Published online Jul 28, 2012. doi: 10.4329/wjr.v4.i7.324
Revised: June 16, 2012
Accepted: June 23, 2012
Published online: July 28, 2012
AIM: To compare different multidetector computed tomography (MDCT) protocols to optimize pancreatic contrast enhancement.
METHODS: Forty consecutive patients underwent contrast-enhanced biphasic MDCT (arterial and portal-venous phase) using a 64-slice MDCT. In 20 patients, the scan protocol was adapted from a previously used 40-channel MDCT scanner with arterial phase scanning initiated 11.1 s after a threshold of 150 HU was reached in the descending aorta, using automatic bolus tracking (Protocol 1). The 11.1-s delay was changed to 15 s in the other 20 patients to reflect the shorter scanning times on the 64-channel MDCT compared to the previous 40-channel system (Protocol 2). HU values were measured in the head and tail of the pancreas in the arterial and portal-venous phase.
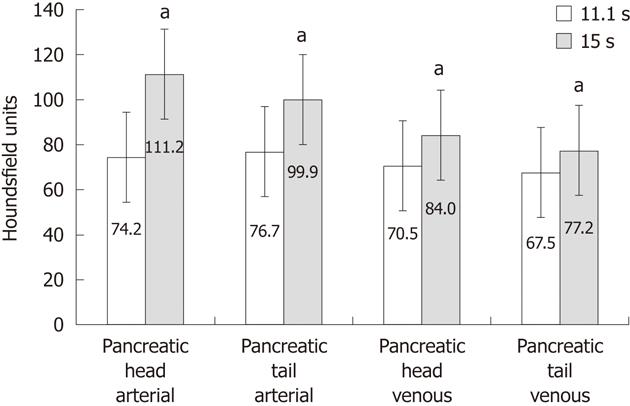
RESULTS: Using an 11.1-s delay, 74.2 HU (head) were measured on average in the arterial phase and 111.2 HU (head) were measured using a 15-s delay (P < 0.0001). For the pancreatic tail, the average attenuation level was 76.73 HU (11.1 s) and 99.89 HU (15 s) respectively (P = 0.0002). HU values were also significantly higher in the portal-venous phase [pancreatic head: 70.5 HU (11.1 s) vs 84.0 HU (15 s) (P = 0.0014); pancreatic tail: 67.45 HU (11.1 s) and 77.18 HU (15 s) using Protocol 2 (P = 0.0071)].
CONCLUSION: Sixty-four MDCT may yield a higher contrast in pancreatic study with (appropriate) optimization of scan delay time.
- Citation: Stuber T, Brambs HJ, Freund W, Juchems MS. Sixty-four MDCT achieves higher contrast in pancreas with optimization of scan time delay. World J Radiol 2012; 4(7): 324-327
- URL: https://www.wjgnet.com/1949-8470/full/v4/i7/324.htm
- DOI: https://dx.doi.org/10.4329/wjr.v4.i7.324
Contrast-enhanced multidetector computed tomography (MDCT) for pancreatic imaging is widely accepted, especially for detection and preoperative staging of pancreatic adenocarcinoma, as well as for diagnosis and follow-up examinations of patients with pancreatitis. Scanning protocols are usually multiphasic with acquirement of arterial and portal-venous phases of contrast material (CM) enhancement.
Several studies[1-3] have been conducted to evaluate the appropriate scan timing to achieve optimal CM enhancement. To the best of our knowledge, the data published to date have evaluated CM enhancement of pancreatic parenchyma with scan protocols for MDCT scanners with up to 16 detector rows. The purpose of our study was to compare different MDCT protocols for a 64-slice MDCT scanner to achieve a better pancreatic contrast enhancement protocol.
Forty consecutive patients underwent biphasic pancreatic examination with a 64-channel MDCT (Brilliance 64; Philips Medizin-Systeme, Hamburg, Germany). The patient group consisted of 22 female and 18 male patients, aged 36-92 years, with a mean age of 68.8 years. Indications for abdominal CT were as follows: follow-up after abdominal tumor [gastrointestinal stromal tumor (GIST): n = 10; cholangiocellular carcinoma (CCC): n = 12]; exclusion of abdominal tumor (CCC: n = 5; GIST: n = 1, carcinoid: n = 1); exclusion of gastrointestinal bleeding: n = 6; exclusion of pancreatitis: n = 2; exclusion of intraductal papillary neoplasia: n = 3.
Written consent was obtained from each patient or patient’s legal representative before CT examination. Exclusion criteria included general contraindications for CT including pregnancy and allergy to CM, as well as known pancreatic tumor and pancreatitis.
Arterial and portal-venous phase images were obtained after intravenous administration of CM (400 mg/mL iomeprol, Imeron 400; Bracco, Milano, Italy) using a power injector (Injektron CT2; Medtron AG, Saarbrücken, Germany) at a dose of 1.2 mL/kg body weight and a rate of 4 mL/s followed by a saline chaser.
In 20 patients, the scan protocol was adapted from a previously used 40-channel MDCT scanner with arterial phase scanning initiated 11.1 s after a threshold of 150 HU was reached in the descending aorta using automatic bolus tracking (Protocol 1). The delay was changed to 15 s in the other 20 patients to reflect the shorter scanning times on the 64-channel MDCT compared to the previous 40-channel system (Protocol 2). The delay of the portal-venous phase acquisition was set to 60 s after onset of arterial phase. For all scans, the scanner parameters were set as follows: arterial phase (120 kv, 200-300 mAs, collimation 64 × 0.625, pitch: 0.9, reconstructed slice thickness: 0.8 mm), portal-venous phase (120 kv, 180-250 mAs, collimation 64 × 0.625, pitch: 0.9, reconstructed slice thickness: 2 mm). CT images were reviewed digitally on a dedicated PACS workstation (Impax 4.5; AGFA Healthcare, Köln, Germany). Attenuation levels were measured in the head and tail of the pancreas in the arterial and portal-venous phase by an attending radiologist with 8 years of experience in reading abdominal CT. The size of the measurement region ranged from 0.45 to 0.55 cm2. Focal lesions within the pancreatic tissue were excluded from measurement areas. The differences between the groups were investigated by an exploratory unpaired t test. P < 0.01 was considered statistically significant.
In the arterial phase, the mean attenuation level in the pancreatic head was 74.2 ± 14.3 (mean ± SD) HU using the 11.1-s delay compared to 111.2 ± 19.9 HU with scan Protocol 2 (P = 0.0001). Attenuation levels ranged from 49.8 to 98.1 HU (11.1 s) and 81.3 to 148.4 HU (15 s). Attenuation measured in the pancreatic tail parenchyma ranged from 54.5 to 98.8 HU (11.1 s) and 73.0 to 139.9 (Protocol 2) with an average parenchymal attenuation level of 76.73 ± 13.8 HU (11.1 s) and 99.89 ± 20.6 HU (15 s) (P = 0.0002).
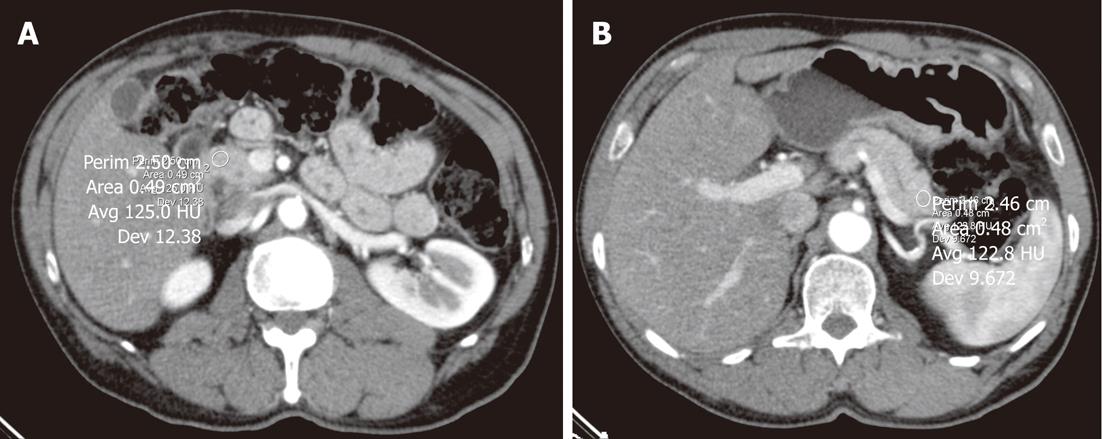
HU values were also significantly higher (P = 0.0014) in the pancreatic head using the longer scan delay (Figure 1). Mean attenuation levels were 70.5 ± 11.3 HU (11.1 s) vs 84.0 HU (15 s). Contrast density within the pancreatic head ranged from 49.5 to 91.6 HU (Protocol 1) and 63.0 to 111.9 HU (15 s). In the pancreatic tail parenchyma, the average enhancement was 67.45 ± 7.7 HU (11.1 s) compared to 77.18 ± 13.2 HU (15 s) using Protocol 2 (P = 0.0071). The range of attenuation in the pancreatic tail was 51.1-83.2 HU (11.s) and 53.6-100.2 HU (15 s). Figure 2 give examples of attenuation levels of pancreatic parenchyma in arterial-phase imaging with a 15-s scan delay.
MDCT is an excellent tool for diagnostic work-up of patients with pancreatic diseases, especially of patients suffering from pancreatic tumors. The role of CT in the assessment of pancreatic diseases has gained more impact since multi-channel CT became widely available[4].
Bae[5] investigated the peak aortic contrast enhancement in a porcine model in 2003 and showed a linear increase in enhancement with duration of CM injection. Since then, examination protocols and scan delay have been subject to several studies. In 2001, McNulty et al[6] demonstrated for a four-channel MDCT that the mean attenuation level of normal pancreatic parenchyma was higher in the pancreatic parenchymal phase than in arterial or portal-venous phase imaging. The mean CM enhancement was 122 compared to 70 and 109 HU, respectively. The delay for the pancreatic parenchymal phase was 35 s after the onset of CM injection. In 2006, Goshima et al[7] examined the enhancement of pancreatic tissue with scan delays ranging from 25 to 80 s after injection of CM, with a fixed duration of 30 s. The CT scanner used in this study was an eight-channel MDCT. The peak enhancement was obtained after a 40-s delay with intense attenuation levels of pancreatic parenchyma ranging from 82.1 to 85.2 HU with delays of 35-45 s. Kondo et al[8] published data for eight-channel MDCT pancreatic imaging showing the most intensive enhancement of the pancreatic parenchyma 15-20 s after triggering of bolus tracking with attenuation levels of 84-85 HU. Ichikawa et al[9] reported a delay of 40 s after injection of CM for the pancreatic parenchymal phase. Images were acquired with a 16-channel MDCT scanner after administration of 100 mL CM. Horton et al[10] described a scan protocol for a 64-channel MDCT scanner in an educational exhibit on MDCT appearance of pancreatic islet cell tumors.
In our study, we found significant differences in attenuation levels of pancreatic parenchyma between the scan protocols with an 11-s vs 15-s delay for the start of the arterial phase. HU values in the portal-venous phase were also significantly higher using Protocol 2 instead of Protocol 1. Our findings suggest that higher pancreatic parenchymal attenuation and therefore increased tumor-to-pancreas contrast can be obtained by optimizing scan protocols when using faster MDCT scanners.
One of the limitations of our study was the relatively small number of 40 patients and the fact that we only used one manufacturer’s 64-channel MDCT scanner. The attenuation levels of pancreatic parenchyma may differ with different types of MDCT generations or scanners. Birnbaum et al[11] assessed intra- and interscanner variability using an anthropomorphic body CT phantom, showing that there are significant differences of CT attenuation levels between different MDCT scanner generations as well as between different manufacturers’ scanners. Further studies should investigate the influence of scan delays for pancreatic imaging with different manufacturer’s scanners.
Sixty-four MDCT may achieve higher contrast in pancreatic studies, with appropriate optimization of scan delay time.
Scanning protocols for pancreatic imaging with multidetector row computed tomography (MDCT) are usually multiphasic with acquisition of arterial and portal-venous phases of contrast material (CM) enhancement. Due to the faster scanning speed, a redesign of scanning protocols is required.
Pancreatic parenchyma can contain benign or malignant lesions that should be classified by pancreatic imaging in order to prevent unnecessary operations. Achievement of optimal CM enhancement is mandatory for evaluation of pancreatic lesions. CT scanners of newer generations consist of more detector rows, allowing faster scanning of patients and thinner imaging slices.
Optimized contrast between normal pancreatic parenchyma and pathological changes can be achieved by adaptation of examination protocols to the faster scanning speed of MDCT. Data published to date evaluate CM enhancement of pancreatic parenchyma with scan protocols for MDCT scanners with up to 16 detector rows. The authors of the present study evaluated scanning protocols of 40- and 64-channel MDCT scanners and found significant differences in contrast attenuation of pancreatic parenchyma between the scan protocol with an 11-s vs 15-s delay for the start of the arterial phase. The findings suggest that higher pancreatic parenchymal attenuation and therefore increased tumor-to-pancreas contrast can be obtained by optimizing scan protocols when using faster MDCT scanners.
The study results suggest that 64 MDCT may achieve higher contrast in pancreatic studies with appropriate optimization of scan delay time. This may help to optimize pancreatic imaging.
It is an interesting paper, but it should be revised before publication.
Peer reviewers: Dr. Kazushi Kishi, Wakayama Medical University, Wakayama City 641-8510, Japan; Dr. Charikleia Triantopoulou, Konstantopouleion Hospital, 3-5, Agias Olgas street, Athens 14233 Nea Ionia, Greece
S- Editor Cheng JX L- Editor Kerr C E- Editor Zheng XM
| 1. | Lu DS, Vedantham S, Krasny RM, Kadell B, Berger WL, Reber HA. Two-phase helical CT for pancreatic tumors: pancreatic versus hepatic phase enhancement of tumor, pancreas, and vascular structures. Radiology. 1996;199:697-701. [PubMed] |
| 2. | Hollett MD, Jorgensen MJ, Jeffrey RB. Quantitative evaluation of pancreatic enhancement during dual-phase helical CT. Radiology. 1995;195:359-361. [PubMed] |
| 3. | Bonaldi VM, Bret PM, Atri M, Garcia P, Reinhold C. A comparison of two injection protocols using helical and dynamic acquisitions in CT examinations of the pancreas. AJR Am J Roentgenol. 1996;167:49-55. [PubMed] |
| 4. | Graf O, Boland GW, Warshaw AL, Fernandez-del-Castillo C, Hahn PF, Mueller PR. Arterial versus portal venous helical CT for revealing pancreatic adenocarcinoma: conspicuity of tumor and critical vascular anatomy. AJR Am J Roentgenol. 1997;169:119-123. [PubMed] |
| 5. | Tamm EP, Balachandran A, Bhosale P, Szklaruk J. Update on 3D and multiplanar MDCT in the assessment of biliary and pancreatic pathology. Abdom Imaging. 2009;34:64-74. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 36] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 6. | Sahani DV, Sainani NI, Blake MA, Crippa S, Mino-Kenudson M, del-Castillo CF. Prospective evaluation of reader performance on MDCT in characterization of cystic pancreatic lesions and prediction of cyst biologic aggressiveness. AJR Am J Roentgenol. 2011;197:W53-W61. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 63] [Cited by in RCA: 63] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 7. | Grieser C, Steffen IG, Grajewski L, Stelter L, Streitparth F, Schnapauff D, Glanemann M, Langrehr J, Andreou A, Neuhaus P. Preoperative multidetector row computed tomography for evaluation and assessment of resection criteria in patients with pancreatic masses. Acta Radiol. 2010;51:1067-1077. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 11] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 8. | Bae KT. Peak contrast enhancement in CT and MR angiography: when does it occur and why Pharmacokinetic study in a porcine model. Radiology. 2003;227:809-816. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 177] [Cited by in RCA: 167] [Article Influence: 7.6] [Reference Citation Analysis (0)] |
| 9. | McNulty NJ, Francis IR, Platt JF, Cohan RH, Korobkin M, Gebremariam A. Multi--detector row helical CT of the pancreas: effect of contrast-enhanced multiphasic imaging on enhancement of the pancreas, peripancreatic vasculature, and pancreatic adenocarcinoma. Radiology. 2001;220:97-102. [PubMed] |
| 10. | Goshima S, Kanematsu M, Kondo H, Yokoyama R, Miyoshi T, Kato H, Tsuge Y, Shiratori Y, Hoshi H, Onozuka M. Pancreas: optimal scan delay for contrast-enhanced multi-detector row CT. Radiology. 2006;241:167-174. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 54] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 11. | Kondo H, Kanematsu M, Goshima S, Miyoshi T, Shiratori Y, Onozuka M, Moriyama N, Bae KT. MDCT of the pancreas: optimizing scanning delay with a bolus-tracking technique for pancreatic, peripancreatic vascular, and hepatic contrast enhancement. AJR Am J Roentgenol. 2007;188:751-756. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 58] [Cited by in RCA: 53] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 12. | Ichikawa T, Erturk SM, Sou H, Nakajima H, Tsukamoto T, Motosugi U, Araki T. MDCT of pancreatic adenocarcinoma: optimal imaging phases and multiplanar reformatted imaging. AJR Am J Roentgenol. 2006;187:1513-1520. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 65] [Cited by in RCA: 59] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 13. | Horton KM, Hruban RH, Yeo C, Fishman EK. Multi-detector row CT of pancreatic islet cell tumors. Radiographics. 2006;26:453-464. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 113] [Cited by in RCA: 83] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 14. | Fenchel S, Fleiter TR, Aschoff AJ, van Gessel R, Brambs HJ, Merkle EM. Effect of iodine concentration of contrast media on contrast enhancement in multislice CT of the pancreas. Br J Radiol. 2004;77:821-830. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 52] [Cited by in RCA: 43] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 15. | Tublin ME, Tessler FN, Cheng SL, Peters TL, McGovern PC. Effect of injection rate of contrast medium on pancreatic and hepatic helical CT. Radiology. 1999;210:97-101. [PubMed] |
| 16. | Birnbaum BA, Hindman N, Lee J, Babb JS. Multi-detector row CT attenuation measurements: assessment of intra- and interscanner variability with an anthropomorphic body CT phantom. Radiology. 2007;242:109-119. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 180] [Cited by in RCA: 204] [Article Influence: 11.3] [Reference Citation Analysis (0)] |