically caused by interventional procedures[1]. During the diagnosis and treatment of cardiovascular intervention, vascular sheath or catheter breakage may occasionally occur, and the residue in the vessel can easily float to various parts of the organ along the blood flow. Despite the low incidence, foreign body embolization can trigger serious and potentially fatal complications. Therefore, the removal of these foreign bodies, whenever possible, is recommended[2]. Herein, we described a case in which a linear foreign body suddenly appeared on imaging during pulsed ablation of atrial fibrillation. Multiposition angiography showed that the foreign body was currently lodged in the pulmonary artery but was hemodynamically stable. We then chose to use an interventional approach to remove the foreign body from the pulmonary artery. This is a rare and serious complication of atrial fibrillation ablation. Therefore, careful manipulation of the guidewire is essential to prevent a similar situation.
A 63-year-old male with a history of paroxysmal atrial fibrillation was referred to our hospital for pulse ablation.
Three years prior to presentation, the patient had palpitations and shortness of breath during intermittent activities such as walking fast or uphill, which could be relieved by rest. On July 14, 2022, the patient felt dizzy and experienced palpitations. The dynamic electrocardiogram showed paroxysmal atrial fibrillation. Therefore, he came to our hospital for diagnosis and treatment.
The patient had a 3-year history of hypertension and was currently treated with antihypertensive drugs with ideal blood pressure control. There was no other medical history. Previous carotid ultrasound indicated carotid plaque formation.
He was born in the original place, had not been to the epidemic area, had no history of smoking, drinking, and had no family genetic history.
The patient’s blood pressure was 136/72 mmHg, the respiratory rate was 18 beats per minute, the pulse was 70 beats per minute, and the temperature was 36.4 °C. The patient’s body mass index was 25.7. Physical examination of the heart, lungs, and abdomen showed no positive signs.
Laboratory tests showed no positive results.
Echocardiography showed normal cardiac morphology and structure, mild valvular regurgitation, normal left ventricular systolic function, and reduced diastolic function. Computed tomography scan of the left atrial and pulmonary vein showed enlargement of the left atrium without abnormal density in the left atrial appendage cavity.
The patient was diagnosed with paroxysmal atrial fibrillation.
A pulse ablation was the recommended treatment. After all the preparations were in place, we prepared the femoral venipuncture. We used an 11F puncture needle sheath (11F, Terumo, Japan), which was from a different manufacturer than the first time the procedure was performed. This sheath has its own guide wire and puncture needle, and the surface of the guide wire is covered by a plastic film. Although we observed the difference in the guide wire, we did not pay attention to it. During the puncture process, the plastic trocar (a part of the 11F puncture needle sheath, Terumo, Japan) became deformed due to the tortuosity of the vein and could not be smoothly delivered into the vein. We were forced to use an ordinary puncture needle (7F, Medtronic, United States) and then deliver the 11F sheath into the femoral vein through the guidewire exchange. After atrial septal puncture and a series of preoperative preparations, pulse ablation was initiated.
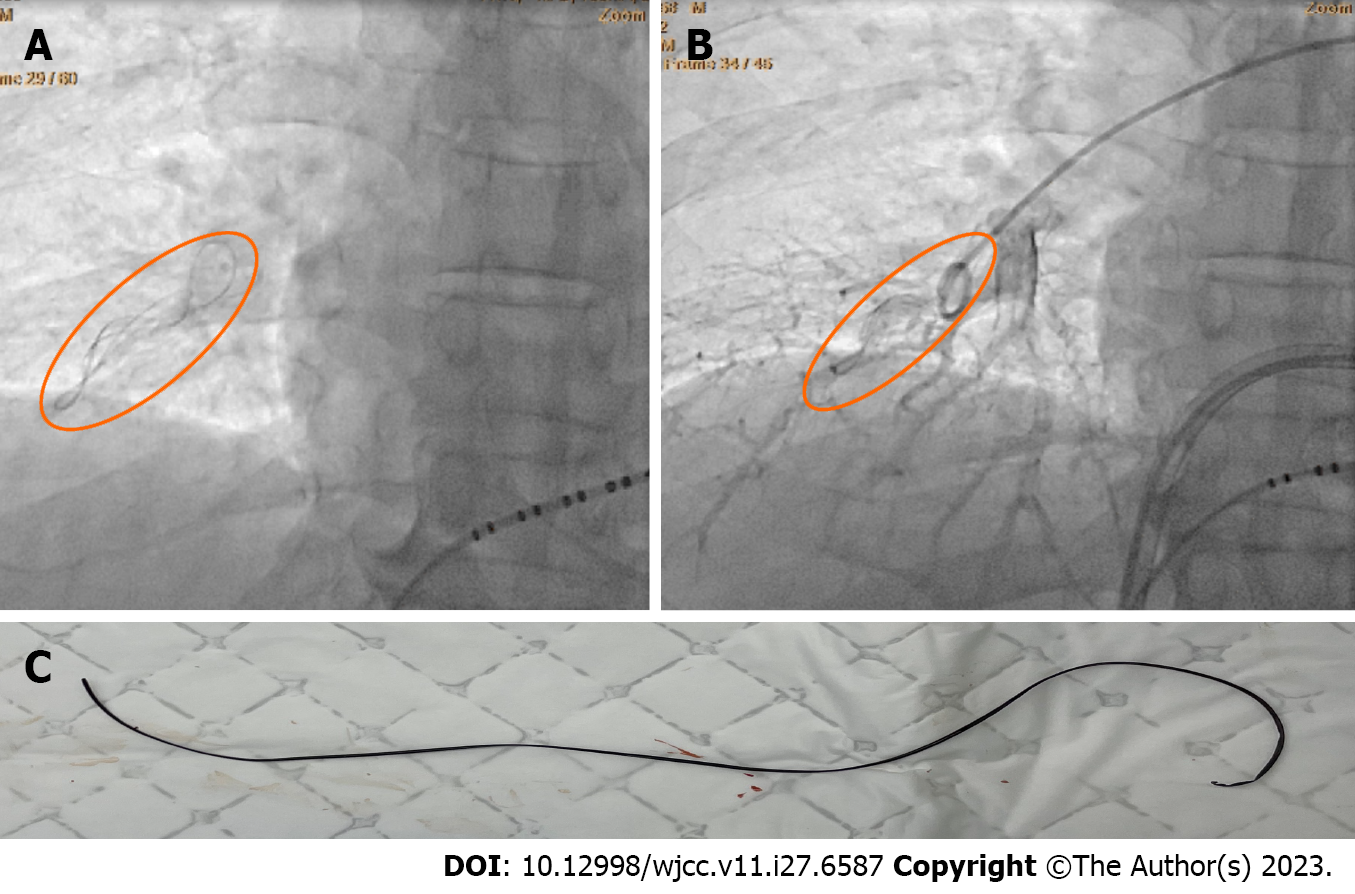
At the beginning of the ablation, we used imaging to guide the position of the ablation catheter, and there was no obvious abnormality. However, when we started to ablate the right inferior pulmonary vein, X-ray showed a linear foreign body in the field of view of the right inferior pulmonary vein, which was fixed and moved in place with the heart contraction (Figure 1A and B). During the operation, sufficient heparin was given to maintain the activated clotting time in the normal range, and the patient’s hemodynamics were stable. Therefore, we successfully completed the right pulmonary vein ablation under X-ray.
Repeated multi-angle fluoroscopy could still clearly see the foreign body without obvious abnormal movement. After excluding the interference of external substances, we immediately performed pulmonary arteriovenous angiography, which confirmed that the foreign body was from the right pulmonary artery (Video). Then the patient received percutaneous intervention for a foreign body removal. It was successfully retrieved with a trap (Shanghai Shape Memory Company, China) (Video). It was a linear substance about 15 cm in length (Figure 1C). The patient returned safely to the ward and was discharged 2 d later.
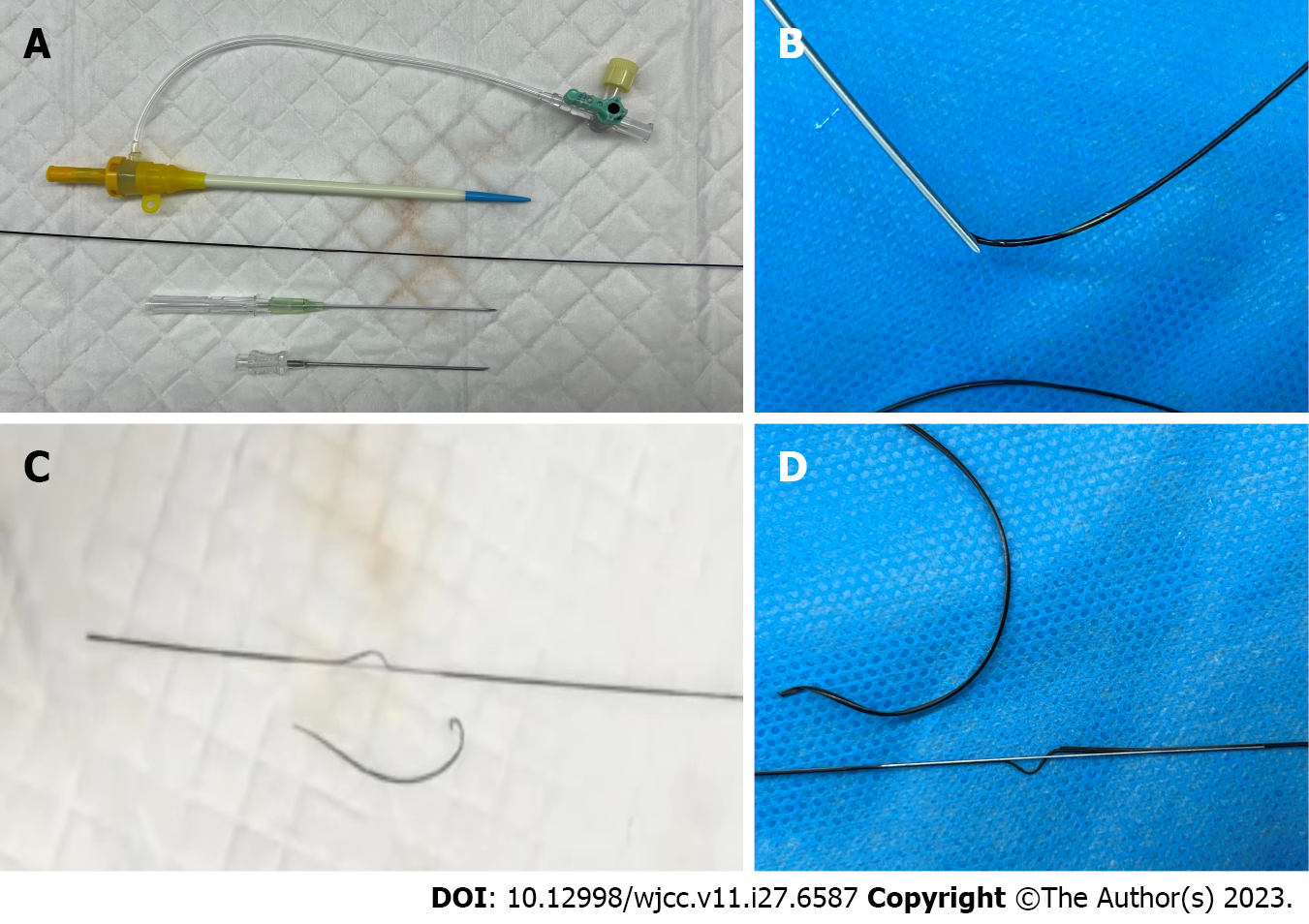
Finally, all the instruments used in the operation were retained and tested, and it was confirmed that the foreign body came from the plastic coating on the surface of the new guide wire (Figure 2A). The foreign body entered the femoral vein and followed the circulation to the pulmonary artery.
Fortunately, the foreign body was found in time during the operation and treated promptly without more serious complications, such as pulmonary embolism. After operation, low molecular weight heparin was injected subcutaneously to prevent thrombosis.
Pulse ablation of atrial fibrillation was successfully completed, and no atrial fibrillation occurred during postoperative follow-up.
The reason why the plastic coating was able to enter the femoral vein was recalled repeatedly. It was considered that the mismatch between the traditional metal puncture needle and the new guide wire used at that time might be related. When the ordinary metal puncture needle and the guide wire were at an angle in the blood vessel and the blood return was not smooth and needed to be withdrawn, the surgeon chose to withdraw the guide wire first, so that the tip of the needle cut off the plastic coating on the surface of the guide wire, resulting in the creation of the foreign body (Figure 2B-D, Video).With the blood flow through the venous system, it gradually entered the right atrium and right ventricle and then flowed into the pulmonary artery. However, these events may have been avoided if the needle had been withdrawn first.
The formation of a foreign body in the pulmonary artery during atrial fibrillation ablation has not been reported in the domestic and foreign literature. In the previous literature, the formation of a foreign body in the pulmonary artery was mostly related to trauma or interventions[3]. Although small foreign bodies may not cause complete pulmonary embolism temporarily, they can lead to intimal thickening and fibrosis and gradually lead to severe embolism. Therefore, once the diagnosis is clear, it should be treated[4]. Percutaneous extraction of embolized catheters using femoral venous access is the gold standard. The right femoral venous access is preferred because it has a high success rate[5].
Although our case was successful, this is a lesson to remember that it is essential to be good at observing, understanding the characteristics of each type of puncture needle sheath, reading the instructions carefully, and complying with the operating procedures strictly. In addition, mismatches between interventional devices from different manufacturers used for femoral venipuncture may result in pulmonary artery foreign bodies.
Provenance and peer review: Unsolicited article; Externally peer reviewed.
Peer-review model: Single blind
Specialty type: Cardiac and cardiovascular systems
Country/Territory of origin: China
Peer-review report’s scientific quality classification
Grade A (Excellent): A
Grade B (Very good): 0
Grade C (Good): 0
Grade D (Fair): D
Grade E (Poor): 0
P-Reviewer: Mishra AK, United States; Quesada A, Spain S-Editor: Chen YL L-Editor: Filipodia P-Editor: Chen YL
| 1. | Ciarrocchi AP, Parisi AM, Campisi A, Mazzarra S, Argnani D, Congiu S, Sanna S, Stella F. A strange case of foreign body embolism in the right lower pulmonary artery. Gen Thorac Cardiovasc Surg. 2021;69:894-896. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 9] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 2. | Leite TFO, Pazinato LV, Bortolini E, Pereira OI, Nomura CH, Filho JMDML. Endovascular Removal of Intravascular Foreign Bodies: A Single-Center Experience and Literature Review. Ann Vasc Surg. 2022;82:362-376. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 10] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 3. | Actis Dato GM, Aidala E, Zattera GF. Foreign bodies in the heart: surgical or medical therapy? Ann Thorac Surg. 1999;68:291-292. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 4. | Du ZZ, Ren H, Song JF. Surgical treatment of pulmonary embolism. Zhongguo Yixue Zazhi. 2006;86:197-199. [DOI] [Full Text] |
| 5. | Motta Leal Filho JM, Carnevale FC, Nasser F, Santos AC, Sousa Junior Wde O, Zurstrassen CE, Affonso BB, Moreira AM. Endovascular techniques and procedures, methods for removal of intravascular foreign bodies. Rev Bras Cir Cardiovasc. 2010;25:202-208. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 17] [Article Influence: 1.2] [Reference Citation Analysis (0)] |