Revised: December 31, 2013
Accepted: February 16, 2014
Published online: March 28, 2014
Processing time: 166 Days and 12.5 Hours
AIM: To systematically review published data on the cost-effectiveness of Fluorine-18-Fluorodeoxyglucose positron emission tomography (FDG-PET) or PET/computed tomography (PET/CT) in tumours other than lung cancer.
METHODS: A comprehensive literature search of studies published in PubMed/MEDLINE, Scopus and Embase databases through the 10th of October in 2013 was carried out. A search algorithm based on a combination of the terms: (1) “PET” or “ PET/computed tomography (PET/CT)” or “positron emission tomography”; and (2) “cost-effectiveness” or “cost-utility” or “cost-efficacy” or “technology assessment” or “health technology assessment” was used. Only cost-effectiveness or cost-utility analyses in English language were included. Exclusion criteria were: (1) articles not within the field of interest of this review; (2) review articles, editorials or letters, conference proceedings; and (3) outcome evaluation studies, cost studies or health technology assessment reports. For each included study, information was collected concerning basic study, type of tumours evaluated, perspective/type of study, results, unit and comparison alternatives.
RESULTS: Sixteen studies were included. Head and neck tumours were evaluated in 4 articles, lymphoma in 4, colon-rectum tumours in 3 and breast tumours in 2. Only one article was retrieved for melanoma, oesophagus and ovary tumours. Cost-effectiveness results of FDG-PET or PET/CT ranged from dominated to dominant.
CONCLUSION: Literature evidence about the cost-effectiveness of FDG-PET or PET/CT in tumours other than lung cancer is still limited. Nevertheless, FDG-PET or PET/CT seems to be cost-effective in selective indications in oncology (staging and restaging of head and neck tumours, staging and treatment evaluation in lymphoma).
Core tip: Evidence based data about the cost-effectiveness of Fluorine-18-Fluorodeoxyglucose positron emission tomography (FDG-PET) or PET/computed tomography (PET/CT) in lung cancer already exist. The aim of our study is to systematically review published data on the cost-effectiveness of FDG-PET or PET/CT in tumours other than lung cancer.
- Citation: Annunziata S, Caldarella C, Treglia G. Cost-effectiveness of Fluorine-18-Fluorodeoxyglucose positron emission tomography in tumours other than lung cancer: A systematic review. World J Radiol 2014; 6(3): 48-55
- URL: https://www.wjgnet.com/1949-8470/full/v6/i3/48.htm
- DOI: https://dx.doi.org/10.4329/wjr.v6.i3.48
Fluorine-18-Fluorodeoxyglucose positron emission tomography (FDG-PET) or PET/computed tomography (PET/CT) is useful imaging techniques to study cellular metabolism. FDG is a glucose analogue which is trapped by cells via the glucose transporters; tumour cells usually show increased glucose metabolism and consequently an increased FDG uptake compared to normal cells. This characteristic allows the visualization of tumour cells by using PET imaging[1].
To date, oncology is the most important application of FDG-PET and PET/CT. The role of FDG-PET or PET/CT in oncology is to stage or restage tumours, to evaluate tumour response to treatment, to define patient prognosis, to guide surgery and radiotherapy[1].
FDG-PET and PET/CT have high costs; therefore it is mandatory to combine the effectiveness evaluation of these methods with economic assessment in different oncologic indications, in order to establish the correct usefulness of these methods in different clinical scenarios[2].
Cost-effectiveness analysis is a way to study both efficacy and cost of a medical procedure. These studies use parameters as “life years gained” (LYG) or disability days saved. In cost-utility analysis, measures change with patient preference and authors refer to “quality-adjusted life years” (QALYs). In cost-benefit analyses, monetary units represent the value of the procedure[3]. Incremental cost-effectiveness ratio (ICER) and incremental cost-utility ratio (ICUR) are ways to measure the cost of an increasing efficacy (or utility) of a medical procedure. Similarly, net monetary benefit (NMB) is used to correlate cost and efficacy, using an equation including the willingness to pay (WTP) value that represents the maximum cost that a patient would pay for a medical procedure.
Evidence based data about the cost-effectiveness of FDG-PET and PET/CT in lung cancer already exist. PET is cost-effective in staging of non-small cell lung carcinoma (NSCLC) and seems to be cost-effective for diagnosing solitary pulmonary nodules (SPN)[4]. Then, PET cost is appropriate in staging of lung cancer and diagnosis of indeterminate SPNs[5].
Cost-effectiveness studies have been published about the use of FDG-PET or PET/CT in tumours other than lung cancer. The aim of our study is to systematically review published data on the cost-effectiveness of FDG-PET and PET/CT in this setting.
A comprehensive computer literature search of the PubMed/MEDLINE, Scopus and Embase databases was carried out to find relevant peer reviewed articles on the cost-effectiveness of PET or PET/CT in patients with either histologically proven or suspected tumours other than lung cancer.
A search algorithm based on a combination of the terms: (1) “PET” or “PET/CT” or “positron emission tomography”; and (2) “cost-effectiveness” or “cost-utility” or “cost-efficacy” or “technology assessment” or “health technology assessment (HTA)” was used. No beginning date limit was used and the search was updated until October 10th, 2013. To expand our search, references of the retrieved articles were also screened for additional studies. Only English studies were included.
All studies or subsets in studies investigating the cost-effectiveness of FDG-PET or PET/CT in patients with suspected tumours other than lung cancer were eligible for inclusion.
The exclusion criteria were: (1) articles not within the field of interest of this review; (2) review articles, editorials or letters, comments, conference proceedings; and (3) outcome evaluation studies, cost studies or health technology assessment reports.
Three researchers (GT, SA and CC) independently reviewed the titles and the abstracts of the retrieved articles, applying the inclusion and exclusion criteria mentioned above. The same three researchers then independently reviewed the full-text version of the articles to confirm their eligibility for inclusion. Disagreements were resolved in a consensus meeting.
For each included study, information was collected concerning basic study (author names, journal, year of publication, country of origin), type of tumours evaluated, perspective/type of study, results, unit and comparison alternatives.
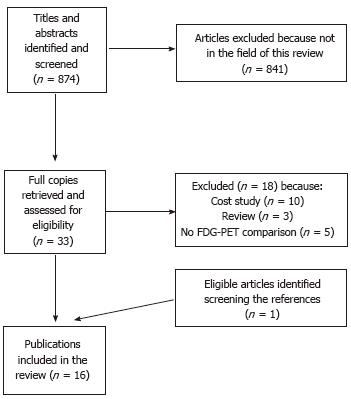
The comprehensive computer literature search revealed 874 articles. Reviewing titles and abstracts, 841 articles were excluded applying the criteria mentioned above. Thirty-three articles were selected and retrieved in full-text version (Figure 1). One study was found screening the references[6] and 18 articles were subsequently excluded[7-24]. Finally, 16 studies were included[6,25-39]. The characteristics of the included studies (Table 1) and a list of excluded studies on economic evaluation assessment, with reasons for exclusion (Table 2) are provided.
| Ref. | Year | Country | Tumour (histology) | Indication | Perspective,type of study | Results, unit and comparison alternatives |
| Hollenbeak et al[25] | 2001 | United States | Neck (various) | Staging | Hospital, decision tree | ICER (US$/LYG (US$/QALY)): 8718 (2505) (CT + PET vs CT) |
| Yen et al[26] | 2009 | Taiwan | Head/neck (nasopharyngeal carcinoma) | Restaging | Hospital, decision tree | ICUR (US$/QALY): 462 (PET + MRI vs MRI) |
| Sher et al[27] | 2010 | United States | Head/neck (squamous cell carcinoma) | Restaging | Public payer (medicare), markov model | ICER (US$/QALY): 1500 (PET-CT vs CT in RD after chemiotherapy) |
| Rabalais et al[28] | 2012 | United States | Head/Neck (various) | Restaging | Public payer (medicare), decision tree | ICER (US $): 3854397 (PET-CT vs neck dissection) |
| Sloka et al[29] | 2005 | Canada | Breast (various) | Staging | Hospital, meta-analysis, decision tree | PET + ALND dominating ALND [cost savings (US $): 695, increase in life expectancy: 7.4 d] |
| Meng et al[30] | 2011 | United Kingdom | Breast (various) | Staging | Health care system, decision tree | NMB (UK£ 30000 per QALY): 1085 (replace SLNB with PET) |
| Klose et al[31] | 2000 | Germany | Lymphoma (various) | Staging | Hospital, micro-costing approach | ICER (€): 3133 (FDG-PET vs CT) |
| Bradbury et al[6] | 2002 | United Kingdom | Lymphoma (HL) | Restaging | Health care system, decision tree and Markov model | WTP (£/LYG): 1000 (PET after positive CT vs CT + PET) |
| Cerci et al[32] | 2010 | Brazil | Lymphoma (HL) | Post-treat | Hospital, decision tree | ICER ($): 3268 (CT + PET + biopsy vs CT + biopsy) |
| Cerci et al[33] | 2011 | Brazil | Lymphoma (HL) | Staging | Hospital, micro-costing approach | ICER ($): 16215 (PET/CT vs CT and biopsy) |
| Park et al[34] | 2001 | United States | Colon-rectum (various) | Restaging | Public payer (medicare), decision tree | ICER (US$/LYG): 16437 (CT + PET vs PET) |
| Lejeune et al[35] | 2005 | France | Colon-rectum (metastases) | Staging | Health care system, decision tree | ICER: dominated (CT vs CT + PET) |
| Wiering et al[36] | 2010 | Netherlands | Colon-rectum (metastases) | Restaging | Health care system, randomized clinical trial | NMB (€): 11060 (CWU vs CWU + FDG-PET) |
| Krug et al[37] | 2010 | Belgium | Melanoma (metastases) | Restaging | Health care system, Markov model | ICER: dominated (PET-TC vs CT). NMB (€):1048, gain of 0.2 LMG |
| Wallace et al[38] | 2002 | United States | Esophagus (various) | Staging | Public payer (medicare), decision tree | Marginal ICER ($/QALY): 60544 (PET + EUS-FNA vs CT + EUS-FNA) |
| Mansueto et al[39] | 2009 | Italy | Ovary (various) | Restaging | Health care system, decision tree | ICER (€/SA): 226.77 (PET/CT for All) |
| Ref. | Year | Country | Tumors(histology) | Reason for exclusion |
| Bongers et al[7] | 2002 | Netherlands | Neck (laryngeal cancer) | Cost study |
| van Hooren et al[8] | 2009 | Netherlands | Neck (laryngeal carcinoma) | Cost study |
| Uly-de Groot et al[9] | 2010 | Netherlands | Head/neck (metastases) | Cost study |
| Kurien et al[10] | 2011 | United States | Head/neck (various) | Cost study |
| Schergerin et al[11] | 2009 | United States | Breast (various) | No PET comparison |
| Auguste et al[12] | 2011 | United Kingdom | Breast (various) | Review |
| Cooper et al[13] | 2011 | United Kingdom | Breast (various) | Review |
| Strobel et al[14] | 2007 | Switzerland | Lymphoma (various) | Cost study |
| Moulin-Romsee et al[15] | 2008 | Belgium | Lymphoma (NHL) | Cost study |
| Brush et al[16] | 2011 | United Kingdom | Colon-rectum (various) | Review |
| von Schulthess et al[17] | 1998 | Switzerland | Melanoma (various) | Cost study |
| Bastiaannet et al[18] | 2012 | Netherlands | Melanoma (various) | Cost study |
| Heinzel et al[19] | 2012 | Germany | Brain (glioma) | Aminoacid PET |
| Heinzel et al[20] | 2012 | Germany | Brain (glioma) | Aminoacid PET |
| Hetzel et al[21] | 2003 | Germany | Bone (metastases) | F18-Fluoride PET |
| Tateishi et al[22] | 2010 | Japan | Bone (metastases) | F18-Fluoride PET |
| Heinrich et al[23] | 2005 | Austria | Pancreas (various) | Cost study |
| Rondina et al[24] | 2012 | United States | Occult (various) | Cost study |
Head and neck tumours were evaluated in 4 articles, lymphoma in 4, colon-rectum tumours in 3 and breast tumours in 2. Only one article was retrieved for melanoma, oesophageal and ovary tumours.
Hollenbeak et al[25] compared PET with CT scan strategy in patients with N0 head and neck squamous cell carcinoma (HNSCC). A cost-effectiveness analysis was undertaken using a decision tree model approach and the perspective was that of the hospital. The ICER for the PET strategy was $8718 per year of life saved, or $2505 per QUALY. Authors also evaluated life expectancy and costs. The PET strategy resulted in a life expectancy of 10.1 years, marginally higher than the 9.9 years expected from the No PET strategy. The PET strategy also resulted in 9.8 QALYs versus 9.4 QALYs for the No PET strategy.
Yen et al[26] defined as the baseline case a 46-year-old male patient who was suspected of having recurrent nasopharyngeal carcinoma (NPC) during his post-treatment follow-up. The analysis for cost-utility is based on the decision-tree model for three different strategies: (1) magnetic resonance imaging (MRI)-only; (2) PET-only; and (3) MRI-PET (performing PET if MRI result is uncertain). The additional cost per additional QALYs for strategy 2 relative to strategy 1 was calculated to be United States $1389 (United States $750/0.54) and that for strategy 3 relative to strategy 1 is calculated to be United States $462 (United States $550/1.19). Strategy 3 dominates over strategy 2 because strategy 3 costs less and yields more QALYs than strategy 2.
Sher et al[27] analysed the cost-effectiveness of CT and PET/CT as predictors of the need for adjuvant neck dissection (AND) compared with ND for all patients with node-positive HNSCC. Authors designed a Markov model to simulate the clinical history of a 50-year-old man with node-positive stage IVA squamous cell carcinoma of the oropharynx. Three strategies were evaluated: carrying out NDs on all patients; NDs only for patients with residual disease (RD) on CT; NDs on patients with RD on PET/CT. With a few exceptions, the PET/CT strategy dominated the other two strategies (ICER of 1500 United States $/QALY for PET-CT versus CT in RD after chemiotherapy).
Rabalais et al[28] considered a patient with an oropharyngeal cancer with pre-treatment N2 disease having a complete response. Standardized costs were obtained using national databases. Four different strategies were analysed: PET/CT only; ND and physical examination (PE); ND + PE + CT; ND + PE + PET/CT. The ICER was of 3854397 United States $ for PET-CT versus neck dissection. The most cost-effective strategy was PET/CT scans on all patients following treatment, and proceed with neck dissections on those with positive scans.
Klose et al[31] measured the ICER of FDG-PET versus CT as diagnostic procedures in the primary staging of malignant lymphomas. ICER were €478 per correctly staged patient for CT versus “no diagnostics” and €3133 for FDG-PET versus CT. Direct costs of the diagnostic procedures were calculated based on the cost accounting system of the University Hospital in Ulm using a micro-costing approach.
Bradbury et al[6] studied patients who have a partial or complete response to induction therapy. They compared five strategies: all for surveillance; all for consolidation; CT only; PET after positive CT; CT + PET. Perspective was that of health care system. Strategies 4 and 5 were cost-effective, provided WTP exceeded £1000/LYG, and for almost all input values considered, provided WTP exceeded £5000/LYG.
In two studies, Cerci et al[32] calculated the cost-effectiveness of PET in hodgkin lymphoma (HL). In both studies, perspective was that of the hospital. In the first one[32], they assessed the cost effectiveness of FDG-PET in patients with HL with unconfirmed complete remission (CRu) or partial remission (PR) after first-line treatment. The ICER comparing the restaging strategy of CT, PET, and biopsy with the restaging strategy of only CT and biopsy (without PET) would be $3268 per true case detected.
In the second study[33], staging costs were studied in more strategies: conventional strategy (strategy I) including physical examination, laboratory tests, bone marrow biopsy (BMB), and CT scans (cervical, thoracic, abdominal, and pelvic); strategy II (with CT + PET) including physical examination, laboratory tests, bilateral BMB, CT scans, and PET scans; strategy III (with PET/CT) including physical examination, laboratory tests, bilateral BMB, and PET-CT scans with diagnostic CT using contrast agent. The ICER of PET/CT strategy was $16215 per patient with modified treatment. PET/CT costs at the beginning and end of treatment would increase total costs of HL staging and first-line treatment by only 2%.
Park et al[34] studied patients with an increase in carcinoembryonic antigen levels of more than 5 ng/mL during follow-up testing after the resection of their primary colorectal cancer. The CT + FDG-PET strategy was higher in mean cost by $429 per patient, but resulted in an increase in the mean life expectancy of 9.527 d per patient. Their perspective was that of public payer (Medicare) and they used a model approach (decision tree).
Lejeune et al[35] compared CT and CT + PET to assess the cost-effectiveness of FDG-PET in the management of metachronous liver metastases of colorectal cancer. CT was a dominated strategy, presenting an extra cost of €2671 ($3213) and a similar expected effectiveness-per-patient compared with CT + PET (1.88 years life expectancy per patient).
Wiering et al[36] evaluated the clinical effectiveness, impact on health care resources and cost-effectiveness of adding FDG-PET to the diagnostic algorithm, during a randomized clinical trial from a health care perspective. Both health-related quality of life and QALYs showed no significant difference between the conventional diagnostic work-up (CDW) and PET groups. NMB ranged from €1004 to €11060 depending on the monetary value given to a QALY. A bootstrap procedure was performed to provide an estimate of the uncertainty surrounding ICER.
Sloka et al[29] conducted a meta-analysis of studies for the accuracy of PET in staging breast cancer. The representative population is a 55-year-old woman presenting with stage I or II breast cancer. Authors compared PET and axillary lymph node dissection (ALND) in selected patients with ALND in all patients. A cost savings of $695 per person is expected for the PET strategy, with an increase in life expectancy (7.4 d), when compared with the non-PET strategy. This cost savings remained in favour of the PET strategy when subjected to a sensitivity analysis. ICER was not calculated.
Meng et al[30] evaluated the cost-effectiveness of MRI and PET compared with sentinel lymph node biopsy (SLNB) for assessment of axillary lymph node metastases in newly-diagnosed early stage breast cancer patients in the United Kingdom. The perspective was that of the health care system. MRI and PET are assessed firstly as a replacement for SLNB and secondly as an additional test prior to SLNB. The baseline SLNB strategy is dominated by the strategies of replacing SLNB with PET, with a NMB of 1085 (measured in United Kingdom £30000 per QALY).
Krug et al[37] performed a cost-effectiveness analysis, using a Markov model over a 10-year-period, to compare two different surveillance programs, either PET/CT or whole-body CT, in patients with suspected pulmonary metastasized melanoma. The Belgian health care payer perspective was adopted. The PET/CT strategy was dominant with a net saving of €1048 and a gain of 0.2 life-months gained.
Wallace et al[38] compared the health care costs and effectiveness of multiple staging options for patients with oesophageal cancer. A decision-analysis model was constructed to compare different staging strategies: CT scan, endoscopic ultrasound with fine-needle aspiration biopsy (EUS-FNA), PET, thoracoscopy/laparoscopy, and combinations of these. The marginal cost-effectiveness ratio for PET + EUS-FNA was $60544 per QALY.
Mansueto et al[39] evaluated the economic impact of the introduction of PET/CT in the early detection of recurrent ovarian cancer through a cost-effectiveness analysis of different diagnostic strategies: (1) CT only or baseline strategy; (2) PET/CT for negative CT or strategy A; and (3) PET/CT for all or strategy B. Strategy A is dominated by strategy B, which is more expensive (€2909 vs€2958), but also more effective (3 cases of surgery avoided) and presented an ICER of €226.77 per surgery avoided (range: €49.50-€433.00).
PET and PET/CT have high costs: in Germany[40], costs per examination range between €600 ($885) and €1000 ($1474); in United States, a median reimbursement is of $952.83; in Great Britain[41], costs may vary between £635-£1300 ($1030-$2109). Reimbursement amount may vary in different country.
Three types of economic evaluation of a medical procedure may be performed: cost-effectiveness analysis (CEA), cost-utility analysis (CUA), and cost-benefit analysis (CBA)[42]. Authors performing CEA analyse medical procedure including costs and LYG. ICER quantifies costs of a medical procedure, considering procedure efficacy. Acceptable ICER limit may vary in different country. CUA analyses costs and efficacy considering QALYs to quantify quality of life, too. CBA counts in monetary units (NMB) advantages of an imaging technique[40]. WTP value represents the maximum cost acceptable for a medical procedure.
Many groups have studied cost-effectiveness of PET/CT. Evidence based data about the cost-effectiveness of FDG-PET and PET/CT in lung cancer already exist. Cost-effectiveness of PET/CT has been studied in staging of NSCLC[43], in diagnosis of a SPN[44] and follow-up of NSCLC[45]. Currently, best PET/CT cost-effectiveness values are in staging NSCLC. German health care system has confirmed cost-effectiveness of FDG-PET/CT in staging and restaging of NSCLC[46].
Many authors made reviews[4,40] or health technology HTA reports[47,48] about the cost-effectiveness of PET in oncology. No systematic reviews about cost-effectiveness of FDG-PET in tumours other than lung cancer have been done until now.
In this study, cost-effectiveness of FDG-PET in staging of head and neck tumours has been analysed in one study. Hollenbeak et al[25] concluded that FDG-PET is cost-effective in staging and treating a N0 carcinoma, but prospective studies are needed to validate these results. Cost-effectiveness of FDG-PET in restaging head and neck tumours is controversial. Yen et al[26] analysed that PET-only strategy will become the most cost-effective for recurrent NPC in patients in the near future as the cost of PET will decrease. Rabalais et al[28] assessed that PET/CT is the most cost-effective strategy for surveillance of the patient with pre-treatment N2 disease, a controlled primary tumour, and a clinically negative neck after completion of chemo-radiotherapy (CRT). Sher et al[27] showed that PET/CT is the dominant, cost-effective strategy after CRT for N2-N3 head and neck squamous cell cancer, determining the necessity for adjuvant ND. Finally, FDG-PET seems to be cost-effective in staging and restaging in patients with head and neck tumours.
Cost-effectiveness of FDG-PET in staging of breast cancer is not clear. Sloka et al[29] found that PET strategy allows cost savings and that the use of this strategy for the staging of breast cancer was economically viable in Canada. Meng et al[30] demonstrated that MRI is more cost-effective than SLNB in diagnosis of axillary metastases. In fact, sensitivity of MRI was higher than PET, with lower costs. In conclusion, more studies are needed to evaluate cost-effectiveness of FDG-PET in patients with breast cancer.
Cost-effectiveness of FDG-PET in restaging HL is discussed. In his first study, Cerci et al[32] showed that for patients with HL presenting in CRu/PR with suspicious residual masses after first-line therapy, restaging FDG-PET was cost effective, producing 1% cost savings to Brazil public health care system. Bradbury et al[6] found that PET seemed to be cost-effective after CT in patients who have had a response to induction therapy. About cost-effectiveness of FDG-PET in staging lymphoma, in his second study, Cerci et al[33] concluded that PET/CT ICER ($16215) in the initial staging and end treatment of patients with HL was acceptable for health system. Klose et al[31] demonstrated that the use of PET could produce cost savings but more studies are needed to confirm the long-term cost-effectiveness of this procedure. Finally, FDG-PET seems to be cost-effective in staging and treatment evaluation in patients with lymphoma.
About cost-effectiveness of FDG-PET in restaging colon-rectum cancer, Wiering et al[36] concluded that FDG-PET in patients with resectable colorectal liver metastases resulted in better patient selection with potential cost savings. Park et al[34] showed the relative cost-effectiveness of using a CT and FDG-PET for managing patients candidates for surgical hepatic resection. Lejeune et al[35] demonstrated the economic value of CT and PET, with the consequence of decreasing the number of inappropriate surgical acts. In conclusion, further studies are needed to conclude that FDG-PET in patients with colon-rectum cancer is cost-effective.
Few evidences are available about cost-effectiveness in other tumours. Krug et al[37] showed that PET/CT strategy was cost-effective in restaging of patients with suspected pulmonary metastases of melanoma. Wallace et al[38] demonstrated that initial PET and EUS-FNA staging were more effective but also more expensive than other imaging strategies in oesophagus cancer. Mansueto et al[39] concluded that PET/CT in patients with suspected ovarian cancer recurrence was more cost-effective than CT only. So, there could be potentially cost-savings for the Italian National and Regional Healthcare System. In these tumours, cost-effectiveness of FDG-PET is not clear.
This study has several limitations. The review included studies with different economic model and perspective, produced in different country. Acceptable cost-effectiveness parameters (ICER, ICUR, LYG and NMB) may vary in different groups and health system. Authors often considered PET included in a complex diagnostic strategy, with the consequence of a not focused PET analysis. Many studies analysed PET scan and not hybrid PET/CT scan. In near future, PET/CT may be more accurate and then more cost-effective than PET scan alone. Only English language and FDG-PET studies have been included.
Finally, literature evidence about the cost-effectiveness of FDG-PET or PET/CT in tumours other than lung cancer is still limited. Not enough studies have been published about ovary cancer, oesophageal carcinoma and melanoma to assess cost-effectiveness of this strategy in medical management. More studies are available about cost-effectiveness of FDG-PET in staging and restaging colon-rectum cancer and staging breast cancer, but without clear economic parameters in favour of PET strategy. FDG-PET or PET/CT seems to be cost-effective in selective indications in oncology (staging and restaging of head and neck tumours, staging and treatment evaluation in lymphoma). Although more studies are needed to assess cost-effectiveness of FDG-PET, application of PET/CT will probably improve efficacy and economic outcome in these indications, in the near future.
Fluorine-18-Fluorodeoxyglucose positron emission tomography (FDG-PET) or PET/computed tomography (PET/CT) are useful imaging techniques to study cellular metabolism.
Cost-effectiveness analysis is a way to study both efficacy and cost of a medical procedure. These studies use parameters as “life years gained” or disability days saved. In cost-utility analysis, measures change with patient preference and authors refer to “quality-adjusted life years”.
In this study, cost-effectiveness of FDG-PET in staging of head and neck tumours has been analysed in one study.
Although more studies are needed to assess cost-effectiveness of FDG-PET, application of PET/CT will probably improve efficacy and economic outcome in these indications, in the near future.
This study is well designed and well done. The authors also realized and pointed out that the literature is limited on the cancer types studies in this article.
P- Reviewers: Chen P, Pan CX S- Editor: Qi Y L- Editor: A E- Editor: Wu HL
| 1. | Treglia G, Cason E, Fagioli G. Recent applications of nuclear medicine in diagnostics (first part). Ital J Med. 2010;4:84-91. |
| 2. | Salvatori M, Oradei M. Economic evaluation of nuclear medicine procedures. Eur J Nucl Med Mol Imaging. 2010;37:1786-1792. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 3] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 3. | Yang Y, Czernin J. Contribution of imaging to cancer care costs. J Nucl Med. 2011;52 Suppl 2:86S-92S. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 31] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 4. | Langer A. A systematic review of PET and PET/CT in oncology: a way to personalize cancer treatment in a cost-effective manner? BMC Health Serv Res. 2010;10:283. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 74] [Cited by in RCA: 61] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 5. | Cao JQ, Rodrigues GB, Louie AV, Zaric GS. Systematic review of the cost-effectiveness of positron-emission tomography in staging of non--small-cell lung cancer and management of solitary pulmonary nodules. Clin Lung Cancer. 2012;13:161-170. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 23] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 6. | Bradbury I, Bonell E, Boynton J, Cummins E, Facey K, Iqbal K, Laking G, McDonald C, Parpia T, Sharp P. Positron emission tomography (PET) imaging in cancer management (Health Technology Assessment Report 2). Glasgow: Health Technology Board for Scotland 2002; . |
| 7. | Bongers V, Hobbelink MG, van Rijk PP, Hordijk GJ. Cost-effectiveness of dual-head 18F-fluorodeoxyglucose PET for the detection of recurrent laryngeal cancer. Cancer Biother Radiopharm. 2002;17:303-306. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 14] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 8. | van Hooren AC, Brouwer J, de Bree R, Hoekstra OS, Leemans CR, Uyl-de Groot CA. The cost-effectiveness of 18FDG-PET in selecting patients with suspicion of recurrent laryngeal carcinoma after radiotherapy for direct laryngoscopy. Eur Arch Otorhinolaryngol. 2009;266:1441-1448. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 16] [Cited by in RCA: 14] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 9. | Uyl-de Groot CA, Senft A, de Bree R, Leemans CR, Hoekstra OS. Chest CT and whole-body 18F-FDG PET are cost-effective in screening for distant metastases in head and neck cancer patients. J Nucl Med. 2010;51:176-182. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 47] [Cited by in RCA: 44] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 10. | Kurien G, Hu J, Harris J, Seikaly H. Cost-effectiveness of positron emission tomography/computed tomography in the management of advanced head and neck cancer. J Otolaryngol Head Neck Surg. 2011;40:468-472. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 11. | Schegerin M, Tosteson AN, Kaufman PA, Paulsen KD, Pogue BW. Prognostic imaging in neoadjuvant chemotherapy of locally-advanced breast cancer should be cost-effective. Breast Cancer Res Treat. 2009;114:537-547. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 31] [Cited by in RCA: 23] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 12. | Auguste P, Barton P, Hyde C, Roberts TE. An economic evaluation of positron emission tomography (PET) and positron emission tomography/computed tomography (PET/CT) for the diagnosis of breast cancer recurrence. Health Technol Assess. 2011;15:iii-iv, 1-54. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 18] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 13. | Cooper KL, Meng Y, Harnan S, Ward SE, Fitzgerald P, Papaioannou D, Wyld L, Ingram C, Wilkinson ID, Lorenz E. Positron emission tomography (PET) and magnetic resonance imaging (MRI) for the assessment of axillary lymph node metastases in early breast cancer: systematic review and economic evaluation. Health Technol Assess. 2011;15:iii-iv, 1-134. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 14. | Strobel K, Schaefer NG, Renner C, Veit-Haibach P, Husarik D, Koma AY, Hany TF. Cost-effective therapy remission assessment in lymphoma patients using 2-[fluorine-18]fluoro-2-deoxy-D-glucose-positron emission tomography/computed tomography: is an end of treatment exam necessary in all patients? Ann Oncol. 2007;18:658-664. [PubMed] |
| 15. | Moulin-Romsee G, Spaepen K, Stroobants S, Mortelmans L. Non-Hodgkin lymphoma: retrospective study on the cost-effectiveness of early treatment response assessment by FDG-PET. Eur J Nucl Med Mol Imaging. 2008;35:1074-1080. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 7] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 16. | Brush J, Boyd K, Chappell F, Crawford F, Dozier M, Fenwick E, Glanville J, McIntosh H, Renehan A, Weller D. The value of FDG positron emission tomography/computerised tomography (PET/CT) in pre-operative staging of colorectal cancer: a systematic review and economic evaluation. Health Technol Assess. 2011;15:1-192, iii-iv. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 92] [Cited by in RCA: 77] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 17. | von Schulthess GK, Steinert HC, Dummer R, Weder W. Cost-effectiveness of whole-body PET imaging in non-small cell lung cancer and malignant melanoma. Acad Radiol. 1998;5 Suppl 2:S300-S302. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 12] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 18. | Bastiaannet E, Uyl-de Groot CA, Brouwers AH, van der Jagt EJ, Hoekstra OS, Oyen W, Verzijlbergen F, van Ooijen B, Thompson JF, Hoekstra HJ. Cost-effectiveness of adding FDG-PET or CT to the diagnostic work-up of patients with stage III melanoma. Ann Surg. 2012;255:771-776. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 35] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 19. | Heinzel A, Stock S, Langen KJ, Müller D. Cost-effectiveness analysis of amino acid PET-guided surgery for supratentorial high-grade gliomas. J Nucl Med. 2012;53:552-558. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 29] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 20. | Heinzel A, Stock S, Langen KJ, Müller D. Cost-effectiveness analysis of FET PET-guided target selection for the diagnosis of gliomas. Eur J Nucl Med Mol Imaging. 2012;39:1089-1096. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 36] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 21. | Hetzel M, Arslandemir C, König HH, Buck AK, Nüssle K, Glatting G, Gabelmann A, Hetzel J, Hombach V, Schirrmeister H. F-18 NaF PET for detection of bone metastases in lung cancer: accuracy, cost-effectiveness, and impact on patient management. J Bone Miner Res. 2003;18:2206-2214. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 141] [Cited by in RCA: 109] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 22. | Tateishi U, Morita S, Taguri M, Shizukuishi K, Minamimoto R, Kawaguchi M, Murano T, Terauchi T, Inoue T, Kim EE. A meta-analysis of (18)F-Fluoride positron emission tomography for assessment of metastatic bone tumor. Ann Nucl Med. 2010;24:523-531. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 74] [Cited by in RCA: 71] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 23. | Heinrich S, Goerres GW, Schäfer M, Sagmeister M, Bauerfeind P, Pestalozzi BC, Hany TF, von Schulthess GK, Clavien PA. Positron emission tomography/computed tomography influences on the management of resectable pancreatic cancer and its cost-effectiveness. Ann Surg. 2005;242:235-243. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 242] [Cited by in RCA: 209] [Article Influence: 10.5] [Reference Citation Analysis (0)] |
| 24. | Rondina MT, Wanner N, Pendleton RC, Kraiss LW, Vinik R, Zimmerman GA, Heilbrun M, Hoffman JM, Morton KA. A pilot study utilizing whole body 18 F-FDG-PET/CT as a comprehensive screening strategy for occult malignancy in patients with unprovoked venous thromboembolism. Thromb Res. 2012;129:22-27. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 21] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 25. | Hollenbeak CS, Lowe VJ, Stack BC. The cost-effectiveness of fluorodeoxyglucose 18-F positron emission tomography in the N0 neck. Cancer. 2001;92:2341-2348. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 26. | Yen RF, Yen MF, Hong RL, Tzen KY, Chien CR, Chen TH. The cost-utility analysis of 18-fluoro-2-deoxyglucose positron emission tomography in the diagnosis of recurrent nasopharyngeal carcinoma. Acad Radiol. 2009;16:54-60. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 24] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 27. | Sher DJ, Tishler RB, Annino D, Punglia RS. Cost-effectiveness of CT and PET-CT for determining the need for adjuvant neck dissection in locally advanced head and neck cancer. Ann Oncol. 2010;21:1072-1077. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 50] [Cited by in RCA: 48] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 28. | Rabalais A, Walvekar RR, Johnson JT, Smith KJ. A cost-effectiveness analysis of positron emission tomography-computed tomography surveillance versus up-front neck dissection for management of the neck for N2 disease after chemoradiotherapy. Laryngoscope. 2012;122:311-314. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 21] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 29. | Sloka JS, Hollett PD, Mathews M. Cost-effectiveness of positron emission tomography in breast cancer. Mol Imaging Biol. 2005;7:351-360. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 17] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 30. | Meng Y, Ward S, Cooper K, Harnan S, Wyld L. Cost-effectiveness of MRI and PET imaging for the evaluation of axillary lymph node metastases in early stage breast cancer. Eur J Surg Oncol. 2011;37:40-46. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 26] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 31. | Klose T, Leidl R, Buchmann I, Brambs HJ, Reske SN. Primary staging of lymphomas: cost-effectiveness of FDG-PET versus computed tomography. Eur J Nucl Med. 2000;27:1457-1464. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 42] [Cited by in RCA: 35] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 32. | Cerci JJ, Trindade E, Pracchia LF, Pitella FA, Linardi CC, Soares J, Delbeke D, Topfer LA, Buccheri V, Meneghetti JC. Cost effectiveness of positron emission tomography in patients with Hodgkin’s lymphoma in unconfirmed complete remission or partial remission after first-line therapy. J Clin Oncol. 2010;28:1415-1421. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 59] [Cited by in RCA: 57] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 33. | Cerci JJ, Trindade E, Buccheri V, Fanti S, Coutinho AM, Zanoni L, Linardi CC, Celli M, Delbeke D, Pracchia LF. Consistency of FDG-PET accuracy and cost-effectiveness in initial staging of patients with Hodgkin lymphoma across jurisdictions. Clin Lymphoma Myeloma Leuk. 2011;11:314-320. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 18] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 34. | Park KC, Schwimmer J, Shepherd JE, Phelps ME, Czernin JR, Schiepers C, Gambhir SS. Decision analysis for the cost-effective management of recurrent colorectal cancer. Ann Surg. 2001;233:310-319. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 62] [Cited by in RCA: 49] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 35. | Lejeune C, Bismuth MJ, Conroy T, Zanni C, Bey P, Bedenne L, Faivre J, Arveux P, Guillemin F. Use of a decision analysis model to assess the cost-effectiveness of 18F-FDG PET in the management of metachronous liver metastases of colorectal cancer. J Nucl Med. 2005;46:2020-2028. [PubMed] |
| 36. | Wiering B, Adang EM, van der Sijp JR, Roumen RM, de Jong KP, Comans EF, Pruim J, Dekker HM, Ruers TJ, Krabbe PF. Added value of positron emission tomography imaging in the surgical treatment of colorectal liver metastases. Nucl Med Commun. 2010;31:938-944. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 28] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 37. | Krug B, Crott R, Roch I, Lonneux M, Beguin C, Baurain JF, Pirson AS, Vander Borght T. Cost-effectiveness analysis of FDG PET-CT in the management of pulmonary metastases from malignant melanoma. Acta Oncol. 2010;49:192-200. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 28] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 38. | Wallace MB, Nietert PJ, Earle C, Krasna MJ, Hawes RH, Hoffman BJ, Reed CE. An analysis of multiple staging management strategies for carcinoma of the esophagus: computed tomography, endoscopic ultrasound, positron emission tomography, and thoracoscopy/laparoscopy. Ann Thorac Surg. 2002;74:1026-1032. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 152] [Cited by in RCA: 121] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 39. | Mansueto M, Grimaldi A, Mangili G, Picchio M, Giovacchini G, Viganò R, Messa C, Fazio F. Positron emission tomography/computed tomography introduction in the clinical management of patients with suspected recurrence of ovarian cancer: a cost-effectiveness analysis. Eur J Cancer Care (Engl). 2009;18:612-619. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 17] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 40. | Buck AK, Herrmann K, Stargardt T, Dechow T, Krause BJ, Schreyögg J. Economic evaluation of PET and PET/CT in oncology: evidence and methodologic approaches. J Nucl Med. 2010;51:401-412. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 82] [Cited by in RCA: 87] [Article Influence: 5.8] [Reference Citation Analysis (0)] |
| 41. | Facey K, Bradbury I, Laking G, Payne E. Overview of the clinical effectiveness of positron emission tomography imaging in selected cancers. Health Technol Assess. 2007;11:iii-iv, xi-267. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 142] [Cited by in RCA: 127] [Article Influence: 7.1] [Reference Citation Analysis (0)] |
| 42. | Drummond M, Sculpher M, Torrance G, O’Brien B, Stoddart G. Methods for the Economic Evaluation of Health Care Programmes. Oxford, UK: Oxford University Press 2005; . |
| 43. | Nguyen VH, Peloquin S, Lacasse Y. Cost-effectiveness of positron emission tomography for the management of potentially operable non-small cell lung cancer in Quebec. Can Respir J. 2005;12:19-25. [PubMed] |
| 44. | Lejeune C, Al Zahouri K, Woronoff-Lemsi MC, Arveux P, Bernard A, Binquet C, Guillemin F. Use of a decision analysis model to assess the medicoeconomic implications of FDG PET imaging in diagnosing a solitary pulmonary nodule. Eur J Health Econ. 2005;6:203-214. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 32] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 45. | van Loon J, Grutters JP, Wanders R, Boersma L, Dingemans AM, Bootsma G, Geraedts W, Pitz C, Simons J, Brans B. 18FDG-PET-CT in the follow-up of non-small cell lung cancer patients after radical radiotherapy with or without chemotherapy: an economic evaluation. Eur J Cancer. 2010;46:110-119. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 41] [Cited by in RCA: 37] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 46. | Abschlussbericht des Gemeinsamen Bundesausschusses nach 91 Abs. 7 SGB V ‘‘Krankenhausbehandlung.’’. Bundesanzeiger. 2006;43:1374. |
| 47. | Cleemput I, Dargent G, Poelmans J, Camberlin C, Van den Bruel A, Ramaekers D. HTA Tomographie par Emission de Positrons en Belgique. Bruxelles: Centre Fédéral d’Expertise des Soins de Santé (KCE) 2005; 22B. |
| 48. | Müller A, Stratmann-Schöne D, Klose T, Leidl R. Overview of economic evaluation of positron-emission tomography. Eur J Health Econ. 2002;3:59-65. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 3] [Article Influence: 0.1] [Reference Citation Analysis (0)] |