Published online Sep 21, 2020. doi: 10.3748/wjg.v26.i35.5272
Peer-review started: April 1, 2020
First decision: April 25, 2020
Revised: April 29, 2020
Accepted: August 25, 2020
Article in press: August 25, 2020
Published online: September 21, 2020
Processing time: 168 Days and 17.3 Hours
Sulfasalazine has been used as a standard-of-care in ulcerative colitis for decades, however, it results in severe adverse symptoms, such as hepatotoxicity, blood disorders, male infertility, and hypospermia. Accordingly, the new treatment strategy has to enhance pharmacological efficacy and stimultaneously minimize side effects.
To compare the anti-inflammatory action of sulfasalazine alone or in combination with herbal medicine for ulcerative colitis in a dextran sodium sulfate (DSS)-induced colitis mouse model.
To induce ulcerative colitis, mice received 5% DSS in drinking water for 7 d. Animals were divided into five groups (n = 9 each) for use as normal (non-DSS), DSS controls, DSS + sulfasalazine (30 mg/kg)-treatment experimentals, DSS + sulfasalazine (60 mg/kg)-treatment experimentals, DSS + sulfasalazine (30 mg/kg) + Citrus unshiu peel and Bupleuri radix mixture (30 mg/kg) (SCPB)-treatment experimentals.
The SCPB treatment showed an outstanding effectiveness in counteracting the ulcerative colitis, as evidenced by reduction in body weight, improvement in crypt morphology, increase in antioxidant defenses, down-regulation of proinflammatory proteins and cytokines, and inhibition of proteins related to apoptosis.
SCPB may represent a promising alternative therapeutic against ulcerative colitis, without inducing adverse effects.
Core Tip: Sulfasalazine has been used widely as a standard-of-care in ulcerative colitis; however, it is associated with a spectrum of side effects after long-term and high-dose intake. Since a single dose of sulfasalazine cannot provide satisfactory therapeutic results, we conducted a comparative evaluation of the pharmacological effect of sulfasalazine alone and when used in combination with Citrus unshiu peel and Bupleuri radix mixture in an experimentally-induced ulcerative colitis mouse model.
- Citation: Shin MR, Park HJ, Seo BI, Roh SS. New approach of medicinal herbs and sulfasalazine mixture on ulcerative colitis induced by dextran sodium sulfate. World J Gastroenterol 2020; 26(35): 5272-5286
- URL: https://www.wjgnet.com/1007-9327/full/v26/i35/5272.htm
- DOI: https://dx.doi.org/10.3748/wjg.v26.i35.5272
Inflammatory bowel diseases (IBDs), including ulcerative colitis (UC) and Crohn’s disease, are chronic and uncontrolled intestinal disorders that have emerged collectively as an important public health problem worldwide[1]. The recommended drugs in clinical use for treatment of IBD patients currently include corticosteroids, sulfasalazine, immunosuppressants, antibiotics, and anti-tumor necrosis factor (TNF)-α antibodies. Conventional therapies also involve combinations of these agents[2,3]. Unfortunately, the incidence and prevalence of IBDs are continuing to increase[4] and the plethora of data from cases treated with the commonly used drugs have revealed a number of side effects and troubling issues, such as blood disorders, hepatotoxicity, hypospermia, male infertility, and economic burden[5]. Thus, alternatives for a safer, cheaper, and more efficacious approach to managing and/or treating IBDs is needed.
Diverse mixtures of herbal medicines have been screened as candidates for alleviating various inflammatory disorders[6,7]. Toki-shakuyaku-san, which is a traditional kampo medicine, was found to down-regulate the inflammatory and apoptotic signaling during colitis[8]. The rhizome mixture of Anemarrhena asphodeloides and Coptidis chinensis was found to exert an anti-colitic effect by inhibiting nuclear factor-kappa B (NF-κB) activation[9]. Moreover, Hange-shashin-to was found to suppress IBD in a rat model of experimental colitis[10]. Ultimately, the collective research findings support the potential benefit of anti-inflammatory herbal combinations in colitis.
Citrus unshiu peel has been used widely throughout East Asia for improving the common cold, dyspepsia, and blood circulation[11]. The Citrus unshiu peel — a seedless and easy-peeling citrus fruit — contains various flavonoids, such as hesperidin, naringin, and nobiletin[12-14]. These active compounds have been reported to exert potent anti-inflammatory, antioxidant, anti-adipogenic, anti-diabetic, anti-microbial, and anti-allergic activities[15,16]. On the other hand, Bupleuri radix has been mainly applied in clinical use for liver-related disease, and the recent pharmacological research has demonstrated its renoprotective and hepatoprotective effects[17,18]. Saikosaponins isolated from Bupleuri radix possess valuable pharmacological activities, including those of anti-inflammatory, antitumor, antiviral, and anti-allergic, working mainly through NF-κB or mitogen-activated protein kinase (MAPK) pathways[19-21]. On the basis of these reports, we estimated that Citrus unshiu peel according to its anti-inflammatory effect and Bupleuri radix according to its hepatoprotective and renoprotective effects may be able to exert therapeutic benefits in UC.
To date, there are no studies on the potential anti-inflammatory effect of a treatment mixture of Citrus unshiu peel and Bupleuri radix nor on its underlying mechanisms. The present study was conducted to evaluate the pharmacological effect of sulfasalazine alone and in combination with Citrus unshiu peel and Bupleuri radix mixture in UC, using a well-established experimentally-induced UC mouse model system.
Dextran sodium sulfate (DSS) (molecular weight: 36000-50000 Da) was purchased from MP Biologicals (Santa Ana, CA, United States). Sulfasalazine (purity ≥ 98%) and phenylmethylsulfonyl fluoride (commonly known as PMSF) were purchased from Sigma-Aldrich (St. Louis, MO, United States). Protease inhibitor mixture solution and ethylenediaminetetraacetic acid (commonly known as EDTA) were purchased from Wako Pure Chemical Industries, Ltd. (Osaka, Japan). 2′,7′-dichlorofluorescein diacetate (referred to as DCF-DA) was obtained from Molecular Probes (Eugene, OR, United States). Pierce bicinchoninic acid protein assay kit was obtained from Thermo Fisher Scientific (Waltham, MA, United States). Enhanced chemiluminescence (commonly known as ECL) western blotting detection reagents and pure nitrocellulose membranes were supplied by GE Healthcare (Chicago, IL, United States). The following antibodies were obtained from Santa Cruz Biotechnology, Inc. (Santa Cruz, CA, United States): (mouse polyclonal) nuclear factor-kappa B p65 (NF-κBp65) (1:1000; SC-372), p47phox (1:1000; SC-14015), Rac 1 (1:1000; SC-217), superoxide dismutase (SOD) 1:1000; SC-11407), glutathione peroxidase-1/2 (GPx-1/2) 1:1000; SC-30147), Bax (1:1000; SC-7480), Bcl-2 (1:1000; SC-7382), monocyte chemoattractant peptide-1 (MCP-1) (1:1000; SC-28879), and intercellular adhesion molecule-1 (ICAM-1) (1:1000; SC-1511-R); (goat polyclonal) tumor necrosis factor-α (TNF-α) (1:1000; SC-1351) and interleukin-1β (IL-1β) (1:1000; SC-1252); (mouse monoclonal) phosphor-extracellular signal-regulated kinase 1/2 (p-ERK1/2) (1:1000; SC-7383), phosphor-p38 (p-p38) (1:1000; SC-7973), cyclooxygenase-2 (COX-2) (1:1000; SC-19999), inducible nitric oxide synthase (iNOS) (1:1000; SC-7271), histone (1:1000; SC-8030), and β-actin (1:1000; SC-4778); and rabbit anti-goat (1:3000; SC-2774), goat anti-rabbit (1:3000; SC-2004), and goat anti-mouse (1:3000; SC-2005) immunoglobulin G (IgG) horseradish peroxidase (HRP)-conjugated secondary antibodies. Mouse monoclonal anti-caspase-3 (1:1000; 3004-100) was purchased from BioVision Inc. (Mountain View, CA, United States). Rabbit polyclonal anti-reduced nicotinamide adenine dinucleotide phosphate oxidase 4 (NOX4) was purchased from LifeSpan BioSciences (Seattle, WA, United States). All other chemicals and reagents were purchased from Sigma-Aldrich (St. Louis, MO, United States).
Bupleuri radix was supplied by Bonchowon (Yeongcheon-si, Gyeongsangnam-do, South Korea) and two herbs were produced according to Korean Good Manufacturing Practice. Dried Bupleuri radix (100 g) was extracted with 10 volumes of water and boiled in distilled water (100°C for 2 h). After filtration, the water extracts were evaporated using a rotary evaporator at 45°C and the solvent was evaporated in vacuo to give an extract with a yield of 26%. In addition, a crude drug preparation of Citrus unshiu peel (Citri unshiu pericarpium) (1 kg; Wansan Medicinal Herbs Co. Ltd., Jeonju-si, South Korea) was extracted with ethanol: H2O (1:1) under reflux (2 L × 3). After the solvent was evaporated under reduced pressure, the crude extract (220 g) was obtained. The two prepared herbs were kept at -80°C until use in animal experiments.
All procedures involving animals were reviewed and approved by the Institutional Animal Care and Use Committee of the Daegu Haany University (No. DHU2017-043). Eight-week-old male BALB/c mice, weighing 22-24 g, were purchased from Orient Bio Animal Center (Seongnam-si, South Korea). Mice were maintained under a 12h light/dark cycle, housed at a controlled temperature of 24 ± 2°C and humidity of approximately 60%). After adaptation (1 wk), acute colitis was induced by oral administration of 5% (w/v) DSS dissolved in drinking water, for 7 d[15]. The colitic mice were divided into four groups (n = 9 each) for use as DSS controls, DSS + sulfasalazine (30 mg/kg)-treatment experimentals, DSS + sulfasalazine (60 mg/kg)-treatment experimentals, DSS + sulfasalazine (30 mg/kg) + Citrus unshiu peel and Bupleuri radix mixture (30 mg/kg) (SCPB)-treatment experimentals. A group of 9 untreated (normal) mice received drinking water without DSS throughout the entire experimental period. Sufasalazine was used as the positive reference agent and it was given at doses of 30 mg/kg/d or 60 mg/kg/d. The 30 mg/kg Citrus unshiu peel and Bupleuri radix mixture was comprised of 25 mg/kg Citrus unshiu peel and 5 mg/kg Bupleuri radix (for a 5:1 ratio) and mixed just before application as the drug treatment. At 18 h after the last dosage was given, 2.5% isoflurane (Troikaa Pharmaceuticals Ltd., India) was administered for blood sample collection (cardiac puncture), sacrifice, and removal of the entire colon. All collected specimens were snap-frozen in liquid nitrogen and stored at -80°C until analysis. Symptomatic index of colitis, such as body weight loss, rectal bleeding, and mucus or watery diarrhea, were observed during experimental periods (before sacrifice).
Serum reactive oxygen species (ROS) concentration was measured by employing the method of Ali et al[22]. Briefly, 25 mmol/L DCF-DA was added to the serum and allowed to incubate for 30 min, after which the changes in fluorescence values were determined at an excitation wavelength of 486 nm and emission wavelength of 530 nm.
For microscopic evaluation, intestine tissue was fixed in 10% neutral-buffered formalin and, after embedding in paraffin, cut into 2 mm sections and stained using hematoxylin and eosin (H&E), for microscopic evaluation. The stained slices were subsequently observed under an optical microscope and analyzed using the iSolution Lite software program (InnerView Co., Seongnam-si, Gyeonggi-do, South Korea).
Protein extraction was performed according to the method of Komatsu[23], with minor modifications. Briefly, colon tissues were processed to obtain the cytosol fraction by homogenization with ice-cold lysis buffer A (250 mL; containing 10 mmol/L HEPES (pH 7.8), 10 mmol/L KCl, 2 mmol/L MgCl2, 1 mmol/L DTT, 0.1 mmol/L EDTA, 0.1 mmol/L PMSF, and 1250 μL protease inhibitor mixture solution). After incubation for 20 min at 4°C, the homogenate was mixed with 10% NP-40 and centrifuged (13400 × g for 2 min at 4°C; 5415R Centrifuge from Eppendorf, Hamburg, Germany). The supernatant liquid (cytosol fraction) was separated into a new e-tube and the pellets were washed twice with buffer A (wash supernatants were discarded). The washed pellets were resuspended with lysis buffer C (20 mL; containing 50 mmol/L HEPES (pH 7.8), 50 mmol/L KCl, 300 mmol/L NaCl, 1 mmol/L DTT, 0.1 mmol/L EDTA, 0.1 mmol/L PMSF, 1% (v/v) glycerol and 100 μL protease inhibitor mixture solution) and incubated for 30 min at 4°C. After centrifugation (13400 × g for 10 min at 4°C), the nuclear fraction was prepared to collect the supernatant. Both cytosol and nuclear fractions were stored at -80°C until analysis.
For the estimation of NF-κBp65 and histone, 12 μg of protein from each nuclear fraction was electrophoresed through 10% sodium dodecylsulfate polyacrylamide gel (commonly known as SDS-PAGE). The electro-separated proteins were then transferred to a nitrocellulose membrane, blocked with 5% (w/v) skim milk solution for 1 h, and incubated with primary antibodies (NF-KBp65 and histone) overnight at 4 °C. After the blots were washed, they were incubated with anti-rabbit or anti-mouse IgG HRP-conjugated secondary antibody for 1 h at room temperature. In addition, 7.5 μg protein of each cytosol fraction was electrophoresed through 8%-12% SDS-PAGE for detection of NOX4, p47phox, Rac1, Bax, Bcl-2, caspase-3, SOD, catalase, GPx-1/2, COX-2, iNOS, TNF-α IL-1β, MCP-1, ICAM-1, and β-actin. Each antigen-antibody complex was visualized using the ECL western blotting detection reagents and measured by chemiluminescence with Sensi-Q 2000 Chemidoc (Lugen Sci Co., Ltd., Gyeonggi-do, South Korea). Band densities were measured using ATTO Densitograph Software (ATTO Corp., Tokyo, Japan) and quantified as the ratio to histone or β-actin. The protein levels of the groups are expressed relative to those of the normal mice group (represented by the value of 1.0).
The data are expressed as the mean ± standard error of the mean. Statistical analysis was performed by one-way ANOVA followed by Least-significant differences (LSD) test using SPSS version 22.0 software (SPSS Inc., Chicago, IL, United States). P values less than 0.05 were considered to indicate statistical significance.
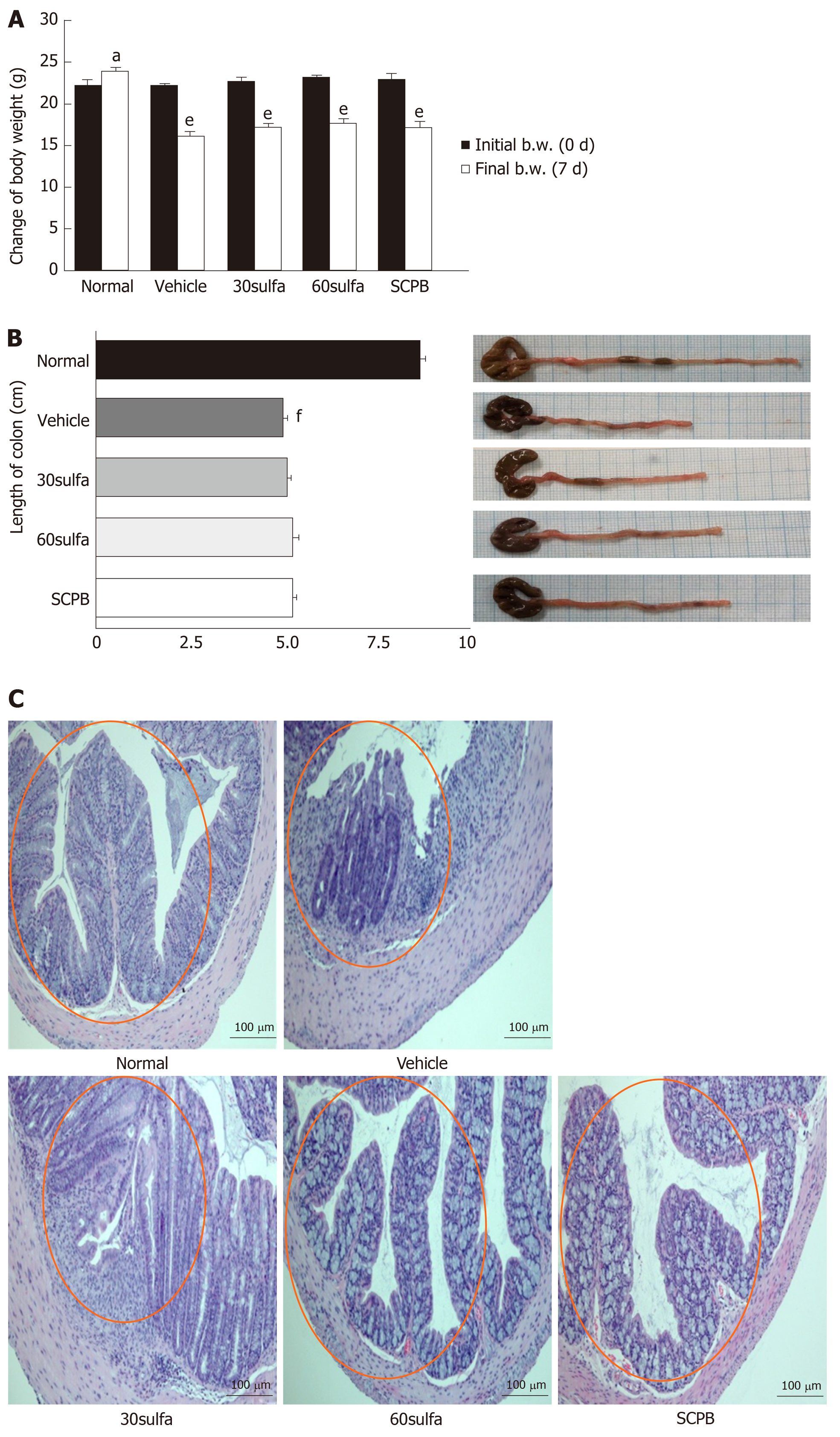
Compared with the normal (non-DSS) group, the DSS control group showed considerably greater body weight loss over the experimental period (P < 0.001). However, oral administration of SCPB and sulfasalazine mildly ameliorated the severity of body weight loss in the DSS control group (Figure 1A). As shown in Figure 1B, the DSS control group showed colon length reduction of 57.94% compared with that of the normal group (P < 0.001); however, the group treated with SCPB showed a 2.8% increase compared with that of the DSS control group but the difference did not reach the threshold for statistical significance.
Colonic inflammation involves the disruption of crypt morphology, resulting in the infiltration of inflammatory cells and thickening of the lamina propria[24]. As shown in Figure 1C, the colons of the DSS control group showed histologic alterations such as infiltration of numerous inflammatory cells, goblet cell degeneration, and crypt distortion consistent with UC. Treatment with sulfasalazine or SCPB appeared to preserve the broad crypt distortion and ameliorate the infiltration of inflammatory cells.
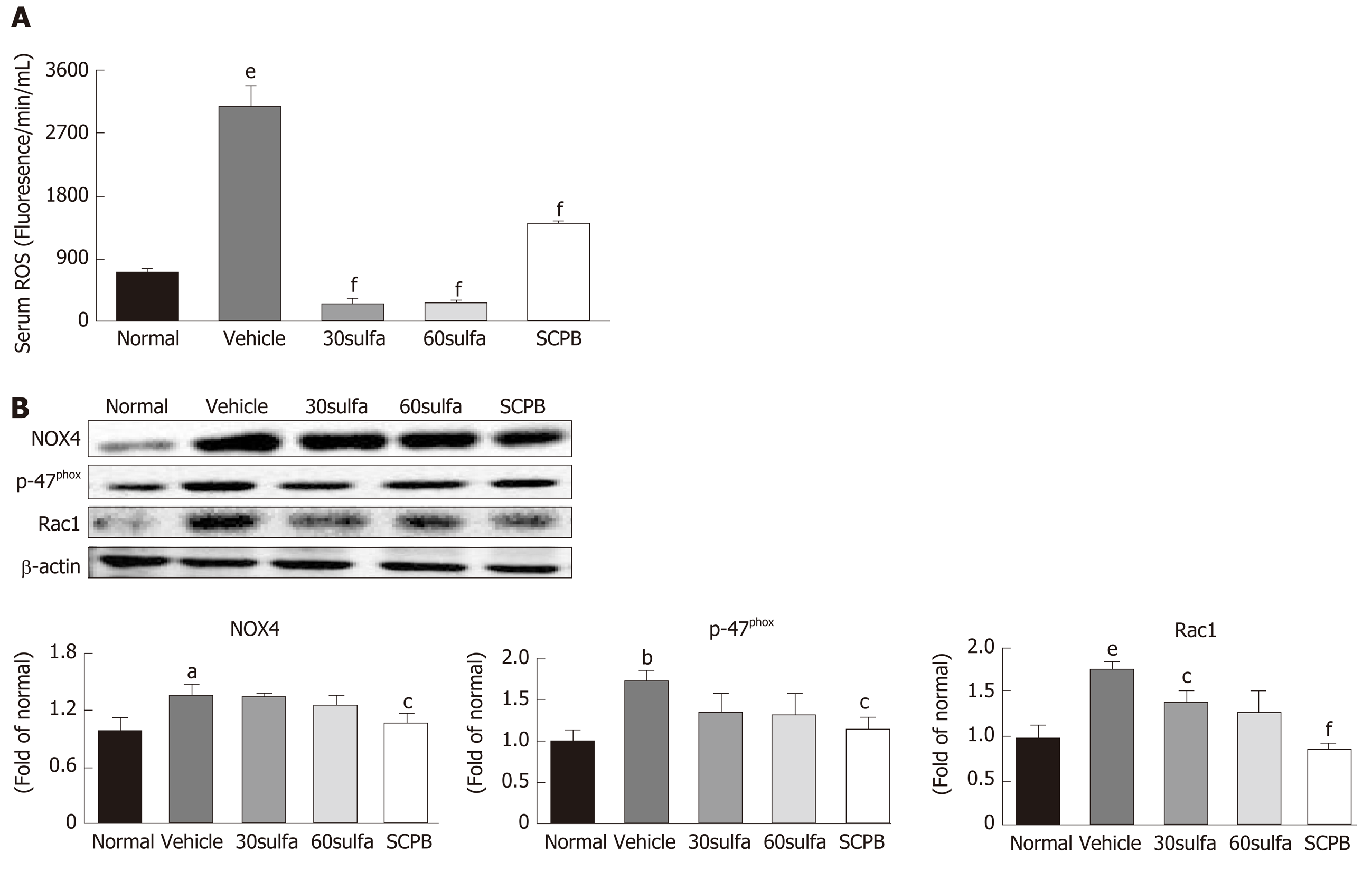
As shown in Figure 2A, serum ROS levels in the DSS control group were markedly higher than that in the normal (non-DSS) group (P < 0.001); however, the administration of sulfasalazine or SCPB appeared to lead to a marked decrease in the DSS-induced elevated levels (P < 0.001). As shown in Figure 2B, the protein expressions of nicotinamide adenine dinucleotide phosphate (NADPH) oxidase enzymes in the DSS control group were significantly elevated compared with those in the normal (non-DSS) group (NOX4, P < 0.05; p47phox, P < 0.01; Rac 1, P < 0.001). However, the SCPB administration appeared to decrease and ameliorate the levels of each, in a manner superior to that of sulfasalazine alone (NOX4, P < 0.05; p47phox, P < 0.05; Rac 1, P < 0.001). The 60 mg/kg sulfasalazine dosage, especially, showed a remarkable tendency towards effecting this decrease, but the difference did not reach the threshold for statistical significance.
Oxidative stress plays a vital role in IBD[25]. The activities of SOD and catalase showed a significant decrease in the DSS control group compared to those in the normal (non-DSS) group (SOD, P < 0.05; catalase, P < 0.001). However, the SPCB treatment significantly elevated the activities of SOD and catalase, but not of GPx-1/2 and the differences did not reach the threshold for statistical significance. These results indicated that SCPB supplementation may decrease the extent of colonic injury via its antioxidant effect (SOD, P < 0.05; catalase, P < 0.01) and do so in a manner superior treatment with sulfasalazine alone (Figure 3).
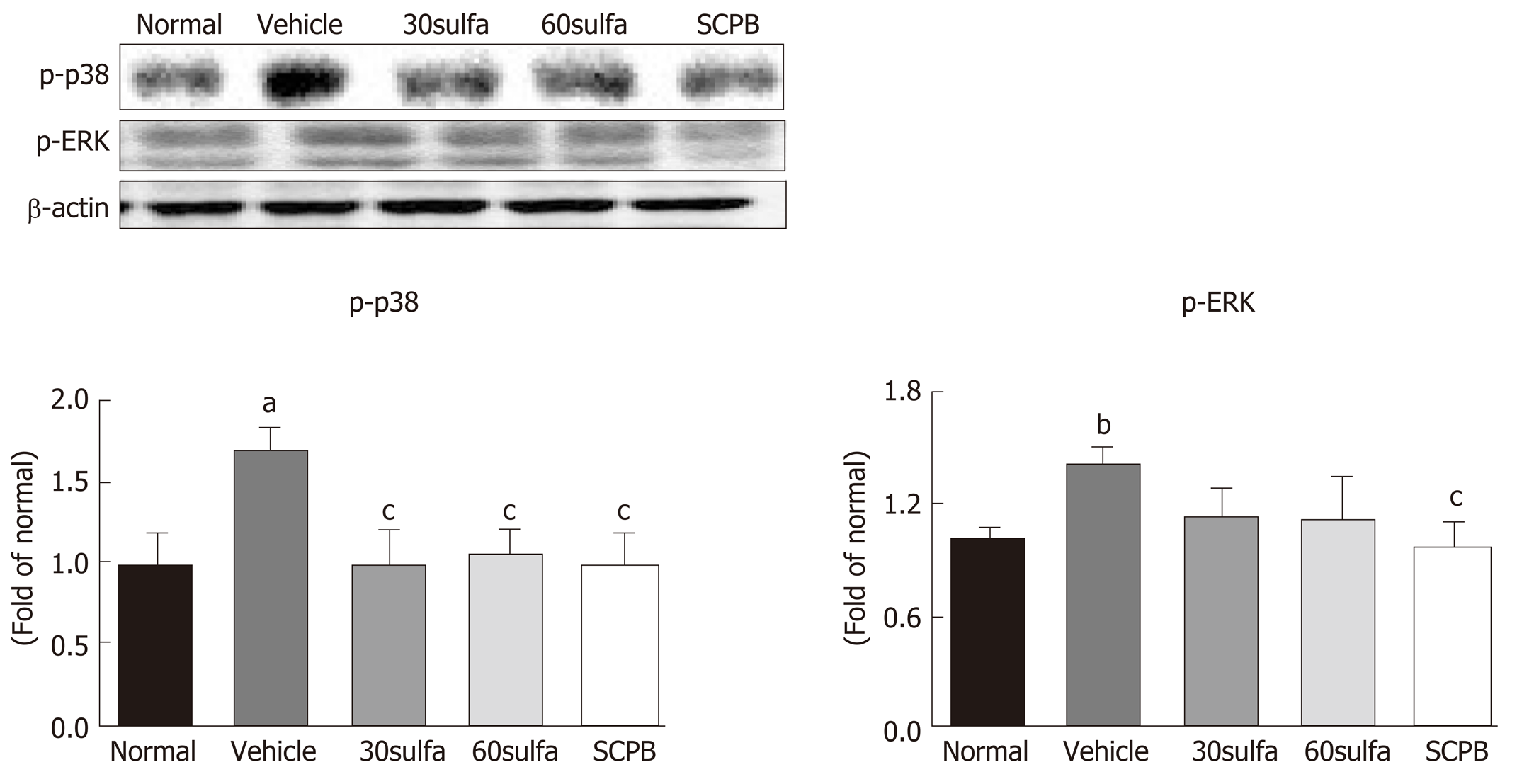
The MAPK pathways can be activated by oxidative stress, leading to inflammation processes and apoptosis[26]. MAPK-related protein expressions showed augmentation in the colons of mice in the DSS control group compared to those of the normal (non-DSS) group (p-p38, P < 0.05; p-ERK1/2; P < 0.01); in contrast, the oral administration of SCPB significantly decreased the expression of both p-p38 and p-ERK1/2, which reached nearly normal levels (P < 0.05), as shown in Figure 4.
It has been confirmed that NF-κB is the central transcription factor in the regulation of proinflammatory mediators (i.e., COX-2 and iNOS), proinflammatory cytokines (i.e., TNF-α and IL-1β), and at least one chemokine (i.e., MCP-1), and one adhesion molecule (i.e., ICAM-1) during inflammation[27]. The DSS control group showed enhanced phosphorylation of NF-κB in colon (P < 0.01), whereas the elevation was significantly reversed upon SCPB (P < 0.05). As important downstream targets of NF-κB, the expressions of COX-2 and iNOS were increased in the DSS control group and markedly blocked in mice given SCPB supplementation (P < 0.05). In contrast, treatment with sulfasalazine alone merely showed a tendency to decrease the expression of the two factors. Moreover, expressions of TNF-α and IL-1β as well as COX-2 and iNOS were noticeably amplified in the DSS control group but administration of both SCPB and sulfasalazine significantly inhibited this effect. These protein levels were down-regulated similarly or to an extent lower than normal levels (Figure 5). Furthermore, the level of MCP-1 and ICAM-1 protein expressions were decreased in the mice who received SCPB.
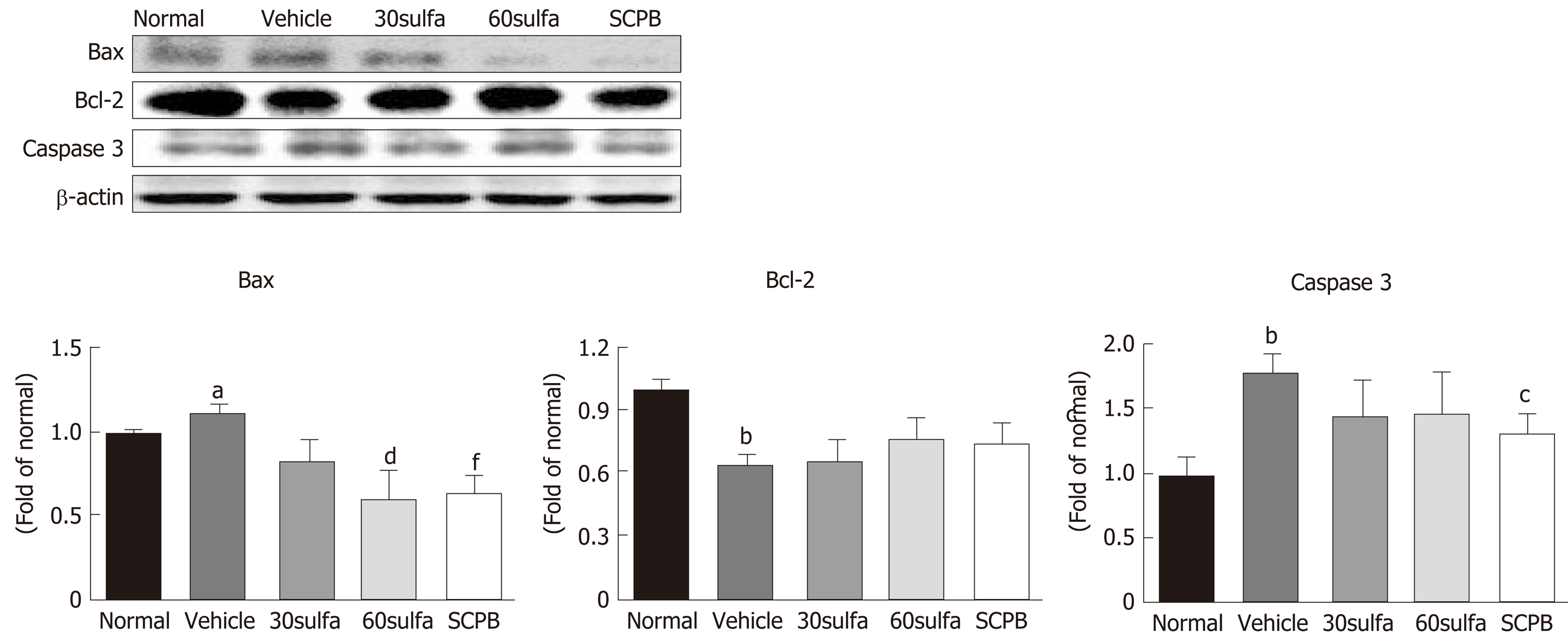
The excess exposure of ROS in the colonic mucosa is known to trigger apoptosis of colon epithelial cells, leading to progression of IBD[28]. The DSS control group showed the disease-characteristic apoptosis features of inflamed colon epithelial cells, supported by an observable increase in Bax and caspase-3 activities (Figure 6). In contrast, the SCPB treatment appeared to lead to marked down-regulation of the DSS-induced Bax and caspase-3 activities (P < 0.001 and P < 0.05, respectively). These findings suggest that SCPB may protect the colon mucosa from apoptosis in DSS-induced colitis. Meanwhile, Bcl-2 protein expression during UC didn’t show a significant difference as only a mild increase.
UC is a type of IBD characterized by chronic inflammation of the intestinal mucosa, manifesting body weight loss, bloody diarrhea, tenesmus, abdominal pain, and fatigue. The incidence and prevalence of UC have been reported over many years and both continue to show a rapid increase worldwide[29]. Nowadays, sulfasalazine, a prodrug of 5-aminosalicylic acid, is currently used as the first-line therapy for mild-to-moderate UC[30]. Although its clinical prescription is executed routinely, the ratios of refractory and relapsed cases are comparatively high[31] and it remains at the limit of poor tolerability due to frequent gastrointestinal side effects[32]. DSS, used for the induction of UC in animal models, causes a marked inflammatory and immune response by affecting DNA replication, inhibiting the overgrowth of epithelial cells, inducing macrophage activation, increasing the release of cytokines, and breaking the balance of gut microflora. The gut microflora itself is a critical player in intestinal permeability with imbalance between beneficial and pathogenic bacteria being implicated in IBD pathogenesis[33]. Consequently, DSS supplementation results in acute UC, which is similar to human UC and making it is an ideal model that has been widely used to study the mechanism of UC and for screening of potential drugs[34,35].
The present study provided, for the first time, a comparative evaluation of the pharmacological efficacy of sulfasalazine combined with Citrus unshiu peel and Bupleuri radix mixture (the ‘SCPB’ treatment described herein), as compared with sulfasalazine alone, in a mouse model of UC. While our the DSS control mice had significantly increased body weight loss and decreased colon length, previous studies have showed length of colon to be inversely correlated with severity of the experimental colitis[36]. In our study, the DSS-induced mice showed significantly decreased final body weight and both the sulfasalazine and SCPB treatments curtailed the body weight loss and the shortening of the colon length. Herein, each groups showed the improvement effect like 30sulfa (1.96%), 60sulfa (5.36%), and SCPB (4.79%) on the colon length compared to the DSS control mice although it was not significant. The DSS-induced colonic mucosal damage persisted till day 7, evidenced by epithelial necrosis, impaired mucosa integrity (with submucosa showing hyperemia and edema), and ulceration, accompanied by infiltration of numerous inflammatory cells, such as monocytes and macrophages[37]; importantly, these pathogenic features appeared to be alleviated by the SCPB treatment.
Excessive ROS, including superoxide radicals (O2-), hydroxyl radicals, hydrogen peroxide and singlet oxygen, may have detrimental effects on such basic cellular components as DNA, proteins, and lipids. The enzymatic process that can generate ROS is the reaction catalyzed by NADPH oxidase[38]. In resting cells, the subunits of NADPH oxidase are present in the cytosol and the membranes. Upon cell activation, the subunits are assembled on a membrane-bound vesicle, which then fuses with the plasma membrane, resulting in the release O2-[38,39]. Accumulation of O2- causes an elevation of the detectable ROS, leading to acceleration of an inflammatory cascade. The influence of ROS in the pathogenesis of gastrointestinal diseases, such as colon cancer and acute and chronic pancreatitis, has been demonstrated[40]. Above all, the previous studies have indicated the importance of ROS-induced oxidative stress in the development of UC[41,42] and overproduction of ROS via NADPH oxidases, including NOX4, p47phox, and Rac 1, has been implicated in tissue damage observed in chronic inflammatory disorders[42]. In the current study, the DSS injury was accompanied by an elevated level of serum ROS, which was decreased upon treatment with either sulfasalazine or SCPB. The protein expressions of NOX4, p47phox, and Rac 1 (the markers of NADPH oxidase activity) were augmented in the colons of the DSS control mice. While the 60 mg/kg sulfasalazine-alone treatment down-regulated the NADPH oxidase activity, the SCPB treatment did so to a much greater extent. Generally, ROS are neutralized by endogenous antioxidant enzymes[43]; namely, SOD converts O2- to hydrogen peroxide, which is subsequently neutralized to water by the actions of catalase and GPx-1/2. IBD patients present with serious impairment in antioxidant enzyme levels in their intestinal mucosa[44]. In our study, the SOD, catalase, and GPx-1/2 enzymic antioxidants were markedly decreased in the mice with DSS-induced colitis. SCPB administration significantly increased the activities of SOD and catalase but not of GPx-1/2. Overall, these results indicate that SCPB regulates antioxidant enzyme activity against oxidative stress in DSS-induced colitis mice; moreover, this effect was superior to that effected by sulfasalazine alone.
NF-κB participates in controlling the activation of various proinflammatory cytokine genes, such as IL-1β, IL-6, and TNF-α, underlying its critical role in the pathogenesis of UC. MAPKs are also implicated in the pathogenic mechanism, and their activity leads to the activation of various nuclear transcription factors. ROS overproduction activates MAPKs, including p38 and ERK1/2. Phosphorylation of p38 has been confirmed after induction of experimental colitis, wherein activation of p38 can greatly promote the activation of immune cells and aggravate inflammation[45]. In particular, p38 MAPK has numerous direct and indirect interactions with NF-κB. Namely, the phosphorylation of p38 MAPK is implicated by leading to the activation of NF-κB. Moreover, the phosphorylation of ERK1/2 MAPKs are also stimulated upon activation of NF-κB[46,47]. In the present study, the colons of DSS-induced colitis mice showed the expected increases in expressions of ERK1/2 and p38, which SCPB treatment was able to decrease significantly. The NF-κB transcription factor plays a critical role in inflammation, facilitating the expression and secretion of various proinflammatory cytokines, mediators, and chemokines to mediate a series of subsequent inflammatory cascades[48]. Blocking NF-κB activation is known to reduce the release of proinflammatory cytokines, thereby alleviating development of the inflammatory response and achieving a therapeutic effect. In this study, we evaluated the inhibitory effect of SCPB on NF-κB activation in DSS-induced colitis mice. The DSS-induced elevation in NF-κB levels was suppressed upon SCPB treatment but the inhibitory effect of SCPB was much lower than that of sulfasalazine alone. These results suggest that SCPB could ameliorate DSS-induced acute colitis by inhibiting NF-κB activation. NF-κB activation exerts a strong influence on the inflammatory response.
Our results also indicate that SCPB significantly inhibited the induction of COX-2 and iNOS expressions and the production of the proinflammatory cytokines TNF-α and IL-1β. Moreover, the SCPB treatment remarkably down-regulated the MCP-1 chemokine and attenuated the adhesion molecule ICAM-1. Excessive exposure of ROS under inflammatory conditions is known to increase epithelial cell apoptosis[49], which is likely to deteriorate epithelial barrier integrity and has an influence on intestinal damage. Thus, we postulated that DSS treatment is responsible for inducing apoptosis through activation of apoptosis proteins, specifically Bax and caspase-3, and suppression of anti-apoptotic protein, namely Bcl-2, as reported by other researchers[50,51]. Indeed, our DSS-induced colitis mice showed a considerable down-regulation of Bax and caspase-3 upon SCPB treatment. However, Bcl-2 just showed a tendency to increase without a significance. Maybe it judged that other anti-apoptotic protein such as survivin must have been is involved in apoptosis.
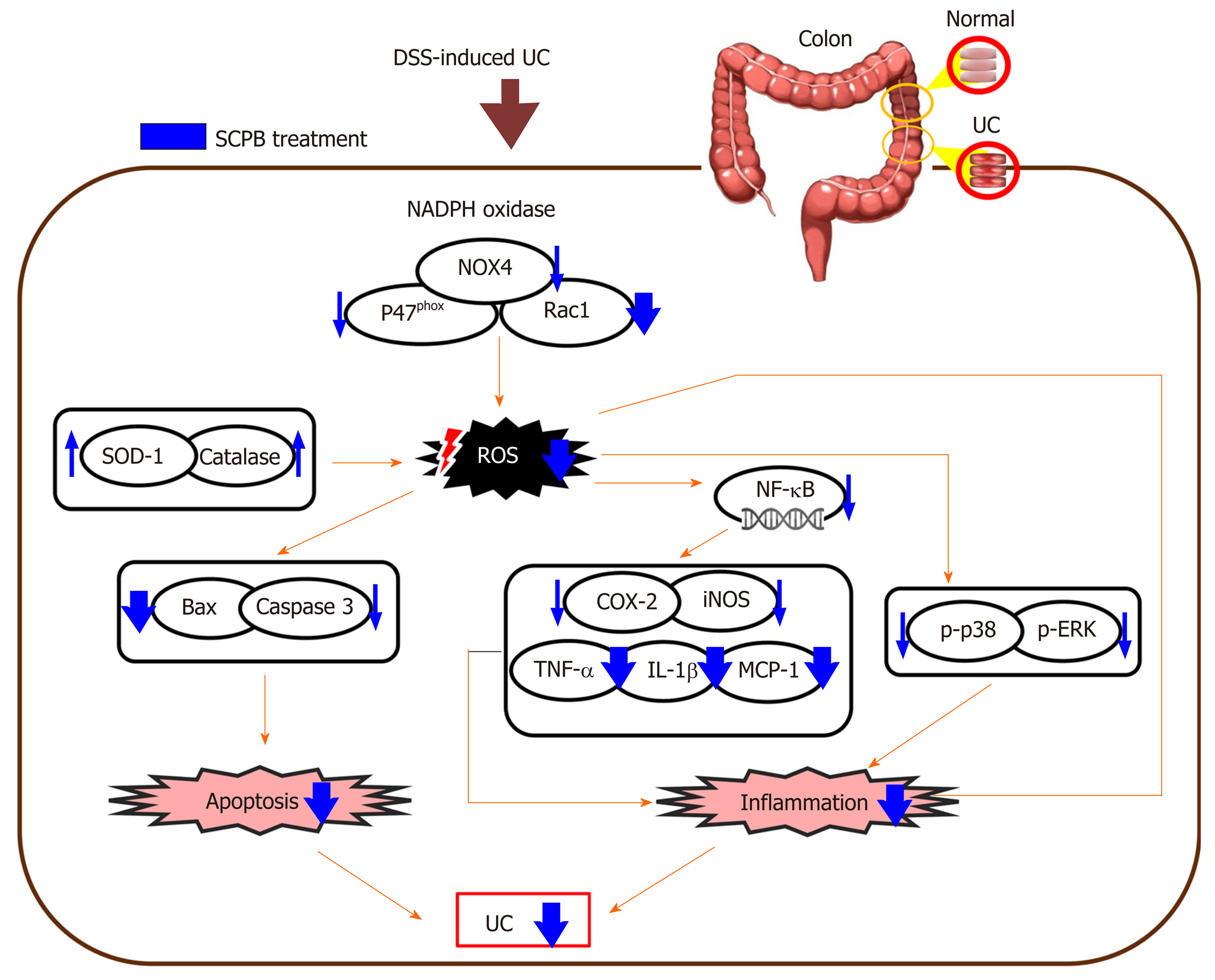
As a result, the administration of SCPB to mice treated with DSS ameliorated acute inflammation and apoptosis in the colon, as shown in Figure 7. Taken together, the present findings suggest that SCPB is an effective inhibitor of DSS-induced colitis in mice. The SCPB treatment showed enhanced therapeutic effect compared to that of the standard sulfasalazine treatment. Nevertheless, the underlying mechanism of SCPB is still ambiguous and further profound researches are needed.
Ulcerative colitis (UC) has high incidence worldwide and is characterized by unintentional weight loss, abdominal pain, mucous and bloody diarrhea, and anemia. Generally, the recommended therapies for UC include anti-inflammatory drugs, antibiotics, immunosuppressants, and anti-tumor necrosis factor-alpha antibodies. Sulfasalazine, a drug composed of 5-aminosalicylic acid and sulfapyridine, has been prescribed as a standard-of-care in UC treatment. Otherwise, it can produce a variety of side effects upon long-term and high-dose intakes. Hence, an alternative approach for a safer, cheaper, and more efficacious management or treatment of UC is needed.
UC is chronic and complex autoimmune inflammatory disorder. The incidence of UC has grown worldwide over the recent decades and the quality of life for patients suffering from UC has been falling quickly, in tandem. The findings from our research will give essential help towards dealing with the problems of these patients, with sulfasalazine with Citrus unshiu peel and Bupleuri radix mixture (referred to as SCPB), one of more safe and effective herbal medicine mixtures, contributing to improving their quality of life.
The present study was conducted to evaluate the pharmacological effect of sulfasalazine alone and as the SCPB combination using an experimentally-induced UC mouse model.
Ulcerative colitis was induced by 5% dextran sodium sulfate in drinking water for 7 d. The pharmacological effect of sulfasalazine alone and SCPB was evaluated using serum analysis, histological exam, and western blotting. The colon tissue was selected as the region of interest for data analysis. One-way ANOVA followed by Least-significant differences (LSD) test were used for statistical inference.
The SCPB treatment significantly inhibited the induction of COX-2 and iNOS expressions and the production of the proinflammatory cytokines TNF-α and IL-1β. Moreover, the SCPB treatment remarkably down-regulated the MCP-1 chemokine and attenuated the adhesion molecule ICAM-1. The SCPB treatment exerted anti-apoptotic effect though a considerable down-regulation of Bax and caspase-3 upon SCPB treatment.
The SCPB supplementation showed enhanced therapeutic effect compared to that of the standard sulfasalazine treatment. Accordingly, SCPB may represent a promising alternative therapeutic against ulcerative colitis without inducing adverse effects.
A single dose of sulfasalazine cannot provide satisfactory therapeutic results because of a spectrum of side effects after long-term and high-dose intake. However, when we used in combination with Citrus unshiu peel and Bupleuri radix mixture in an experimentally-induced ulcerative colitis mouse model, its inflammation was alleviated significantly. SCPB therapy may be more efficious for symptom improvement of patients with ulcerative colitis in future.
Manuscript source: Unsolicited manuscript
Specialty type: Gastroenterology and hepatology
Country/Territory of origin: South Korea
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): 0
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Exbrayat JM S-Editor: Gong ZM L-Editor: A P-Editor: Zhang YL
| 1. | Snider AJ, Kawamori T, Bradshaw SG, Orr KA, Gilkeson GS, Hannun YA, Obeid LM. A role for sphingosine kinase 1 in dextran sulfate sodium-induced colitis. FASEB J. 2009;23:143-152. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 151] [Cited by in RCA: 166] [Article Influence: 9.8] [Reference Citation Analysis (0)] |
| 2. | Larussa T, Imeneo M, Luzza F. Potential role of nutraceutical compounds in inflammatory bowel disease. World J Gastroenterol. 2017;23:2483-2492. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 60] [Cited by in RCA: 52] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 3. | Ross AS, Cohen RD. Medical therapy for ulcerative colitis: the state of the art and beyond. Curr Gastroenterol Rep. 2004;6:488-495. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 16] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 4. | de Souza HS, Fiocchi C. Immunopathogenesis of IBD: current state of the art. Nat Rev Gastroenterol Hepatol. 2016;13:13-27. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1185] [Cited by in RCA: 1120] [Article Influence: 124.4] [Reference Citation Analysis (1)] |
| 5. | Linares V, Alonso V, Domingo JL. Oxidative stress as a mechanism underlying sulfasalazine-induced toxicity. Expert Opin Drug Saf. 2011;10:253-263. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 61] [Cited by in RCA: 84] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 6. | Akinbo F, Eze G. Combined Effects of Medicinal Plants on Induced Upper Gastrointestinal Tract Injury in Wistar Rats. Ethiop J Health Sci. 2016;26:573-580. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 7] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 7. | Jeong SJ, Kim OS, Yoo SR, Seo CS, Kim Y, Shin HK. Anti-inflammatory and antioxidant activity of the traditional herbal formula Gwakhyangjeonggi-san via enhancement of heme oxygenase-1 expression in RAW264.7 macrophages. Mol Med Rep. 2016;13:4365-4371. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 15] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 8. | Sreedhar R, Arumugam S, Thandavarayan RA, Giridharan VV, Karuppagounder V, Pitchaimani V, Afrin R, Harima M, Nakamura T, Ueno K, Nakamura M, Suzuki K, Watanabe K. Toki-shakuyaku-san, a Japanese kampo medicine, reduces colon inflammation in a mouse model of acute colitis. Int Immunopharmacol. 2015;29:869-875. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 11] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 9. | Jang SE, Jeong JJ, Hyam SR, Han MJ, Kim DH. Anticolitic Effect of the Rhizome Mixture of Anemarrhena asphodeloides and Coptidis chinensis (AC-mix) in Mice. Biomol Ther (Seoul). 2013;21:398-404. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 10] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 10. | Kawashima K, Nomura A, Makino T, Saito K, Kano Y. Pharmacological properties of traditional medicine (XXIX): effect of Hange-shashin-to and the combinations of its herbal constituents on rat experimental colitis. Biol Pharm Bull. 2004;27:1599-1603. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 39] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 11. | Oh YC, Cho WK, Jeong YH, Im GY, Yang MC, Hwang YH, Ma JY. Anti-inflammatory effect of Citrus Unshiu peel in LPS-stimulated RAW 264.7 macrophage cells. Am J Chin Med. 2012;40:611-629. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 45] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 12. | Lim DW, Lee Y, Kim YT. Preventive effects of Citrus unshiu peel extracts on bone and lipid metabolism in OVX rats. Molecules. 2014;19:783-794. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 27] [Cited by in RCA: 28] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 13. | Lu Y, Zhang C, Bucheli P, Wei D. Citrus flavonoids in fruit and traditional Chinese medicinal food ingredients in China. Plant Foods Hum Nutr. 2006;61:57-65. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 96] [Cited by in RCA: 90] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 14. | Zhang C, Lu Y, Tao L, Tao X, Su X, Wei D. Tyrosinase inhibitory effects and inhibition mechanisms of nobiletin and hesperidin from citrus peel crude extracts. J Enzyme Inhib Med Chem. 2007;22:91-98. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 28] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 15. | Kim A, Im M, Gu MJ, Ma JY. Citrus unshiu peel extract alleviates cancer-induced weight loss in mice bearing CT-26 adenocarcinoma. Sci Rep. 2016;6:24214. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 23] [Cited by in RCA: 29] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 16. | Lim H, Yeo E, Song E, Chang YH, Han BK, Choi HJ, Hwang J. Bioconversion of Citrus unshiu peel extracts with cytolase suppresses adipogenic activity in 3T3-L1 cells. Nutr Res Pract. 2015;9:599-605. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 30] [Cited by in RCA: 33] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 17. | Kang SJ, Lee YJ, Kim BM, Kim YJ, Woo HD, Jeon HK, Chung HW. Effect of Bupleuri Radix extracts on the toxicity of 5-fluorouracil in HepG2 hepatoma cells and normal human lymphocytes. Basic Clin Pharmacol Toxicol. 2008;103:305-313. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 40] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 18. | Ashour ML, Wink M. Genus Bupleurum: a review of its phytochemistry, pharmacology and modes of action. J Pharm Pharmacol. 2011;63:305-321. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 161] [Cited by in RCA: 186] [Article Influence: 12.4] [Reference Citation Analysis (0)] |
| 19. | Yuan B, Yang R, Ma Y, Zhou S, Zhang X, Liu Y. A systematic review of the active saikosaponins and extracts isolated from Radix Bupleuri and their applications. Pharm Biol. 2017;55:620-635. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 115] [Cited by in RCA: 142] [Article Influence: 17.8] [Reference Citation Analysis (0)] |
| 20. | Xie JY, Di HY, Li H, Cheng XQ, Zhang YY, Chen DF. Bupleurum chinense DC polysaccharides attenuates lipopolysaccharide-induced acute lung injury in mice. Phytomedicine. 2012;19:130-137. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 67] [Cited by in RCA: 79] [Article Influence: 6.1] [Reference Citation Analysis (0)] |
| 21. | Wang C, Zhang T, Cui X, Li S, Zhao X, Zhong X. Hepatoprotective effects of a chinese herbal formula, longyin decoction, on carbon-tetrachloride-induced liver injury in chickens. Evid Based Complement Alternat Med. 2013;2013:392743. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 11] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 22. | Ali SF, LeBel CP, Bondy SC. Reactive oxygen species formation as a biomarker of methylmercury and trimethyltin neurotoxicity. Neurotoxicology. 1992;13:637-648. [PubMed] |
| 23. | Komatsu S. Extraction of nuclear proteins. Methods Mol Biol. 2007;355:73-77. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 23] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 24. | Jin BR, Chung KS, Cheon SY, Lee M, Hwang S, Noh Hwang S, Rhee KJ, An HJ. Rosmarinic acid suppresses colonic inflammation in dextran sulphate sodium (DSS)-induced mice via dual inhibition of NF-κB and STAT3 activation. Sci Rep. 2017;7:46252. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 116] [Cited by in RCA: 130] [Article Influence: 16.3] [Reference Citation Analysis (0)] |
| 25. | Yan H, Wang H, Zhang X, Li X, Yu J. Ascorbic acid ameliorates oxidative stress and inflammation in dextran sulfate sodium-induced ulcerative colitis in mice. Int J Clin Exp Med. 2015;8:20245-20253. [PubMed] |
| 26. | Yan X, Wu H, Wu Z, Hua F, Liang D, Sun H, Yang Y, Huang D, Bian JS. The New Synthetic H2S-Releasing SDSS Protects MC3T3-E1 Osteoblasts against H2O2-Induced Apoptosis by Suppressing Oxidative Stress, Inhibiting MAPKs, and Activating the PI3K/Akt Pathway. Front Pharmacol. 2017;8:07. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 30] [Cited by in RCA: 38] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 27. | Schuliga M. NF-kappaB Signaling in Chronic Inflammatory Airway Disease. Biomolecules. 2015;5:1266-1283. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 252] [Cited by in RCA: 335] [Article Influence: 33.5] [Reference Citation Analysis (0)] |
| 28. | Kruidenier L, Kuiper I, Lamers CB, Verspaget HW. Intestinal oxidative damage in inflammatory bowel disease: semi-quantification, localization, and association with mucosal antioxidants. J Pathol. 2003;201:28-36. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 262] [Cited by in RCA: 281] [Article Influence: 12.8] [Reference Citation Analysis (0)] |
| 29. | Lerebours E, Savoye G, Guedon C. [Epidemiology and natural history of chronic inflammatory bowel disease]. Gastroenterol Clin Biol. 2003;27:S76-S80. [PubMed] |
| 30. | Tindall WN, Boltri JM, Wilhelm SM. Mild-to-moderate ulcerative colitis: your role in patient compliance and health care costs. J Manag Care Pharm. 2007;13:S2-12; quiz S13-4. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 14] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 31. | Watanabe Y, Murata T, Amakawa M, Miyake Y, Handa T, Konishi K, Matsumura Y, Tanaka T, Takeuchi K. KAG-308, a newly-identified EP4-selective agonist shows efficacy for treating ulcerative colitis and can bring about lower risk of colorectal carcinogenesis by oral administration. Eur J Pharmacol. 2015;754:179-189. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 29] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 32. | Tabit CE, Holbrook M, Shenouda SM, Dohadwala MM, Widlansky ME, Frame AA, Kim BH, Duess MA, Kluge MA, Levit A, Keaney JF, Vita JA, Hamburg NM. Effect of sulfasalazine on inflammation and endothelial function in patients with established coronary artery disease. Vasc Med. 2012;17:101-107. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 27] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 33. | Mizoguchi A. Animal models of inflammatory bowel disease. Prog Mol Biol Transl Sci. 2012;105:263-320. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 166] [Cited by in RCA: 186] [Article Influence: 14.3] [Reference Citation Analysis (0)] |
| 34. | Woo JK, Choi S, Kang JH, Kim DE, Hurh BS, Jeon JE, Kim SY, Oh SH. Fermented barley and soybean (BS) mixture enhances intestinal barrier function in dextran sulfate sodium (DSS)-induced colitis mouse model. BMC Complement Altern Med. 2016;16:498. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 52] [Cited by in RCA: 57] [Article Influence: 6.3] [Reference Citation Analysis (0)] |
| 35. | Huang YF, Zhou JT, Qu C, Dou YX, Huang QH, Lin ZX, Xian YF, Xie JH, Xie YL, Lai XP, Su ZR. Anti-inflammatory effects of Brucea javanica oil emulsion by suppressing NF-κB activation on dextran sulfate sodium-induced ulcerative colitis in mice. J Ethnopharmacol. 2017;198:389-398. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 63] [Article Influence: 7.9] [Reference Citation Analysis (0)] |
| 36. | Lyu W, Jia H, Deng C, Saito K, Yamada S, Kato H. Zeolite-Containing Mixture Supplementation Ameliorated Dextran Sodium Sulfate-Induced Colitis in Mice by Suppressing the Inflammatory Bowel Disease Pathway and Improving Apoptosis in Colon Mucosa. Nutrients. 2017;9. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 6] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 37. | Zhang ZL, Fan HY, Yang MY, Zhang ZK, Liu K. Therapeutic effect of a hydroxynaphthoquinone fraction on dextran sulfate sodium-induced ulcerative colitis. World J Gastroenterol. 2014;20:15310-15318. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 23] [Cited by in RCA: 26] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 38. | Ushio-Fukai M, Nakamura Y. Reactive oxygen species and angiogenesis: NADPH oxidase as target for cancer therapy. Cancer Lett. 2008;266:37-52. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 513] [Cited by in RCA: 468] [Article Influence: 27.5] [Reference Citation Analysis (0)] |
| 39. | Yao J, Cao X, Zhang R, Li YX, Xu ZL, Zhang DG, Wang LS, Wang JY. Protective Effect of Baicalin Against Experimental Colitis via Suppression of Oxidant Stress and Apoptosis. Pharmacogn Mag. 2016;12:225-234. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 36] [Cited by in RCA: 54] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 40. | Kim YJ, Kim EH, Hahm KB. Oxidative stress in inflammation-based gastrointestinal tract diseases: challenges and opportunities. J Gastroenterol Hepatol. 2012;27:1004-1010. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 138] [Cited by in RCA: 172] [Article Influence: 13.2] [Reference Citation Analysis (0)] |
| 41. | Patlevič P, Vašková J, Švorc P, Vaško L, Švorc P. Reactive oxygen species and antioxidant defense in human gastrointestinal diseases. Integr Med Res. 2016;5:250-258. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 172] [Cited by in RCA: 146] [Article Influence: 16.2] [Reference Citation Analysis (0)] |
| 42. | Mitani T, Yoshioka Y, Furuyashiki T, Yamashita Y, Shirai Y, Ashida H. Enzymatically synthesized glycogen inhibits colitis through decreasing oxidative stress. Free Radic Biol Med. 2017;106:355-367. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 32] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 43. | da Costa Gonçalves F, Grings M, Nunes NS, Pinto FO, Garcez TN, Visioli F, Leipnitz G, Paz AH. Antioxidant properties of mesenchymal stem cells against oxidative stress in a murine model of colitis. Biotechnol Lett. 2017;39:613-622. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 41] [Article Influence: 5.1] [Reference Citation Analysis (0)] |
| 44. | Yeom Y, Kim Y. The Sasa quelpaertensis Leaf Extract Inhibits the Dextran Sulfate Sodium-induced Mouse Colitis Through Modulation of Antioxidant Enzyme Expression. J Cancer Prev. 2015;20:136-146. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 16] [Cited by in RCA: 15] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 45. | Seo JH, Lim JW, Kim H. Differential Role of ERK and p38 on NF- κ B Activation in Helicobacter pylori-Infected Gastric Epithelial Cells. J Cancer Prev. 2013;18:346-350. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 19] [Cited by in RCA: 23] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 46. | Feng YJ, Li YY, Lin XH, Li K, Cao MH. Anti-inflammatory effect of cannabinoid agonist WIN55, 212 on mouse experimental colitis is related to inhibition of p38MAPK. World J Gastroenterol. 2016;22:9515-9524. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 25] [Cited by in RCA: 25] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 47. | Tahir AA, Sani NF, Murad NA, Makpol S, Ngah WZ, Yusof YA. Combined ginger extract & Gelam honey modulate Ras/ERK and PI3K/AKT pathway genes in colon cancer HT29 cells. Nutr J. 2015;14:31. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 78] [Cited by in RCA: 69] [Article Influence: 6.9] [Reference Citation Analysis (0)] |
| 48. | Feng J, Guo C, Zhu Y, Pang L, Yang Z, Zou Y, Zheng X. Baicalin down regulates the expression of TLR4 and NFkB-p65 in colon tissue in mice with colitis induced by dextran sulfate sodium. Int J Clin Exp Med. 2014;7:4063-4072. [PubMed] |
| 49. | Thompson WL, Van Eldik LJ. Inflammatory cytokines stimulate the chemokines CCL2/MCP-1 and CCL7/MCP-3 through NFkB and MAPK dependent pathways in rat astrocytes [corrected]. Brain Res. 2009;1287:47-57. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 185] [Cited by in RCA: 180] [Article Influence: 11.3] [Reference Citation Analysis (0)] |
| 50. | Redza-Dutordoir M, Averill-Bates DA. Activation of apoptosis signalling pathways by reactive oxygen species. Biochim Biophys Acta. 2016;1863:2977-2992. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1530] [Cited by in RCA: 2434] [Article Influence: 270.4] [Reference Citation Analysis (0)] |
| 51. | Ju J, Lee GY, Kim YS, Chang HK, Do MS, Park KY. Bamboo Salt Suppresses Colon Carcinogenesis in C57BL/6 Mice with Chemically Induced Colitis. J Med Food. 2016;19:1015-1022. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 9] [Article Influence: 1.1] [Reference Citation Analysis (0)] |