Published online May 26, 2023. doi: 10.12998/wjcc.v11.i15.3578
Peer-review started: January 5, 2023
First decision: February 8, 2023
Revised: February 16, 2023
Accepted: April 14, 2023
Article in press: April 14, 2023
Published online: May 26, 2023
Processing time: 140 Days and 1.8 Hours
Massive intragastric clotting (MIC) makes endoscopic therapy difficult in patients with acute upper gastrointestinal bleeding. Literature data on how to address this problem are limited. Here, we report on a case of massive stomach bleeding with MIC that was successfully treated endoscopically using an overtube of single-balloon enteroscopy.
A 62-year-old gentleman with metastatic lung cancer was admitted to the intensive care unit due to tarry stools and hematemesis of 1500 mL of blood during hospitalization. Emergent esophagogastroduodenoscopy revealed massive blood clots and fresh blood in the stomach with evidence of active bleeding. Bleeding sites could not be observed even by changing the patient’s position and aggressive endoscope suction. The MIC was successfully removed using an overtube connected with a suction pipe, which was inserted into the stomach with an overtube of a single-balloon enteroscope. An ultrathin gastroscope was also introduced through the nose into the stomach to guide the suction. A massive blood clot was successfully removed, and an ulcer with oozing bleeding at the inferior lesser curvature of the upper gastric body was revealed, facilitating endoscopic hemostatic therapy.
This technique appears to be a previously unreported method to suction MIC out of the stomach in patients with acute upper gastrointestinal bleeding. This technique could be considered when other methods are not available or if they fail to remove massive blood clots in the stomach.
Core Tip: It is difficult to deal with massive intragastric clotting (MIC) in the stomach in acute upper gastrointestinal bleeding (UGIB). We suggest a new and simple way to deal with acute UGIB with massive intragastric clotting when the suction of the endoscope can’t remove it with common materials found in the endoscope department. An ultrathin electronic gastroscope was inserted through the nose to provide vision and an over tube of single-balloon enteroscope was inserted into the mouth to suction the massive blood clots out with a negative pressure of 2 kPa. This is a good way to provide a visual field and to stop bleeding in UGIB when other methods are not available or are unhelpful.
- Citation: Liu SX, Shi B, Liu YF, Shan JY, Sun B. Promising way to address massive intragastric clotting in patients with acute upper gastrointestinal bleeding: A case report. World J Clin Cases 2023; 11(15): 3578-3582
- URL: https://www.wjgnet.com/2307-8960/full/v11/i15/3578.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v11.i15.3578
Acute upper gastrointestinal bleeding (UGIB) is a commonly encountered emergency associated with high morbidity and mortality. Peptic ulcers are the most common cause of acute UGIB. A clear view of the gastrointestinal tract is vital to finding the bleeding site and conducting hemostatic therapy, especially in patients whose UGIB leads to massive intragastric clotting (MIC). In UGIB, approximately 13% of endoscopic exams have an unclear visual field, and new lesions are found in near-term gastroscopic reexamination in 41% of patients. Moreover, a poor endoscopic visual field is positively correlated with rebleeding and mortality[1]. Herein, we report on a method of using an overtube for single-balloon enteroscopy to remove the MIC, and this technique provided a clear view of a bleeding ulcer that was successfully managed via endoscopic hemostasis.
A 62-year-old gentleman was admitted to the intensive care unit (ICU) for persistent hematemesis and unstable hemodynamics.
He had four attacks of hematemesis (approximately 1500 mL of blood) that occurred within 24 h of hospitalization.
The patient had a history of adenocarcinoma of the lung and underwent radical resection of pulmonary carcinoma in July 2020. The latest computed tomography (CT) scan in October 2022 revealed multiple solid nodules and lymphadenopathy in the mediastinum consistent with tumor metastasis. He underwent upper endoscopy in June 2020, which revealed erosive gastritis. He denied any history of hypertensive disease, blood coagulation disorders, or chronic liver disease.
The patient denied a family history of gastric cancer.
In the ICU, the patient was hemodynamically unstable (pulse of 102 bpm, blood pressure of 95/60 mmHg) during anti-shock treatment. He was afebrile, with a respiratory rate of 25 rpm and an oxygen saturation of 95%. His abdomen was nondistended with hyperactive bowel sounds. There was no hepatosplenomegaly or palpable abdominal mass.
Complete blood cell count revealed a hemoglobin level of 42 g/L and a platelet level of 91 × 109/L. The patient had poor coagulation function with fibrinogenopenia (< 1 g/L), metabolic acidosis, and hypoproteinemia. A strongly positive fecal occult blood test was observed before hospitalization in outpatient care.
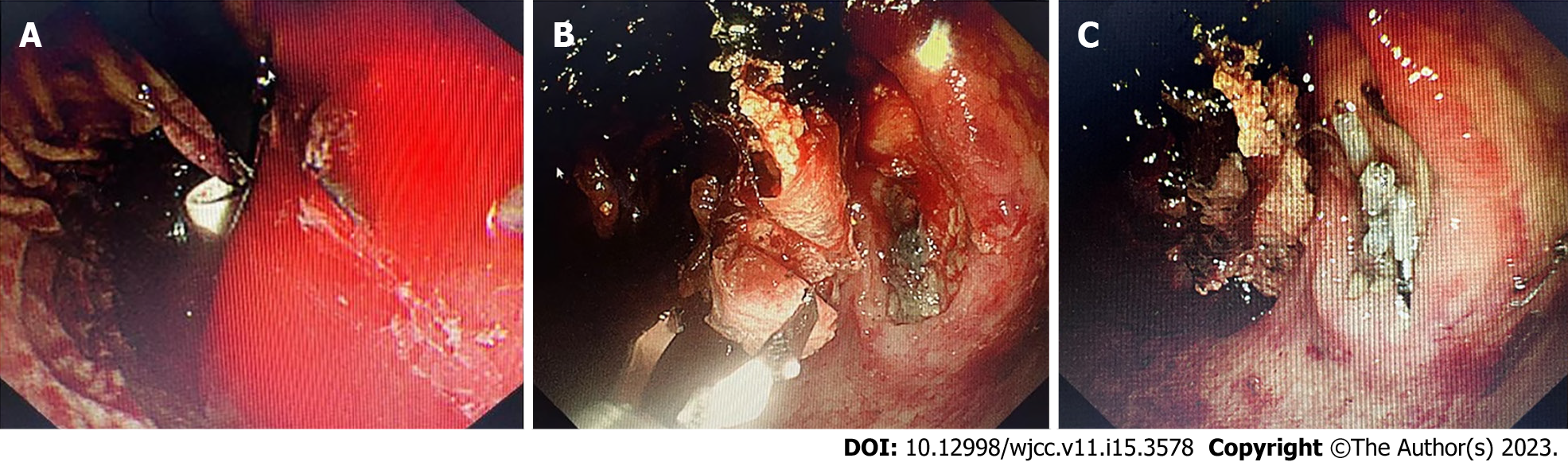
After blood transfusion and fluid resuscitation, 80 mg of omeprazole was administered intravenously. Emergent esophagogastroduodenoscopy (EGD) was performed after airway intubation. A massive amount of blood clots and fresh blood with evidence of active bleeding were observed in the stomach. The blood clots could not be aspirated by the endoscope or removed by disposable mesh. The bleeding site could not be seen due to the poor field of vision due to active bleeding, even after changing the patient’s position (Figure 1A). To remove the blood clot, a single-balloon enteroscope loaded with an overtube was introduced into the stomach, and the enteroscope was withdrawn. An ultrathin gastroscope (5 mm in diameter GIF-XP260 N Olympus, Japan) was inserted into the stomach through the nose to monitor the suction. The overtube was connected to suction with a pressure of 2 kPa to suction the MIC and fresh blood (Figure 1A, Video 1), after which a 2.0 cm × 1.5 cm ulcer with oozing bleeding was finally observed at the inferior lesser curvature of the upper stomach body (Figure 1B).
After successfully removing the blood clots, the ultrathin gastroscope and the overtube were withdrawn, and an epinephrine solution (1:20000) was injected around the ulcer. Three hemostatic clips were deployed at the bleeding site and successfully stopped the bleeding (Figure 1C).
The final diagnosis was acute upper GI bleeding due to a gastric ulcer (likely a metastatic malignancy).
The patient’s condition became stable after endoscopic hemostasis. A total of 400 mL of plasma, 4 units of red blood cell suspension and 2 units of cryoprecipitate were transfused. Calcium gluconate was used to rectify the patient’s metabolic acidosis. Three milligrams of somatostatin was used to stop the bleeding.
There was no evidence of active bleeding after endoscopic treatment, and a follow-up EGD was scheduled. The follow-up gastroscopic pathological examination indicated adenocarcinoma.
There are few studies evaluating the efficacy of clearing MIC in UGIB. Some available information about removing blood clots in the stomach can be acquired from case reports and small case series. Controlled trials have not been reported. As a result, there is no proven, absolutely superior treatment modality for clearing MIC. We present a case showing successful sweeping of the MIC away using an overtube designed for single-balloon enteroscopy. Our experience may reinforce the selection of the best, most effective modality and aid in creating guidelines for the management of UGIB.
Shi[2] and Cai et al[3] reported 23 and 18 UGIB patients with MIC, respectively, and they cleared the MIC using a gastric washing machine. The front of the flushing pipe of the gastric washing machine was connected with a string, and foreign forceps were inserted through the working channel of a gastroscope to grip the string of the flushing pipe. By using this method, the flushing pipe was introduced into the stomach with the gastroscope. The gastric washing machine was switched on to flush repeatedly until the stomach was clean and the bleeding spots were exposed. Zhou et al[4] and Xiong et al[5] reported a 12-patient and a 3-patient series with UGIB, and they took a similar approach to fix a suction tube on the endoscope and enter the stomach to suction the MIC out. Zhang et al[6] used a biopsy channel-accessible net with the function of suction; then, food residue was hitched and dragged out together with an endoscope to expose the hemorrhagic spot.
In our case, the patient’s attending doctor called the endoscopist first (due to the massive bleeding) and then performed CT-angiography to locate and stop the bleeding in case of hemostasis failure by the endoscopists. During the endoscopy, we changed the patient’s position, but the site of bleeding could not be identified. We failed to use common mesh to hitch and drag the MIC out. To remove huge blood clots that were continuously created due to active bleeding, we tried an overtube of single-balloon enteroscopy. Our method, when compared to the methods reported above, requires few preparations and does not require a flushing pipe or suction tube on the endoscope. The maneuverability of the overtube is probably more convenient than using a regular gastroscope fixed with a flushing pipe or suction tube. However, methods previously described can settle MIC using only an endoscope and a suction tube, and our method requires an ultrathin gastroscope to monitor suction and adjust the overtube position.
It is difficult to judge which method is better because of the lack of clinical studies. Our case can contribute to strengthening the acceptance of endoscopic therapeutic modalities, especially UGIB with MIC, which lacks a fully evaluated and established best treatment modality.
When a large amount of blood and MIC are encountered in the stomach during emergency endoscopy, rapid clearance of the intragastric blood clot is essential to provide a clear view and find the bleeding site in time. Using an overtube of single-balloon enteroscopy to suction massive blood clots out could be considered when other methods are not available or are unhelpful.
Provenance and peer review: Unsolicited article; Externally peer reviewed.
Peer-review model: Single blind
Specialty type: Emergency medicine
Country/Territory of origin: China
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): B
Grade C (Good): 0
Grade D (Fair): D
Grade E (Poor): 0
P-Reviewer: Ferreira GSA, Brazil; Paparoupa M, Germany S-Editor: Ma YJ L-Editor: Filipodia P-Editor: Yu HG
| 1. | Stollman NH, Putcha RV, Neustater BR, Tagle M, Raskin JB, Rogers AI. The uncleared fundal pool in acute upper gastrointestinal bleeding: implications and outcomes. Gastrointest Endosc. 1997;46:324-327. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 37] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 2. | Shi RY. [Application and nursing of endoscopic entogastric blood cleaning in acute upper gastrointestinal hemorrhage]. Zhonghua Xiandai Huli Zazhi. 2007;13:1605-1606. [DOI] [Full Text] |
| 3. | Cai XY, Zhu HM, Song Y, Wang F. [Application of Endoscopic Endogastric Blood Cleaning in Acute Upper Gastrointestinal Hemorrhage]. Xiandai Zhenduan Yu Zhiliao. 2006;5:304-305. [DOI] [Full Text] |
| 4. | Zhou SY, Duan ZH. [The effect of suction tube combined with gastroscopy on the removal of massive blood clots during upper gastrointestinal bleeding]. Zhongguo Zhongxiyi Jiehe Xiaohua Zazhi. 2019;27:474-475. [DOI] [Full Text] |
| 5. | Xiong KW, Cheng SL, Yang J, Jin HB, Zhang XF. [Three cases of upper gastrointestinal hemorrhage were treated by suction tube combined with endoscopy]. Zhonghua Xiaohua Neijing Zazhi. 2019;2:140-141. [DOI] [Full Text] |
| 6. | Zhang P, Jiang J, Ma XY, Zhou W, Li XY, Chen L, Qi LP, Wang JF, Yuan F. [Application of suction mesh in endoscopic diagnosis and treatment of massive upper gastrointestinal bleeding]. Zhongguo Zhongxiyi Jiehe Xiaohua Zazhi. 2013;21:314-315. [DOI] [Full Text] |