Published online Sep 14, 2019. doi: 10.3748/wjg.v25.i34.5134
Peer-review started: April 18, 2019
First decision: July 22, 2019
Revised: July 30, 2019
Accepted: August 19, 2019
Article in press: August 19, 2019
Published online: September 14, 2019
Processing time: 147 Days and 7.8 Hours
Tong Xie Yao Fang is a representative traditional Chinese prescription for the treatment of liver and spleen deficiency, abdominal pain and diarrhea. It has a unique function in the treatment of gastrointestinal dysfunction including irritable bowel syndrome (IBS), is a common functional bowel disease. Its main symptoms are recurrent abdominal pain, diarrhea, constipation or alternations between diarrhea and constipation.
There are obvious differences in metabolites between TCM syndromes. By comparing the body fluid metabolism maps of model animals, metabolomics can discover disease biomarkers, analyze the differences in metabolic pathways and understand the pathological process and the metabolic pathways of substances in the body. Thus, the evaluation of animal models tends to be comprehensive and objective. This may provide further understanding between the interaction between Tong Xie Yao Fang and the IBS model.
To evaluate the effect of Tong Xie Yao Fang on IBS rats by using metabolomics method.
Wistar rats were used to establish IBS models, and then randomly divided into four groups: A model control group and three Tong Xie Yao Fang treatment groups (high, medium and low doses). A normal, non-IBS group was established. The rats were treated for 2 wk. On days 0 and 14 of the experimental model, urine was collected for 12 h and was analyzed by ultra-performance liquid chromatography quadrupole time-of-flight mass spectrometry. Nine potential biomarkers were identified, and six major metabolic pathways were found to be related to IBS.
In the study of metabonomics, nine potential biomarkers including L-serine, 4-methylgallic acid, L-threonine, succinylacetone, prolyl-hydroxyproline, valyl-serine, acetyl citrate, marmesin rutinoside and 5-hydroxy-L-tryptophan were identified in urine, which were assigned to amino acids, organic acids, succinyl and glycosides. Furthermore, the metabolic pathway of L-serine, L-threonine and 5-hydroxy-L-tryptophan was found in the Kyoto Encyclopedia of Genes and Genomes, which mainly involved the metabolism of cysteine and methionine, vitamin B6 metabolism, serotonin synapse, tryptophan metabolism, sphingolipid metabolism, digestion, absorption of protein and amino acid metabolism. These pathways are related to intestinal dysfunction, inflammatory syndrome, nervous system dysfunction and other diseases.
Tong Xie Yao Fang has pharmacological effects on IBS, and its mechanism may be related to the metabolism of the nine potential biomarkers identified above in urine.
Core tip: Effects of Tong Xie Yao Fang on endogenous metabolites in urine of irritable bowel syndrome model rats were investigated through ultra-performance liquid chromatography quadrupole time-of-flight mass spectrometry. Tong Xie Yao Fang has the function of callback endogenous metabolite. Nine potential biomarkers were identified, and six main metabolic pathways were analyzed. They were related to neurotransmitter metabolism, inflammatory immunity, emotional changes and energy metabolism in irritable bowel syndrome disease, which may be the biological basis of irritable bowel syndrome spleen deficiency and liver hyperactivity syndrome.
- Citation: Zhao XY, Wang JW, Yin Y, Li K, Zhang M, Yan FP. Effect of Tong Xie Yao Fang on endogenous metabolites in urine of irritable bowel syndrome model rats. World J Gastroenterol 2019; 25(34): 5134-5151
- URL: https://www.wjgnet.com/1007-9327/full/v25/i34/5134.htm
- DOI: https://dx.doi.org/10.3748/wjg.v25.i34.5134
Tong Xie Yao Fang is a representative traditional Chinese prescription for the treatment of liver and spleen deficiency, abdominal pain and diarrhea. This prescription is composed of Atractylodis Macrocephalae Rhizoma (fried), Paeoniae Radix Alba (fried), Citri Reticulatae Pericarpium (fried) and Saposhnikoviae Radix (fried). It has a unique function in the treatment of gastrointestinal dysfunction including irritable bowel syndrome (IBS)[1,2].
IBS is a common functional bowel disease, and its main symptoms are recurrent abdominal pain, diarrhea, constipation or alternations between diarrhea and constipation. It is believed that the pathogenesis of IBS involves abnormal interaction between the brain and intestine and is a type of biological-psychological-social disorder. The pathogenesis of IBS is complex and varied, and its pathophysiological basis is mainly gastrointestinal motility and visceral sensory abnormalities.
Animal models of IBS are mostly duplicated from the perspective of emotion, chemical stimulation, physical stimulation and other causes. However, there is currently no unified and recognized method for animal models combining IBS with spleen deficiency and liver hyperactivity. Research in traditional Chinese medicine (TCM) and its mechanism of action related to IBS lacks systematisms and consistency, and further research is restricted. Whether the animal models reflect the cha-racteristics of IBS determines the reasonableness of the research results. Therefore, how to verify IBS in animal models has become an important factor in research. This is based on the function and responsiveness of prescriptions for various syndromes to evaluate the correlation between prescriptions and syndromes[3,4]. Prescription medicine is the carrier of syndrome differentiation and disease syndrome. We can verify syndrome with a prescription to estimate the correlation between the syndrome and the prescription[5].
However, it is worth thinking about how to expound the overall effect of prescription drugs on disease and syndromes in a comprehensive and systematic way. The complexity of a syndrome has brought many difficulties to the combination of disease and syndrome and correlations between prescription and syndrome. By studying the whole change in small molecule metabolites, metabolomics can restore the related biological events, thus revealing the essence of an organism's biological state and the mechanism of drug action. Metabolomics has the characteristics of systemic methodology such as overall dynamics, synthesis and analysis and has similar characteristics to the overall concept of TCM treatment of diseases[6,7].
There are obvious differences in metabolites between TCM syndromes[8]. By comparing the body fluid metabolism maps of model animals, metabolomics can discover disease biomarkers, analyze the differences in metabolic pathways and understand the pathological process and the metabolic pathways of substances in the body. Thus, the evaluation of animal models tends to be comprehensive and objective[9]. Prescription drugs can play a special role in some of the metabolic pathways in which these markers are located causing the metabolic network to return to normal or improve. Through the combination of metabolomics and correlation between the syndrome and the prescription theory, the mechanism and essence of the animal model are clearly defined.
Therefore, by combining systematic biology such as metabonomics with the correlation of TCM prescription and syndromes, the attributes of animal models can be clearly defined. Through the effect of the prescription on the model, the prescription is used to determine the model of the syndrome from the perspective of metabolites in the body verifying the TCM syndrome with a prescription, clarifying the mechanism and essence of the prescription and confirming the correlation between the prescription and syndrome[10]. Thus, the IBS combination model and the representative prescription can be studied as an organic system by metabolomics research methods.
In this study, we evaluated the effect of Tong Xie Yao Fang on an IBS animal model, studied the regulatory effect of the prescription on the model and clarified the difference in the regulation of endogenous metabolites in the IBS model by Tong Xie Yao Fang. Furthermore, their metabolic patterns were established by exploring the biomarkers. Based on the changing rules of substance quality in vivo, the function essence of Tong Xie Yao Fang and the syndromes essence of the IBS model were explored.
Tong Xie Yao Fang was prepared with large head atractylodes rhizome (Rhizoma Atractylodis Macrocephalae), white peony root (Radix Paeoniae Alba), dried tangerine peel (Pericarpium Citri Reticulatae) and divaricate saposhnikovia root (Radix Saposhnikoviae), which were purchased from the Second Affiliated Hospital of Heilongjiang University of Chinese Medicine and composed in 6:4:3:2 proportions. Raw components were soaked in a 10 times volume of distilled water for 0.5 h and boiled twice, first for 1.5 h and then for 1 h. Two of the boiled ingredients were filtered, mixed together and concentrated in a 1:1 ratio (100% concentration) and stored at 4 °C for later use. Tong Xie Yao Fang was diluted in distilled water to a concentration of 0.203 (clinically equivalent), 0.406, and 0.812 g/mL and stored at room temperature before use.
The following reagents were used: Acetonitrile (chromatographic grade, A998-4; Thermo Fisher Scientific, Waltham, MA, United States); methanol (chromatographic grade, CAS-67-56-1; Dikma Technologies, Foothill Ranch, CA, United States); formic acid (chromatographic grade, FS0630-015; Tedia, Fairfield, OH, United States); and distilled water (GB19298; Watsons, China).
Ultra-performance liquid chromatography quadrupole time-of-flight mass spectrometry (UPLC-Q-TOF-MS) system: Acquity Ultra type UPLC, Triple TOF 5600+ type mass spectrometer equipped with electrospray ionization (AB SCIEX, Redwood City, CA, United States), MassLynxV4.1 workstation (Waters); KDC-40 type low-speed centrifuge (Zhongjia Branch of Keda Chuangxin Co., Ltd., China); D-78532 type centrifuge (Hettich, Tuttligen, Germany); Vortex3000 type whirl mixer (Wiggens, Germany); Academic UPW SYSTEM (Milli-Q, United States); Forma 995 type ultra-low temperature refrigerator (Thermo Fisher Scientific); B3200S-T type ultrasonic oscillometer (Branson Ultrasonics Corporation, Shanghai, China); KDC-160HR type high speed tabletop refrigerated centrifuge (Zhongjia Branch of Keda Chuangxin, China); SK-1 type swift mixer (Jiangsu Medical Instrument Factory, China); cp2465 type angioplasty balloon (EV3, United States); E206Fr type children catheter (3 mL; Shenyang Bosilin Medical Instrument Co., Ltd., China); and DYM type segmental epidural catheter (1.0 × 1; Yangzhou Huaxia Medical Device Co., Ltd., China).
This study was approved by the Ethics Committee of the Heilongjiang University of Chinese Medicine. All animal experimental procedures were performed in accordance with the Regulations for the Administration of Affairs Concerning Experimental Animals approved by the State Council of People’s Republic of China. Wistar female and male rats (clean grade), aged 8 d and body weight 11 ± 2 g, were purchased from Heilongjiang University of Chinese Medicine (HDZD P00102006). The mother rats and their newborn rats were fed in the cage together, and they had free access to food and water at room temperature of 21-24 °C with humidity of 50%-60%. By using the rectal dilatation stimulation method[11] combined with the mother and offspring separation method[12] for the newborn rats from age 8 to 12 d, the angioplasty balloon (15 mm long) was inserted into the rectum 2 cm from the end of the balloon to the anus, and the intestinal tract was slowly dilated. The operation was performed twice daily for 1 min each time and at an interval of 30 min. On days 13-17, the rectum was dilated by balloon angioplasty (20 mm long). On days 18-21, the catheter for children was used to expand the rectum, and 0.1 mL water was injected without changing other conditions. After rectal dilatation every day, neonatal rats were placed in cages separated from the maternal rats for 1 h, and then put back into the cages with the maternal rats. After modeling for 2 wk, the abdominal withdrawal reflex model was used to evaluate the success of the IBS model. IBS model rats were randomly divided into four groups by weight with ten rats in each group: A model group (M) and groups treated with high-, medium- and low-dose Tong Xie Yao Fang denoted as G, Z and D groups, respectively. Another ten rats were used as the normal group (K). The rats for G, Z and D groups were given 8.12, 4.06, and 2.03 g/kg Tong Xie Yao Fang decoction, respectively. The rats in the normal group and model group were given with same amount of saline. All groups were treated once daily for 2 wk.
On days 0 and 14 of the experimental model, urine was collected for 12 h, and then centrifuged at 4 °C at 13000 r/min for 10 min. The supernatant was collected as the urine samples and stored in a -80 °C freezer until use. Urine samples were unfrozen at normal temperature. Next, 100 μL urine was centrifuged at 4 °C at 10000 r/min for 10 min, and the supernatant was absorbed into a glass sample bottle.
Metabolomics data were measured by UPLC-Q-TOF-MS. Chromatographic conditions were as follows: Rapid resolution chromatographic column (2.1 mm × 100 mm, 1.8 μm); flow rate: 0.4 mL/min; column temperature: 30 °C; detector scanning range: 190-400 nm; detection wavelength: 210, 254 and 280 nm; injection volume: 2 μL; mobile phase: 0.1% formic acid aqueous solution (A) and -0.1% formic acid acetonitrile solution (B); gradient elution: 0-3 min, 98%-48% A, 3-10 min, 48%-2% A, 10-12 min, 2%-98% A, 12-14 min and 98% A. Mass spectrometry (MS) conditions were as follows: Positive/negative ion primary MS with electrospray ion source and online mass correction with LockSprayTM correction system; scanning detection: m/z 50-1500; scanning time: 0.2 s; capillary voltage: 3.0 kV; cone voltage of sample: 35 V; extraction voltage: 4.0 V; ion source temperature: 120 °C; desolvent temperature: 350 °C; cone gas flow: 50 L/h; desolvent nitrogen flow: 650 L/h; and impact energy: 6-30 V.
The data were processed using SPSS version 17.0 software and expressed as mean x ± standard deviation. On the basis of evaluating the variance of the original data in accordance with normal distribution, the differences between groups were compared by single factor ANOVA, and the differences between groups were analyzed by t-test. P < 0.05 meant that the difference was statistically significant.
The determined MS data of urine metabolism profile were obtained by data dimension reduction and MS matrix information using Marker lynx software. Data were analyzed by unsupervised principal component analysis (PCA) of ssLynxV4.1 workstation software, and PCA score chart was obtained to reflect the clustering degree of each group. Orthogonal partial least squares discriminant analysis (OPLS-DA) was used to obtain the OPLS-DA score chart reflecting the contribution rate of the metabolic contour and to draw the scores plot. The farther the distance points in the load diagram, the greater the contribution of ions to the metabolic contour trajectory. The metabolic group map of each group was analyzed by pattern recognition, and the observed values of each group were distinguished. The measurement data were collected for statistical analysis. Potential biomarkers were screened out based on variable importance in projection (VIP) and VIP confidence interval estimation. Ions of VIP > 1.5 were taken for comparison among groups, and the t test was used for inter-group difference. P < 0.05 was considered as the screening condition to obtain potential biomarkers. Secondary MS analysis was conducted for the biomarkers. The structural analysis of the biomarkers was carried out based on its relative molecular mass and molecular group structure. Based on the results of the analysis, the biological significance of biomarker information retrieval and the metabolic pathway of biomarkers were analyzed and explained using the human metabolic group database, Scripps Metabolic and Mass Spectrometry Center, Kyoto Encyclopedia of Genes and Genomes and published literature. Thus, the core biomarkers closely related to the occurrence and development of IBS model were screened according to the literature.
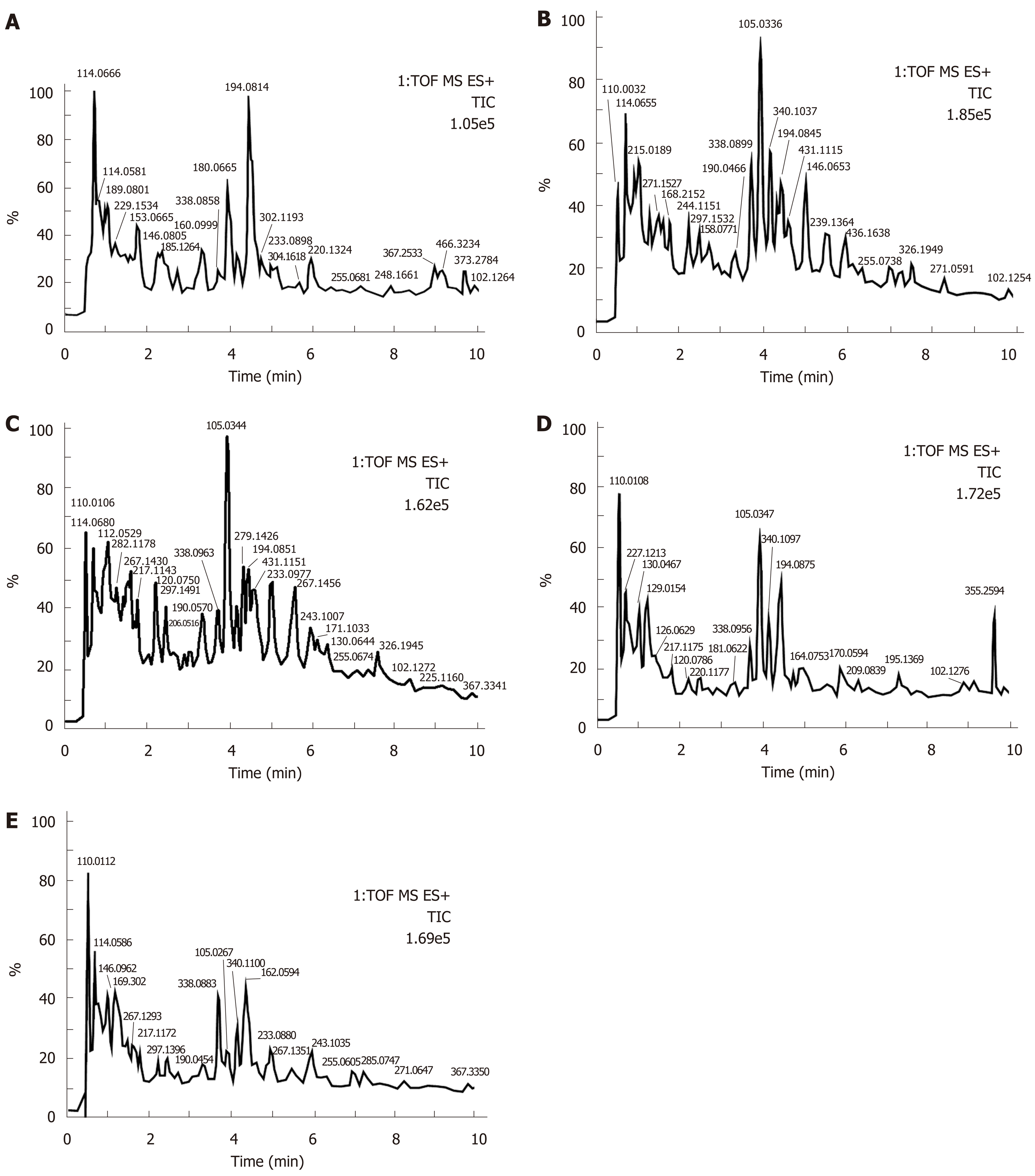
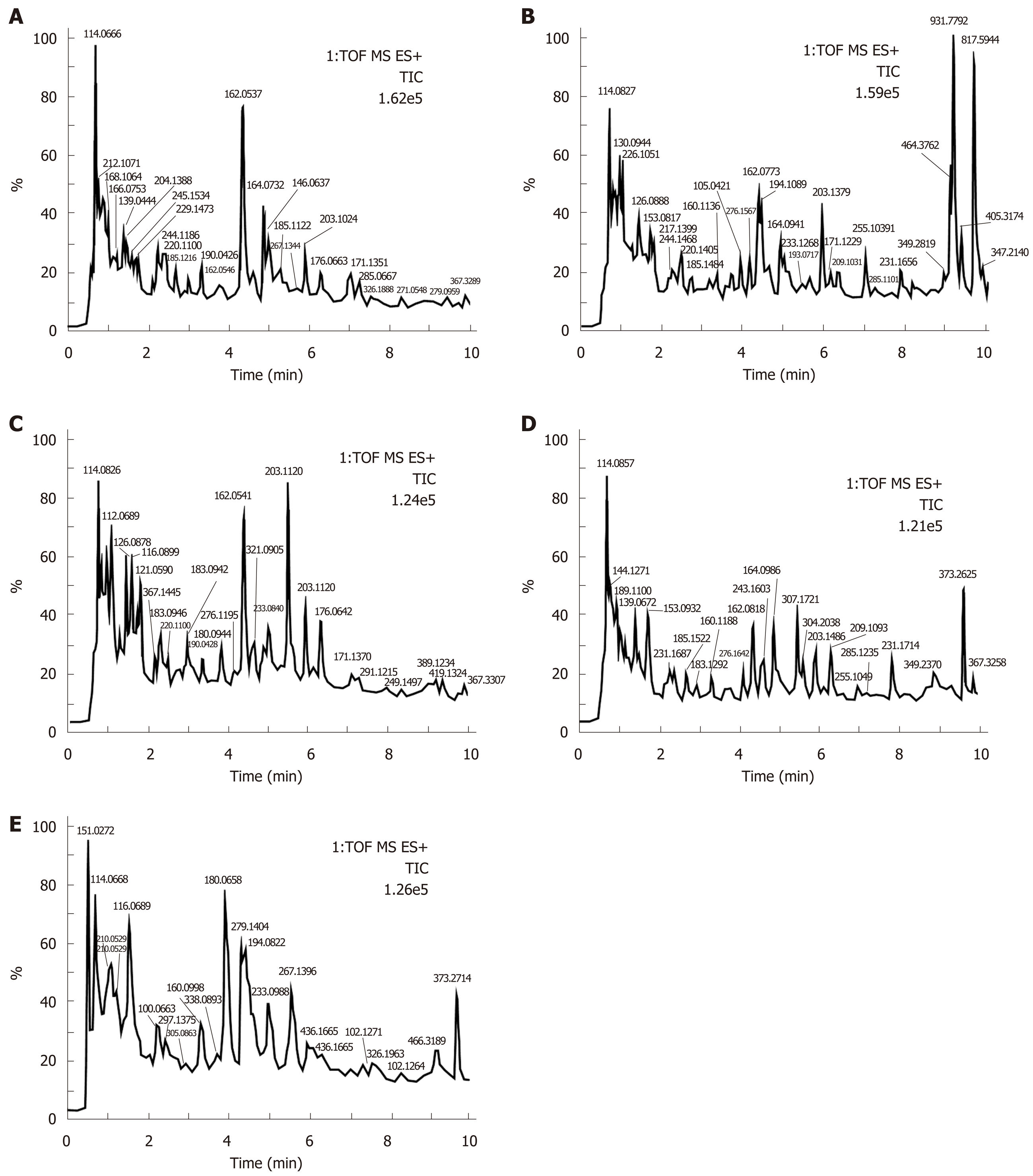
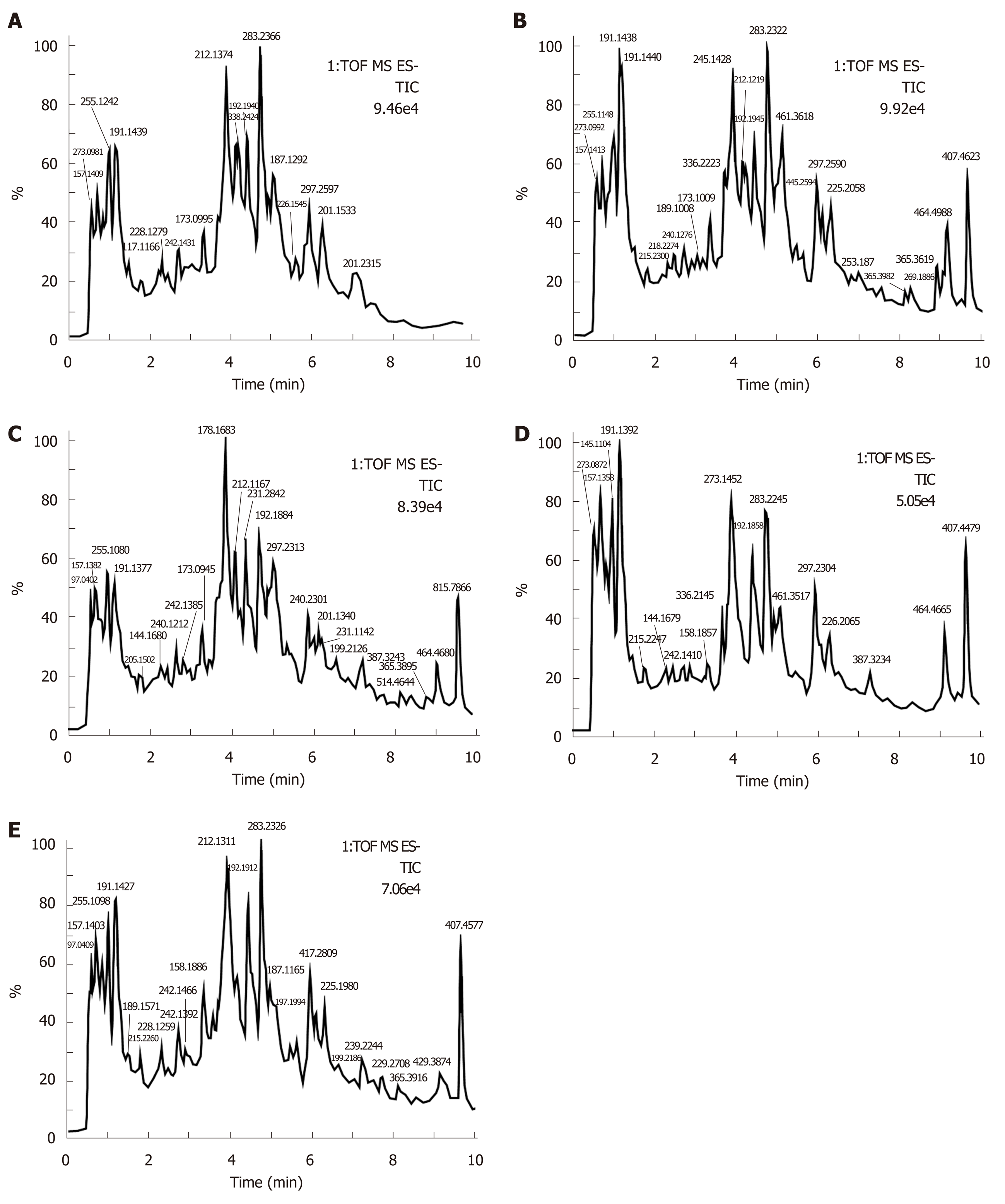
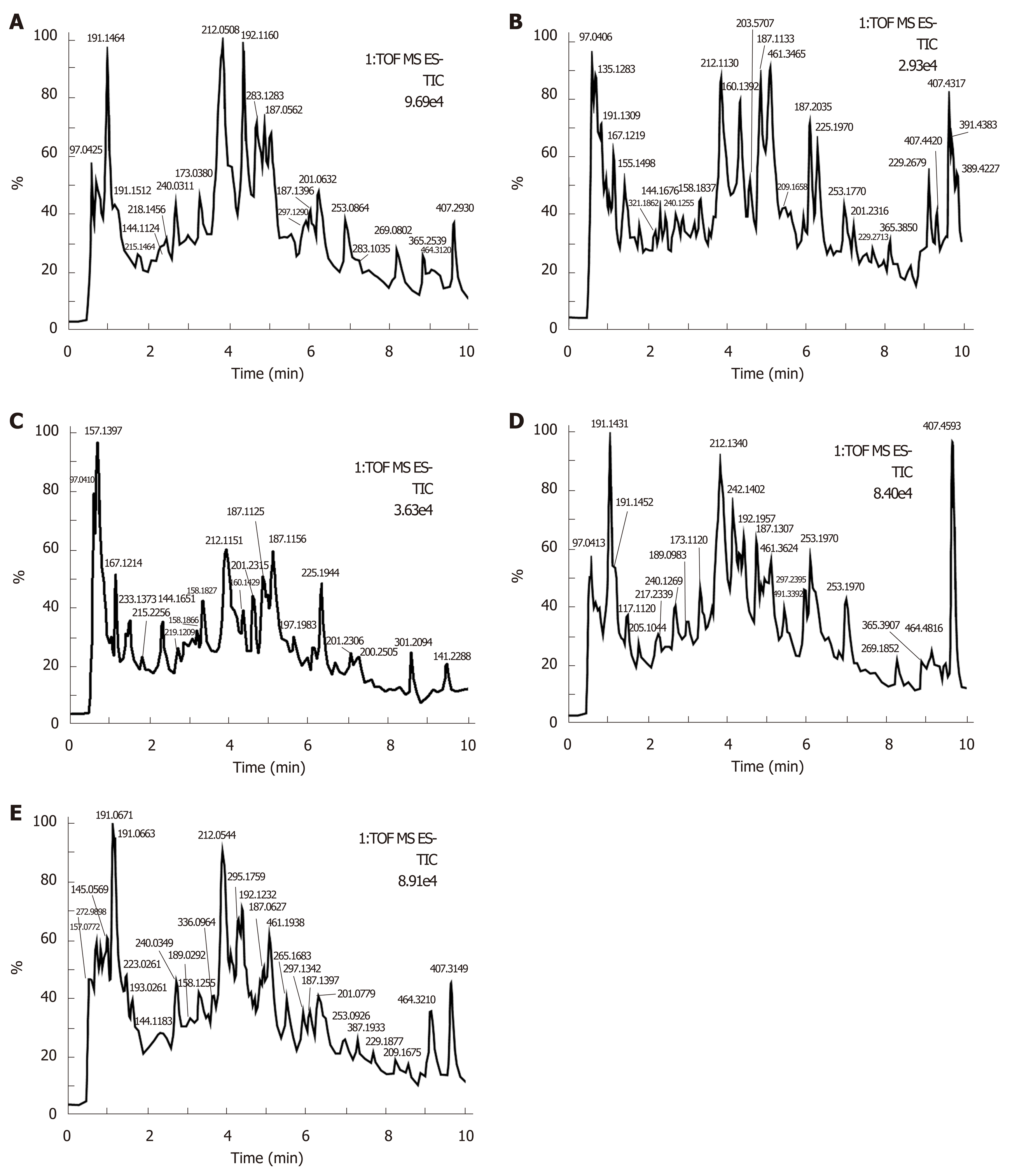
Urine samples of rats on days 0 and 14 were analyzed based on the optimized analysis conditions of UPLC-Q-TOF-MS. In the positive and negative ion scanning mode, the urine samples were scanned and analyzed within a set mass range, and base peak ion of the mass spectrum profile was obtained (Figures 1-4). The urine samples from the different groups had a better differentiation degree and different metabolite spectrum showing better separation and response effect.
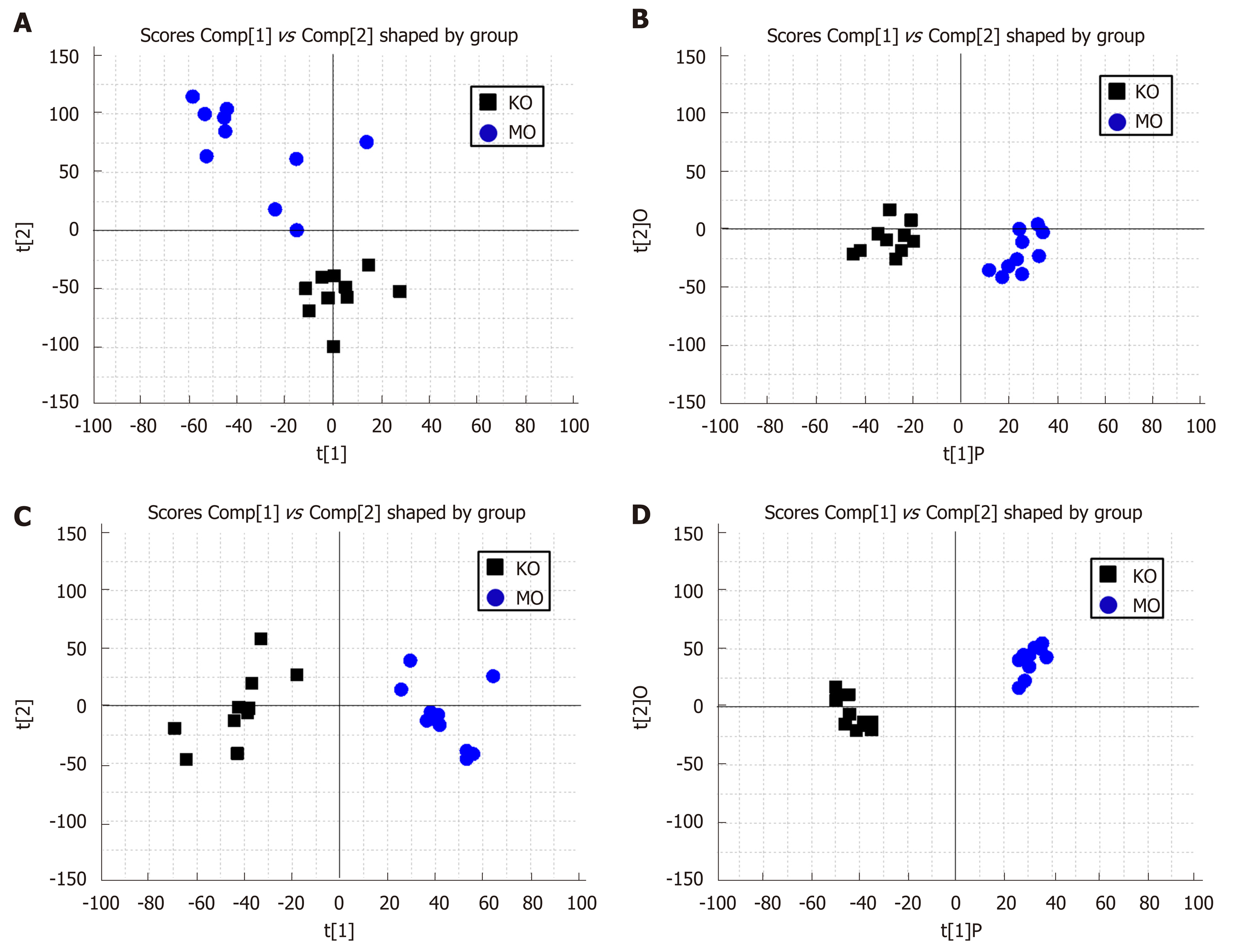
Urine metabolomics study of IBS disease model: The PCA and OPLS-DA score charts are shown in Figure 5 and Figure 6. There was no overlap of data points in urine of IBS model rats compared with that of the normal control group, and the data was obviously classified in a different quadrant. The obvious separation status in score plots suggested that the urine metabolism in two groups was distinguished well. This indicated that there was an obvious difference in metabolites of rats between the normal group and IBS model group. Before and 14 d after medication, the separation in the two score charts was relatively obvious, indicating that the IBS model rats were stable within 14 d.
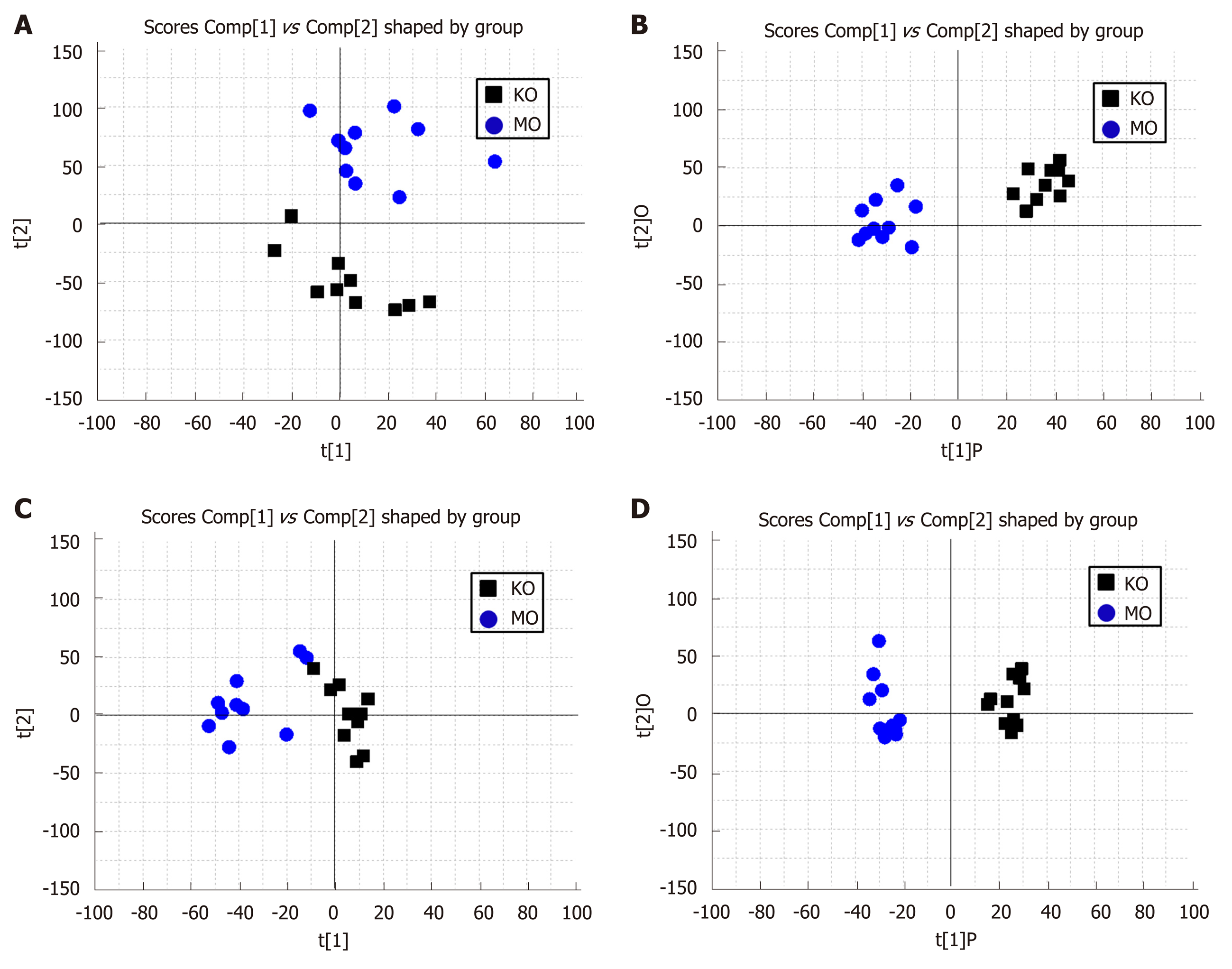
Urine metabolomics study on intervention of Tong Xie Yao Fang on adaptive IBS disease model: The PCA and OPLS-DA score charts are displayed in Figure 7. Compared with Tong Xie Yao Fang groups, the data points for urine in IBS rats (0 d) have overlap and were clearly classified in the same quadrant, showing unseparated state in the score charts. The metabolites in the model group and Tong Xie Yao Fang groups were the same induction by rectal dilatation and maternal separation stimulation, indicating successful modeling of IBS. Compared with the normal group, the data points for urine in IBS model rats and Tong Xie Yao Fang groups exhibited no overlap and were clearly classified in different quadrants, showing obvious separation state in score plots and well-distinguished well metabolism. This indicated that after modeling of rats, there were obvious differences in metabolites between IBS rats and normal rats, and the metabolite component in the urine showed significant changes.
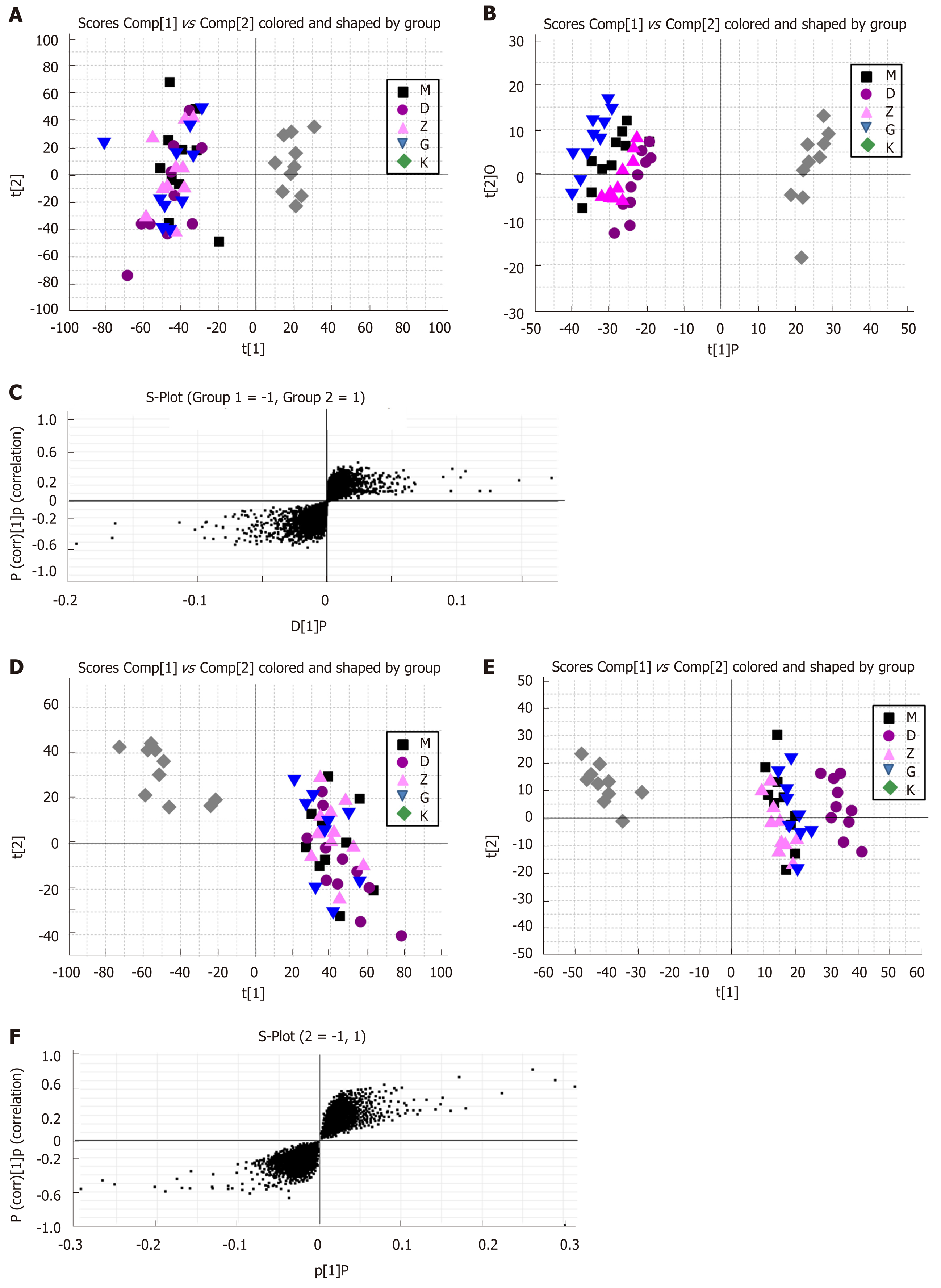
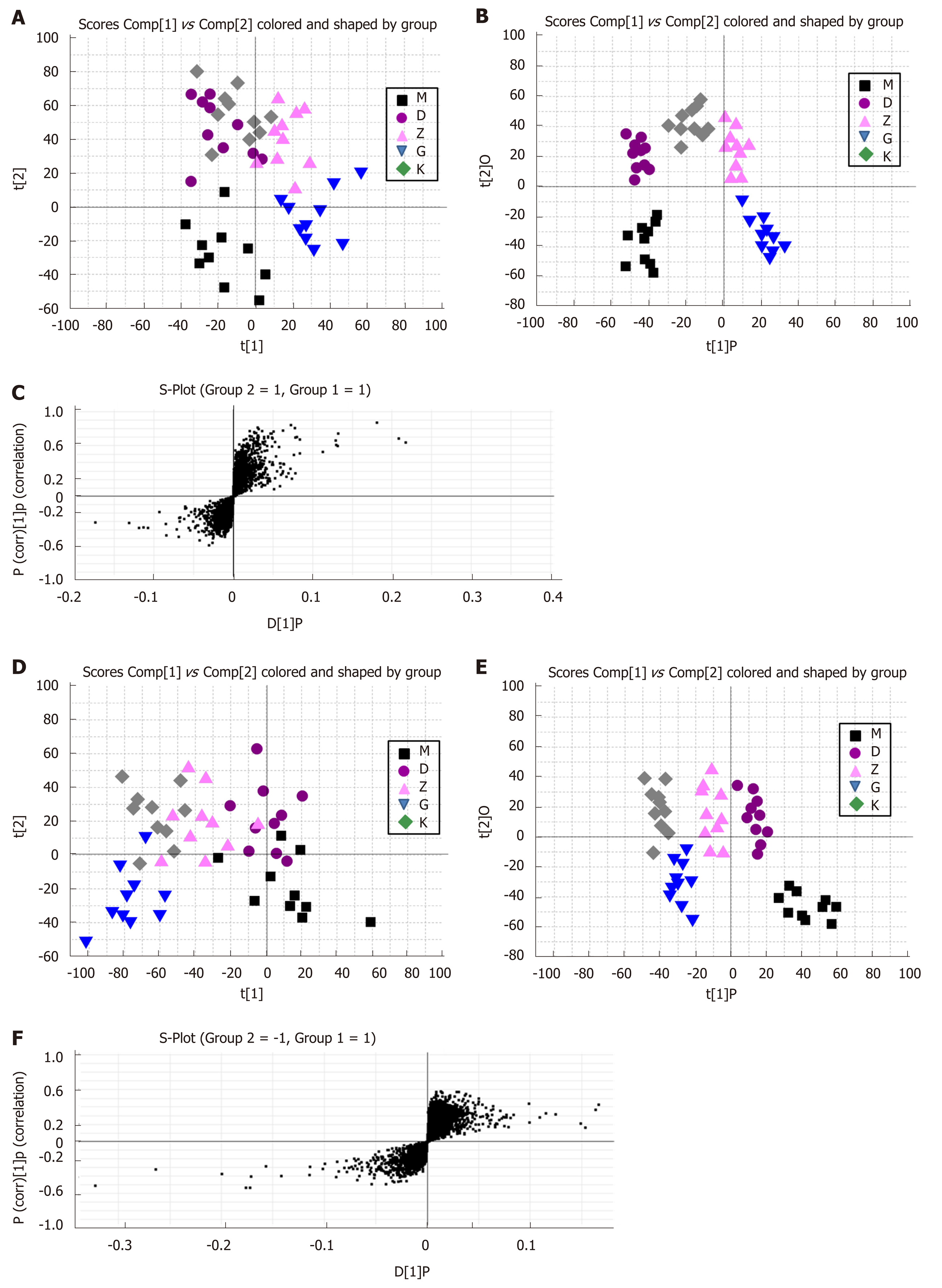
The PCA and OPLS-DA score plots are shown in Figure 8. The data points for urine in the IBS model rats and Tong Xie Yao Fang groups treated for 14 d were dispersed and clearly classified in different quadrants, showing separation in score plots and distinct urine metabolism. The results illustrate that the metabolic products have obvious changes after treatment with Tong Xie Yao Fang in the IBS model rats compared with the model control group. Tong Xie Yao Fang treatment groups showed separation in score plots, but the degree of differentiation was not obvious. The distribution of data points in the medium-dose and high-dose groups was similar to that of the normal group.
Further research showed that the urine samples of rats in each group showed complete separation status in the 2D space of the PCA score chart under the condition of positive and negative ions. This indicated that physiological function was changed by rectal distention and maternal separation stimulation. This reflected changes in urine metabolic profile of rats as well as liver stagnation and spleen deficiency syndrome of IBS and metabolic characterization of Tong Xie Yao Fang treatment. The scores chart for evaluating the contribution of the metabolic profile grouping was obtained by analyzing the metabolic profile of samples with OPLS-DA. In addition, pattern recognition analysis was conducted for metabolomics profiles of urine samples. As shown in Figures 5-7, the data points in each group exhibited no/less overlap, indicating that there were differences among the groups. Based on VIP and VIP confidence interval, the potential biomarkers were evaluated.
Potential biomarkers were screened according to VIP, and the differential variables with VIP > 1.5 were selected. The screened differential variables were verified by Anova, and the differential variables with P < 0.05 were considered potential biomarkers.
Based on the obtained identification results of molecular ion fragments, nine kinds of biomarkers in urine were identified through the human metabolic group database and METLIN, which are related to the metabolites of the Tong Xie Yao Fang treating IBS and showing a certain uptrend or downtrend. These biomarkers belong to amino acids, organic acids, succinyl and glycosides. Meanwhile, the metabolic pathways of L-serine, L-threonine and 5-hydroxy-L-tryptophan (5-HTP) can be searched in the Kyoto Encyclopedia of Genes and Genomes (Table 1). These pathways mainly include cysteine and methionine metabolism, vitamin B6 metabolism, serotonin synapse, tryptophan metabolism, sphingolipid metabolism, protein digestion and absorption and amino acid metabolism (Table 1 and Table 2).
| No. | HMDB ID | Retention time/min | M/Z | Chemical formula | VIP | Select the ions | Common name | Expression trend | |||
| M vs K | G vs M | Z vs M | D vs M | ||||||||
| 1 | HMDB00187 | 3.854 | 105.04 | C3H7NO3 | 2.00494 | [M + H]+ | L-serine | ↑ | ↓ | ↓ | ↓ |
| 2 | HMDB13198 | 8.663 | 184.04 | C8H8O5 | 4.85675 | [M-H] + | 4-methylgallic acid | ↑ | ↓ | ↓ | ↓ |
| 3 | HMDB00167 | 3.204 | 119.06 | C4H9NO3 | 3.76891 | [M + H]- | L-threonine | ↓ | ↑ | ↑ | ↑ |
| 4 | HMDB00635 | 2.915 | 158.06 | C7H10O4 | 8.66271 | [M-H]- | Succinylacetone | ↑ | ↓ | ↓ | ↓ |
| 5 | HMDB29018 | 1.084 | 228.11 | C10H16N2O4 | 5.22312 | [M + H]+ | Prolyl-hydroxyproline | ↑ | ↓ | ↓ | ↓ |
| 6 | HMDB29136 | 4.445 | 204.11 | C8H16N2O4 | 4.11234 | [M + H]- | Valyl-serine | ↓ | ↑ | ↑ | ↑ |
| 7 | HMDB59808 | 4.954 | 232.02 | C8H8O8 | 2.23843 | [M + H]+ | Acetyl citrate | ↓ | ↑ | ↑ | ↑ |
| 8 | HMDB41413 | 7.827 | 554.20 | C26H24O13 | 9.34210 | [M + H]+ | Marmesin rutinoside | ↑ | ↓ | ↓ | ↓ |
| 9 | HMDB00472 | 1.213 | 220.08 | C11H12N2O3 | 5.13710 | [M + H]- | 5-hydroxy-L-tryptophan | ↑ | ↓ | ↓ | ↓ |
| No. | Common name | Metabolic pathway ID | Metabolic pathway name |
| 1 | L-serine | map00270 | Cysteine and methionine metabolism |
| map00600 | Sphingolipid metabolism | ||
| map04974, map01230, map00260 | Protein digestion and absorption; biosynthesis of amino acid; glycine, serine and threonine metabolism | ||
| 2 | L-threonine | map00750 | Vitamin B6 metabolism |
| map04974, map01230, map00260 | Protein digestion and absorption; biosynthesis of amino acid; glycine, serine and threonine metabolism | ||
| 3 | 5-hydroxy-L-tryptophan | map04726 | Serotonergic synapse |
| map00380 | Tryptophan metabolism |
Metabonomics is the systematic scientific study of metabolic product changes and their ability to reveal the metabolic nature of the life activities of an organism. After the effect of changes in external conditions on the overall state of the body, the effect of the external environment on the metabolites is studied by taking all the small molecular substances as the observation target. Metabolomics is an important research method of systems biology, which has the characteristics of measuring overall metabolic dynamics, synthesis and analysis. It studies the metabolic changes in metabolism and metabolites caused by drugs. The changes in endogenous metabolites can directly reflect the changes in biochemical processes in vivo. Drugs have specific effects on certain processes of metabolic pathways involved with the main biomarkers, which causes marked changes in the endogenous metabolites[9]. Metabonomics has the technical characteristics of overall comprehensive information representation and analysis of provenance. By detecting the metabolic fingerprints of body fluids and analyzing the causes of metabolic spectrum changes, the changes in endogenous metabolites induced by drugs can be studied, and the role of Chinese medicines in metabolic regulation and their exact mechanism of action can be explored. Thus, it may clarify the relationship between compound prescriptions and disease syndromes.
Tong Xie Yao Fang was first recorded in “Danxi Xinfa”·cathartic volume, which is used to treat diarrhea with pain caused by spleen deficiency and liver hyperactivity. Liver and spleen deficiency syndrome is due to liver drainage, spleen-soil deficiency, transversely invading spleen and spleen transport dereliction of duty. Tong Xie Yao Fang can tone the spleen, clear damp, stop diarrhea, knead liver to soothe qi and relieve pain and make the spleen healthy and liver soft. Then, the pain and diarrhea are resolved.
At present, the rectal distention stimulation of the suckling rat is a widely used method and the most reasonable animal model for IBS, which is a method of local mechanical stimulus. Mother/child separation is an early life event that can simulate emotional anxiety and causes increased stress response and visceral hyper-sensitivity[13]. Our research group reproduced the IBS model by combining the above two methods. Tong Xie Yao Fang had a significant effect of tonifying the spleen and liver stagnation on the IBS model derived from the combination of rectal distention and mother/child separation of neonatal rats. The model symptoms were spleen deficiency and liver hyperactivity and were related to the prescription of Tong Xie Yao Fang and syndrome.
In this study, the metabonomics of IBS rat urine was studied by UPLC-Q-TOF-MS analysis combined with Mass Lynx software. Compared to the metabolic results of the normal group, the contents of L-serine, succinylacetone, proline-hydroxyproline, valyl-serine, marmesin rutinoside and 5-hydroxy-L-tryptophan (5-HTP) increased while the contents of L-threonine and acetyl citrate decreased in the Tong Xie Yao Fang treatment groups and the model group,. Tong Xie Yao Fang decreased the contents of L-serine, succinylacetone, proline-hydroxyproline, valyl-serine, marmesin rutinoside and 5-HTP and increased the contents of L-threonine and acetyl citrate. The metabolic pathways involved serotonin synapse, tryptophan metabolism, cysteine and methionine metabolism, vitamin B6 metabolism, sphingolipid metabolism and biosynthesis of proteins and amino acids. The metabolic biomarkers may be L-serine, 5-HTP, L-threonine, valyl-serine and acetyl citrate. Therefore, it is speculated that the regulatory mechanism of Tong Xie Yao Fang may involve the following aspects.
Serotonin (5-HT) escapes from presynaptic cells and transmits information to postsynaptic cells, thus acting as a neurotransmitter. 5-HTP is involved in the serotonin synapse pathway and tryptophan metabolism. In this pathway, 5-HTP is primarily involved in serotonin synthesis. 5-HTP is converted from the tryptophan hydroxylase through tryptophan followed by decarboxylation to synthesize 5-HT. 5-HT is a neurotransmitter that widely exists in the nervous system and gastrointestinal tract and participates in the regulation of psychological and neural functions. As a signal transduction molecule, it can be an important neurotransmitter in the brain-gut axis[14]. 5-HT in the digestive tract can enhance the sensitivity of the gastrointestinal splanchnic nerves, regulate the movement of the gastrointestinal tract and participate in the regulation of intestinal sensation, secretion and movement. 5-HT in the central nervous system can cause mental and behavioral disorders and regulate mood and sleep. 5-HT signaling disorder is closely related to IBS, and both physiological and pathological stimuli can lead to an increase in 5-HT release. Studies have shown that the sensory hypersensitivity in IBS patients may be related to increased sensitivity of visceral afferent nerves, increased excitability of spinal dorsal horn neurons and changes in central sensory regulation. The change in 5-HT level is closely related to the occurrence and development of many complex diseases and syndromes, including IBS and plays a dominant role in its pathogenesis. High concentrations of 5-HT can enhance the sensitivity to external stress of visceral afferent nerve endings and the enteric nervous system and then stimulate the release and secretion of various neurotransmitters, stimulate and expand the activity and participate in the biochemical signaling process of brain-gut interaction.
A previous study showed that the content of 5-HT in the brain-gut axis of IBS model rats was significantly higher than that in the normal group, which also confirmed the view that an increase in 5-HT level is an important part of the pathogenesis of IBS. The increase of 5-HTP metabolism in the urine of IBS model rats indicates that there are pathological mechanisms of abnormal secretion, release and metabolism of 5-HT in the IBS model, which is consistent with previous studies[15]. Tong Xie Yao Fang can reduce the 5-HTP content in urine. Tong Xie Yao Fang may be involved in the regulation of IBS visceral hypersensitivity and gastrointestinal motility by regulating 5-HT metabolism and synapses to relieve IBS in model rats. It is suggested that the improvement of spleen deficiency and liver hyperactivity of IBS by Tong Xie Yao Fang is related to the regulation of the serotonin synaptic pathway and tryptophan metabolism.
Halfcystine (Hcy) is synthesized from methionine and L-serine via cystathionine, which is the intermediate product of the cysteine and methionine metabolism. Hcy has high biological activity and is involved in a variety of inflammatory and immune disorders. Studies have shown that mild inflammation and immune activation of intestinal mucosa also play a key role in the pathogenesis of IBS. Hcy is closely related to IBS inflammatory immune pathogenesis[16]. Impaired intestinal barrier function plays an important role in the pathogenesis of IBS. Hcy can produce a large number of oxidative free radicals that damage the intestinal mucosal mechanical barrier[17] and changes intestinal permeability, leading to massive invasion of inflammatory factors and aggravation of IBS pathophysiology[18]. Inflammatory factors such as Hcy and tumor necrosis factor-α (TNF-α) promote each other in the process of inflammatory immunity, aggravating the inflammatory response[19].
In addition, the content of Hcy is positively correlated with the incidence of depression. IBS patients are often accompanied by depression, anxiety and other psychological disorders. The hypothesis of the pathophysiology of the biological-psychological- sociological model of IBS emphasizes the importance of emotional disturbance in the pathogenesis of IBS[20]. Psychological stress may alter systemic and intestinal immunity. The dispose of central pivot on mental disorders and stimulation of visceral injury may involve brain-gut axis dysfunction. Experimental studies have shown that the consumption of sugar and water and the open field test were improved in rats after the intervention of Hcy metabolic coenzyme, indicating that the level of Hcy is related to anxiety-like behavior or depression-like behavior in IBS rats. The content of Hcy decreases and anxiety-like behavior or depression-like behavior is also reduced[16]. Therefore, it can be inferred that Hcy is closely related to not only IBS inflammatory immune response but also psychological stress such as IBS-related depression.
As a key substrate for the metabolism of sulfur transfer in Hcy, L-serine content increases in the urine of IBS model rats, suggesting abnormality of the metabolic pathway of Hcy sulfur transfer in IBS rats. The abnormal metabolism of L-serine in the process of IBS indicates that L-serine is involved in the pathophysiological process. It is suggested that Tong Xie Yao Fang regulates cysteine and methionine metabolism through L-serine and improves the intestinal reaction and emotional changes of IBS. Tong Xie Yao Fang improves liver hyperactivity syndromes such as emotional depression, irritability, abdominal pain, abdominal distension and borborygmus of IBS rats, which is related to regulation of the cysteine and methionine metabolism pathways embodying the effects of “restricting” the liver.
L-threonine is involved in the metabolism of vitamin B6. O-phospho- 4-hydroxy-L-threonine can be converted to 4-hydroxy-L-threonine by the enzyme to form pyridoxine, and pyridoxal and pyridoxamine can be transformed into each other. Vitamin B6 is involved in the formation of serotonin, which can increase the serotonin concentration. Additionally, vitamin B6 as a coenzyme participates in various metabolic reactions such as amino acids and proteins. Lack of vitamin B6 can lead to the stagnation of protein hydrolysis and conversion to fat, thus stopping growth. The level of L-threonine amount increases after taking Tong Xie Yao Fang, enhancing vitamin B6 synthesis, increasing the serotonin content and promoting the protein metabolism.
L-serine is involved in the synthesis of sphingolipids. Sphingolipids and their metabolites play an important role in maintaining cell growth and signal transduction. Ceramide is the simplest structure of sphingolipid, the precursor of synthetic complex sphingolipid, which is an intermediate in the metabolic and transformation pathway[21]. Sphingolipids can regulate immune function and inflammatory response. TNF-α can directly result in the production and release of ceramide from mitochondria[22]. It has been demonstrated that the clinical symptoms of IBS are associated with low inflammatory response. Many researchers have reported that TNF-α plays a major role in the development of IBS inflammatory immune response[23,24]. TNF-α is a pro-inflammatory cytokine with various biological activities. It interacts with other cytokines to induce or increase the production of inflammatory mediators and participates in the development of inflammatory immune responses. The level of L-serine decreases after treatment with Tong Xie Yao Fang, which indicates that the content of ceramide synthesized by L-serine is reduced, and the inflammatory immune response of IBS is alleviated. The mechanism may be related to the reduction of pro-inflammatory factor TNF-α involved in the inflammatory immune response.
L-serine and L-threonine are also involved in the biosynthesis of proteins, amino acids and sugars. Energy metabolism is the release, transfer and utilization of energy produced in metabolic processes and is closely related to the theory of “spleen governing movement transformation” that is an important part of the spleen-stomach doctrines in TCM. L-threonine can promote growth and improve immune function. Serine plays a role in the metabolism of fats and fatty acids, the growth of muscles and maintains the immune system. As a tricarboxylic acid substrate, acetyl citrate participates in the tricarboxylic acid cycle as a source of energy. It is suggested that IBS rats have the disturbance of energy metabolism, immune dysfunction and growth inhibition, which are characteristics of spleen deficiency syndrome in TCM. In addition, L-serine and L-threonine are involved in amino acid metabolism. Tong Xie Yao Fang can increase or decrease the related metabolites and make the metabolic network return to normal or improve, indicating that Tong Xie Yao Fang can improve the energy metabolism from sugar and amino acid metabolism in IBS spleen deficiency syndrome. These results suggest that Tong Xie Yao Fang can improve the body spleen deficiency and other spleen deficiency syndromes in IBS rats, enhance energy metabolism and regulate immune function, which reflects the function of tonifying spleen.
In summary, endogenous metabolites evidently change after the replication of IBS model with Tong Xie Yao Fang treatment. The identified metabolic pathways include serotonin synapse and tryptophan metabolism, cysteine and methionine metabolism, vitamin B6 metabolism, sphingolipid metabolism and biosynthesis of proteins, amino acids and sugars. Due to the complexity of regulation, we do not fully understand the biological significance of abnormal expression of endogenous metabolites. However, the results suggest that the abnormal characteristics of metabolites might form the biological basis of liver hyperactivity and spleen-deficiency syndrome in IBS models. Tong Xie Yao Fang plays a complex role in regulating endogenous metabolites related to the syndrome of liver and spleen deficiency, representing the effects of supporting the spleen and restricting the liver.
The establishment of disease and syndrome combined with animal model in traditional Chinese medicine (TCM) is an important link to realize the objectiveness, standardization and scientificity of TCM. At present, the model construction method of the disease and syndrome combination for irritable bowel syndrome (IBS) is mainly based on the modern medical disease animal model combined with syndrome related etiology and disease mechanism. There are obvious differences in metabolic products among TCM syndromes. Metabonomics finds biomarkers of diseases by comparing the metabolic profiles of animal body fluids, analyzing the differences of metabolic pathways and understanding the pathological process and metabolic pathways of substances in the body. Thus, the evaluation of animal models tends to be comprehensive and objective. Therefore, through the combination of metabonomics and other systems biology with TCM prescription syndrome, we can clearly define the attributes of animal model syndrome. Through identical formulas, different models and different formulas, we can determine the model of syndrome from the perspective of metabolic products in vivo, clarify the mechanism and essence of prescriptions and drugs and clarify the correlation between prescriptions and syndromes. This research idea not only conforms to the research requirements of TCM prescriptions and syndromes but also follows the regularity between phenomena and essence in modern science.
Tong Xie Yao Fang is effective in the treatment of IBS. The overall concept of TCM theory and the treatment of evidence differentiation require that the clinical differentiation of IBS must be accurate. Therefore, the establishment of a syndrome-binding IBS model is the key to research of IBS in TCM. In recent years, the study of disease syndrome combined with animal model has developed rapidly and has become a new direction of animal model development in TCM research. At present, many scholars have provided a suitable combination model of disease and syndrome for the study of TCM in the treatment of IBS, which reflects the advantages of TCM on IBS syndrome differentiation. Therefore, in the aspect of disease and syndrome combination model replication, it is closely related to the advanced research methods of modern medicine. Through the combination of metabonomics and other system biology with TCM prescription syndrome, the attributes of IBS disease syndrome combined with animal model syndrome can be clearly defined. Through the improvement of the construction method and train of thought of the disease syndrome model, a more mature disease syndrome combined with animal model would be obtained, and the scientific connotation of TCM will be expounded.
The research objective is to discover the biomarkers of Tong Xie Yao Fang and establish its metabolic model characteristics through its influence on metabolites of IBS. The action essence of Tong Xie Yao Fang and the syndrome essence of its disease model are explored based on the changing law of substance quality in vivo.
In this study, Wistar rats were used to establish the IBS models, and then randomly divided into four groups: Model control group, Tong Xie Yao Fang treatment groups (high, medium, low doses). A normal, non-IBS group was established. The rats were treated for 2 wk. On days 0 and 14 of the experimental model, urine was collected for 12 h and was analyzed by ultra-performance liquid chromatography quadrupole time-of-flight mass spectrometry. Nine potential biomarkers were identified, and six major metabolic pathways were found to be related to IBS.
In the study of metabonomics, nine potential biomarkers including L-serine, 4-methylgallic acid, L-threonine, succinylacetone, prolyl-hydroxyproline, valyl-serine, acetyl citrate, marmesin rutinoside and 5-hydroxy-L-tryptophan were identified in urine, which were assigned to amino acids, organic acids, succinyl and glycosides. Furthermore, the metabolic pathway of L-serine, L-threonine and 5-hydroxy-L-tryptophan was found in the Kyoto Encyclopedia of Genes and Genomes, which mainly involved the metabolism of cysteine and methionine, vitamin B6 metabolism, serotonin synapse, tryptophan metabolism, sphingolipid metabolism, digestion and absorption of protein and amino acid metabolism. These pathways are related to intestinal dysfunction, inflammatory syndrome, nervous system dysfunction and other diseases. However, due to the complexity of regulation, we do not fully understand the biological significance of abnormal expression of endogenous metabolites.
The endogenous metabolites changed significantly for the IBS model after the intervention of Tong Xie Yao Fang. Tong Xie Yao Fang plays a complex regulatory role in endogenous metabolites associated with liver spleen deficiency syndrome. It is suggested that the improvement of spleen deficiency and liver hyperactivity of IBS by Tong Xie Yao Fang is related to the regulation of the serotonin synaptic pathway and tryptophan metabolism. It was confirmed that the rectal dilatation stimulation combined with maternal-infant separation of IBS animal model was the best model for the adaptation of Tong Xie Yao Fang. In this study, through metabonomics related research on Tong Xie Yao Fang, endogenous metabolites in animal models were evident, suggesting the importance of syndrome differentiation and treatment of clinical syndrome in TCM.
Metabonomics, genomics, transcriptome, and proteomics have the characteristics of systematic methodology such as overall dynamics, synthesis and analysis and are similar to the overall concept of TCM in the treatment of diseases. By means of systematic biology research method, prescriptions and syndromes can be integrated into an organic system for research. Therefore, the subject not only meets the research requirements of prescriptions and syndromes in TCM but also conforms to the regularity of the relationship between phenomena and essence in modern science.
Manuscript source: Unsolicited manuscript
Specialty type: Gastroenterology and hepatology
Country of origin: China
Peer-review report classification
Grade A (Excellent): 0
Grade B (Very good): B
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Tarantino G, Soares RLS S-Editor: Ma RY L-Editor: Filipodia E-Editor: Zhang YL
| 1. | Bian Z, Wu T, Liu L, Miao J, Wong H, Song L, Sung JJ. Effectiveness of the Chinese herbal formula TongXieYaoFang for irritable bowel syndrome: a systematic review. J Altern Complement Med. 2006;12:401-407. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 47] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 2. | Yin Y, Zhong L, Wang JW, Zhao XY, Zhao WJ, Kuang HX. Tong Xie Yao Fang relieves irritable bowel syndrome in rats via mechanisms involving regulation of 5-hydroxytryptamine and substance P. World J Gastroenterol. 2015;21:4536-4546. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 17] [Cited by in RCA: 18] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 3. | Xiong XJ, Wang J, Wang SH, He QY, Tang YL, Fu YK. A Survey of the theoretical Research on the relationship between prescriptions and Diseases Syndromes in Traditional Chinese Medicine. Zhonghua Zhongyiyao Zaizhi. 2009;24:1624-1626. |
| 4. | Xu SJ, Ma YG, Yang FL. Thoughts and methods of Research on prescription and Syndromes of traditional Chinese Medicine. Sichuan Zhongyi Zazhi. 2007;25:16-18. [DOI] [Full Text] |
| 5. | Fan X, Wang J, Jiang YW, Tao CH, Liu SL, Li JG. Primary study on chronic heart failure rats with Yang deficiency syndrome based on theory of correspondence of prescriptions with syndromes. Zhonghua Zhongyiyao Zazhi. 2015;30:4275-4279. |
| 6. | Chen J, Deng J, Zhou J, Xie ZJ, Gan J, Wen CP. Metabonomics of Artemisia annua and soft-shelled turtle A in combination treatment of systemic lupus erythematosus in mice. Zhongguo Yaolixue Tongbao. 2016;32:727-732. [DOI] [Full Text] |
| 7. | Wang TS, Xie M. Metabonomics and Modern Study of Traditional Chinese Medicine. Zhongyi Zazhi. 2006;47:723-725. [DOI] [Full Text] |
| 8. | Jing L, He W, Liu SM, Huang ZH, Liu DM, Zu JX. Research on the effect of Coptis chinensis - Scutellaria baicalensis and Coptis chinensis. Scutellaria baicalensis-Cortex Phellodendri for the 2,4-dinitrophenol-induced fever syndrome model on metabolomics. Zhongyao Yaoli Yu Linchuang. 2011;27:67-71. [DOI] [Full Text] |
| 9. | Zhou HG, Chen HB, Wang RP, Zhang Y, Wu MH. Metabonomics and its application in TCM formula study. Zhongguo Yaolixue Tongbao. 2013;29:161-165. [DOI] [Full Text] |
| 10. | Deng X. Application of Metabonomics in the Research of traditional Chinese Medicine. Yunnan Zhongyi Zhongyao Zazhi. 2010;31:73-75. [DOI] [Full Text] |
| 11. | Al-Chaer ED, Kawasaki M, Pasricha PJ. A new model of chronic visceral hypersensitivity in adult rats induced by colon irritation during postnatal development. Gastroenterology. 2000;119:1276-1285. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 534] [Cited by in RCA: 554] [Article Influence: 22.2] [Reference Citation Analysis (0)] |
| 12. | Larauche M, Mulak A, Taché Y. Stress-related alterations of visceral sensation: animal models for irritable bowel syndrome study. J Neurogastroenterol Motil. 2011;17:213-234. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 62] [Cited by in RCA: 65] [Article Influence: 4.6] [Reference Citation Analysis (1)] |
| 13. | Bian ZX, Qin HY, Tian SL, Qi SD. Combined effect of early life stress and acute stress on colonic sensory and motor responses through serotonin pathways: differences between proximal and distal colon in rats. Stress. 2011;14:448-458. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 20] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 14. | Lu M, Zhang W, Yao Q, Lu XM, Li SL, Ju JM. Effect of Changkang Fang on serotonin transporter expression in brain-gut axis of visceral hypersensitive rats with irritable bowel syndrome. Shijie Huaren Xiaohua Zazhi. 2015;23:1231-1237. [RCA] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 1] [Cited by in RCA: 2] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 15. | Wang JW, Xu FH, Yin Y, Zhang JY, Kuang HX. Effects of Tong Xie Yao Fang Formula on multiple factors-induced rat model of irritable bowel syndrome based on the theory of correlation between formula and syndrome. Zhonghua Zhongyiyao Zazhi. 2017;32:553-559. |
| 16. | Zhao Y, Qian L. Homocysteine-mediated intestinal epithelial barrier dysfunction in the rat model of irritable bowel syndrome caused by maternal separation. Acta Biochim Biophys Sin (Shanghai). 2014;46:917-919. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 12] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 17. | Zhang ZZ, Wang Y, Wang L, Lin KR. Prevention and treatment of intestinal barrier dysfunction by N-acetylcysteine. Linchuang Junyi Zazhi. 2007;35:756-759. [DOI] [Full Text] |
| 18. | Danese S, Sgambato A, Papa A, Scaldaferri F, Pola R, Sans M, Lovecchio M, Gasbarrini G, Cittadini A, Gasbarrini A. Homocysteine triggers mucosal microvascular activation in inflammatory bowel disease. Am J Gastroenterol. 2005;100:886-895. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 83] [Cited by in RCA: 97] [Article Influence: 4.9] [Reference Citation Analysis (0)] |
| 19. | Yang RX, Zhang JD, Luo WM, Guo RC, Zhu YY, Wang SH. Effects of“YiShen HuoXue Capsule”on Hcy, ET, TNF-α and NO in Patients with Unstable Angina. Shanghai Zhongyiyao Zazhi. 2006;40:22-24. [DOI] [Full Text] |
| 20. | Wu JC. Psychological Co-morbidity in Functional Gastrointestinal Disorders: Epidemiology, Mechanisms and Management. J Neurogastroenterol Motil. 2012;18:13-18. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 69] [Cited by in RCA: 88] [Article Influence: 6.8] [Reference Citation Analysis (0)] |
| 21. | Munoz-Olaya JM, Matabosch X, Bedia C, Egido-Gabás M, Casas J, Llebaria A, Delgado A, Fabriàs G. Synthesis and biological activity of a novel inhibitor of dihydroceramide desaturase. ChemMedChem. 2008;3:946-953. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 57] [Cited by in RCA: 58] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 22. | Bionda C, Portoukalian J, Schmitt D, Rodriguez-Lafrasse C, Ardail D. Subcellular compartmentalization of ceramide metabolism: MAM (mitochondria-associated membrane) and/or mitochondria? Biochem J. 2004;382:527-533. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 192] [Cited by in RCA: 208] [Article Influence: 10.4] [Reference Citation Analysis (0)] |
| 23. | Zhuang LL, Hu TM, Huang SF, Huang GX. Effects of Huangshu enema on serum levels of TNF-α in patients with irritable bowel syndrome. Shijie Huaren Xiaohua Zazhi. 2014;22:144-148. [RCA] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 1] [Cited by in RCA: 1] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 24. | Xiang FM, Jiang YP, Deng KH. Effect of ShengQing JiangZhuo herbs on the level of TNF-α and IL-10 in serum of patients with IBS. Zhongguo Zhongxiyi Jiehe Xiaohua Zazhi. 2014;22:638-639, 643. [DOI] [Full Text] |