Copyright
©The Author(s) 2015.
World J Radiol. Nov 28, 2015; 7(11): 375-381
Published online Nov 28, 2015. doi: 10.4329/wjr.v7.i11.375
Published online Nov 28, 2015. doi: 10.4329/wjr.v7.i11.375
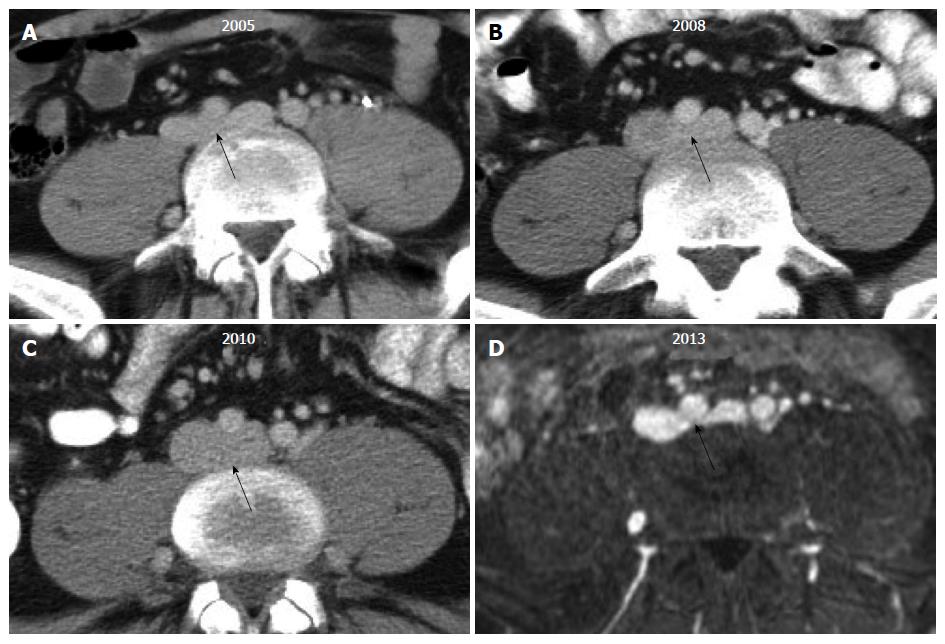
Figure 1 Transverse computed tomography and magnetic resonance images of the proximal left common iliac vein (black arrow) in a single patient across multiple time points illustrate the challenge of diagnosing May-Thurner syndrome.
The degree of venous compression can vary substantially from one imaging study to another based upon the patient’s volume status.
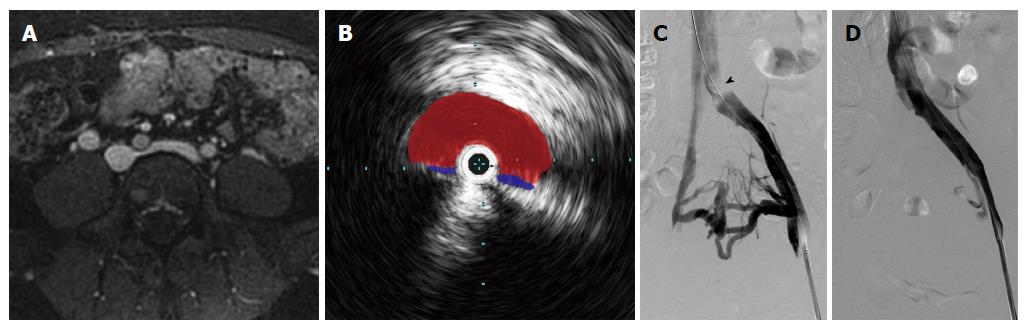
Figure 2 The appearance of May-Thurner syndrome on multiple imaging modalities from a single patient.
A: Axial T1 fat-saturated magnetic resonance image following the administration of an intravascular contrast agent demonstrates > 50% narrowing of the left common iliac vein by the overlying right common iliac artery; B: Intravascular ultrasound with the transducer within the left common iliac vein (blue) demonstrates near complete obliteration of the vessel’s lumen due to compression by the right common iliac artery (red); C: Digital subtraction angiography with contrast injection from a vascular sheath in the left external iliac vein demonstrates an obliquely oriented silhouette of the right common iliac artery compressing the left common iliac vein (arrowhead); multiple left-to-right pelvic collaterals are also present, signifying that the compression is hemodynamically significant; D: Following the placement of an uncovered stent, the compression is resolved, and there is no longer filling of the cross-pelvic collaterals.
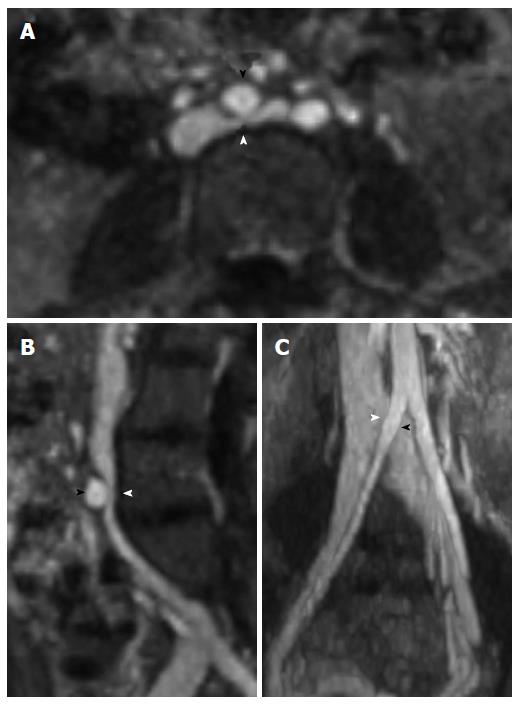
Figure 3 Magnetic resonance venography with axial (A), sagittal (B), and coronal (C) reformatted images demonstrating May-Thurner syndrome anatomy with compression of the left common iliac vein (white arrowhead) by the right common iliac artery (black arrowhead).
- Citation: Brinegar KN, Sheth RA, Khademhosseini A, Bautista J, Oklu R. Iliac vein compression syndrome: Clinical, imaging and pathologic findings. World J Radiol 2015; 7(11): 375-381
- URL: https://www.wjgnet.com/1949-8470/full/v7/i11/375.htm
- DOI: https://dx.doi.org/10.4329/wjr.v7.i11.375