Published online Aug 14, 2013. doi: 10.3748/wjg.v19.i30.5021
Revised: April 27, 2013
Accepted: May 7, 2013
Published online: August 14, 2013
Processing time: 131 Days and 19.7 Hours
Mucocele of the appendix due to endometriosis is extremely rare, and there are only 10 previously reported cases in the English literature. We report a case of mucocele of the appendix due to endometriosis and provide the first review of the literature. A 43-year-old woman was admitted to the hospital because of recurrent right lower abdominal pain during her menstrual periods. Colonoscopy revealed submucosal tumor-like elevations of the appendiceal orifice. Computed tomography and magnetic resonance imaging of the abdomen suggested cystic lesions near the appendix. Consequently, mucocele of the appendix was suspected preoperatively. An open ileocecal resection was performed. Multiple cystic lesions were observed around the appendix. The cystic lesions contained mucus. Histopathological examination was consistent with a mucocele of the appendix due to endometriosis. The postoperative course was uneventful. We present the first review of the literature to clarify the clinical features.
Core tip: We report an extremely rare case of mucocele of the appendix due to endometriosis. Although it is uncommon, preoperative diagnosis of the mucocele is important; however, diagnosis is difficult using imaging modalities. We report a more accurate diagnostic possibility using preoperative imaging modalities, such as colonoscopy, ultrasonography, computed tomography, and magnetic resonance imaging. Furthermore, this report is important because it is the first review of the literature for mucocele of the appendix due to endometriosis.
- Citation: Tsuda M, Yamashita Y, Azuma S, Akamatsu T, Seta T, Urai S, Uenoyama Y, Deguchi Y, Ono K, Chiba T. Mucocele of the appendix due to endometriosis: A rare case report. World J Gastroenterol 2013; 19(30): 5021-5024
- URL: https://www.wjgnet.com/1007-9327/full/v19/i30/5021.htm
- DOI: https://dx.doi.org/10.3748/wjg.v19.i30.5021
Mucocele of the appendix is an uncommon disease. It is observed in 0.2%-0.3% of appendectomies and 8%-10% of appendiceal tumors[1]. According to the modern classification[2,3], mucocele of the appendix includes four histological groups: simple mucocele, mucosal hyperplasia, mucinous cystadenoma, and mucinous cystadenocarcinoma. Simple mucocele is caused by mucus distention secondary to an obstruction of the appendix due to fecaliths, post-inflammatory scarring, or rarely, endometriosis. There are only 10 previously reported cases of mucocele of the appendix due to endometriosis in the English literature[4-12]. We present a rare case of mucocele of the appendix due to endometriosis and a review of the literature.
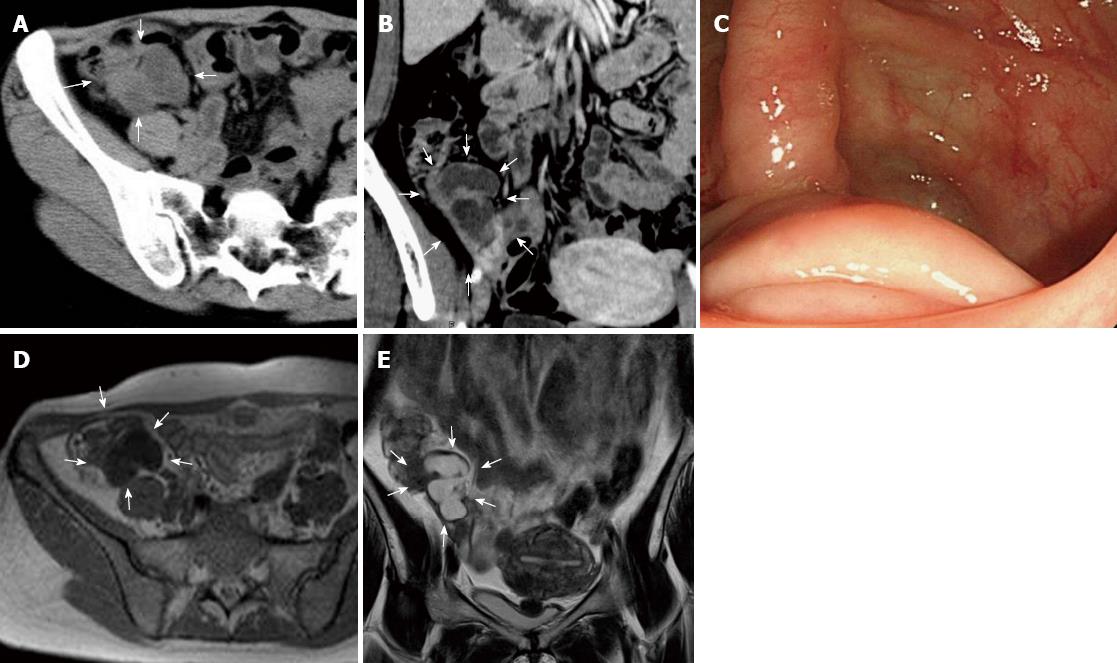
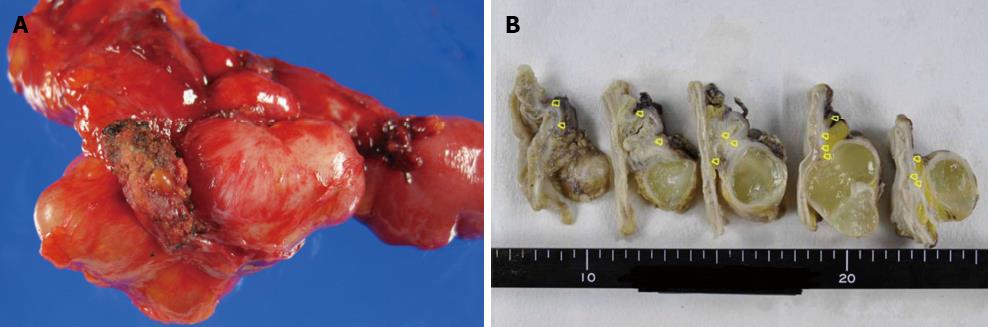
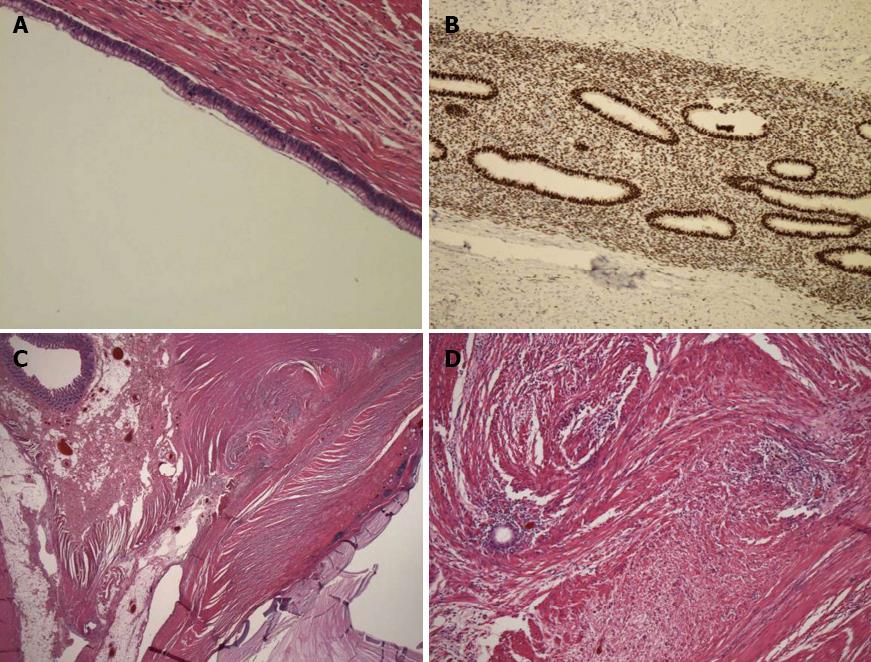
A 43-year-old woman was admitted to the hospital because of recurrent right lower abdominal pain during her menstrual periods. On physical examination, she presented with mild right lower abdominal tenderness without rigidity. Her blood and urine tests were normal. Abdominal computed tomography (CT) revealed low-density lesions near the appendix. Colonoscopy revealed submucosal tumor-like elevations of the appendiceal orifice. A biopsy was performed and result was negative. Subsequent magnetic resonance imaging (MRI) revealed hyperintensity on T2-weighted imaging (WI) (Figure 1). Consequently, mucocele of the appendix was diagnosed preoperatively. Her recurrent right lower abdominal pain during menstrual periods suggested the involvement of endometriosis. Our patient was offered open surgical resection because malignancy could not be ruled out. During surgery, several cystic lesions were observed around the appendix. Features of endometriosis were not observed in the pelvis, the uterus, or the rest of the abdominal cavity. An open ileocecal resection was performed. Multiple cystic lesions were observed around the appendix. The contents of the cystic lesions consisted of mucus (Figure 2). Histopathological examination indicated that the cysts were a simple type of mucocele and that endometriosis and smooth muscle hypertrophy were present in the muscle layer of the appendix around the mucocele (Figure 3). Consequently, we reached a diagnosis that the mucocele of the appendix was due to endometriosis. The postoperative course was uneventful.
A mucocele of the appendix is a rare lesion. It occurs in 0.2%-0.3% of all appendectomies performed and 8%-10% of all resected appendiceal tumors[1]. Endometriosis of the appendix is also a rare lesion, and is observed in 0.054%-0.8% of all appendectomies performed[13-15]. Finally, mucocele of the appendix due to endometriosis is extremely rare.
According to the modern classification[2,3], mucocele of the appendix includes four histological groups: simple mucocele, mucosal hyperplasia, mucinous cystadenoma, and mucinous cystadenocarcinoma. A simple mucocele is characterized by degenerative epithelial changes due to obstruction and distention of the appendix. This type represents 20%-30% of cases. A simple mucocele is caused by mucus distention secondary to an obstruction of the appendix due to fecaliths, post-inflammatory scarring, or rarely, endometriosis. Mucosal hyperplasia is similar to a hyperplastic colon polyp histologically. This type represents 20%-30% of cases. Mucinous cystadenoma is a neoplasm that presents with a tubular or papillary pattern, with mucus production and adenomatous epithelium. This type represents 30%-50% of cases. Mucinous cystadenocarcinoma differs from cystadenoma because glandular and stromal invasion is involved. Previously, it was believed that only mucinous cystadenocarcinoma could cause pseudomyxoma peritonei (PMP), but it has recently been reported that other types of mucocele can cause PMP. Ruiz-Tovar et al[3] presented a case of simple mucocele that was apparently not perforated and developed PMP.
Consequently, the preoperative diagnosis of mucocele of the appendix is crucial. Colonoscopy, ultrasonography (USG), CT and MRI are used for diagnosis. On colonoscopy, the appearance of the appendiceal orifice at the center of the mound has been called the “volcano sign”. USG can be used to differentiate between acute appendicitis and mucocele. Dilatation of the appendiceal lumen to ≥ 15 mm suggests mucocele with 83% sensitivity and 92% specificity. CT offers better specificity in establishing a diagnosis of mucocele. The typical features are cystic masses that are well circumscribed with low attenuation. Wall calcifications are observed in 50% of cases, and they strongly suggest mucocele. In addition, enhancing nodules in the mucocele wall suggest cystadenocarcinoma. MRI is also useful in establishing a diagnosis of mucocele. On MRI, mucocele appears as a cystic mass with low to intermediate signal intensity on T1-WI and high signal intensity on T2-WI. These findings can be attributed to the high protein content of a mucocele[16]. In our case, the CT, MRI and colonoscopy imaging results were compatible with these findings.
When mucocele of the appendix is diagnosed preoperatively, open surgery is favored over laparoscopy to prevent rupture of the mucocele, which may induce PMP. If mucocele is detected during a laparoscopic procedure, the patient must undergo conversion to open surgery.
Appendiceal endometriosis is diagnosed pathologically. Glandular tissue, endometrial stroma, and hemorrhage are typically assessed in patients who present with endometriosis[17]. Approximately half of the cases of endometriosis of the appendix involve the body and half involve the tip of the appendix. Muscular and seromuscular involvement occurs in two-thirds of patients, and the serosal surface is involved in one-third of patients. The mucosa is not involved and the submucosa is involved in one-third of patients. There was no relationship between the location of the endometriotic foci and the symptoms of our patient, who had endometriosis with muscular involvement.
Hapke et al[5] noted that the progression of mucocele of the appendix due to endometriosis consists of the following steps. Endometriosis results in smooth muscle hypertrophy of the appendix, including the muscularis mucosa, with obstruction of some of the gland crypts. These obstructions lead to local increased mucin production from multiple small cysts. Ultimately, several of these small cysts coalesce, resulting in a single layer cyst that can be dissected through the submucosa proximally. In our case, multiple small cysts were observed surrounding the appendix. These findings confirm the proposal of Hapke et al[5].
There are only 10 previously reported cases of a similar condition in the English literature[4-12]. We reviewed these reported cases and the present case. The mean age at presentation was 34 years (22-56 years). The patients presented various symptoms: four had recurrent abdominal pain during menstrual periods; three had chronic pelvic pain; two had acute abdominal pain with vomiting; one had increasing menorrhagia (she had complicated uterine myomas); and another had no symptoms. Preoperative diagnosis of mucocele was made in five cases; diagnostic laparoscopy was performed in five cases; and in one case, it was found by chance during surgery. Open surgery was performed in six cases, and two experienced rupture during surgery. The mean tumor size was 2.5 cm (1.3-5.5 cm). Nine cases had a single cyst, and two had multiple cysts. One case was complicated with intussusception and another with ureteric obstruction.
In summary, we report a rare case of mucocele of the appendix due to endometriosis and provide the first review of the literature.
P- Reviewer Liu Y S- Editor Gou SX L- Editor Kerr C E- Editor Li JY
| 1. | García Lozano A, Vázquez Tarrago A, Castro García C, Richart Aznar J, Gómez Abril S, Martínez Abad M. Mucocele of the appendix: Presentation of 31 cases. Cir Esp. 2010;87:108-112. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 28] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 2. | Higa E, Rosai J, Pizzimbono CA, Wise L. Mucosal hyperplasia, mucinous cystadenoma, and mucinous cystadenocarcinoma of the appendix. A re-evaluation of appendiceal “mucocele”. Cancer. 1973;32:1525-1541. [PubMed] |
| 3. | Ruiz-Tovar J, Teruel DG, Castiñeiras VM, Dehesa AS, Quindós PL, Molina EM. Mucocele of the appendix. World J Surg. 2007;31:542-548. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 74] [Cited by in RCA: 81] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 4. | Driman DK, Melega DE, Vilos GA, Plewes EA. Mucocele of the appendix secondary to endometriosis. Report of two cases, one with localized pseudomyxoma peritonei. Am J Clin Pathol. 2000;113:860-864. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 32] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 5. | Hapke MR, Bigelow B. Mucocele of the appendix secondary to obstruction by endometriosis. Hum Pathol. 1977;8:585-589. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 26] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 6. | Kimura H, Konishi K, Yabushita K, Maeda K, Tsuji M, Miwa A. Intussusception of a mucocele of the appendix secondary to an obstruction by endometriosis: report of a case. Surg Today. 1999;29:629-632. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 20] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 7. | Nopajaroonsri C, Mreyoud N. Retention mucocele of appendix due to endometriosis. South Med J. 1994;87:833-835. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 15] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 8. | O’Sullivan MJ, Kumar U, Kiely EA. Ureteric obstruction with mucocoele of the appendix due to endometriosis. BJOG. 2001;108:124-125. [PubMed] |
| 9. | Abrao MS, Podgaec S, Carvalho FM, Gonçalves MO, Dias JA, Averbach M. Bowel endometriosis and mucocele of the appendix. J Minim Invasive Gynecol. 2005;12:299-300. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 10. | Miyakura Y, Kumano H, Horie H, A T Lefor, Yamaguchi T. Rupture of appendiceal mucocele due to endometriosis: report of a case. Clin J Gastroenterol. 2012;5:220-224 [DOI 10.1007/s12328-012-0302-9]. |
| 11. | Kohout E. Mucocele of the appendix caused by endometriosis. Am J Obstet Gynecol. 1960;79:1181-1183. [PubMed] |
| 12. | Shemilt P. Endometrioma of the caecum causing mucocele of the appendix. Br J Surg. 1949;37:118-120. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 10] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 13. | Collins DC. 71,000 Human appendix specimens. a final report, summarizing forty years’ study. Am J Proctol. 1963;14:265-281. [PubMed] |
| 14. | Uohara JK, Kovara TY. Endometriosis of the appendix. Report of twelve cases and review of the literature. Am J Obstet Gynecol. 1975;121:423-426. [PubMed] |
| 15. | Berker B, Lashay N, Davarpanah R, Marziali M, Nezhat CH, Nezhat C. Laparoscopic appendectomy in patients with endometriosis. J Minim Invasive Gynecol. 2005;12:206-209. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 42] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 16. | Koga H, Aoyagi K, Honda H, Fujishima M. Appendiceal mucocele: sonographic and MR imaging findings. AJR Am J Roentgenol. 1995;165:1552. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 9] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 17. | Uncu H, Taner D. Appendiceal endometriosis: two case reports. Arch Gynecol Obstet. 2008;278:273-275. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 18] [Article Influence: 1.1] [Reference Citation Analysis (0)] |