Published online Aug 15, 2015. doi: 10.4291/wjgp.v6.i3.62
Peer-review started: January 29, 2015
First decision: April 27, 2015
Revised: May 9, 2015
Accepted: June 15, 2015
Article in press: June 16, 2015
Published online: August 15, 2015
Processing time: 200 Days and 6.2 Hours
Anemia is a common extraintestinal manifestation of inflammatory bowel disease (IBD) and is frequently overlooked as a complication. Patients with IBD are commonly found to have iron deficiency anemia (IDA) secondary to chronic blood loss, and impaired iron absorption due to tissue inflammation. Patients with iron deficiency may not always manifest with signs and symptoms; so, hemoglobin levels in patients with IBD must be regularly monitored for earlier detection of anemia. IDA in IBD is associated with poor quality of life, necessitating prompt diagnosis and appropriate treatment. IDA is often associated with inflammation in patients with IBD. Thus, commonly used laboratory parameters are inadequate to diagnose IDA, and newer iron indices, such as reticulocyte hemoglobin content or percentage of hypochromic red cells or zinc protoporphyrin, are required to differentiate IDA from anemia of chronic disease. Oral iron preparations are available and are used in patients with mild disease activity. These preparations are inexpensive and convenient, but can produce gastrointestinal side effects, such as abdominal pain and diarrhea, that limit their use and patient compliance. These preparations are partly absorbed due to inflammation. Non-absorbed iron can be toxic and worsen IBD disease activity. Although cost-effective intravenous iron formulations are widely available and have improved safety profiles, physicians are reluctant to use them. We present a review of the pathophysiologic mechanisms of IDA in IBD, improved diagnostic and therapeutic strategies, efficacy, and safety of iron replacement in IBD.
Core tip: Iron deficiency anemia (IDA) is increasingly recognized as a common complication in patients with inflammatory bowel disease (IBD). IDA has a significant impact on quality of life and health care costs. This comprehensive review article discusses the latest advances in understanding the pathophysiologic mechanisms involved in development of IDA in patients with IBD, and reviews new diagnostic tests and therapeutic options with high safety indexes for the management of IDA. This article aims at increasing physician awareness and understanding of the complex mechanisms involved in IDA, and the current cutting-edge approach for the management of IDA in patients with IBD.
- Citation: Kaitha S, Bashir M, Ali T. Iron deficiency anemia in inflammatory bowel disease. World J Gastrointest Pathophysiol 2015; 6(3): 62-72
- URL: https://www.wjgnet.com/2150-5330/full/v6/i3/62.htm
- DOI: https://dx.doi.org/10.4291/wjgp.v6.i3.62
Inflammatory bowel disease (IBD) describes a set of chronic gastrointestinal illnesses, including Crohn’s disease (CD) and ulcerative colitis (UC), of multifactorial etiology, which proceed with periods of relapse and remission. Extraintestinal complications are common in IBD, and are reported in more than 25% of patients[1]. Anemia is one of the most common manifestations of IBD[2]. One-third of patients with IBD have hemoglobin levels below 12 g/dL[3]. The anemic state is strongly correlated with quality of life, and is an important problem in the therapeutic management of patients with chronic disease[4].
Most cases of anemia in patients with IBD result from functional or absolute iron deficiency. Functional iron deficiency is a state in which there is insufficient availability of iron for incorporation into erythroid precursors despite normal or increased body iron stores[5,6]. In patients with absolute iron deficiency, iron is stored in the bone marrow. Other parts of the monocyte-macrophage system in the liver and spleen become depleted, making iron unavailable for normal or increased rates of erythropoiesis. This may occur as the result of poor dietary intake of iron, reduced iron absorption, and/or increased blood loss.
Signs and symptoms of iron deficiency depend on the severity and chronicity of the anemia, in addition to the usual signs of anemia, including fatigue, pallor, and reduced exercise capacity. Cheilosis and koilonychia are signs of advanced tissue iron deficiency which are not frequently seen in the modern world, due to early diagnosis and timely correction.
Key symptoms of anemia, such as dyspnea and tachycardia, are caused by decreased blood oxygen levels and peripheral hypoxia. Compensatory blood shifting from the mesenteric arteries may worsen perfusion of the intestinal mucosa[7]. Motility disorder, nausea, anorexia, and even malabsorption have been attributed to anemia. Reduced metabolic and energy efficiency during physical activity also contribute to weight loss in anemia[8].
Central hypoxia may lead to symptoms such as headache, dizziness, vertigo, or tinnitus. Several studies have confirmed that treatment of anemia improves cognitive function[9]. Iron is a component of hemoglobin myoglobin, cytochromes, and many other enzymes. Thus, anemia negatively impacts almost every aspect of daily life in patients with IBD. Men with iron deficiency anemia (IDA) may suffer from impotence. Loss of libido contributes to impaired quality of life in both sexes[10]. In addition, latent iron deficiency may be responsible for “non-hematological” symptoms such as hair loss, paresthesias of the hands and feet, and reduced cognitive function, and may also be significantly associated with restless leg syndrome.
Anemia and iron deficiency have a dramatic impact on patients’ quality of life, yet anemia in patients with IBD is still underdiagnosed and undertreated. In the United States, annual emergency room visits for anemia average around 209000[11], drastically maximizing health care costs. In a patient population with the predisposition for anemia, like patients with IBD, early diagnosis and management of iron deficiency can promptly reduce hospital visits, improve quality of life, reduce loss of work, and, ultimately, lower health care costs.
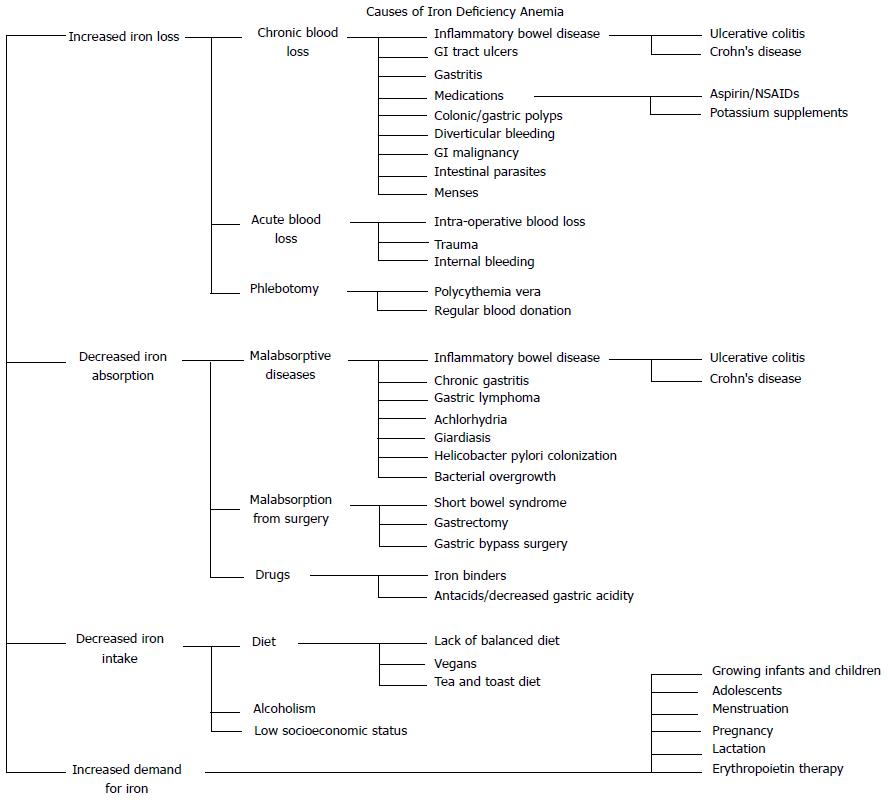
Anemia in IBD patients involves multiple pathogenic mechanisms resulting in low hemoglobin levels and compromised quality of life. Although ongoing blood loss from chronically inflamed intestinal mucosa and micronutrient deficiency (iron and B12) are the main mechanisms underlying the development of anemia in patients with IBD, chronic inflammation, hemolysis, and medication-induced myelosuppression may also play important roles in both the development of anemia and the management of this condition[12,13]. Anemia of chronic disease (ACD) and IDA are the two most common causes of anemia in patients with IBD[14,15]. Patients with IDA and concomitant ACD tend to have more severe anemia compared with patients with ACD alone[14]. Table 1 presents the causes of anemia in patients with IBD. Figure 1 outlines causes of IDA.
| Common causes | Less common causes | Rare causes |
| Iron deficiency anemia | B12 deficiency | Hemolysis |
| Anemia of chronic inflammation | Folic acid deficiency | Chronic renal insufficiency |
| Medications causing B12/Folate deficiency | Myelodysplastic syndrome | |
| Medication induced aplasia | ||
| Congenital hemoglobinopathies | ||
| Protein starvation | ||
| Anemia in liver disease |
Up to 3-4 g of iron is stored in the human body. Around 1-2 mg of iron is lost every day through desquamation of epithelial cells of the skin, gastrointestinal tract, bile ducts, and urinary tract, and through blood loss in menstruating women[16].
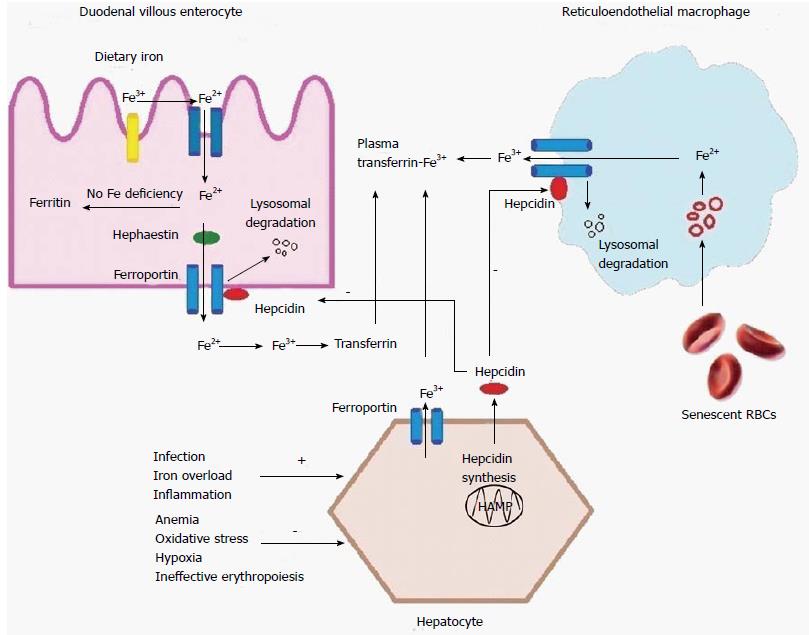
Iron homeostasis is strictly maintained by iron absorption from the duodenal enterocytes, and is tightly regulated by hepcidin (Figure 2). Hepcidin is a 25-amino-acid peptide hormone, has intrinsic antimicrobial activity, and is an acute-phase protein that is primarily synthesized by hepatocytes[17]. Cellular targets for hepcidin and iron-exporting cells are villous enterocytes, reticuloendothelial macrophages, and hepatocytes. Hepcidin binds to the basolateral transporter and iron exporter ferroportin 1, leading to its phosphorylation, internalization by binding to JAK 2, and lysosomal degradation, thus preventing iron release into the plasma[16]. Increased hepcidin levels downregulate ferroportin, thereby reducing iron efflux from the enterocytes and macrophages, causing hypoferremia. The increase in enterocyte iron content reduces the expression of enterocyte brush border reductase (Dcytb) and divalent metal transporter 1 (DMT1) on villous enterocytes, inhibiting dietary iron absorption causing iron deficiency anemia[18]. Therefore, by regulating the expression of DMT1 and ferroportin, hepcidin acts as a negative regulator of iron absorption in the duodenum and of iron release from the enterocytes and macrophages.
Hepcidin expression is upregulated by iron overload, infection, and inflammation, through proinflammatory cytokines such as interleukin (IL)-6 via the JAK 2 mediated STAT 3 signaling, thus limiting iron absorption[16,19]. Hepcidin expression is downregulated by hypoxia, oxidative stress, iron deficiency anemia, and ineffective erythropoiesis, thus increasing iron availability (Figure 2)[20].
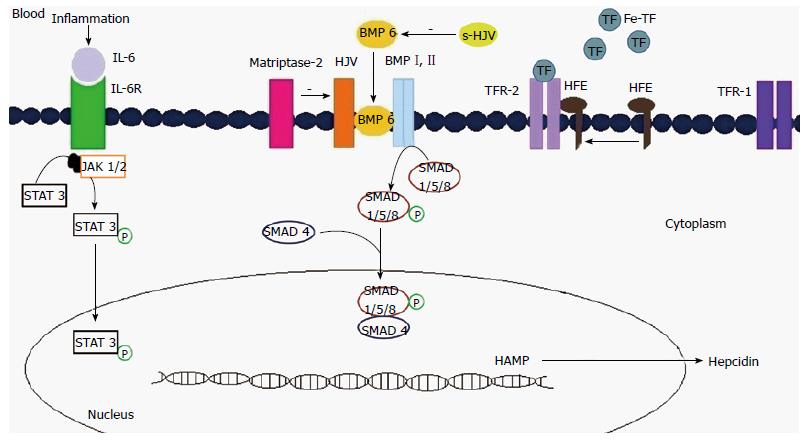
Hepcidin expression is mediated by two signaling pathways that involve bone morphogenetic protein (BMP) and transferrin receptor 2 (TfR2; Figure 3). The BMP signaling pathway includes BMP 6, hemojuvelin (HJV), and SMAD4, which constitute the major signaling pathway for hepcidin expression; TfR2 and the hereditary hemochromatosis protein (HFE)-dependent signaling pathway modulate this response[21,22]. In high iron conditions, transferrin-iron in the plasma forms a complex with HFE and TfR2 to promote hepcidin expression[21]. In iron-deficient conditions, there is downregulation of TfR2 and upregulation of TfR1. HFE is sequestered by TfR1, preventing its interaction with TfR2, thereby downregulating hepcidin expression (Figure 3)[21,23].
Healthcare providers screen for IDA by measuring hemoglobin, serum ferritin, and C-reactive protein (CRP). Based on expert opinion and common clinical practice, screening is recommended at least every 3 mo for outpatients with active disease, and once every 6 to 12 mo for patients in remission or with mild disease; screening is not applicable to hospitalized patients[24].
The World Health Organization (WHO) definitions of anemia also apply to patients with IBD. WHO defines anemia as hemoglobin levels < 13 g/dL (hematocrit < 39%) in males, < 12 g/dL (hematocrit < 36%) in nonpregnant females, and < 11 g/dL (hematocrit < 33%) in pregnant females[25]. Severe IDA is defined as hemoglobin levels < 10 g/dL.
If a patient meets WHO criteria for anemia, a basic anemia workup should be initiated to determine the cause of anemia. The basic workup includes serum ferritin, transferrin, transferrin saturation, and CRP levels. If the cause of anemia is unclear despite the results of the above workup, more extensive testing is recommended. Further tests include vitamin B12, folic acid, haptoglobin, lactate dehydrogenase, creatinine, and reticulocyte counts[24].
Both IDA and ACD often coexist with IBD, and the treatment for each differs. There is no single laboratory parameter that differentiates one from the other. Consequently, supplementary laboratory tests are required to differentiate IDA from ACD. These tests include soluble transferrin receptor, soluble transferrin receptor-ferritin index, reticulocyte hemoglobin concentration, zinc protoporphyrin, the percentage of hypochromic red cells, and hepcidin levels[16]. IDA in IBD is diagnosed based on a combination of factors, taking inflammation into account. The laboratory findings in IDA, ACD, mixed IDA, and ACD are shown in Table 2[16,22].
| Laboratory measures | IDA | ACD | IDA and ACD |
| Serum iron | ↓ | ↓ | ↓ |
| Hemoglobin | ↓ | ↓ | ↓ |
| MCV | ↓ | ↓ or normal | ↓ or normal |
| CRP | Normal | ↑↑ | ↑ |
| Serum ferritin | ↓ | ↑ | ↑ or normal |
| Transferrin | ↑ | ↓ or normal | ↓ |
| Transferrin saturation | ↓ | ↓ | ↓ |
| sTfR | ↑ | ↓ | ↑ or normal |
| sTfR- Ferritin index | High (> 2) | Low (< 1) | High (> 2) |
| Reticulocyte Hb content (CHr, pg) | < 28 | ≥ 28 | < 28 |
| Zinc protoporphyrin (μmol/mol heme) | > 40 | < 40 | > 40 |
| Percentage of hypochromic RBC | > 5 | < 5 | > 5 |
| Hepcidin | ↓ | ↑ | ↑ |
Serum ferritin is a measure of stored iron content in the reticuloendothelial system; in absolute iron deficiency, the serum ferritin concentration is < 15 μg/L[16]. Serum ferritin is an acute-phase reactant; normal or high levels may be found in inflammatory conditions despite iron deficiency[26]. Therefore, the guidelines recommend that in patients with quiescent IBD without biochemical or clinical evidence of inflammation, iron deficiency is defined as serum ferritin < 30 g/L or transferrin saturation (TSAT) < 16%[24]. In the presence of active IBD with inflammation, as evidenced by elevated CRP, the guidelines give a cut-off level of serum ferritin < 100 g/L to increase sensitivity and specificity[24,27].
Microcytosis (low mean corpuscular volume, MCV) and hypochromia (low mean corpuscular hemoglobin, MCH), available from the complete blood count, are indicators of absolute iron deficiency. High MCV is found secondary to vitamin B12 and folate deficiency, the use of certain medications (thiopurines; azathioprine or 6-mercaptopurine), alcoholism, and hypothyroidism[24]. Therefore, normal or high MCV does not exclude IDA as a possibility. In patients with ACD, MCV may be low or normal.
Serum transferrin carries Fe3+ in plasma and delivers iron from the sites of iron absorption (duodenal enterocytes and macrophages) to all tissues. Therefore, its level is higher in IDA. However, as it is an acute-phase protein, its level can be decreased during inflammation, despite normal or low iron stores.
Transferrin saturation (TSAT), an indicator of the iron load of circulating transferrin, gives an indirect measure of extent of iron utilization[16]. TSAT is the ratio of serum iron and total iron-binding capacity, multiplied by 100. It is decreased in both IDA and ACD. Pregnancy and oral contraceptives increase plasma transferrin levels; therefore, TSAT may be low in such patients, despite normal iron stores[16]. Hepcidin is increased during inflammation and decreased in IDA. It prevents iron absorption, causes retention of iron in the macrophages, and inhibits erythropoiesis.
Soluble transferrin receptor (sTfR) is a measure of erythropoietic activity. It is directly proportional to erythropoietic activity and inversely proportional to tissue iron availability[28]. sTfR is used to differentiate iron deficiency (increased sTfR and low serum ferritin) from inflammation (normal sTfR and serum ferritin) and to diagnose a combination of iron deficiency and inflammation (increased sTfR and normal serum ferritin)[24,27]. However, its use is limited due to its cost and unavailability in many laboratories.
The sTfR/log ferritin ratio (sTfR-ferritin index) may be an early indicator of depletion of iron stores[29]. A ratio < 1 suggests ACD and excludes iron deficiency, while a ratio > 2 suggests either IDA or mixed IDA and ACD[27].
Functional iron deficiency is the imbalance between the iron requirements of the erythroid marrow and the iron supply, when the body cannot supply iron rapidly enough to maintain an increased erythropoietic rate. This leads to reduced reticulocyte and erythrocyte cellular hemoglobin (Hb) content[30]. Reticulocyte hemoglobin content (CHr) and the percentage of hypochromic RBC are indicators of red cell hemoglobinization and, thus, functional iron deficiency, regardless of inflammatory states[30]. In IDA, CHr > 40 and hypochromic RBCs > 5%[31].
Iron binds to protoporphyrin IX to form heme. In the absence of iron, zinc binds to protoporphyrin to form zinc protoporphyrin (ZPP). ZPP indicates iron levels in the bone marrow during erythropoiesis and is unaffected by ACD or inflammation[16].
It is important to realize that IDA commonly accompanies IBD. The treatment of IDA should not be overlooked. Iron supplementation should be started as soon as a patient is found to have iron deficiency anemia. If a patient has iron deficiency without anemia, the decision to initiate iron therapy depends on the clinical scenario and the patient’s preference[24]. The treatment options vs frequent laboratory monitoring should be discussed with the patient. The decision to initiate therapy and the type of therapy is determined by symptoms, severity of anemia, IBD disease activity, comorbidities, and risks associated with therapy[24]. Anemia impairs quality of life, even in the absence of specific symptoms, in patients with IBD. Iron therapy leads to significant improvement in the quality of life (QOL)[32]. Therefore, the therapeutic goals of IDA are to normalize hemoglobin, serum ferritin, and TSAT levels, replenish iron stores (serum ferritin > 100 g/L), avoid the need for blood transfusions, and improve the QOL. Three treatment options are available for iron deficiency anemia in IBD: oral iron, parenteral iron, and erythropoietin[33].
After starting iron therapy, an increase in reticulocyte count occurs within 2 wk, hemoglobin rises by 2 g/dL within 4 wk, and hemoglobin level returns to normal within 8 wk. Oral iron therapy should be continued for at least 6 mo after the hemoglobin has normalized, in order to replenish iron stores[34].
To assess the response to therapy, hemoglobin should be measured within 4 wk of the initiation of iron therapy. After 4 wk of iron therapy, response to treatment is considered appropriate or optimal, if hemoglobin rises by at least 2 g/dL; partial, if hemoglobin rises by 1-1.9 g/dL; absent, if hemoglobin rises less than 1 g/dL[24,35].
If the response to iron therapy is suboptimal, oral iron administration should be changed to intravenous iron therapy, erythropoietic agents should be added to intravenous iron therapy, or causes of anemia should be reassessed. A serum ferritin > 100 g/L indicates appropriate iron stores in a patient taking oral iron[24]. Serum ferritin is falsely high and is not useful for monitoring intravenous iron supplementation, in such cases a TfS > 50% indicates iron overload[36].
Indications[16]: Anemia with hemoglobin > 10 g/dL, Quiescent or mildly active disease, in which oral iron absorption is not affected[37] in the absence of absolute indications for intravenous therapy (as mentioned below).
Advantages: There are some advantages, e.g., convenience and inexpensive, in oral iron therapy.
Limitations[33]: (1) intolerance and non-compliance due to side effects: abdominal pain, nausea, bloating, diarrhea; (2) impaired absorption due to duodenal inflammation, intestinal resection, severe disease activity; (3) partial or incomplete absorption; (4) non-absorbed iron can be toxic and worsen disease activity in IBD as a result of oxidative stress, neutrophilic infiltration, increased cytokines, and activation of NF-kappa B[38]; (5) experimental studies in animal models showed increased colon carcinogenesis with oral iron supplementation by inducing local oxidative stress at sites of active inflammation[39,40]; (6) slow response to therapy, cannot compensate for ongoing excessive blood loss; and (7) effective for short periods.
Available oral iron formulations: (1) ferrous fumarate has 106 mg elemental iron/tablet; (2) ferrous sulfate has 65 mg elemental iron/tablet; (3) ferrous gluconate has 28-36 mg iron/tablet; and (4) ferrous sulfate Elixir: 44 mg/5 mL (used if intolerant to oral iron tablets).
A maximum of 10-20 mg of oral iron can be absorbed per day. The recommended maximum daily dose is up to 100 mg elemental iron per day, as higher doses do not increase its absorption and efficacy, and the side effects of oral iron are dose-related[24,26]. Oral iron should be started at a low dose after meals. If well tolerated, the dose can then be increased and should be taken on an empty stomach to increase absorption. Iron should be given two hours before, or four hours after, ingestion of antacids. Iron is best absorbed as the ferrous (Fe++) salt form in a mildly acidic medium, so a 250 mg ascorbic acid tablet or a half-glass of orange juice can be added at the time of iron administration to enhance the degree of iron absorption. Soy protein, dietary calcium, phytates (bran, oats, rye), cereals, tea, antacids such as H2 receptor blockers, and proton pump inhibitors prevent absorption of nonheme iron.
According to the international consensus statement, the preferred route of iron supplementation in IBD is intravenous[24].
Indications[24,41]: (1) severe anemia, hemoglobin < 10 g/dL; (2) intolerance to oral iron therapy; (3) failure of oral iron therapy; (4) need for quicker and prolonged response; and (5) active disease (CRP > 5 mg/L).
Advantages[34]: (1) repletion of iron stores in unaffected by inflammation, intestinal resection; (2) rapid reversal of IDA; (3) relatively better tolerance and fewer side effects; (4) compliance can be monitored; (5) a single dose is sufficient for a few intravenous (IV) iron formulations (ferric carboxymaltose; low-molecular weight iron dextran); and (6) concurrent use of erythropoietin.
Limitations: (1) need for IV access and hospital staff for administration; (2) expensive; (3) inconvenience (travel, obtain IV access); and (4) iron dextran causes life-threatening anaphylactic reactions.
Available IV iron formulations: There are various IV iron preparations currently available for treatment of IDA. Their country-to-country availability, manufacturers, dosing, maximum and minimum infusion times, adverse reactions, costs, and FDA pregnancy category are provided in Table 3. The use of high molecular weight iron dextran is obsolete, due to the associated high risk of life-threatening anaphylactic reactions.
| Iron dextran (LMW) | Irongluconate | Ironsucrose | Ferriccarboxymaltose | Ferumoxytol | Ironisomaltoside | |
| Product/Europe Product/United States | CosmoFer® INFeD® | Ferrlecit® Ferrlecit® | Venofer® Venofer® | Ferinject® Injectafer® | Rienso® Feraheme® | Monofer® Not available in United States |
| Manufacturer | Pharmacosmos | Sanofi-Aventis | Vifor | Vifor | AMAG | Pharmacosmos |
| Test dose required | Yes | No | Yes (in Europe)/No | No | No | No |
| Maximum approved dose | 20 mg/kg | 125 mg | 200 mg (500 mg in few countries) 7 mg/kg | Ferinject- 1000 mg, or up to maximum of 20 mg/kg Injectafer-1500 mg if patient’s weight > 50 kg 15 mg/kg if < 50 kg | 1020 mg | 20 mg/kg |
| Iron dextran (LMW) | Iron gluconate | Iron sucrose | Ferric carboxymaltose | Ferumoxytol | Iron isomaltoside | |
| Maximum injectable single dose | 100 mg (2 mL) | 125 mg (10 mL) | 200 mg (10 mL) | Ferinject- 1000 mg or up to maximum of 20 mg/kg Injectafer- 750 mg (15 mL) | 510 mg (17 mL) | 200 mg (2 mL) |
| Maximum infusion time | 360 min (6 h) | 30-60 min | 210 min (3.5 h) | 15 min | 15 min | 15 min |
| Maximum injection time | 2 min | 10 min | 5-10 min | Bolus push over 7.5 min | 17 s (1 mL/s) | Bolus push |
| Dose-related reactions | Dextran induced IgE -mediated anaphylaxis, hypotension, edema | Hypotension, edema | Hypotension, edema | None reported | None reported | None reported |
| Relative risk of adverse side effects | Moderate | Low | Very low | None reported | Very low | None reported |
| Costs per 500 mg in €1 Costs per maximum single injectable dose in United States dollars | 84-86 € $37.70 | 52-56 € $76.32 | 105-100 € $120 | 170-175 € $993.75 | 82.12 $658.54 | 170-175 € Not available |
| FDA Pregnancy category | INFeD-category C Cosmofer - no data available | B | B | C | C | Can be used in 2nd and 3rd trimester |
| Additional comments | FDA approved for IDA in CKD receiving hemodialysis and supplemental epoetin therapy | FDA approved for IDA in CKD patients | Has been studied in patients with IDA associated with CKD either dialysis and nondialysis dependant, IBD, CHF, post-partum and pregnancy patients. Transient hypophosphatemia has been reported | FDA approved for IDA in CKD patients May transiently interfere with “tissue” diagnostic ability of MRI for up to 3 mo and “vascular” MRI for up to 2 d | Very low immunogenic potential |
Low molecular weight (LMW)-iron dextran (Cosmofer, INFeD) is more efficacious than oral iron in significantly raising hemoglobin levels within 8 wk[42]. LMW-iron dextran was associated with IgE-mediated anaphylactic reactions in up to 5.7% of patients during test dose infusion in a case-matched study[42,43]. Therefore, a black box warning that a test dose is required prior to its infusion is now included in the package insert. Its administration is time-consuming and infusions can take up to 4-6 h.
Iron gluconate (Ferrlecit) is indicated for patients with chronic kidney disease (CKD) receiving hemodialysis and supplemental epoetin therapy. A test dose is not required prior to its use. It has benzyl alcohol as a preservative.
Iron sucrose (Venofer) is indicated for IDA in CKD patients and requires a test dose only in Europe. It has been widely used for IDA due to its efficacy, safety, and better tolerability[44]. But, its use has been limited, due to an increased number of applications, and its infusion can take up to 3.5 h.
Ferric carboxymaltose (Ferinject, Injectafer) has been studied in patients with iron deficiency of different etiologies, such as non-dialysis and dialysis-dependent chronic kidney disease (CKD), IBD, heavy menstrual bleeding, post-partum IDA, or patients with chronic heart failure and IDA. It has been shown to be efficacious and well-tolerated when compared with oral iron[45] and iron sucrose[46].
Ganzoni’s formula is useful to estimate individual iron requirements[47]: Iron deficit (mg) = body weight (kg) x [target Hb-actual Hb (g/dL) x 2.4] + stored iron (500 mg).
However, it is inconvenient, inconsistently applied in clinical practice, and underestimates iron requirements[45]. A simplified method was used by the authors to calculate the cumulative iron dose (Table 4) for the ferric carboxymaltose group, instead of the traditional Ganzoni’s formula used in the iron sucrose group[46]. Ferric carboxymaltose is administered in 1-2 infusions, with each infusion given one week apart. It can be infused in 15 min, thus increasing the compliance rate. The use of ferric carboxymaltose for IDA was shown to be more cost effective and convenient than iron sucrose[48]. Transient hypophosphatemia, without clinical symptoms, was observed in a clinical study[46].
| Hemoglobin (g/dL) | Body weight < 70 kg | Body weight > 70 kg |
| > 10 | 1000 mg | 1500 mg |
| 7-10 | 1500 mg | 2000 mg |
Ferumoxytol (Rienso, Feraheme) is indicated for IDA in patients with chronic kidney disease (CKD). It has a rapid administration time (minimum of 17 s for 510 mg dose), with a second dose given in 3-8 d. However, the safety and efficacy of infusion of 1020 mg of ferumoxytol over 15 min has been demonstrated in a single arm, open-label trial conducted at one center[49]. Ferumoxytol is composed of superparamagnetic iron oxide nanoparticles coated with a low molecular weight semisynthetic carbohydrate. This agent may transiently interfere with the tissue diagnostic ability of MRI for up to 3 mo, and with vascular MRI for up to 2 d, which is a limitation for patients with IBD who will need an MRI within 3 mo[50]. If MR imaging is required within 3 mo after ferumoxytol administration, T1- or proton density-weighted MR pulse sequences are used to minimize the effects of the agent, and the radiologist should also be notified.
Iron isomaltoside 1000 (Monofer) is the newest IV iron product, but it is not available in the United States. This agent has very low immunogenic potential and a very low content of labile and free iron, enabling healthcare workers to administer a rapid high-dose infusion in doses exceeding 1000 mg in a single infusion, without the need for a test dose[51].
There is a component of anemia that is secondary to chronic inflammation in patients with IBD. Erythropoiesis-stimulating agents (ESA) are expensive and have risks associated with their administration. Therefore, these agents are recommended for treatment of anemia associated with IBD in patients who do not respond to IV iron therapy, when immunosuppressive therapy has not suppressed inflammation, and for patients requiring blood transfusions[52].
When patients are treated with ESAs, functional iron deficiency develops. Functional iron deficiency refers to the failure of iron supply or transport and insufficient availability of iron for erythropoiesis, despite normal body iron stores. Therefore, ESAs are used in combination with IV iron therapy[52]. The increased hepcidin levels in ACD prevent oral absorption of iron. Therefore, IV iron supplementation should be given instead of oral iron.
The need for red blood cell transfusion depends on the rate of bleeding, hemodynamic stability, hemoglobin level, and comorbidities. It is not a substitute for treatment of IDA with oral or IV iron supplementation. Its use in chronic anemia should be avoided, due to potential side effects and cost[24].
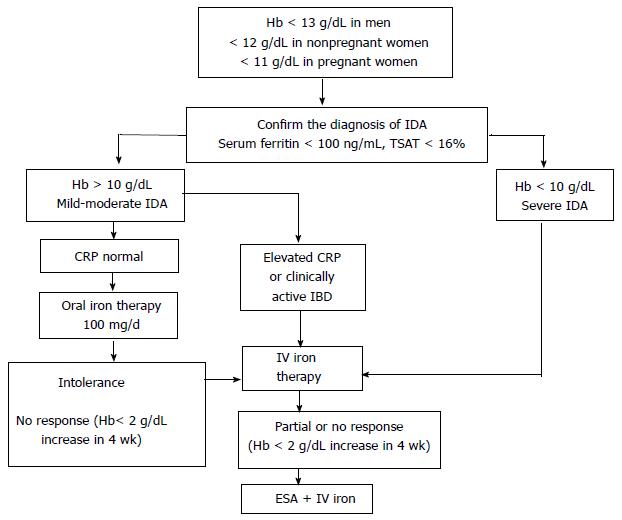
IDA is the most common anemia in IBD. Therefore, anemic patients with IBD should be evaluated for IDA. IDA mandates adequate and appropriate treatment, as it influences the patient’s quality of life and morbidity. It should be considered as an extraintestinal manifestation of IBD. The basic workup may be insufficient to diagnose IDA in the presence of inflammation. Table 2 summarizes the laboratory parameters necessary to differentiate IDA from ACD. Recent clinical trials support IV iron therapy as a preferable option, especially in clinically active IBD and moderate-severe IDA. IV iron therapy was shown to have better tolerability and efficacy, with fewer infusions, a better safety profile, and, accordingly, improved patient compliance. Figure 4 summarizes the management of IDA in IBD[16]. The ultimate goal is to normalize hemoglobin levels.
P- Reviewer: Capasso R, Chow WK S- Editor: Tian YL L- Editor: A E- Editor: Wu HL
| 1. | Calvo P, Pablo L. Managing IBD outside the gut: ocular manifestations. Dig Dis. 2013;31:229-232. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 21] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 2. | Hindryckx P, Amininejad L, Van De Vijver E, Bossuyt P. Belgian recommendations for the management of anemia in patients with inflammatory bowel disease. Acta Gastroenterol Belg. 2014;77:333-344. [PubMed] |
| 3. | Oldenburg B, Koningsberger JC, Van Berge Henegouwen GP, Van Asbeck BS, Marx JJ. Iron and inflammatory bowel disease. Aliment Pharmacol Ther. 2001;15:429-438. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 62] [Cited by in RCA: 63] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 4. | Crawford J. Anemia and lung cancer. Lung Cancer. 2002;38 Suppl 3:S75-S78. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 10] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 5. | Goodnough LT, Nemeth E, Ganz T. Detection, evaluation, and management of iron-restricted erythropoiesis. Blood. 2010;116:4754-4761. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 273] [Cited by in RCA: 288] [Article Influence: 19.2] [Reference Citation Analysis (0)] |
| 6. | Thomas DW, Hinchliffe RF, Briggs C, Macdougall IC, Littlewood T, Cavill I. Guideline for the laboratory diagnosis of functional iron deficiency. Br J Haematol. 2013;161:639-648. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 241] [Cited by in RCA: 256] [Article Influence: 21.3] [Reference Citation Analysis (0)] |
| 7. | Vatner SF. Effects of hemorrhage on regional blood flow distribution in dogs and primates. J Clin Invest. 1974;54:225-235. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 143] [Cited by in RCA: 138] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 8. | Daneryd P, Svanberg E, Körner U, Lindholm E, Sandström R, Brevinge H, Pettersson C, Bosaeus I, Lundholm K. Protection of metabolic and exercise capacity in unselected weight-losing cancer patients following treatment with recombinant erythropoietin: a randomized prospective study. Cancer Res. 1998;58:5374-5379. [PubMed] |
| 9. | Pickett JL, Theberge DC, Brown WS, Schweitzer SU, Nissenson AR. Normalizing hematocrit in dialysis patients improves brain function. Am J Kidney Dis. 1999;33:1122-1130. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 176] [Cited by in RCA: 168] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 10. | Ludwig H, Strasser K. Symptomatology of anemia. Semin Oncol. 2001;28:7-14. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 15] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 12. | Dallalio G, Law E, Means RT. Hepcidin inhibits in vitro erythroid colony formation at reduced erythropoietin concentrations. Blood. 2006;107:2702-2704. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 96] [Cited by in RCA: 106] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 13. | Dieleman LA, Heizer WD. Nutritional issues in inflammatory bowel disease. Gastroenterol Clin North Am. 1998;27:435-451. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 50] [Cited by in RCA: 45] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 14. | Gomollón F, Gisbert JP. Anemia and inflammatory bowel diseases. World J Gastroenterol. 2009;15:4659-4665. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 126] [Cited by in RCA: 131] [Article Influence: 8.2] [Reference Citation Analysis (0)] |
| 15. | Semrin G, Fishman DS, Bousvaros A, Zholudev A, Saunders AC, Correia CE, Nemeth E, Grand RJ, Weinstein DA. Impaired intestinal iron absorption in Crohn’s disease correlates with disease activity and markers of inflammation. Inflamm Bowel Dis. 2006;12:1101-1106. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 135] [Cited by in RCA: 137] [Article Influence: 7.2] [Reference Citation Analysis (0)] |
| 16. | Stein J, Dignass AU. Management of iron deficiency anemia in inflammatory bowel disease - a practical approach. Ann Gastroenterol. 2013;26:104-113. [PubMed] |
| 17. | Ganz T. Molecular control of iron transport. J Am Soc Nephrol. 2007;18:394-400. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 233] [Cited by in RCA: 220] [Article Influence: 12.2] [Reference Citation Analysis (0)] |
| 18. | De Domenico I, Lo E, Ward DM, Kaplan J. Hepcidin-induced internalization of ferroportin requires binding and cooperative interaction with Jak2. Proc Natl Acad Sci USA. 2009;106:3800-3805. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 96] [Cited by in RCA: 104] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 19. | Nemeth E, Rivera S, Gabayan V, Keller C, Taudorf S, Pedersen BK, Ganz T. IL-6 mediates hypoferremia of inflammation by inducing the synthesis of the iron regulatory hormone hepcidin. J Clin Invest. 2004;113:1271-1276. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 67] [Cited by in RCA: 847] [Article Influence: 40.3] [Reference Citation Analysis (0)] |
| 20. | Nicolas G, Chauvet C, Viatte L, Danan JL, Bigard X, Devaux I, Beaumont C, Kahn A, Vaulont S. The gene encoding the iron regulatory peptide hepcidin is regulated by anemia, hypoxia, and inflammation. J Clin Invest. 2002;110:1037-1044. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 479] [Article Influence: 20.8] [Reference Citation Analysis (0)] |
| 21. | Knutson MD. Iron-sensing proteins that regulate hepcidin and enteric iron absorption. Annu Rev Nutr. 2010;30:149-171. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 61] [Cited by in RCA: 64] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 22. | Stein J, Hartmann F, Dignass AU. Diagnosis and management of iron deficiency anemia in patients with IBD. Nat Rev Gastroenterol Hepatol. 2010;7:599-610. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 188] [Cited by in RCA: 184] [Article Influence: 12.3] [Reference Citation Analysis (0)] |
| 23. | Anderson GJ, Frazer DM, McLaren GD. Iron absorption and metabolism. Curr Opin Gastroenterol. 2009;25:129-135. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 129] [Cited by in RCA: 118] [Article Influence: 7.4] [Reference Citation Analysis (0)] |
| 24. | Gasche C, Berstad A, Befrits R, Beglinger C, Dignass A, Erichsen K, Gomollon F, Hjortswang H, Koutroubakis I, Kulnigg S. Guidelines on the diagnosis and management of iron deficiency and anemia in inflammatory bowel diseases. Inflamm Bowel Dis. 2007;13:1545-1553. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 322] [Cited by in RCA: 313] [Article Influence: 17.4] [Reference Citation Analysis (3)] |
| 25. | WHO/UNICEF/UNU. Iron Deficiency Anemia: Assessment, Prevention and Control (Accessed 1998). Available from: http://www.who.int/nutrition/publications/en/ida_assessment_prevention_control.pdf. |
| 26. | Gomollón F, Gisbert JP. Current management of iron deficiency anemia in inflammatory bowel diseases: a practical guide. Drugs. 2013;73:1761-1770. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 29] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 27. | Weiss G, Goodnough LT. Anemia of chronic disease. N Engl J Med. 2005;352:1011-1023. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2133] [Cited by in RCA: 2165] [Article Influence: 108.3] [Reference Citation Analysis (0)] |
| 28. | Lok CN, Loh TT. Regulation of transferrin function and expression: review and update. Biol Signals Recept. 1998;7:157-178. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 50] [Cited by in RCA: 52] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 29. | Punnonen K, Irjala K, Rajamäki A. Serum transferrin receptor, ferritin and TfR-F index in identification of latent iron deficiency. Eur J Haematol. 1998;60:135-137. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 23] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 30. | Thomas C, Thomas L. Biochemical markers and hematologic indices in the diagnosis of functional iron deficiency. Clin Chem. 2002;48:1066-1076. [PubMed] |
| 31. | Reinisch W, Staun M, Bhandari S, Muñoz M. State of the iron: how to diagnose and efficiently treat iron deficiency anemia in inflammatory bowel disease. J Crohns Colitis. 2013;7:429-440. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 52] [Cited by in RCA: 56] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 32. | Wells CW, Lewis S, Barton JR, Corbett S. Effects of changes in hemoglobin level on quality of life and cognitive function in inflammatory bowel disease patients. Inflamm Bowel Dis. 2006;12:123-130. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 188] [Cited by in RCA: 213] [Article Influence: 11.2] [Reference Citation Analysis (0)] |
| 33. | de la Morena F, Gisbert JP. Anemia and inflammatory bowel disease. Rev Esp Enferm Dig. 2008;100:285-293. [PubMed] |
| 34. | Bayraktar UD, Bayraktar S. Treatment of iron deficiency anemia associated with gastrointestinal tract diseases. World J Gastroenterol. 2010;16:2720-2725. [PubMed] |
| 35. | Gasche C. Anemia in IBD: the overlooked villain. Inflamm Bowel Dis. 2000;6:142-150; discussion 151. [PubMed] |
| 36. | Ali M, Rigolosi R, Fayemi AO, Braun EV, Frascino J, Singer R. Failure of serum ferritin levels to predict bone-marrow iron content after intravenous iron-dextran therapy. Lancet. 1982;1:652-655. [PubMed] |
| 37. | Lomer MC, Cook WB, Jan-Mohamed HJ, Hutchinson C, Liu DY, Hider RC, Powell JJ. Iron requirements based upon iron absorption tests are poorly predicted by haematological indices in patients with inactive inflammatory bowel disease. Br J Nutr. 2012;107:1806-1811. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 26] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 38. | Carrier JC, Aghdassi E, Jeejeebhoy K, Allard JP. Exacerbation of dextran sulfate sodium-induced colitis by dietary iron supplementation: role of NF-kappaB. Int J Colorectal Dis. 2006;21:381-387. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 45] [Cited by in RCA: 53] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 39. | Kulnigg S, Gasche C. Systematic review: managing anaemia in Crohn’s disease. Aliment Pharmacol Ther. 2006;24:1507-1523. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 209] [Cited by in RCA: 220] [Article Influence: 11.6] [Reference Citation Analysis (0)] |
| 40. | Liao J, Seril DN, Lu GG, Zhang M, Toyokuni S, Yang AL, Yang GY. Increased susceptibility of chronic ulcerative colitis-induced carcinoma development in DNA repair enzyme Ogg1 deficient mice. Mol Carcinog. 2008;47:638-646. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 45] [Cited by in RCA: 47] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 41. | Gisbert JP, Gomollón F. Common misconceptions in the diagnosis and management of anemia in inflammatory bowel disease. Am J Gastroenterol. 2008;103:1299-1307. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 144] [Cited by in RCA: 154] [Article Influence: 9.1] [Reference Citation Analysis (0)] |
| 42. | Khalil A, Goodhand JR, Wahed M, Yeung J, Ali FR, Rampton DS. Efficacy and tolerability of intravenous iron dextran and oral iron in inflammatory bowel disease: a case-matched study in clinical practice. Eur J Gastroenterol Hepatol. 2011;23:1029-1035. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 25] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 43. | Koutroubakis IE, Oustamanolakis P, Karakoidas C, Mantzaris GJ, Kouroumalis EA. Safety and efficacy of total-dose infusion of low molecular weight iron dextran for iron deficiency anemia in patients with inflammatory bowel disease. Dig Dis Sci. 2010;55:2327-2331. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 30] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 44. | Schröder O, Mickisch O, Seidler U, de Weerth A, Dignass AU, Herfarth H, Reinshagen M, Schreiber S, Junge U, Schrott M. Intravenous iron sucrose versus oral iron supplementation for the treatment of iron deficiency anemia in patients with inflammatory bowel disease--a randomized, controlled, open-label, multicenter study. Am J Gastroenterol. 2005;100:2503-2509. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 163] [Cited by in RCA: 162] [Article Influence: 8.1] [Reference Citation Analysis (0)] |
| 45. | Kulnigg S, Stoinov S, Simanenkov V, Dudar LV, Karnafel W, Garcia LC, Sambuelli AM, D’Haens G, Gasche C. A novel intravenous iron formulation for treatment of anemia in inflammatory bowel disease: the ferric carboxymaltose (FERINJECT) randomized controlled trial. Am J Gastroenterol. 2008;103:1182-1192. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 219] [Cited by in RCA: 252] [Article Influence: 14.8] [Reference Citation Analysis (0)] |
| 46. | Evstatiev R, Marteau P, Iqbal T, Khalif IL, Stein J, Bokemeyer B, Chopey IV, Gutzwiller FS, Riopel L, Gasche C. FERGIcor, a randomized controlled trial on ferric carboxymaltose for iron deficiency anemia in inflammatory bowel disease. Gastroenterology. 2011;141:846-853.e1-2. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 263] [Cited by in RCA: 244] [Article Influence: 17.4] [Reference Citation Analysis (0)] |
| 47. | Ganzoni AM. Intravenous iron-dextran: therapeutic and experimental possibilities. Schweiz Med Wochenschr. 1970;100:301-303. [PubMed] |
| 48. | Bager P, Dahlerup JF. The health care cost of intravenous iron treatment in IBD patients depends on the economic evaluation perspective. J Crohns Colitis. 2010;4:427-430. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 29] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 49. | Auerbach M, Strauss W, Auerbach S, Rineer S, Bahrain H. Safety and efficacy of total dose infusion of 1,020 mg of ferumoxytol administered over 15 min. Am J Hematol. 2013;88:944-947. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 56] [Cited by in RCA: 62] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 50. | Bruining DH, Loftus EV. Technology Insight: new techniques for imaging the gut in patients with IBD. Nat Clin Pract Gastroenterol Hepatol. 2008;5:154-161. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 18] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 51. | Jahn MR, Andreasen HB, Fütterer S, Nawroth T, Schünemann V, Kolb U, Hofmeister W, Muñoz M, Bock K, Meldal M. A comparative study of the physicochemical properties of iron isomaltoside 1000 (Monofer), a new intravenous iron preparation and its clinical implications. Eur J Pharm Biopharm. 2011;78:480-491. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 148] [Cited by in RCA: 191] [Article Influence: 13.6] [Reference Citation Analysis (0)] |
| 52. | Moreno López R, Sicilia Aladrén B, Gomollón García F. Use of agents stimulating erythropoiesis in digestive diseases. World J Gastroenterol. 2009;15:4675-4685. [PubMed] |