Published online Jul 18, 2016. doi: 10.5312/wjo.v7.i7.452
Peer-review started: January 26, 2016
First decision: March 1, 2016
Revised: March 12, 2016
Accepted: May 10, 2016
Article in press: May 11, 2016
Published online: July 18, 2016
Processing time: 168 Days and 14.8 Hours
A 64-year-old-female presented with progressive left foot weakness, low back and radicular pain after a left sided S1 transforaminal epidural steroid injection (ESI). Magnetic resonance imaging revealed left side L5-S1 large extradural heterogeneous mass with layering areas suggesting different stages of hematoma formation. Past medical history was significant for peripheral vascular disease and transient ischemic attacks, for which she took aspirin and clopidogrel (antiplatelet agent). These medications were discontinued one week prior to ESI. Although synovial cysts associated with facet arthropathy are common, hemorrhagic cyst is not. To the best of the authors’ knowledge, this is the first reported case of symptomatic hemorrhagic lumbar facet synovial cyst following ESI on a patient taking anti-platelet medications.
Core tip: With modern advances in magnetic resonance imaging studies, synovial cysts are seen with degenerative lumbar facet disease. A symptomatic synovial cyst usually presents with a gradual onset low back pain originating from facet arthropathy and radicular pain or neurogenic claudication due to nerve roots compression. Previous reports showed synovial cyst can present with a progressive radicular pain and weakness secondary to spontaneous hemorrhage into the cyst. To the authors’ best knowledge, this is the first case report of iatrogenic hemorrhagic lumbar synovial cyst.
- Citation: Elgafy H, Peters N, Lea JE, Wetzel RM. Hemorrhagic lumbar synovial facet cyst secondary to transforaminal epidural injection: A case report and review of the literature. World J Orthop 2016; 7(7): 452-457
- URL: https://www.wjgnet.com/2218-5836/full/v7/i7/452.htm
- DOI: https://dx.doi.org/10.5312/wjo.v7.i7.452
Synovial cysts are relatively uncommon in the spine. Most cases are associated with facet joint arthritis and degenerative spondylolisthesis and occur most frequently at the L4-5 level. With modern advances in imaging studies, synovial cysts are becoming more evident as a common component of degenerative lumbar facet disease. Normally synovial cysts cause a gradual onset of symptoms that are typically indistinguishable from disc herniation or spinal stenosis[1,2]. The purpose of the current study was to present a case of progressive radicular pain and weakness secondary to hemorrhage into a lumbar synovial cyst after transforaminal epidural injection. To the authors’ best knowledge, this is the first case report of iatrogenic hemorrhagic lumbar synovial cyst.
A 64-year-old female patient was referred to the spine clinic with three weeks history of increasing low back pain radiating to the posterior aspect of the left thigh and leg. She also complained of a new-onset weakness in her left foot and difficulty with ambulation, which started after a left sided S1 transforaminal epidural steroid injection (ESI) that was performed by pain management physician. Past medical history was significant for hypertension, peripheral vascular disease and transient ischemic attacks, for which she took aspirin and clopidogrel (antiplatelet agent used in coronary artery disease, peripheral vascular disease, and cerebrovascular disease). These medications were discontinued one week prior to ESI. She had a several year history of L4-5 degenerative spondylolisthesis, multilevel disc degeneration and spinal stenosis and radiculopathy that had previously been effectively treated by ESI. Neurological examination revealed positive straight leg raise on the left side, diminished sensation over left L5, S1 nerve root dermatomes, and decreased motor strength (2/5) in extensor hallucis longus (EHL), plantar and dorsiflexion of the ankle on the left.
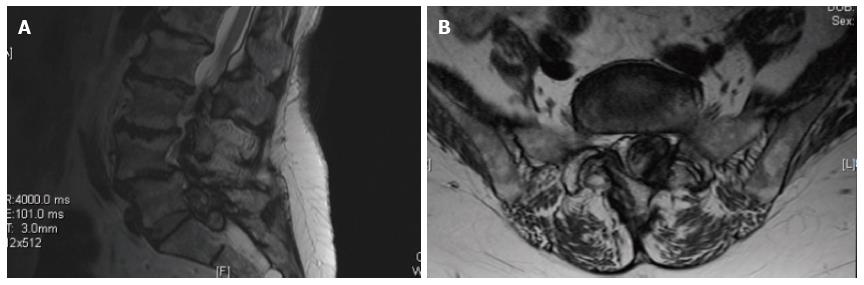
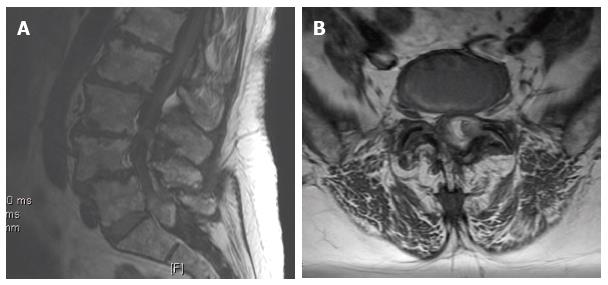
Plain radiographs showed severe multilevel disc degeneration and a grade I spondylolisthesis at L4-L5. Magnetic resonance imaging (MRI) showed an intraspinal extradural heterogeneous mass with decreased signal centrally within the T2 weighted sequences at L5-S1 on to the left side with displacement of the thecal sac to the right (Figure 1). In STIR images, the lesion appeared heterogeneous but predominantly low in signal intensity and in T1 weighted images, it showed heterogeneous increased signal and layering areas suggesting different stages of hematoma formation (Figure 2). Blood work including erythrocyte sedimentation rate, C-reactive protein, uric acid level, coagulation and platelet studies were within normal limits.
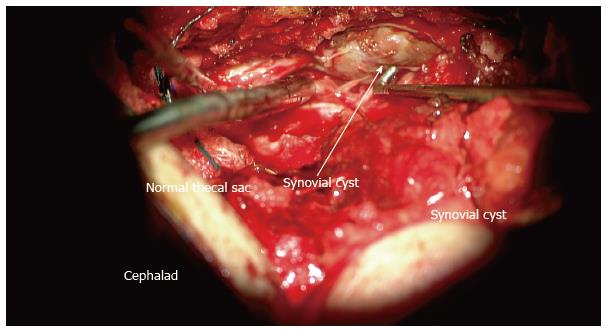
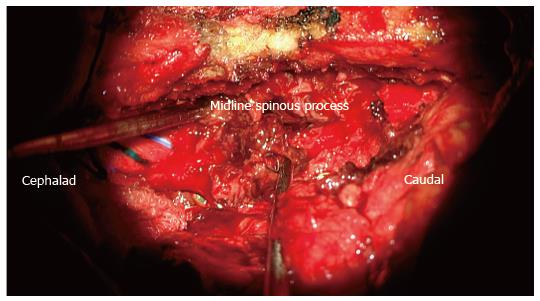
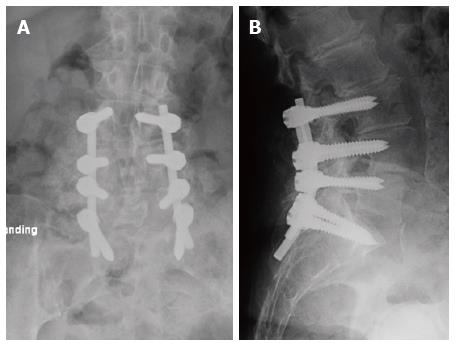
The working diagnosis was a hemorrhagic synovial cyst with a differential diagnosis of sequestrated disc, epidural metastasis and infection. Surgical treatment was indicated due to the increased back, leg pain, progressive left foot weakness and the severity of the spinal canal stenosis. The goal of the surgical treatment was decompression, excision of the lesion and L3-S1 instrumented fusion for the degenerative changes. The patient underwent L3-S1 midline sparing left side laminotomy, facetectomy and foraminotomy. The surgical microscope was used to identify the thecal sac above and below the lesion (Figure 3). Grossly, the lesion appeared to be a hematoma within a synovial cyst (Figure 4). This was impinging upon the transversing L5 and S1 nerve roots on the left side. The intraspinal cyst was then excised without sustaining any dural tear and L3-S1 instrumentation and posterolateral fusion performed for the degenerative lumbar spine (Figure 5). Postoperative histology assessment of the excised lesion confirmed the diagnosis of hematoma within a synovial cyst. At two weeks follow up, the patient’s radicular pain had resolved. Additionally, she had improved strength in EHL, plantar and dorsiflexion of the left ankle. Two months post-operatively, the patient regained full strength, denied any radicular or back pain and remained pain free at the last follow up at two years.
The most common location of intraspinal synovial cyst is L4-5 motion segment as it is the most mobile level allowing for more degeneration of the facet joint. Symptomatic synovial cysts present with low back pain originating from facet arthropathy and radicular pain or neurogenic claudication due to nerve roots compression[1-3]. The synovial cyst in the current case was located at L5-S1 rather than the most come L4-5 level with presenting symptoms of diminished sensation over left L5, S1 nerve root dermatomes and weakness of EHL, plantar and dorsiflexion of the left ankle. Acute exacerbation of the patient’s symptoms was related to hemorrhage inside the cyst. There are previous reports of spontaneous hemorrhage without epidural injection. However, in the current case report, the timing of the presenting symptoms supports the thought that introduction of a needle into a pre-existing synovial cyst had led to subsequent intra-cystic hemorrhage and onset of radicular symptoms and weakness.
To the best of the authors’ knowledge, there have been no published reports of hemorrhagic synovial cyst following ESI on a patient taking anti-platelet medications. There have been several reported cases of symptomatic epidural hematoma following ESI. The literature reports an incidence of 1:150000 to 1:220000 for epidural hematoma following epidural anesthesia, however the incidence following transforaminal ESI is not quantified[4-6].
MRI is the study of choice for diagnosing, however their radiographic characteristics vary in the literature. Acutely, the cysts have been described as appearing hypo-intense on T1 weighted images while appearing hyper-intense on T2 weighted images. However, in the more commonly imaged subacute period, both the T1 and T2 signals may appear as hyper- or hypo-intense depending on the intracystic methemoglobin and hemosiderin content and the amount of calcification in the cyst wall[7,8]. The current case showed heterogeneous signals in the T2 and T1 weighted images with the signal predominantly decreased in T2 and increased in T1 with layering areas, which is consistent with the subacute interval between the onset of symptoms and the timing of the MRI.
The mainstay of surgical treatment is excision of the cyst and decompression of the involved neural structures. The role of fusion at the time of cyst excision and decompression remains controversial in patients displaying preoperative spondylolisthesis. The need for fusion is influenced by symptomatic preoperative instability as evidenced by dynamic radiographs or intraoperative instability that may be created by iatrogenic resection of spinal structures such as the pars interarticularis or the facet joints[3]. Epstein et al[9] treated 80 patients with cyst excision and decompression without fusion. Thirty-five patients demonstrated preoperative Meyerding grade 1 spondylolisthesis. At two years follow up, 58% of patients who had no evidence of preoperative spondylolisthesis and 63% of patients with preoperative spondylolisthesis demonstrated good or excellent surgeon based outcomes. However, a moderate improvement was noted in only 2 of 8 SF-36 measures. Eleven patients had progression of listhesis and two patients required surgical stabilization. Bydon et al[10] in a systemic review noted that 811 patients (84%) underwent decompressive excision alone while 155 patients (16%) had concomitant fusion. They reported that 6.2% of the patients required further operative intervention, the majority of which were for instability and mechanical back pain. Additionally, they found that cyst recurrence occurred in 1.8% of patients who underwent decompression alone while no cases of recurrent cysts were found in patients who underwent fusion.
Surgical excision and decompression of lumbar cysts are not without complication. Banning et al[11] reported dural tear in 3 of 29 (9%) patients who underwent laminotomy and cyst excision. Larger cysts or cysts that are calcified due to chronicity can become adherent to the dura making their dissection more complex. Other reported complications include spinal nerve injury, epidural hematoma, seroma, and cyst recurrence[12].
Definitive diagnosis is typically reached by histologic examination. Hemorrhagic synovial cysts are characterized by hematologic, fibrous and endothelial elements. Hemosiderin or blood may be seen depending on the acuity and size of the hemorrhage[7,8,13]. The patient’s pathology in the current study demonstrated blood elements, fibrin and synovium consistent with the diagnosis of hemorrhagic synovial cyst.
Anticoagulation has been implicated in the pathogenesis of hemorrhagic cysts. Nourbakhsh et al[8] as well as Eck and Triantafyllou, reported cases of radiculopathy secondary to hemorrhagic cyst formation in patients taking warfarin. Both patients required surgical decompression and experienced postoperative resolution of their symptoms[8,13]. Spontaneous spinal epidural hematoma in patients taking anti-platelet medication has been reported in the literature[14-16]. Much research has been directed at spinal anesthesia in patients taking anti-thrombotic or anti-platelet medications. There is no current data that suggest low dose aspirin is associated with increased risk of epidural hematoma in the setting of a normal platelet count. Current guidelines set forth by the American Society of Regional Anesthesia and Pan Medicine call for cessation of clopidogrel 7 d prior to a neuraxial procedure such as ESI[17,18]. The patient presented in the current report had discontinued the anti-platelet medication in a manner consistent with published guidelines, and coagulation and platelet studies were within normal limits before the transforaminal ESI. However, the timing of the presenting symptoms as well as the radiographic and histologic findings support the thought that introduction of a needle into a pre-existing synovial cyst had led to subsequent intra-cystic hemorrhage and onset of radicular symptoms and weakness.
A 64-year-old female presented with progressive left foot weakness, low back and radicular pain after a left sided S1 transforaminal epidural steroid injection (ESI). Past medical history was significant for peripheral vascular disease and transient ischemic attacks, for which she took aspirin and clopidogrel (antiplatelet agent). These medications were discontinued one week prior to ESI.
Neurological examination revealed positive straight leg raise on the left side, diminished sensation over left L5, S1 nerve root dermatomes, and decreased motor strength (2/5) in extensor hallucis longus, plantar and dorsiflexion of the ankle on the left.
Sequestrated disc, epidural metastasis and infection.
Blood work including erythrocyte sedimentation rate, C-reactive protein, uric acid level, coagulation and platelet studies were within normal limits.
Plain radiographs showed severe multilevel disc degeneration and a grade I spondylolisthesis at L4-L5. Magnetic resonance imaging showed an intraspinal extradural heterogeneous mass with decreased signal centrally within the T2 weighted sequences at L5-S1 on to the left side with displacement of the thecal sac to the right.
The patient underwent midline sparing left side laminotomy, facetectomy and foraminotomy. The intraspinal cyst was then excised under the surgical microscope.
To the best of the authors’ knowledge, this is the first reported case of symptomatic hemorrhagic lumbar facet synovial cyst following ESI on a patient taking anti-platelet medications.
Intraspinal extradural synovial cysts are associated with facet joint arthritis and degenerative spondylolisthesis and occur most frequently at the L4-5 level.
Patients taking anticoagulation or anti-platelet medication should be informed that even if they stop their medication at the time recommended, there is still a possibility of intraspinal bleeding that may result in progressive neurological deficit after transforaminal ESI. Furthermore, transforaminal ESI may be avoided at the level, where a synovial cyst presents, to mitigate such a complication.
The authors present an interesting case of a hemorrhagic synovial cyst developing after a transforaminal epidural steroid injection.
Manuscript source: Invited manuscript
P- Reviewer: Bydon A, Peng BG, Recnik G, Sharma G, Tokuhashi Y S- Editor: Qiu S L- Editor: A E- Editor: Wu HL
| 1. | Wilby MJ, Fraser RD, Vernon-Roberts B, Moore RJ. The prevalence and pathogenesis of synovial cysts within the ligamentum flavum in patients with lumbar spinal stenosis and radiculopathy. Spine (Phila Pa 1976). 2009;34:2518-2524. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 26] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 2. | Shah RV, Lutz GE. Lumbar intraspinal synovial cysts: conservative management and review of the world’s literature. Spine J. 2003;3:479-488. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 99] [Cited by in RCA: 92] [Article Influence: 4.2] [Reference Citation Analysis (0)] |
| 3. | Sabo RA, Tracy PT, Weinger JM. A series of 60 juxtafacet cysts: clinical presentation, the role of spinal instability, and treatment. J Neurosurg. 1996;85:560-565. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 133] [Cited by in RCA: 132] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 4. | Stoll A, Sanchez M. Epidural hematoma after epidural block: implications for its use in pain management. Surg Neurol. 2002;57:235-240. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 78] [Cited by in RCA: 60] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 5. | Xu R, Bydon M, Gokaslan ZL, Wolinsky JP, Witham TF, Bydon A. Epidural steroid injection resulting in epidural hematoma in a patient despite strict adherence to anticoagulation guidelines. J Neurosurg Spine. 2009;11:358-364. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 39] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 6. | Shanthanna H, Park J. Acute epidural haematoma following epidural steroid injection in a patient with spinal stenosis. Anaesthesia. 2011;66:837-839. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 22] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 7. | Ramieri A, Domenicucci M, Seferi A, Paolini S, Petrozza V, Delfini R. Lumbar hemorrhagic synovial cysts: diagnosis, pathogenesis, and treatment. Report of 3 cases. Surg Neurol. 2006;65:385-390, discussion 390. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 34] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 8. | Nourbakhsh A, Garges KJ. Lumbar synovial joint hematoma in a patient on anticoagulation treatment. Spine (Phila Pa 1976). 2007;32:E300-E302. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 10] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 9. | Epstein NE. Lumbar laminectomy for the resection of synovial cysts and coexisting lumbar spinal stenosis or degenerative spondylolisthesis: an outcome study. Spine (Phila Pa 1976). 2004;29:1049-1055; discussion 1056. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 49] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 10. | Bydon A, Xu R, Parker SL, McGirt MJ, Bydon M, Gokaslan ZL, Witham TF. Recurrent back and leg pain and cyst reformation after surgical resection of spinal synovial cysts: systematic review of reported postoperative outcomes. Spine J. 2010;10:820-826. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 94] [Cited by in RCA: 98] [Article Influence: 6.5] [Reference Citation Analysis (1)] |
| 11. | Banning CS, Thorell WE, Leibrock LG. Patient outcome after resection of lumbar juxtafacet cysts. Spine (Phila Pa 1976). 2001;26:969-972. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 71] [Cited by in RCA: 69] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 12. | Lyons MK, Atkinson JL, Wharen RE, Deen HG, Zimmerman RS, Lemens SM. Surgical evaluation and management of lumbar synovial cysts: the Mayo Clinic experience. J Neurosurg. 2000;93:53-57. [PubMed] |
| 13. | Eck JC, Triantafyllou SJ. Hemorrhagic lumbar synovial facet cyst secondary to anticoagulation therapy. Spine J. 2005;5:451-453. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 22] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 14. | Wang L, Liu G, Subramaniam S, Wong TA, Kumar N. Spontaneous spinal epidural haematoma after antiplatelet treatment: a report of two cases. J Orthop Surg (Hong Kong). 2012;20:386-390. [PubMed] |
| 15. | Sung JH, Hong JT, Son BC, Lee SW. Clopidogrel-induced spontaneous spinal epidural hematoma. J Korean Med Sci. 2007;22:577-579. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 32] [Cited by in RCA: 31] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 16. | Lim SH, Hong BY, Cho YR, Kim HS, Lee JI, Kim HW, Ko YJ. Relapsed spontaneous spinal epidural hematoma associated with aspirin and clopidogrel. Neurol Sci. 2011;32:687-689. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 13] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 17. | Vandermeulen E. Regional anaesthesia and anticoagulation. Best Pract Res Clin Anaesthesiol. 2010;24:121-131. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 17] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 18. | Horlocker TT, Wedel DJ, Rowlingson JC, Enneking FK, Kopp SL, Benzon HT, Brown DL, Heit JA, Mulroy MF, Rosenquist RW. Regional anesthesia in the patient receiving antithrombotic or thrombolytic therapy: American Society of Regional Anesthesia and Pain Medicine Evidence-Based Guidelines (Third Edition). Reg Anesth Pain Med. 2010;35:64-101. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 896] [Cited by in RCA: 670] [Article Influence: 44.7] [Reference Citation Analysis (0)] |