Published online Jul 18, 2014. doi: 10.5312/wjo.v5.i3.368
Revised: April 7, 2014
Accepted: April 16, 2014
Published online: July 18, 2014
Processing time: 215 Days and 20.3 Hours
AIM: To evaluate short- to medium term outcome of total elbow arthroplasty (TEA) in complex fractures of the distal humerus.
METHODS: A consecutive series of 24 complex distal humerus fractures operated with TEA in the period 2006-2012 was evaluated with the Mayo Elbow Performance score (MEPS), plain radiographs, complications and overall satisfaction. The indications for surgery were 1: AO type B3 or C3 or Sheffield type 3 fracture and age above 65 or 2: fracture and severe rheumatoid arthritis. Mean follow-up time was 21 mo.
RESULTS: Twenty patients were followed up. Four patients, of which 3 had died, were lost to follow up. According to the AO classification there were 17 C3, 1 B2 and 2 A2 fractures. Mean follow-up was 21 months (range 4-54). Mean MEPS was 94 (range 65-100). Mean flexion was 114 degrees (range 80-140). According to MEPS there were 15 excellent, 4 good and 1 fair result. Patient satisfaction: 8 excellent, 10 good, 2 fair and 1 poor. There were two revisions due to infection treated successfully with revision and three months of antibiotics. In two patients the locking split had loosened. One was referred to re-insertion and one chose yearly controls. Two patients had persistent dysaesthesia of their 5th finger, but were able to discriminate between sharp and blunt.
CONCLUSION: Our study suggests that TEA in complex fractures of the distal humerus in elderly patients can result in acceptable short- to medium term outcome.
Core tip: The number of distal humerus fractures in the elderly has increased in the last decades. The results after open reduction internal fixation in elderly with complex fractures of the distal humerus are highly variable with many failures and often poor outcome. We retrospectively reviewed a consecutive series of patients treated with total elbow arthroplasty (TEA) for complex fractures of the distal humerus. Our aim was to report short- to medium-term outcome. According to the Mayo Elbow Performance Score there were 15 patients with excellent results, 4 good, 1 fair and none poor. Our study suggests that TEA on fractures of the distal humerus in elderly patients can result in acceptable short- to medium-term outcome.
- Citation: Sørensen BW, Brorson S, Olsen BS. Primary total elbow arthroplasty in complex fractures of the distal humerus. World J Orthop 2014; 5(3): 368-372
- URL: https://www.wjgnet.com/2218-5836/full/v5/i3/368.htm
- DOI: https://dx.doi.org/10.5312/wjo.v5.i3.368
The number of distal humerus fractures in the elderly has increased in the last decades. Palvanen et al[1] reported that in Finnish women the annual rate of osteoporotic fractures of the distal humerus increased from 11 per 100000 in 1970 to 30 per 100000 in 1995 with a 9-fold increase in women aged > 80 years. In elderly patients with poor bone quality the fractures are often complicated by multiple fragments and articular involvement which can lead to pain, joint stiffness and impaired elbow function. The results after open reduction internal fixation (ORIF) in elderly with complex fractures of the distal humerus are highly variable with many failures and often poor outcome[2-9].
Studies have reported good results of primary total elbow arthroplasty (TEA) in the treatment of complex distal humerus fractures in the elderly[10-20]. Data from these studies shows that out of 194 operated elbows 10 (5.2%) received component revision. Ten (5.2%) were treated for varying degrees of infection. Sixteen (8.2%) had varying degree of ulnar nerve symptoms. The mean Mayo Elbow Performance Score (MEPS) was 91.
To our knowledge only 2 studies compare ORIF with TEA in treatment of distal humerus fractures. Frankle et al´s[16] retrospective review compares 12 ORIF´s with 12 TEA´s in patients older than 65. They found that 25% of the ORIF group was converted to TEA due to fixation failure. According to the MEPS 67% scored excellent or good in the ORIF group whereas 100% in the TEA Group scored excellent or good[16]. McKee et al´s[20] prospective, randomized trial compares 20 patients in each group ORIF/TEA with a mean age of 78. They found that 25% of the ORIF was intra-operatively converted to TEA. According to MEPS 53% of the ORIF group scored excellent or good whereas 100% in the TEA group scored excellent or good[20].
We retrospectively reviewed a consecutive series of patients treated with TEA for complex fractures of the distal humerus. Our aim was to report short- to medium-term outcome after total elbow arthroplasty on complex fractures of the distal humerus.
Between January 2006 and October 2012, we treated 24 patients with primary total elbow arthroplasty for complex fracture of the distal humerus using the Coonrad-Morrey semi-constrained prosthesis. Twenty out of 24 patients were retrospectively reviewed. Three patients had died and one we were not able to reach: The indications for surgery were 1: AO type B3 or C3 or Sheffield type 3 fracture and age above 65 or 2: fracture and severe rheumatoid arthritis. Two patients were younger than 65. They were both planned to have ORIF but were intraoperatively converted to arthroplasty because of inability to reach an acceptable reduction and fixation of the multiple fragments of the fracture. 17 patients had a type C3 fracture according to AO classification[21], 2 had type A2 fracture and 1 had a B3 fracture. According to the Sheffield classification[22] 18 had a type 3 fracture, 2 had a type 1 fracture. Two patients also suffered an ipsilateral olecranon fracture. Mean age was 77 (range, 55-95). Fifteen fractures involved the dominant extremity and five the non-dominant extremity. The mean interval between injury and operation was 9.1 d (range 1-22) and the mean postoperative stay was 1.8 d (range 1-4). Mean follow-up time was 21 months (range 4-52).
Nineteen patients were clinically examined and interviewed by the first author. 1 patient was interviewed by phone and did not have clinical function measured or radiographs taken. Clinical function was reviewed using the Mayo Elbow Performance Score[23]. Furthermore patients were asked to rate their overall satisfaction on a four-part ranking scale: “poor”, “fair”, “good” or “excellent”. The range of motion was measured using a hand-held goniometer[24]. Stability of the joint was determined based on history and physical examination. Radiographs were taken within few days of the clinical examination. They were evaluated to determine radiolucent lines. Primary radiographs and in some cases CT-scans were reviewed to classify the fractures
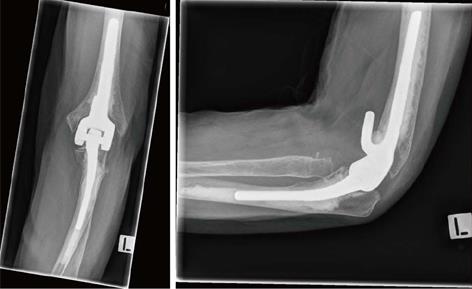
The Coonrad-Morrey semi-constrained total elbow prosthesis was used in all cases[25] (Figure 1). The patients were placed in a lateral supine position. A tourniquet was used. A midline skin incision was made and the ulnar nerve identified and protected throughout the procedure. The triceps was split by a reversed Y-shaped incision. The radial head was excised to the level of the annular ligament. The distal humerus was then resected and the humeral and ulnar medullary canals were reamed. Trial components were inserted and range of motion was checked. Then the canals were cemented and the prosthesis inserted and assembled. The triceps were sutured and the skin closed in layers. An extension splint was used for two weeks to allow wound healing. Physiotherapy was begun at day 14 d postoperative.
In one case the patient prior had an ipsilateral olecranon fracture, treated with two Kirschner wires and cerclage. The osteosynthesis material was left in situ during the implantation of the TEA. In another case the patient at the trauma sustained an ipsilateral olecranon fracture and intercondylar distal humerus fracture. In this case the TEA was implanted through the olecranon fracture with preservation of the triceps tendon, followed by osteosynthesis of the olecranon fracture, using two Kirschner wires and cerclage. The cerclage but not the Kirschner wires were later removed.
The average MEPS was 94 (range 65-100) (Table 1). According to the MEPS there were 15 patients with excellent results, 4 good and 1 fair. Fifteen patients had no pain, 4 had mild pain and only 1 had moderate pain. Mean arc of flexion was 114 (80-140) degrees. Mean forearm rotation was 165 (range 110-180) degrees. Two patients were revised because of deep infection. The infected patients were after the revision treated with oral antibiotics for respectively two and three months and were respectively one and two months hereafter found without clinical or biochemical signs of infection. In two cases the 2-piece locking pin had loosened. One patient was re-operated with insertion of a new locking pin, the other patient is followed at yearly controls. Two patients reported dysaesthesia of their 4th and 5th finger, but were both able to discriminate between sharp and blunt impact. In total 6 complications were observed (Table 2). The patients reported their results as: 8 excellent, 10 good, 2 fair and none poor.
| Points | No. of elbows | Mean score points | |
| Pain (maximum 45 points) | |||
| None | 45 | 15 | |
| Mild | 30 | 4 | |
| Moderate | 15 | 1 | |
| Severe | 0 | 41 | |
| Range of movement, degrees (maximum 20 points) | |||
| Arc > 100 | 20 | 17 | |
| Arc 50 to 100 | 15 | 3 | |
| Arc < 50 | 5 | 19 | |
| Stability (maximum 10 points) | |||
| Stable | 10 | 20 | |
| Moderate unstable | 5 | ||
| Grossly unstable | 0 | 10 | |
| Function (maximum 25 points) | |||
| Comb hair | 5 | 19 | |
| Feed oneself | 5 | 20 | |
| Personal hygiene | 5 | 19 | |
| Put on shirt | 5 | 20 | |
| Put on shoes | 5 | 20 | 25 |
| Mean total (maximum 100) | 94 |
| Age | Gender | Affected side (Dominant extr.) | Classification (AO) | Associated diagnosis | Days at hospital after surgery | Complications | Arc of flexion (sum - degrees) | Rotation(Degrees) | MEPS |
| 79 | F | R ( R ) | B3 | 1 | Ulnar palsy | 110 | 180 | 100 | |
| 66 | F | R ( R ) | C3 | 1 | Ulnar palsy | 135 | 180 | 100 | |
| 95 | F | L ( R ) | C3 | 1 | 105 | 180 | 100 | ||
| 63 | F | R ( R ) | C3 | 1 | 100 | 100 | 65 | ||
| 74 | F | R ( R ) | C3 | Olecranon fracture | 1 | 80 | 170 | 90 | |
| 83 | M | R ( R ) | C3 | 2 | 105 | 110 | 85 | ||
| 75 | F | R ( R ) | C3 | 3 | 110 | 180 | 85 | ||
| 74 | F | R ( R ) | C3 | 1 | Infection | 105 | 180 | 100 | |
| 89 | F | R ( R ) | C3 | 2 | 135 | 180 | 85 | ||
| 89 | F | R ( R ) | C3 | Olecranon fracture | 2 | 140 | 165 | 100 | |
| 81 | F | L ( R ) | C3 | 4 | 125 | 180 | 100 | ||
| 55 | M | R ( R ) | C3 | 4 | 120 | 170 | 100 | ||
| 81 | F | R ( R ) | C3 | 1 | Infection | 130 | 160 | 85 | |
| 67 | F | R ( R ) | A2 | Rheumatoid arthritis | 1 | 105 | 115 | 100 | |
| 73 | F | L ( R ) | C3 | 1 | Loose locking pin | 80 | 160 | 95 | |
| 89 | F | L ( R ) | C3 | 2 | 110 | 180 | 100 | ||
| 76 | F | R ( R ) | A2 | Rheumatoid arthritis | 1 | Ulnar palsy | 120 | 170 | 100 |
| 56 | F | R ( R ) | C3 | 2 | Loose locking pin | 90 | 180 | 95 | |
| 88 | F | R ( R ) | C3 | 1 | 130 | 180 | 100 | ||
| 88 | F | L ( R ) | C3 | 4 | 135 | 180 | 100 |
Comminuted distal humerus fractures in elderly are difficult to treat. The standard treatment for younger patients is ORIF. In the elderly, however, this treatment often results in less good results. John et al[4] had 20% fair and poor results in their series of 49 elderly patients with distal humerus fractures treated with ORIF. Kocher et al[6] had 25% fair and poor results in their retrospective review of 33 cases. Korner et al[7] had 42% fair and poor results in their retrospective review of 45 patients. An older review by Helfet et al[2] reported less good results in 25% in a compilation of 9 studies made from 1985 to 1990. Current studies on TEA in distal humerus fracture mainly consist of small case series[10-15,17-19], a retrospective case-control study[16], and a randomized trial[20] . Our study shows comparable results with 95% good or excellent results.
The Coonrad-Morrey semi-constrained elbow prosthesis has been reported to be an effective treatment for patients with rheumatoid arthritis (RA). Gill et al[26] found 86% good or excellent result with the Coonrad-Morrey prosthesis at 10-15 years follow-up on 41 RA patients. The rate of survival of the prosthesis was 92.4%. Park et al[27] had an 8 years survival rate of 100% in 35 RA patients. Plaschke et al[28] showed that TEA revision can give a good outcome. At 4.4 years follow up 20 patients scored mean 79 according to MEPS. The mean age of the TEA´s was 9.5 years before revision[28].
Wang et al[29] concludes in a Cochrane review from 2013 that the quality of the available evidence is limited and more studies are needed to determine the most appropriate surgical intervention for AO Type C distal humerus fractures in adults.
We acknowledge that this is a relatively short term retrospective study with no control group. Randomized studies are needed to assess the outcome after interventions for complex fractures of the distal humerus
In conclusion, our study suggests that TEA on fractures of the distal humerus in elderly patients can result in acceptable short- to medium-term outcome. However, the optimal treatment for complex fractures of the distal humerus has yet to be determined.
Osteoporotic fractures of the distal humerus have increased within the last 40 years. The results of osteosynthesis on distal humerus fractures in elderly are variable and studies show up to 42% less-then-good results according to Mayo Elbow Performance score. Total elbow arthroplasty (TEA) has gained popularity in the treatment of complicated distal humerus fractures in elderly.
TEA is a relatively new treatment option for distal humeral fractures. In this study the authors report acceptable short- to medium-term results.
Studies have reported good results of primary TEA in the treatment of complex distal humerus fractures in the elderly. Data from these studies shows that out of 194 operated elbows 10 (5.2%) received component revision. Ten (5.2%) were treated for varying degrees of infection. Sixteen (8.2%) had varying degree of ulnar nerve symptoms. This study shows comparable results in a Scandinavian context with average Mayo Elbow Performance Score of 94.
This study suggests that TEA on fractures of the distal humerus in elderly patients can result in acceptable short- to medium-term outcome. However, the optimal treatment for complex fractures of the distal humerus has yet to be determined.
The Mayo Elbow Performance Score is used in most studies where the results of operative intervention in distal humerus fracture are reported. The total score reflects pain, range of movement, stability and function.
This is a well written case series with appropriate documentation and referencing for the problem discussed. As noted, this is a complex problem with a relatively high rate of complications.
P- Reviewer: Bener A S- Editor: Song XX L- Editor: A E- Editor: Lu YJ
| 1. | Palvanen M, Niemi S, Parkkari J, Kannus P. Osteoporotic fractures of the distal humerus in elderly women. Ann Intern Med. 2003;139:W-W61. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 23] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 2. | Helfet DL, Schmeling GJ. Bicondylar intraarticular fractures of the distal humerus in adults. Clin Orthop Relat Res. 1993;26-36. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 140] [Cited by in RCA: 101] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 3. | Huang TL, Chiu FY, Chuang TY, Chen TH. The results of open reduction and internal fixation in elderly patients with severe fractures of the distal humerus: a critical analysis of the results. J Trauma. 2005;58:62-69. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 121] [Cited by in RCA: 102] [Article Influence: 5.1] [Reference Citation Analysis (0)] |
| 4. | John H, Rosso R, Neff U, Bodoky A, Regazzoni P, Harder F. [Distal humerus fractures in patients over 75 years of age. Long-term results of osteosynthesis]. Helv Chir Acta. 1993;60:219-224. [PubMed] |
| 5. | John H, Rosso R, Neff U, Bodoky A, Regazzoni P, Harder F. Operative treatment of distal humeral fractures in the elderly. J Bone Joint Surg Br. 1994;76:793-796. [PubMed] |
| 6. | Kocher M, Melcher GA, Leutenegger A, Rüedi T. [Elbow fractures in elderly patients]. Swiss Surg. 1997;3:167-171. [PubMed] |
| 7. | Korner J, Lill H, Müller LP, Hessmann M, Kopf K, Goldhahn J, Gonschorek O, Josten C, Rommens PM. Distal humerus fractures in elderly patients: results after open reduction and internal fixation. Osteoporos Int. 2005;16 Suppl 2:S73-S79. [PubMed] |
| 8. | O’Driscoll SW. Optimizing stability in distal humeral fracture fixation. J Shoulder Elbow Surg. 2005;14:186S-194S. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 182] [Cited by in RCA: 148] [Article Influence: 7.4] [Reference Citation Analysis (0)] |
| 9. | Srinivasan K, Agarwal M, Matthews SJ, Giannoudis PV. Fractures of the distal humerus in the elderly: is internal fixation the treatment of choice? Clin Orthop Relat Res. 2005;222-230. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 104] [Cited by in RCA: 69] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 10. | Chalidis B, Dimitriou C, Papadopoulos P, Petsatodis G, Giannoudis PV. Total elbow arthroplasty for the treatment of insufficient distal humeral fractures. A retrospective clinical study and review of the literature. Injury. 2009;40:582-590. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 88] [Cited by in RCA: 62] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 11. | Lee KT, Lai CH, Singh S. Results of total elbow arthroplasty in the treatment of distal humerus fractures in elderly Asian patients. J Trauma. 2006;61:889-892. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 35] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 12. | Ducrot G, Ehlinger M, Adam P, Di Marco A, Clavert P, Bonnomet F. Complex fractures of the distal humerus in the elderly: is primary total elbow arthroplasty a valid treatment alternative? A series of 20 cases. Orthop Traumatol Surg Res. 2013;99:10-20. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 38] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 13. | Cobb TK, Morrey BF. Total elbow arthroplasty as primary treatment for distal humeral fractures in elderly patients. J Bone Joint Surg Am. 1997;79:826-832. [PubMed] |
| 14. | Gambirasio R, Riand N, Stern R, Hoffmeyer P. Total elbow replacement for complex fractures of the distal humerus. An option for the elderly patient. J Bone Joint Surg Br. 2001;83:974-978. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 114] [Cited by in RCA: 83] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 15. | Garcia JA, Mykula R, Stanley D. Complex fractures of the distal humerus in the elderly. The role of total elbow replacement as primary treatment. J Bone Joint Surg Br. 2002;84:812-816. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 121] [Cited by in RCA: 82] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 16. | Frankle MA, Herscovici D, DiPasquale TG, Vasey MB, Sanders RW. A comparison of open reduction and internal fixation and primary total elbow arthroplasty in the treatment of intraarticular distal humerus fractures in women older than age 65. J Orthop Trauma. 2003;17:473-480. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 287] [Cited by in RCA: 211] [Article Influence: 9.6] [Reference Citation Analysis (0)] |
| 17. | Prasad N, Dent C. Outcome of total elbow replacement for distal humeral fractures in the elderly: a comparison of primary surgery and surgery after failed internal fixation or conservative treatment. J Bone Joint Surg Br. 2008;90:343-348. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 118] [Cited by in RCA: 87] [Article Influence: 5.1] [Reference Citation Analysis (0)] |
| 18. | Ray PS, Kakarlapudi K, Rajsekhar C, Bhamra MS. Total elbow arthroplasty as primary treatment for distal humeral fractures in elderly patients. Injury. 2000;31:687-692. [PubMed] |
| 19. | Kamineni S, Morrey BF. Distal humeral fractures treated with noncustom total elbow replacement. J Bone Joint Surg Am. 2004;86-A:940-947. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 19] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 20. | McKee MD, Veillette CJ, Hall JA, Schemitsch EH, Wild LM, McCormack R, Perey B, Goetz T, Zomar M, Moon K. A multicenter, prospective, randomized, controlled trial of open reduction--internal fixation versus total elbow arthroplasty for displaced intra-articular distal humeral fractures in elderly patients. J Shoulder Elbow Surg. 2009;18:3-12. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 340] [Cited by in RCA: 270] [Article Influence: 15.9] [Reference Citation Analysis (0)] |
| 21. | Muller ME, Nazarian S, Koch P, Shatzker J. The comprehensive classification of fractures of the long bones. Berlin: Springer 1990; . |
| 22. | Davies MB, Stanley D. A clinically applicable fracture classification for distal humeral fractures. J Shoulder Elbow Surg. 2006;15:602-608. [PubMed] |
| 23. | Morrey BF, An KN, Chao ETS. The elbow and its disorders. 2nd ed. Philadelphia: Saunders 1993; 86-89. |
| 24. | Chapleau J, Canet F, Petit Y, Laflamme GY, Rouleau DM. Validity of goniometric elbow measurements: comparative study with a radiographic method. Clin Orthop Relat Res. 2011;469:3134-3140. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 104] [Cited by in RCA: 113] [Article Influence: 8.1] [Reference Citation Analysis (0)] |
| 25. | Morrey BF, An KN, Chao ETS. The elbow and its disorders. 2nd ed. Philadelphia: Saunders 1993; 648-64. |
| 26. | Gill DR, Morrey BF. The Coonrad-Morrey total elbow arthroplasty in patients who have rheumatoid arthritis. A ten to fifteen-year follow-up study. J Bone Joint Surg Am. 1998;80:1327-1335. [PubMed] |
| 27. | Park SE, Kim JY, Cho SW, Rhee SK, Kwon SY. Complications and revision rate compared by type of total elbow arthroplasty. J Shoulder Elbow Surg. 2013;22:1121-1127. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 45] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 28. | Plaschke HC, Thillemann T, Belling-Sørensen AK, Olsen B. Revision total elbow arthroplasty with the linked Coonrad-Morrey total elbow arthroplasty: a retrospective study of twenty procedures. Int Orthop. 2013;37:853-858. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 16] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 29. | Wang Y, Zhuo Q, Tang P, Yang W. Surgical interventions for treating distal humeral fractures in adults. Cochrane Database Syst Rev. 2013;1:CD009890. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 13] [Article Influence: 1.1] [Reference Citation Analysis (0)] |