Published online Mar 28, 2015. doi: 10.3748/wjg.v21.i12.3755
Peer-review started: October 3, 2014
First decision: October 29, 2014
Revised: November 17, 2014
Accepted: January 16, 2015
Article in press: January 16, 2015
Published online: March 28, 2015
Processing time: 178 Days and 17.6 Hours
Hepatic angiomyolipomas (AMLs) are typically benign tumors containing varying amounts of smooth muscle cells, adipose tissue, and vessels, and are commonly found in the kidney and occasionally in the liver. The preoperative diagnosis of hepatic AML is primarily made from imaging and fine-needle aspiration biopsy results, though limited experience for such diagnoses can result in misdiagnosis. Some uncommon features of hepatic AML have been reported in the literature without an objective or qualitative consensus. As the majority of cases are benign, conservative treatment of AMLs is recommended. However, in rare cases, liver transplantation has been implemented. Only five cases of malignant hepatic AML have been reported. We report a rare case of recurrent posthepatectomy malignant hepatic AML that was misdiagnosed as liver cancer in a 37-year-old woman, which was treated by liver transplantation. The imaging and pathologic findings are presented in order to provide a more concise description to aid in future diagnoses.
Core tip: Hepatic angiomyolipomas (AMLs) are typically benign tumors, with rare reports of malignant cases. Because there is a lack of experience for preoperative diagnosis, hepatic AMLs can easily be misdiagnosed. This case report not only presents some characteristics of hepatic AML and diagnostic indicators of malignancy, but also describes the successful treatment with liver transplantation.
- Citation: Wang WT, Li ZQ, Zhang GH, Guo Y, Teng MJ. Liver transplantation for recurrent posthepatectomy malignant hepatic angiomyolipoma: A case report. World J Gastroenterol 2015; 21(12): 3755-3758
- URL: https://www.wjgnet.com/1007-9327/full/v21/i12/3755.htm
- DOI: https://dx.doi.org/10.3748/wjg.v21.i12.3755
Angiomyolipoma (AML) is a rare mesenchyme-derived neoplasm that most commonly occurs in the kidney, but can also be found in the liver. Hepatic AML was first reported by Ishak[1] in 1976, and has since been considered a benign tumor requiring conservative treatment. However, a malignant case with evidence of recurrence has been more recently been reported[2]. The first case of liver transplantation for hepatic AML was reported in 2010[3], and only two additional cases have since been described[3,4]. We report a case of a Chinese woman with recurrent posthepatectomy malignant hepatic AMLs who required liver transplantation. The details of this case will help for future diagnosis and treatment of malignant hepatic AML.
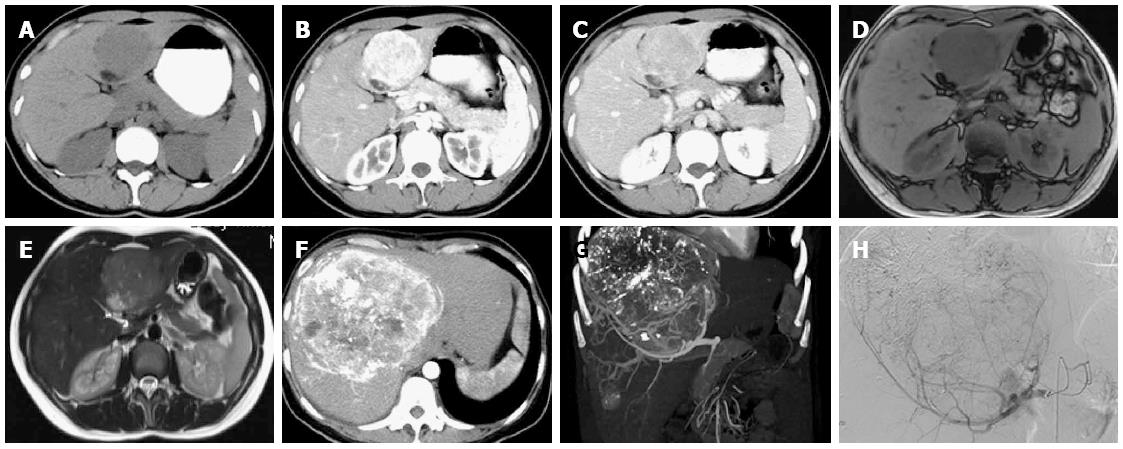
A 37-year-old Chinese woman had been diagnosed with liver cancer two years before. An abdominal enhanced computed tomography (CT) scan in 2011 showed a hepatic mass with early-phase hyperattenuation and late-phase hypoattenuation, measuring 7 cm × 9 cm in the left lobe (Figure 1A-C). Magnetic resonance imaging revealed a mass with hypointensity on T1-weighted, hyperintensity on T2-weighted, and hyperintensity on diffusion-weighted images (Figure 1D and E), and the patient underwent hepatic resection. Pathologic evaluation of the specimen indicated that the tumor was a hepatic AML.
The patient was subsequently lost to follow-up after surgery, during which time she gave birth to a baby and was not diagnosed during health checkups. She was admitted to our hospital in 2014 for further examination of a hepatic tumor that had been found incidentally during examinations. There was no medical history of other malignant diseases, and the blood exams were negative for tumor markers and viral markers. Enhanced CT showed two hepatic masses 13.0 cm × 12.0 cm and 2.3 cm × 1.8 cm in the right lobe (Figure 1F and G). On angiography, the tumor was shown as a circumscribed hypervascular mass (Figure 1H). After transcatheter arterial chemoembolization, liver transplantation was performed.
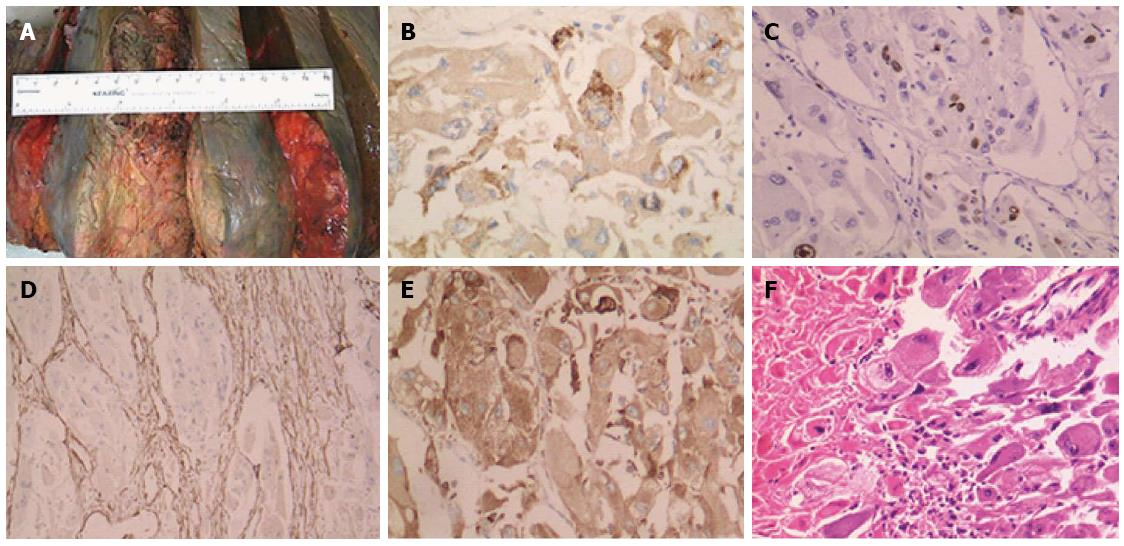
The two tumors appeared gray and white; the larger tumor measured 15 cm in diameter (Figure 2A), while the smaller one measured 3 cm in diameter. The diagnosis of hepatic AML was confirmed by immunohistochemical examination. Most of the epithelioid cells were immunopositive for human melanoma black-45 (Figure 2B), and there was no evidence of vascular invasion or extrahepatic metastasis. Nuclear atypia and Ki-67 antigenicity (4%) were found (Figure 2C). Additional indicators of malignancy were found (Figure 2D-F), and the final pathologic diagnosis was malignant hepatic AML. The patient recovered well and is currently healthy.
Of the 200 cases of hepatic AML reported, only five have described malignancies[2-5], and three with hepatic recurrence[5]; this is the sixth reported case of malignant hepatic AML. Most of the patients were asymptomatic, and preoperatively diagnosed from imaging and fine-needle aspiration biopsy findings. Because of the rarity of objectively malignant cases, it is difficult to distinguish benign from malignant hepatic AML, and subsequently, to determine whether to treat the patient conservatively or with surgery. Conservative treatment has been recommended for the patients with: (1) tumors smaller than 5 cm; (2) hepatic AML determined by fine-needle aspiration biopsy; (3) good compliance; and (4) hepatitis virus[6]. In contrast, surgery is the only accepted treatment for patients with: (1) multiple or large, unresectable lesions; (2) serious life-threatening complications; and (3) tumors with a malignant potential, for whom liver transplantation is available[2,7-9].
Liver transplantation has been proposed for the treatment of benign liver diseases[10], but only approximately 50 cases have been reported worldwide. However, there are only two reported cases of liver transplantation for AML. The first case was reported by Dumortier et al[3], describing a patient who died of multi-organ lesions after liver transplantation. The other report by Vagefi et al[4] involved a 20 cm mass, for which the authors suggested liver transplantation referral in similar cases because the lesions are not amenable to resection. However, the tumors in these two cases were consistent with benign hepatic AMLs.
A model was proposed for predicting malignant behavior of renal AMLs, incorporating the following features: ≥ 2 mitotic figures per 10 high-powered fields, atypical epithelioid cells, atypical mitotic figures and necrosis; the preoperative diagnostic accuracy rate was 78%[6]. In accordance, the case presented here also showed atypical epithelioid cells, atypical mitotic figures and necrosis. We also observed cells positive for human melanoma black-45 and Ki-67, which have been suggested as indicators of hepatic AML malignancy by Mizuguchi et al[7]. However, whether the predictive model of renal AML is applicable for hepatic AML requires further research.
Although malignant hepatic AML is extremely rare, a possible diagnosis should not be ignored. As liver transplantation has been the method of treatment for hepatic AML, preoperative evaluation and discussion must be made with caution.
A 37-year-old woman with recurrent posthepatectomy malignant hepatic angiomyolipoma (AML) without symptoms was misdiagnosed with liver cancer.
Recurrent posthepatectomy malignant hepatic AML.
Hepatic malignant tumor; Focal nodular hepatic fatty infiltration; Hepatic hemangioma.
WBC, 8.20 k/μL; hemoglobin, 12.10 g/dL; alpha-fetoprotein 1.31 ng/mL; liver function tests were within normal limits.
Enhanced computed tomography showed two hepatic masses with early-phase hyperattenuation and late-phase hypoattenuation, measuring 13.0 cm × 12.0 cm and 2.3 cm × 1.8 cm in the right lobe; upon angiography, the tumor was shown as a circumscribed hypervascular mass.
Benign AMLs have little or no mitotic activity, which was present in this case (human melanoma black-45-, smooth muscle actin- and CD68-positive).
The patient received a liver transplantation.
Malignant hepatic AML is extremely rare, and there are no proposed models for predicting malignancy.
AML is a rare mesenchyme-derived neoplasm, typically seen as benign tumors in the kidney, but can also be found in the liver.
This case report not only presents the features of malignant hepatic AML, but also applies liver transplantation as a treatment method.
The authors of the case report entitled “Liver transplantation for recurrent posthepatectomy malignant hepatic AML” present a problem of the use of liver transplantation as a method of treatment of liver malignant tumors. This case report is well written.
P- Reviewer: Karatapanis S, Marcos R, Owczarek D S- Editor: Ma YJ L- Editor: A E- Editor: Wang CH
| 1. | Ishak KG. Mesenchymal tumors of the liver. Hepatocellular carcinoma. New York: John Wiley and Sons 1976; 247-307. [RCA] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 11] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 2. | Dalle I, Sciot R, de Vos R, Aerts R, van Damme B, Desmet V, Roskams T. Malignant angiomyolipoma of the liver: a hitherto unreported variant. Histopathology. 2000;36:443-450. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 154] [Cited by in RCA: 135] [Article Influence: 5.4] [Reference Citation Analysis (0)] |
| 3. | Dumortier J, Guillaud O, Walter T, Ber CE, Partensky C, Boillot O, Scoazec JY. Liver transplantation for multiple angiomyolipomas complicating tuberous sclerosis complex. Gastroenterol Clin Biol. 2010;34:494-498. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 6] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 4. | Vagefi PA, Eilers H, Hiniker A, Freise CE. Liver transplantation for giant hepatic angiomyolipoma. Liver Transpl. 2011;17:985-986. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 7] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 5. | Yang CY, Ho MC, Jeng YM, Hu RH, Wu YM, Lee PH. Management of hepatic angiomyolipoma. J Gastrointest Surg. 2007;11:452-457. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 98] [Cited by in RCA: 73] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 6. | Brimo F, Robinson B, Guo C, Zhou M, Latour M, Epstein JI. Renal epithelioid angiomyolipoma with atypia: a series of 40 cases with emphasis on clinicopathologic prognostic indicators of malignancy. Am J Surg Pathol. 2010;34:715-722. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 149] [Cited by in RCA: 162] [Article Influence: 10.8] [Reference Citation Analysis (0)] |
| 7. | Mizuguchi T, Katsuramaki T, Nobuoka T, Nishikage A, Oshima H, Kawasaki H, Kimura S, Satoh M, Hirata K. Growth of hepatic angiomyolipoma indicating malignant potential. J Gastroenterol Hepatol. 2004;19:1328-1330. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 8. | Parfitt JR, Bella AJ, Izawa JI, Wehrli BM. Malignant neoplasm of perivascular epithelioid cells of the liver. Arch Pathol Lab Med. 2006;130:1219-1222. [PubMed] |
| 9. | Deng YF, Lin Q, Zhang SH, Ling YM, He JK, Chen XF. Malignant angiomyolipoma in the liver: a case report with pathological and molecular analysis. Pathol Res Pract. 2008;204:911-918. [PubMed] |
| 10. | Tepetes K, Selby R, Webb M, Madariaga JR, Iwatsuki S, Starzl TE. Orthotopic liver transplantation for benign hepatic neoplasms. Arch Surg. 1995;130:153-156. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 85] [Cited by in RCA: 63] [Article Influence: 2.1] [Reference Citation Analysis (0)] |