Published online Jul 28, 2014. doi: 10.4329/wjr.v6.i7.507
Revised: June 1, 2014
Accepted: June 14, 2014
Published online: July 28, 2014
Processing time: 116 Days and 22.7 Hours
Craniosynostosis is a pathologic condition which is characterized by the premature fusion of cranial sutures. It may occur alone or in association with other anomalies making up various syndromes. Crouzon syndrome is the most common craniosynostosis syndrome. Bicoronal sutures fusion is most commonly involved in Crouzon syndrome. There have only been a handful of cases of squamosal suture synostosis described in the surgery literature with the few ones described in Crouzon syndrome associated with other types of craniosynostosis. To the best of our knowledge, we are presenting the first case of isolated bilateral squamosal suture synostosis in a patient with Crouzon syndrome in a radiology journal with emphasis on its radiological appearance.
Core tip: We report the unique case of isolated bilateral squamosal suture synostosis in a 13-mo old patient with Crouzon syndrome. Although bicoronal sutures are most commonly involved in patients with Crouzon syndrome, it is important to be familiar with this rare entity of craniosynostosis in order to prevent misdiagnosis or delayed surgical treatment.
- Citation: Tandon YK, Rubin M, Kahlifa M, Doumit G, Naffaa L. Bilateral squamosal suture synostosis: A rare form of isolated craniosynostosis in Crouzon syndrome. World J Radiol 2014; 6(7): 507-510
- URL: https://www.wjgnet.com/1949-8470/full/v6/i7/507.htm
- DOI: https://dx.doi.org/10.4329/wjr.v6.i7.507
Crouzon syndrome is a very rare autosomal dominant craniofacial dysostosis that occurs in approximately 16 in 1 million live births[1-3]. It was described in 1912 by a French neurologist, Octave Crouzon, in a mother and son exhibiting a triad of skull deformities, facial anomalies and exophthalmos[4]. Typically Crouzon syndrome has been associated with bicoronal synostosis leading to a characteristic tall, flattened forehead. Midface hypoplasia, a beaked nose, and proptosis have also been described as characteristic features[5,6].
To the best of our knowledge, there have been no cases of Crouzon syndrome associated with isolated bilateral squamosal suture craniosynostosis described in the literature. We report the radiological appearance of bilateral premature squamosal craniosynostosis found in a 13 mo-old female with Crouzon syndrome during her work up for skull deformity.
The patient was a 13 mo-old female who was born at 37 wk gestation and had a normal neonatal course. The patient’s father carried a diagnosis of Crouzon syndrome. Her family history was otherwise unremarkable. Her past surgical history includes bilateral tear duct probing for bilateral nasolacrimal obstruction. On physical exam, the patient was noted to have macrocephaly (> 97% percentile for age) associated with a prominent forehead and relatively narrowed temples, proptosis, low set ears, orbital hypertelorism and the right cheek was higher and fuller than the left cheek. Given the family history of Crouzon syndrome and the patient’s dysmorphic features, Crouzon syndrome was suspected. Genetic testing was done to confirm diagnosis and a mutation in the FGFR2 gene was noted. The patient was then referred to our radiology department to have a head CT performed to rule out craniosynostosis.
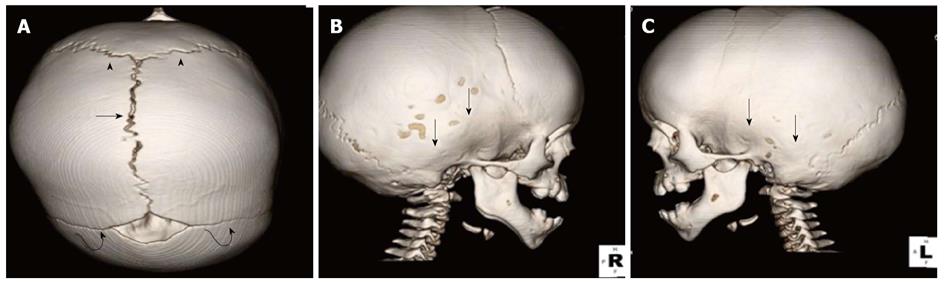
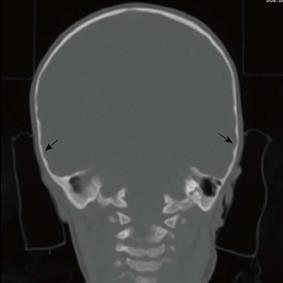
CT of the head without intravenous contrast was performed in our institution for further evaluation using the following technique: GE Medical Systems, Pitch: 0.625:1, Pixel spacing: 0.400 mm/0.400 mm, Kvp 120, mA 109, rotate time: 0.8, ST 3.75 mm, FOV 20 cm, Tilt 0, W: 90, L: 40. Two dimensional images (2D) in the sagittal and coronal planes were reformatted at ST of 3 mm as well as three dimensional images of the skull (3D). The 3D images demonstrate normal appearance of the bilateral coronal and lambdoid sutures and normal appearance of the sagittal suture (Figure 1A). The metopic suture is not visualized, having normally fused. However, there is premature fusion of the squamosal sutures bilaterally (Figure 1B). Coronal 2D reformatted image (Figure 2) shows the local thumb printing (beaten copper) appearance of the inner cortex in the region of bilateral squamosal suture fusion.
The correction of the craniofacial deformities in a patient with Crouzon syndrome and bilateral squamosal craniosynostosis is accomplished through a series of operations over time with respect to the growth and development of the craniofacial skeleton. Around the first year of age, the patient will undergo subtotal cranial vault remodeling to release the fused sutures and correct the skull shape deformities. Subsequently, at around 7 years of age, the patient will be scheduled to undergo either a facial bipartition or Lefort III advancement to correct the hypertelorism or midface hypoplasia. At skeletal maturity, the patient will undergo orthognatic surgery to correct malocclusion when necessary.
The development of the human calvaria is a complex process that is still not completely understood. There are 5 primary ossification centers which meet to form 6 main sutures. When this process occurs normally, it culminates to a normally shaped adult head[7].
Craniosynostosis is a pathologic condition which is characterized by the premature fusion of cranial sutures which results in deformity of the vault and cranial base and is often associated with neurological sequelae secondary to alteration in cranial volume and restriction in brain growth. It may occur alone or in association with other anomalies making up various syndromes[8].
Craniosynostosis is estimated to affect approximately 1 in 2500 children[9,10]. Different etiologies of craniosynostosis include metabolic anomalies, teratogens, genetic anomalies, and abnormal intrauterine pressures[11].
Among the craniosynostosis that are attributed to genetics, most have been associated with a mutation involving 1 of 3 fibroblast growth factor receptors (FGFRs) which include FGFR1, FGFR2, or FGFR3[11]. In the majority of cases, Crouzon syndrome is caused by mutations in the fibroblast growth factor 2 (FGFR2) gene on chromosome 10q26[1,12,13]. However, in patients with Crouzon syndrome and acanthosis nigricans, FGFR3 mutations have also been identified[14]. FGFR gene family mutations have also been found in patients with other syndromic craniosynostosis including Pfeiffer syndrome, Jackson-Weiss syndrome, Apert, and Saethre-Chotzen’s syndromes[15,16].
Our patient tested positive for FGFR2 mutation which is also found in Pfeiffer and Apert Syndromes[17]. Pfeiffer and Aper syndromes share common features with Crouzon syndrome including craniosynostosis, hypertelorism, proptosis, maxillary bone hypoplasia and autosomal dominance inheritance. However Pfeiffer and Apert syndromes are acrocephalosyndactyly syndromes associated with brachydactyly and syndactyly which our patient did not have and which helped in confirming the diagnosis of Crouzon syndrome[18,19].
The gold standard imaging modality in diagnosing craniosynostosis is CT scan with 3D surface-rendered reconstruction[20]. MRI has no significant role in the diagnosis of craniosynostosis or facial anomalies associated with Crouzon syndrome as it has poor details to bones. MRI of the brain may be indicated in the future only if patient develops neurologic symptoms.
The sagittal suture is most commonly affected in non syndromic craniosynostosis and is estimated to be affected in 40%-60% of cases[21]. This is followed by the coronal suture that is affected in 20%-30% of the cases and the metopic suture in less than 10% of the cases[21]. The pattern of suture involvement determines the shape of the skull defect[21]. There have been more than 100 different types of syndromes which have been identified to be associated with craniosynostosis[9,10].
Crouzon syndrome is one of the most common of the craniosynostosis syndromes[21]. It account for up to 4.8% of all cases of craniosynostosis[13]. The coronal and sagittal sutures are most commonly involved in Crouzon syndrome[13].
There have only been a handful of cases of squamosal suture synostosis described in the surgery literature, the few described in Crouzon patients were always associated with other type of craniosynostosis[10,22]. This is the first reported case of isolated squamosal suture synostosis in a patient with Crouzon syndrome. The squamosal suture arches posteriorly from the pterion and connects the temporal squama with the inferior border of the parietal bone[10].
The treatment of craniosynostosis syndromes requires a multidisciplinary team including plastic surgeons, pediatricians, ENT specialist, radiologists, neurosurgeons, and clinical genetic specialist[23,24]. Surgical correction is undertaken to correct craniofacial deformities and functional problems such as elevated intracranial pressure, airway obstruction, ocular exposure and malocclusion. Surgical techniques that are commonly utilized include fronto-orbital advancement or cranial vault remodeling in first year of life to correct craniosynostosis[25]. Hypertelorism is usually corrected with facial bipartition at age 7. Distraction osteogenesis is commonly used with midface osteotomies to correct midface hypoplasia as it has multiple advantages over conventional mid-facial advancement such as the monobloc or LeFort III. Distraction techniques have been shown to reduce operating time, reduce blood loss, reduce infection, eliminate need of bone graft, and allow for large advancement of the midface. Class III malocclusion which is commonly seen in syndromic craniosynostosis patients is corrected at skeletal maturity with a Lefort I advancement or double jaw surgery[26-32].
In a conclusion, although squamosal suture craniosynostosis is an extremely rare entity, especially when associated with Crouzon syndrome, it is extremely important for the radiologist to be familiar with its radiological appearance in order to prevent misdiagnosis and delayed treatment.
Thirteen-month-old female patient with Crouzon syndrome was found to have isolated bilateral squamosal suture synostosis.
The patient was noted to have macrocephaly associated with a prominent forehead and relatively narrowed temples, proptosis, low set ears, orbital hypertelorism and asymmetry in appearance of the cheeks.
Pfeiffer and Apert syndromes.
Mutation in the FGFR2 gene was noted.
Computed tomography finding: The three dimensional (3D) images demonstrate normal appearance of the bilateral coronal and lambdoid sutures and normal appearance to the sagittal suture. However, there is bony bridging in the region of squamosal sutures bilaterally indicating premature synostosis. Coronal 2D reformatted image shows the local thumb printing (beaten copper) appearance of the inner cortex in the region of bilateral squamosal suture fusion.
The treatment of craniosynostosis syndromes requires a multidisciplinary team including plastic surgeons, pediatricians, ENT specialists, radiologists, neurosurgeons, and clinical genetic specialists. A series of corrective operations will be performed over time.
The authors report the unique case of isolated bilateral squamosal suture synostosis in a patient with Crouzon syndrome. Although bicoronal sutures are most commonly involved in patients with Crouzon syndrome, it is important to be familiar with this rare entity of craniosynostosis in order to prevent misdiagnosis or delayed surgical treatment.
This is a simple case report on a young patient with Crouzon syndrome. It is concise, well written and well illustrated.
P- Reviewer: Cho SY, Lakhdar F S- Editor: Wen LL L- Editor: A E- Editor: Lu YJ
| 1. | Reardon W, Winter RM, Rutland P, Pulleyn LJ, Jones BM, Malcolm S. Mutations in the fibroblast growth factor receptor 2 gene cause Crouzon syndrome. Nat Genet. 1994;8:98-103. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 551] [Cited by in RCA: 508] [Article Influence: 16.4] [Reference Citation Analysis (0)] |
| 2. | Mulliken JB, Steinberger D, Kunze S, Müller U. Molecular diagnosis of bilateral coronal synostosis. Plast Reconstr Surg. 1999;104:1603-1615. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 78] [Cited by in RCA: 70] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 3. | Cohen MM, Kreiborg S. Birth prevalence studies of the Crouzon syndrome: comparison of direct and indirect methods. Clin Genet. 1992;41:12-15. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 111] [Cited by in RCA: 109] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 4. | Babic GS, Babic RR. Ophthalmological and Radiological picture of Crouzon syndrome-A case report. Acta Medica Medianae. 2009;48:37-40. |
| 5. | Kreiborg S, Cohen MM. Is craniofacial morphology in Apert and Crouzon syndromes the same? Acta Odontol Scand. 1998;56:339-341. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 30] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 6. | Kreiborg S. Craniofacial growth in plagiocephaly and Crouzon syndrome. Scand J Plast Reconstr Surg. 1981;15:187-197. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 46] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 7. | Podda S, Ciminello FS, Wolfe SA. “Congenital Synostoses.” Medscape. Cited: 2014-03-20. Available from: http://emedicine.medscape.com/article/1280365-overview. |
| 8. | Gorlin RJ, Cohen MM, Hennekam RC. Syndromes with craniosynostosis: General aspects and well known syndromes. New York: Oxford university press 2001; 654-670. |
| 9. | Silva DL, Neto FX, Carneiro SG, Palheta AC, Monteiro MC, Cunha SC, Nunes CT. Crouzon’s Syndrome: Literature Review. Intl Arch Otorhinolaryngol. 2008;12:436-441. |
| 10. | Ranger A, Chaudhary N, Matic D. Craniosynostosis involving the squamous temporal sutures: a rare and possibly underreported etiology for cranial vault asymmetry. J Craniofac Surg. 2010;21:1547-1550. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 18] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 11. | Aleck K. Craniosynostosis syndromes in the genomic era. Semin Pediatr Neurol. 2004;11:256-261. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 25] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 12. | Rutland P, Pulleyn LJ, Reardon W, Baraitser M, Hayward R, Jones B, Malcolm S, Winter RM, Oldridge M, Slaney SF. Identical mutations in the FGFR2 gene cause both Pfeiffer and Crouzon syndrome phenotypes. Nat Genet. 1995;9:173-176. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 333] [Cited by in RCA: 311] [Article Influence: 10.4] [Reference Citation Analysis (0)] |
| 13. | Guledgud M, Patil K, Pai E, Deshpande P. Crouzon Syndrome. Int J Contemp Dent. 2011;2:80-83. |
| 14. | Meyers GA, Orlow SJ, Munro IR, Przylepa KA, Jabs EW. Fibroblast growth factor receptor 3 (FGFR3) transmembrane mutation in Crouzon syndrome with acanthosis nigricans. Nat Genet. 1995;11:462-464. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 292] [Cited by in RCA: 269] [Article Influence: 9.0] [Reference Citation Analysis (0)] |
| 15. | Nagase T, Nagase M, Hirose S, Ohmori K. Crouzon syndrome with acanthosis nigricans: case report and mutational analysis. Cleft Palate Craniofac J. 2000;37:78-82. [PubMed] |
| 16. | Maloth S, Padamashree S, Rema J, Yalsangi S, Ramadoss T, Kalladka M. Diagnosis of Crouzon’s syndrome. Hong Kong Dent J. 2010;7:95-100. |
| 17. | Passos-Bueno MR, Wilcox WR, Jabs EW, Sertié AL, Alonso LG, Kitoh H. Clinical spectrum of fibroblast growth factor receptor mutations. Hum Mutat. 1999;14:115-125. [PubMed] |
| 18. | Pfeiffer RA. [Dominant hereditary acrocephalosyndactylia]. Z Kinderheilkd. 1964;90:301-320. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 153] [Cited by in RCA: 120] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 19. | Kaplan LC. Clinical assessment and multispecialty management of Apert syndrome. Clin Plast Surg. 1991;18:217-225. [PubMed] |
| 20. | Vannier MW, Hildebolt CF, Marsh JL, Pilgram TK, McAlister WH, Shackelford GD, Offutt CJ, Knapp RH. Craniosynostosis: diagnostic value of three-dimensional CT reconstruction. Radiology. 1989;173:669-673. [PubMed] |
| 21. | Panigrahi I. Craniosynostosis genetics: The mystery unfolds. Indian J Hum Genet. 2011;17:48-53. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 31] [Cited by in RCA: 30] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 22. | Smartt JM, Singh DJ, Reid RR, Hellinger JC, Hsu VM, Bartlett SP. Squamosal suture synostosis: a cause of atypical skull asymmetry. Plast Reconstr Surg. 2012;130:165-176. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 22] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 23. | Kawamoto HK, Heller JB, Heller MM, Urrego A, Gabbay JS, Wasson KL, Bradley JP. Craniofrontonasal dysplasia: a surgical treatment algorithm. Plast Reconstr Surg. 2007;120:1943-1956. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 37] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 24. | Clayman MA, Murad GJ, Steele MH, Seagle MB, Pincus DW. History of craniosynostosis surgery and the evolution of minimally invasive endoscopic techniques: the University of Florida experience. Ann Plast Surg. 2007;58:285-287. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 42] [Cited by in RCA: 49] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 25. | Kirmi O, Lo SJ, Johnson D, Anslow P. Craniosynostosis: a radiological and surgical perspective. Semin Ultrasound CT MR. 2009;30:492-512. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 65] [Cited by in RCA: 62] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 26. | Shand JM, Smith KS, Heggie AA. The role of distraction osteogenesis in the management of craniofacial syndromes. Oral Maxillofac Surg Clin North Am. 2004;16:525-540. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 9] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 27. | Nout E, Cesteleyn LL, van der Wal KG, van Adrichem LN, Mathijssen IM, Wolvius EB. Advancement of the midface, from conventional Le Fort III osteotomy to Le Fort III distraction: review of the literature. Int J Oral Maxillofac Surg. 2008;37:781-789. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 66] [Cited by in RCA: 64] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 28. | Fearon JA. Halo distraction of the Le Fort III in syndromic craniosynostosis: a long-term assessment. Plast Reconstr Surg. 2005;115:1524-1536. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 132] [Cited by in RCA: 145] [Article Influence: 7.3] [Reference Citation Analysis (0)] |
| 29. | Yu JC, Fearon J, Havlik RJ, Buchman SR, Polley JW. Distraction Osteogenesis of the Craniofacial Skeleton. Plast Reconstr Surg. 2004;114:1E-20E. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 56] [Cited by in RCA: 50] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 30. | Fearon JA. The Le Fort III osteotomy: to distract or not to distract? Plast Reconstr Surg. 2001;107:1091-1103; discussion 1104-1106. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 105] [Cited by in RCA: 98] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 31. | Cedars MG, Linck DL, Chin M, Toth BA. Advancement of the midface using distraction techniques. Plast Reconstr Surg. 1999;103:429-441. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 89] [Cited by in RCA: 85] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 32. | Moore MH, Abbott AH. Extradural deadspace after infant fronto-orbital advancement in Apert syndrome. Cleft Palate Craniofac J. 1996;33:202-205. [PubMed] |