Published online Mar 21, 2010. doi: 10.3748/wjg.v16.i11.1422
Revised: January 12, 2010
Accepted: January 19, 2010
Published online: March 21, 2010
The authors report a giant hepatocellular carcinoma (HCC) with a diameter over 30 cm and weight over 10 kg that was resected completely. A 62-year-old man was admitted because of continuous abdominal uplift. A computed tomography scan demonstrated that the entire abdomen was filled with a giant tumor containing both cystic and solid components with a size of 29 cm × 22 cm. The huge tumor was successfully resected without any complication, such as massive hemorrhage or visceral injuries. The size and weight of the tumor were 35 cm × 30 cm × 15 cm and 10 050 g, respectively. Pathological examination showed that the tumor was a well-differentiated HCC, and α-fetoprotein was positive. Postoperative syndrome, characterized by hypovolemic shock, diarrhea and urine retention, was observed and induced by abdominal decompression. This syndrome was resolved with expectant treatment. The patient was still alive without recurrence after a 27-mo follow-up.
- Citation: Ba MC, Cui SZ, Lin SQ, Tang YQ, Wu YB, Zhang XL. Resection of a giant hepatocellular carcinoma weighing over ten kilograms. World J Gastroenterol 2010; 16(11): 1422-1424
- URL: https://www.wjgnet.com/1007-9327/full/v16/i11/1422.htm
- DOI: https://dx.doi.org/10.3748/wjg.v16.i11.1422
Primary hepatocellular carcinoma (HCC) is the most common malignant tumor in Asia, especially in China. Liver neoplasms with diameters of ≤ 5 cm, 5-10 cm, and > 10 cm are designated as small, big, and giant HCC, respectively[1]. However, a diameter over 20 cm is extremely rare. Here, we report a giant HCC with a diameter over 30 cm that weighed over 10 kg.
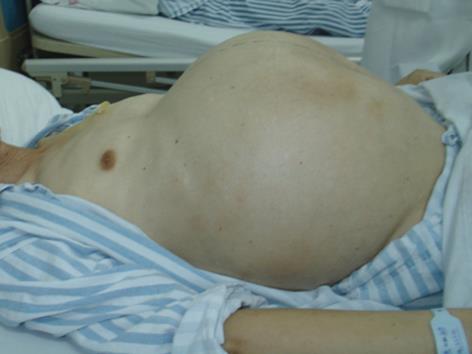
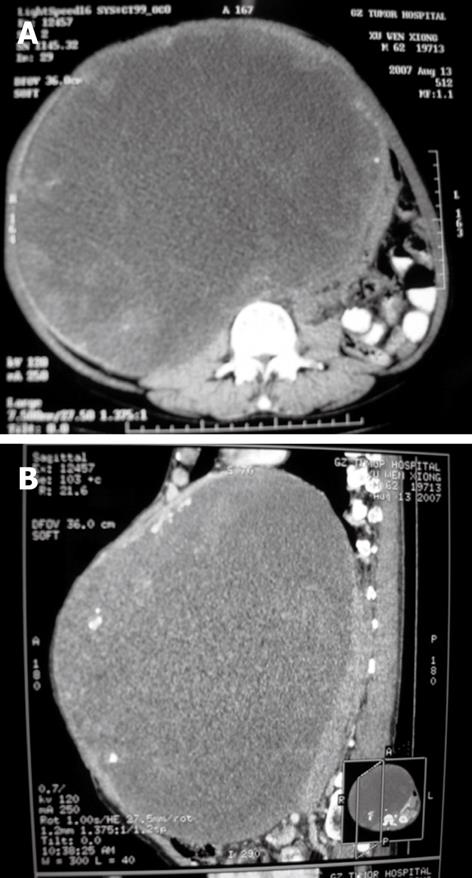
A 62-year-old man had a history of progressive abdominal uplift with unknown etiology for 2 years (Figure 1). He was admitted because of difficult defecation. A computed tomography (CT) scan revealed that the entire abdomen was filled with a huge cystic mixed lesion (Figure 2). An enhanced scan demonstrated the poorly-circumscribed lesion under the right lobe of the liver compressing the surrounding organs. The patient had no history of hepatitis, smoking, or drinking. Upon physical examination, no superficial lymphadenectasis, icteric sclera, or liver palm, and spider telangiectasias were observed. Abnormal cardiac and lung function were not observed. Blood serum study showed that the hepatitis B surface antibody was positive and hepatitis B surface antigen, hepatitis B e antigen HBeAg, hepatitis B e antibody, and hepatitis B core antibody were all negative. Tumor markers such as α-fetoprotein (AFP), cancer embryonic antigen, carbohydrate antigen 199 (CA199), CA125, and CA724 were detected and their values were all within the normal limits. B-type ultrasonic examination demonstrated a relatively well-circumscribed tumor that measured 30 cm × 30 cm × 25 cm. Preoperative glucose tolerance was normal.
Surgical resection under general anesthesia was performed in our hospital on August 30, 2007. Most of the organs in abdominal cavity, including the right kidney, duodenum, abdominal aorta, inferior vena cava, spleen, stomach, small intestine, ascending colon, transverse colon, and urinary bladder were deformed due to the compression by the giant HCC. The right lobe of the liver and diaphragm were adhered closely, the entire right lobe of liver was compressed as thin as a piece of paper. The left lobe of the liver was hypertrophied with normal appearance. Hepatic cirrhosis was not observed. This giant tumor was close to the second portal hepatic vein, and compressed the first and the third portal hepatic vein, blood supply of the tumor was from the hepatic artery, abdominal aorta, renal artery, and collateral circulations. This well-circumscribed tumor was encompassed in a pseudocapsule. The huge tumor and the right lobe of the liver were successfully resected. The injury of abdominal aorta and duodenal serosa was repaired during operation. The intraoperative course was uneventful, which took 185 min, and no intraoperative complication occurred during the operation. Intraoperative blood loss was 600 mL and blood transfusion was 1200 mL. The patient resumed breathing on his own uneventfully. His tracheal intubation was pulled out at the end of operation, and he was sent to ICU for intensive observation and treatment for 48 h.
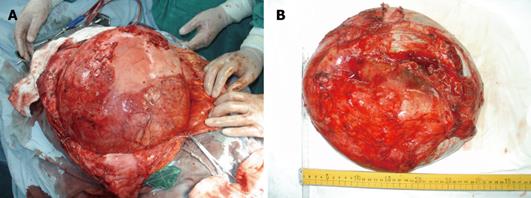
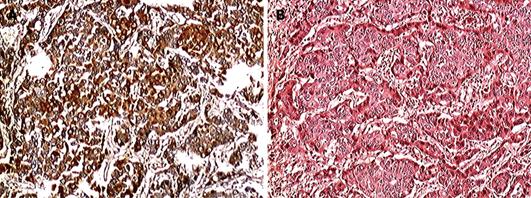
Postoperative tumor size and weight turned out to be 35 cm × 30 cm ×15 cm and 10 050 g, respectively (Figure 3). Grossly, the tumor had cystic degeneration and was encompassed in a pseudocapsule. Histological examination showed that the tumor was infected by a fungus and was a well-differentiated HCC (Figure 4A). Immunohistochemical staining showed that the tumor was AFP positive (++) (Figure 4B).
Hypovolemic shock was observed 18 h after operation and he recovered 36 h after blood and fluid intravenous transfusions. The patient was treated with fluid intravenous transfusion and total parenteral nutrition after operation in the department of abdominal surgery for 5 d. Postoperative liver function was normal, and no liver failure occurred. His catheter was removed on postoperative day 3 and he urinated without medical aid. However, urinary retention was observed on postoperative day 6, he resumed his self-urination by re-indwelling the catheter, which was pulled out 4 d later. Gastrointestinal function recovered 5 d after operation and he was given semi-liquid diet. Additionally, he had serious diarrhea 9 d after operation, which was relieved by intravenous injections of anisodamine hydrochloride 20 mg once a day and a 9 g oral dose of montmorillonite powder once a day for 4 d. Postoperative acute heart failure (CHF) occurred at day 7 after operation and the patient recovered after treatment with cardiotonics, diuresis and vascular dilation for 2 d. The right pleural effusion occurred 8 d after operation and was treated by CT guided percutaneous drainage. Other postoperative recovery was successful, and surgical incision healed well.
Studies on surgical resection of huge hepatic carcinoma have been reported since the 1950s in China. Currently, surgical resection is still the best way to achieve a long-term survival for patients with huge hepatic carcinoma, especially for patients without cardiac, renal, or lung dysfunction or coagulation disturbances[2,3]. However, the prevention of hemorrhages and postoperative hepatic failure are vital for a successful resection of huge hepatic carcinomas. Therefore, surgeons must be skillful at surgical techniques and have a breadth of clinical experience[2,4,5]. In this case, resection of the huge tumor was performed because the left lobe of the liver was compensatory hypertrophy and liver function was normal.
To complete the operation uneventfully and avoid possible complications during tumor excisions depends on the patient status and clinical experience of surgeons[2,6]. A higher incidence of complications and mortality were found during mass excisions, including hemorrhage and injury of abdominal aorta, inferior vena cava, portal hepatic vein, small intestine, etc[7,8]. In this case, the surgery was uneventful except some complications.
In this case, postoperative syndromes characterized by hypovolemic shock, urinary retention, CHF, diarrhea, and pleural effusion were observed due to serious intra-abdominal pressure from a huge liver tumor. This syndrome was relieved with expectant treatment. The optimal treatment protocol of syndromes induced by abdominal decompression after surgical resection of huge hepatic carcinomas has not been defined and further studies are needed.
To our knowledge, this tumor 10 050 g in weight is the largest malignant hepatic carcinoma found to date.
Peer reviewer: Ji-Ping Wang, MD, PhD, Division of Surgical Oncology, Brigham and Women’s Hospital, 75 Francis Street, Boston, MA 02115, United States
S- Editor Wang JL L- Editor Ma JY E- Editor Ma WH
| 1. | Cho YB, Lee KU, Lee HW, Cho EH, Yang SH, Cho JY, Yi NJ, Suh KS. Outcomes of hepatic resection for a single large hepatocellular carcinoma. World J Surg. 2007;31:795-801. |
| 2. | Kubo S, Takemura S, Yamamoto S, Hai S, Ichikawa T, Kodai S, Hiroji S, Shuto T, Hirohashi K, Tanaka H. Risk factors for massive blood loss during liver resection for hepatocellular carcinoma in patients with cirrhosis. Hepatogastroenterology. 2007;54:830-833. |
| 3. | Chen XP, Qiu FZ, Wu ZD, Zhang ZW, Huang ZY, Chen YF. Long-term outcome of resection of large hepatocellular carcinoma. Br J Surg. 2006;93:600-606. |
| 4. | McKay A, You I, Bigam D, Lafreniere R, Sutherland F, Ghali W, Dixon E. Impact of surgeon training on outcomes after resective hepatic surgery. Ann Surg Oncol. 2008;15:1348-1355. |
| 5. | Abdalla EK, Denys A, Hasegawa K, Leung TW, Makuuchi M, Murthy R, Ribero D, Zorzi D, Vauthey JN, Torzilli G. Treatment of large and advanced hepatocellular carcinoma. Ann Surg Oncol. 2008;15:979-985. |
| 6. | Chen XP, Qiu FZ, Wu ZD, Zhang BX. Chinese experience with hepatectomy for huge hepatocellular carcinoma. Br J Surg. 2004;91:322-326. |
| 7. | Shah SA, Wei AC, Cleary SP, Yang I, McGilvray ID, Gallinger S, Grant DR, Greig PD. Prognosis and results after resection of very large (>or=10 cm) hepatocellular carcinoma. J Gastrointest Surg. 2007;11:589-595. |
| 8. | Capussotti L, Muratore A, Amisano M, Massucco P, Polastri R, Bouzari H. Liver resection for large-size hepatocellular carcinomas in 47 non-cirrhotic patients--no mortality and long-term survival. Hepatogastroenterology. 2006;53:768-772. |