Published online Aug 27, 2025. doi: 10.4240/wjgs.v17.i8.108656
Revised: May 26, 2025
Accepted: July 1, 2025
Published online: August 27, 2025
Processing time: 128 Days and 3.5 Hours
Inferior mesenteric arteriovenous fistula (IMAVF) is an extremely rare condition characterized by abnormal communication between the inferior mesenteric artery and vein. IMAVF often mimics ischemic bowel disease and ulcerative colitis (UC), leading to diagnostic challenges and treatment failures.
Three consecutive cases presented with non-specific symptoms including perianal pain and bloody diarrhea were reported. Initial diagnosis included acute severe UC and ischemic colitis. Pathology suggested ischemic changes, and with further contrast-enhanced computed tomography together with digital subtraction an
We presented the largest single center IMAVF series with detailed clinical characteristics, facilitating early diagnosis for similar cases in the future.
Core Tip: Inferior mesenteric arteriovenous fistula (IMAVF) is a rare condition characterized by abnormal communication between the inferior mesenteric artery and vein. Presentations of IMAVF are usually non-specific and therefore poses diagnostic challenge and delay. We reported three consecutive cases of IMAVF that mimics ulcerative colitis and ischemic bowel disease, and provided a brief literature review, aiming to facilitate rapid recognition and timely treatment in clinical practice.
- Citation: Mei SB, Liu J, Wang Y, Hu P, Cao Q. Inferior mesenteric arteriovenous fistula: Three case reports. World J Gastrointest Surg 2025; 17(8): 108656
- URL: https://www.wjgnet.com/1948-9366/full/v17/i8/108656.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v17.i8.108656
Inferior mesenteric arteriovenous fistula (IMAVF) is a rare condition involving abnormal communication between the inferior mesenteric artery and vein. It’s a rare clinical condition with limited case report[1]. IMAVF may result in various non-specific clinical manifestations, including abdominal pain, diarrhea, abdominal mass, ischemic bowel disease, portal hypertension, and even heart failure[2]. When presenting with abdominal pain, diarrhea, and bloody stool, IMAVF is frequently misdiagnosed as ischemic bowel disease or inflammatory bowel disease (IBD), such as ulcerative colitis (UC). We reported three consecutive cases of IMAVF, constituting the largest single-center case series to date. A literature review was also conducted to summarize the clinical characteristics, diagnostic approaches, and treatment strategies for this rare condition.
Case 1: A 48-year-old male was referred to our hospital in March 2024 due to persistent severe pain in the perianal region and lower abdomen, accompanied by mucopurulent bloody stool for one month.
Case 2: A 72-year-old male was referred to our hospital in April 2024 with recurrent abdominal pain and diarrhea for three months.
Case 3: A 40-year-old male was referred to our hospital in June 2024 due to severe perianal pain and diarrhea lasting for five days.
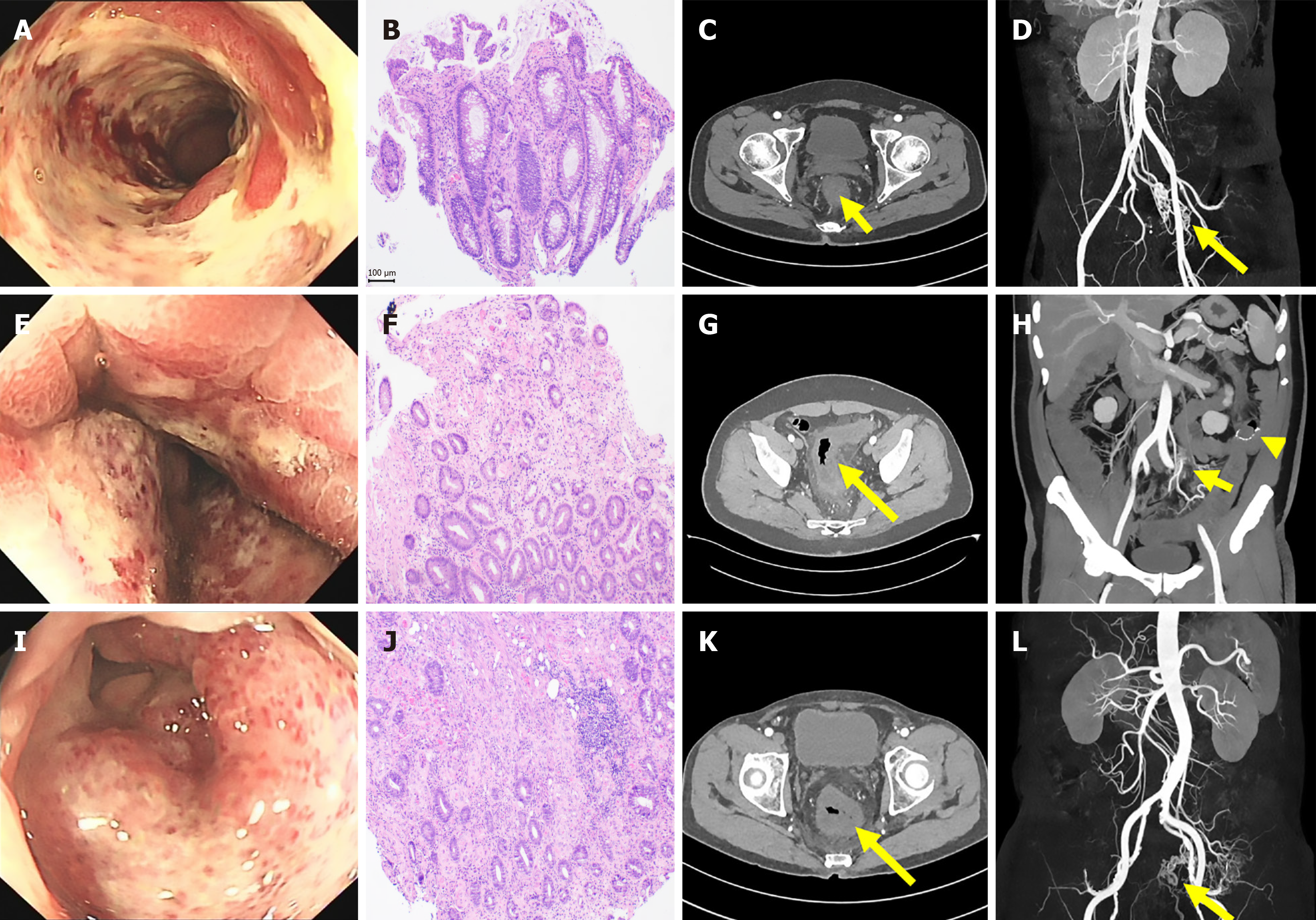
Case 1: He developed recurrent abdominal pain and diarrhea for three months. Colonoscopy performed at a local hospital revealed diffuse rectal erosion with ulceration, leading to a suspected diagnosis of acute severe UC. Based on this diagnosis, the patient was treated with steroids and subsequently with infliximab, both of which were ineffective. He continued to experience severe pain requiring multiple analgesics, and the bloody diarrhea persisted. Due to the lack of treatment response, a second colonoscopy was performed, revealing diffuse ulcers extending from the rectum to 15 cm proximal to the sigmoid colon (Figure 1A). Histopathology indicated ischemic changes and vascular lesions (Figure 1B).
Case 2: He had a maximum of over ten times diarrhea per day and suffered from persistent dull pain at the left lower quadrant. Colonoscopy showed diffuse swelling of the rectosigmoid mucosa, more pronounced toward the anal side (Figure 1E). Histopathology indicated ischemic changes of the colonic mucosa (Figure 2F).
Case 3: He presented with persistent and severe perianal pain, which responded poorly to non-steroidal anti-inflammatory drugs and antispasmodic medications. Colonoscopy showed diffuse hyperemia of the mucosa distal to the anastomosis (Figure 1I), and histopathology suggested acute ischemic changes (Figure 2J).
Case 1: The patient had a history of appendectomy 30 years ago.
Case 2: The patient had no prior history of abdominal surgery or trauma.
Case 3: Six months ago, he was diagnosed with descending colon cancer and underwent laparoscopic left hemicolectomy, with preservation of the rectum and sigmoid colon, together with mesenteric lymph node dissection and pelvic adhesion lysis.
No significant findings for all three cases.
Case 1: Physical examination revealed tenderness in the mid-lower and left lower abdomen.
Case 2 and case 3: Physical examination revealed tenderness in the left lower abdomen.
Case 1: Laboratory tests showed a white blood cell (WBC) count of 19.7 × 109/L and a high-sensitivity C-reactive protein level of 21.4 mg/L. Stool test for occult blood and WBC were all negative. Other laboratory findings were unremarkable.
Case 2: Stool test for occult blood was positive.
Case 3: Stool test for occult blood as well as WBC were all positive.
Case 1: Contrast-enhanced computed tomography (CT) of the abdomen showed a thickened rectal wall surrounded by tortuous and dilated small vessels (Figure 1C). These findings excluded IBD and raised suspicion of a vascular etiology. CT angiography (CTA) reconstruction confirmed the presence of IMAVF (Figure 1D).
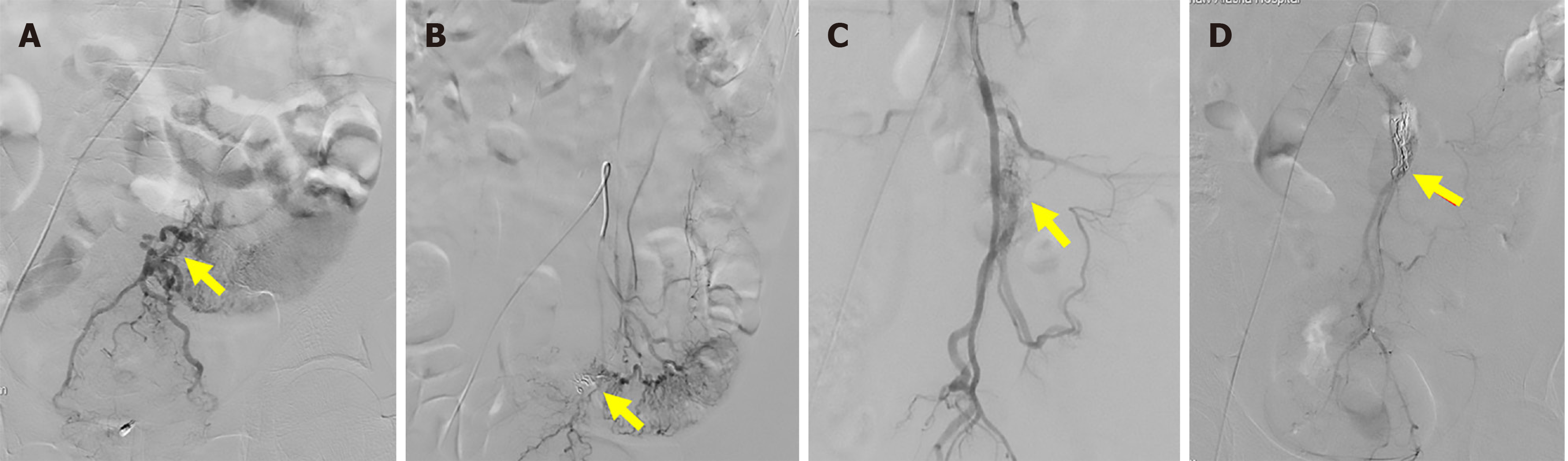
Case 2: Abdominal CTA revealed cavernous transformation of the portal vein, narrowing of the splenic and superior mesenteric veins, multiple small varices around the stomach and mesentery, and edema with thickening of the rectosigmoid wall accompanied by exudation (Figure 1G and H). Digital subtraction angiography (DSA) demonstrated increased and disorganized vascular branches of the sigmoid colon with extensive varices, confirming the diagnosis of IMAVF (Figure 3A and B).
Case 3: Abdominal CTA revealed swelling of the colonic wall distal to the anastomosis, surrounded by blurry exudates, and identified an IMAVF (Figure 1K and L). DSA further confirmed the diagnosis by demonstrating increased and disorganized vascular branches of the sigmoid colon with multiple varices.
Idiopathic IMAVF.
IMAVF with secondary portal hypertension.
IMAVF secondary to left hemicolectomy.
The patient underwent vascular embolization at another hospital (imaging not retrieved), resulting in rapid improvement of both pain and bloody diarrhea.
The patient underwent vascular embolization, resulting in symptom improvement.
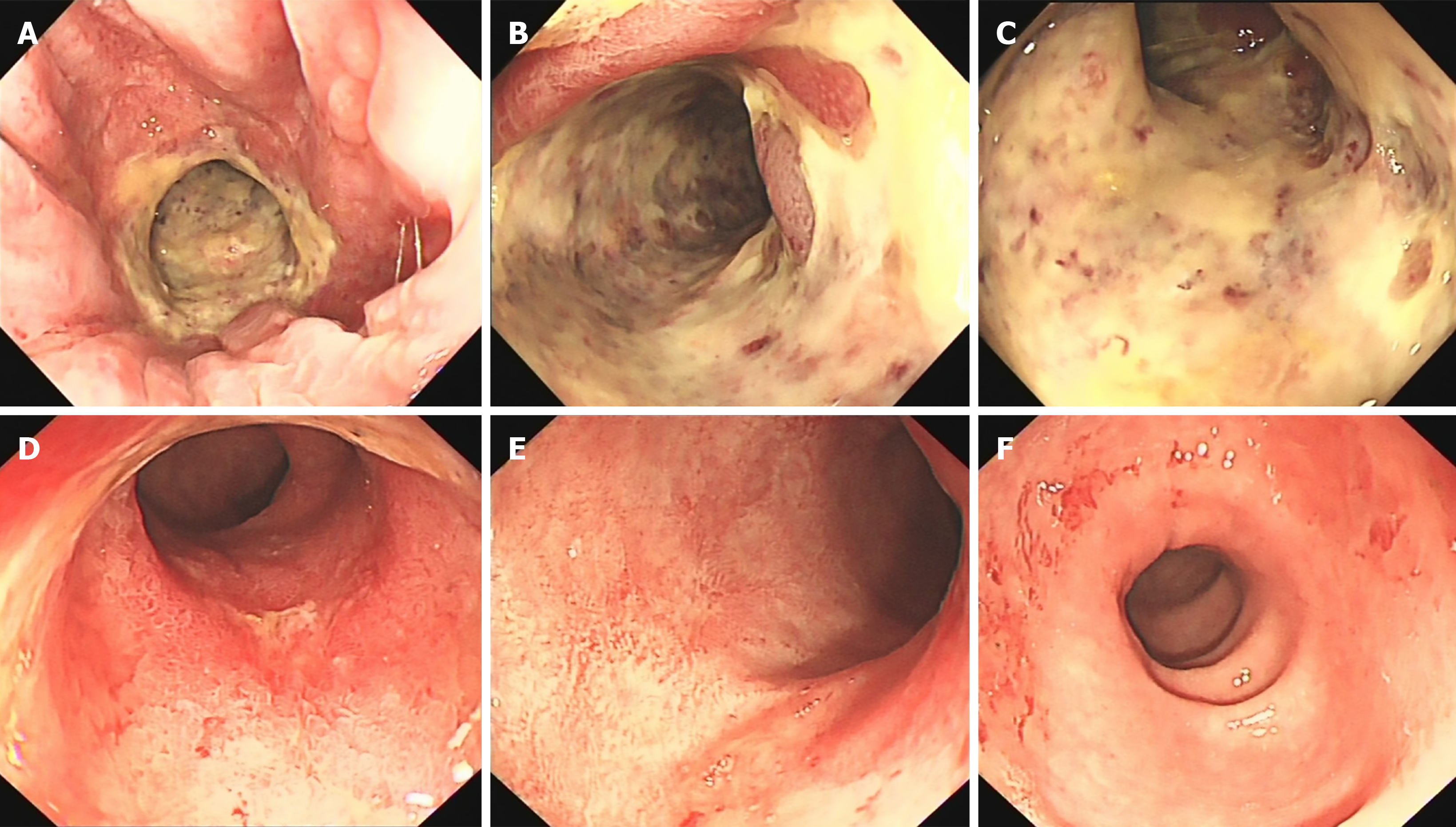
Follow-up colonoscopy for this patient one month later showed significant ulcer healing (Figure 2).
Follow-up colonoscopy three months later showed resolution of mucosal ischemia, and abdominal CT indicated remission of colonic edema.
Follow-up abdominal CT two months later showed marked improvement in colonic wall edema and exudation.
IMAVF[3] is an extremely rare condition, with no more than fifty cases from previous literature[4-8]. IMAVF that can be classified as congenital, secondary, or idiopathic when no apparent cause is identified. Congenital arteriovenous malformations arise from undifferentiated embryonic vessels that fail to differentiate into arteries and veins, resulting in abnormal vascular connections. Secondary IMAVF typically results from trauma, such as blunt or penetrating abdominal injury, or from iatrogenic causes, including arterial catheterization, cholangiography, splenoportography, or surgical procedures such as left colectomy or sigmoidectomy[1]. Previous reports have also implicated specific drugs, such as bevacizumab, in the development of IMAVF[9]. We summarized all cases of IMAVF from the previous literature and summarized the epidemiological characteristics of the disease[3] as follows: (1) The age of onset ranged from 22 years to 81 years, with a mean age of 56 years and a median age of 61 years; (2) The male-to-female ratio is approximately 3.7:1; and (3) Secondary IMAVF accounts for about 38% of reported cases[4-8].
The pathophysiological features of IMAVF are generally associated with reduced perfusion to the affected tissues and increased venous pressure distal to the fistula. In the current case report, the first and second cases were considered idiopathic, while the third was attributed to iatrogenic causes following abdominal surgery. The steal phenomenon among intestinal arteries caused by the fistula leads to ischemic mucosal necrosis, while diversion of arterial blood from the inferior mesenteric artery into the portal circulation may result in portal hypertension, manifesting as variceal bleeding, ascites, and splenomegaly. Increased portal blood flow can induce a compensatory rise in hepatic vascular resistance[10]. Approximately 50% of patients with visceral arteriovenous fistulas develop portal hypertension. Fabre et al[11] reported that increased venous return may also contribute to heart failure in some cases, and that embolization of the fistula can improve cardiac function and increase ejection fraction. IMAVF can present with various nonspecific clinical manifestations, including abdominal pain, diarrhea, abdominal mass, portal hypertension, and even heart failure[2]. When presenting with abdominal pain, diarrhea, and hematochezia, IMAVF can be misdiagnosed as ischemic bowel disease or UC.
All three patients in our series presented with clinical manifestations of mucosal ischemic necrosis, with the second case additionally complicated by portal hypertension. IMAVF-related bowel disease is particularly challenging to distinguish from ischemic bowel disease and UC, often resulting in misdiagnosis and delayed treatment. The key characteristics derived from our cases are summarized as follows. First, the disease typically has a short course, with either acute or subacute onset. Second, pain is a prominent feature, especially severe pain located at the perianal area, as well as dull pain at lower abdomen, which often required multiple analgesics with limited relief. Third, abdominal trauma and surgery consists high risk factors for secondary IMAVF, such as the case of the third IMAVF in the current report. Forth, endoscopic findings closely mimic those of ischemic bowel disease and UC. Notably, IMAVF often involves the rectum, which may aid in distinguishing it from ischemic bowel disease, while pathological findings of ischemic changes can help differentiate it from UC. Fifth, radiological findings may be subtle and easily overlooked on initial review. Characteristic imaging features include early enhancement of the inferior mesenteric vein and its branches during the arterial phase of CTA, accompanied by dilated, disorganized local vasculature.
Treatment options for IMAVF include surgery, arterial embolization, and medical therapy. According to our review of the existing literature[3-7], approximately 20 (43%) patients underwent surgical treatment, 19 (40%) patients received embolization therapy, 5 (11%) patients were treated with a combination approach, and 3 (6%) patients were managed conservatively[8].
Arterial embolization is minimally invasive and repeatable, but may result in extensive thrombosis, ischemic necrosis, or incomplete embolization[9]. It is not recommended for fistulas larger than 8–9 mm due to the risk of ectopic embolism[12]. Five cases of post-embolization complications have been reported, including incomplete embolization and bowel necrosis or perforation, which required surgical resection. Surgical resection of the fistula and affected bowel segment remains a viable option, depending on the extent and severity of ischemia[13]. A total of 20 surgically treated cases have been documented. Medical management is appropriate only for asymptomatic patients with mild ischemic changes and no portal hypertension. In one report, a patient managed conservatively showed gradual improvement over one month, with abdominal CTA revealing collateral vein formation, reduced venous congestion, and resolution of left colonic wall edema, which was confirmed by colonoscopy[1]. All three patients in our series were treated with embolization, resulting in significant symptom improvement without recurrence or complications during follow-up. Although the three cases provided by our center currently represent the largest single-center series reported in the literature, the sample size remains too small to fully represent all the clinical manifestations and treatment outcomes of IMAVF. The generalizability of the conclusions drawn in this study regarding the disease characteristics of IMAVF is limited. More cases are needed in the future to validate the clinical, endoscopic, imaging, and pathological features, as well as the treatment efficacy of IMAVF primarily presenting with lower gastrointestinal symptoms.
We reported three consecutive cases of IMAVF presenting with abdominal pain, diarrhea, and bloody stools, constituting the largest single-center case series to date. We further summarized the key clinical, endoscopic, pathological, and radiological features of IMAVF and outlined important considerations for differentiating IMAVF from other conditions such as ischemic bowel disease and UC. These insights may facilitate earlier recognition and timely intervention in future clinical practice.
| 1. | Cubisino A, Schembri V, Guiu B. Inferior mesenteric arteriovenous fistula with colonic ischemia: a case report and review of the literature. Clin J Gastroenterol. 2021;14:1131-1135. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 7] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 2. | Das Gupta J, Rana MA, Delu A, Guliani S, Langsfeld M, Marek J. Spontaneous inferior mesenteric arteriovenous fistula as a cause of severe portal hypertension and cardiomyopathy. J Vasc Surg Cases Innov Tech. 2019;5:113-116. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 9] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 3. | Munechika T, Shiokawa K, Takeshita I, Shimokobe H, Sahara K, Matsumoto Y, Aisu N, Yoshimatsu G, Hasegawa S. Laparoscopic sigmoid colectomy for transverse colonic varices due to an inferior mesenteric arteriovenous fistula. Surg Case Rep. 2024;10:112. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 4. | Borkowski A, Młodzik J, Jodłowski G, Madurska M, Malinowski M, Skóra J, Janczak D. Type II endoleak accompanied by an arteriovenous fistula between the inferior mesenteric artery and the inferior vena cava as a complication of endovascular aneurysm repair. Proc (Bayl Univ Med Cent). 2023;36:103-105. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 5. | Pedersen V, Ohrlander T, Frevert S, Malina M. Giant Inferior Mesenteric Vein Aneurysm Secondary to Iatrogenic Inferior Mesenteric Arteriovenous Fistula. J Endovasc Ther. 2024;31:491-494. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 6. | Su BY, Wang YC, Weng MJ, Chen MC. Trans-arterial embolization of a Yakes type IIb inferior mesenteric arteriovenous malformation: A case report and literature review for angio-architecture analysis. Radiol Case Rep. 2023;18:1620-1627. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 7. | Xiao H, Song Q, Wang YT, Dong D. [Massive ascites and gastrointestinal bleeding caused by idiopathic inferior mesenteric arteriovenous fistula: a case report]. Zhonghua Nei Ke Za Zhi. 2023;62:852-854. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 8. | Saito N, Inoue M, Ishida K, Taguchi H, Haga M, Shimoda E, Morimoto K, Takahama J, Tanaka T. A Case of Refractory Esophageal Varices Caused by an Inferior Mesenteric Arteriovenous Malformation with All Portal System Occlusion Successfully Treated via Transarterial Embolization. Interv Radiol (Higashimatsuyama). 2023;8:83-87. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 9. | Doi A, Takeda H, Umemoto K, Oumi R, Wada S, Hamaguchi S, Mimura H, Arai H, Horie Y, Mizukami T, Izawa N, Ogura T, Nakajima TE, Sunakawa Y. Inferior mesenteric arteriovenous fistula during treatment with bevacizumab in colorectal cancer patient: A case report. World J Gastrointest Oncol. 2020;12:1364-1371. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 3] [Cited by in RCA: 3] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 10. | Capron JP, Gineston JL, Remond A, Lallement PY, Delamarre J, Revert R, Veyssier P. Inferior mesenteric arteriovenous fistula associated with portal hypertension and acute ischemic colitis. Successful occlusion by intraarterial embolization with steel coils. Gastroenterology. 1984;86:351-355. [PubMed] |
| 11. | Fabre A, Abita T, Lachachi F, Rudelli P, Carlier M, Bocquel JB, Remond A, Pech de Laclause B, Maisonnette F, Durand-Fontanier S, Valleix D, Descottes B, Reix T. [Inferior mesenteric arteriovenous fistulas. Report of a case]. Ann Chir. 2005;130:417-420. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 10] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 12. | Faghihi Langroudi T, Shabestari AA, Pourghorban R, Pourghorban R. Idiopathic inferior mesenteric arteriovenous fistula: a rare cause of pulsatile abdominal mass. Indian J Surg. 2015;77:84-86. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 6] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 13. | Athanasiou A, Michalinos A, Alexandrou A, Georgopoulos S, Felekouras E. Inferior mesenteric arteriovenous fistula: case report and world-literature review. World J Gastroenterol. 2014;20:8298-8303. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 27] [Cited by in RCA: 34] [Article Influence: 3.1] [Reference Citation Analysis (0)] |