Peer-review started: May 15, 2014
First decision: June 27, 2014
Revised: July 9, 2014
Accepted: July 27, 2014
Article in press: July 29, 2014
Published online: January 18, 2015
Processing time: 250 Days and 15.8 Hours
Technique of subtalar arthroscopy is rapidly evolving. Increasing number of traditional open procedures for the subtalar joint can now be done arthroscopically. It is hoped that less wound complications, faster rehabilitation and better cosmetic outcomes can be achieved with this minimally invasive technique.
Core tip: With the advance of small joint arthroscopy, different zones of the anterior and posterior subtalar joint can be approached arthroscopically. These can widen the list of indications for the subtalar arthroscopy.
- Citation: Lui TH, Tong SC. Subtalar arthroscopy: When, why and how. World J Orthop 2015; 6(1): 56-61
- URL: https://www.wjgnet.com/2218-5836/full/v6/i1/56.htm
- DOI: https://dx.doi.org/10.5312/wjo.v6.i1.56
Subtalar arthroscopy was first described in 1980s. After its introduction, subtalar arthroscopy has been employed in various diagnostic and therapeutic procedures. The list of its application is ever expanding. With proper use of this powerful tool, many traditional procedures can be done minimally invasively to reduce wound complications and to achieve better outcomes.
In 1985, Parisien et al[1] published their experience in experimental subtalar arthroscopy in six lower limb cadaver specimens. They described anterior and posterior portals for approaching the posterior facet of subtalar joint using 2.7-mm arthroscope. They concluded that subtalar arthroscopy would be possibly indicated in assessment of the state of subtalar joint cartilage in cases of degenerative arthritis and infection; visualization of the joint after intraarticular fracture; management of sinus tarsi syndrome as well as loose body removal.
Frey et al[2] introduced the middle portals for subtalar arthroscopy in 1994. She discussed the relative safety of the anterior, middle and posterior portals by measuring their distance from neurovascular structures and tendons on lateral side of the foot in 15 specimens.
Since its introduction, subtalar arthroscopy has thrived. The list of indications for its application is continuously expanding to include different diagnostic and therapeutic purposes.
Patient positioning: Standard posterior subtalar arthroscopy can be performed under spinal or general anaesthesia. It can be performed with the patient in lateral, prone or supine position depending on the concomitant procedures needed. Distraction is not routinely required.
Instruments: The subtalar joint can be approached with 30 degrees 2.7-mm arthroscope. Siddiqui et al[3] has also reported the use of 2.4-mm zero-degree arthroscope for subtalar arthroscopy.
Portals: The tip of the lateral malleolus is the landmark for portal placement. Anterolateral portal is made just above the angle of Gissane and is about 2 cm anterior and 1cm distal to fibular tip. Posterolateral portal is made at the lateral side of the Achilles tendon just above the posterosuperior calcaneal tubercle and is about 2 cm posterior and 1cm proximal to fibular tip. Middle portal is placed just anterior to the tip of fibula. All the portals are made with the “nick and spread” technique.
The abovementioned portals can only approach the lateral part of the subtalar joint. To approach the posteromedial part of the posterior subtalar joint, posterolateral and posteromedial portals can be used[4-7]. These portals are made when posterior ankle arthroscopy together with subtalar arthroscopy is performed.
Patient positioning: Patient is prone position with a thigh tourniquet.
Portals: With the foot in neutral position, a straight line is drawn parallel to the sole at the level fibular tip. The posterolateral portal is made just proximal to this line and tangential to the lateral border of the Achilles tendon. It should be just above the superoposterior calcaneal tubercle. The posteromedial portal is made at the same level just medial to the medial border of the Achilles tendon. In case of zone 2 flexor hallucis longus tendoscopy is planned, the posteromedial portal would be at the point of intersection of the medial border of the Achilles tendon and the projection line at the inferior border of 1st metatarsal and substentaculum tali
Apart from posterior talocalcaneal articulation, the subtalar joint also consists of the anterior talocalcaneonavicular articulation. It includes the posterior articular facet of the navicular bone, the plantar spring ligament, the anterior and middle facet of the talus. This articulation is separated from the posterior articulation by the tarsal tunnel and sinus tarsi. The posterior articulation has a separate joint capsule and does not communicate with the anterior articulation.
Traditionally, to expose this anterior articulation, extensive medial approach is required. Anterior subtalar arthroscopy to treat anterior subtalar joint pathologies has been reported in 2008[8].
Patient positioning: The positioning is the same as standard subtalar arthroscopy. Lateral position is the most preferred one and the prone position is the least preferred one.
Portals: Primary visualization portal slightly dorsal to the angle of Gissane (consistent with the anterolateral portal of posterior subtalar arthroscopy). Primary working portal (consistent with the dorsolateral midtarsal portal for arthroscopic triple arthrodesis, see later) at the junction between the talonavicular and calcaneocuboid joints. These portals can be located by a needle and checked under fluoroscopy. The portals are interchangeable.
Surgical technique: Using a 2.7 mm, 30-degree arthros-cope and arthroscopic shaver, the soft tissue at the junction between the talonavicular joint and calcaneocuboid joint is removed. The inferior corner of the lateral talar head will then be exposed. The talar head contour is then traced dorsally to the talonavicular joint and proximally to the anterior and middle calcaneal facets. This technique requires only resection of lateral capsule of the talonavicular joint. Most of the important ligamentous structures of the sinus tarsi are preserved.
This anterior arthroscopy technique has been applied in resection of symptomatic talocalcaneal coalition and synovectomy for the middle calcaneal facet synovitis.
With these two portals, an average of 95% of the anterior subtalar articulations can be reached[9]. Sural nerve is located at an average distance of 13 mm plantar to the primary working portal whereas the dorsal intermediate branch of the superficial peroneal nerve is at an average distance of 10 mm medial to the primary working portal.
Even with all the portals described, the anteromedial part of posterior subtalar joint and the medial gutter of the anterior subtalar joint are still relatively inaccessible. In order to achieve an all-around subtalar arthroscopy, medial portals are therefore required. Mekhail et al[10] described a medial portal for subtalar arthroscopy in his cadaveric study in 1995. Clinical application of the medial subtalar arthroscopy has been reported in 2012[11].
Patient positioning: Patient is in supine position with the hip abducted.
Portals: Medial subtalar portals include the standard posteromedial portal, locating at medial border of Achilles tendon; The medial midtarsal portal, which is just above the tibialis posterior tendon insertion onto the navicular tubercle; And the medial tarsal canal portal.
Surgical technique: The medial tarsal canal portal is made with inside-out technique. The lateral portion of the tarsal canal is first cleared up with shaver via the anterolateral and middle portals for standard subtalar arthroscopy. The lateral opening of the tarsal canal is then identified. Under arthroscopic guidance, a Kirschner wire is inserted into the tarsal canal. The position of the Kirschner wire is confirmed with fluoroscopy. The medial tarsal canal portal can then be made on medial side of the foot. The foot is kept pronated so that the medial end of the tarsal canal opens to allow passage of arthroscopic instruments.
Lui et al[12] evaluated the safety of the tarsal canal portal and found that there is risk of injury to the flexor digitorum longus tendon and the posterior tibial neurovascular bundle. It is advised that when making the medial tarsal canal portal, it is better to align the Kirschner wire/Wissenger rod anteromedially to reduce the chance neurovascular injury. The tarsal canal portal should be used with caution.
Restoring articular congruity of the subtalar joint improves the outcome of calcaneal fractures. Traditionally, this is achieved by open reduction and internal fixation using the standard lateral extensile approach[13-15]. The major drawback of the open approach is wound complications including infection, wound dehiscence, haematoma and wound edge necrosis[16-19]. To minimize these complications, minimally invasive technique was developed to treat calcaneal fractures. Subtalar arthroscopy complements intra-operative fluoroscopy for anatomical reduction of articular surface[20-22].
Surgical technique: After manipulation and temporary fixation of the fracture fragments percutaneously with K-wires or pins, the subtalar cartilage congruity can be checked with subtalar arthroscopy. Fixation can then be accomplished with screws.
Outcome: Rammelt et al[22] reported no wound complications in his series of 18 patients with calcaneal fractures treated with arthroscopically assisted percutaneous reduction and fixation. Similarly, Schuberth et al[20] reported no soft tissue complications in his 10 patients treated with percutaneous fixation under arthroscopic assistance.
Arthroscopic subtalar arthrodesis was first developed by Tasto[23] in 1992. The arthroscopic technique was intended to yield less morbidity and preserve blood supply, as well as preserve proprioception and neurosensory input of the subtalar joint. Tasto[23] reported that all 25 patients of his series have radiological and clinical union, with the average time of fusion of 8.9 wk.
Surgical technique: The procedure can be done with the patient in lateral or prone position under general or regional anaesthesia. Supine position is less favorable for the screw placement. Standard portals include the anterolateral portal and the middle portal. Accessory portals are sometimes used for better instrumentation or visualization[24]. Posterolateral and posteromedial portals can also be used for subtalar arthrodesis. Bone graft/bone substitute is not usually required. Fixation can be accomplished with one or two cannulated screws inserted in either antegrade or retrograde fashion under X-ray control[23-25].
Outcome: Lee reported 16 cases of post-traumatic subtalar arthritis after calcaneal fracture treated with subtalar arthrodesis using the posterior 2-portal approach in prone position[25]. The union rate was 94% at a mean of 11 wk in his series.
Subtalar arthroscopy also has a role in triple arthrodesis. Traditionally, triple arthrodesis is done in open fashion with extensive surgical exposure. With the advancement of arthroscopic technique, triple arthrodesis can now be done arthroscopically.
The advantage of having arthrodesis done arthroscopically is that it allows better intra-articular visualization, more complete cartilage debridement, preservation of subchondral bone and better cosmetic results[26]. Arthroscopic triple arthrodesis has been reported in 2006[27].
Surgical technique: The subtalar joint is approached with anterolateral and middle portals. The mid-tarsal joints are approached with lateral, dorsolateral (i.e., working portal for anterior subtalar arthroscopy), dorsomedial and medial portals. Articular cartilage is denuded with a small periosteal elevator, arthroscopic curette and arthroscopic osteotome. The subchondral bone is then microfractured with an arthroscopic awl. Fixation is accomplished with 7.3 mm cannulated screw for the subtalar joint and 4.0 mm cannulated screws for the mid-tarsal joints. The junction space between the talus, navicular, calcaneus and cuboid is packed with autologous cancellous bone graft harvested from the ipsilateral iliac wing.
Outcome: Lui applied this technique to a patient with post-polio equinovarus deformity[27]. Solid fusion was achieved 4 mo after the procedure. In 2009, Lui[28] reported his results of arthroscopic triple arthrodesis for 10 feet with Muller Weiss disease. Solid fusion was achieved in average of 21 wk. There were no wound complications or neurovascular injury. The limit of the degree of deformity correction with this arthroscopic approach is yet to be determined although the degree of deformity correction have been increased by “closing wedge procedure” [29,30].
Apart from treating intra-articular pathologies, endoscopy can be employed in treating extra-articular pathologies, in particular, complications of calcaneal fractures[29].
Calcaneofibular impingement: Lateral calcaneal cortical bulging frequently occurs in patients whose calcaneal fracture are treated conservatively. This can cause calcaneofibular or peroneal impingement syndrome or shoe wear problems. Typically, patients complain of pain under the tip of lateral malleolus. Physical examination reveals tenderness on palpation under the tip of the fibula. Hindfoot valgus test may provoke the pain. The diagnosis can be confirmed with CT scan[31]. Lateral calcaneal ostectomy should be considered if conservative treatment cannot relieve the symptoms[32-34].
Traditionally, lateral calcaneal ostectomy is performed as an open procedure. It is important to have adequate removal of lateral bone in order to decompress the calcaneofibular recess and the far lateral arthrosis should be excised in order to have good clinical results[35]. Examination of the entire subtalar joint posterior facet can be difficult with open procedure. Excessive or inadequate debridement of cartilage may result. Endoscopic lateral calcaneal ostectomy for calcaneofibular impingement has been reported in 2007[36].
Surgical technique: Subtalar joint is examined with anterolateral and middle subtalar portals using 2.7 mm 30 degrees arthroscope. After dealing with the intra-articular pathology, lateral calcaneal ostectomy is performed using 4.0 mm 30 degrees arthroscopy and acrominizer. Lateral subtalar capsule and lateral subtalar ligamentous structures are stripped from lateral calcaneal cortical surface with arthroscopic shaver or a small periosteal elevator in the middle portal. A plantar portal, locating at plantar border of lateral calcaneal cortex (plantar to the cortical bulge), is used to approach the plantar half of the lateral cortical bulge. Posterolateral portal is sometimes required for complete soft tissue stripping. By switching the portals for visualization and instrumentation, complete lateral bulge ostectomy can be achieved. With this minimal invasive approach, wound complication can be reduced and immediate subtalar mobilization can be started without risking the wound healing.
Bauer et al[31] also described his two-portals endoscopic technique for treating calcaneofibular impingement in 2011. Apart from excising the lateral cortical bulge, scar tissue and fibrosis on the lateral cortex of the calcaneus and around lateral malleolus is excised. The peroneal tendons are also debrided along its course from retromalleolar groove and then distally.
Subtalar arthroscopy can also be used to treat post-traumatic subtalar stiffness[29,37].
Surgical technique: Under posterior subtalar arthroscopy, fibrous bands at sinus tarsi and dense fibrous tissue of lateral subtalar gutter can be debrided. The most lateral part of the interosseous talocalcaneal ligament is released. Posterior capsule release and debridement of fibrous tissue at posterior corner of subtalar joint can then be carried out. Finally, lateral subtalar capsule and lateral subtalar ligamentous structures are stripped from lateral calcaneal surface to regain subtalar motion.
Some tarsal coalitions can also been treated arthroscopically. Lui described his arthroscopic technique in resection of calcaneonavicular coalition or the “ too long” anterior process of calcaneus with 2 portals (i.e., visualization portal and working portal for anterior subtalar arthroscopy)[38]. Bonasia used posteromedial and posterolateral portals for resection of talocalcaneal coalition arthroscopically[5]. Field has also reported his technique of arthroscopic assisted resection of middle facet coalition in 2009.
Lateral approach and posterior approach are the standard approaches for subtalar arthroscopy. With the lateral approach, majority of the posterior subtalar joint can be visualized except the medial part of posterior subtalar joint.
There are two solutions for this problem. Firstly, a combined posterior and lateral approach can be done with the patient put in prone position. Secondly, joint distraction can be applied[5]. However, traction can increase the tension of the neurovascular structures as well. In majority of time, it would distract the ankle joint rather than the subtalar joint.
Anterior subtalar joint cannot be reached with the standard middle, anterolateral portals due to the ligamentous structures at the sinus tarsi and the thick intraosseous ligaments inside the tarsal canal. In order to perform anterior subtalar arthroscopy, two other portals have to be established as described above. The portals tracts are along the lateral border of the anterior subtalar joint and the anterior border of the posterior subtalar joint. This can avoid damage of the important ligaments of the sinus tarsi[8,9]. However, with these extra portals, only the lateral anterior subtalar joint can be reached. The medial part of the anterior subtalar joint can just be seen but cannot be reached.
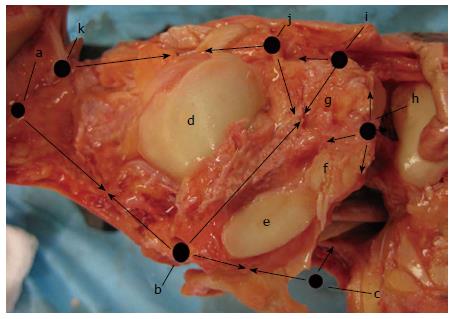
With the development of medial subtalar arthroscopy, medial part of the anterior and posterior subtalar joint, tarsal canal can now be reached. Medial tarsal canal portal and the medial midtarsal portal are established with the medial tarsal canal portal being the keystone portal for medial subtalar arthroscopy (Figure 1). The main indication of medial subtalar arthroscopy is extensive synovitis in tarsal canal and medial anterior subtalar joint. Structures at risk during medial subtalar arthroscopy include flexor digitorum longus tendon, posterior tibial neurovascular bundles and medial talar branch of the posterior tibial artery.
In order to prevent damage to these structures, portal tract of medial tarsal canal should be made anterior to the flexor digitorum longus tendon, immediately behind the posterior tibial tendon. During insertion of the guide rod, it should be directed anteromedially with foot in pronation to open up the medial orifice of the tarsal canal[11]. During medial subtalar arthroscopy, the medical capsule should not be stripped dorsally to prevent injury to the medial talar branch of the posterior tibial artery[11].
Technique of subtalar arthroscopy is continuously evolving. With the advancement of the arthroscopic technique, increasing number of traditional open procedures can now be done arthroscopically. This allows less soft tissue dissection, better cosmesis and shorter duration of recovery.
P- Reviewer: Nikolaou VS S- Editor: Song XX L- Editor: A E- Editor: Wu HL
| 1. | Parisien JS, Vangsness T. Arthroscopy of the subtalar joint: an experimental approach. Arthroscopy. 1985;1:53-57. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 93] [Cited by in RCA: 70] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 2. | Frey C, Gasser S, Feder K. Arthroscopy of the subtalar joint. Foot Ankle Int. 1994;15:424-428. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 83] [Cited by in RCA: 58] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 3. | Siddiqui MA, Chong KW, Yeo W, Rao MS, Rikhraj IS. Subtalar arthroscopy using a 2.4-mm zero-degree arthroscope: indication, technical experience, and results. Foot Ankle Spec. 2010;3:167-171. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 6] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 4. | Beimers L, de Leeuw PA, van Dijk CN. A 3-portal approach for arthroscopic subtalar arthrodesis. Knee Surg Sports Traumatol Arthrosc. 2009;17:830-834. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 63] [Cited by in RCA: 51] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 5. | Bonasia DE, Phisitkul P, Saltzman CL, Barg A, Amendola A. Arthroscopic resection of talocalcaneal coalitions. Arthroscopy. 2011;27:430-435. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 37] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 6. | Amendola A, Lee KB, Saltzman CL, Suh JS. Technique and early experience with posterior arthroscopic subtalar arthrodesis. Foot Ankle Int. 2007;28:298-302. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 104] [Cited by in RCA: 80] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 7. | Field C, Ng A. Resection of middle facet coalition with arthroscopic guidance. J Foot Ankle Surg. 2009;48:273-276. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 16] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 8. | Lui TH. Clinical tips: anterior subtalar (talocalcaneonavicular) arthroscopy. Foot Ankle Int. 2008;29:94-96. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 35] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 9. | Lui TH, Chan KB, Chan LK. Portal safety and efficacy of anterior subtalar arthroscopy: a cadaveric study. Knee Surg Sports Traumatol Arthrosc. 2010;18:233-237. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 34] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 10. | Mekhail AO, Heck BE, Ebraheim NA, Jackson WT. Arthroscopy of the subtalar joint: establishing a medial portal. Foot Ankle Int. 1995;16:427-432. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 31] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 11. | Lui TH. Medial subtalar arthroscopy. Foot Ankle Int. 2012;33:1018-1023. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 20] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 12. | Lui TH, Chan LK, Chan KB. Medial subtalar arthroscopy: a cadaveric study of the tarsal canal portal. Knee Surg Sports Traumatol Arthrosc. 2013;21:1279-1282. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 23] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 13. | Zwipp H, Tscherne H, Thermann H, Weber T. Osteosynthesis of displaced intraarticular fractures of the calcaneus. Results in 123 cases. Clin Orthop Relat Res. 1993;76-86. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 115] [Cited by in RCA: 87] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 14. | Benirschke SK, Sangeorzan BJ. Extensive intraarticular fractures of the foot. Surgical management of calcaneal fractures. Clin Orthop Relat Res. 1993;128-134. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 290] [Cited by in RCA: 229] [Article Influence: 7.2] [Reference Citation Analysis (0)] |
| 15. | Stephenson JR. Treatment of displaced intra-articular fractures of the calcaneus using medial and lateral approaches, internal fixation, and early motion. J Bone Joint Surg Am. 1987;69:115-130. [PubMed] |
| 16. | Abidi NA, Dhawan S, Gruen GS, Vogt MT, Conti SF. Wound-healing risk factors after open reduction and internal fixation of calcaneal fractures. Foot Ankle Int. 1998;19:856-861. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 59] [Cited by in RCA: 56] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 18. | Folk JW, Starr AJ, Early JS. Early wound complications of operative treatment of calcaneus fractures: analysis of 190 fractures. J Orthop Trauma. 1999;13:369-372. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 288] [Cited by in RCA: 257] [Article Influence: 9.9] [Reference Citation Analysis (0)] |
| 19. | Watson TS. Soft tissue complications following calcaneal fractures. Foot Ankle Clin. 2007;12:107-123. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 26] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 20. | Schuberth JM, Cobb MD, Talarico RH. Minimally invasive arthroscopic-assisted reduction with percutaneous fixation in the management of intra-articular calcaneal fractures: a review of 24 cases. J Foot Ankle Surg. 2009;48:315-322. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 73] [Cited by in RCA: 71] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 21. | Gavlik JM, Rammelt S, Zwipp H. The use of subtalar arthroscopy in open reduction and internal fixation of intra-articular calcaneal fractures. Injury. 2002;33:63-71. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 66] [Cited by in RCA: 60] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 22. | Rammelt S, Gavlik JM, Barthel S, Zwipp H. The value of subtalar arthroscopy in the management of intra-articular calcaneus fractures. Foot Ankle Int. 2002;23:906-916. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 109] [Cited by in RCA: 81] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 23. | Tasto JP. Arthroscopy of the subtalar joint and arthroscopic subtalar arthrodesis. Instr Course Lect. 2006;55:555-564. [PubMed] |
| 24. | El Shazly O, Nassar W, El Badrawy A. Arthroscopic subtalar fusion for post-traumatic subtalar arthritis. Arthroscopy. 2009;25:783-787. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 41] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 25. | Lee KB, Park CH, Seon JK, Kim MS. Arthroscopic subtalar arthrodesis using a posterior 2-portal approach in the prone position. Arthroscopy. 2010;26:230-238. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 49] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 26. | Lui TH, Chan LK. Safety and efficacy of talonavicular arthroscopy in arthroscopic triple arthrodesis. A cadaveric study. Knee Surg Sports Traumatol Arthrosc. 2010;18:607-611. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 33] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 27. | Lui TH. New technique of arthroscopic triple arthrodesis. Arthroscopy. 2006;22:464.e1-464.e5. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 52] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 28. | Lui TH. Arthroscopic triple arthrodesis in patients with Müller Weiss disease. Foot Ankle Surg. 2009;15:119-122. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 54] [Cited by in RCA: 52] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 29. | Lui TH, Chan KB. Arthroscopic management of late complications of calcaneal fractures. Knee Surg Sports Traumatol Arthrosc. 2013;21:1293-1299. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 19] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 30. | Lui TH. Case report: correction of neglected club foot deformity by arthroscopic assisted triple arthrodesis. Arch Orthop Trauma Surg. 2010;130:1007-1011. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 19] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 31. | Bauer T, Deranlot J, Hardy P. Endoscopic treatment of calcaneo-fibular impingement. Knee Surg Sports Traumatol Arthrosc. 2011;19:131-136. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 15] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 32. | Braly WG, Bishop JO, Tullos HS. Lateral decompression for malunited os calcis fractures. Foot Ankle. 1985;6:90-96. [PubMed] |
| 33. | Clare MP, Lee WE, Sanders RW. Intermediate to long-term results of a treatment protocol for calcaneal fracture malunions. J Bone Joint Surg Am. 2005;87:963-973. [PubMed] |
| 34. | Stephens HM, Sanders R. Calcaneal malunions: results of a prognostic computed tomography classification system. Foot Ankle Int. 1996;17:395-401. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 111] [Cited by in RCA: 92] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 35. | Myerson M, Quill GE. Late complications of fractures of the calcaneus. J Bone Joint Surg Am. 1993;75:331-341. [PubMed] |
| 36. | Lui TH. Endoscopic lateral calcaneal ostectomy for calcaneofibular impingement. Arch Orthop Trauma Surg. 2007;127:265-267. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 20] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 37. | Lui TH. Arthroscopic subtalar release of post-traumatic subtalar stiffness. Arthroscopy. 2006;22:1364.e1-1364.e4. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 17] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 38. | Lui TH. Arthroscopic resection of the calcaneonavicular coalition or the “too long” anterior process of the calcaneus. Arthroscopy. 2006;22:903.e1-903.e4. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 39] [Article Influence: 2.1] [Reference Citation Analysis (0)] |