Published online Mar 21, 2015. doi: 10.3748/wjg.v21.i11.3435
Peer-review started: July 25, 2014
First decision: August 15, 2014
Revised: September 21, 2014
Accepted: November 11, 2014
Article in press: November 11, 2014
Published online: March 21, 2015
Processing time: 238 Days and 0.6 Hours
We report a patient with small intestinal metastasis from lung squamous cell carcinoma. A 66-year-old man who underwent radical lung cancer surgery was admitted to our hospital. Before starting his fifth cycle of chemotherapy, he was found to have a positive fecal occult blood test. Abdominal computed tomography scan revealed an ileal tumor with mesenteric lymph node enlargement. He underwent laparoscopic resection of the involved small intestine and mesentery. Histopathological analysis confirmed metastasis from lung cancer. We conducted a review of the literature and 64 documented cases of small intestinal metastasis from lung cancer were found. The pathologic diagnosis, clinical presentation, site of metastasis, and survival time in these cases were reviewed.
Core tip: Gastrointestinal tract metastases from lung cancer are relatively rare. We describe a patient with melena due to small intestinal metastasis from lung squamous cell carcinoma. We collected 64 similar documented cases from 2000 to date, and reviewed the pathologic diagnosis, clinical presentation, site of metastasis, treatment, and survival time.
- Citation: Liu W, Zhou W, Qi WL, Ma YD, Xu YY. Gastrointestinal hemorrhage due to ileal metastasis from primary lung cancer. World J Gastroenterol 2015; 21(11): 3435-3440
- URL: https://www.wjgnet.com/1007-9327/full/v21/i11/3435.htm
- DOI: https://dx.doi.org/10.3748/wjg.v21.i11.3435
Lung cancer is a malignant tumor with high incidence and mortality[1]. The prognosis of lung cancer is poor as metastases are often present at the time of diagnosis. Distant metastases are usually found in the adrenal glands, bone, liver, brain, and kidney, however, metastases in the gastrointestinal tract are relatively rare[2]. In this report, we present a patient with gastrointestinal bleeding due to ileal metastasis from primary lung carcinoma.
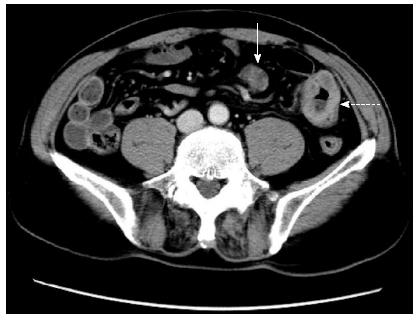
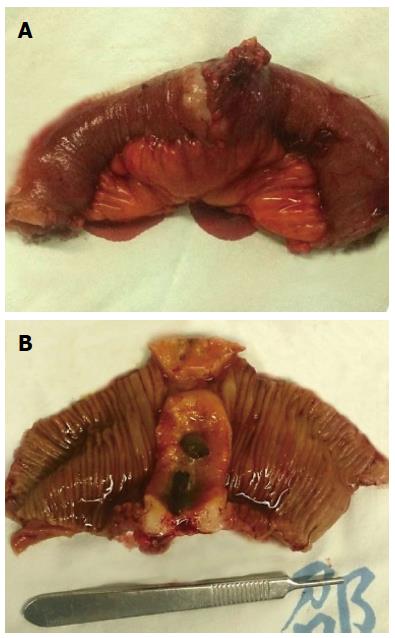
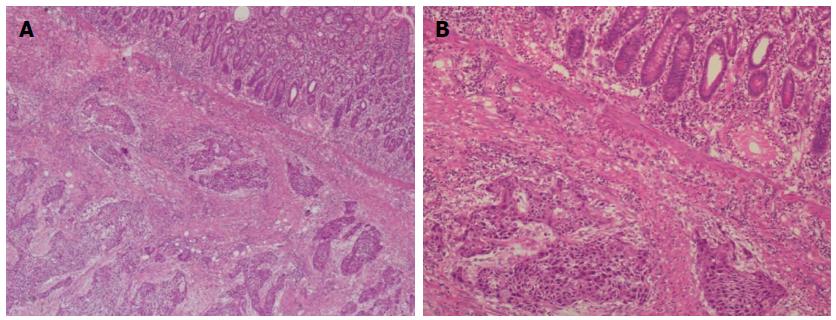
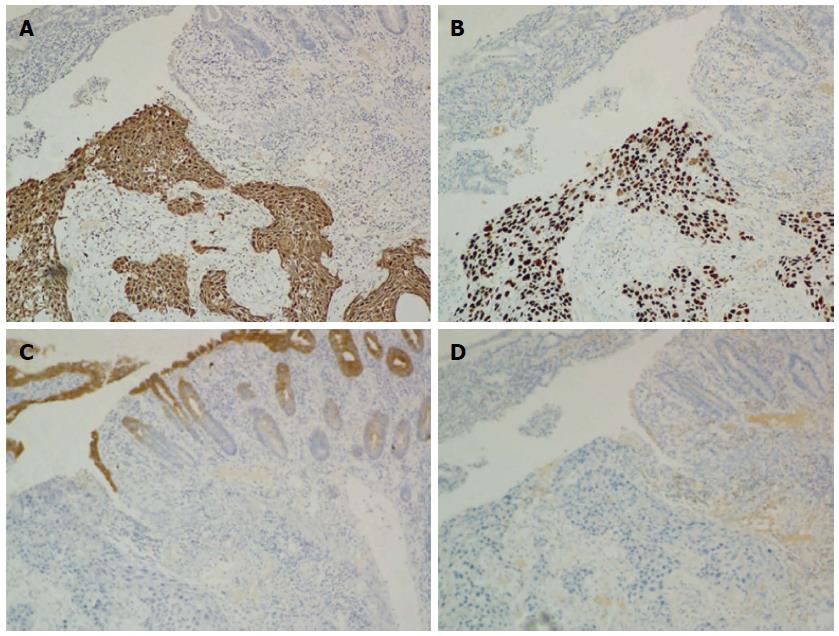
A 66-year-old male patient who presented with shortness of breath and hemoptysis for 1 wk was admitted to our hospital on May 8, 2013. On chest computed tomography (CT), a mass was seen in the right lower lobe. He underwent a right lower lobectomy with lymph node dissection on May 10, 2013. At surgery, a 3.5 cm mass was found in the right upper lobe near the right lung hilum. In addition, hilum, carina, and mediastinum lymphadenopathy were found. The pathological study confirmed moderately differentiated squamous cell carcinoma with lymph node metastasis (1+/38) (T2N1M0). The patient received four cycles of adjuvant chemotherapy with docetaxel/nedaplatin from June 2013 to September 2013. Just before the fifth cycle of chemotherapy (January 3, 2014), the patient complained of melena. The stool examination for occult blood was strongly positive. On abdominal examination, no abnormalities were found. Colonoscopy also revealed no abnormalities. An abdominal CT scan revealed ileal wall thickening and nearby mesenteric lymph node enlargement, indicating a malignant ileal tumor (Figure 1). Tumor markers were within normal ranges, including CEA which was 2.75 ng/mL. A complete blood count showed anemia with a hemoglobin (Hb) level of 9.6 g/dL. The patient then underwent laparoscopic exploration. A 4.5 cm × 3.0 cm small intestinal tumor with serosal infiltration was found 150 cm from the cecum (Figure 2). Lymph node enlargement was seen near the mesenteric root. The involved small bowel and mesentery were resected. Histopathological analysis confirmed that the tumor was a moderately differentiated squamous cell carcinoma (Figure 3). Immunohistochemically, tumor cells were positive for CKH and P63, but negative for CK20 and CK7 (Figure 4), indicating a metastasis from primary lung carcinoma. One of the two resected mesenteric lymph nodes contained metastasis, and the surgical margins were negative. The patient had no postoperative complications and was discharged 5 days after surgery. Postoperatively, he underwent four cycles of chemotherapy with gemcitabine/nedaplatin. Brain magnetic resonance imaging and SPECT/CT during chemotherapy revealed no other metastasis. The patient is still alive with no recurrence.
We searched the PubMed database for relevant English language publications from 2000 to June 2014 using the MeSH terms “Gastrointestinal Neoplasms/complications”, “Gastrointestinal Neoplasms/secondary”, and “Lung Neoplasms/pathology”. The age and sex of patients, pathologic diagnosis, clinical presentation, site of metastasis, and the survival time of the reported cases were reviewed and analyzed. In total, 64 cases were identified and reviewed[3-33], including 58 (90.6%) male and 6 (9.4%) female patients. The mean age of these patients was 61.4 years (ranging from 36 years to 88 years).
In lung cancer, metastases to the gastrointestinal tract are quite rare and mostly found in the advanced stages of the disease. Yang et al[21] reported that the incidence of symptomatic gastrointestinal metastasis from primary lung cancer was 1.77%. However, the prevalence at autopsy is much higher, ranging from 4.7% to 14%[34,35]. This can be explained by the fact that most patients with small bowel metastases have no specific symptoms. In the 64 documented cases, 59 patients had certain clinical presentations, of whom 22 (37.3%) had perforation, 19 (32.2%) had obstruction, 10 (16.9%) had hemorrhage and 8 (13.6%) had intussusception. Perforation was the most common symptom in patients with bowel metastases. The toxicity of chemotherapy is likely to be the etiology of bowel perforation[30].
In the 64 documented cases, 57 patients had metastatic sites. The jejunum was the most common site in 50.9% (29/57) of patients, followed by the ileum in 33.3% (19/57), and the duodenum in 15.8% (9/57). The general route of gastrointestinal metastasis has been suggested to be hematogenous metastasis through the spinal veins or lymphogenous metastasis from the mediastinum through the retroperitoneum and mesentery[9]. The difference in incidence between these metastatic sites may be because the jejunum and ileum have a more abundant blood supply and lymphoid tissues.
In lung cancer, all tumor cell types may develop small intestinal metastases. Adenocarcinoma (31.6%, 18/57), squamous cell carcinoma (28.1%, 16/57) and large cell carcinoma (24.6%, 14/57) were most common, followed by other types such as carcinosarcoma, adenosquamous, and neuroendocrine carcinoma (10.5%, 6/57) and small cell carcinoma (5.3%, 3/57). Yoshimoto et al[34] reported that patients with large cell carcinoma had a significantly higher rate of gastrointestinal metastases (P = 0.004, OR = 3.524) compared with patients with non-large cell carcinoma. However, the reasons for this are unknown.
Due to the unclear clinical symptoms in patients with small bowel metastases, early diagnosis and treatment are difficult. CT plays an important role in identifying the exact cause of abdominal symptoms in patients with lung cancer[36]. The metastatic lesions were seen on CT scans as wall thickening, an intraluminal polypoid mass or an exophytic mass. PET-CT may be more accurate than CT or other conventional imaging methods for the diagnosis of metastatic malignant sites. However, due to the high cost and the lack of clinical cases, the role of PET-CT in the diagnosis of lung cancer gastrointestinal metastasis is still controversial. Capsule endoscopy has the capability of providing visual images of the bowel and is superior in many aspects of gastrointestinal disease evaluation and management. It can provide help in identifying the presence of small intestinal metastasis when a patient with lung cancer presents with suspected small intestinal bleeding. However, it may have a limited role in patients with bowel perforation and obstruction.
As most lung cancer patients with gastrointestinal metastasis exhibit bowel perforation or an acute abdomen, surgical intervention is required. Dabaja et al[37] showed that the 5-year overall survival rate was significantly higher for patients who underwent surgery compared with patients who did not. Laparoscopic surgery not only has the advantages of less trauma, less blood loss and quicker recovery, but also has huge potential in diagnosis. Postoperative chemotherapy and individualized treatment may improve the survival rate for these lung cancer patients. For the lung cancer patient with distant metastasis, the guideline indicates that cisplatin/pemetrexed is recommended for patients with non-squamous non-small cell lung cancer; for patients with squamous cell carcinoma, cisplatin/gemcitabine is an option[38]. The chemotherapy regimen should be changed when there are other metastases present.
Many patients with small bowel metastases had synchronous metastasis in other organs. PAUL reported that 46 patients had small bowel metastasis of 431 autopsies on patients with lung cancer. In addition, all patients with small bowel metastases had at least one other metastatic site with an average of 4.8 sites such as the adrenal gland, liver, and kidney. This indicated that gastrointestinal metastasis is a late symptom of lung cancer and a poor prognostic indicator in the course of lung cancer[39]. In the documented cases, the median survival time was 3 months after detection of small bowel metastases in 48 patients. The poor prognosis was mainly due to late detection, the malignant biological behavior of lung cancer, abdominal infections, surgical complications, and other metastases. Brain and bone are common sites of distant metastases in lung cancer. In contrast, the median survival time of patients with bone metastases was 7 mo. Patients with brain metastases had a median survival of 3-6 mo[40]. Metastases to the small bowel have a worse prognosis than metastases to the brain and bone.
Due to better diagnostic methods and prolonged survival of lung cancer patients, gastrointestinal metastases are more common. When abdominal symptoms are present or persistent positive occult blood tests are found, bowel metastases should be considered. Abdominal CT has high value in diagnosing gastrointestinal metastases. With regard to the treatment of gastrointestinal metastases from lung cancer, surgery can be a curative treatment option. Chemotherapy and supportive care can improve the prognosis.
A 66-year-old man with a history of radical lung cancer surgery presented with melena.
Gastrointestinal hemorrhage; Postoperative lung cancer.
Primary small intestinal carcinoma; colorectal cancer; peptic ulcer.
Tumor markers were within normal ranges, including CEA which was 2.75 ng/mL. A complete blood count showed anemia with an Hb level of 9.6 g/dL.
An abdominal CT scan revealed ileal wall thickening and nearby mesenteric lymph node enlargement, indicating a malignant ileal tumor.
Histopathological analysis confirmed a moderately differentiated squamous cell carcinoma; immunohistochemistry indicated metastasis from primary lung carcinoma.
The patient underwent resection of the involved small bowel and mesentery. Postoperatively, he received four cycles of chemotherapy with gemcitabine/nedaplatin.
Gastrointestinal tract metastases from lung cancer are relatively rare, and the clinical symptoms are unclear. The general route of gastrointestinal metastasis and the prognosis are also unclear.
When abdominal symptoms are present or persistent positive occult blood tests are found in patient with lung cancer, bowel metastases should be considered
The authors reported a rare and interesting case of a patient with small intestine metastasis from lung squamous cell carcinoma, and they reviewed 64 documented cases with small intestine metastasis from lung cancer.
P- Reviewer: Tsuchiya A, Herszenyi L, Keishiro A S- Editor: Yu J L- Editor: A E- Editor: Ma S
| 1. | Siegel R, Naishadham D, Jemal A. Cancer statistics, 2013. CA Cancer J Clin. 2013;63:11-30. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9215] [Cited by in RCA: 9856] [Article Influence: 821.3] [Reference Citation Analysis (4)] |
| 2. | Hoffman PC, Mauer AM, Vokes EE. Lung cancer. Lancet. 2000;355:479-485. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 498] [Cited by in RCA: 535] [Article Influence: 21.4] [Reference Citation Analysis (0)] |
| 3. | Song Y, Li M, Shan J, Ye X, Tang S, Fang X, Ding K, Yuan Y. Acute small bowel obstruction: a rare initial presentation for the metastasis of the large-cell carcinoma of the lung. World J Surg Oncol. 2012;10:26. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 12] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 4. | Salemis NS, Nikou E, Liatsos C, Gakis C, Karagkiouzis G, Gourgiotis S. Small bowel perforation secondary to metastatic non-small cell lung cancer. A rare entity with a dismal prognosis. J Gastrointest Cancer. 2012;43:391-395. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 12] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 5. | Mulder MC, Kist JW, Consten EC, Verheijen PM. Gastrointestinal metastasis as the first presentation of lung carcinoma. Int J Colorectal Dis. 2012;27:839-840. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 6. | Jung LY, Jeon SY, Kim SR, Chung MJ, Lee YC. Pulmonary sarcomatoid carcinoma accompanying duodenal involvement. Am J Respir Crit Care Med. 2012;185:899-900. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 4] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 7. | Guner A, Karyagar S, Livaoglu A, Kece C, Kucuktulu U. Small Bowel Intussusception due to Metastasized Sarcomatoid Carcinoma of the Lung: A Rare Cause of Intestinal Obstruction in Adults. Case Rep Surg. 2012;2012:962683. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 7] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 8. | Nishizawa Y, Kobayashi A, Saito N, Nagai K, Sugito M, Ito M, Nishizawa Y. Surgical management of small bowel metastases from primary carcinoma of the lung. Surg Today. 2012;42:233-237. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 22] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 9. | Yamada H, Akahane T, Horiuchi A, Shimada R, Shibuya H, Hayama T, Nozawa K, Ishihara S, Matsuda K, Watanabe T. A case of lung squamous cell carcinoma with metastases to the duodenum and small intestine. Int Surg. 2011;96:176-181. [PubMed] |
| 10. | Lee PC, Lo C, Lin MT, Liang JT, Lin BR. Role of surgical intervention in managing gastrointestinal metastases from lung cancer. World J Gastroenterol. 2011;17:4314-4320. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 52] [Cited by in RCA: 65] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 11. | Bugiantella W, Cavazzoni E, Graziosi L, Valiani S, Franceschini MS, Donini A. Small bowel metastasis from lung cancer: a possible cause of acute abdomen. Case report and literature review. G Chir. 2011;32:120-122. [PubMed] |
| 12. | Sayilir A, Oztaş E, Onal IK, Kurt M, Kekıllı M, Akdoğ G, Ibış M. Small bowel obstruction: a presenting symptom of squamous cell carcinoma of the lung. Turk J Gastroenterol. 2011;22:440-442. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 13. | Kim SY, Ha HK, Park SW, Kang J, Kim KW, Lee SS, Park SH, Kim AY. Gastrointestinal metastasis from primary lung cancer: CT findings and clinicopathologic features. AJR Am J Roentgenol. 2009;193:W197-W201. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 69] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 14. | Chiu WK, Lin YC, Wang LT, Chen JH, Yu JC, Hsieh CB. Jejunojejunal intussusception secondary to metastasis from adenocarcinoma of the lung--a case report. Acta Chir Belg. 2009;109:519-522. [PubMed] |
| 15. | Huang YJ, Wu MH, Lin MT. Multiple small-bowel intussusceptions caused by metastatic malignant melanoma. Am J Surg. 2008;196:e1-e2. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 13] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 16. | Kagohashi K, Kadono K, Satoh H, Ohtsuka M. Intussusception due to intestinal metastasis from lung cancer. Lung Cancer. 2007;57:247-248. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 17. | Goh BK, Yeo AW, Koong HN, Ooi LL, Wong WK. Laparotomy for acute complications of gastrointestinal metastases from lung cancer: is it a worthwhile or futile effort? Surg Today. 2007;37:370-374. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 41] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 18. | Kostakou C, Khaldi L, Flossos A, Kapsoritakis AN, Potamianos SP. Melena: a rare complication of duodenal metastases from primary carcinoma of the lung. World J Gastroenterol. 2007;13:1282-1285. [PubMed] |
| 19. | Gómez-Patiño JA, Almaraz CS, Sánchez MI. [Primary lung carcinoma with intestinal metastases: 3 cases in a series of 420 patients]. Arch Bronconeumol. 2007;43:472-473. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 20. | Yuksel O, Uyar P, Sahin TT, Demirhan B. Small bowel perforation due to metastatic lung squamous cell carcinoma. Saudi Med J. 2007;28:631-633. [PubMed] |
| 21. | Yang CJ, Hwang JJ, Kang WY, Chong IW, Wang TH, Sheu CC, Tsai JR, Huang MS. Gastro-intestinal metastasis of primary lung carcinoma: clinical presentations and outcome. Lung Cancer. 2006;54:319-323. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 114] [Cited by in RCA: 151] [Article Influence: 7.9] [Reference Citation Analysis (0)] |
| 22. | Kanemoto K, Kurishima K, Ishikawa H, Shiotani S, Satoh H, Ohtsuka M. Small intestinal metastasis from small cell lung cancer. Intern Med. 2006;45:967-970. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 16] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 23. | Alvarez Laso C, Paredes Aracil E, Azcano González E, Ots Gutiérrez JR, Bernabeu Miralles M, Compañ Rosique A. Small bowel occlusion due to intussusception of a single metastasis of lung cancer. Clin Transl Oncol. 2006;8:833-834. [PubMed] |
| 24. | Yilmaz S, Dursun M, Canoruç F, Bayan K, Büyükbayram H. Upper gastrointestinal bleeding caused by small-cell lung cancer: a case report. Dig Dis Sci. 2006;51:788-790. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 7] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 25. | Tomas D, Ledinsky M, Belicza M, Kruslin B. Multiple metastases to the small bowel from large cell bronchial carcinomas. World J Gastroenterol. 2005;11:1399-1402. [PubMed] |
| 26. | Burnette RE, Ballard BR. Metastatic pleomorphic carcinoma of lung presenting as abdominal pain. J Natl Med Assoc. 2004;96:1657-1660. [PubMed] |
| 27. | Felsher J, Brodsky J, Brody F. Laparoscopic small bowel resection of metastatic pulmonary carcinosarcoma. J Laparoendosc Adv Surg Tech A. 2003;13:397-400. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 9] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 28. | Sakorafas GH, Pavlakis G, Grigoriadis KD. Small bowel perforation secondary to metastatic lung cancer: a case report and review of the literature. Mt Sinai J Med. 2003;70:130-132. [PubMed] |
| 29. | Testini M, Trabucco S, Di Venere B, Piscitelli D. Ileal intussusception due to intestinal metastases from primary malignant melanoma of the lung. Am Surg. 2002;68:377-379. [PubMed] |
| 30. | Yuen JS, Chow PK, Ahmed Q. Metastatic lung cancer causing bowel perforations: spontaneous or chemotherapy-related? ANZ J Surg. 2002;72:245-246. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 16] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 31. | Cremon C, Barbara G, De Giorgio R, Salvioli B, Epifanio G, Gizzi G, Stanghellini V, Corinaldesi R. Upper gastrointestinal bleeding due to duodenal metastasis from primary lung carcinoma. Dig Liver Dis. 2002;34:141-143. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 12] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 32. | Lee KA, Lee SK, Seo DW, Kim MH. Duodenal metastasis from lung cancer presenting as obstructive jaundice. Gastrointest Endosc. 2001;54:228. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 9] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 33. | Chagpar A, Moyana TN, Chappell EW. Isolated metachronous jejunal metastases after resection of bronchogenic carcinoma. Can J Surg. 2000;43:57-58. [PubMed] |
| 34. | Yoshimoto A, Kasahara K, Kawashima A. Gastrointestinal metastases from primary lung cancer. Eur J Cancer. 2006;42:3157-3160. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 72] [Cited by in RCA: 101] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 35. | Antler AS, Ough Y, Pitchumoni CS, Davidian M, Thelmo W. Gastrointestinal metastases from malignant tumors of the lung. Cancer. 1982;49:170-172. [PubMed] |
| 36. | Rossi G, Marchioni A, Romagnani E, Bertolini F, Longo L, Cavazza A, Barbieri F. Primary lung cancer presenting with gastrointestinal tract involvement: clinicopathologic and immunohistochemical features in a series of 18 consecutive cases. J Thorac Oncol. 2007;2:115-120. [PubMed] |
| 37. | Dabaja BS, Suki D, Pro B, Bonnen M, Ajani J. Adenocarcinoma of the small bowel: presentation, prognostic factors, and outcome of 217 patients. Cancer. 2004;101:518-526. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 357] [Cited by in RCA: 350] [Article Influence: 16.7] [Reference Citation Analysis (0)] |
| 38. | Ettinger DS, Akerley W, Borghaei H, Chang AC, Cheney RT, Chirieac LR, D’Amico TA, Demmy TL, Ganti AK, Govindan R. Non-small cell lung cancer. J Natl Compr Canc Netw. 2012;10:1236-1271. [PubMed] |
| 39. | McNeill PM, Wagman LD, Neifeld JP. Small bowel metastases from primary carcinoma of the lung. Cancer. 1987;59:1486-1489. [PubMed] |
| 40. | D’Antonio C, Passaro A, Gori B, Del Signore E, Migliorino MR, Ricciardi S, Fulvi A, de Marinis F. Bone and brain metastasis in lung cancer: recent advances in therapeutic strategies. Ther Adv Med Oncol. 2014;6:101-114. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 135] [Cited by in RCA: 167] [Article Influence: 15.2] [Reference Citation Analysis (0)] |