Published online Mar 21, 2015. doi: 10.3748/wjg.v21.i11.3300
Peer-review started: August 20, 2014
First decision: September 27, 2014
Revised: November 3, 2014
Accepted: December 8, 2014
Article in press: December 8, 2014
Published online: March 21, 2015
Processing time: 212 Days and 1.8 Hours
AIM: To compare outcomes from radiofrequency ablation (RFA) and hepatectomy for treatment of colorectal liver metastasis (CRLM).
METHODS: From January 2000 to December 2009, 408 patients underwent curative intent treatment for CRLM. We excluded patients using the criteria: size of CRLM > 3 cm, number of CRLM ≥ 5, percutaneous RFA, follow-up period < 12 mo, double primary cancer, or treatment with both RFA and hepatectomy. We matched 51 patients who underwent RFA with 102 patients who underwent hepatectomy by propensity scores.
RESULTS: The median follow-up period was 45 mo (range, 12 mo to 158 mo). Hepatic recurrence was more frequent in the RFA than the hepatectomy group (P = 0.021) although extrahepatic recurrence curves were similar (P = 0.716). Survival curves of hepatectomy group were better than that of RFA for multiple, large (> 2 cm) CRLM (P = 0.034). However, survival curves were similar for single or small (≤ 2 cm) CRLM (P = 0.714, P = 0.740).
CONCLUSION: Hepatectomy is better than RFA for the treatment of CRLM. However, RFA might be suitable for selected patients with single, small (≤ 2 cm) CRLM.
Core tip: Previous studies reported that hepatectomy is better than radiofrequency ablation (RFA) to improve survival outcomes in the patients with colorectal liver metastasis (CRLM). However, there is still controversy that RFA is beneficial in selected patients. In this study, hepatectomy was better than RFA for the treatment of CRLM. However, RFA might be suitable for selected patients with single, small CRLM (≤ 2 cm).
-
Citation: Lee H, Heo JS, Cho YB, Yun SH, Kim HC, Lee WY, Choi SH, Choi DW. Hepatectomy
vs radiofrequency ablation for colorectal liver metastasis: A propensity score analysis. World J Gastroenterol 2015; 21(11): 3300-3307 - URL: https://www.wjgnet.com/1007-9327/full/v21/i11/3300.htm
- DOI: https://dx.doi.org/10.3748/wjg.v21.i11.3300
Hepatectomy is the standard treatment for colorectal liver metastasis (CRLM). Estimated 5-year overall survival (OS) rates are between 27% and 58%[1]. However, hepatectomy is difficult to perform and has a high complication rate. To reduce morbidity, radiofrequency ablation (RFA) has been used for decades to treat patients with CRLM[2,3].
Numerous studies have reported that RFA is a safe and feasible treatment option for a limited population of patients with CRLM[4]. RFA has a low risk of complications and is an effective treatment[3,5-8]. Recent studies, however, demonstrated that hepatectomy is superior to RFA and that RFA should be used only in patients unsuitable for hepatectomy[9-11]. However, outcomes after RFA to treat CRLM have rarely been evaluated according to location, number, and synchronicity of metastases even though these are important considerations in a treatment plan. Moreover, a recent study reported that survival was comparable for CRLM patients who underwent RFA or hepatectomy, despite the high local recurrence rate observed after RFA[2].
A randomized controlled trial to compare the outcomes of RFA and hepatectomy would be difficult. Instead, propensity score matching analysis has been used to minimize bias in evaluating the effectiveness of RFA in patients with hepatocellular carcinoma[12-14]. However, no propensity score analysis for patients with CRLM has been published.
Our aim in this study was to use propensity score matching to determine if survival outcomes were different between patients who underwent RFA and patients who underwent hepatectomy.
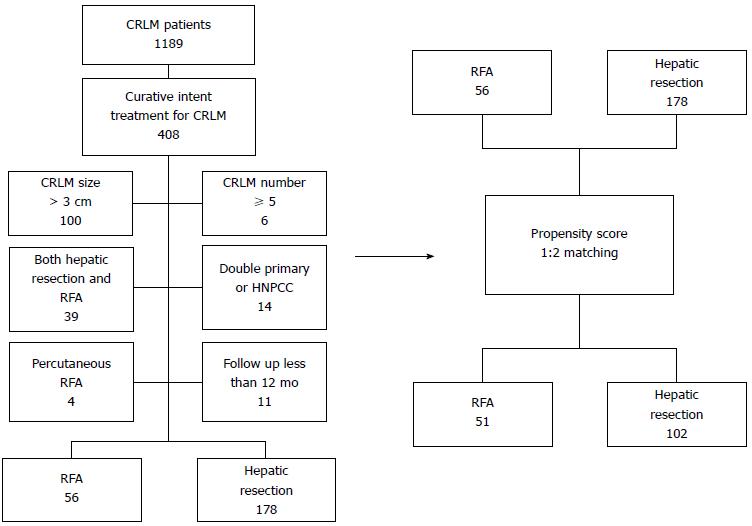
We reviewed 1189 colorectal cancer patients with liver metastasis between January 2000 and December 2009. We identified 408 patients who underwent curative intent hepatectomy or intraoperative RFA to treat CRLM. Exclusion criteria were CRLM size > 3 cm, number ≥ 5, percutaneous RFA, follow-up period < 12 mo, double primary cancer, hereditary nonpolyposis colorectal cancer (HNPCC), or treatment by both RFA and hepatectomy. Based on these criteria, 174 patients were excluded: 100 for CRLM size > 3 cm, 6 for CRLM number ≥ 5, 4 for percutaneous RFA, 11 for follow-up < 12 mo, 11 for double primary cancer, 3 for HNPCC, and 39 for both RFA and hepatectomy.
We calculated propensity scores using a multivariable logistic model considering the variables sex; age; preoperative carcinoembryonic antigen (CEA) level; location of the primary colon cancer; number, location and maximal size of CRLM; tumor node metastasis (TNM) stage; lymphatic invasion; vascular invasion; neoadjuvant chemotherapy; adjuvant chemotherapy; and cell differentiation. Using the logit of the estimated propensity score, one case from the RFA group was matched to two cases from the hepatectomy group using a caliper of 0.2. Covariate balance and surgical outcomes between the matched groups were evaluated after matching. We could not take indocyanine green (ICG) clearance test for calculating propensity score because we did not performed ICG retention test in every patients with colorectal liver metastasis. We routinely checked ICG retention rate in selected patients with chronic liver disease.
We matched 51 patients who underwent RFA with 102 patients who underwent hepatectomy using propensity scores. From RFA group, 5 patients were not matched and from the hepatectomy group, 76 were not matched (Figure 1).
We investigated extrahepatic metastases preoperatively using computed tomography (CT) and positron emission tomography images. All patients underwent prior surgical excision of a primary colorectal cancer. In the RFA group, an interventional radiologist performed RFA using open surgical or laparoscopic approaches with a 460 KHz generator expendable needle radiofrequency system (model 500 or 1500; RITA Medical Systems, Mountain View, CA; Cool Tip, Radionics Corporation, Burlington, MA). For lesions at the liver surface or adjacent to the intestine, patients were treated by laparoscopic or intraoperative RFA. For all patients who underwent RFA, complete necrosis of liver metastases was confirmed by intraoperative ultrasonography and CT or magnetic resonance imaging within 1 week of the procedure.
To prevent recurrence, we recommended adjuvant chemotherapy based on fluorouracil (5-FU) for all patients. Postoperative surveillance for recurrence was performed every 3 to 6 mo for the first 3 years and annually thereafter; this included physical examination, chest X-ray, and abdominal CT scanning. Local recurrence was defined as recurrence at the RFA-ablated area or resection margin of the hepatectomy. In addition to medical records, Roentgen images were reviewed retrospectively to identify recurrence patterns. Endpoints were time to tumor recurrence and time to death.
Sex, age, preoperative CEA level, location of the primary colon cancer, number, location and size of CRLM, TNM stage, lymphatic invasion, vascular invasion, cell differentiation, comorbidity, postoperative complication, recurrence, site of recurrence, death, disease-free survival (DFS), and OS were recorded for each patient. TNM staging, lymphatic invasion, vascular invasion, and cell differentiation were determined from the primary colorectal cancer. However, postoperative complications, recurrence, and site of recurrence were associated with the CRLM. Complication severity was classified using the Clavien-Dindo (CD) grading system[15]. CD scores of two or higher were regarded as a significant morbidity case. American Joint Committee on Cancer (AJCC) 7th TNM classification was used to define disease stage[16].
Statistical analyses were used the statistical software SPSS (SPSS for Windows version 20.0, Chicago, IL). Categorical variables are reported as numbers (percentages). Continuous variables are reported as medians (ranges). Categorical variables were compared using a χ2 or Fisher’s exact test. Continuous variables were compared using the Mann-Whitney U test. Survival was calculated by Kaplan-Meier survival analysis and Cox proportional hazard model. Differences in survival curves were assessed by multivariate analyses that included clinically important factors such as sex, age, T stage, lymph node involvement, and primary tumor location. We calculated hazard ratio (HR) and 95%CI. P-values less than 0.05 were considered statistically significant.
The hepatectomy group comprised 102 patients and the RFA group comprised 51. Median age was 60 years (range, 30 years to 79 years) and median follow-up duration was 45 mo (range, 12 mo to 158 mo). In the hepatectomy group, 29 patients (28%) were women; in the RFA group, 16 (31%) were women. CRLM had a colon cancer origin in 53 patients (52%) in the hepatectomy group and 29 (57%) in the RFA group.
Analysis of patient characteristics revealed no significant differences between groups in sex; age; preoperative CEA level; primary tumor location (colon or rectum); neoadjuvant chemotherapy; adjuvant chemotherapy; number, location, or maximal diameter of CRLM; TNM stage; lymphatic invasion; vascular invasion; histological differentiation or comorbidities. Median diameter of CRLM was 1.7 cm (range, 0.2 cm to 3.0 cm) in the hepatectomy group and 1.8 cm (range, 1.0 cm to 3.0 cm) in the RFA group. A single CRLM was seen in 63 patients (62%) in the hepatectomy group and 29 (57%) in the RFA group. The CRLM was located in the unilateral hemiliver in 80 patients (78%) in the hepatectomy group and 38 (75%) in the RFA group. All characteristics were appropriately distributed between the two groups (Table 1).
| Hepatectomy | RFA | P | |
| n = 102 | n = 51 | ||
| Sex (M/F) | 73/29 | 35/16 | 0.71 |
| Age (years) median (range) | 60 (3-79) | 58.5 (35-79) | 0.99 |
| Preoperative CEA (ng/mL) median (range) | 4.4 (0.1-202) | 6.5 (0.9-144) | 0.19 |
| Size of liver metastases, median (range) | 1.7 (0.2-3.0) | 1.8 (1.0-3.0) | 0.26 |
| Number of liver metastasis | |||
| Single | 63 (62) | 29 (57) | 0.56 |
| Multiple | 39 (38) | 22 (43) | |
| Metastasis type | |||
| Synchronous | 76 (75) | 33 (65) | 0.21 |
| Metachronous | 26 (25) | 18 (35) | |
| Location of liver metastasis | |||
| Unilobal | 80 (78) | 38 (75) | 0.59 |
| Bilobal | 22 (22) | 13 (25) | |
| N stage | |||
| N0 | 30 (29) | 13 (25) | 0.61 |
| N1, N2 | 72 (71) | 38 (75) | |
| Location of primary colorectal cancer | |||
| Colon | 53 (52) | 29 (57) | 0.57 |
| Rectum | 49 (48) | 22 (43) | |
| Histological differentiation1 | |||
| High grade | 88 (86) | 45 (88) | 0.73 |
| Low grade | 14 (14) | 6 (12) | |
| Comorbidity | |||
| Liver cirrhosis2 | 5 (5) | 6 (12) | 0.18 |
| Diabetes mellitus | 20 (20) | 13 (25) | 0.40 |
| Hypertension | 29 (28) | 12 (24) | 0.52 |
| Cardiovascular disease | 3 (3) | 1 (2) | 0.72 |
| Pulmonary disease | 6 (6) | 2 (4) | 0.99 |
| Neoadjuvant chemotherapy | |||
| Yes | 6 (6) | 5 (10) | 0.30 |
| No | 70 (94) | 28 (90) | |
| Adjuvant chemotherapy | |||
| Yes | 95 (93) | 46 (90) | 0.54 |
| No | 7 (7) | 5 (10) |
Postoperative complications (CD score ≥ 2) developed in 28 patients (27%) after hepatectomy and 5 (10%) after RFA (P = 0.012). However, no significant differences were noted in complication rates for treatment of CRLM. Perihepatic fluid collection or hepatic abscess were seen in 5 patients (5%) in the hepatic resection group and 2 (4%) in the RFA group (P = 0.99) with no postoperative mortality.
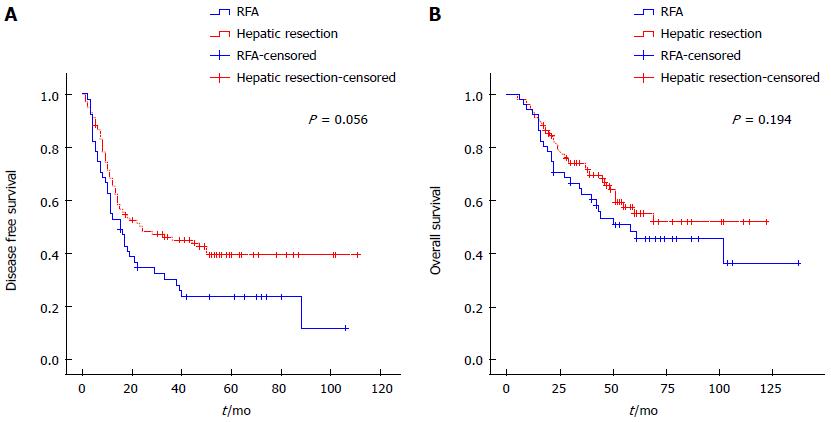
During follow-up, 98 of 152 patients (64%) experienced recurrence after hepatectomy or RFA. Hepatic recurrences were more common in the RFA than in the hepatectomy group (P = 0.021). Extrahepatic recurrences were not significantly different between the two groups (P = 0.716) (Figure 2).
DFS was 68.4% at 1 year, 45.2% at 3 years, and 39.7% at 5 years after hepatectomy and 52.9%, 30.4%, and 23.9% after RFA (P = 0.056). OS rates were 93.1% at 1 year, 73.9% at 3 years, and 55.2% at 5 years after hepatectomy and 92.2%, 62.4%, and 48.2% after RFA, respectively. Differences in OS curves were significant between the hepatectomy and RFA groups (P = 0.194) (Figure 3).
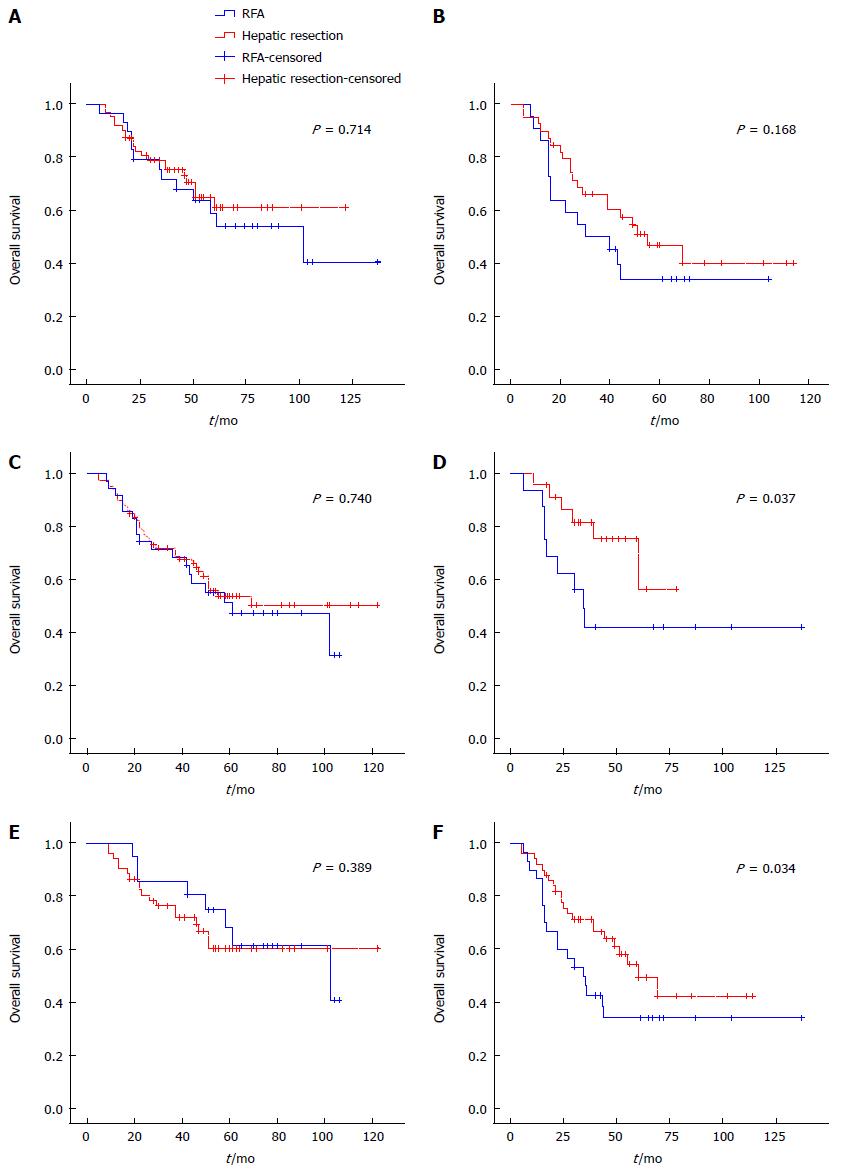
We performed subgroup analysis according to CRLM number, size, and location. Survival curves were similar between the two groups for single or small (≤ 2 cm) CRLM (P = 0.714 and P = 0.740). However, the trend was that survival curves for the hepatectomy group were better than for the RFA group for multiple, large (> 2 cm) CRLM (P = 0.034) (Figure 4). No significant differences were seen by tumor distribution.
Associations between RFA, sex, age, CRLM size or number, synchronicity, CRLM location, T stage, N stage, adjuvant chemotherapy, histologic grade and DFS were evaluated using a Cox proportional hazard model. In multivariate analysis, RFA, lymph node metastasis and poorly differentiated grade were significant risk factors for recurrence (HR = 1.57, P = 0.040 for RFA; HR = 1.94, P = 0.015 for lymph node metastasis; and HR = 1.79, P = 0.049 for histologic grade) (Table 2).
| Factors | Univariate analysis of DFS | Multivariate analysis of DFS | ||
| P | HR | 95%CI | P1 | |
| Radiofrequency ablation | 0.033 | 1.57 | 1.02-2.41 | 0.040 |
| Female sex | 0.890 | |||
| Age | 0.270 | |||
| CEA (ng/mL) | 0.130 | 1.03 | 0.99-1.01 | 0.480 |
| Size (cm) | 0.210 | |||
| Multiple | 0.140 | 1.01 | 0.65-1.57 | 0.970 |
| Metachronous | 0.089 | 0.75 | 0.45-1.24 | 0.260 |
| Bilobal | 0.300 | |||
| T22 | 0.130 | 0.55 | 0.18-1.65 | 0.290 |
| T32 | 0.090 | 0.78 | 0.41-1.49 | 0.450 |
| Lymph node metastasis | 0.003 | 1.94 | 1.14-3.31 | 0.015 |
| Adjuvant chemotherapy | 0.810 | |||
| Poorly differentiated grade | 0.033 | 1.79 | 1.01-3.18 | 0.049 |
Survival of colorectal cancer patients has improved over the last decades, largely due to newly developed surgical techniques and chemotherapeutic agents. In addition, techniques such as RFA have also been developed. We found that, by Cox regression multivariate analysis, RFA for CRLM was associated with a high recurrence rate. The hepatic recurrence rate was significantly higher after RFA than after hepatectomy by recurrence pattern analysis. However, oncologic outcomes were similar after RFA and hepatectomy for single or small (≤ 2 cm) CRLM.
We found significant differences in complication rates between the hepatectomy and RFA groups although the overall complication rate was low in both RFA and hepatectomy groups. Other studies also reported that RFA is less invasive than hepatectomy[5-8]. However, RFA should be considered as only an alternative treatment for patients not indicated for hepatectomy[2,9-11,17-21].
Hepatectomy is not always possible, however. A sufficient volume of remnant liver must be present before hepatectomy to reduce surgical risk. Portal blood pressure and biliary drainage are also important factors. If the estimated volume of the remnant liver is too small, portal vein embolization is useful to decrease surgical risk[22].
In our study, survival outcomes were similar in the RFA and hepatectomy groups, in particular for patients with single or small CRLM. However, the location of CRLM was not a significant factor for survival outcomes. Therefore, RFA might be substitute treatment for selected patients with single, small CRLM. The optimum diameter of CRLM for RFA has been controversial. Some studies suggest that RFA is acceptable if the CRLM are less than 3 cm in diameter[18,20,23,24]. However, other studies showed that RFA is associated with higher local recurrence rates, even for CRLMs less than 3 cm[19,25,26]. In this study, survival curves for the hepatic resection group were higher than for the RFA group for tumor size > 2 cm, although the difference was not significant.
A study reported that OS of an RFA group was comparable to OS for a hepatectomy group despite a high rate of local recurrence after RFA. This finding might be due to similar rates of extrahepatic recurrence, a crucial survival factor[2]. In our study, we verified RFA using a variety of criteria. RFA was associated not only with high local recurrence, but also poor OS. Cluster of differentiation 95 (CD95) is thought to affect the recurrence of cancer after RFA because of the potential of RFA to cause hypoxic damage. CD95 can induce apoptosis, but can also promote tumorigenesis in apoptosis-resistant tumor cells[27].
We used propensity score matching to minimize possible bias from stratification. We also used a Cox proportional hazard model to analyze multiple variables of RFA, sex, age, CEA, size, number of CRLM, metachronicity, bilobal distribution, TN stage, adjuvant chemotherapy, and cell differentiation. We found that RFA, lymph node metastasis and poorly differentiated cell type were associated with poor prognosis. Lymph node metastasis is a well-known prognostic factor for colorectal cancer treatment[28]. In this study, the lymph node metastasis and poorly differentiated type were poor prognostic factors.
To overcome the shortcomings of RFA, microwave ablation was developed to treat hepatic neoplasms[29-32]. Recent studies reported that microwave ablation is safe and has a low complication rate, even for tumors located near major vessels. Patients who underwent microwave ablation showed enhanced survival relative to a conventional hepatectomy group based on short-term follow-up results[32,33]. However, few published studies have examined a large number of patients followed for a long period of time.
This study has several limitations that should be considered. The major drawback was that it was neither randomized nor prospective. However, conducting randomization for RFA is difficult so we reduced bias using propensity score matching. Although we could not evaluate ICG clearance test and comorbidity rate to calculate propensity score, it does not seem an essential component to evaluate oncologic outcomes. Moreover, the comorbidity rate was not significantly different between the two groups.
In conclusion, our long-term follow-up survival analysis revealed that hepatectomy was superior to RFA for treating CRLM. RFA was associated with hepatic recurrence and was a poor prognostic factor. However, RFA might be an option for selected patients with single, small (≤ 2 cm) CRLM.
Numerous studies have reported that radiofrequency ablation (RFA) is a safe and feasible treatment option for a limited population of patients with colorectal liver metastasis (CRLM). Recent studies, however, demonstrated that hepatectomy is superior to RFA and that RFA should be used only in patients unsuitable for hepatectomy. However, outcomes after RFA to treat CRLM have rarely been evaluated according to location, number, and synchronicity of metastases even though these are important considerations in a treatment plan. Moreover, randomized controlled trial is difficult to do to compare the outcomes after hepatectomy and RFA.
Propensity score matching is widely used in recent studies when randomized controlled trial is difficult to apply. The aim in this study was to use propensity score matching to determine if survival outcomes were different between patients who underwent RFA and patients who underwent hepatectomy.
A randomized controlled trial to compare the outcomes of radiofrequency ablation (RFA) and hepatectomy would be difficult. Instead, propensity score matching analysis has been used to minimize bias in evaluating the effectiveness of RFA in patients with hepatocellular carcinoma. However, no propensity score analysis for patients with CRLM has been published.
The long-term follow-up survival analysis revealed that hepatectomy was superior to RFA for treating CRLM. RFA was associated with hepatic recurrence and was a poor prognostic factor. However, RFA might be an option for selected patients with single, small (≤ 2 cm) CRLM.
This is a good descriptive study and the methodology was so good. The particular point of this article is “propensity score analysis”. The authors used this method to match patients between these two groups and tried to overcome bias resulting from retrospective study.
P- Reviewer: Boin IFSF, Hsu WH S- Editor: Yu J L- Editor: A E- Editor: Liu XM
| 1. | White RR, Avital I, Sofocleous CT, Brown KT, Brody LA, Covey A, Getrajdman GI, Jarnagin WR, Dematteo RP, Fong Y. Rates and patterns of recurrence for percutaneous radiofrequency ablation and open wedge resection for solitary colorectal liver metastasis. J Gastrointest Surg. 2007;11:256-263. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 92] [Cited by in RCA: 96] [Article Influence: 5.3] [Reference Citation Analysis (1)] |
| 2. | Otto G, Düber C, Hoppe-Lotichius M, König J, Heise M, Pitton MB. Radiofrequency ablation as first-line treatment in patients with early colorectal liver metastases amenable to surgery. Ann Surg. 2010;251:796-803. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 101] [Cited by in RCA: 98] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 3. | Pathak S, Jones R, Tang JM, Parmar C, Fenwick S, Malik H, Poston G. Ablative therapies for colorectal liver metastases: a systematic review. Colorectal Dis. 2011;13:e252-e265. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 131] [Cited by in RCA: 124] [Article Influence: 8.9] [Reference Citation Analysis (0)] |
| 4. | Kingham TP, Tanoue M, Eaton A, Rocha FG, Do R, Allen P, De Matteo RP, D’Angelica M, Fong Y, Jarnagin WR. Patterns of recurrence after ablation of colorectal cancer liver metastases. Ann Surg Oncol. 2012;19:834-841. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 39] [Cited by in RCA: 42] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 5. | Yoon HM, Kim JH, Shin YM, Won HJ, Kim PN. Percutaneous radiofrequency ablation using internally cooled wet electrodes for treatment of colorectal liver metastases. Clin Radiol. 2012;67:122-127. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 10] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 6. | Livraghi T, Meloni F, Solbiati L, Zanus G. Complications of microwave ablation for liver tumors: results of a multicenter study. Cardiovasc Intervent Radiol. 2012;35:868-874. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 196] [Cited by in RCA: 183] [Article Influence: 14.1] [Reference Citation Analysis (0)] |
| 7. | Van Tilborg AA, Meijerink MR, Sietses C, Van Waesberghe JH, Mackintosh MO, Meijer S, Van Kuijk C, Van Den Tol P. Long-term results of radiofrequency ablation for unresectable colorectal liver metastases: a potentially curative intervention. Br J Radiol. 2011;84:556-565. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 83] [Cited by in RCA: 91] [Article Influence: 6.1] [Reference Citation Analysis (0)] |
| 8. | Cirimbei C, Prunoiu V, Marincaş M, Daha C, Cirimbei S, Stefan I, Man C, Brătucu E, Pantiş C, Rădoi S. [Radiofrequency ablation for liver metastases--mini invasive therapeutic option for patients with unresecable tumors]. Chirurgia (Bucur). 2011;106:465-473. [PubMed] |
| 9. | Wu YZ, Li B, Wang T, Wang SJ, Zhou YM. Radiofrequency ablation vs hepatic resection for solitary colorectal liver metastasis: a meta-analysis. World J Gastroenterol. 2011;17:4143-4148. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 46] [Cited by in RCA: 46] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 10. | Lee KH, Kim HO, Yoo CH, Son BH, Park YL, Cho YK, Kim H, Han WK. Comparison of radiofrequency ablation and resection for hepatic metastasis from colorectal cancer. Korean J Gastroenterol. 2012;59:218-223. [PubMed] |
| 11. | Mayo SC, Pawlik TM. Thermal ablative therapies for secondary hepatic malignancies. Cancer J. 2010;16:111-117. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 24] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 12. | Lee YH, Hsu CY, Chu CW, Liu PH, Hsia CY, Huang YH, Su CW, Chiou YY, Lin HC, Huo TI. Radiofrequency Ablation is Better Than Surgical Resection in Patients With Hepatocellular Carcinoma Within the Milan Criteria and Preserved Liver Function: A Retrospective Study Using Propensity Score Analyses. J Clin Gastroenterol. 2015;49:242-249. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 32] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 13. | Takuma Y, Takabatake H, Morimoto Y, Toshikuni N, Kayahara T, Makino Y, Yamamoto H. Comparison of combined transcatheter arterial chemoembolization and radiofrequency ablation with surgical resection by using propensity score matching in patients with hepatocellular carcinoma within Milan criteria. Radiology. 2013;269:927-937. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 70] [Cited by in RCA: 71] [Article Influence: 5.9] [Reference Citation Analysis (0)] |
| 14. | Liu PH, Lee YH, Hsu CY, Huang YH, Chiou YY, Lin HC, Huo TI. Survival advantage of radiofrequency ablation over transarterial chemoembolization for patients with hepatocellular carcinoma and good performance status within the Milan criteria. Ann Surg Oncol. 2014;21:3835-3843. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 16] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 15. | Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240:205-213. [PubMed] |
| 16. | Edge SB, Compton CC. The American Joint Committee on Cancer: the 7th edition of the AJCC cancer staging manual and the future of TNM. Ann Surg Oncol. 2010;17:1471-1474. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5537] [Cited by in RCA: 6457] [Article Influence: 430.5] [Reference Citation Analysis (0)] |
| 17. | Reuter NP, Woodall CE, Scoggins CR, McMasters KM, Martin RC. Radiofrequency ablation vs. resection for hepatic colorectal metastasis: therapeutically equivalent? J Gastrointest Surg. 2009;13:486-491. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 95] [Cited by in RCA: 88] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 18. | Hur H, Ko YT, Min BS, Kim KS, Choi JS, Sohn SK, Cho CH, Ko HK, Lee JT, Kim NK. Comparative study of resection and radiofrequency ablation in the treatment of solitary colorectal liver metastases. Am J Surg. 2009;197:728-736. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 156] [Cited by in RCA: 161] [Article Influence: 9.5] [Reference Citation Analysis (0)] |
| 19. | Park IJ, Kim HC, Yu CS, Kim PN, Won HJ, Kim JC. Radiofrequency ablation for metachronous liver metastasis from colorectal cancer after curative surgery. Ann Surg Oncol. 2008;15:227-232. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 78] [Cited by in RCA: 74] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 20. | Mulier S, Ruers T, Jamart J, Michel L, Marchal G, Ni Y. Radiofrequency ablation versus resection for resectable colorectal liver metastases: time for a randomized trial? An update. Dig Surg. 2008;25:445-460. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 97] [Cited by in RCA: 102] [Article Influence: 6.4] [Reference Citation Analysis (0)] |
| 21. | Lee WS, Yun SH, Chun HK, Lee WY, Kim SJ, Choi SH, Heo JS, Joh JW, Choi D, Kim SH. Clinical outcomes of hepatic resection and radiofrequency ablation in patients with solitary colorectal liver metastasis. J Clin Gastroenterol. 2008;42:945-949. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 117] [Cited by in RCA: 117] [Article Influence: 6.9] [Reference Citation Analysis (0)] |
| 22. | Adams RB, Aloia TA, Loyer E, Pawlik TM, Taouli B, Vauthey JN. Selection for hepatic resection of colorectal liver metastases: expert consensus statement. HPB (Oxford). 2013;15:91-103. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 210] [Cited by in RCA: 223] [Article Influence: 18.6] [Reference Citation Analysis (0)] |
| 23. | Abitabile P, Hartl U, Lange J, Maurer CA. Radiofrequency ablation permits an effective treatment for colorectal liver metastasis. Eur J Surg Oncol. 2007;33:67-71. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 101] [Cited by in RCA: 103] [Article Influence: 5.4] [Reference Citation Analysis (0)] |
| 24. | Valls C, Ramos E, Leiva D, Ruiz S, Martinez L, Rafecas A. Safety and Efficacy of Ultrasound-Guided Radiofrequency Ablation of Recurrent Colorectal Cancer Liver Metastases after Hepatectomy. Scand J Surg. 2014;Epub ahead of print. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 18] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 25. | Ko S, Jo H, Yun S, Park E, Kim S, Seo HI. Comparative analysis of radiofrequency ablation and resection for resectable colorectal liver metastases. World J Gastroenterol. 2014;20:525-531. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 34] [Cited by in RCA: 34] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 26. | Nishiwada S, Ko S, Mukogawa T, Ishikawa H, Matsusaka M, Nakatani T, Kikuchi E, Watanabe A. Comparison between percutaneous radiofrequency ablation and surgical hepatectomy focusing on local disease control rate for colorectal liver metastases. Hepatogastroenterology. 2014;61:436-441. [PubMed] |
| 27. | Nijkamp MW, Hoogwater FJ, Steller EJ, Westendorp BF, van der Meulen TA, Leenders MW, Borel Rinkes IH, Kranenburg O. CD95 is a key mediator of invasion and accelerated outgrowth of mouse colorectal liver metastases following radiofrequency ablation. J Hepatol. 2010;53:1069-1077. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 50] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 28. | Ryuk JP, Choi GS, Park JS, Kim HJ, Park SY, Yoon GS, Jun SH, Kwon YC. Predictive factors and the prognosis of recurrence of colorectal cancer within 2 years after curative resection. Ann Surg Treat Res. 2014;86:143-151. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 87] [Cited by in RCA: 114] [Article Influence: 10.4] [Reference Citation Analysis (0)] |
| 29. | Stättner S, Jones RP, Yip VS, Buchanan K, Poston GJ, Malik HZ, Fenwick SW. Microwave ablation with or without resection for colorectal liver metastases. Eur J Surg Oncol. 2013;39:844-849. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 41] [Cited by in RCA: 52] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 30. | Groeschl RT, Pilgrim CH, Hanna EM, Simo KA, Swan RZ, Sindram D, Martinie JB, Iannitti DA, Bloomston M, Schmidt C. Microwave ablation for hepatic malignancies: a multiinstitutional analysis. Ann Surg. 2014;259:1195-1200. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 149] [Cited by in RCA: 179] [Article Influence: 16.3] [Reference Citation Analysis (0)] |
| 31. | Bala MM, Riemsma RP, Wolff R, Kleijnen J. Microwave coagulation for liver metastases. Cochrane Database Syst Rev. 2013;10:CD010163. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 11] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 32. | Correa-Gallego C, Fong Y, Gonen M, D’Angelica MI, Allen PJ, DeMatteo RP, Jarnagin WR, Kingham TP. A retrospective comparison of microwave ablation vs. radiofrequency ablation for colorectal cancer hepatic metastases. Ann Surg Oncol. 2014;21:4278-4283. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 108] [Cited by in RCA: 126] [Article Influence: 11.5] [Reference Citation Analysis (0)] |
| 33. | Ierardi AM, Floridi C, Fontana F, Chini C, Giorlando F, Piacentino F, Brunese L, Pinotti G, Bacuzzi A, Carrafiello G. Microwave ablation of liver metastases to overcome the limitations of radiofrequency ablation. Radiol Med. 2013;118:949-961. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 56] [Article Influence: 4.7] [Reference Citation Analysis (0)] |