Published online Jan 21, 2013. doi: 10.3748/wjg.v19.i3.394
Revised: November 23, 2012
Accepted: December 15, 2012
Published online: January 21, 2013
Processing time: 116 Days and 19.6 Hours
AIM: To compare the clinical outcome of single-incision laparoscopic cholecystectomy (SILC) with three-port laparoscopic cholecystectomy (TPLC).
METHODS: Between 2009 and 2011, one hundred and two patients with symptomatic benign gallbladder diseases were randomized to SILC (n = 49) or TPLC (n = 53). The primary end point was post operative pain score (at 6 h and 7 d). Secondary end points were blood loss, operation duration, overall complications, postoperative analgesic requirements, length of hospital stay, cosmetic result and total cost. Surgical techniques were standardized and all operations were performed by one experienced surgeon, who had performed more than 500 laparoscopic cholecystectomies.
RESULTS: One patient in the SILC group required conversion to two-port LC. There were no open conversions or major complications in either treatment groups. There were no differences in terms of estimated blood loss (mean ± SD, 14 ± 6.0 mL vs 15 ± 4.0 mL), operation duration (mean ± SD, 41.8 ± 17.0 min vs 38.5 ± 22.0 min), port-site complications (contusion at incision: 5 cases vs 4 cases and hematoma at incision: 2 cases vs 1 case), total cost (mean ± SD, 12 075 ± 1047 RMB vs 11 982 ± 1153 RMB) and hospital stay (mean ± SD, 1.0 ± 0.5 d vs 1.0 ± 0.2 d) , respectively. TPLC had a significantly worse visual analogue pain score at 8 h after surgery (mean ± SD, 3.5 ± 1.6 vs 2.0 ± 1.5), however, the scores were similar on day 7 (mean ± SD, 2.5 ± 1.4 vs 2.0 ± 1.3). Cosmetic satisfaction, as determined by a survey at 2 mo follow-up favored SILC (mean ± SD, 8 ± 0.4 vs 6 ± 0.2).
CONCLUSION: SILC is a safe and feasible approach in selected patients. The main advantages are a better cosmetic result and less pain.
-
Citation: Pan MX, Jiang ZS, Cheng Y, Xu XP, Zhang Z, Qin JS, He GL, Xu TC, Zhou CJ, Liu HY, Gao Y. Single-incision
vs three-port laparoscopic cholecystectomy: Prospective randomized study. World J Gastroenterol 2013; 19(3): 394-398 - URL: https://www.wjgnet.com/1007-9327/full/v19/i3/394.htm
- DOI: https://dx.doi.org/10.3748/wjg.v19.i3.394
Laparoscopic cholecystectomy (LC) has become one of the most effective procedures for the treatment of benign gallbladder pathology since its introduction in 1985[1]. However, surgical standards of practice continue to evolve toward less invasive approaches, therefore many researchers have attempted to minimize the invasiveness by reducing the number and size of the ports. In this context, single-port laparoscopic cholecystectomy (SILC) emerged in 1997[2]. The proposed advantages of SILC include fewer port sites with the potential for decreased pain, cosmetic benefit and faster recovery[3-10]. Some investigators have predicted that it may become a standard approach to LC[11,12]. However, it has also been suggested that SILC has many disadvantages, such as the technique is difficult to handle, prolonged operative time, cost of special instruments and increased risk of per-operative complications[9,13]. It is difficult to make an unbiased comparison between SILC and multi-port LC because of lack of prospective, randomized controlled trials (RCT). Therefore, we designed and conducted this RCT to evaluate the advantages and disadvantages of SILC and three-port laparoscopic cholecystectomy (TPLC).
Inclusion criteria were as follows: (1) patients aged between 18 and 70 years; (2) body mass index less than 40 kg/m2; (3) preoperative diagnosis of symptomatic gallstones or gallbladder polyps, and (4) willing to comply with the protocol requirements and signed written informed consent.
Exclusion criteria were as follows: (1) American Society of Anesthesiologists class IV and V; (2) Patients with contraindication to laparoscopy; (3) Patients with suspected Mirizzi syndrome, common duct stones or malignancy; (4) Patients with previous upper abdominal surgery; (5) Patients on long-term anticoagulant treatment; (6) Acute cholecystitis or choledocholiathiasis; and (7) Gallstones > 3 cm in diameter.
Eligible patients were randomized into two groups (SILC and TPLC) using sealed opaque envelopes which contained a computer-generated random number. Before the trial, all patients underwent basic investigations such as blood tests, electrocardiogram, ultrasonography of the abdomen and radiologic imaging such as chest radiograph. All operations were performed by one experienced surgeon, who had performed more than 500 laparoscopic cholecystectomies.
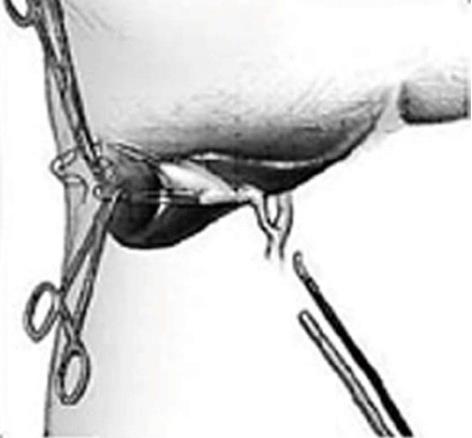
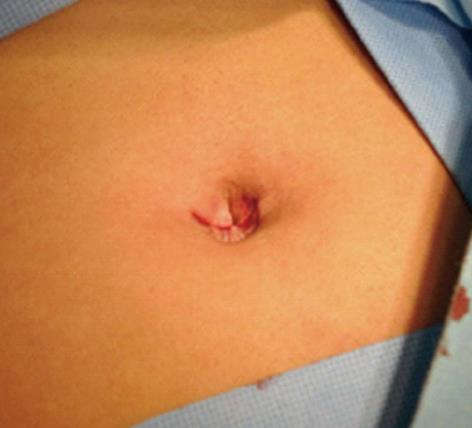
Surgical techniques were standardized. SILC was performed with the help of 2 slings of sutures, which included four steps: (1) Under general anesthesia, a 20 mm (approximately) bracket-shaped skin incision was made through the inner margin of the umbilicus and a pneumoperitoneum was set at 13 mmHg. One 10 mm trocar (Kanger, Tong Lu, China) to allow the insertion of a 30 degree laparoscope (Olympus, Tokyo, Japan) was inserted through the abdomen at the left side of the incision and a 5 mm trocar (Kanger, Tong Lu, China) was inserted at the right side for the harmonic scalpel. The tissues between the trocars were preserved to prevent air leakage; (2) The first suture using a straight needle was inserted through the right 7th intercostal space in the anterior axillary line, and the seromuscular layer of the gallbladder fundus was punctured and retracted toward the anterior abdominal wall. Hartmann’s pouch was punctured and retracted using the second suture to expose Calot’s triangle (Figure 1); (3) The harmonic scalpel (Ethicon Endo-Surgery, Cincinnati, OH, United States) was used to dissect Calot’s triangle. Once the cystic artery and duct have been exposed, the cystic artery was cut using the harmonic scalpel, and the cystic duct was triple clipped and divided; and (4) The harmonic scalpel was used to dissect the gallbladder from the gallbladder fossa. When the gallbladder was free, the 5 mm trocar was exchanged for a 10 mm one, and through the 10 mm port, a specemen bag was inserted and the gallbladder was extracted after removal of the suspending sutures from the abdominal wall. The umbilical incision was closed and restored and no drainage tube was left in place (Figure 2).
In TPLC, a sub-umbilical incision, sub-xiphoid incision and right sub-costal incision were made. A 10 mm trocar placed in the sub-umbilical incision allowed the introduction of laparoscope and the other two trocars, a 10 mm and a 5 mm, respectively, were placed for the grasp and harmonic scalpel. The operation was performed following the routine TPLC procedure[14], however, the cystic artery was divided and cut using the harmonic scalpel instead of being clipped and divided. The primary end-point of the study was the postoperative pain score (at 6 h and 7 d). Secondary end-points included blood loss, operation duration, overall complications (intra- and post-operative complications), postoperative analgesic requirements, length of hospital stay, cosmetic result and total cost. A standard visual analog scale [range, 0 (no pain) to 10 (maximum pain)] was used for assessments at 8 h after surgery and on postoperative day 7. Cosmetic satisfaction of the surgical scar was rated on a scale [range, 0 (worst) to 10 (best)], and was evaluated at the 2-mo follow-up visit.
Statistical analysis was accomplished using the SPSS program for Windows 12.0 (SPSS, Chicago, IL, United States). The χ2 test or the t test was used as indicated. All data were presented as mean ± SD. All P values were 2-sided. A P value of 0.05 was considered statistically significant.
From January 2009 to March 2011, 108 eligible patients were randomized to SILC (n = 51) or TPLC (n = 57). Two patients in the TPLC group and four patients in the SILC group refused to participate before surgery. In total, 102 patients (SILC, n = 49; TPLC, n = 53) were analyzed. Demographic variables in the two groups were similar (Table 1). All patients in the TPLC group successfully underwent three-port laparoscopic cholecystectomy without conversion to open surgery. Of 49 patients in the SILC group, one patient was converted to two-port LC due to anatomical difficulties and the operator felt it was unsafe to proceed with SILC. Overall, No major intra- or post-operative complications, such as biliary injury, abscess, bleeding, biliary collection or port-site hernia were observed in the two treatment groups. Several patients experienced port-site complications such as contusion and hematoma, however, all recovered a few days after surgery. There were no significant differences in estimated blood loss (14 ± 6.0 mL vs 15 ± 4.0 mL; P = 0.2643), operation duration (41.8 ± 17.0 min vs 38.5 ± 22.0 min; P = 0.4222), port-site complications (contusion at incision: 5 cases vs 4 cases; P = 0.7350 and hematoma at incision: 2 vs 1; P = 0.6070), hospital stay (1.0 ± 0.5 d vs 1.0 ± 0.2 d; P = 1.0000) and total cost (12 075 ± 1047 RMB vs 11 982 ± 1153 RMB; P = 0.6715) between the SILC and TPLC groups. However, the TPLC group had a significantly worse visual analogue pain score at 8 h after surgery (3.5 ± 1.6 vs 2.0 ± 1.5; P = 0.0000), but the score was similar on day 7 (2.5 ± 1.4 vs 2.0 ± 1.3; P = 0.0651). Cosmetic satisfaction as shown by the cosmetic score was significantly higher in the SILC group than in the TPLC group (8 ± 0.4 vs 6 ± 0.2; P = 0.0000) (Table 1).
| SILC (n = 49) | TPLC (n = 53) | P value | |
| Age (yr) | 43.8 ± 14.0 | 45.2 ± 11.0 | 0.5493 |
| Female | 26 | 31 | 0.5810 |
| WI (kg/m2) | 24.3 ± 6.0 | 25.1 ± 5.0 | 0.4649 |
| ASA | 1.5 ± 0.2 | 1.6 ± 0.3 | 0.0676 |
| Clinical diagnosis | 0.7790 | ||
| Cholecystolithiasis | 32 | 36 | |
| Cystic polyps | 17 | 17 | |
| Operation duration (min) | 41.8 ± 17.0 | 38.5 ± 22.0 | 0.4222 |
| EBL (mL) | 14 ± 6.0 | 15 ± 4.0 | 0.2643 |
| VAS (1–10) | |||
| 8 h after surgery | 2.0 ± 1.5 | 3.5 ± 1.6 | 0.0000 |
| Day 7 after surgery | 2.0 ± 1.3 | 2.5 ± 1.4 | 0.0651 |
| Complications | |||
| Contusion at incision | 5 | 4 | 0.7350 |
| Hematoma at incision | 2 | 1 | 0.6070 |
| Hospital stay (d) | 1.0 ± 0.5 | 1.0 ± 0.2 | 1.0000 |
| Cosmetic score | 8 ± 0.4 | 6 ± 0.2 | 0.0000 |
| Total cost (RMB) | 12 075 ± 1047 | 11 982 ± 1153 | 0.6715 |
SILC has attracted wide attention because of its potential cosmetic results. It may even be possible for this approach to become a gold standard for cholecystectomy[11,12]. However, there is still a long way to go before this approach is a gold standard, as standardization, safety, and the cosmetic results of SILC require validation[15]. Although recent reports have focused on comparisons between SILC and multi-port LC, the safety, better cosmetic results and faster recovery following SILC have been agreed, however, SILC has not been standardized and there is much technical variation. On the one hand, different surgeons have attempted SILC in different ways. For example, in exposing Calot’s triangle, trials using sutures, Kirschner wires and loop retractors have been reported, in addition to different manipulative instruments, such as straight instruments and reticulating instruments[7]. On the other hand, devices used to prevent air leakage vary from one surgeon to another: some use common trocars[8], some tend to use SILS multi-port[7] and others favor self-designed devices such as sterile gloves[16]. In our center, we have tried many approaches in the initial stage. For example, to prevent air leakage, we have tried tri-port and gel-port, but due to their high cost in special ports and larger lesions of about 3 cm requiring a trans-umbilical incision these devices are no longer used. We decided to select routine trocars in our practice because they were sufficient to prevent air leakage and were more economical. With regard to the selection of surgical instruments, we use the suture suspension method in SILC, which requires only a 30 degree laparoscope and a manipulative instrument, eliminating the need for more instruments intra-operatively.
In practice, we focus on improving the auxiliary procedure with suspension sutures. To achieve ideal exposure of Calot’s triangle, we select the puncture spot at the superior chest wall along the costal margin so that the suspension suture can draw the liver up a bit more than in other places, different to Piskun et al[17] that the puncture spot should be selected at the inferior costal margin. In addition, the harmonic scalpel is effective for occluding 3 mm blood vessels and dissecting tissues[18]. In our experience, cystic arteries in the trial were cut using the harmonic scalpel, indicating the safety of this scalpel. Intra-operative management of the gallbladder is critical for the safety in SILC. Initially, we were perplexed as to how to handle intra-operative bile leakage. First, we placed the suspension sutures into the seromuscular layer to avoid perforation of the cyst wall, but this was inevitable sometimes. Subsequently, we found that this technique was useful as long as evacuating and repeated rinsing were conducted.
There have been a few comparisons between SILC and conventional multi-port LC[19-22]. These studies concluded that SILC is superior to multi-port LC in terms of cosmetic outcome, but not in terms of total cost, surgical time and postoperative pain. A similar cosmetic outcome in both treatment groups was observed in our study. However, there was no significant difference in the total cost between SILC and traditional LC when standard materials were selected. In addition, we found that SILC resulted in less postoperative pain than TPLC, and no significant difference in operation duration was observed between the two techniques. The higher pain score may be explained by the fact that there are more incisions in TPLC and the size of the incisions is larger than those in SILC. The different outcome of surgical time could be explained by difference in experience of the surgeon in SILC.
In conclusion, the results of this prospective trial demonstrate that SILC is a safe procedure when conducted by experienced surgeons, with some outcomes similar to that of TPLC, however, SILC was superior in terms of cosmetic outcome and postoperative pain. In the future, more high-powered randomized studies comparing SILC with conventional LC will be needed to validate its objective benefits and clinical role during the follow-up.
Laparoscopic cholecystectomy (LC) has been regarded as the “gold standard” for the management of benign gallbladder diseases since its introduction in 1985. However, surgical standards of practice continue to evolve toward less invasive approaches, therefore many researchers have attempted to minimize the invasiveness by reducing the number and size of the ports. In this context, single-incision laparoscopic cholecytectomy (SILC) emerged as a complement to standard LC. The proposed advantages of SILC include fewer port sites with the potential for decreased pain, cosmetic benefit and faster recovery. Some investigators have predicted that it may become a standard approach in LC. However, it has also been suggested that SILC has many disadvantages, such as the technique is difficult to handle, prolonged operative time, cost of special instruments and increased risk of per-operative complications. Therefore, it is difficult to make an unbiased comparison between SILC and multi-port LC due to the lack of prospective, randomized controlled trials.
SILC has attracted wide attention because of its potential cosmetic results. However, it is unknown whether SILC could become a new standard preocedure, and therefore it is necessary to compare the clinical outcome of SILC and multiple-port laparoscopic cholecystectomy.
This prospective randomized study was performed to explore the safety and feasibility of SILC for the treatment of benign gallbladder diseases, and to compare the clinical outcomes with three-port laparoscopic cholecystectomy (TPLC).
In selected patients with benign gallbladder diseases, single-incision laparoscopic cholecystectomy is safe and feasible. The main advantages are that SILC result in a better cosmetic outcome and less pain compared with TPLC.
SILC is a minimally invasive surgical procedure in which cholecystectomy is accomplished exclusively through a single 15-25 mm incision in the patient’s navel. It is complementary to standard LC and an alternative to natural orifice transluminal endoscopic surgery. Unlike the traditional multi-port laparoscopic approach, SILC leaves only a single small scar in the navel.
The authors have compared the clinical outcomes of SILC with TPLC and have concluded that SILC is a safe and feasible approach in selected patients. The main advantage is its better cosmetic result and less pain. The study is well organized and the content is adequately written, patient number is good and the authors have used good technique (harmonic for cystic artery).
P- Reviewers De Nardi P, Shah OJ S- Editor Wen LL L- Editor A E- Editor Li JY
| 1. | Solomon D, Bell RL, Duffy AJ, Roberts KE. Single-port cholecystectomy: small scar, short learning curve. Surg Endosc. 2010;24:2954-2957. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 85] [Cited by in RCA: 91] [Article Influence: 6.1] [Reference Citation Analysis (0)] |
| 2. | Navarra G, Pozza E, Occhionorelli S, Carcoforo P, Donini I. One-wound laparoscopic cholecystectomy. Br J Surg. 1997;84:695. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 30] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 3. | Barbaros U, Sümer A, Tunca F, Gözkün O, Demirel T, Bilge O, Randazzo V, Dinççağ A, Seven R, Mercan S. Our early experiences with single-incision laparoscopic surgery: the first 32 patients. Surg Laparosc Endosc Percutan Tech. 2010;20:306-311. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 27] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 4. | Yu WB, Zhang GY, Li F, Yang QY, Hu SY. Transumbilical single port laparoscopic cholecystectomy with a simple technique: initial experience of 33 cases. Minim Invasive Ther Allied Technol. 2010;19:340-344. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 11] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 5. | Gajda Z. 3 attempts at isolating lectures on dentistry at the Jagellonian University in the 1st half of the 19th century. Czas Stomatol. 1979;32:199-202. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 16] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 6. | Hirano Y, Watanabe T, Uchida T, Yoshida S, Tawaraya K, Kato H, Hosokawa O. Single-incision laparoscopic cholecystectomy: single institution experience and literature review. World J Gastroenterol. 2010;16:270-274. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 76] [Cited by in RCA: 79] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 7. | Ponsky TA. Single port laparoscopic cholecystectomy in adults and children: tools and techniques. J Am Coll Surg. 2009;209:e1-e6. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 22] [Reference Citation Analysis (0)] |
| 8. | Kirschniak A, Bollmann S, Pointner R, Granderath FA. Transumbilical single-incision laparoscopic cholecystectomy: preliminary experiences. Surg Laparosc Endosc Percutan Tech. 2009;19:436-438. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 23] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 9. | Edwards C, Bradshaw A, Ahearne P, Dematos P, Humble T, Johnson R, Mauterer D, Soosaar P. Single-incision laparoscopic cholecystectomy is feasible: initial experience with 80 cases. Surg Endosc. 2010;24:2241-2247. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 70] [Cited by in RCA: 74] [Article Influence: 4.9] [Reference Citation Analysis (0)] |
| 10. | Rivas H, Varela E, Scott D. Single-incision laparoscopic cholecystectomy: initial evaluation of a large series of patients. Surg Endosc. 2010;24:1403-1412. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 153] [Cited by in RCA: 149] [Article Influence: 9.9] [Reference Citation Analysis (0)] |
| 11. | Emami CN, Garrett D, Anselmo D, Torres M, Nguyen NX. Single-incision laparoscopic cholecystectomy in children: a feasible alternative to the standard laparoscopic approach. J Pediatr Surg. 2011;46:1909-1912. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 22] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 12. | Jacob DA, Raakow R. Single-port transumbilical endoscopic cholecystectomy: a new standard? Dtsch Med Wochenschr. 2010;135:1363-1367. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 7] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 13. | Elsey JK, Feliciano DV. Initial experience with single-incision laparoscopic cholecystectomy. J Am Coll Surg. 2010;210:620-624, 624-626. [PubMed] |
| 14. | Trichak S. Three-port vs standard four-port laparoscopic cholecystectomy. Surg Endosc. 2003;17:1434-1436. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 53] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 15. | Allemann P, Schafer M, Demartines N. Critical appraisal of single port access cholecystectomy. Br J Surg. 2010;97:1476-1480. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 56] [Cited by in RCA: 57] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 16. | Song SC, Ho CY, Kim MJ, Kim WS, You DD, Choi DW, Choi SH, Heo JS. Clinical Analysis of Single-Port Laparoscopic Cholecystectomies: Early Experience. J Korean Surg Soc. 2011;80:43-50. [RCA] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 5] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 17. | Piskun G, Rajpal S. Transumbilical laparoscopic cholecystectomy utilizes no incisions outside the umbilicus. J Laparoendosc Adv Surg Tech A. 1999;9:361-364. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 325] [Cited by in RCA: 304] [Article Influence: 11.7] [Reference Citation Analysis (0)] |
| 18. | Bessa SS, Al-Fayoumi TA, Katri KM, Awad AT. Clipless laparoscopic cholecystectomy by ultrasonic dissection. J Laparoendosc Adv Surg Tech A. 2008;18:593-598. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 20] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 19. | Leung D, Yetasook AK, Carbray J, Butt Z, Hoeger Y, Denham W, Barrera E, Ujiki MB. Single-incision surgery has higher cost with equivalent pain and quality-of-life scores compared with multiple-incision laparoscopic cholecystectomy: a prospective randomized blinded comparison. J Am Coll Surg. 2012;215:702-708. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 418] [Cited by in RCA: 240] [Article Influence: 17.1] [Reference Citation Analysis (0)] |
| 20. | Lee PC, Lo C, Lai PS, Chang JJ, Huang SJ, Lin MT, Lee PH. Randomized clinical trial of single-incision laparoscopic cholecystectomy versus minilaparoscopic cholecystectomy. Br J Surg. 2010;97:1007-1012. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 127] [Cited by in RCA: 136] [Article Influence: 9.1] [Reference Citation Analysis (0)] |
| 21. | Lai EC, Yang GP, Tang CN, Yih PC, Chan OC, Li MK. Prospective randomized comparative study of single incision laparoscopic cholecystectomy versus conventional four-port laparoscopic cholecystectomy. Am J Surg. 2011;202:254-258. [PubMed] |
| 22. | Gangl O, Hofer W, Tomaselli F, Sautner T, Függer R. Single incision laparoscopic cholecystectomy (SILC) versus laparoscopic cholecystectomy (LC)-a matched pair analysis. Langenbecks Arch Surg. 2011;396:819-824. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 47] [Cited by in RCA: 56] [Article Influence: 4.0] [Reference Citation Analysis (0)] |