Published online Jan 21, 2011. doi: 10.3748/wjg.v17.i3.372
Revised: September 7, 2010
Accepted: September 14, 2010
Published online: January 21, 2011
AIM: To evaluate the factors associated with liver function alterations after laparoscopy-assisted gastrectomy (LAG) for gastric cancer.
METHODS: We collected the data of gastrectomy patients with gastric cancer and divided them into 2 groups: open gastrectomy (OG) and LAG. We also collected the data of patients with colon cancer to evaluate the effect of liver manipulations during surgery on liver function alterations. Serum aspartate aminotransferase (AST), alanine aminotransferase (ALT), total bilirubin, and alkaline phosphatase were measured on the preoperative day and postoperative day 1 (POD1), POD3, POD5, and POD7.
RESULTS: No changes in liver function were observed after the operation in patients with colon cancer (n = 121). However, in gastric cancer patients (n = 215), AST and ALT levels increased until POD5 compared to those in colon cancer patients and these findings were observed both in the LAG and OG without a significant difference except at POD1. The mean hepatic enzyme levels at POD1 in the LAG group were significantly higher than those in the OG group (P = 0.047 for AST and P = 0.039 for ALT). The factors associated with elevated ALT on POD1 in patients with gastric cancer were body mass index (P < 0.001), operation time (P < 0.001), intraoperative hepatic injury (P = 0.048), and ligation of an aberrant left hepatic artery (P = 0.052) but not type of operation (OG vs LAG, P = 0.094).
CONCLUSION: We conclude that the liver function alteration after LAG may have been caused by direct liver manipulation or aberrant hepatic artery ligation rather than the CO2 pneumoperitoneum.
- Citation: Jeong GA, Cho GS, Shin EJ, Lee MS, Kim HC, Song OP. Liver function alterations after laparoscopy-assisted gastrectomy for gastric cancer and its clinical significance. World J Gastroenterol 2011; 17(3): 372-378
- URL: https://www.wjgnet.com/1007-9327/full/v17/i3/372.htm
- DOI: https://dx.doi.org/10.3748/wjg.v17.i3.372
While laparoscopic surgery has some limitations, such as a longer operating time and a more difficult surgical procedure than open surgery, it also has several advantages, such as less postoperative pain, an earlier recovery, and esthetic merits. A major difference between laparoscopic and open surgery is that CO2 is used to create a pneumoperitoneum during laparoscopic surgery, which may result in respiratory and hemodynamic changes[1]. According to many studies, a laparoscopic cholecystectomy, a standard surgical procedure for gallbladder disease, results in an alteration of postoperative liver function more frequently than open cholecystectomy, and the cause of such a liver function alteration is believed to be the pneumoperitoneum created by the CO2[1-5]. Based on previous studies, laparoscopy-assisted gastrectomy (LAG) is expected to result in liver function alterations resulting from the CO2 pneumoperitoneum; this occurs because the CO2 exposure time is much longer in LAG because of the difficulty of the surgical technique and a longer operating time compared to laparoscopic cholecystectomy.
We investigated whether liver function alterations take place in patients who undergo LAG for gastric cancer and whether other factors affect liver function besides a CO2 pneumoperitoneum. We also investigated the effect of the liver function alterations on the clinical results. To do this, the postoperative liver functions of patients who underwent open gastrectomy (OG) and of patients who underwent LAG were compared. In addition, the postoperative liver functions of patients who underwent open colectomy (OC) and of patients who underwent laparoscopy-assisted colectomy (LAC) for colon cancer were compared.
We collected data from 237 consecutive patients who received a radical gastrectomy for gastric cancer at Soonchunhyang University Bucheon Hospital between January 2006 and December 2007. Of these 237 patients, 22 were excluded: 6 had hepatic cirrhosis, 5 had undergone hepatic resection simultaneously with gastrectomy for benign hepatic diseases or hepatic metastasis, 10 had received endoscopic treatment for biliary tract stones before the surgery or intraoperatively had undergone biliary system surgery, and one patient had intraoperatively received a biliary system iatrogenic injury. These patients were excluded because the surgical techniques may have affected their liver function during surgery. However, patients whose liver function was normal, including those who had hepatitis or fatty liver before the operation, and patients who underwent a cholecystectomy simultaneously, were not excluded.
Patients who underwent a colectomy without direct liver manipulation during the operation were the control group for the gastrectomy patients because we thought that traction or manipulation of the liver during the operation might affect postoperative liver function. Of the 133 patients who underwent a radical colectomy for colon cancer during the same period, those included in the study were selected according to the same exclusion criteria.
The patients were divided into 4 groups based on diagnosis and surgical technique: LAG group, OG group, LAC group, and OC group.
The patients’ clinicopathologic characteristics, hepatic disease history, surgical method, surgical outcome, and liver function before and after surgery were retrospectively examined using their medical records. Serum aspartate aminotransferase (AST), alanine aminotransferase (ALT), total bilirubin (Bil), and alkaline phosphatase (ALP) were measured preoperatively and examined at postoperative day 1 (POD1), POD3, POD5, and POD7. The normal reference levels were AST 5-40 IU/L, ALT 0-40 IU/L, Bil 0.2-1.2 mg/dL, and ALP 35-115 IU/L. Patients who had hepatic enzyme levels higher than the normal reference level were defined as the “elevated” group, and patients with a normal reference level were defined as the ’normal’ group.
The operations were performed in the supine position for OG patients, in the reverse-Trendelenburg position for LAG patients, and in the Trendelenburg position for OC and LAC patients. For LAG and LAC, CO2 was insufflated via a trocar to insert the laparoscope, and the pneumoperitoneal pressure was maintained at 12 mmHg or less. In patients undergoing LAG and OG, the range of the gastric resection or lymph node dissection depended on the tumor location or preoperative TNM stage; for gastric cancer invading the submucosal layer or deeper, a D2 lymph node dissection was performed according to the Japanese Gastric Cancer Guidelines. In the LAG and OG groups, to provide an operative field in the upper pancreatic border, the left lobe of the liver was lifted when the lesser curvature of the stomach was dissected. For the LAC and OC groups, the extent of colon resection was also determined based on tumor location and lesion stage before the surgery, and no difference was observed between the 2 groups.
All values are expressed as the mean ± SD. The χ2-test, the independent t-test, and the paired t-test were conducted using SPSS software (version 15.0 for Windows; SPSS Inc., Chicago, IL, USA). P values < 0.05 were considered statistically significant.
Two hundred and fifteen patients with gastric cancer participated in our study (124 patients in the OG group, 91 patients in the LAG group). The mean age of the patients was 58.6 years, with 164 males and 51 females. Of the patients with gastric cancer, 31 (14.4%) had underlying liver diseases: fatty liver in 15 and viral hepatitis in 16. A combined operation was performed in 46 cases (21.4%), most frequently a splenectomy, followed by a cholecystectomy, adrenalectomy, or distal pancreatectomy. Stage I was the most common TNM stage in both the OG and LAG groups (137 patients, 63.7%), but significantly more stage I patients were in the LAG group (92.3%) than in the OG group (P < 0.001). A combined operation was performed more frequently in the OG group than in the LAG group (P = 0.004), and the operating time was significantly longer in the LAG group (203 min) than in the OG group (165 min, P < 0.001). No significant differences between the 2 groups were observed for age, presence or absence of underlying liver disease, type of anesthetic agent used, or postoperative complications.
Among the patients with colon cancer, 121 were included in the study. Their mean age was 60.9 years, and they consisted of 65 males and 56 females. No differences in gender, age, presence or absence of an underlying liver disease, combined operation rate, anesthetic agent, or postoperative complications were observed between the LAC (43 patients) and the OC groups (78 patients), whereas significant differences were found between the 2 groups for operating time and hospital stay after the operation, operating time being significantly longer in the LAC group and length of stay significantly longer in the OC group (Table 1).
| Variables | Stomach cancer (n = 215) | Colon cancer (n = 121) | ||||
| LAG (n = 91) | OG (n = 124) | P | LAC (n = 43) | OC (n = 78) | P | |
| Gender (M:F) | 70:21 | 94:30 | NS | 22:21 | 43:35 | NS |
| Age (yr, mean ± SD) | 57.1 ± 13.2 | 59.7 ± 11.9 | NS | 58.9 ± 10.3 | 62.0 ± 13.5 | NS |
| BMI (kg/m2, mean ± SD) | 23.8 ± 3.2 | 23.5 ± 3.4 | NS | 24.2 ± 3.6 | 24.7 ± 2.9 | NS |
| Underlying liver disease | NS | NS | ||||
| No | 81 (89.0) | 103 (83.1) | 30 (69.8) | 66 (84.6) | ||
| Yes | 10 (11.0) | 21 (16.9) | 13 (30.2) | 12 (15.4) | ||
| Fatty liver | 6 | 9 | 11 | 8 | ||
| Hepatitis | 4 | 12 | 2 | 4 | ||
| TNM stage | < 0.001 | 0.004 | ||||
| I | 84 (92.3) | 53 (42.7) | 18 (41.9) | 15 (19.2) | ||
| II | 4 (4.4) | 22 (17.7) | 8 (18.6) | 35 (44.9) | ||
| III | 3 (3.3) | 30 (24.3) | 17 (39.5) | 28 (35.9) | ||
| IV | 0 | 19 (15.3) | 0 | 0 | ||
| Operation time (min, mean ± SD) | 230.1 ± 77.6 | 165.2 ± 52.1 | < 0.001 | 252.5 ± 77.2 | 184.1 ± 62.4 | < 0.001 |
| Combined operation | 0.004 | NS | ||||
| No | 80 (87.9) | 89 (71.8) | 42 (97.7) | 74 (94.9) | ||
| Yes | 11 (12.1) | 35 (28.2) | 1 (2.3) | 4 (5.1) | ||
| Anesthetic agent | NS | NS | ||||
| Sevoflurane | 21 (23.1) | 45 (36.3) | 15 (34.9) | 18 (23.1) | ||
| Desflurane | 70 (76.9) | 79 (63.7) | 28 (65.1) | 60 (76.9) | ||
| Postoperative morbidity | 8 (8.8) | 16 (12.9) | NS | 1 (2.3) | 5 (6.4) | NS |
| Postoperative mortality | 1 | 1 | 1 | 0 | ||
| Hospital stay (d, mean ± SD) | 10.7 ± 16.0 | 14.9 ± 12.6 | NS | 12.7 ± 3.8 | 17.9 ± 12.3 | 0.007 |
Postoperative complications occurred in 24 (11.2%) patients who underwent a gastrectomy: wound infection in 7, anastomotic leakage in 5, postoperative bleeding in 5, intra-abdominal fluid collection in 5, and other complications in 2. Six cases of complications (5%) occurred in patients who underwent a colectomy: postoperative ileus in 3, anastomotic leak in one, and wound infection in one.
Two patients who underwent a gastrectomy (one each in the OG and LAG groups) and one patient who underwent a colectomy (LAC group) died after the operation. Thus, the postoperative mortality rate was 0.9% and 0.8% in patients who underwent a gastrectomy and colectomy, respectively. The causes of death were postoperative pneumonia (2 patients in the gastrectomy group) and sepsis (one patient in the colectomy group); no patient died of postoperative hepatic failure.
The postoperative AST and ALT levels were significantly higher than the preoperative levels in both the OG and LAG groups until POD5 (Table 2).
| Variables | Stomach cancer (n = 215) | Colon cancer (n = 121) | ||||
| LAG (n = 91) | OG (n = 124) | P1 | LAC (n = 43) | OC (n = 78) | P2 | |
| AST (IU/L) | ||||||
| Preoperative | 22.1 ± 7.6 | 21.8 ± 7.3 | NS | 20.8 ± 8.7 | 19.9 ± 6.3 | NS |
| POD1 | 73.8 ± 67.2a | 57.6 ± 45.9a | 0.047 | 23.2 ± 11.8 | 22.2 ± 11.5 | NS |
| POD3 | 41.1 ± 43.5a | 38.4 ± 24.3a | NS | 22.9 ± 9.5 | 22.4 ± 8.4 | NS |
| POD5 | 28.9 ± 24.1a | 29.5 ± 18.1a | NS | 25.3 ± 10.8 | 22.3 ± 10.8 | NS |
| POD7 | 24.0 ± 11.6 | 22.2 ± 11.3 | NS | 28.9 ± 26.2 | 24.7 ± 13.4 | NS |
| ALT (IU/L) | ||||||
| Preoperative | 23.9 ± 13.5 | 23.8 ± 15.8 | NS | 24.1 ± 3.7 | 17.0 ± 2.6 | 0.045 |
| POD1 | 89.1 ± 103.7a | 63.3 ± 65.9a | 0.039 | 18.4 ± 8.1 | 17.4 ± 15.0 | NS |
| POD3 | 62.2 ± 97.3a | 51.5 ± 57.6a | NS | 16.6 ± 6.5 | 15.9 ± 9.6 | NS |
| POD5 | 43.2 ± 49.1a | 39.4 ± 40.6a | NS | 20.6 ± 13.9 | 16.4 ± 8.5 | NS |
| POD7 | 33.7 ± 25.4 | 26.9 ± 17.9 | 0.033 | 32.1 ± 43.8 | 21.0 ± 25.4 | NS |
| Total bilirubin (mg/dL) | ||||||
| Preoperative | 0.6 ± 0.2 | 0.5 ± 0.3 | NS | 0.5 ± 0.2 | 0.5 ± 0.3 | NS |
| POD1 | 0.8 ± 0.3 | 0.7 ± 0.3 | NS | 0.7 ± 0.4 | 0.6 ± 0.3 | NS |
| POD3 | 0.8 ± 0.4 | 0.7 ± 0.5 | NS | 0.4 ± 0.2 | 0.4 ± 0.2 | NS |
| POD5 | 0.7 ± 0.3 | 0.6 ± 0.3 | NS | 0.5 ± 0.2 | 0.4 ± 0.2 | NS |
| POD7 | 0.7 ± 0.3 | 0.5 ± 0.2 | NS | 0.5 ± 0.2 | 0.4 ± 0.2 | NS |
| ALP (IU/L) | ||||||
| Preoperative | 65.6 ± 17.6 | 65.8 ± 22.1 | NS | 69.1 ± 20.3 | 64.4 ± 22.2 | NS |
| POD1 | 46.7 ± 11.9 | 47.8 ± 14.6 | NS | 49.9 ± 15.5 | 44.6 ± 13.3 | NS |
| POD3 | 44.2 ± 10.5 | 45.8 ± 14.5 | NS | 44.1 ± 11.7 | 41.9 ± 10.2 | NS |
| POD5 | 50.6 ± 23.5 | 48.6 ± 15.6 | NS | 47.5 ± 18.7 | 43.2 ± 11.3 | NS |
| POD7 | 57.9 ± 38.3 | 54.7 ± 22.6 | NS | 51.1 ± 24.1 | 47.2 ± 13.1 | NS |
The mean hepatic enzyme levels at POD1 in the LAG group were significantly higher than those in the OG group (P = 0.047 for AST and P = 0.039 for ALT). No changes in preoperative or postoperative Bil and ALP levels were observed in either group.
No significant changes in the pre- and postoperative AST, ALT, Bil, and ALP levels were observed among patients who underwent a colectomy, and the changes were not significantly different between the LAC and OC groups (Table 2).
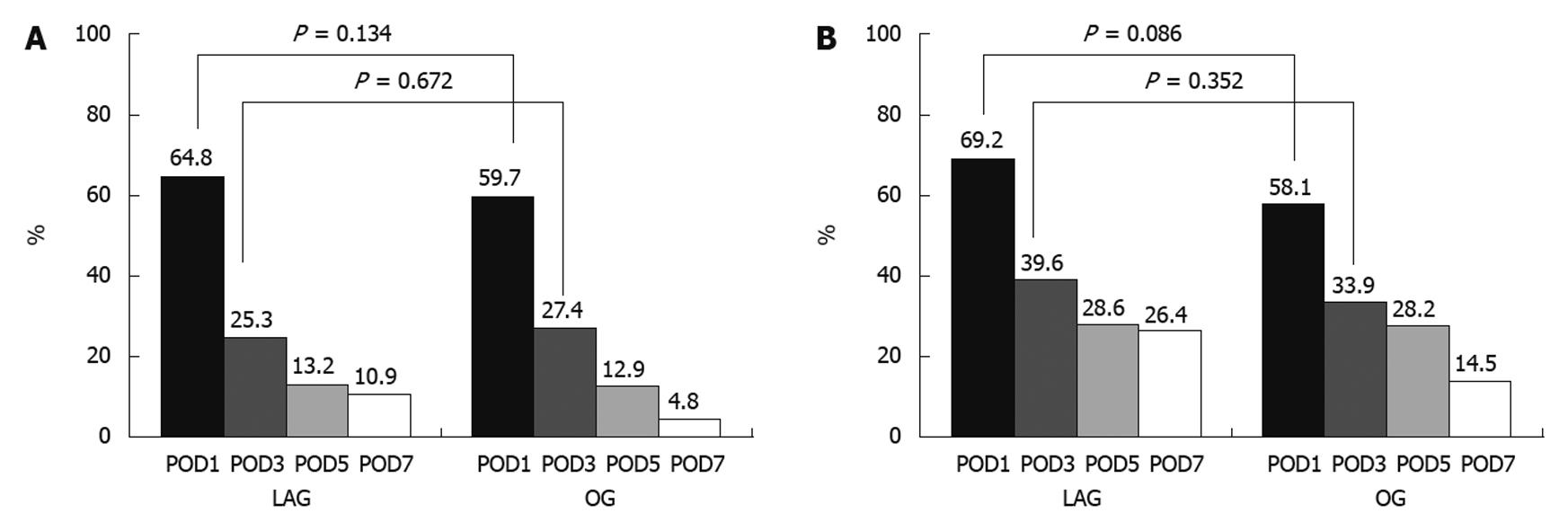
Approximately 65% of the patients in the LAG group and 59.7% in the OG group showed increased levels of AST at POD1, and 25.3% in the LAG group and 27.4% in the OG group showed increased levels of AST at POD3 (P > 0.05). Similar to the results with AST, 69.2% of the patients in the LAG group and 58.1% in the OG group showed increased levels of ALT at POD1, and 39.6% in the LAG group and 33.9% in the OG group showed increased levels at POD3 (P > 0.05, Figure 1).
Among the patients who underwent a gastrectomy, 13 showed more than a 5-fold increase in ALT levels from the normal level at POD1 (8 patients in the LAG group and 5 patients in the OG group). Of these 13 patients, 3 showed more than a 10-fold increase (2 patients in the LAG group and one patient in the OG group).
Unlike LAG, no change in liver function was observed after LAC when using a CO2 pneumoperitoneum. Therefore, the characteristics of the patients who showed liver function alterations after LAG were examined to identify other factors that could cause changes in postoperative liver function. For this purpose, we investigated the ALT level at POD1, at which the change in postoperative liver function for those who underwent a gastrectomy was most prominent. The patients who underwent a gastrectomy were classified into 2 groups: a normal group that had a normal ALT range and an elevated group having higher ALT levels than the reference. We also examined their clinical features and surgical findings.
The changes in the ALT levels at POD1 for patients who underwent a gastrectomy were not significantly affected by gender, age, underlying liver disease, presence or absence of postoperative complications, type of anesthetic agent, or intraoperative transfusion. The body mass index (BMI) was significantly higher in the elevated group than in the normal group, and the operating time in the elevated group was significantly longer than in the normal group. Furthermore, 7.4% of the patients who experienced intraoperative hepatic injury showed increased ALT levels, which was a significantly higher proportion than in the patients who did not experience intraoperative hepatic injury (P = 0.048). Of the patients with normal ALT levels, 1.3% of patients had ligation of an aberrant left hepatic artery during the operation, whereas in the elevated group, 5.9% of patients had ligation of this artery, although this result had no statistical significance (P = 0.052). Thirty-five percent of the patients in the normal group underwent LAG, whereas 46.7% of the patients in the elevated group underwent LAG, but no significant difference was found (P = 0.094) (Table 3).
| Variables | Normal group (n = 80) | Elevated group (n = 135) | P value |
| Gender (M:F) | 59:21 | 105:30 | 0.502 |
| Age (yr, mean ± SD) | 58.6 ± 13.4 | 58.6 ± 12.0 | 0.981 |
| BMI (kg/m2, mean ± SD) | 22.3 ± 3.3 | 24.4 ± 3.0 | < 0.001 |
| Underlying liver disease | 0.153 | ||
| No | 70 (87.5) | 114 (84.4) | |
| Yes | 10 (12.5) | 21 (15.6) | |
| Fatty liver | 2 (2.5) | 13 (9.7) | |
| Hepatitis | 8 (10.0) | 8 (5.9) | |
| Operation time (min, mean ± SD) | 168.9 ± 61.4 | 206.7 ± 73.6 | < 0.001 |
| Types of operation | 0.094 | ||
| Open | 52 (65.0) | 72 (53.3) | |
| Laparoscopy-assisted | 28 (35.0) | 63 (46.7) | |
| Combined operation | 0.093 | ||
| No | 58 (72.5) | 111 (82.2) | |
| Yes | 22 (27.5) | 24 (17.8) | |
| Anesthetic agent | 0.979 | ||
| Sevoflurane | 24 (30.0) | 40 (29.6) | |
| Desflurane | 56 (70.0) | 95 (70.4) | |
| Intraoperative transfusion | 0.894 | ||
| No | 71 (88.8) | 119 (88.1) | |
| Yes | 9 (11.3) | 16 (11.9) | |
| Aberrant left hepatic artery | 0.052 | ||
| Absence or preservation | 79 (98.8) | 127 (94.1) | |
| Artery ligation | 1 (1.3) | 8 (5.9) | |
| Intraoperative hepatic injury | 0.048 | ||
| No | 79 (98.8) | 125 (92.6) | |
| Yes | 1 (1.3) | 10 (7.4) | |
| Mean ALT at POD1 (± SD) | 28.2 ± 8.1 | 101.4 ± 97.1 | < 0.001 |
Pneumoperitoneum, which is created by CO2 insufflation during a laparoscopic operation, results in postoperative transient liver function abnormalities. Halevy et al[6] first reported that aminotransferase levels increased significantly after laparoscopic cholecystectomy. They suggested that the increase in aminotransferase was due to increased intra-abdominal pressure, pressure against the liver with the lifting of the gall bladder, damage to the liver parenchyma by electrocautery, deformity of the extrahepatic biliary duct, the possibility of introducing a small stone into the biliary duct, or damage to the left hepatic artery during surgery. Other studies have reported that a laparoscopic cholecystectomy was more likely to result in liver function abnormalities than an open cholecystectomy and suggested that the cause of the abnormalities was reduced blood flow into the hepatic portal vein as a result of the increased intra-abdominal pressure caused by the pneumoperitoneum; the degree of pneumoperitoneal pressure is related to the degree of liver function abnormality[2,7].
Animal studies have also shown that a pneumoperitoneum directly damages rat liver tissue, that the degree of damage is related to pneumoperitoneal pressure, and that the persistence of the pressure at 15 mmHg or more for 60 min or longer may result in irreversible hepatic damage[8]. Contrary to these reports, a study on 1034 patients who underwent laparoscopic cholecystectomy reported that only 3.9% of the patients had a mild elevation in hepatic enzyme levels after the operation, and that the number of liver function abnormality cases after laparoscopic cholecystectomy was much lower than in other studies[9].
Very few studies have reported liver function abnormalities after LAG for gastric cancer. Etoh et al[10] and Kim et al[11] reported that liver function abnormalities occurred in patients who underwent LAG but not in those who had OG. They asserted that liver function abnormalities may occur after LAG due to the CO2 pneumoperitoneum, although objective evidence for their assertion was unavailable.
Because LAG is more difficult to perform than OG, the operating time can be longer, and consequently, the exposure time of the intra-abdominal organs to the pneumoperitoneum may also be longer than in OG. Given this, a pneumoperitoneum was expected to cause liver function abnormalities. Thus, this study sought to determine whether postoperative liver function abnormalities would occur in patients who underwent LAG.
The change in the absolute hepatic enzyme levels was more marked in the LAG group than in the OG group. Moreover, consistent with the results of previous studies, this change was most prominent on POD1, but the level returned to normal on POD5. When the patients were divided into an elevated enzyme group and a normal group, the frequency of change in the absolute hepatic enzyme levels in the elevated group did not differ between the LAG and OG groups (Figure 1). Furthermore, when the patients who underwent a colectomy, in which the hepatic parenchyma and the vessels around the liver were not excessively manipulated, were divided into LAC and OC groups, no liver function abnormalities were found in either group. Thus, we presumed that the major cause of liver function abnormalities after LAG may not be the pneumoperitoneum. Similar to this result, Nguyen et al[12] also reported no difference in the increase in hepatic enzyme levels between patients who underwent laparoscopic and open gastric bypass. They performed laparoscopic and open Roux-en-Y gastric bypass on obese patients and found that the hepatic enzyme level increase was highest in the first 24 h after the operation, and that liver function returned to normal 72 h after the operation. They also reported no significant difference in the hepatic enzyme level increase between those who underwent a laparoscopic vs an open operation, and they asserted that a prolonged pneumoperitoneum in patients who underwent the laparoscopic operation would not have greatly affected the change in the postoperative hepatic enzyme levels. The statistical significance of the effect of prolonged operating time on the increase in hepatic enzyme level after gastrectomy in the present study can be attributed to the long exposure time to the pneumoperitoneum. However, it can also be attributed to the long ischemic time of the liver due to extended liver traction.
Thus, we divided our patients into a group with normal liver function and a group with elevated liver function, based on the ALT level at POD1, at which the liver function abnormality was most prominent, to determine whether liver function after LAG is influenced by factors other than a pneumoperitoneum. The change in liver function was based on the ALT level because ALT exists mostly in the liver, unlike AST, and is the gold-standard clinical chemistry marker for liver injury[13,14]. The classification of the elevated group was based on the normal ALT reference range of 0-40 IU/L, which is used at the authors’ hospital. As a result, the surgical technique (OG and LAG) did not affect the increase in the ALT levels after the operation, but the BMI in the elevated group was significantly higher than in the normal group. Also, the operating time was significantly longer in the elevated group than in the normal group. When the hepatic parenchyma was damaged or when the aberrant left hepatic artery was ligated, the ALT level increased.
Many studies on liver function abnormalities after a laparoscopic operation have reported that the cause of postoperative liver function abnormality was hepatic ischemia caused by reduced portal flow due to the pneumoperitoneum[8]. However, we did not find any liver function abnormalities after LAC, whereas liver function abnormalities after an open gastrectomy were found when the hepatic parenchyma was directly damaged or when the aberrant hepatic artery was ligated. Given these conditions, the causes of liver function abnormalities after LAG can be attributed to excessive liver traction, direct damage to the hepatic parenchyma, ligation of an aberrant hepatic artery during the operation, or reduced portal flow due to the pneumoperitoneum.
Patients who underwent a gastrectomy showed significantly increased hepatic enzyme levels on POD1, regardless of the surgical technique, which returned to normal on POD5. This transient liver function abnormality was not clinically meaningful because it did not cause hepatic failure or clinical symptoms. However, as patients with hepatic cirrhosis or decreased liver function were not included in this study, further research is required to determine whether LAG is safe for patients with decreased liver function. The assumption was made that LAG could be performed safely in patients with decreased liver function by taking the greatest possible care with ligation of the aberrant hepatic artery and not damaging the hepatic parenchyma, or if the major cause of the liver function abnormality after LAG was damage to the hepatic parenchyma due to excessive liver traction.
A major difference between laparoscopic and open surgery is that carbon dioxide (CO2) is used to create a pneumoperitoneum during laparoscopic surgery, which may result in respiratory and hemodynamic changes. According to many studies, a laparoscopic cholecystectomy, a standard surgical procedure for gallbladder disease, results in an alteration of postoperative liver function more frequently than open cholecystectomy, and the cause of such liver function alteration is believed to be the pneumoperitoneum created by CO2. Based on previous studies, laparoscopy-assisted gastrectomy (LAG) is expected to result in liver function alterations due to the CO2 pneumoperitoneum.The paper investigated whether liver function alterations take place in patients who undergo LAG for gastric cancer and whether other factors affect liver function besides a CO2 pneumoperitoneum.
In the study, patients who underwent a colectomy without direct liver manipulation during the operation were the control group for the gastrectomy patients because the authors thought that traction or manipulation of the liver during the operation might affect postoperative liver function. The change in the absolute hepatic enzyme levels was more remarkable in the LAG group than in the open gastrectomy (OG) group. Moreover, consistent with the results of previous studies, this change was most prominent on postoperative day 1 (POD1), but the level returned to normal on POD5. When the patients were divided into an elevated group and a normal group, the frequency of change in the absolute hepatic enzyme levels in the elevated group did not differ between the LAG and OG groups. Furthermore, when the patients who underwent a colectomy, in which the hepatic parenchyma and the vessels around the liver were not excessively manipulated, were divided into laparoscopy-assisted colectomy (LAC) and open colectomy groups, no liver function abnormalities were found in either group. Thus, authors presumed that the major cause of liver function abnormalities after LAG may not be the pneumoperitoneum.
Many studies on liver function abnormalities after a laparoscopic operation have reported that the cause of postoperative liver function abnormality was hepatic ischemia caused by reduced portal flow due to the pneumoperitoneum. However, authors did not find any liver function abnormalities after LAC, whereas liver function abnormalities after an open gastrectomy were found when the hepatic parenchyma was directly damaged or when the aberrant hepatic artery was ligated. Given these conditions, the causes of liver function abnormalities after LAG can be attributed to excessive liver traction, direct damage to the hepatic parenchyma, ligation of an aberrant hepatic artery during the operation, or reduced portal flow due to the pneumoperitoneum. The assumption was made that LAG could be performed safely on patients with decreased liver function by taking the greatest possible care with the aberrant hepatic artery ligation and not damaging the hepatic parenchyma, or doing so if the major cause of the liver function abnormality after LAG was damage to the hepatic parenchyma due to excessive liver traction.
This is a well designed and researched paper. The positive findings show more marked changes in liver function after a laparoscopy-assisted gastrectomy for gastric cancer than after an open gastrectomy, lasting for up to 5 d, these differences are related to body mass index (BMI) and longer operation time. The authors could have suggested that these could be explained by the heavier retraction of the liver which would be required in patients with a greater BMI and the greater duration of the retraction in the laparoscopy group.
Peer reviewer: Frank I Tovey, OBE, ChM, FRCS, Honorary Research Fellow, Department of Surgery, University College London, London, United Kingdom
S- Editor Shi ZF L- Editor Cant MR E- Editor Ma WH
| 1. | Morino M, Giraudo G, Festa V. Alterations in hepatic function during laparoscopic surgery. An experimental clinical study. Surg Endosc. 1998;12:968-972. |
| 2. | Gutt CN, Oniu T, Mehrabi A, Schemmer P, Kashfi A, Kraus T, Büchler MW. Circulatory and respiratory complications of carbon dioxide insufflation. Dig Surg. 2004;21:95-105. |
| 3. | Andrei VE, Schein M, Margolis M, Rucinski JC, Wise L. Liver enzymes are commonly elevated following laparoscopic cholecystectomy: is elevated intra-abdominal pressure the cause? Dig Surg. 1998;15:256-259. |
| 4. | Kotake Y, Takeda J, Matsumoto M, Tagawa M, Kikuchi H. Subclinical hepatic dysfunction in laparoscopic cholecystectomy and laparoscopic colectomy. Br J Anaesth. 2001;87:774-777. |
| 5. | Tan M, Xu FF, Peng JS, Li DM, Chen LH, Lv BJ, Zhao ZX, Huang C, Zheng CX. Changes in the level of serum liver enzymes after laparoscopic surgery. World J Gastroenterol. 2003;9:364-367. |
| 6. | Halevy A, Gold-Deutch R, Negri M, Lin G, Shlamkovich N, Evans S, Cotariu D, Scapa E, Bahar M, Sackier JM. Are elevated liver enzymes and bilirubin levels significant after laparoscopic cholecystectomy in the absence of bile duct injury? Ann Surg. 1994;219:362-364. |
| 7. | Hasukić S. Postoperative changes in liver function tests: randomized comparison of low- and high-pressure laparoscopic cholecystectomy. Surg Endosc. 2005;19:1451-1455. |
| 8. | Szold A, Weinbroum AA. Carbon dioxide pneumoperitoneum-related liver injury is pressure dependent: A study in an isolated-perfused organ model. Surg Endosc. 2008;22:365-371. |
| 9. | Bickel A, Weiar A, Eitan A. Evaluation of liver enzymes following elective laparoscopic cholecystectomy: are they really elevated? J Gastrointest Surg. 2008;12:1418-1421. |
| 10. | Etoh T, Shiraishi N, Tajima M, Shiromizu A, Yasuda K, Inomata M, Kitano S. Transient liver dysfunction after laparoscopic gastrectomy for gastric cancer patients. World J Surg. 2007;31:1115-1120. |
| 11. | Kim SG, Song KY, Kim SN, Park CH. Alterations in hepatic function after laparoscopic assisted distal gastrectomy: a prospective study. J Korean Surg Soc. 2007;72:46-50. |
| 12. | Nguyen NT, Braley S, Fleming NW, Lambourne L, Rivers R, Wolfe BM. Comparison of postoperative hepatic function after laparoscopic versus open gastric bypass. Am J Surg. 2003;186:40-44. |
| 13. | Amacher DE. Serum transaminase elevations as indicators of hepatic injury following the administration of drugs. Regul Toxicol Pharmacol. 1998;27:119-130. |
| 14. | Ozer J, Ratner M, Shaw M, Bailey W, Schomaker S. The current state of serum biomarkers of hepatotoxicity. Toxicology. 2008;245:194-205. |