Published online May 2, 2015. doi: 10.5314/wjd.v4.i2.114
Peer-review started: September 29, 2014
First decision: October 28, 2015
Revised: January 25, 2015
Accepted: April 1, 2015
Article in press: April 7, 2015
Published online: May 2, 2015
Processing time: 211 Days and 6 Hours
Naevus dysmorphia is a form of appearance concern/body image dissatisfaction, which describes a preoccupation with the appearance of a clinically small melanocytic naevus. The naevus is perceived by the patient to be disfiguring. Such perception leads to maladaptive behaviours and is often associated with low mood, as well as high levels of anxiety and social avoidance. Affected individuals form a diverse group. However, what they have in common is that the distress experienced is disproportionate to the objective visual appearance of the mole. There is a range of severity of the impact on the individual’s well being. Naevus dysmorphia may or may not be a cutaneous manifestation of body dysmorphic disorder (BDD). It is essential that patients with naevus dysmorphia are identified and distinguished from patients requesting removal of a mole for other uncomplicated cosmetic reason. Patients with naevus dysmorphia can be challenging to treat and communicate with. Surgical excision of the naevus will not address the underlying psychopathology and so it may not result in long-term positive outcome. Ideally, a detailed psychological assessment and formulation can be made potentially followed by psychological therapy tailored to the needs of the individual. A therapeutic trial of appropriate psychopharmacological course may be indicated in certain cases, e.g., when symptoms of a depressive disorder, anxiety disorder or BDD are present. A case series of 10 patients with naevus dysmorphia is presented, in order to highlight the above issues.
Core tip: Naevus dysmorphia is a form of body image dissatisfaction. A preoccupation with a simple melanocytic naevus that causes significant distress to the individual and impacts on their wellbeing are central features. Symptoms are often consistent with body dysmorphic disorder but the impact can be less severe. Patients tend to present to dermatology or cosmetic surgery requesting removal of a mole. An extended history is needed to fully assess the perceived “problem”. Excision alone will not necessarily address the underlying psychological issues. Liaison with clinical/health psychology and/or psychiatry can be desirable in individual cases.
- Citation: Affleck AG, Wray E, Chouliara Z. Identifying and managing naevus dysmorphia in clinical practice. World J Dermatol 2015; 4(2): 114-119
- URL: https://www.wjgnet.com/2218-6190/full/v4/i2/114.htm
- DOI: https://dx.doi.org/10.5314/wjd.v4.i2.114
Naevus dysmorphia is a specific form of body image concern/appearance concern, which describes a morbid preoccupation with the appearance of a clinically small melanocytic naevus, which the individual is convinced is unsightly resulting in distress, behavioural adaptations and negative impact on their wellbeing. An extended history is desirable including assessment for associated psychiatric disorders including body dysmorphic disorder (BDD), depressive disorder and suicidal ideation. Patients often present to general or cosmetic dermatology or cosmetic surgery clinics requesting surgical removal of the “offending” mole. Simple excision does not necessarily address the underlying reasons for the person’s overvalued perceptions of their appearance and preoccupation with the feature. A detailed psychological assessment and appropriate psychological therapy is recommended.
We are not aware of any previous detailed descriptions or case series of naevus dysmorphia per se.
A 16-year-old girl presented with 2 moles on her right arm and 2 moles on right lower leg which she had found “disgusting”. The appearance of the moles had distressed her to such an extent that she bought Dermatend®[1] on the internet and treated the areas in an attempt to remove them. Dermatend® contains the escharotic agent Sanguinaria canadensis which has been marketed as a skin tag and mole remover. On attendance at clinic it became apparent that she was generally distressed by the appearance her skin (cutaneous dysmorphia) stating that “she hated her pale skin and all her moles” and wished to have 3 further moles removed from her face.
Excision of the pink plaques at the site of the Dermatend® application was performed in order to obtain a histological diagnosis. A discussion around body image disorders appeared to be productive and a referral to health psychology was made. However, the patient did not attend for psychological therapy and was lost to follow-up.
A 36-year-old man presented with a small intradermal naevus above his left eyebrow. He had previously undergone multiple minor surgical procedures to correct perceived defects including 2 rhinoplasties and removal of a chickenpox scar. The index mole was small and inconspicuous, but was causing him such a high level of anxiety and distress that he stated he would “remove it himself with a kitchen knife”, if he was not offered excision. Significantly, he had been recently removed from his GP register for aggressive behaviour.
He had had a shave excision of the naevus due to the favourable risk:benefit ratio. He was also referred to health psychology, but he failed to attend.
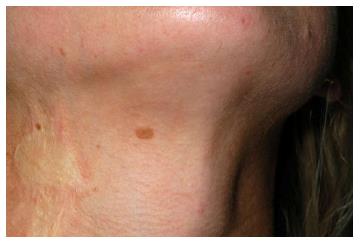
A 29-year-old woman presented with multiple small melanocytic naevi on her left check, neck and left lower lip. She appeared very self-conscious of the appearance of the moles and described them as “ugly”. She had adopted safety behaviours, such as covering her face with her hands regularly to hide the moles and constantly checking her appearance in the mirror. Her husband reassured her constantly that she “looked fine” and that he did not notice the moles.
Interestingly, she had a skin graft on her left neck following a burn in childhood adjacent to one of the problematic moles. However, the appearance of the graft did not seem to concern her, despite it being more obvious to the onlooker than the mole (Figure 1). She retained good insight of the fact that other people did not view the moles in the same way as she did. She had a shave biopsy of one mole and engaged in a course of cognitive behavioural therapy with good outcome.
An 18-year-old girl presented with a 1 cm congenital melanocytic naevus on her left thigh which she found “repulsive”.
She had become more concerned with the appearance over the past 4 years and had started to adopt avoidance behaviours, such as wearing tights and avoiding swimming, in order to conceal the appearance of the mole. She reported doing gymnastics as a child and being ashamed to wear a leotard out of fear that the mole would be exposed. She recalled that her mother had advised her to “cover it with a plaster”. She was reassured of the benign nature of the mole and warned of the risks of excision including unpredictable scarring, bleeding and surgical site infection. Nevertheless, she remained adamant that she “must have the mole removed”. She did not wish to undergo a psychological assessment. A separate referral was made by the GP to plastic surgery, who excised the mole.
A 16-year-old hairdresser presented with a mole on her left cheek. Over the past year she had become more aware of the mole. She described it as “dirty and horrible.” She stated that the mole was “all she could see when she looked in the mirror” and that she would be keen to remove it herself, if this was possible. She always wore heavy make-up and smiled as much as possible to try to hide the mole in the left nasolabial fold. She was advised of the risks of unpredictable scarring on a prominent part of the face and surgical intervention was not performed. She was offered referral to health psychology for further assessment and psychological therapy, but she declined.
A 16-year-old school girl presented with concern about the appearance of a small mole on her left infraclavicular skin which she had “hated” for 6 years. When she said or heard the word “mole” she her felt nauseous. She refused to expose the mole in public. She missed physical education classes and avoided wearing low-cut tops. On further enquiry, she also had significant concerns about several other aspects of her appearance, including “a big nose”, “large forehead, and “oily skin”, despite minimal objective findings. Depressive symptomatology with suicidal ideation were present. She did engage with clinical psychology and psychiatry and her psychological symptoms improved using a multidisciplinary approach (excision of the naevus, Cognitive Behavioural Therapy, and oral fluoxetine).
A 48-year-old woman presented with distress about the appearance of a mole on her cheek which had several terminal hairs growing within it. She thought about this mole every day and became anxious with social avoidance behaviours and ideas of reference, i.e., that people were noticing it and thinking it was “horrible”. She lived with a daily fear of negative evaluation of this mole. She had a past history of depressive disorder and panic attacks. A simple excision biopsy was performed. A discussion and psycho-education about body image and appearance distress was provided. The patient reported increased wellbeing 2 mo post-treatment at review.
A 28-year-old single woman demanded removal of multiple small moles from her body. She described these as “disgusting”. She claimed they had caused her to become depressed and unable to take appropriately care of her 3-year-old daughter on holiday. She said she had always “hated” her moles since her early teens. She avoided socialising and attributed this to her moles, which she considered “very ugly” and “making her look like a Dalmatian”. She blamed her moles for the fact that she can’t look after her child properly. She had a history of depressive disorder, self-harm and recreational drug misuse. She felt that removing all her moles would “fix” many of her problems in life. She threatened with suicide if she was refused excision. It was felt that her expectations were not realistic and a referral to health psychology was suggested in the first instance. However, she declined psychology referral and was lost to follow-up.
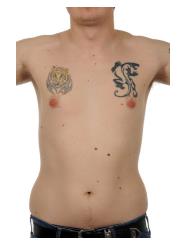
A 24-year-old single man, had asked his GP if he could have all his moles removed as he “hated” them so much. He said he’d “rather have lots of scars than lots of moles”. He was very anxious about going on holidays abroad, because he felt unable to take his top off at the beach or swimming pool. He attributed this to the shame he felt about his appearance. He avoided communal changing rooms or showers. He had a significant history of childhood psychological trauma.
On skin examination of his torso, several large tattoos were noticed (Figure 2). On further discussion he disclosed that he used tattoos to distract attention from the moles. In specific, he said that he “got tattooed to try and take people’s eye off the moles”, so they “noticed the tattoos more than the moles”. An excision biopsy of a naevus on the right flank was performed. This mole was particularly troubling him aesthetically. Efforts were also made to engage him in psycho-education about body image concerns. Referral to a Clinical/Health Psychologist was also suggested. However, the patient was lost to follow up.
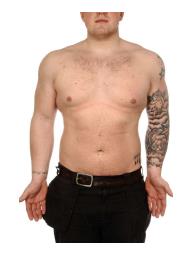
An 18-year-old man presented as extremely self-conscious about moles on his trunk, especially on his back, since the age of 13 years old. He said he had avoided swimming ever since. He exhibited several avoidance behaviours, e.g., persistently avoiding mirrors and refraining from using communal changing rooms. He was a body builder and had developed striae distensae around anterior axillary folds. On enquiry, he presented with considerable insight into his unhelpful perception about his skin and felt that his concerns may appear “stupid” to others. However, he was unable to change his beliefs and behaviours. He had a large circumferential tattoo on his left arm and another group of tattoos across his shoulders and right wrist (Figure 3). He said the reason for his tattoos was to distract his and others’ attention from the moles. However, despite this, he still thought about his moles every day, including the ones in the tattooed areas. Two naevi were excised from his back. Discussions around his body image were productive and advice on coping mechanisms was provided, whereas web-based cognitive behavioural therapy was suggested mainly to improve self-confidence and help reframing his negative thoughts about appearance.
This case series illustrates a range of manifestations of naevus dysmorphia. The discrepancy between objective/clinical (visibility of the naevus) and perceived “severity” is common to all cases, as are obsessive thoughts, preoccupation, and social anxiety/avoidance. The use of emotionally charged language, such as “horrible” or “disgusting”, to describe the appearance of the naevi is another common feature. Non-attendance at clinic follow-up was common, which may be due to avoidance or denial of underlying emotional issues perhaps. In some cases there was a history of negative life events. In some cases there was associated low mood, self-harm and suicidal ideation, as well as anger/frustration. In our clinical experience, in most cases, the issues around the egosyntonic nature of naevus dysmorphia were striking, i.e., the statements and experiences about the naevi and the skin are actually reflective of basic cognitions and emotions about the self. This is further demonstrated by the use of emotionally charged language these patients use to describe their naevi, i.e., “hate, ugly, horrible, disgusting, repulsive”, etc., which are indicative of their low self-worth and point towards deeply seated feelings of shame about the self. When such feelings are verbalised during appropriate treatment positive outcomes can occur with great relief[2].
As depressive symptomatology, anxiety, shame and guilt can be indicative of psychological trauma, one could suggest that the above presentations might be manifestations of previous or ongoing complex and relational psychological trauma presentations. Psychological trauma in skin disorders and dermatology in general is largely under-researched. Some of the authors are currently undertaking a pilot study to establish the prevalence of psychological trauma in dermatology (AF and ZC). The findings of this investigation will be presented elsewhere.
In put clinical experience, the self-concept of the individual underlies their presentation and may explain the range of reactions and prognosis. The self-concept, i.e., how we see ourselves and how we think others see us, is very complex and evolves across the lifespan, with many factors both genetic and acquired contributing. The self-concept may be especially brittle in adolescence when a degree of appearance concern is common[3].
Modern society’s rigid “Barbie doll” stereotypes of health and beauty likely contribute to unrealistic expectations regarding appearance, which contribute to appearance-related concerns[4]. Children and adolescents are exposed to images of certain body sizes and shapes portrayed by the media, where some features are depicted as more beautiful and desirable than others, e.g., being very slim, having “flawless skin”, no body or facial hair and looking eternally youthful[3]. Other influences on body dissatisfaction include parents’ beliefs and behaviours and peers/social interaction. Genetic and neurochemical factors may have a role to play. Previous psychological trauma, which may not have been previously disclosed, may also contribute to body image anxiety and associated low self-esteem. Psychological trauma could also account for persistent and treatment resistant symptoms of depression and anxiety. By adolescence, some individuals are so anxious about their appearance that they seek to alter it by seeking cosmetic surgery, dieting to lose weight, taking supplements or even anabolic steroids to increase muscle mass or performing excessive exercise regimens to try and achieve “the perfect figure”. These behaviours are thought to be a response to an internalised sociocultural appearance ideal[5].
“Clear” skin is considered beautiful and desirable by many adolescents especially girls. Any minor blemish, such as a mole, may be considered undesirable. In certain individuals, their beliefs, feelings and behaviours around the mole start to impact considerably on daily life.
When meeting a patient with disproportionate concern about the appearance of a small naevus, the dermatologist is called to be psychologically-minded and take a detailed history. Relational skills are vital with good communication being crucial in developing a therapeutic relationship based on person centred care, i.e., developing trust, empathy and acceptance of the patent's individual circumstances and needs.
A discussion around the topic of “body image concern” is useful in patient engagement. Appearance value and valence are important topics. In specific, a person may think he/she is not good looking, but, if appearance does not matter that much to them, then they will not be as distressed as someone else for whom appearance is a key aspect they use to define their self-worth. When “red flags” are found that suggest severe appearance distress and BDD[6], e.g., significant preoccupation, marked distress, lack of insight into the unrealistic nature of the cognitions about the naevus, extreme behaviours or avoidance related to the mole, regular checking behaviours, and large negative impact on daily life, then referral to psychiatry is desirable. However, in practice, the threshold for diagnosing BDD remains subjective and differentiation from “normal”-albeit excessive-appearance concern can be difficult.
The three diagnostic criteria for the diagnosis of BDD are[7]; (1) Preoccupation with some imagined defect in appearance or markedly excessive concern about a slight physical anomaly; (2) The preoccupation causes clinically significant distress or impairment in social, occupational or other important areas of functioning; and (3) The preoccupation is not better accounted for by another psychiatric disorder.
The presence of disabling anxiety or depressive symptomatology, excessive concern about other aspects of body image, history of psychological trauma, history of mental illness, history of extreme dieting or self-induced vomiting/use of laxatives and/or diuretics for weight control, suicidal ideation[8]/self harm or suicidal attempts should prompt further assessment by clinical psychology or psychiatry. An empathic non judgemental approach is needed to facilitate engagement. A discussion around and psycho-education about the pros and cons of surgically excision of the mole is necessary. In individual cases when the risk: benefit ratio is favourable then excision might be a reasonable and even beneficial course of action.
It is desirable for Dermatologists to have a good up-to-date understanding of the psychology of appearance and appearance concerns, over and above BDD alone. A proportion of 65% of patients with BDD will present with a perceived defect on their skin and will attend Dermatology outpatient clinics[9].
A study by Phillips had shown that 11.9% of 268 patients attending dermatology outpatients screened positive for body dysmorphic disorder which is significantly higher than the general population level of 1%-2%[10].
BDD is undoubtedly a serious concern in dermatology. However, an understanding of the wider range of appearance distress and body image dissatisfaction is also very important, if we are to make effective, safe and person centred clinical decisions. Management of patients with naevus dysmorphia is challenging. On one hand, simply reassuring the patient and discharging will often result in “doctor-shopping” for another opinion, in seeking private treatment or in often risky attempts of “home treatment”. On the other hand, simply excising the lesion will not cure the problem as it does not address the underlying body image concern and the vicious circle of anxiety, low mood and anxiety, which can eventually lead to “revolving door” effects or disengagement with health services. The situation needs to be handled gently and empathetically. It is essential that the patient feels that you are on their side and want to help, rather than against them. Therefore, engaging the patient is the first step, whereas normalization, i.e., explaining that other people have similar problems and have managed to manage effectively, as well as psycho-education about appearance distress and how best to cope with it are essential. Psychology referral might also be required for some patients. There are several treatment options which need to be tailored to the individual and the level of insight that they retain. These include surgical removal of the lesion, psychological therapies, and use selective serotonin uptake inhibitors. Several of these options can be used alone or in in combination and a pragmatic approach is often required.
Physical removal of a mole BDD is controversial. A study carried out by Philips examined medical or physical treatment, e.g., removal of a lesion in patients with BDD. Twelve out of 16 patients in the study had a lesion excised and 75% of these did not report a change in symptoms of BDD. However, a second study by Mühlbauer et al[11] showed that there was a subset of patients that would benefit from removal a lesion and derived criteria for excision of lesions in BDD patients. They found patients with mild BDD, and a minor lesion, with realistic expectations of a simple procedure for a real, albeit minor defect would benefit from surgical excision[11].
Ten patients with obsessive thoughts, social anxiety and behavioural changes related to a disproportionate distress about the appearance of a clinically small mole.
Patients with naevus dysmorphia clinically have a small benign naevus or a number of naevi.
The differential diagnosis is severe and often complex appearance concern or body dysmorphic disorder.
Removal of the naevus may be considered, but is cautioned when patient expectation is unrealistic and psychological “red flags” are present.
Readers can get further information from texts on body dysmorphic disorder and the psychology of appearance.
Dysmorphia–a disproportionate concern regarding an aspect of appearance [as been used in conjunction with muscle, acne and skin (cutaneous) previously in the literature].
The paper highlighted main challenges in patient engagement, the blurred boundary between expected and pathological appearance concern and the lack of evidence to know when excision of the mole is safe, reasonable and justified, and when it is cautioned or contraindicated. Dermatologists need to be aware of the discrepancy between perceived and clinical severity and how this is manifested in patients with suspected naevi dysmorphia and other similar types of appearance disturbances. Being able to assess psychological “red flags” within the context of a non-judgmental and trusting therapeutic relationship are key for safe, effective and person centred clinical management of patient with such difficulties.
This is an interesting case series report concerning one naevus dysmorphia which is a traumatic problem of many people in “postindustrial society”. The considerable value of this work is presentation of psychological and sociological aspects of this body dysmorphic disorders, because these questions are often passed over in publications concerning somatic diseases.
P- Reviewer: Bugaj AM, Guarneri F, Yap FBB S- Editor: Song XX L- Editor: A E- Editor: Lu YJ
| 2. | Wolf R, Ronat J, Feuerman EJ. Minor aesthetic blemishes: the patient’s unasked request. J Nerv Ment Dis. 1983;171:452-453. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 3. | Sebastian C, Burnett S, Blakemore SJ. Development of the self-concept during adolescence. Trends Cogn Sci. 2008;12:441-446. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 244] [Cited by in RCA: 244] [Article Influence: 15.3] [Reference Citation Analysis (0)] |
| 4. | Spitzer BL, Henderson KA, Zivian MT. Gender differences in population versus media body sizes: A comparison over four decades. Adolescence. 1999;24:677-87. |
| 5. | Gilbert P. The evolution of social attractiveness and its role in shame, humiliation, guilt and therapy. Br J Med Psychol. 1997;70:113-147. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 298] [Cited by in RCA: 215] [Article Influence: 7.7] [Reference Citation Analysis (0)] |
| 6. | Dufresne RG, Phillips KA, Vittorio CC, Wilkel CS. A screening questionnaire for body dysmorphic disorder in a cosmetic dermatologic surgery practice. Dermatol Surg. 2001;27:457-462. [PubMed] |
| 7. | American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. (DSM IV-TR). 4th ed. USA: American Psychiatric Publishing, Inc 2000; . |
| 8. | Cotterill JA. Dermatological non-disease: a common and potentially fatal disturbance of cutaneous body image. Br J Dermatol. 1981;104:611-619. [PubMed] |
| 9. | Phillips KA, Dufresne RG, Wilkel CS, Vittorio CC. Rate of body dysmorphic disorder in dermatology patients. J Am Acad Dermatol. 2000;42:436-441. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 178] [Cited by in RCA: 149] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 10. | Phillips KA, Grant J, Siniscalchi J, Albertini RS. Surgical and nonpsychiatric medical treatment of patients with body dysmorphic disorder. Psychosomatics. 2001;42:504-510. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 225] [Cited by in RCA: 189] [Article Influence: 7.9] [Reference Citation Analysis (0)] |
| 11. | Mühlbauer W, Holm C, Wood DL. The thersites complex in plastic surgical patients. Plast Reconstr Surg. 2001;107:319-326. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 15] [Article Influence: 0.6] [Reference Citation Analysis (0)] |