Published online Feb 28, 2012. doi: 10.3748/wjg.v18.i8.806
Revised: June 9, 2011
Accepted: June 16, 2011
Published online: February 28, 2012
AIM: To access the short-term outcomes of simultaneous laparoscopic surgery combined with resection for synchronous lesions in patients with colorectal cancer.
METHODS: Between March 1996 and April 2010 prospectively collected data were reviewed from 93 consecutive patients who had colorectal cancer and underwent simultaneous multiple organ resection (combined group) and 1090 patients who underwent conventional laparoscopic right hemicolectomy or laparoscopic low/anterior resection for colorectal cancer (non-combined group). In the combined group, there were nine gastric resections, three nephrectomies, nine adrenalectomies, 56 cholecystectomies, and 21 gynecologic resections. In addition, five patients underwent simultaneous laparoscopic resection for three organs. The patient demographics, intra-operative outcomes, surgical morbidity, and short-term outcomes were compared between the two groups (the combined and non-combined groups).
RESULTS: There were no significant differences in the clinicopathological variables between the two groups. The operating time was significantly longer in the combined group than in the non-combined group, regardless of tumor location (laparoscopic right hemicolectomy and laparoscopic low/anterior resection groups; P = 0.048 and P < 0.001, respectively). The other intra-operative outcomes, such as the complications and open conversion rate, were similar in both groups. The rate of post-operative morbidity in the combined group was similar to the non-combined group (combined vs non-combined, 15.1% vs 13.5%, P = 0.667). Oncological safety for the colon and synchronous lesions were obtained in the combined group.
CONCLUSION: Simultaneous laparoscopic multiple organ resection combined with colorectal cancer is a safe and feasible option in selected patients.
- Citation: Kim HJ, Choi GS, Park JS, Park SY, Jun SH. Simultaneous laparoscopic multi-organ resection combined with colorectal cancer: Comparison with non-combined surgery. World J Gastroenterol 2012; 18(8): 806-813
- URL: https://www.wjgnet.com/1007-9327/full/v18/i8/806.htm
- DOI: https://dx.doi.org/10.3748/wjg.v18.i8.806
The laparoscopic approach for colorectal cancer was in-troduced during the last decade, and the oncological sa-fety and short-term outcomes have been demonstrated in randomized prospective trials[1-5]. As a result, the laparoscopic approach has been increasingly used to treat colorectal cancer, and this approach for other abdominal organs has also been widely accepted and performed[6-9]. The remarkable development of the laparoscopic approach is due to its unique benefits over open surgery, such as less pain, shorter hospital stay, faster recovery period, and better cosmetic results.
Simultaneous resection of synchronous abdominal lesions requiring surgical intervention is likely to benefit patients by reducing psychological and physiological stress related to re-operation. Some patients with sporadic colorectal cancer have one or more co-existing intra-abdominal diseases that require simultaneous resection with the primary colorectal cancer. This combined surgery could result in increased tissue injury and morbidity related to the longer operative time, as well as a larger or more radical incision, especially when the target organ is distant from the colorectal cancer. Fortunately, the laparoscopic approach can be applied to almost all intra-abdominal surgical procedures. Well-planned positioning of trocars, and a common mini-incision for retrieval of specimens, would maximize the advantages of laparoscopic surgery, even in cases with simultaneous multi-organ resection. However, the laparoscopic approach for greater than two co-existing abdominal disorders, especially colorectal cancer, is rarely performed and is the subject of few case reports in the literature[10-14]. Furthermore, no studies have compared laparoscopic combined resection in colorectal cancer patients with conventional laparoscopic colorectal resection. Therefore, it remains unknown whether or not a laparoscopic approach is safe and beneficial in patients with colorectal cancer undergoing simultaneous combined resection on synchronous abdominal lesions.
In the present study, we clarified the feasibility of simultaneous laparoscopic surgery combined with resection for synchronous lesions in patients with colorectal cancer. The study will elucidate the oncological outcomes in combined resection by comparing findings in patients who underwent conventional laparoscopic non-combined colorectal resection. We also described the technical details related to laparoscopic multiple organ resection combined with colorectal cancer.
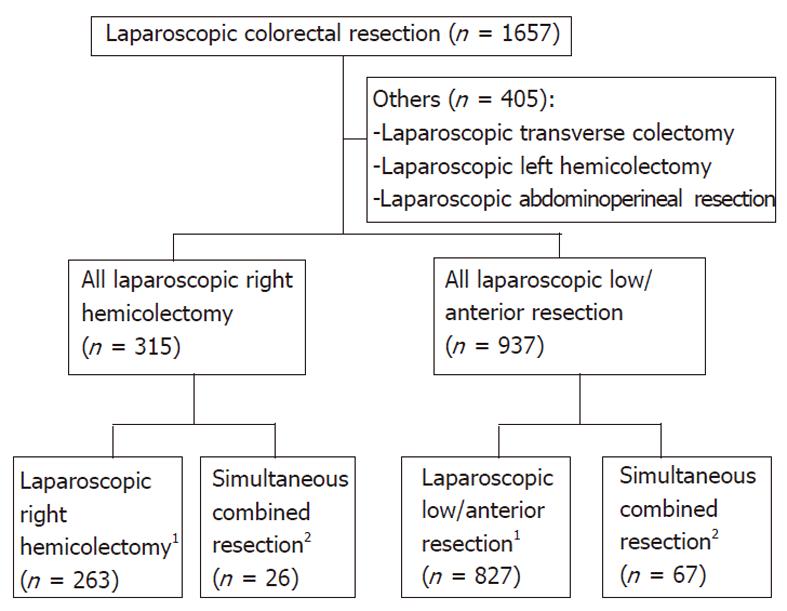
Between January 1996 and March 2010, 1657 patients underwent laparoscopic resection for colorectal cancer by one surgeon at the Kyungpook National University Hospital in Daegu, South Korea. Three hundred fifteen patients underwent laparoscopic right hemicolectomy and 937 patients underwent laparoscopic anterior or low anterior resection. Patients who had distant metastases, including metastasis of the liver, en-bloc regional resection due to T4 serosal invasive lesions, or patients who underwent palliative resection or emergency operations caused by perforation or obstruction of the colon and rectum, were excluded. Patients who underwent transverse colectomy or left hemicolectomy were also excluded because of the absence of simultaneous resection during these surgical procedures. Therefore, 263 patients who underwent laparoscopic right hemicolectomies were matched to 26 patients who underwent combined organ resections with right hemicolectomies. In addition, 827 patients who underwent single low/anterior resections were matched to 67 patients who underwent simultaneous low/anterior resections and other intra-abdominal organ procedures (Figure 1).
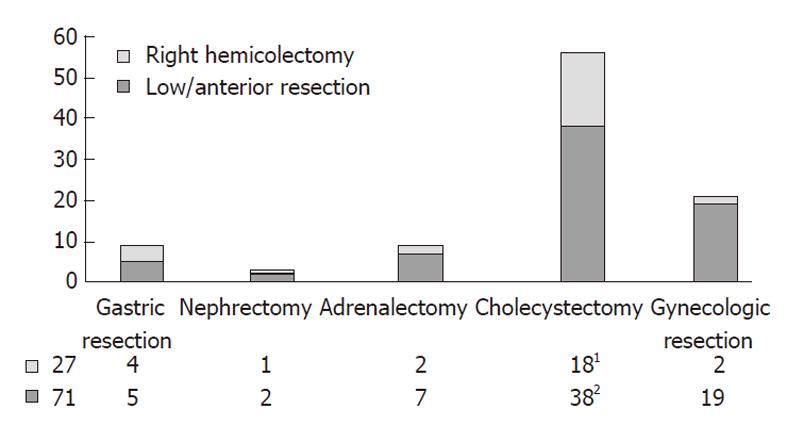
Figure 2 shows the type of simultaneous combined resection according to the location of synchronous ab-dominal lesions, distinguished between the primary colorectal resections. Five gastric resections were laparoscopically-assisted distal gastrectomies with more than D1+α lymph node dissection for gastric cancer[15], and four were laparoscopic gastric wedge resections for submucosal tumors. Five patients underwent laparoscopic simultaneous resection of three organs.
Data on patient demographics, medical co-morbidities, operative details related to laparoscopic combined resections, short-term post-operative outcomes, and pathological findings were collected prospectively and entered into a database of colorectal malignancies.
The following tests and studies were performed pre-operatively: tumor markers; colonoscopy; abdominal computed tomography; and positron emission tomography. Endocrine function tests, ultrasonography, and gastroduodenoscopy were also performed when synchronous lesions were noted for surgical planning purposes.
All surgeries were performed with curative intent, irrespective of the location of the synchronous lesions. All procedures were performed by one surgeon (Choi GS), and the same surgeon performed the combined multiple abdominal resections.
Laparoscopic right hemicolectomy: The patients were placed in the supine or modified lithotomy position in Trendelenburg slightly tilted to the left side. An 11-mm infra-umbilical camera port was placed, two 5-mm trocars were introduced into the right upper and lower quadrants as operating ports, and two additional 5-mm trocars were placed in the left as assistant ports. The surgical technique for the laparoscopic right hemicolectomy was described in a previous report[16]. After D3 lymph node dissection and full mobilization of the right colon, the surgeon moved to the other abdominal lesions. No additional trocars were required. The surgeon changed his position to the right only when performing an operation on left-side lesions. During gastric resections the heads of the patients were elevated, and during nephrectomies the patients were changed to the lateral decubitus position. Ileocolic anastomosis was performed intra- or extra-corporeally, and the other abdominal organs were resected using a routine approach, as described previously[6-8,15,17,18]. Mini-laparotomies were then performed in the upper midline or midline, to extend the umbilical port through which the specimens were extracted and anastomoses were performed.
Laparoscopic low/anterior resection: Initially, the pa-tient was placed in the modified lithotomy position in Trendelenburg with a slight tilt to the right side. An 11-mm infra-umbilical camera port was placed, a 12-mm trocar was placed in the right lower quadrant, and two additional 5-mm trocars were placed in the right upper and left lower quadrant as operating and assistant ports. The surgical technique used at our institution for the laparoscopic anterior and low anterior resections with total mesorectal excision has been previously described[16,19]. Following transection of the rectum, the surgeon approached the other abdominal lesions. In gastric resections and right nephrectomies, an additional trocar was required in the left upper quadrant. The positions of the surgeon and patients were changed in the same way for laparoscopic right hemicolectomies. Then, mini-laparotomies were performed in the upper midline or midline to extend the umbilical port, or the left lower quadrant transversely. The specimen was extracted and an anastomosis was performed.
Data analysis was performed using SPSS 17.0 (SPSS, Inc., Chicago, IL, United States). Clinicopathological variables between the groups were compared using the Fisher’s exact test for categorical data and the Student’s t test for continuous variables. A P value < 0.05 was considered statistically significant.
The clinical characteristics of the patients are summarized in Table 1. All 293 patients underwent elective laparoscopic right hemicolectomy. The two groups (non-combined and combined) were similar with respect to the distribution of age, gender, body mass index and American Society of Anesthesiologists score. Fifty-three (20%) and five patients (19.2%) had a history of previous abdominal surgery in the non-combined and combined groups, respectively (P = 0.911).
| Right hemicolectomy | Low/anterior resection | |||||
| NC group | C group | P value | NC group | C group | P value | |
| (n = 263) | (n = 26) | (n = 827) | (n = 67) | |||
| Age at surgery (yr)1 | 62.7 (28-87) | 65.1 (39-87) | 0.314 | 62.4 (21-92) | 62.3 (38-85) | 0.980 |
| Gender (%) | 0.893 | 0.053 | ||||
| Male | 125 (47.5) | 12 (46.2) | 495 (59.9) | 32 (47.8) | ||
| Female | 138 (52.5) | 14 (53.8) | 332 (40.1) | 35 (52.2) | ||
| BMI (kg/m2)1 | 23.9 (14-22.9) | 23.1 (18.6-30.3) | 0.731 | 23.5 (14.4-40.5) | 24.1 (16.8-31.9) | 0.105 |
| ASA score (%) | 0.510 | 0.666 | ||||
| I | 153 (58.2) | 15 (57.7) | 469 (56.7) | 40 (59.7) | ||
| II | 97 (36.9) | 10 (38.5) | 313 (37.8) | 25 (37.3) | ||
| III | 13 (4.9) | 1 (3.8) | 45 (5.4) | 2 (3) | ||
| History of abdominal surgery (%) | 53 (20.2) | 5 (19.2) | 0.911 | 187 (22.6) | 16 (23.9) | 0.812 |
| Type of resection | 0.602 | |||||
| Right hemicolectomy | 268 (100) | 26 (100) | ||||
| Anterior resection | 350 (42.3) | 29 (43.3) | ||||
| Low anterior resection | 397 (48) | 34 (50.7) | ||||
| Colo-anal anastomosis | 80 (9.7) | 4 (6) | ||||
Table 2 presents data on the surgical aspects and pathological results of primary colon cancer. The mean operating time was significantly longer in the combined group than in the non-combined group [189.6 min (range, 65-397 min) vs 166.9 min (range, 210-320 min), P = 0.048]. Intra-operative complications and conversion to open surgery were similar in both groups. In the combined group, bile leakage due to gallbladder perforation occurred during cholecystectomy in one patient. Conversion to open surgery was required in one patient to remove common bile duct stones noted during intra-operative cholangiography. In this case, we converted to open surgery followed by choledocolithotomy with T-tube insertion. However, we used a right subcostal incision for biliary surgery as well for retrieval of the specimen and performing an anastomosis. There were no significant differences between the groups in the mean post-operative hospital stay (7.8 d in the non-combined group vs 8.6 d in the combined group, P = 0.363) or in the overall and major post-operative complications (P = 0.513 and P = 0.910, respectively).
| Right hemicolectomy | Low/anterior resection | |||||
| NC group | C group | P value | NC group | C group | P value | |
| (n = 263) | (n = 26) | (n = 827) | (n = 67) | |||
| Operation time (min)1 | 166.9 (65-397) | 189.6 (120-320) | 0.048 | 178 (60-430) | 228.1 (80-480) | < 0.001 |
| Intraoperative complication (%) | 6 (2.3) | 1 (3.8) | 0.621 | 43 (5.2) | 5 (7.5) | 0.429 |
| Conversion to open surgery (%) | 2 (0.8) | 1 (3.8) | 0.139 | 4 (0.5) | 1 (1.5) | 0.287 |
| Diverting stoma formation (%) | 0 | 0 | 18 (2.2) | 0 | 0.282 | |
| Postoperative hospital stay (d)1 | 7.8 (4-41) | 8.6 (5-22) | 0.363 | 7.9 (4-34) | 8.8 (5-31) | 0.104 |
| Postoperative complication (%) | ||||||
| Overall | 38 (14.4) | 5 (19.2) | 0.513 | 109 (13.2) | 9 (13.4) | 0.953 |
| Major | 9 (3.4) | 1 (3.8) | 0.910 | 30 (3.6) | 4 (6) | 0.335 |
| Colon pathology1 | ||||||
| Tumor size (cm) | 5.3 (1-15) | 5.5 (2-12) | 0.803 | 4.0 (0.5-17) | 4.2 (0.5-8) | 0.468 |
| Proximal margin (cm) | 18.8 (2-72) | 16.8 (5-45) | 0.394 | 14.1 (1-54.5) | 14 (5.5-30) | 0.943 |
| Distal margin (cm) | 16.9 (1-60) | 18 (3-37) | 0.598 | 4.4 (1-30) | 4.4 (1-14) | 0.945 |
| Retrieved LN | 32.5 (2-93) | 27.4 (7-62) | 0.157 | 16.5 (1-80) | 17.9 (5-65) | 0.264 |
| AJCC stage (%) | 0.352 | 0.803 | ||||
| I | 63 (24) | 3 (11.5) | 277 (33.5) | 20 (29.9) | ||
| II | 119 (45.2) | 14 (53.8) | 282 (34.1) | 25 (37.3) | ||
| III | 81 (30.8) | 9 (34.6) | 268 (32.4) | 22 (32.8) | ||
There were no significant differences between the groups in colon tumor size, proximal and distal margins (all cases had clear resection margins), number of retrieved lymph nodes and American Joint Committee on Cancer stage (6th edition).
The non-combined and combined groups were similar with respect to clinical characteristics of patients who underwent laparoscopic low/anterior resections (Table 1). In laparoscopic resection for primary colorectal cancer, 350 (42.3%) and 29 patients (43.3%) underwent anterior resections, 397 (48%) and 34 patients (50.7%) underwent low anterior resections, and the remaining 80 (9.7%) and four patients (6%) underwent low anterior resections with colo-anal anastomoses, respectively. No significant differences existed between the two groups (P = 0.602).
The mean operating time was significantly longer in the combined group than in the non-combined group [228.1 min (range, 80-480 min) vs 178 min (range, 60-430 min), P≤ 0.001]. The rate of intra-operative complications and conversion to open surgery was similar in both groups. In the combined group, one patient was converted to open surgery because of massive intra-abdominal adhesions associated with two previous operations. There were no cases requiring protective diverting stoma in the combined group. In contrast, 18 patients in the non-combined group required protective diverting stomas (P = 0.282). There were no significant differences between the groups in the mean post-operative hospital stay (7.9 d in the non-combined group vs 8.8 d in the combined group, P = 0.104) or in the overall and major post-operative complications (P = 0.953 and P = 0.335, respectively).
The two groups were similar regarding primary colo-rectal pathology. All cases were performed safely in terms of oncological outcomes.
The post-operative complications in both groups are shown in Table 3. There were no significant differences between the groups (P = 0.667). In the combined group, post-operative complications developed in 14 patients (15.1%). Three patients had anastomosis leakages that were controlled by conservative management without the need to perform a temporary stoma. Two patients underwent percutaneous drainage to resolve pelvic fluid collections or intra-abdominal abscesses. One patient had bile leakage related to combined procedures on post-operative 1 d, but this resolved with a Jackson-Pratt (JP) drainage for 1 d without other surgical interventions. Two patients experienced dietary delay because of post-operative ileus controlled by an nasogastric tube. The remaining patient developed a cerebral infarction without post-operative sequelae. There were no 30-d operative mortalities.
| Non-combined group | Combined group | P value | |
| (n = 1090) | (n = 93) | ||
| Postoperative complication (%) | 147 (13.5) | 14 (15.1) | 0.667 |
| Bleeding | 7 | 0 | |
| Anastomosis leakage | 27 | 3 | |
| Intra-abdominal abscess | 9 | 1 | |
| Ascites | 8 | 1 | |
| Wound problem | 15 | 4 | |
| Delayed bowel movement | 29 | 2 | |
| Bile leakage | 0 | 1 | |
| Urinary retention | 10 | 0 | |
| Respiratory problem | 25 | 1 | |
| Phlebitis in injection site | 13 | 0 | |
| Cerebral infarction | 1 | 1 | |
| Deep vein thrombosis | 1 | 0 | |
| Acute renal failure | 1 | 0 | |
| Urinary tract infection | 1 | 0 |
The pathological data of synchronous lesions are summarized in Table 4. Five early gastric cancers (EGCs) were detected in the stomach; three gastrointestinal stromal tumors and one schwannoma were also discovered. In the five EGC cases, the entire tumor was confined to the mucosa with 45, 31, 17, 17 and 16 lymph nodes retrieved, respectively. There were no lymph node metastases. The other synchronous lesions also had clear resection margins. Two patients who underwent nephrectomies were diagnosed with renal cell carcinomas (RCCs) and one lesion, which was diagnosed with RCC pre-operatively, was a leiomyoma. Eight lesions were adrenal adenomas, and the remaining lesion was diagnosed with adrenal metastasis. Fifty-five cholecystectomies involved cholelithiases, and one cholecystectomy was a primary gallbladder cancer confined to the mucosa with a clear resection margin, which did not require additional resection. In 21 gynecological resections, two lesions were leiomyomas of the uterus and four were serous cystadenomas; seven lesions were endometriomas, six were ovarian cysts, one was a teratoma, and one was an ovarian abscess.
| Synchronous lesion pathology (n = 98) | |||
| Stomach (n = 9) | Gall bladder (n = 56) | ||
| EGC | 5 | Primary malignancy | 1 |
| GIST | 3 | Stone | 55 |
| Schwannoma | 1 | Gynecologic resection (n = 21) | |
| Kidney (n = 3) | Uterine leiomyoma | 2 | |
| RCC | 2 | Serous cystadenoma | 4 |
| Leiomyoma | 1 | Endometriosis | 7 |
| Adrenal gland (n = 9) | Cyst | 6 | |
| Adrenal metastasis | 1 | Teratoma | 1 |
| Adenoma | 8 | Abscess | 1 |
In the present study, we report on the laparoscopic approach for synchronous multiple abdominal lesions in colorectal cancer patients. Our data showed that this approach is feasible and safe in terms of peri-operative and oncological outcomes.
Minimally invasive laparoscopic surgery has been introduced as an option for patients with colorectal cancer, and many advantages of this surgery have been reported. Attenuated surgical trauma offers faster bowel recovery compared with open surgery, thus reducing post-operative ileus related to decreased expression of inflammatory cytokines[1-3,20]. Furthermore, this approach offers good cosmetic results, reduced post-operative pain and short-term morbidity, and improved quality of life. Combined surgery for synchronous lesions also has potential advantages[10-13]. The patients may minimize the length of hospital stay and have a single, rather than multiple, hospital admission. Cardiac and pulmonary burden related to multiple anesthetic exposures were reduced by combining surgery. Thus, combined surgery reduces the cost related to the hospital stay. If combined surgery for synchronous lesions is performed with a laparoscopic approach, there are also potential advantages over open combined surgery. This approach is available in multi-quadrant abdominal operations with better visualization of the operative field and without additional skin incisions. Furthermore, this approach may reduce the number of trocar incisions by reusing the ports and improving cosmesis. Therefore, there are reduced concerns about delaying the post-operative recovery and impairing post-operative quality of life according to open combined resections.
Simultaneous laparoscopic resection for co-existing abdominal lesions has been reported in several case series, the benefits of which have been previously described[10-13,21]. Most recently, in relation to colorectal cancer patients, laparoscopic resection for synchronous gastric cancer was reported in seven patients with synchronous double primary cancers[11]. All of these reports suggest that simultaneous laparoscopic combined resection is the best choice in patients with co-existing abdominal lesions, in terms of technical feasibility and oncological safety. However, the previous studies emphasized the need for large-scale studies related to simultaneous laparoscopic combined resection owing to the study limitations that prevented a demonstration of actual benefit[10-13]. This present study overcomes these limitations by including 93 patients who underwent laparoscopic combined resection with colorectal cancer and 1090 patients who underwent conventional laparoscopic colorectal resections at our institution. The number of patients included thus enables a comparison of peri-operative and oncological outcomes, including the presence of synchronous cancer and the multiple locations of co-existing abdominal lesions.
In relation to the technical aspects of the procedure, an additional port was inserted in cases of gastric resection and right renal cell carcinoma only in patients with left colon cancer. We shared the trocars in resection of synchronous multiple organs. It is very important to plan the position of ports and mini-incisions appropriately to share the trocars and incisions, not only for exposure and removal of synchronous lesions, but also for colorectal cancer to minimize the number of unnecessary trocars. We modified the number and location of the ports so that we could accomplish multiple surgeries with a minimum number of trocars, but with the same ease. For example, in the case of a cholecystectomy with left colon cancer, the left trocar as an assistant port was placed at a higher level than in standard cases.
In the present study, the mean operative time in the combined group was significantly longer than in the non-combined group. However, the mean operative times were only 20 and 40 min, respectively, compared to the non-combined conventional laparoscopic right hemicolectomy and laparoscopic low/anterior resection. This time is acceptable, as surgeries for more than two lesions were performed, thus avoiding the need for additional operations at a later stage.
Intra-operative complications occurred in six patients; in two of the cases, conversion to open surgery was necessary because of a common bile duct stone discovered intra-operatively and a massive adhesion due to previous abdominal surgery. Although complications developed post-operatively in 14 patients, none required surgical intervention. Anastomotic leakage, which occurred in three patients, was treated by conservative management with bowel rest, percutaneous drainage insertion, and rectal tube insertion. Anastomotic leakage was reported to occur in 0.5%-27% of patients in published series[22,23]; in the current study, anastomotic leakage occurred in 2.5% of patients in the non-combined group and 3.2% of the patients in the combined group. Furthermore, there was only one complication associated with the combined resection; specifically, bile leakage occurring on postoperative 1 d in the combined group, which was resolved through JP drainage for 1 d without other surgical interventions. Our data, therefore, show that laparoscopic combined resection does not increase peri-operative complications in selected patients.
The results of histopathological examinations of the mean number of retrieved lymph nodes and the length of the distal margins in the combined group were similar to the non-combined group, suggesting that oncological safety for colorectal cancer was obtained in both groups. Furthermore, nine patients with synchronous malignancies had clear resection margins. The median follow-up of these patients was 36.6 mo; there was one recurrence in a patient undergoing adrenalectomy for adrenal metastasis that metastasized to the brain in nine months. For primary colorectal cancer, the recurrence rate between the both groups was not significantly different in both laparoscopic right hemicolectomy (combined vs non-combined, 11.5% vs 8.7%, P = 0.716) and laparoscopic low/anterior resection (combined vs. non-combined, 10.2% vs 7.2%, P = 0.289). The five-year overall survival was also similar in both groups, regardless of tumor location (laparoscopic right hemicolectomy; combined vs non-combined, 93.3% vs 86.5%, P = 0.665, laparoscopic low/anterior resection groups; combined vs non-combined, 96.6% vs 96.4%, P = 0.565). Our study showed oncological safety for both colorectal and synchronous cancers.
The retrospective nature of our study posed some limitations. It is uncertain whether or not the longer operative time in the combined group accounts for the reason why the combined resection was difficult or why the primary tumor resection was technically difficult. The time required for colorectal and synchronous lesion resections was not shown; therefore, we did not estimate the results according to conventional resections of other abdominal lesions. Thus, a comparison of the time required for conventional resection of other organs is needed with the time required for combined laparoscopic resection of synchronous lesions.
Following the recent introduction of the Da Vinci system, robotic surgery has been attempted in various fields. Colorectal surgery has been considered one indication for robotic surgery because of advantages such as a magnified three-dimensional visual field and articulating instruments[24-27]. However, various disadvantages have also been reported, one of which is motion limitation in multi-quadrant operations. Our study included 10 cases of robotic-assisted laparoscopic combined resections. Although seven patients in our study underwent a hybrid-surgical technique that involved colectomies and a laparoscopic approach for combined resection, the remaining three patients underwent complete robotic-assisted combined resection for synchronous lesions, low anterior resection with left nephrectomy and anterior resection with aderenalectomy, and right hemicolectomy with cholecystectomy. During nephrectomy, we re-docked after the position change, but the total operating time (340 min) and peri-operative outcomes were acceptable. Therefore, we sought to determine the possibility of using the robotic system in multi-quadrant surgery.
In conclusion, we have demonstrated that simultaneous laparoscopic resection for multiple synchronous abdominal lesions in colorectal cancer patients is safe and feasible. The advantages of this approach with co-existing abdominal lesions include a reduced number of sequential operations and a reduction in hospital stay and overall morbidity. Compared to conventional non-combined colorectal resection, the combined approach has acceptable peri-operative outcomes. Based on these findings, we suggest that simultaneous laparoscopic resection is the best choice for managing co-existing abdominal lesions in colorectal cancer patients.
The laparoscopic approach is now routinely employed for colorectal cancer on basis of its unique benefits over open surgery and can be applied to almost all intra-abdominal surgical procedures. Simultaneous resection of synchronous abdominal lesions requiring surgical intervention is likely to benefit patients by reducing psychological and physiological stress related to re-operation. If so, when patients with colorectal cancer have co-existing abdominal lesions, is a laparoscopic combined resection safe and beneficial?
The laparoscopic approach for synchronous multiple abdominal lesions in colorectal cancer patients laparoscopic combined resection does not increase peri-operative complications and secures the oncological safety for both colorectal and synchronous cancers. Therefore, in selected patients, laparoscopic combined resection is feasible and safe.
Simultaneous laparoscopic resection for co-existing abdominal lesions has been reported in several case series, the benefits of which have been previously described. However, the previous studies emphasized the need for large-scale studies related to simultaneous laparoscopic combined resection owing to the study limitations that prevented a demonstration of actual benefit. This present study overcame these limitations by including 93 patients who underwent laparoscopic combined resection with colorectal cancer and 1090 patients who underwent conventional laparoscopic colorectal resections at the institution. This enabled a comparison of peri-operative and oncological outcomes, including the presence of synchronous cancer and the multiple locations of co-existing abdominal lesions.
Simultaneous laparoscopic resection is the best choice for managing co-existing abdominal lesions in colorectal cancer patients.
This is a comparative study on retrospective data on a topic of current interest, although studies to date have suggested more complications with combined procedures that have been done as open surgery.
Peer reviewer: Yik-Hong Ho, Professor, Department of Surgery, School of Medicine, James Cook University, Townsville 4811, Australia
S- Editor Sun H L- Editor Stewart GJ E- Editor Li JY
| 1. | A comparison of laparoscopically assisted and open colectomy for colon cancer. N Engl J Med. 2004;350:2050-2059. [PubMed] |
| 2. | Veldkamp R, Kuhry E, Hop WC, Jeekel J, Kazemier G, Bonjer HJ, Haglind E, Påhlman L, Cuesta MA, Msika S. Laparoscopic surgery versus open surgery for colon cancer: short-term outcomes of a randomised trial. Lancet Oncol. 2005;6:477-484. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1691] [Cited by in RCA: 1681] [Article Influence: 84.1] [Reference Citation Analysis (0)] |
| 3. | Guillou PJ, Quirke P, Thorpe H, Walker J, Jayne DG, Smith AM, Heath RM, Brown JM. Short-term endpoints of conventional versus laparoscopic-assisted surgery in patients with colorectal cancer (MRC CLASICC trial): multicentre, randomised controlled trial. Lancet. 2005;365:1718-1726. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2360] [Cited by in RCA: 2298] [Article Influence: 114.9] [Reference Citation Analysis (0)] |
| 4. | Lacy AM, Delgado S, Castells A, Prins HA, Arroyo V, Ibarzabal A, Pique JM. The long-term results of a randomized clinical trial of laparoscopy-assisted versus open surgery for colon cancer. Ann Surg. 2008;248:1-7. [PubMed] |
| 5. | Jayne DG, Guillou PJ, Thorpe H, Quirke P, Copeland J, Smith AM, Heath RM, Brown JM. Randomized trial of laparoscopic-assisted resection of colorectal carcinoma: 3-year results of the UK MRC CLASICC Trial Group. J Clin Oncol. 2007;25:3061-3068. [PubMed] |
| 6. | Cadeddu JA, Ono Y, Clayman RV, Barrett PH, Janetschek G, Fentie DD, McDougall EM, Moore RG, Kinukawa T, Elbahnasy AM. Laparoscopic nephrectomy for renal cell cancer: evaluation of efficacy and safety: a multicenter experience. Urology. 1998;52:773-777. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 218] [Cited by in RCA: 185] [Article Influence: 6.9] [Reference Citation Analysis (0)] |
| 7. | Chan KM, Yeh TS, Jan YY, Chen MF. Laparoscopic cholecystectomy for early gallbladder carcinoma: long-term outcome in comparison with conventional open cholecystectomy. Surg Endosc. 2006;20:1867-1871. [PubMed] |
| 8. | Hevia Suárez M, Abascal Junquera JM, Boix P, Dieguez M, Delgado E, Abascal García JM, Abascal García R. Surgical experience and results in transperitoneal laparoscopic adrenalectomy. Actas Urol Esp. 2010;34:412-416. [PubMed] |
| 9. | Huscher CG, Mingoli A, Sgarzini G, Sansonetti A, Di Paola M, Recher A, Ponzano C. Laparoscopic versus open subtotal gastrectomy for distal gastric cancer: five-year results of a randomized prospective trial. Ann Surg. 2005;241:232-237. [PubMed] |
| 10. | Matsui H, Okamoto Y, Ishii A, Ishizu K, Kondoh Y, Igarashi N, Ogoshi K, Makuuchi H. Laparoscopy-assisted combined resection for synchronous gastric and colorectal cancer: report of three cases. Surg Today. 2009;39:434-439. [PubMed] |
| 11. | Tokunaga M, Hiki N, Fukunaga T, Kuroyanagi H, Miki A, Akiyoshi T, Yamaguchi T. Laparoscopic surgery for synchronous gastric and colorectal cancer: a preliminary experience. Langenbecks Arch Surg. 2010;395:207-210. [PubMed] |
| 12. | Zhu QL, Zheng MH, Feng B, Lu AG, Wang ML, Li JW, Hu WG, Zang L, Mao ZH, Dong F. Simultaneous laparoscopy-assisted low anterior resection and distal gastrectomy for synchronous carcinoma of rectum and stomach. World J Gastroenterol. 2008;14:3435-3437. [PubMed] |
| 13. | Tagaya N, Kasama K, Suzuki N, Taketsuka S, Horie K, Kubota K. Simultaneous laparoscopic treatment for diseases of the gallbladder, stomach, and colon. Surg Laparosc Endosc Percutan Tech. 2005;15:169-171. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 6] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 14. | Akiyoshi T, Kuroyanagi H, Oya M, Saiura A, Ohyama S, Fujimoto Y, Ueno M, Koga R, Seki M, Hiki N. Laparoscopic rectal resection for primary rectal cancer combined with open upper major abdominal surgery: initial experience. Hepatogastroenterology. 2009;56:571-574. [PubMed] |
| 15. | Shiraishi N, Yasuda K, Kitano S. Laparoscopic gastrectomy with lymph node dissection for gastric cancer. Gastric Cancer. 2006;9:167-176. [PubMed] |
| 16. | Park IJ, Choi GS, Lim KH, Kang BM, Jun SH. Multidimensional analysis of the learning curve for laparoscopic colorectal surgery: lessons from 1,000 cases of laparoscopic colorectal surgery. Surg Endosc. 2009;23:839-846. [PubMed] |
| 17. | Ono Y, Katoh N, Kinukawa T, Sahashi M, Ohshima S. Laparoscopic nephrectomy, radical nephrectomy and adrenalectomy: Nagoya experience. J Urol. 1994;152:1962-1966. [PubMed] |
| 18. | Bailey RW, Zucker KA, Flowers JL, Scovill WA, Graham SM, Imbembo AL. Laparoscopic cholecystectomy. Experience with 375 consecutive patients. Ann Surg. 1991;214:531-540; discussion 531-540. |
| 19. | Park IJ, Choi GS, Lim KH, Kang BM, Jun SH. Laparoscopic resection of extraperitoneal rectal cancer: a comparative analysis with open resection. Surg Endosc. 2009;23:1818-1824. [PubMed] |
| 20. | Whelan RL, Franklin M, Holubar SD, Donahue J, Fowler R, Munger C, Doorman J, Balli JE, Glass J, Gonzalez JJ. Postoperative cell mediated immune response is better preserved after laparoscopic vs open colorectal resection in humans. Surg Endosc. 2003;17:972-978. [PubMed] |
| 21. | Wadhwa A, Chowbey PK, Sharma A, Khullar R, Soni V, Baijal M. Combined procedures in laparoscopic surgery. Surg Laparosc Endosc Percutan Tech. 2003;13:382-386. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 43] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 22. | Bärlehner E, Benhidjeb T, Anders S, Schicke B. Laparoscopic resection for rectal cancer: outcomes in 194 patients and review of the literature. Surg Endosc. 2005;19:757-766. [PubMed] |
| 23. | Breukink S, Pierie J, Wiggers T. Laparoscopic versus open total mesorectal excision for rectal cancer. Cochrane Database Syst Rev. 2006;CD005200. [PubMed] |
| 24. | Ballantyne GH. The pitfalls of laparoscopic surgery: challenges for robotics and telerobotic surgery. Surg Laparosc Endosc Percutan Tech. 2002;12:1-5. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 104] [Cited by in RCA: 98] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 25. | Ruurda JP, Broeders IA, Simmermacher RP, Borel Rinkes IH, Van Vroonhoven TJ. Feasibility of robot-assisted laparoscopic surgery: an evaluation of 35 robot-assisted laparoscopic cholecystectomies. Surg Laparosc Endosc Percutan Tech. 2002;12:41-45. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 64] [Cited by in RCA: 56] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 26. | Cadière GB, Himpens J, Vertruyen M, Bruyns J, Germay O, Leman G, Izizaw R. Evaluation of telesurgical (robotic) NISSEN fundoplication. Surg Endosc. 2001;15:918-923. [PubMed] |
| 27. | Choi GS, Park IJ, Kang BM, Lim KH, Jun SH. A novel approach of robotic-assisted anterior resection with transanal or transvaginal retrieval of the specimen for colorectal cancer. Surg Endosc. 2009;23:2831-2835. [PubMed] |