Published online Sep 26, 2021. doi: 10.4330/wjc.v13.i9.438
Peer-review started: December 31, 2020
First decision: March 31, 2021
Revised: April 10, 2021
Accepted: July 19, 2021
Article in press: July 19, 2021
Published online: September 26, 2021
Processing time: 260 Days and 13.7 Hours
Experiencing various forms of violence in either childhood or adulthood has been associated with cardiovascular disease, both shortly after the event and during follow-up, particularly in women. The coronavirus disease 2019 pandemic has heightened the risk of domestic violence with serious sequelae for mental and cardiovascular health in women, possibly due to several contributing factors, ranging from lockdown, stay at home regulations, job losses, anxiety, and stress. Accordingly, it remains paramount to enforce proactive preventive strategies, at both the family and individual level, maintain a high level of attention to recognize all forms of violence or abuse, and guarantee a multidisciplinary team approach for victims of interpersonal or domestic violence in order to address physical, sexual, and emotional domains and offer a personalized care.
Core Tip: Interpersonal violence has been associated with cardiovascular disease, particularly in women. The coronavirus disease 2019 pandemic has heightened the risk of domestic violence with serious sequelae for mental and cardiovascular health in women. There is a need of research aimed to better understanding the impact of intimate partner violence on cardiovascular risk in women, both shortly after the event and during follow-up. It is important to prevent violence and to guarantee a multidisciplinary team approach for patients who have experienced interpersonal violence in order to address physical, sexual, and emotional domains.
- Citation: Mazza M, Marano G, Gonsalez del Castillo A, Chieffo D, Albano G, Biondi-Zoccai G, Galiuto L, Sani G, Romagnoli E. Interpersonal violence: Serious sequelae for heart disease in women. World J Cardiol 2021; 13(9): 438-445
- URL: https://www.wjgnet.com/1949-8462/full/v13/i9/438.htm
- DOI: https://dx.doi.org/10.4330/wjc.v13.i9.438
Interpersonal violence represents a serious public health issue. It is defined as physical or sexual violence, emotional abuse, and stalking, and is experienced by more than 30% of women in United States. It is globally recognized as the leading cause of homicide death for women. Psychological violence has been recognized as a traumatic event equal to other types of abuse (e.g., physical or sexual violence). It causes severe consequences, not only for the victims and families involved, but also to the whole society.
It is well known that intimate partner violence has short-term and long-term effects on the physical and mental health of victims and their children[1]. Epidemiological studies have highlighted an increased risk of chronic medical conditions (including asthma, arthritis, autoimmune disorders, cancer, stroke, diabetes mellitus, hyperten
It has been recently suggested that intimate partner violence might increase the risk of cardiovascular disease in women. Chandan et al[3] conducted a retrospective study in a cohort of 18547 women from a United Kingdom primary care registry that found that women with a history of intimate partner violence had a 31% increased risk for later cardiovascular disease (in particular a 50% increased risk for ischemic heart disease), a 51% increased risk for diabetes mellitus, and a 44% increased risk for total mortality[3]. In general, chronic diseases, including cardiovascular disease and hypertension, cancer, sexually transmitted infections, drug and alcohol abuse, smoking, diabetes, and elevated cortisol, have been ascertained at greater rates in women who have been victims of intimate partner violence[4].
Scott-Storey[5] developed a conceptual model to portray direct and indirect pathways by which severity of lifetime abuse (physical, sexual, and/or psychological) may affect women’s cardiovascular risk. According to this model, there are three pathways through which lifetime abuse may increase cardiovascular disease risk among women. First, lifetime abuse as a chronic stressor contributes to creating a state of vulnerability, potentially causing significant neuroendocrine, metabolic, hemostatic, and immunologic changes within the body (for example, elevated blood pressure, a clinically important early indicator of cardiovascular risk)[6]. It is probable that chronic upregulation of the so-called fight-or-flight hormones, chronic inflammation, or dysregulation of the hypothalamic pituitary axis may contribute to poor heart health. Second, coping strategies used by victims of abuse to deal with stress, such as smoking and overeating, represent cardiovascular risk behaviors, and tend to persist long after the experience of abuse situation has ended. Third, it has been largely demonstrated that women with histories of abuse have higher incidence of depressive disorders and depressive symptoms, and depression strictly correlates to chronically elevated levels of cortisol, catecholamines, and inflammatory markers, all of which promote the development and progression of cardiovascular disease[7]. Recently it has been highlighted that women suffering from high levels of depressive symptoms in the immediate period after leaving an abusive partner may be most at risk for persistent mental illness after the separation: this reinforces the need for early depression intervention and treatment. It has been also hypothesized that women who experience less change in their depressive symptoms over time may have higher cardiovascular risk, and therefore, may be considered a potential target group for primary and secondary prevention of cardiovascular disease[5].
Biological mechanisms underlying physical health sequelae of interpersonal violence are very poorly understood: it can be hypothesized that intimate partner violence induces a chronic inflammatory state, but further studies are needed focusing on biomarkers of inflammation and specific markers of disease in abused women, including C-reactive protein, cortisol, erythrocyte sedimentation rate, and cardiac biomarkers (troponin, creatine kinase myocardial band, brain-natriuretic-peptide)[4]. There is evidence for a link between intimate partner violence and the development of endocrine diseases, including diabetes. Additionally, interpersonal violence has been associated with lowered cortisol awakening response, flattened diurnal cortisol patterns, and higher midday cortisol. Given that cortisol is considered a biomarker of physical and psychological stress states and is involved in endocrine disease states, the effect of interpersonal violence on cortisol levels may be a promising area of future research[8].
There is a bi-directional relationship between mental health disorders (including depression, anxiety, and/or cognitive dysfunction) and cardiovascular diseases. Autonomic dysfunction and inflammation may contribute to the increased cardiovascular mortality risk associated with depression, and a mutation of the ryanodine receptor sarcoplasmic reticulum calcium release channel can result in cardiac arrhythmias and seizures[9]. Complex interrelated disease mechanisms also regard specific syndromes in which pre-existing neurological or psychiatric illnesses may predispose and contribute to cardiovascular involvement (as in Takotsubo syndrome), or in which psycho-physical stress, dysregulation of the interplay between innate immune and central nervous systems, and/or pre-existing cardiovascular disease lead to secondary mental health disorders and brain damage (as in peripartum cardiomyopathy and atrial fibrillation).
Many studies have shown a mutual bond between the cardiovascular system and depression. Patients with cardiovascular disease who are also depressed have a worse outcome than those patients who are not depressed. A graded relationship can be described: the more severe the depression, the higher the subsequent risk of mortality and other cardiovascular events[10].
Depression is considered an independent risk factor for the development of cardiovascular diseases and contributes to a worse prognosis, further increasing the risk of mortality or subsequent major adverse cardiovascular events, such as nonfatal stroke, nonfatal myocardial infarction, and cardiovascular death. After a stroke, women present poorer quality of life than men due to different risk factors among which one of the most frequent is depression[11-14]. This association between depression and cardiovascular diseases has been confirmed for both men and women, for different age groups, and in various cultures; furthermore, the strength of this link is similar to that of other risk factors, such as smoking and high cholesterol[15]. The relationship between depression and cardiovascular disease has been analyzed through etiological and prognostic studies. The possibility has been ascertained that depression exerts a direct influence on psychophysiological mechanisms, whose alterations result in the development of atherosclerosis, and thus, lead to coronary events. Additionally, psychobiological models have identified different mechanisms of connection between depression and coronary artery disease. Other studies have shown that indirect mechanisms are based on the possibility that depression can favor cardiovascular disorders by modulating some coronary risk factors. This hypothesis has given rise to a line of research aimed at identifying various behavioral and psycho-social mediators that can explain the association between depression and coronary heart disease[11,12]. It has been also outlined that mind-body interventions, such as meditation, mindfulness and yoga can promote beneficial effects on stress reduction acting through modulation on cortisol secretion, blood pressure, heart rate variability, and immune reactions, and thus positively preserving women's cardiovascular health[15].
A growing body of research suggests that experiencing violence in either childhood or adulthood is associated with cardiovascular disease. The effects of violence may differ by life course stage. For example, violence exposure in childhood deserves a special attention, as biological mechanisms used to compensate for chronic stress exposure may be detrimental to health, leading to an early development of cardiovascular diseases. Furthermore, unhealthy habits used to cope with stress (lifestyle factors and substance use behaviors) can be formed during these early years, and could contribute to greater cardiovascular risk in childhood that may persist into adulthood. In addition, physiological development of the brain and other organ systems can be derailed under chronic exposure to stress, disrupting emerging brain architecture, as well as cognitive and behavioral functioning, and making children particularly vulnerable to the effects of violence and abuse with long-term consequences on the development of chronic disease, including cardiovascular disease[16]. Children who are exposed to threats to themselves, their family, or their community have an increased risk of subsequent myocardial infarction, stroke, ischemic heart disease, coronary heart disease, and/or death from one of these conditions. It should be noted that children from racial and ethnic minority groups or lower economic backgrounds face higher rates of such experiences, and may therefore be considered at higher risk for cardiovascular disease[17].
Long-term effects of violence exposure have been noted in relation to depression, aggression, substance use, and risk-taking behaviors. Many children and adults exposed to violence may develop post-traumatic stress disorder and depression, frequently associated with obesity, hypertension, and adverse cardiac outcomes[18]. Additionally, studies have documented an association of interpersonal violence exposure with tobacco use, alcohol use, poor dietary habits, and sedentary lifestyle, all of which potentially linked to cardiovascular health[19-21].
The coronavirus disease 2019 (COVID-19) pandemic has produced in a few weeks a substantial disruption worldwide. In the COVID era, affectivity and sexuality are remodeled: social distancing slows down the spread of the Coronavirus but represses or changes the need for relationships. A high global prevalence of depression and anxiety during the COVID-19 pandemic has been described, with a wide variance based on the region and country, as a direct effect of physical distancing measures imposed by national governments[22].
It has been shown that physical distancing (mostly referred to as social distancing) may deteriorate physical and mental health. In particular, reduced social connection is associated with chronic physical symptoms, including cardiovascular disease, reduced nutrition, higher probability of hospital readmissions, reduced vaccine uptake, early mortality, depression with suicidal ideation, social anxiety, psychotic symptoms, and cognitive impairment[23]. In general, psychosocial risk factors such as stress, social isolation, low socioeconomic status, hostility, anger, and stress-related psychiatric disorders are known to have negative impacts on health outcomes, but their effects on ischemic heart disease, particularly in women, have not yet been fully demonstrated[24].
A heightened risk of domestic violence has been associated with the restriction of travels imposed by many governments to prevent the spread of COVID-19 and other infection-reducing measures. The reasons for this include social isolation, exposure to economic and psychological stressors, increase in negative coping mechanisms (such as alcohol or drugs misuse), and inability to access usual health and social services[25]. During quarantine due to COVID-19, home became a dangerous place for victims of domestic violence because they are bound to stay the whole day with abusing partners and isolated from the others who could potentially give support. Present vulnerabilities can exacerbate family violence perpetration and prey victimization, and can aggravate maladaptive or dysfunctional relationships, directly impacting on cardiovascular system. It has been observed that women during quarantine report significant post-traumatic stress symptoms, and may show depression or anxiety, risk factors for the development or worsening of cardiovascular disease[26]. Currently, the pandemic has brought direct cardiac complications of infection and a potential impact on the standard acute and chronic management of cardiovascular disorders, compromising cardioprotective medications and health behavior regimens[27]. In addition, physical and social isolation can exacerbate maladaptive thought processes (such as anger, loneliness, pessimism, obsessive-compulsive behaviors, hopelessness, helplessness, and/or frustration) or extreme response to stress (such as hypervigilance or alcohol or drugs abuse) that may have consequences on population cardiovascular health[28]. Anxieties and fears related to risk of infection could result in missed cardiovascular or psychiatric medication scripts or delayed referral to psychologists or other specialists, and non-adherence or self-management of dietary, smoking, or physical activity recommendations.
Particularly in COVID, it should be mandatory to provide funding sources to provide telephone or remote counseling services to manage and prevent crisis situations[29]. As the global health community faces up to the spread of COVID-19, the ongoing epidemic wave of violence against women should be addressed.
Cardiovascular disease is the leading cause of death in women worldwide; for women living with cardiovascular problems, the chronicity of the disease translates into substantial disability. There are sex and gender-related disparities in cardiovascular disease (including delayed onset and atypical clinical characteristics in women, non-traditional gender-specific risk factors, unconscious gender biases, underrepresentation of women in research trials, and a lack of disease awareness in racial and ethnic minorities), and significant healthcare disparities and gaps still exist in the care of female patients. For example, women are less likely to receive an early diagnosis and timely interventions for a cardiovascular disease and often have worse outcomes than men after acute coronary syndromes). Recognizing nontraditional cardiovascular disease risk factors represents an important opportunity to improve healthcare quality in women[30]. Doing so would help guarantee a multidisciplinary team approach for patients who have experienced interpersonal violence to address physical, sexual, and emotional domains of abuse and their several sequelae. Because it has been stressed that there are multiple pathways through which an experience of violence can affect cardiovascular risk, the best approach to the patients seems to be a multimodal intervention focusing concurrently on chronic stress, depressive symptoms, and cardiovascular risk behaviors[31]. Screening for psychiatric and psychological symptoms in cardiological clinical practice might necessitate increased downstream support from mental health providers, including immediate evaluation of suspected suicidality, and clinicians should be aware that treatments that improve cardiovascular function should also benefit coexisting mood disorders[32].
A routine screening with standardized instruments and trained staffs in clinical settings should be recommended, including social services and behavioral health providers. Hospitals should develop violence intervention programs in collaboration with community-based services addressing mental health and other risk factors. Specific home visitation programs should help support children and families exposed to violence. Intervention strategies should focus on traditional gender role transformation to minimize the relationship power-gap and prevent violence against women. There should be strict implementation of the legislation to penalize and possibly rehabilitate the perpetrators, and there should be widespread diffusion of digital platforms for seeking help.
It is important to disseminate as widely as possible the knowledge and tools related to prevention and to improve the empowerment of women subjected to interpersonal violence[33].
Research has a pivotal role in understanding the impact of interpersonal violence on cardiovascular risk in women, with a special focus on the mechanisms underlying biological, psychological and psychosocial underpinnings. The investigation of potential epigenetic mechanisms by which violence exposure may contribute to heart disease by changing gene expression should not be overlooked, and other ways that the effects of violence exposure on the heart may be translated from generation to generation should be investigated[16]. Further studies designed to explore the chronicity and severity of violence exposure are needed to elucidate the relation between long-term effects of abuse and cardiovascular outcomes.
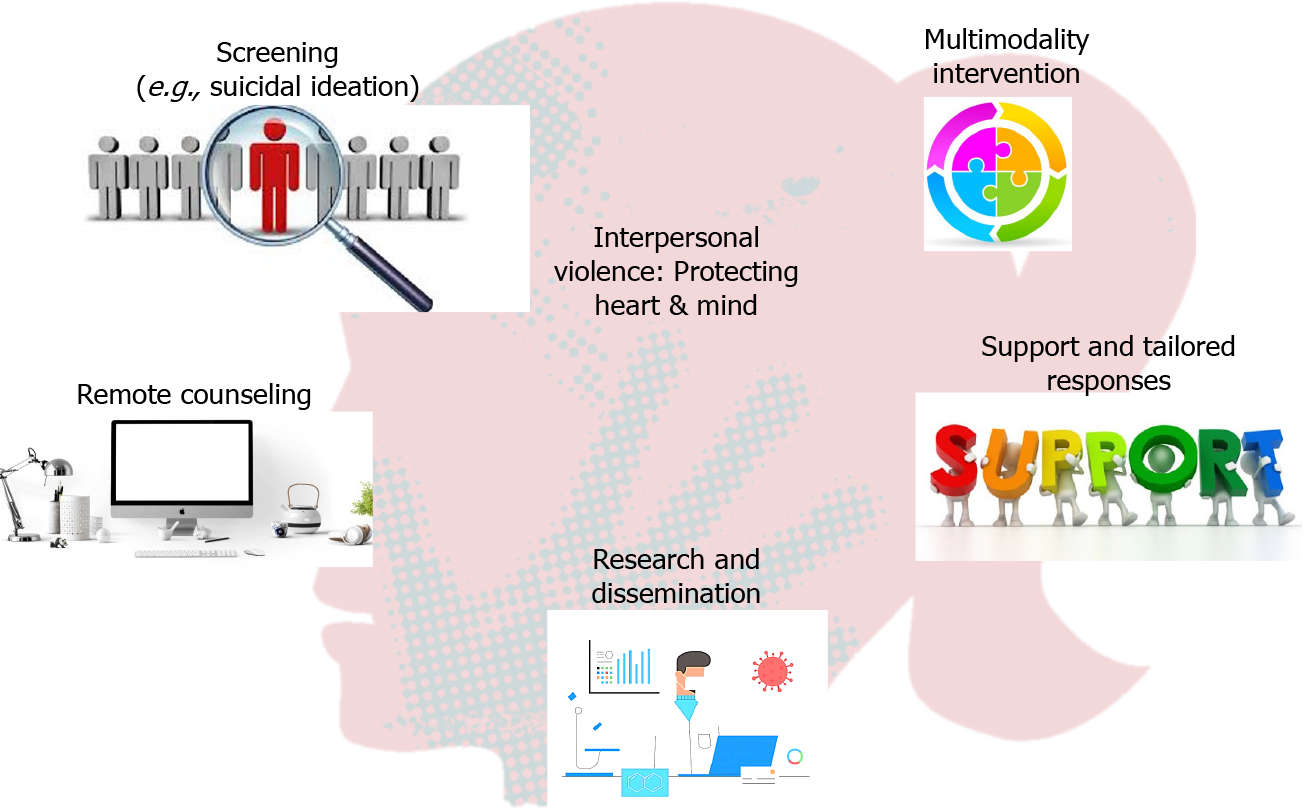
Intimate partner violence is a very complex issue, and is often difficult to identify because patients may present nonspecific sign and symptoms. Clinicians across all health care settings must be prepared to provide emotional and practical support, and to tailor personalized care to individual needs. Mental and physical health consequences related to interpersonal violence may persist long after the abusive situation has ended[34-36], and there is an urgent need to prevent long-term adverse effects and to extend periods of follow-up (Figure 1).
Prevention of violence against women of all ages, and interpersonal violence in general, is mandatory around the world. Cardiovascular disease and gender violence undoubtedly represent a key priority and a significant physical and mental health challenge facing women and clinicians today.
Manuscript source: Invited manuscript
Specialty type: Cardiac and cardiovascular systems
Country/Territory of origin: Italy
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): B
Grade C (Good): 0
Grade D (Fair): D
Grade E (Poor): 0
P-Reviewer: Li CY, Nashawi M S-Editor: Gao CC L-Editor: Filipodia P-Editor: Ma YJ
| 1. | Miller E, McCaw B. Intimate Partner Violence. N Engl J Med. 2019;380:850-857. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 130] [Cited by in RCA: 156] [Article Influence: 26.0] [Reference Citation Analysis (2)] |
| 2. | Breiding MJ, Black MC, Ryan GW. Chronic disease and health risk behaviors associated with intimate partner violence-18 U.S. states/territories, 2005. Ann Epidemiol. 2008;18:538-544. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 199] [Cited by in RCA: 195] [Article Influence: 11.5] [Reference Citation Analysis (0)] |
| 3. | Chandan JS, Thomas T, Bradbury-Jones C, Taylor J, Bandyopadhyay S, Nirantharakumar K. Risk of Cardiometabolic Disease and All-Cause Mortality in Female Survivors of Domestic Abuse. J Am Heart Assoc. 2020;9:e014580. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 49] [Cited by in RCA: 49] [Article Influence: 9.8] [Reference Citation Analysis (0)] |
| 4. | Stubbs A, Szoeke C. The Effect of Intimate Partner Violence on the Physical Health and Health-Related Behaviors of Women: A Systematic Review of the Literature. Trauma Violence Abuse. 2021;1524838020985541. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 159] [Article Influence: 53.0] [Reference Citation Analysis (0)] |
| 5. | Scott-Storey KA. Abuse as a gendered risk factor for cardiovascular disease: a conceptual model. J Cardiovasc Nurs. 2013;28:E1-E8. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 16] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 6. | Scott J, McMillian-Bohler J, Johnson R, Simmons LA. Adverse Childhood Experiences and Blood Pressure in Women in the United States: A Systematic Review. J Midwifery Womens Health. 2021;66:78-87. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 15] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 7. | D'Elia ATD, Juruena MF, Coimbra BM, Mello MF, Mello AF. Posttraumatic stress disorder (PTSD) and depression severity in sexually assaulted women: hypothalamic-pituitary-adrenal (HPA) axis alterations. BMC Psychiatry. 2021;21:174. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 21] [Cited by in RCA: 16] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 8. | Bacchus LJ, Ranganathan M, Watts C, Devries K. Recent intimate partner violence against women and health: a systematic review and meta-analysis of cohort studies. BMJ Open. 2018;8:e019995. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 162] [Cited by in RCA: 232] [Article Influence: 33.1] [Reference Citation Analysis (0)] |
| 9. | Schnabel RB, Hasenfuß G, Buchmann S, Kahl KG, Aeschbacher S, Osswald S, Angermann CE. Heart and brain interactions : Pathophysiology and management of cardio-psycho-neurological disorders. Herz. 2021;46:138-149. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 21] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 10. | Hare DL, Toukhsati SR, Johansson P, Jaarsma T. Depression and cardiovascular disease: a clinical review. Eur Heart J. 2014;35:1365-1372. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 599] [Cited by in RCA: 862] [Article Influence: 71.8] [Reference Citation Analysis (0)] |
| 11. | Thomas Q, Crespy V, Duloquin G, Ndiaye M, Sauvant M, Béjot Y, Giroud M. Stroke in women: When gender matters. Rev Neurol (Paris). 2021;. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 14] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 12. | Marano G, Harnic D, Lotrionte M, Biondi-Zoccai G, Abbate A, Romagnoli E, Mazza M. Depression and the cardiovascular system: increasing evidence of a link and therapeutic implications. Expert Rev Cardiovasc Ther. 2009;7:1123-1147. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 11] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 13. | Zambrano J, Celano CM, Januzzi JL, Massey CN, Chung WJ, Millstein RA, Huffman JC. Psychiatric and Psychological Interventions for Depression in Patients With Heart Disease: A Scoping Review. J Am Heart Assoc. 2020;9:e018686. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 56] [Cited by in RCA: 60] [Article Influence: 12.0] [Reference Citation Analysis (0)] |
| 14. | Manfrini O, Cenko E, Bugiardini R. Gender Differences in Residual Risk Factors for Major Adverse Cardiovascular Events Following ACS and How to Bridge the Gap. Curr Atheroscler Rep. 2020;22:65. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 15. | Yang HJ, Koh E, Kang Y. Susceptibility of Women to Cardiovascular Disease and the Prevention Potential of Mind-Body Intervention by Changes in Neural Circuits and Cardiovascular Physiology. Biomolecules. 2021;11. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 14] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 16. | Suglia SF, Sapra KJ, Koenen KC. Violence and cardiovascular health: a systematic review. Am J Prev Med. 2015;48:205-212. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 68] [Cited by in RCA: 79] [Article Influence: 7.9] [Reference Citation Analysis (0)] |
| 17. | Kuehn BM. Getting to the Heart of Sex Differences: Growing Evidence Suggests Women's Heart Disease Is Physiologically Distinct. Circulation. 2020;141:1198-1199. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 18. | Edmondson D, von Känel R. Post-traumatic stress disorder and cardiovascular disease. Lancet Psychiatry. 2017;4:320-329. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 181] [Cited by in RCA: 220] [Article Influence: 27.5] [Reference Citation Analysis (0)] |
| 19. | Jamison LE, Howell KH, Decker KM, Schwartz LE, Thurston IB. Associations between Substance Use and Depressive Symptoms among Women Experiencing Intimate Partner Violence. J Trauma Dissociation. 2021;1-15. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 3] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 20. | Weiss NH, Schick MR, Contractor AA, Reyes ME, Suazo NC, Sullivan TP. Racial/Ethnic Differences in Alcohol and Drug Misuse Among IPV-Victimized Women: Exploring the Role of Difficulties Regulating Positive Emotions. J Interpers Violence. 2020;886260520943735. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 7] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 21. | Frazier T, Yount KM. Intimate partner violence screening and the comparative effects of screening mode on disclosure of sensitive health behaviours and exposures in clinical settings. Public Health. 2017;143:52-59. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 7] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 22. | Castaldelli-Maia JM, Marziali ME, Lu Z, Martins SS. Investigating the effect of national government physical distancing measures on depression and anxiety during the COVID-19 pandemic through meta-analysis and meta-regression. Psychol Med. 2021;51:881-893. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 89] [Cited by in RCA: 77] [Article Influence: 19.3] [Reference Citation Analysis (0)] |
| 23. | Morina N, Kip A, Hoppen TH, Priebe S, Meyer T. Potential impact of physical distancing on physical and mental health: a rapid narrative umbrella review of meta-analyses on the link between social connection and health. BMJ Open. 2021;11:e042335. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 66] [Cited by in RCA: 53] [Article Influence: 13.3] [Reference Citation Analysis (0)] |
| 24. | Varghese T, Hayek SS, Shekiladze N, Schultz WM, Wenger NK. Psychosocial Risk Factors Related to Ischemic Heart Disease in Women. Curr Pharm Des. 2016;22:3853-3870. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 25. | Gulati G, Kelly BD. Domestic violence against women and the COVID-19 pandemic: What is the role of psychiatry? Int J Law Psychiatry. 2020;71:101594. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 93] [Cited by in RCA: 60] [Article Influence: 12.0] [Reference Citation Analysis (0)] |
| 26. | Mazza M, Marano G, Antonazzo B, Cavarretta E, DI Nicola M, Janiri L, Sani G, Frati G, Romagnoli E. What about heart and mind in the COVID-19 era? Minerva Cardiol Angiol. 2021;69:222-226. [PubMed] |
| 27. | Wosik J, Clowse MEB, Overton R, Adagarla B, Economou-Zavlanos N, Cavalier J, Henao R, Piccini JP, Thomas L, Pencina MJ, Pagidipati NJ. Impact of the COVID-19 pandemic on patterns of outpatient cardiovascular care. Am Heart J. 2021;231:1-5. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 47] [Cited by in RCA: 66] [Article Influence: 16.5] [Reference Citation Analysis (0)] |
| 28. | O'Neil A, Nicholls SJ, Redfern J, Brown A, Hare DL. Mental Health and Psychosocial Challenges in the COVID-19 Pandemic: Food for Thought for Cardiovascular Health Care Professionals. Heart Lung Circ. 2020;29:960-963. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 15] [Cited by in RCA: 12] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 29. | Wang J, Wei H, Zhou L. Hotline services in China during COVID-19 pandemic. J Affect Disord. 2020;275:125-126. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 24] [Cited by in RCA: 29] [Article Influence: 5.8] [Reference Citation Analysis (0)] |
| 30. | El-Serag R, Thurston RC. Matters of the Heart and Mind: Interpersonal Violence and Cardiovascular Disease in Women. J Am Heart Assoc. 2020;9:e015479. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 18] [Cited by in RCA: 33] [Article Influence: 6.6] [Reference Citation Analysis (0)] |
| 31. | Scott-Storey KA, Hodgins M, Wuest J. Modeling lifetime abuse and cardiovascular disease risk among women. BMC Cardiovasc Disord. 2019;19:224. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 8] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 32. | Nielsen RE, Banner J, Jensen SE. Cardiovascular disease in patients with severe mental illness. Nat Rev Cardiol. 2021;18:136-145. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 61] [Cited by in RCA: 218] [Article Influence: 43.6] [Reference Citation Analysis (0)] |
| 33. | El Morr C, Layal M. Effectiveness of ICT-based intimate partner violence interventions: a systematic review. BMC Public Health. 2020;20:1372. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 19] [Cited by in RCA: 38] [Article Influence: 7.6] [Reference Citation Analysis (0)] |
| 34. | MacMillan HL, Kimber M, Stewart DE. Intimate Partner Violence: Recognizing and Responding Safely. JAMA. 2020;324:1201-1202. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 10] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 35. | Lucas S, Heimer G. To prevent sexual violence against women, we need to know more about those who become victims. Scand J Public Health. 2021;49:251-253. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 36. | Sharma V, Ausubel E, Heckman C, Patrick E, Save D, Kelly JTD. Mitigating gender-based violence risk in the context of COVID-19: lessons from humanitarian crises. BMJ Glob Health. 2021;6. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 7] [Article Influence: 1.8] [Reference Citation Analysis (0)] |