Published online Apr 16, 2013. doi: 10.12998/wjcc.v1.i1.67
Revised: February 14, 2013
Accepted: March 21, 2013
Published online: April 16, 2013
Processing time: 106 Days and 4.1 Hours
Parkinson’s disease is an idiopathic disorder of the central nervous system, characterized by resting tremors, muscular rigidity, slow and decreased movements. Oral rehabilitation of these patients requires special care, especially in those cases where the patient’s socioeconomic status is not good and patient cannot come several times for fabrication of a complete denture. This clinical report presents a case of a Parkinson’s patient who was completely rehabilitated in 3 appointments using special techniques. Border molding, final impression and jaw relation procedures were done in one appointment by using a custom tray with detachable handles and occlusal rims.
Core tip: Parkinson’s disease is a debilitating disease. Patients cannot visit the dentist frequently for procedures like complete denture, especially when the disease is at an advanced stage. The matter becomes worse when the patient is poor and unable to bear the cost. This case report presents a solution to above mentioned problem in a simple and lucid manner, where patient has to visit the dentist only thrice, at no extra cost.
- Citation: Singh Y, Saini M, Garg N. Oral rehabilitation of a Parkinson’s patient: A case report. World J Clin Cases 2013; 1(1): 67-70
- URL: https://www.wjgnet.com/2307-8960/full/v1/i1/67.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v1.i1.67
Parkinson’s disease is a chronic, progressive, neurodegenerative disorder, characterized by resting tremor (in hands, arms, legs, jaw and face), rigidity and stiffness (limbs and trunk), and postural instability or impaired balance and coordination[1-3].
It is the fourth most common neurodegenerative disorder[2]. It is characterized by resting tremors, muscular rigidity, slow and decreased movement and postural instability. It is a major cause of disability, social isolation, loss of self esteem and depression. Oral rehabilitation of these patients requires a multidisciplinary approach[3] and special care because, due to increased tremors, increased saliva, diminished adaptive skills and poor muscle control by the patient, prosthodontic procedures become difficult to perform and retention of dentures is compromised[4]. Also, the patient finds it difficult to care for and maintain the denture. Therefore, prosthodontic procedures become difficult to perform and require special care and attention. Moreover, the patient cannot visit the dentist several times due to his medical condition[5].
Previous studies[6-10] have been done on the fabrication of complete denture for patients suffering from Parkinson’s disease. The main drawback was its cost. The Parkinson’s patient who belongs to a poor socio-economic status cannot afford such therapy. Here, tich buttons were used instead of metal styli to solve this problem. Tich buttons are cheap and more easily available than metal styli.
This clinical report describes the fabrication of complete denture for a patient suffering from Parkinson’s disease by using certain modifications, like combining border molding, final impression and jaw relation procedures in one appointment[11] by using a custom tray with detachable handles and occlusal rims with the help of tich buttons and use of non-anatomic or monoplane teeth that helped in delivery of the denture in three appointments.
A 55-year-old male patient reported to the dental OPD, Subharti Dental College, Meerut for the fabrication of complete denture. The patient had a 5-year medical history of Parkinson’s disease and was on drug therapy. His physical and financial condition led to planning a denture with certain modifications.
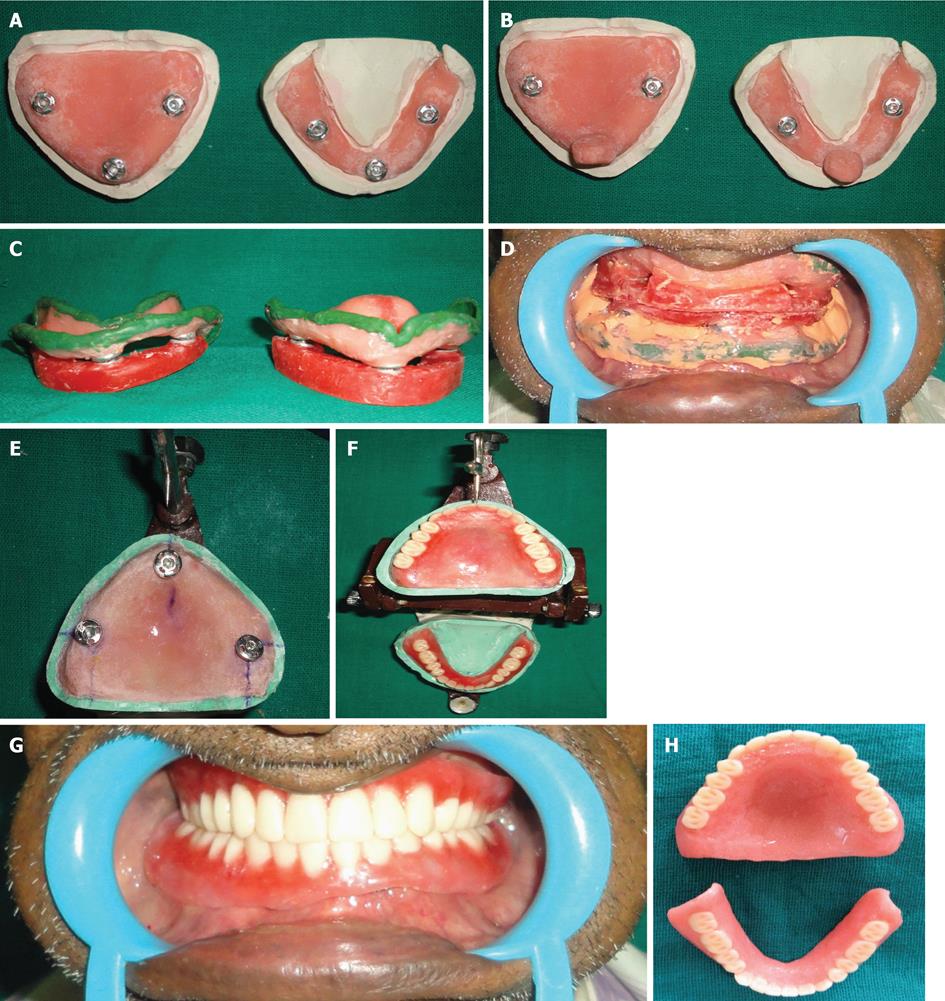
On the first day, primary impressions were made with an impression compound in the conventional manner and the primary cast was obtained and the acrylic resin was mixed and adapted on the primary cast to make a custom tray in the conventional manner. Before the acrylic resin set, the sleeve of one tich button was inserted in the anterior region and two in the posterior region (Figure 1A). Surveyor was used for this so as to make the long axis of all vertical and parallel to each other. Now the other part of the tich button was placed on the anterior and handles were made (Figure 1B). After setting, the handles were separated from the tray and all tich buttons locked with its other part and occlusal rims were fabricated on it. Now the maxillary and mandibular custom trays were ready for making impressions with the detachable handles and occlusal rims, depending on the procedure. On the second appointment, with the handles attached, border molding was completed. Now the handles were removed and occlusal rims were attached and vertical and centric jaw relation records were established in a conventional manner (Figure 1C). The final impression was made with zinc oxide eugenol with handles reattached. After the final impression, both occlusal rims were reattached and sealed at the established vertical and centric relation (Figure 1D). Custom tray and final impressions from occlusal rims were separated and handles reattached and impressions were poured after beading and boxing. Occlusal rims were reattached and measurements of the proper position of buttons and height of the rims noted to avoid any error in placing buttons on denture bases. Finally, mounting was done. Denture bases were fabricated in the conventional manner but at the same time placing sleeves of buttons on it before setting (Figure 1E). Position of the buttons can be verified by rims as well as measurements taken before. Now the rims reattached on the new sleeves and teeth arrangement was done using monoplane teeth (Figure 1F). On the third appointment, trial dentures were checked in the patient’s mouth for esthetics, phonetics, border extensions, midline and vertical dimension (Figure 1G). To avoid a fourth visit, wax up and carving were done at the time of teeth arrangement. Dentures were cured and polished and delivered to the patient (Figure 1H).
Parkinson’s disease is a chronic, progressive, neurodegenerative disorder, characterized by resting tremor (in hands, arms, legs, jaw and face), rigidity and stiffness (limbs and trunk), and postural instability or impaired balance and coordination. There are peculiar clinical features of this disease, like resting tremors, muscular rigidity and hypokinesia, facial impassiveness and cogwheel type of rigidity[12].
Dentists face many problems[13,14] in fabrication of complete denture in such patients because increased tremors, increased saliva, diminished adaptive skills and poor muscle control make impression making and jaw relation recording difficult, causing compromised retention. When the center of gravity is displaced, there may be tendency to fall forward/backward. The tongue may dislodge the mandibular denture and facial muscles that are rigid or uncontrollable may prevent a maxillary denture from maintaining a retentive seal. Also, the patient finds it difficult to care for and maintain the denture.
The patient was not able to visit several times for the procedure. Therefore, border molding, final impression and jaw relation procedures were combined in one appointment by using a custom tray with detachable handles and occlusal rims with the help of tich buttons. In such cases, facebow transfer and Gothic arch tracings cannot be recorded due to the medical condition of the patient. This eliminated the use of a semi or fully adjustable articulator. Monoplane teeth were used to compensate for the variable centric relation.
The technique described here is relatively simple and a drastic departure from the conventional procedure. With this technique, complete denture was delivered in three visits and was also very economical for the patient. Although this technique increases laboratory time, it reduces the clinical visits to a greater extent without compromising the basic principles of complete denture fabrication.
P- Reviewers Panciani PP, Teive HAG S- Editor Zhai HH L- Editor Roemmele A E- Editor Zheng XM
| 1. | Walker BR, Boon NA, Colledge NR. Davidson’s principles and practice of Medicine. 20th ed. Edinburgh: Churchill Livingston 2006; 1218. |
| 2. | Dirks SJ, Paunovich ED, Terezhalmy GT, Chiodo LK. The patient with Parkinson’s disease. Quintessence Int. 2003;34:379-393. [PubMed] |
| 3. | Fiske J, Hyland K. Parkinson’s disease and oral care. Dent Update. 2000;27:58-65. [PubMed] |
| 4. | Rahn AO, Heartwell CM. Textbook of complete dentures. 5th ed. Philadelphia: Lea and Febiger 1993; 134. |
| 5. | Persson M, Osterberg T, Granérus AK, Karlsson S. Influence of Parkinson’s disease on oral health. Acta Odontol Scand. 1992;50:37-42. [PubMed] |
| 6. | Heckmann SM, Heckmann JG, Weber HP. Clinical outcomes of three Parkinson‘s disease patients treated with mandibular implant overdentures. Clin Oral Implants Res. 2000;11:566-571. [PubMed] |
| 7. | Omprakash YV, Hallikerimath RB, Gangadhar SA. Prosthodontic management of a case of Parkinson’s disease - A case report. J Indian Prosthodont Soc. 2004;4:21-24. |
| 8. | Chu FC, Deng FL, Siu AS, Chow TW. Implant-tissue supported, magnet-retained mandibular overdenture for an edentulous patient with Parkinson’s disease: a clinical report. J Prosthet Dent. 2004;91:219-222. [PubMed] |
| 9. | Packer M, Nikitin V, Coward T, Davis DM, Fiske J. The potential benefits of dental implants on the oral health quality of life of people with Parkinson’s disease. Gerodontology. 2009;26:11-18. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 31] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 11. | Ansari IH. A one-appointment impression and centric relation record technique for compromised complete denture patients. J Prosthet Dent. 1997;78:320-323. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 5] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 12. | Friedlander AH, Mahler M, Norman KM, Ettinger RL. Parkinson disease: systemic and orofacial manifestations, medical and dental management. J Am Dent Assoc. 2009;140:658-669. [PubMed] |
| 13. | Langer A. Prosthodontic failures in patients with systemic disorders. J Oral Rehabil. 1979;6:13-19. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 11] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 14. | Kieser J, Jones G, Borlase G, MacFadyen E. Dental treatment of patients with neurodegenerative disease. N Z Dent J. 1999;95:130-134. [PubMed] |