Copyright
©The Author(s) 2014.
World J Diabetes. Feb 15, 2015; 6(1): 109-124
Published online Feb 15, 2015. doi: 10.4239/wjd.v6.i1.109
Published online Feb 15, 2015. doi: 10.4239/wjd.v6.i1.109
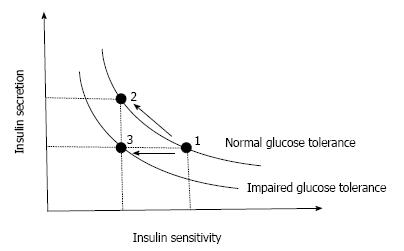
Figure 1 Insulin secretion-insulin sensitivity relationship.
In a physiological condition, when insulin sensitivity decreases, insulin secretion increases to maintain normoglycemia (1→2), showing a hyperbolic curve. When insulin secretion fails to compensate, the hyperbolic curve shifts to the left and abnormal glucose tolerance develops (1→3).
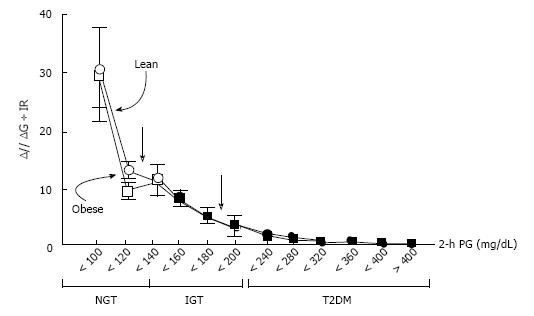
Figure 2 Insulin secretion/insulin resistance (disposition) index (I/G ÷ IR) during 75g-oral glucose tolerance test in individuals with normal glucose tolerance, impaired glucose tolerance, and type 2 diabetes as a function of the 2 h plasma glucose concentration in lean and obese subjects.
I/G: Insulinogenic index (Insulin 0-30 min/Glucose 0-30 min); IR: Homeostasis model assessment of insulin resistance [HOMA-IR; fasting insulin (mU/L) x glucose (mmol/L)/22.5]. Adapted from ref.[9]. NGT: Normal glucose tolerance; IGT: Impaired glucose tolerance; T2DM: Type 2 diabetes; PG: Plasma glucose.
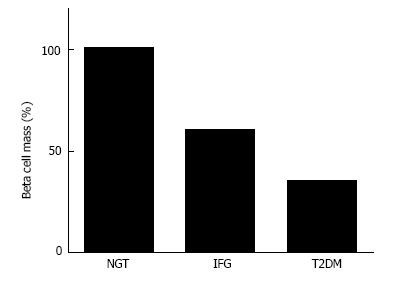
Figure 3 β-cell mass in patients with normal glucose tolerance, impaired fasting glycemia and type 2 diabetes.
Adapted and modified from the study by Butler et al[12]. NGT: Normal glucose tolerance; IFG: Impaired fasting glycemia; T2DM: Type 2 diabetes.
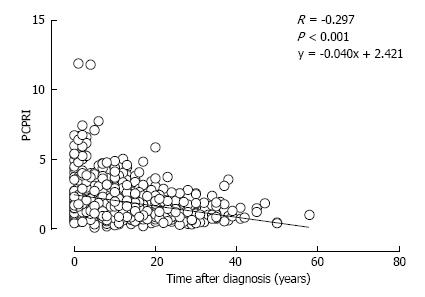
Figure 4 Relationship between postprandial C-peptide to glucose ratio (postprandial C-peptide index) and time after diagnosis in patients with Type 2 diabetes.
Reproduced with permission from ref.[51]. PCPRI: Postprandial C-peptide index.
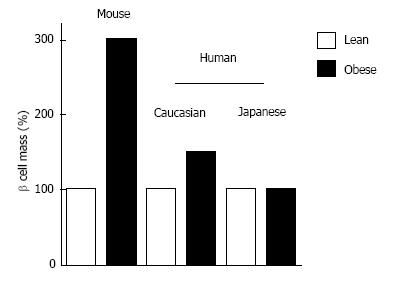
Figure 5 Change in β-cell mass with obesity.
In mice, β-cell mass increases 3-fold with obesity. In humans, a 50% increase in β-cell mass has been reported in Caucasians, while no increase was reported in Japanese. Adopted and modified from ref.[54,59,85].
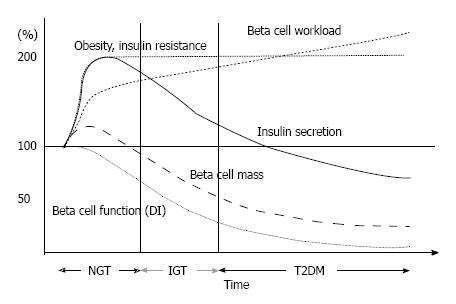
Figure 6 Hypothesis for change in β-cell function and mass during development of abnormal glucose tolerance.
The magnitude of the increased demand for insulin due to insulin resistance caused by excess caloric intake and physical inactivity exceeds the magnitude of β-cell mass expansion, resulting in an increase in β-cell workload. In individuals who are susceptible to type 2 diabetes (T2DM), increased β-cell workload may lead to β-cell failure and the development of T2DM. Adopted and modified from ref.[109].
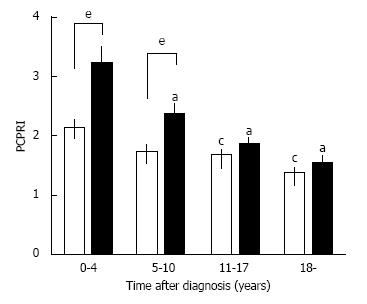
Figure 7 Postprandial C-peptide to glucose ratio (postprandial C-peptide index; PCPRI) in subjects according to obesity and time after diagnosis (0-4, 5-10, 11-17 and ≥ 18 years).
There were significant differences in PCPRI between lean (open bars) and obese subjects (solid bars) in the first and second quartiles of time after diagnosis, but no significant difference was observed in the third and fourth quartiles. aP < 0.05 vs obese subjects ≤ 4 yr after diagnosis, cP < 0.05 vs lean subjects ≤ 4 yr after diagnosis, eP < 0.05 vs lean subjects. Reproduced with permission from ref.[51].
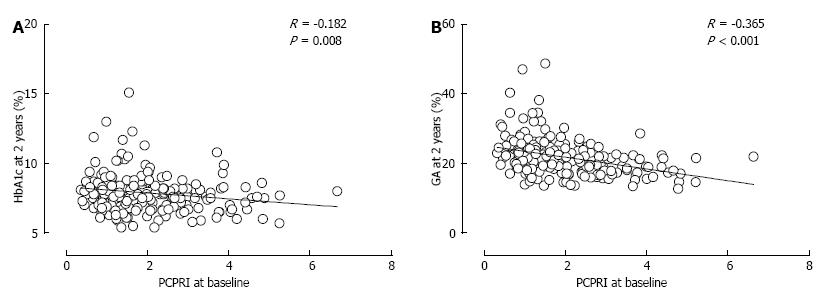
Figure 8 Correlation between baseline postprandial C-peptide index and HbA1c (A) and glycated albumin (B) after 2 years.
Reproduced with permission from ref.[93]. PCPRI: Postprandial C-peptide index; GA: Glycated albumin.
Figure 9 Correlation between postprandial C-peptide index and glycated albumin to HbA1c ratio in patients with type 2 diabetes (A) and type 1 diabetes (B).
In Figure 9B, the data of patients with type 1 diabetes are superimposed on the data of those with type 2 diabetes (gray circles and dotted line). Reproduced with permission from ref.[97]. PCPRI: Postprandial C-peptide index; GA: Glycated albumin.
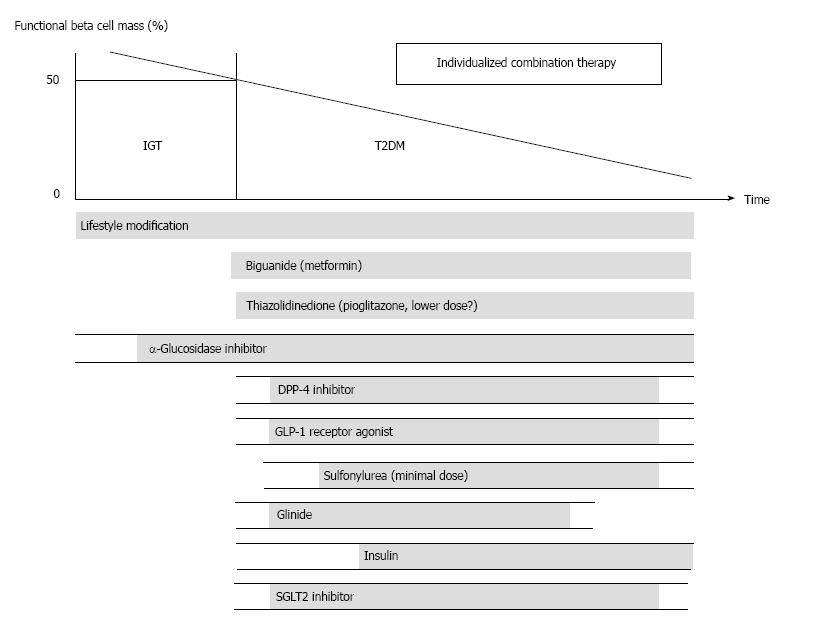
Figure 10 Proposed concept of treatment strategy for type 2 diabetes in relation to functional β-cell mass.
α-glucosidase inhibitor is partly approved for use in patients with impaired glucose tolerance in Japan. Medications not approved in Japan are not included in the figure. Since currently no single therapy or agent can cure and even manage type 2 diabetes (T2DM), an effective combination of current medications in addition to lifestyle modification aiming at reduction in β-cell workload is important to preserve or recover β-cell function. Adopted and modified from ref.[108,109]. IGT: Impaired glucose tolerance.
- Citation: Saisho Y. β-cell dysfunction: Its critical role in prevention and management of type 2 diabetes. World J Diabetes 2015; 6(1): 109-124
- URL: https://www.wjgnet.com/1948-9358/full/v6/i1/109.htm
- DOI: https://dx.doi.org/10.4239/wjd.v6.i1.109