Published online Aug 18, 2016. doi: 10.5312/wjo.v7.i8.475
Peer-review started: February 16, 2016
First decision: March 24, 2016
Revised: April 5, 2016
Accepted: June 1, 2016
Article in press: June 3, 2016
Published online: August 18, 2016
Processing time: 184 Days and 6.6 Hours
AIM: To enhance non-technical skills and to analyse participant’s experience of a course tailored for orthopaedic surgeons.
METHODS: A Delphi technique was used to develop a course in human factors specific to orthopaedic residents. Twenty-six residents (six per course) participated in total with seven course facilitators all trained in Crisis Resource Management providing structured feedback. Six scenarios recreated challenging real-life situations using high-fidelity mannequins and simulated patients. Environments included a simulated operating suite, clinic room and ward setting. All were undertaken in a purpose built simulation suite utilising actors, mock operating rooms, mock clinical rooms and a high fidelity adult patient simulator organised through a simulation control room. Participants completed a 5-point Likert scale questionnaire (strongly disagree to strongly agree) before and after the course. This assessed their understanding of non-technical skills, scenario validity, relevance to orthopaedic training and predicted impact of the course on future practice. A course evaluation questionnaire was also completed to assess participants’ feedback on the value and quality of the course itself.
RESULTS: Twenty-six orthopaedic residents participated (24 male, 2 female; post-graduation 5-10 years), mean year of residency program 2.6 out of 6 years required in the United Kingdom. Pre-course questionnaires showed that while the majority of candidates recognised the importance of non-technical (NT) skills in orthopaedic training they demonstrated poor understanding of non-technical skills and their role. This improved significantly after the course (Likert score 3.0-4.2) and the perceived importance of these skills was reported as good or very good in 100%. The course was reported as enjoyable and provided an unthreatening learning environment with the candidates placing particular value on the learning opportunity provided by reflecting on their performance. All agreed that the course achieved its intended aims with realistic simulation scenarios. Participants believed patient care, patient safety and team working would all improve with further human factors training (4.4-4.6). and felt that NT skills learnt through simulation-based training should become an integral component of their training program.
CONCLUSION: Participants demonstrated improved understanding of non-technical performance, recognised its relevance to patient safety and expressed a desire for its integration in training.
Core tip: We have developed what we believe to be the first non-technical skills course specifically catering to the unique issues affecting orthopaedic surgeons in everyday practice. Participants demonstrated an improved understanding of the importance of non-technical performance, recognised its relevance to improving patient safety and expressed a desire for it to become an integral part of training. Non-technical skills training may also provide a means of identifying and supporting trainees in difficulty.
- Citation: Heaton SR, Little Z, Akhtar K, Ramachandran M, Lee J. Using simulation to train orthopaedic trainees in non-technical skills: A pilot study. World J Orthop 2016; 7(8): 475-480
- URL: https://www.wjgnet.com/2218-5836/full/v7/i8/475.htm
- DOI: https://dx.doi.org/10.5312/wjo.v7.i8.475
Non-technical (NT) skills are those abilities of a surgeon that may influence performance but do not relate directly to clinical knowledge or surgical technique. These “human factors” can be divided into cognitive skills or social skills and include situational awareness, decision-making, communication, teamwork and leadership[1].
Such interpersonal skills have traditionally been overlooked in training programs, with a premium placed on technical skills such as surgical dexterity, clinical expertise and factual knowledge. While these are essential factors in successful and safe patient interactions, there is increasing evidence that sub-optimal human factors can have negative effects on final patient outcomes. This can lead to adverse events during surgery and also during patient or staff interactions[2]. Communication errors have been shown to be causal factors for up to 43% of surgical errors[3], which suggests that technical skills alone are not sufficient to minimise risk sufficiently.
NT skills have already been noted to be of importance in non-medical fields and within some medical specialities. The National Aeronautics and Space Administration found that 70% of errors in the aviation industry were due to human factors such as failures in communication, leadership and decision-making[4]. This led to the development of Crew Resource Management (CRM) training in order to enable individuals to manage human performance limits and improve safety. CRM training has subsequently been adopted in the manufacturing, military and nuclear industries[5], civil aviation and oil exploration[6]. The anaesthetics community[7,8] has largely driven CRM in medicine with the development of Anaesthetic Crisis Resource Management[9]. This allows a participant to practice team-training skills in a simulated environment and then receive feedback on their performance. This has been well received with the significant majority of people confirming it has benefited their regular practice[10]. Cardiac surgery[11], operating room personnel[12,13], general surgery[14,15], nursing[16], obstetrics[17] and undergraduate medical curricula[18] are all increasingly recognising the importance of NT skills.
The Royal College of Surgeons of Edinburgh has produced a course designed for surgeons called NOTSS: Non-Technical Skills for Surgeons. It rates behaviour in surgeons and evaluates various non-technical skills with feedback given by consultants (attendings) based on structured observations[19]. A scoring system has been developed termed the Oxford Non-Technical Skills scale[20], which solely focuses on team work in an operating theatre. It is therefore somewhat surprising that the only specific orthopaedic communication roles in routine training are limited to the Advanced Trauma Life Support simulated moulages, which are still heavily loaded towards technical skills.
Twenty-six orthopaedic residents participated in total. The faculty consisted of three orthopaedic attendings, one senior resident and three full-time course facilitators from the department of medical simulation trained in Crisis Resource Management. Each course was undertaken with six participants and seven staff members.
The faculty used a Delphi technique[21] to devise six scenarios occurring in a realistic physical environment supported by a multidisciplinary team. These were based on actual events experienced by faculty members or reported in the General Medical Council archives[22] and were designed to immerse participants in the scenario and represent real-life challenging situations so as to test trainees’ NT skills across the range (Table 1).
| Setting | Scenario |
| Clinic | Discussing a surgical complication with an upset patient |
| Clinic | Breaking bad news to an anxious patient |
| Operating room | Managing a large team in crisis during a bone cement implantation reaction |
| Operating room | Dealing with an intoxicated senior colleague |
| Ward | Managing team members in a critically ill patient setting |
| Ward | Making a complex referral to an obstructive colleague |
Each participant agreed to be filmed for feedback purposes and signed a confidentially agreement. They then filled in a pre-course questionnaire about their understanding of NT skills. An introductory presentation was delivered by the course leader describing the aims of the course and the outline for the day’s activities.
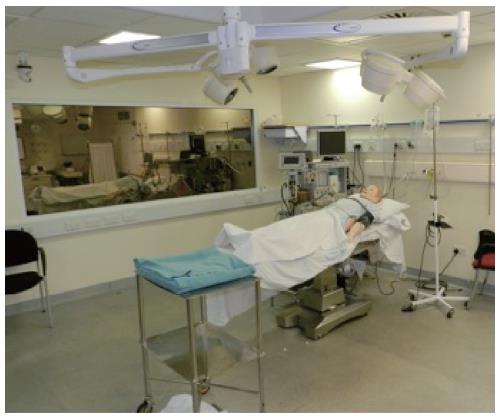
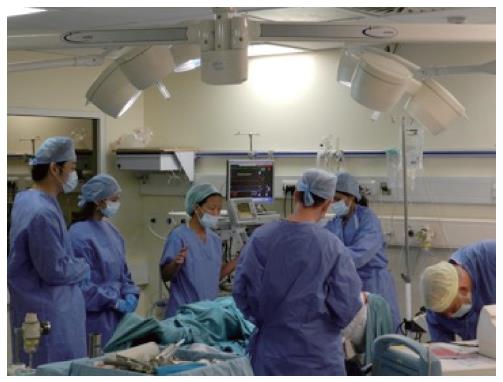
The scenarios were viewed directly through one-way screens by the other candidates and faculty members and were also concomitantly filmed for feedback purposes. Each scenario was undertaken in a purpose built simulation suite, which included a high fidelity adult patient simulator, actors as simulated patients, a mock operating room (Figure 1), outpatient clinic room or in-patient ward setting. All scenarios were controlled from the simulation control centre (Figures 2 and 3).
Two examples are described in detail below with the instructions for the candidate and the Simulated Patient plus the end point aims.
Discussing a surgical complication with an upset patient: (1) candidates brief. The patient has had an ankle fracture and a subsequent operation leading to chronic syndesmotic injury with pain. The original operation was poorly performed, leading to the current situation. The patient now needs revision surgery and returns to clinic today to discuss this. The patient has sent a complaint letter to the hospital demanding compensation and for the initial surgeon to be disciplined. The patient is unhappy with the response they have received; (2) patients brief: You have come back for your follow-up, which is to discuss the next part of your treatment. You are not satisfied by the response you have received, you feel entitled to compensation and you want that surgeon who did the operation to be suspended; and (3) end point aim: Empathises with patient, manages the situation and the patient appropriately, explains the hospital’s formal complaints procedure and how to proceed. Is aware of the formal complaints procedure. Comes to an acceptable management plan for the clinical problem.
Dealing with an intoxicated senior colleague: (1) candidates brief: You are in the operating room, the patient has received general anaesthesia and you are preparing to assist your attending in a total knee replacement. This is your first week working with this attending; (2) attending’s brief: Display signs of being intoxicated and inability to keep focus on the task. If candidate does not realise the situation then scrub nurse to take them aside and express concern. If candidate asks directly if you are drunk, deny it vehemently and express annoyance at their question; (3) scrub nurse: Wait for candidate to start scrubbing and whilst consultant is fiddling with setup, suggest to the candidate that the consultant is drunk. Tell the candidate in no uncertain terms that they must take action to protect patient safety; and (4) end point aim: To prevent the attending from operating. Arrange for another surgeon or decide to abandon the procedure and wake up the patient. Put patient safety first followed by duty of care to colleague. Plan for discussion with department director and suggest occupational health referral. Keep accurate and appropriate records (Figure 3).
All questions were answered on a 5 point Likert-type scale (strongly disagree to strongly agree). A questionnaire (Table 2) was designed to determine participants’ understanding of NT skills and their perceptions of the relevance and importance of these in orthopaedics, both before and after training.
| Please indicate how inclined you are to agree with the following statements |
| I have a good understanding of non-technical skills |
| Non-technical skills are important in orthopaedic training |
| Non-technical skills simulation should be an integral part of orthopaedic training |
A course evaluation questionnaire (Table 3) was designed to assess participants’ feedback on the value and quality of the course.
| Please indicate how inclined you are to agree with the following statements |
| I enjoyed this simulation day |
| It was useful to reflect on my performance |
| The course met the initial aims as presented in the introductory lecture |
| I thought the simulation scenarios were realistic |
| Simulation provided an unthreatening learning environment |
| This course will improve my team working |
| This course will improve my practice in terms of patient care |
| This course will improve my practice in terms of patient safety |
A debriefing session was conducted after each scenario, during which the participant reflected on their own performance and received constructive feedback from their peers and the faculty. Following debriefing after the final scenario of the day, the NT skills perception questionnaire was completed again, together with the course evaluation questionnaire.
Twenty-six participants took part, 24 were male and 2 were female (post-graduation 5-10). The mean year of training on the residency program was 2.6 (out of the 6 training years required in the United Kingdom).
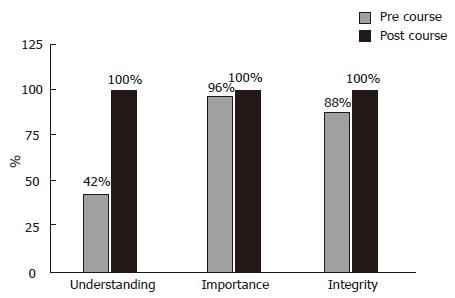
In terms of the understanding Prior to the course, the majority of participants recognised the importance of NT skills in orthopaedic training but only 42% reported a good understanding of them. The course increased the reported understanding of NT skills and further emphasised their importance in orthopaedic training. Moreover, all participants valued NT skills and thought that simulation-based training should become an integral component of orthopaedic training (Figure 4).
All participants enjoyed the course and valued reflecting on their performance. All agreed or strongly agreed that the course achieved its intended aims (Table 4).
| Please indicate how inclined you are to agree with the following statements | Agree or strongly agree (%) |
| I enjoyed this simulation day | 100 |
| It was useful to reflect on my performance | 100 |
| The course met the initial aims as presented in the introductory lecture | 100 |
| I thought the simulation scenarios were realistic | 92 |
| Simulation provided an unthreatening learning environment | 96 |
| This course will improve my team working | 88 |
| This course will improve my practice in terms of patient care | 88 |
| This course will improve my practice in terms of patient safety | 88 |
The majority found the simulation scenarios realistic and all but one reported that the course provided an unthreatening learning environment. Furthermore, 88% of participants agreed or strongly agreed that the course would improve their clinical practice in terms of team working, patient care and patient safety.
We have developed and piloted a new NT skills simulation course specifically for orthopaedic trainees. This simulation-based training was shown to provide a realistic, enjoyable and unthreatening learning environment and was well accepted by trainees. Course participants were able to reflect on their performances in various clinical scenarios and to improve their understanding of NT skills. The majority of those taking part felt that the course would improve team working and patient care. Their perception of the relevance of NT skills to orthopaedic training and their importance in clinical practice became more positive after experiencing the course. Participants demonstrated an improved understanding of the importance of non-technical performance, recognised its relevance to improving patient safety and expressed a desire for it to become a part of their training.
The purpose of this course was to provide teaching and feedback on NT skills specific to orthopaedic surgery with immersion in high fidelity environments simulating the operating room and outpatient clinic settings. The participants were shown the importance of NT skills in routine practice and were able to demonstrate and practice these skills in a safe environment, without posing risk to patients. They were able to critically evaluate their own performances and those of others, as well as receiving guided feedback from the experienced faculty. This allowed identification of areas for consolidation or improvement in order to prepare trainees for more senior clinical roles.
The importance of reflection in clinical training continues to grow and it is invaluable for surgeons of all grades to reflect on their own practice in order to ensure ongoing professional and personal development, as well as improvement in their practice.
It has been proposed that learners can be helped stepwise through this learning cycle by the creation of appropriate experiences and by assessment and feedback to facilitate transformation[23]. A training programme such as outlined in this paper can be one way of achieving this safely.
There is relatively little emphasis on NT skills in the orthopaedic literature, although their importance in obtaining successful clinical outcomes is clear and well recognised in many high-risk fields. We have described a way to use simulation to develop NT skills in orthopaedics in a risk-free environment and this was well received by trainees. Similar NT skills courses exist in other medical specialties, but this is the first we are aware of to focus specifically on the unique issues affecting orthopaedic surgeons. This course is becoming an integral component of our registrar training programme and may also provide a means for identifying and supporting the trainee in difficulty. There is growing evidence for NT skills to be embedded into the orthopaedic training curriculum and the use of simulation may be a means of achieving this.
We thank the Barts Simulation team who facilitated the course at the Education Academy Simulation centre at the Royal London Hospital.
Non-technical skills include situational awareness, decision-making, communication, teamwork and leadership. Evidence suggests these attributes are the key to reducing errors and avoiding adverse events.
Training in non-technical skills is widely used in many high-risk industries and some medical specialties. Simulation-based training in the orthopaedic community is based predominantly on technical skills such as dexterity with little emphasis on human factors training.
The authors have developed what they believe to be the first non-technical skills course specifically catering to the unique issues affecting orthopaedic surgeons in everyday practice.
Non-technical skills include situational awareness, decision-making, communication, teamwork and leadership.
The paper is very well presented.
Manuscript source: Invited manuscript
Specialty type: Orthopedics
Country of origin: United Kingdom
Peer-review report classification
Grade A (Excellent): 0
Grade B (Very good): B
Grade C (Good): 0
Grade D (Fair): 0
Grade E (Poor): 0
P- Reviewer: Drosos GI S- Editor: Qiu S L- Editor: A E- Editor: Wu HL
| 1. | Yule S, Flin R, Maran N, Rowley D, Youngson G, Paterson-Brown S. Surgeons’ non-technical skills in the operating room: reliability testing of the NOTSS behavior rating system. World J Surg. 2008;32:548-556. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 349] [Cited by in RCA: 328] [Article Influence: 19.3] [Reference Citation Analysis (0)] |
| 2. | Christian CK, Gustafson ML, Roth EM, Sheridan TB, Gandhi TK, Dwyer K, Zinner MJ, Dierks MM. A prospective study of patient safety in the operating room. Surgery. 2006;139:159-173. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 338] [Cited by in RCA: 314] [Article Influence: 16.5] [Reference Citation Analysis (0)] |
| 3. | Gawande AA, Zinner MJ, Studdert DM, Brennan TA. Analysis of errors reported by surgeons at three teaching hospitals. Surgery. 2003;133:614-621. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 709] [Cited by in RCA: 711] [Article Influence: 32.3] [Reference Citation Analysis (0)] |
| 4. | Helmreich RL, Merritt AC, Wilhelm JA. The evolution of Crew Resource Management training in commercial aviation. Int J Aviat Psychol. 1999;9:19-32. [PubMed] |
| 5. | Flin R, O’Connor P, Mearns K. Crew resource management: improving safety in high reliability industries. Team Performance Management. 2002;8:68-78. [RCA] [DOI] [Full Text] [Cited by in Crossref: 116] [Cited by in RCA: 66] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 6. | Flin R, Goeters K, Amalberti R. The development of the NOTECHS system for evaluating pilots’ CRM skills. Human Factors and Aerospace Safety. 2003;3:95-117. |
| 7. | Fletcher GC, McGeorge P, Flin RH, Glavin RJ, Maran NJ. The role of non-technical skills in anaesthesia: a review of current literature. Br J Anaesth. 2002;88:418-429. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 302] [Cited by in RCA: 265] [Article Influence: 11.5] [Reference Citation Analysis (0)] |
| 8. | Manser T, Harrison TK, Gaba DM, Howard SK. Coordination patterns related to high clinical performance in a simulated anesthetic crisis. Anesth Analg. 2009;108:1606-1615. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 85] [Cited by in RCA: 73] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 9. | Holzman RS, Cooper JB, Gaba DM, Philip JH, Small SD, Feinstein D. Anesthesia crisis resource management: real-life simulation training in operating room crises. J Clin Anesth. 1995;7:675-687. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 224] [Cited by in RCA: 182] [Article Influence: 6.1] [Reference Citation Analysis (0)] |
| 10. | Aggarwal R, Undre S, Moorthy K, Vincent C, Darzi A. The simulated operating theatre: comprehensive training for surgical teams. Qual Saf Health Care. 2004;13 Suppl 1:i27-i32. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 131] [Cited by in RCA: 104] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 11. | Wahr JA, Prager RL, Abernathy JH, Martinez EA, Salas E, Seifert PC, Groom RC, Spiess BD, Searles BE, Sundt TM. Patient safety in the cardiac operating room: human factors and teamwork: a scientific statement from the American Heart Association. Circulation. 2013;128:1139-1169. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 169] [Cited by in RCA: 188] [Article Influence: 15.7] [Reference Citation Analysis (0)] |
| 12. | Paige JT, Kozmenko V, Yang T, Gururaja RP, Hilton CW, Cohn I, Chauvin SW. Attitudinal changes resulting from repetitive training of operating room personnel using of high-fidelity simulation at the point of care. Am Surg. 2009;75:584-590; discussion 590-591. [PubMed] |
| 13. | Undre S, Koutantji M, Sevdalis N, Gautama S, Selvapatt N, Williams S, Sains P, McCulloch P, Darzi A, Vincent C. Multidisciplinary crisis simulations: the way forward for training surgical teams. World J Surg. 2007;31:1843-1853. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 160] [Cited by in RCA: 151] [Article Influence: 8.4] [Reference Citation Analysis (0)] |
| 14. | Powers KA, Rehrig ST, Irias N, Albano HA, Malinow A, Jones SB, Moorman DW, Pawlowski JB, Jones DB. Simulated laparoscopic operating room crisis: An approach to enhance the surgical team performance. Surg Endosc. 2008;22:885-900. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 65] [Cited by in RCA: 58] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 15. | Powers K, Rehrig ST, Schwaitzberg SD, Callery MP, Jones DB. Seasoned surgeons assessed in a laparoscopic surgical crisis. J Gastrointest Surg. 2009;13:994-1003. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 12] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 16. | Mitchell L, Flin R. Non-technical skills of the operating theatre scrub nurse: literature review. J Adv Nurs. 2008;63:15-24. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 112] [Cited by in RCA: 100] [Article Influence: 5.9] [Reference Citation Analysis (0)] |
| 17. | Robertson B, Schumacher L, Gosman G, Kanfer R, Kelley M, DeVita M. Simulation-based crisis team training for multidisciplinary obstetric providers. Simul Healthc. 2009;4:77-83. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 93] [Cited by in RCA: 93] [Article Influence: 5.8] [Reference Citation Analysis (0)] |
| 18. | Pilpel D, Schor R, Benbassat J. Barriers to acceptance of medical error: the case for a teaching program (695). Med Educ. 1998;32:3-7. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 38] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 19. | Flin R, Yule S, McKenzie L, Paterson-Brown S, Maran N. Attitudes to teamwork and safety in the operating theatre. Surgeon. 2006;4:145-151. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 124] [Cited by in RCA: 117] [Article Influence: 6.2] [Reference Citation Analysis (0)] |
| 20. | Mishra A, Catchpole K, McCulloch P. The Oxford NOTECHS System: reliability and validity of a tool for measuring teamwork behaviour in the operating theatre. Qual Saf Health Care. 2009;18:104-108. [PubMed] |
| 21. | de Villiers MR, de Villiers PJ, Kent AP. The Delphi technique in health sciences education research. Med Teach. 2005;27:639-643. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 471] [Cited by in RCA: 591] [Article Influence: 29.6] [Reference Citation Analysis (0)] |
| 22. | General Medical Council archives. [accessed 2014 Dec 8]. Available from: http: //www.gmc-uk.org/index.asp accessed 12/8/14. |
| 23. | Maudsley G, Strivens J. Promoting professional knowledge, experiential learning and critical thinking for medical students. Med Educ. 2000;34:535-544. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 243] [Cited by in RCA: 176] [Article Influence: 7.0] [Reference Citation Analysis (0)] |