Published online Sep 15, 2019. doi: 10.4239/wjd.v10.i9.485
Peer-review started: June 19, 2019
First decision: August 2, 2019
Revised: August 19, 2019
Accepted: August 27, 2019
Article in press: August 27, 2019
Published online: September 15, 2019
Processing time: 88 Days and 19.1 Hours
The purpose of this article was to increase the knowledge about oral manifestations and complications associated with diabetes mellitus. An overview was performed on Google, especially in recent reliable papers in relation to diabetes mellitus and its oral manifestations (keywords were “diabetes mellitus”, “oral manifestations”, and “oral complications”). Data were collected and the results were declared. Diabetes mellitus is one of the most common chronic disorders characterized by hyperglycemia. This disease can have many complications in various regions of the body, including the oral cavity. The important oral manifestations and complications related to diabetes include xerostomia, dental caries, gingivitis, periodontal disease, increased tendency to oral infections, burning mouth, taste disturbance, and poor wound healing. Oral complications in diabetic patients are considered major complications and can affect patients’ quality of life. There is evidence that chronic oral complications in these patients have negative effects on blood glucose control, so prevention and management of the oral complications are important.
Core tip: Since diabetes mellitus is a common disease and can have some annoying manifestations in the patient’s mouth, it is important for physicians to be aware of these manifestations and to treat them properly.
- Citation: Rohani B. Oral manifestations in patients with diabetes mellitus. World J Diabetes 2019; 10(9): 485-489
- URL: https://www.wjgnet.com/1948-9358/full/v10/i9/485.htm
- DOI: https://dx.doi.org/10.4239/wjd.v10.i9.485
Diabetes mellitus (DM) is a chronic metabolic disease characterized by hyperglycemia due to either a deficiency of insulin secretion or resistance to the action of insulin or both[1-3]. Chronic hyperglycemia leads to different complications in various regions of the body including the oral cavity, so blood glucose control is very critical[4]. Possible mechanisms that may be related to oral complications of diabetes include impaired neutrophil function, increased collagenase activity, and a reduction in collagen synthesis, microangiopathy, and neuropathy[4].
The oral manifestations and complications related to DM include dry mouth (xerostomia), tooth decay (including root caries), periapical lesions, gingivitis, periodontal disease, oral candidiasis, burning mouth (especially glossodynia), altered taste, geographic tongue, coated and fissured tongue, oral lichen planus (OLP), recurrent aphthous stomatitis, increased tendency to infections, and defective wound healing[1-8]. The intensity of diabetic complications is usually proportional to the degree and duration of hyperglycemia[5]. In this study, we briefly reviewed DM and its oral manifestations and complications in recent reliable scientific papers.
People with diabetes experience salivary dysfunction, which can lead to decreased salivary flow and change in saliva composition. The estimated universal prevalence of xerostomia among diabetic patients ranges between 34% and 51%[1,2]. Xerostomia can lead to numerous problems such as difficulty in eating, swallowing, and speaking. It can actually have a negative effect on patients’ quality of life. Many studies have detected impaired salivary function in adults with diabetes. The etiology is unknown, but may be related to polyuria, autonomic neuropathies, and microvascular changes and alterations in the basement membranes of salivary glands[2,4,5,7,8]. There is a significant relationship between the degree of xerostomia and glucose levels in saliva. Notably, the highest level of salivary dysfunction is observed in diabetics with poor glycemic control[4,5].
Diabetic patients are susceptible to the development of new and recurrent dental caries. Reduced cleansing and buffering capacity of the saliva, increase of carbohydrate in the saliva, and increased level of oral yeasts, mutans streptococci and lactobacilli can lead to an increase in the incidence of tooth decay. In addition, chronic hyperglycemia may cause irreversible pulpitis leading to pulp necrosis[1,2,5,7,8]. Some studies have shown that apical periodon-titis and radiolucent periapical lesions are more common in diabetic compared to nondiabetic individuals[1,5,9].
Poor glycemic control can be associated with the outbreak and progression of gingivitis, periodontitis, and alveolar bone loss. Periodontal disease has been reported with increased incidence and prevalence in patients with type 1 and 2 diabetes. Prevalence of severe periodontitis in diabetic patients compared to nondiabetics has been found to be 59.6%:39%[3,7,8,10].
Possible mechanisms for explanation of increased susceptibility to periodontal diseases include alterations in host defense response (such as neutrophil dysfunction), subgingival microflora, structure and metabolism of collagen, vascularity, and gingival crevicular fluid and also, inheritance patterns. Furthermore, several risk factors have been reported, which make these patients more susceptible to the development of periodontal disease including poor oral hygiene, poor metabolic control, longer duration of diabetes, and smoking[3,6-8].
It is noteworthy that numerous studies have shown that periodontal disease has a negative impact on diabetes, and the treatment of periodontal disease has a desirable effect on blood glucose control. The elimination of pathogens by treatment leads to a decrease of inflammation, which in turn reduces insulin resistance; this in turn decreases glucose levels. Therefore, there is a two-way relationship between periodontal disease and diabetes[1,3,5,10]. In adults, periodontal disease is the main reason for tooth mobility and consequently, loss of it. Therefore, treatment of periodontitis, in addition to lowering blood glucose levels, can prevent tooth loss[11].
Patients with diabetes are more susceptible to the development of various oral infections including fungal and bacterial infections. Decreased salivary flow rate and the absence of its antimicrobial effects can cause these infections. In addition, an impaired defense mechanism and poor metabolic control may play an important role in developing infection[2,7,8].
Oral candidiasis is an opportunistic fungal infection. The prevalence of that is increasing, as it is one of the most common fungal infections. Higher candida colonization rates were reported in patients with diabetes type 1 when compared to type 2 (84% vs 68%, respectively), while the percentage in nondiabetic subjects was about 27%[2,12].
Oral candidiasis can be developed by numerous predisposing factors including xerostomia. Salivary dysfunction in these patients can contribute to higher carriage of fungi. Candida-related lesions include denture stomatitis, angular chelitis, and median rhomboid glossitis[2] (Figure 1). Candida infection is more prevalent in diabetic patients who smoke, wear dentures, have poor glycemic control, and use steroids and broad spectrum antibiotics[2,7,8].
Burning sensation or dysesthesia in the oral cavity of diabetic patients is attributed to poor glycemic control, metabolic alterations in oral mucosa, angiopathy, candida infection, and neuropathy[1]. Neuropathic pain in these patients can be manifested as burning, tingling, or even as electric shock or stabbing sensation that these symptoms may be very debilitating. These pain sensations have a considerable effect on the physical and psychological functions, and are associated with the level of sleep disturbance, anxiety, and depression[1,4].
Taste dysfunction can occur in patients with poorly controlled diabetes. In a cross-sectional study, among diabetic or prediabetic patients, 5.7% had a sweet taste disorder and 8.6% had a salt taste disorder[8,13]. Salivary dysfunction can cause altered taste sensation or raise of detection thresholds. Neuropathy also increases the threshold of taste. This sensory dysfunction can inhibit the ability to maintain a good diet and can lead to poor glucose regulation[1,2,4,7,8].
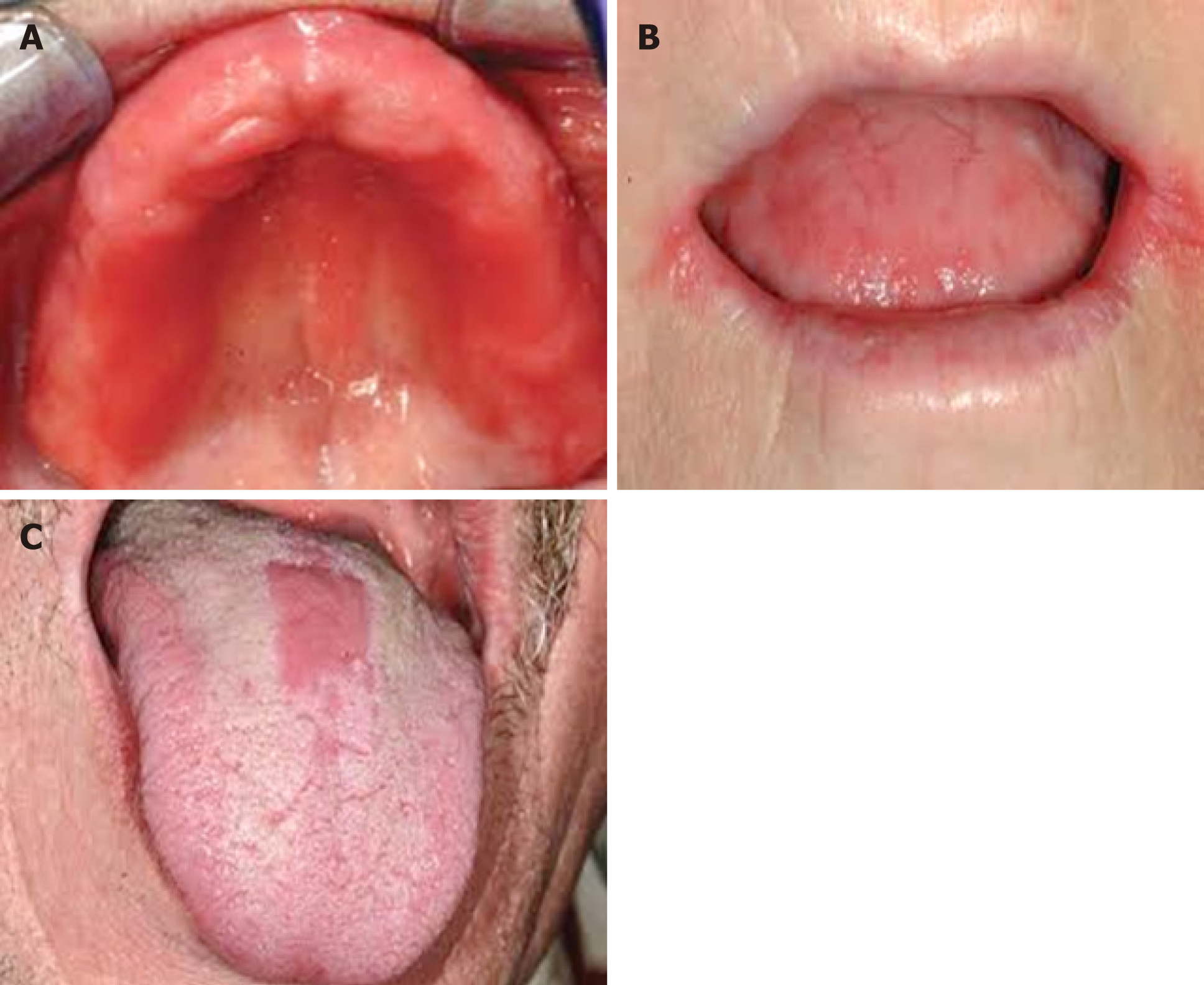
Some oral mucosa alterations such as coated and fissured tongue, geographic tongue, recurrent aphthous stomatitis, and some premalignant lesions including lichen planus can be associated with diabetes[1,2,5,7,8] (Figure 2). Susceptibility of these patients to oral cavity changes is still controversial, but insufficient control of diabetes, immuno-logical alteration, microcirculatory changes with decline of blood supply, xerostomia and alteration in salivary flow and composition, and smoking have been mentioned[1]. OLP occurs more frequently in patients with type 1 diabetes compared to type 2, because type 1 diabetes is considered an autoimmune disease, and OLP has an underlying autoimmune mechanism[2,8]. Acute hyperglycemia causes changes in the immune responsiveness in diabetic patients[2].
Delayed healing of soft and hard tissues in diabetic patients is a well-known complication during oral surgeries[2,8]. Based on some studies, effective factors in the prolonged wound healing of these patients include delayed vascularization, diminished blood flow and hypoxia, a reduction in innate immunity, decreased growth factor production, and psychological stress[2,14].
Oral complications in patients with DM are considered major complications of the disease and can impress the patients’ quality of life. There is evidence that chronic and persistent oral complications in these patients adversely affect blood glucose control. Thus, prevention and management of oral complications due to diabetes are considerable.
Manuscript source: Unsolicited manuscript
Specialty type: Endocrinology and metabolism
Country of origin: Iran
Peer-review report classification
Grade A (Excellent): 0
Grade B (Very good): 0
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Hamad ARA S-Editor: Ma RY L-Editor: Filipodia E-Editor: Xing YX
| 1. | Cicmil S, Mladenović I, Krunić J, Ivanović D, Stojanović N. Oral Alterations in Diabetes Mellitus. Balk J Dent Med. 2018;22:7-14. [RCA] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 8] [Article Influence: 1.1] [Reference Citation Analysis (4)] |
| 2. | Al-Maskari AY, Al-Maskari MY, Al-Sudairy S. Oral Manifestations and Complications of Diabetes Mellitus: A review. Sultan Qaboos Univ Med J. 2011;11:179-186. [PubMed] |
| 3. | Indurkar MS, Maurya AS, Indurkar S. Oral Manifestations of Diabetes. Clin Diabetes. 2016;34:54-57. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 19] [Cited by in RCA: 26] [Article Influence: 2.9] [Reference Citation Analysis (1)] |
| 4. | Cicmil A, Govedarica O, Lečić J, Mališ S, Cicmil S, Čakić S. Oral Symptoms and Mucosal Lesions in Patients with Diabetes Mellitus Type 2. Balk J Dent Med. 2017;21:50-54. [RCA] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 5] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 5. | Mauri-Obradors E, Estrugo-Devesa A, Jané-Salas E, Viñas M, López-López J. Oral manifestations of Diabetes Mellitus. A systematic review. Med Oral Patol Oral Cir Bucal. 2017;22:e586-e594. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 37] [Cited by in RCA: 78] [Article Influence: 9.8] [Reference Citation Analysis (2)] |
| 6. | Trentin MS, Verardi G, De C Ferreira M, de Carli JP, da Silva SO, Lima IF, Paranhos LR. Most Frequent Oral Lesions in Patients with Type 2 Diabetes Mellitus. J Contemp Dent Pract. 2017;18:107-111. [PubMed] |
| 7. | Ship JA. Diabetes and oral health: an overview. J Am Dent Assoc. 2003;134 Spec No:4S-10S. [PubMed] |
| 8. | Khan T. Oral manifestations and complications of diabetes mellitus: A review. Int J Med Health Res. 2018;4:50-52. [DOI] [Full Text] |
| 9. | López-López J, Jané-Salas E, Estrugo-Devesa A, Velasco-Ortega E, Martín-González J, Segura-Egea JJ. Periapical and endodontic status of type 2 diabetic patients in Catalonia, Spain: a cross-sectional study. J Endod. 2011;37:598-601. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 72] [Cited by in RCA: 85] [Article Influence: 6.1] [Reference Citation Analysis (0)] |
| 10. | Daniel R, Gokulanathan S, Shanmugasundaram N, Lakshmigandhan M, Kavin T. Diabetes and periodontal disease. J Pharm Bioallied Sci. 2012;4:S280-S282. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 38] [Article Influence: 2.9] [Reference Citation Analysis (1)] |
| 11. | Taboza ZA, Costa KL, Silveira VR, Furlaneto FA, Montenegro R, Russell S, Dasanayake A, Rego RO. Periodontitis, edentulism and glycemic control in patients with type 2 diabetes: a cross-sectional study. BMJ Open Diabetes Res Care. 2018;6:e000453. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 22] [Cited by in RCA: 24] [Article Influence: 3.4] [Reference Citation Analysis (1)] |
| 12. | Rodrigues CF, Rodrigues ME, Henriques M. Candida sp. Infections in Patients with Diabetes Mellitus. J Clin Med. 2019;8. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 92] [Cited by in RCA: 154] [Article Influence: 25.7] [Reference Citation Analysis (0)] |
| 13. | Tsujimoto T, Imai K, Kanda S, Kakei M, Kajio H, Sugiyama T. Sweet taste disorder and vascular complications in patients with abnormal glucose tolerance. Int J Cardiol. 2016;221:637-641. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 14] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 14. | Abiko Y, Selimovic D. The mechanism of protracted wound healing on oral mucosa in diabetes. Review. Bosn J Basic Med Sci. 2010;10:186-191. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 41] [Article Influence: 2.9] [Reference Citation Analysis (0)] |