Published online Oct 16, 2016. doi: 10.4253/wjge.v8.i18.669
Peer-review started: May 16, 2016
First decision: July 4, 2016
Revised: July 11, 2016
Accepted: July 29, 2016
Article in press: August 1, 2016
Published online: October 16, 2016
Processing time: 153 Days and 12.8 Hours
Per oral endoscopic myotomy (POEM) is a novel endoscopic procedure for achalasia treatment. Due to its novelty and high success rates, a repeat procedure is usually not warranted, making the feasibility and safety of such approach unknown. We report the first case of a successful repeat POEM done at the same site of a previously uncompleted POEM. An 84-year-old female with type 2 achalasia presented for a POEM procedure. The procedure was aborted at the end of tunneling and before myotomy due to hypotension, which later resolved spontaneously. POEM was re-attempted at the same site of the original tunnel 1 year afterward, and surprisingly we didn’t encounter any submucosal fibrosis. The procedure felt similar to a native POEM and a myotomy was performed uneventfully. Our case is the first to suggest that submucosal tunneling during a repeat POEM can be done at the same site. Hypotension during POEM is a rare complication that should be recognized as a potential result of tension capnothorax, it can however, be managed with close supportive care.
Core tip: Per oral endoscopic myotomy (POEM) is a novel method of treating achalasia. More is being learnt about potential complications as it increases in popularity. This is the first case of a repeat submucosal tunneling done at the same site of a prior POEM attempt which was aborted just before myotomy. No complications or difficulties were encountered during the second attempt. This may suggest that submucosal tunneling does not cause fibrosis, and that repeat POEM after a technically unsuccessful attempt could be done at the same site and orientation of the original tunnel.
- Citation: Wehbeh AN, Mekaroonkamol P, Cai Q. Same site submucosal tunneling for a repeat per oral endoscopic myotomy: A safe and feasible option. World J Gastrointest Endosc 2016; 8(18): 669-673
- URL: https://www.wjgnet.com/1948-5190/full/v8/i18/669.htm
- DOI: https://dx.doi.org/10.4253/wjge.v8.i18.669
Per oral endoscopic myotomy (POEM) is a novel endoscopic procedure for achalasia treatment. The principle techniques involve endoscopic submucosal tunneling followed by a myotomy[1]. Overall, it has success rates reportedly ranging between 82% to 100% and can be safely performed with a small number of reported major complications[1-3]. However, one of the complications that can occur is hemodynamic instability, which has been reported in up to 20% of patients in one study[4]. Due to its novelty and the high success rates, repeat procedure is rarely warranted, making the feasibility and safety of such approach unknown. Here, we report the first case of a repeat submucosal tunneling successfully performed at the same site of a previous POEM procedure.
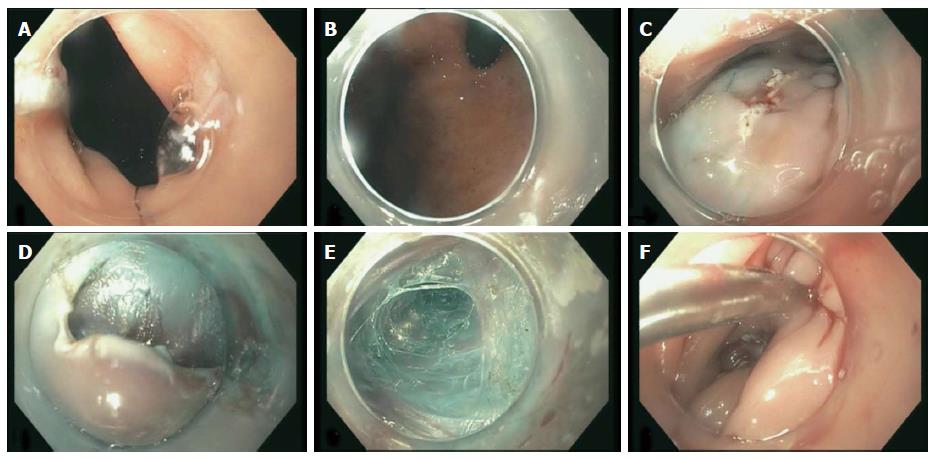
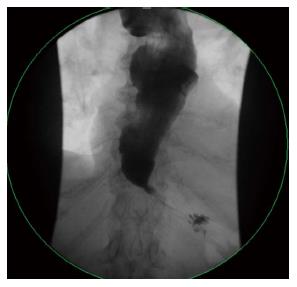
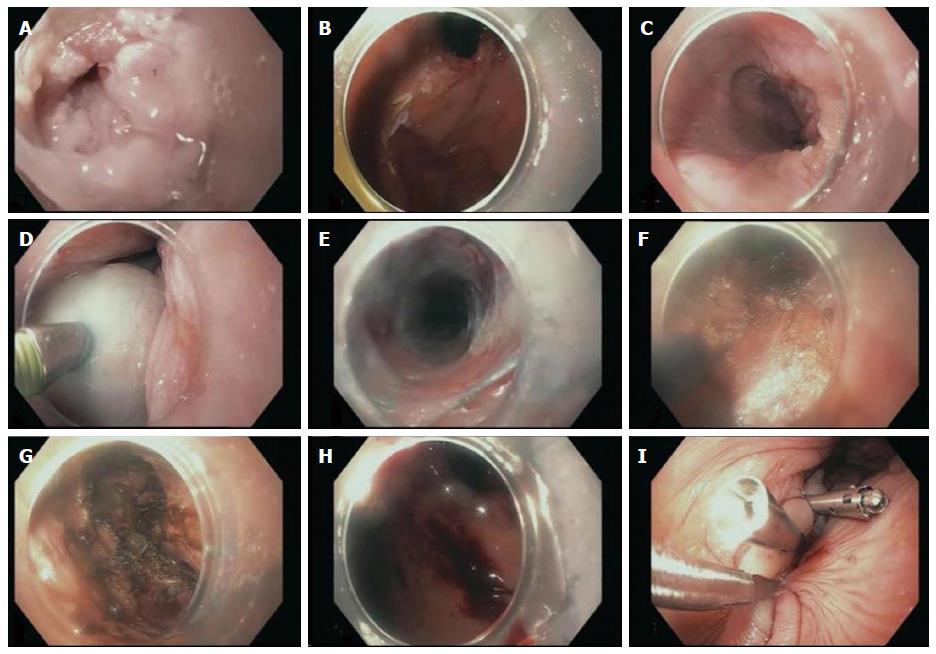
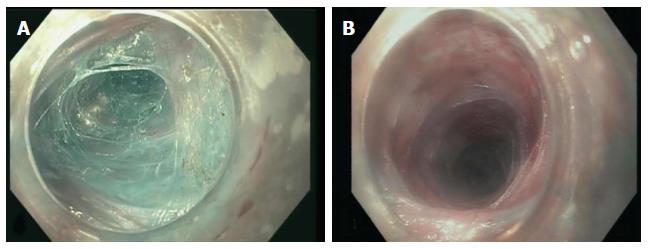
An 84-year-old female presented with progressive dysphagia to both solids and liquids and failure to thrive over several months. Her other medical problems included gastroesophageal reflux disease, hypertension, deep vein thrombosis, severe osteoarthritis of both hips, lower extremities contracture, and chronic low back pain. Initial laboratory work up was essentially unrevealing. Manometry study confirmed severe achalasia type 2. The decision was made to proceed with POEM procedure. During endoscopy, she was placed in supine position which was standard practice at our institution. Incision site was first injected with a premixed solution of saline and methylene blue (5 mL/500 mL) followed by careful dissection to the submucosal layer using a triangle-tip knife. A submucosal tunnel was being made from the incision site to 2 cm distal to the cardia, but after a complete submucosal tunneling process just before myotomy (Figure 1), she developed severe hypotension and bradycardia. Consequently, the procedure was aborted. Chest X-ray revealed left apical pneumothorax, pneumomediastinum, pneumoperitoneum, and extensive subcutaneous emphysema. Her hypotension resolved with supportive care within minutes of aborting the procedure. A gastrografin swallow study was obtained which did not show any evidence of contrast leakage, but it demonstrated a grossly dilated esophagus consistent with achalasia, and postoperative edema with slow emptying at the gastroesophageal junction (Figure 2). Thereafter, she underwent an upper endoscopy with Botulinum injection every 2-3 mo but eventually her symptoms stopped responding to botulinum treatment. Repeat POEM was thus performed 1 year later. She was placed in the same supine position due to her medical comorbidities. A severely dilated sigmoid esophagus was observed (Figure 3A). The GE junction was tight, and some pressure was required to traverse the endoscope, consistent with known achalasia. Due to great difficulty orienting the endoscope on a different plane, submucosal incision was made at the exact same site (Figure 3C) of the original tunnel, and surprisingly we did not encounter any submucosal fibrosis or technical challenges. The repeat tunneling at the same submucosal plane was successfully completed and felt similar to a native POEM (Figure 4). A myotomy was quickly and uneventfully performed followed by mucosal closure with hemostatic clips (Figure 3). The length of the myotomy was 8 cm, which is the standard at our institution. At 4-wk follow up her symptoms remarkably improved, as shown by a decreased Eckhardt score from 9 to 4. Her reflux symptoms also remained stable on the same dose of omeprazole.
Our case is the first to highlight the feasibility and safety of performing a repeat POEM at a location where submucosal tunneling was previously performed. As discussed above, there are limited scenarios where repeat POEM would be considered. They include intraprocedural complications resulting in incomplete procedure, insufficient symptomatic relieve, and recurrent symptoms after an initial improvement[5]. The question remains as whether it is feasible to repeat a POEM procedure, and if so what would the best approach be.
POEM on a site of prior endoscopic mucosal resection is considered relatively contraindicated due to fear of encountering fibrosis[2]. Recent report on repeat POEM procedures opted to create submucosal tunnel at the opposite side of the scarred mucosectomy area due to concern for an obliterated submucosal space[5]. However, this did not apply to our case, meaning that submucosal fibrosis does not necessarily result from a first POEM attempt. Although theoretically myotomy may lead to fibrosis, but this hasn’t been confirmed in the literature. In addition, myotomy is performed from 3 cm proximal to gastroesophageal junction and is therefore unlikely to impact the development of submucosal fibrosis in the proximal tunnel.
Moreover, the opposite site approach may not always be feasible due to different patient position and endoscopic orientation as in our case where patient position is very limited. Therefore, we opted for the same posterior approach as it allowed most flexible endoscopic maneuverability. Same site repeat POEM also preserves the opposite side of the esophagus for other potential procedures. Similar to our findings, double POEM was recently reported whereby tunneling was done more proximal to original tunnel to extend the myotomy[6].
Hypotension during POEM is a rare complication that should be recognized as a potential sign of tension capnothorax; it can however, be managed with close supportive care[7,8]. Other commonly reported physical findings include subcutaneous emphysema, mediastinal emphysema, and pneumoperitoneum without hemodynamic instability, all of which are believed to be normal physiologic reaction to the procedure[9].
In summary, this report suggests that should POEM need to be re-attempted, same site operation, including incision, submucosal tunneling and myotomy, is a viable method.
An 84-year-old female with progressive dysphagia to both solids and liquids and failure to thrive.
She had severely dilated sigmoid esophagus and tight gastroesophageal junction upon passing gastroscope, consistent with manometry-proven achalasia type 2.
Differential includes esophageal cancer causing pseudoachalasia, stricture, extrinsic compressive mass, and esophagogastric junction outflow obstruction.
Laboratory testing on initial presentation was essentially unremarkable.
No imaging was required to make the diagnosis. Manometry study revealed panesophageal pressurization and elevated integrated resting pressure, diagnostic of achalasia type 2.
Biopsy was not required to establish the diagnosis.
Per oral endoscopic myotomy (POEM) was performed twice: the first submucosal tunneling was completed without myotomy due to hemodynamic instability. The second attempt was successfully performed via the same site tunneling.
Only 2 other reports on repeat POEM were found, but neither of them reports on performing repeat submucosal tunneling on the same site and orientation of the original tunnel.
POEM has been demonstrated to be safe and effective for treating achalasia, regardless of the previous treatment history, including previous POEM therapy. Generally, the opposite site approach was recommended to avoid the potential fibrosis. In the present case, POEM was performed at exactly the same site of a previous POEM procedure.
Manuscript source: Invited manuscript
Specialty Type: Gastroenterology and hepatology
Country of Origin: United States
Peer-Review Report Classification
Grade A (Excellent): 0
Grade B (Very good): 0
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P- Reviewer: Liu DL S- Editor: Gong ZM L- Editor: A E- Editor: Wu HL
| 1. | Bechara R, Ikeda H, Inoue H. Peroral endoscopic myotomy: an evolving treatment for achalasia. Nat Rev Gastroenterol Hepatol. 2015;12:410-426. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 57] [Cited by in RCA: 60] [Article Influence: 6.0] [Reference Citation Analysis (1)] |
| 2. | Stavropoulos SN, Modayil RJ, Friedel D, Savides T. The International Per Oral Endoscopic Myotomy Survey (IPOEMS): a snapshot of the global POEM experience. Surg Endosc. 2013;27:3322-3338. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 190] [Cited by in RCA: 202] [Article Influence: 16.8] [Reference Citation Analysis (0)] |
| 3. | Talukdar R, Inoue H, Nageshwar Reddy D. Efficacy of peroral endoscopic myotomy (POEM) in the treatment of achalasia: a systematic review and meta-analysis. Surg Endosc. 2015;29:3030-3046. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 141] [Cited by in RCA: 115] [Article Influence: 11.5] [Reference Citation Analysis (0)] |
| 4. | Kurian AA, Dunst CM, Sharata A, Bhayani NH, Reavis KM, Swanström LL. Peroral endoscopic esophageal myotomy: defining the learning curve. Gastrointest Endosc. 2013;77:719-725. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 153] [Cited by in RCA: 147] [Article Influence: 12.3] [Reference Citation Analysis (0)] |
| 5. | Li QL, Yao LQ, Xu XY, Zhu JY, Xu MD, Zhang YQ, Chen WF, Zhou PH. Repeat peroral endoscopic myotomy: a salvage option for persistent/recurrent symptoms. Endoscopy. 2016;48:134-140. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 19] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 6. | Kumbhari V, Tieu AH, Azola A, Saxena P, Ngamruengphong S, El Zein MH, Khashab MA. Double peroral endoscopic myotomy for achalasia. Gastrointest Endosc. 2015;82:953. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 7. | Phillips S, Falk GL. Surgical tension pneumothorax during laparoscopic repair of massive hiatus hernia: a different situation requiring different management. Anaesth Intensive Care. 2011;39:1120-1123. [PubMed] |
| 8. | Tang A, Huddleston P, Attaluri P, Cruz A, Joseph S, Lavy D. Clinical cases of nonsurgical pneumoperitoneum: categorizing the disease and treatment options. Am Surg. 2015;81:E206-E208. [PubMed] |
| 9. | Ren Z, Zhong Y, Zhou P, Xu M, Cai M, Li L, Shi Q, Yao L. Perioperative management and treatment for complications during and after peroral endoscopic myotomy (POEM) for esophageal achalasia (EA) (data from 119 cases). Surg Endosc. 2012;26:3267-3272. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 175] [Cited by in RCA: 165] [Article Influence: 12.7] [Reference Citation Analysis (0)] |