Published online Jul 6, 2022. doi: 10.12998/wjcc.v10.i19.6688
Peer-review started: January 13, 2022
First decision: April 8, 2022
Revised: April 15, 2022
Accepted: May 17, 2022
Article in press: May 17, 2022
Published online: July 6, 2022
Processing time: 162 Days and 4.5 Hours
Morbihan disease is a rare cutaneous disorder characterized by non-pitting edema and erythema of the upper two-thirds of the face. In severe cases, orbital and facial contour changes may affect the visual field, and there is no guideline for the standard treatment of this disease. Existing treatment methods have been reported to be associated with long medication cycle, easy recurrence after drug withdrawal, and multiple adverse reactions.
A 55-year-old Chinese woman presented to our hospital with non-pitting edema and erythema of the upper two thirds of her face for 5 mo. Physical examination showed obvious edema and erythema on the upper face. The boundary was unclear, the lesions were hard and non-pitting, and infiltration was obvious by touch. Pathological examination revealed mild hyperkeratosis of the epidermis, nodular inflammatory lesions in the dermis, epithelioid granuloma, and inflammatory cell infiltration with lymphocytes and histiocytes around skin appendages and blood vessels. Alcian blue staining, acid fast staining, silver staining and periodic acid-Schiff staining were negative. The patient was diagnosed with Morbihan disease. She was treated with prednisone acetate and tripterygium wilfordii polyglycoside tablets for 4 mo, and the edema was slightly reduced, but transaminase levels were significantly increased. Compound glycyrrhizin capsules were administered for liver protection for 1 mo; however, facial edema did not significantly improve and transaminase levels continued to increase. Total glucosides of paeony capsules were then administered for 4 mo, and transaminase level returned to normal and the patient’s facial edema disappeared completely.
Total glucosides of paeony has a remarkable effect in Morbihan disease, without adverse reactions.
Core Tip: Morbihan disease is a rare skin disease characterized by non-pitting edema and erythema of the upper two-thirds of the face. The orbital and facial contour changes can affect the field of vision and cause disfiguring damage if not treated in time. The specific pathogenesis is unclear, and there is no standard treatment guideline for this disease. Thus, it is necessary to identify a safe and effective treatment. We treated a case of Morbihan disease with total glucosides of paeony and achieved very good results with no adverse reactions. The treatment of Morbihan disease with total glucosides of paeony has not previously been reported.
- Citation: Zhou LF, Lu R. Successful treatment of Morbihan disease with total glucosides of paeony: A case report. World J Clin Cases 2022; 10(19): 6688-6694
- URL: https://www.wjgnet.com/2307-8960/full/v10/i19/6688.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v10.i19.6688
Morbihan disease, also known as Morbihan syndrome, is a rare skin disease named by Gorin et al[1] in 1991, with only a few sporadic cases reported worldwide. The main clinical manifestations are edema and erythema of the upper two-thirds of the face without obvious discomfort. Development of the disease can cause malformation and visual field defects, affecting patients’ quality of life[2]. Therefore, early diagnosis and treatment are of great significance. Currently, there is no standard treatment for Morbihan disease. We describe a 55-year-old female patient who received total glucosides of paeony for this rare disease with good efficacy and no adverse reactions.
A 55-year-old female patient presented to our Department of Dermatology with non-pitting edema and erythema of the upper two-thirds of the face for 5 mo.
The patient had edema and erythema of the upper two-thirds of the face 5 mo ago, and there was no itching or discomfort related to the skin lesions. The patient had previously been treated in two hospitals, where the doctors considered her condition considered to be caused by an allergy and treated her with antihistamines, but this treatment was ineffective. The primary skin lesions gradually became worse.
The patient was previously healthy and denied any history of acne, rosacea, erysipelas, allergies, diabetes, or other diseases.
The patient denied genetic diseases, and there was no similar disease in the family.
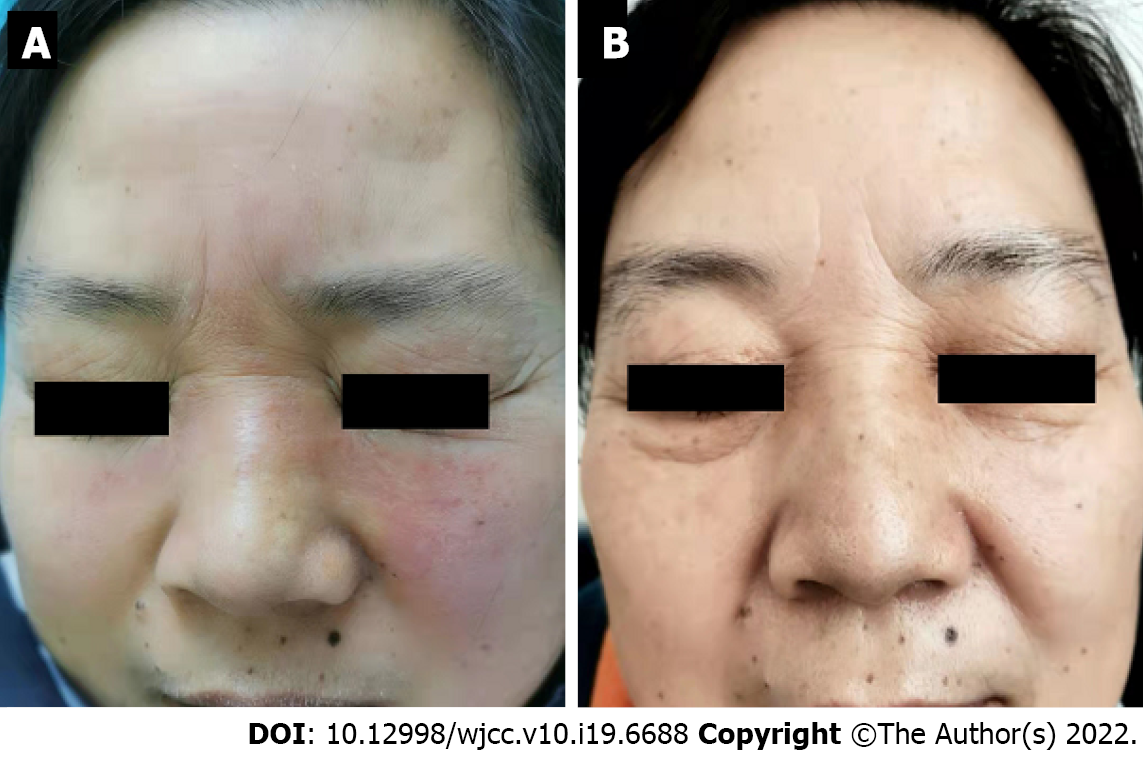
On physical examination, temperature, pulse, respiration, and blood pressure were normal. Examination of the heart, lungs, abdomen, and nervous system showed no abnormalities. Dermatological findings showed obvious edema and erythema on the forehead, between the eyebrows, and on both eyelids, nose, and both cheeks. The skin lesions were hard and non-pitting, and had unclear boundaries and obvious infiltration by touch (Figure 1A). The rest of the skin showed no abnormalities. No visual field damage was observed.
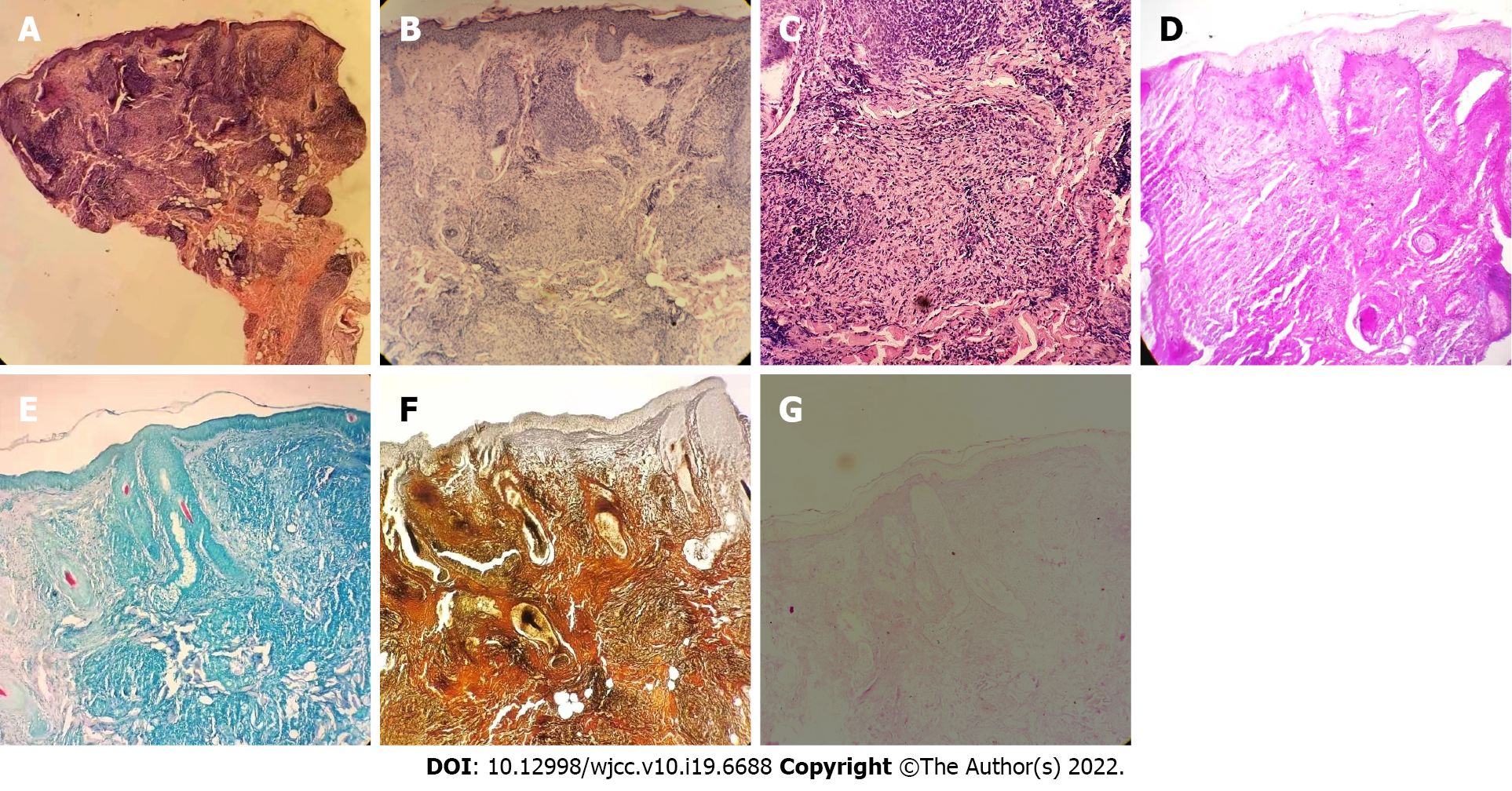
Routine blood tests, renal function, and electrolytes were all within the normal range. Routine urine test showed positive occult blood (1+), and other values were normal. The tuberculin test, antinuclear antibody spectrum, and anti-double stranded DNA antibody were negative. All immunological indicators were normal. Liver function analysis showed that alanine aminotransferase (ALA) was 44 U/L, and other values were normal. Histopathological examination of skin lesions on the left side of the face revealed mild hyperkeratosis of the epidermis, nodular inflammatory lesions in the dermis, epithelioid granuloma, and inflammatory cell infiltration dominated by lymphocytes and histiocytes around skin appendages and blood vessels (Figure 2A-C). Alcian blue staining, acid fast staining, silver staining, and periodic acid-Schiff (PAS) staining were all negative (Figure 2D-G).
A chest X-ray showed no abnormalities.
The patient was diagnosed with Morbihan disease.
Facial edema was significantly reduced after treatment with prednisone acetate tablets 20 mg/d for 1 mo. When prednisone acetate was reduced to 10 mg/d for 2 mo, facial edema increased. Prednisone acetate was discontinued, and tripterygium wilfordii polyglycoside tablets were prescribed at 6 tablets/d. After 4 mo of this treatment, facial edema was slightly relieved. Liver function examination showed that ALA was 73 U/L and aspartate aminotransferase (ASA) was 56 U/L, both of which were higher than the values before treatment. Elevated aminotransferase was found to be caused by tripterygium wilfordii polyglycoside, thus oral liver-protecting compound glycyrrhizin at 225 mg/d was initiated. After 1 mo of treatment, facial edema did not significantly improve, and liver function reexamination showed that ALA (86 U/L) and ASA (62 U/L) levels were still high. Therefore, oral administration of tripterygium wilfordii polyglycoside and compound glycyrrhizin was discontinued, and total glucosides of paeony capsules at 0.6 g 3 times/day were prescribed. After 1 mo of treatment, facial edema was significantly reduced. Liver function reexamination showed that ALA was 69 U/L and ASA was 58 U/L, both of which were decreased. After another mo of treatment with total glucosides of paeony capsules, liver function reexamination showed that ALA was 47.31 U/L and ASA was 37.35 U/L, both of which returned to normal and facial edema was further alleviated. After subsequent 2 mo of maintenance treatment with total glucosides of paeony capsules, facial edema completely disappeared (Figure 1B), and liver function indexes returned to normal.
Facial edema disappeared completely after 4 mo of treatment with total glucosides of paeony. The patient was followed for almost 1 year and was in good physical condition without facial edema.
The specific potential cause of Morbihan disease is unclear, and some scholars believe that it is a rare complication of acne[3]. Some researchers suggest that it is related to rosacea[4,5], and its pathogenesis may be related to chronic inflammation, which affects lymphatic reflux and leads to local skin edema[6]. Recent studies have suggested that edema may be associated with non-insulin-dependent diabetes mellitus[7,8]. Our patient had no history of acne, rosacea, or diabetes, and the specific cause of the disease was unclear.
The histopathology of this disease is mainly non-specific inflammation, which is manifested by telangiectasis and infiltration of inflammatory cells such as lymphocytes around hair follicles and blood vessels[9], and granulomatous tissue can also be seen in a few cases[2]. The histopathological findings of the skin lesions in the present patient were nodular inflammatory lesions in the dermis, epithelioid granuloma, and inflammatory cell infiltration dominated by lymphocytes and histiocytes around skin appendages and blood vessels. This is consistent with the existing case reports of Morbihan disease[4,10-12].
This disease should be distinguished from angioedema, dermatomyositis, lupus erythematosus, chronic actinic dermatitis, skin tuberculosis, and sarcoidosis. The present patient had no history of allergy or family inheritance. The skin lesions showed infiltrating edema, which did not subside within a short time, and pruritus was not observed. Eosinophils were not increased, and antihistamine treatment was ineffective, which excluded angioedema. The patient had no violet erythema on the eyelids, no fatigue, no muscle soreness, no specific Gottron papules on the dorsal joints of the limbs, and no immunological positive indicators, and histopathology did not show liquefaction degeneration of basal cells or mucin deposition in the dermis, which excluded dermatomyositis. The patient's skin lesions were not butterfly erythema, without hair follicle horn plug and adherent scales, without light sensitivity, and with no abnormal immunological indicators and no mucin deposition in the dermis, which ruled out lupus erythematosus. The patient had no mossy lesions, no pruritus, no history of long-term outdoor exposure, and no light sensitivity; therefore, chronic actinic dermatitis was ruled out. The tuberculin test was negative, and lung examination showed no abnormalities; acid-fast staining, silver staining, and PAS staining were negative, and histopathology showed no caseous necrosis, thus excluding skin tuberculosis. The patient's lung was normal and histopathological findings showed no tuberous granuloma; therefore, sarcoidosis was ruled out. The patient presented with chronic non-pitting edema of the upper two-thirds of the face and no pruritus in the edematous area. Histopathology showed non-specific inflammation, and the final diagnosis was Morbihan disease.
In terms of the treatment of Morbihan disease, a review of the existing literature showed that most cases were treated with glucocorticoids and tetracycline antibiotics[10], and thalidomide treatment has also been reported[13]. The latest report shows that good results were achieved with isotretinoic acid combined with ketotifen for the treatment of Morbihan disease[14]. Glucocorticoids, tetracycline antibiotics, thalidomide, and isotretinoic acid agents have been reported to have direct or indirect anti-inflammatory effects, indicating that anti-inflammation is a very important treatment in this disease. The histopathological findings of nonspecific inflammation in Morbihan disease seem to support this.
Existing treatment methods for Morbihan disease have shortcomings such as long treatment cycle, disease recurrence after drug withdrawal, and multiple side effects. In the present case, the patient was treated with a glucocorticoid in the early stage, and inflammation was controlled within a short period. However, the disease recurred after reduction of the hormone, indicating that it is difficult to achieve a complete cure with only anti-inflammatory treatment. In addition to anti-inflammatory treatment, it is necessary to eliminate the initial factors causing inflammation. The clinical characteristics of this disease include chronic recurrence. Isotretinoic acid treatment of this disease has achieved good results, and analysis has found that isotretinoic acid has both anti-inflammatory and immunomodulatory effects, suggesting that inflammation in this disease may be related to immunity. The major disadvantages of isotretinoic acid are the occurrence of adverse reactions after long-term use, and patient’s poor tolerance. There are reported cases of tripterygium wilfordii treatment achieving good results[15]. Our patient also received tripterygium wilfordii treatment, but developed elevated transaminase levels during treatment, and finally had to terminate tripterygium wilfordii. Therefore, it was necessary to identify an effective drug with few side effects.
Total glucosides of paeony is a Chinese patent medicine, which is extracted from Radix paeoniae alba and have anti-inflammatory[16], anti-organ injury[17], and immune regulation effects[18]. Total glucosides of paeony was approved by the China Food and Drug Administration for the treatment of rheumatoid arthritis in 1998, and its clinical therapeutic effect is remarkable[19]. In addition, total glucosides of paeony has been shown to be effective in the treatment of psoriasis[20], Sjogren's syndrome[21], and other autoimmune diseases. Studies have shown that total glucosides of paeony combined with other drugs has obvious advantages in treating autoimmune diseases, which can significantly alleviate the symptoms of patients and reduce the side effects of drugs. Some researchers used total glucosides of paeony combined with methotrexate (MTX) and leflunomide in the treatment of rheumatoid arthritis, which significantly reduced the toxic effect on the liver[22]. Feng et al[23] used total glucosides of paeony combined with MTX in the treatment of rheumatoid arthritis, and its efficacy was superior to that of MTX alone[23]. It has been shown that total glucosides of paeony plays an important role in multiple processes of autoimmune diseases, and inhibits the maturation of dendritic cells by selectively blocking the activation of the TLR4/5 signaling pathway in order to avoid immune-mediated inflammation[24]. In view of the significant effect of total glucosides of paeony on chronic inflammatory autoimmune diseases, the patient in this report was treated with total glucosides of paeony capsules, and the effect was obvious with no adverse reactions, and there was no recurrence after almost 1 year of drug withdrawal. The adverse reactions of total glucosides of paeony are rare, and the reported adverse reactions are only mild diarrhea[25]. According to the literature, diarrhea is the most likely adverse reaction of total glucosides of paeony in the treatment of Morbihan disease.
The pathophysiological mechanism of Morbihan disease is not fully understood. There is a relatively consistent view among researchers that edema in Morbihan disease is mainly caused by lymphatic obstruction or poor lymphatic return due to inflammation[26]. Studies have shown that the nitric oxide signaling pathway may be involved in the destruction of the integrity of lymphatic vessels[7], and total glucosides of paeony can effectively inhibit the production of nitric oxide and other inflammatory factors in macrophages in the rheumatoid arthritis model[27], and can play an anti-inflammatory role by inhibiting the activation and recruitment of inflammatory cells[28]. Therefore, it is speculated that the mechanism of total glucosides of paeony in the treatment of Morbihan disease is to maintain the integrity of lymphatic vessels and prevent the occurrence of edema through the similar anti-inflammatory mechanism mentioned above.
Morbihan disease is rare, and only one case has been reported in China to date. Therefore, it is difficult to carry out research on the multi-center large-sample treatment at present. However, the report of an effective treatment strategy in a single case may still be helpful in treating patients with Morbihan disease and in further study of this disease.
Morbihan disease is rare, and no standard treatment is currently available. Reported treatments for Morbihan disease have shortcomings such as long medication cycle, disease recurrence after drug withdrawal, and many side effects. This patient was treated with total glucosides of paeony with good effects and no adverse reactions. The patient was followed for almost 1 year without recurrence, suggesting that total glucoside of paeony is an effective agent for Morbihan disease. To our knowledge, this is the first reported case of Morbihan disease treated with total glucosides of paeony with good results.
We sincerely thank all the medical staff who were involved in the treatment of this patient.
Provenance and peer review: Unsolicited article; Externally peer reviewed.
Peer-review model: Single blind
Specialty type: Medicine, research and experimental
Country/Territory of origin: China
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): B, B, B
Grade C (Good): C, C, C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Bugaj AM, Poland; Islamoglu MS, Turkey; Lambrecht NW, United States; Lim SC, South Korea; Sadighha A, Iran; Toyoshima O, Japan A-Editor: Yao QG S-Editor: Fan JR L-Editor: Wang TQ P-Editor: Fan JR
| 1. | Gorin I, Gaitz JP, Chevrier C, Lessana-Leibowitch M, Fortier P, Escande JP. Maladie du Morbihan: Essais therapeutiques. Deuxième présentation Paris: Abstract. Journées Dermatologiques de Paris 1991; 111. |
| 2. | Lamparter J, Kottler U, Cursiefen C, Pfeiffer N, Pitz S. [Morbus Morbihan : A rare cause of edematous swelling of the eyelids]. Ophthalmologe. 2010;107:553-557. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 14] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 3. | Connelly MG, Winkelmann RK. Solid facial edema as a complication of acne vulgaris. Arch Dermatol. 1985;121:87-90. [PubMed] |
| 4. | Nagasaka T, Koyama T, Matsumura K, Chen KR. Persistent lymphoedema in Morbihan disease: formation of perilymphatic epithelioid cell granulomas as a possible pathogenesis. Clin Exp Dermatol. 2008;33:764-767. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 38] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 5. | Scerri L, Saihan EM. Persistent facial swelling in a patient with rosacea. Rosacea lymphedema. Arch Dermatol. 1995;131:1071, 1074. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 18] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 6. | Morales-Burgos A, Alvarez Del Manzano G, Sánchez JL, Cruz CL. Persistent eyelid swelling in a patient with rosacea. P R Health Sci J. 2009;28:80-82. [PubMed] |
| 7. | Scallan JP, Hill MA, Davis MJ. Lymphatic vascular integrity is disrupted in type 2 diabetes due to impaired nitric oxide signalling. Cardiovasc Res. 2015;107:89-97. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 86] [Cited by in RCA: 117] [Article Influence: 11.7] [Reference Citation Analysis (0)] |
| 8. | Moriguchi P, Sannomiya P, Lara PF, Oliveira-Filho RM, Greco KV, Sudo-Hayashi LS. Lymphatic system changes in diabetes mellitus: role of insulin and hyperglycemia. Diabetes Metab Res Rev. 2005;21:150-157. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 44] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 9. | Jungfer B, Jansen T, Przybilla B, Plewig G. Solid persistent facial edema of acne: successful treatment with isotretinoin and ketotifen. Dermatology. 1993;187:34-37. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 27] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 10. | Ranu H, Lee J, Hee TH. Therapeutic hotline: Successful treatment of Morbihan's disease with oral prednisolone and doxycycline. Dermatol Ther. 2010;23:682-685. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 17] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 11. | Hu SW, Robinson M, Meehan SA, Cohen DE. Morbihan disease. Dermatol Online J. 2012;18:27. [PubMed] |
| 12. | Vasconcelos RC, Eid NT, Eid RT, Moriya FS, Braga BB, Michalany AO. Morbihan syndrome: a case report and literature review. An Bras Dermatol. 2016;91:157-159. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 15] [Cited by in RCA: 13] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 13. | Laugier P, Gilardi S. [Chronic erythematous oedema of the upper face (Degos). Morbihan disease (author's transl)]. Ann Dermatol Venereol. 1981;108:507-513. [PubMed] |
| 14. | Mazzatenta C, Giorgino G, Rubegni P, de Aloe G, Fimiani M. Solid persistent facial oedema (Morbihan's disease) following rosacea, successfully treated with isotretinoin and ketotifen. Br J Dermatol. 1997;137:1020-1021. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 22] [Article Influence: 0.8] [Reference Citation Analysis (1)] |
| 15. | Yu X, Qu T, Jin H, Fang K. Morbihan disease treated with Tripterygium wilfordii successfully. J Dermatol. 2018;45:e122-e123. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.3] [Reference Citation Analysis (1)] |
| 16. | Wang C, Yuan J, Wu HX, Chang Y, Wang QT, Wu YJ, Zhou P, Yang XD, Yu J, Wei W. Total glucosides of paeony inhibit the inflammatory responses of mice with allergic contact dermatitis by restoring the balanced secretion of pro-/anti-inflammatory cytokines. Int Immunopharmacol. 2015;24:325-334. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 32] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 17. | Su J, Zhang P, Zhang JJ, Qi XM, Wu YG, Shen JJ. Effects of total glucosides of paeony on oxidative stress in the kidney from diabetic rats. Phytomedicine. 2010;17:254-260. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 62] [Cited by in RCA: 62] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 18. | Deng H, Yan C, Xiao T, Yuan D, Xu J. Total glucosides of Paeonia lactiflora Pall inhibit vascular endothelial growth factor-induced angiogenesis. J Ethnopharmacol. 2010;127:781-785. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 18] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 19. | Luo J, Jin DE, Yang GY, Zhang YZ, Wang JM, Kong WP, Tao QW. Total glucosides of paeony for rheumatoid arthritis: A systematic review of randomized controlled trials. Complement Ther Med. 2017;34:46-56. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 42] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 20. | Zheng Q, Jiang W, Sun X, Ma T, Xu W, Shen F, Li H, Xie S, Li B, Li X. Total glucosides of paeony for the treatment of psoriasis: A systematic review and meta-analysis of randomized controlled trials. Phytomedicine. 2019;62:152940. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 26] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 21. | Feng Z, Zhang BQ, Zhu YM, Yu BB, Fu L, Zhou LL, Zhou XP, Lu Y. The Effectiveness and Safety of Total Glucosides of Paeony in Primary Sjögren's Syndrome: A Systematic Review and Meta-Analysis. Front Pharmacol. 2019;10:550. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 26] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 22. | Xiang N, Li XM, Zhang MJ, Zhao DB, Zhu P, Zuo XX, Yang M, Su Y, Li ZG, Chen Z, Li XP. Total glucosides of paeony can reduce the hepatotoxicity caused by Methotrexate and Leflunomide combination treatment of active rheumatoid arthritis. Int Immunopharmacol. 2015;28:802-807. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 41] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 23. | Feng ZT, Xu J, He GC, Cai SJ, Li J, Mei ZG. A systemic review and meta-analysis of the clinical efficacy and safety of total glucosides of peony combined with methotrexate in rheumatoid arthritis. Clin Rheumatol. 2018;37:35-42. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 20] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 24. | Zhou Z, Lin J, Huo R, Huang W, Zhang J, Wang L, Sun Y, Shen B, Li N. Total glucosides of paeony attenuated functional maturation of dendritic cells via blocking TLR4/5 signaling in vivo. Int Immunopharmacol. 2012;14:275-282. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 44] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 25. | Long JW, Wang YY, Pi XM, Tu YT. Clinical observation on the treatment of chronic urticaria with total glucosides of paeony capsule combined with citirizine. Chin J Integr Med. 2010;16:353-356. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 16] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 26. | Donthi D, Nenow J, Samia A, Phillips C, Papalas J, Prenshaw K. Morbihan disease: A diagnostic dilemma: two cases with successful resolution. SAGE Open Med Case Rep. 2021;9:2050313X211023655. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 11] [Article Influence: 2.8] [Reference Citation Analysis (1)] |
| 27. | He DY, Dai SM. Anti-inflammatory and immunomodulatory effects of paeonia lactiflora pall., a traditional chinese herbal medicine. Front Pharmacol. 2011;2:10. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 220] [Cited by in RCA: 227] [Article Influence: 16.2] [Reference Citation Analysis (1)] |
| 28. | Li H, Cao XY, Dang WZ, Jiang B, Zou J, Shen XY. Total Glucosides of Paeony protects against collagen-induced mouse arthritis via inhibiting follicular helper T cell differentiation. Phytomedicine. 2019;65:153091. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 28] [Article Influence: 4.7] [Reference Citation Analysis (0)] |