Published online Sep 7, 2009. doi: 10.3748/wjg.15.4201
Revised: August 5, 2009
Accepted: August 12, 2009
Published online: September 7, 2009
This report describes a method for percutaneous transhepatic biliary stenting with a BLAKE Silicone Drain, and discusses the usefulness of placement of the drain connected to a J-VAC Suction Reservoir for the treatment of stenotic hepaticojejunostomy. Percutaneous transhepatic biliary drainage was performed under ultrasonographic guidance in a patient with stenotic hepaticojejunostomy after hepatectomy for hepatic hilum malignancy. The technique used was as follows. After dilatation of the drainage root, an 11-Fr tube with several side holes was passed through the stenosis of the hepaticojejunostomy. A 10-Fr BLAKE Silicone Drain is flexible, which precludes one-step insertion. One week after insertion of the 11-Fr tube, a 0.035-inch guidewire was inserted into the tube. After removal of the 11-Fr tube, the guidewire was put into the channel of a 10-Fr BLAKE Silicone Drain. The drain was inserted into the jejunal limb through the intrahepatic bile duct and was connected to a J-VAC Suction Reservoir. Low-pressure continued suction was applied. Patients can be discharged after insertion of the 10-Fr BLAKE Silicone Drain connected to the J-VAC Suction Reservoir. Placement of a percutaneous transhepatic biliary stent using a 10-Fr BLAKE Silicone Drain connected to a J-VAC Suction Reservoir is useful for the treatment of stenotic hepaticojejunostomy.
- Citation: Yoshida H, Mamada Y, Taniai N, Mineta S, Mizuguchi Y, Kawano Y, Sasaki J, Nakamura Y, Aimoto T, Tajiri T. Placement of percutaneous transhepatic biliary stent using a silicone drain with channels. World J Gastroenterol 2009; 15(33): 4201-4203
- URL: https://www.wjgnet.com/1007-9327/full/v15/i33/4201.htm
- DOI: https://dx.doi.org/10.3748/wjg.15.4201
In most operations for hepatic hilum malignancy, the intrahepatic bile duct at the hilum is divided from the hepatic artery, portal vein, and surrounding tissues. Biliary complications, such as leakage or stenosis, are caused occasionally by the presence of several small bilioenteric anastomoses[1]. Stenosis of a bilioenteric anastomosis increases the risk of cholangitis and requires the long-term placement of a stent.
The BLAKE Silicone Drain (Ethicon, NJ, USA) is made of silicone; the entire drain is flexible, and channels along the sides, instead of holes, facilitate drainage. It is always used with a continuous suction device (J-VAC Suction Reservoir; Ethicon), which creates a closed drainage system. Drainage is very efficient: a larger area is in contact with tissue as compared with perforated drains, and fluid is efficiently removed by capillary pressure.
We have reported previously the effectiveness of a BLAKE Silicone Drain connected to a J-VAC Suction Reservoir for the management of pancreatic fistula[2]. We also reported that a 10-Fr BLAKE Silicone Drain has been used as an external stent for a bilioenteric anastomosis during surgery for hepatic hilar malignancy[3].
This report describes a method for percutaneous transhepatic biliary stenting with a BLAKE Silicone Drain, and discusses the usefulness of placement of the drain connected to a J-VAC Suction Reservoir for the treatment of stenotic hepaticojejunostomy.
A 68-year-old man with intrahepatic cholangiocarcinoma invading the hepatic hilum underwent extended left hepatectomy combined with en bloc resection of the extrahepatic bile duct and extended lymph node dissection.
Bilioenteric continuity was reestablished by two hepaticojejunostomies of the anterior and posterior branches of the hepatic ducts, performed using a Roux-en-Y jejunal limb. Silicone drains with an internal lumen and side holes, made by cutting a 5-Fr radiopaque tube for pancreatic drainage (Sumitomo Bakelite, Tokyo, Japan), were used as an internal stent for each bilioenteric anastomosis. Two external drainage catheters (19-Fr BLAKE Silicone Drain) were positioned at the cut surface of the liver and connected to the J-VAC Suction Reservoir. Fixation of the greater omentum was performed to avoid delayed gastric emptying[4]. After operation, major bile leakage occurred, but resolved gradually. The drainage catheter was removed on postoperative day 12, and the patient was discharged on postoperative day 18.
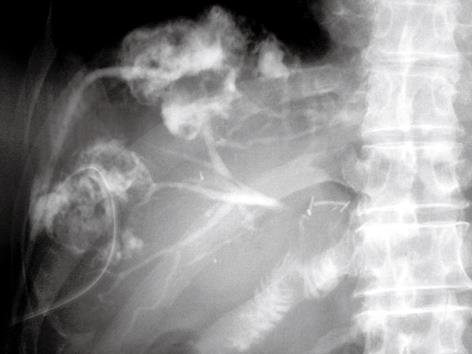
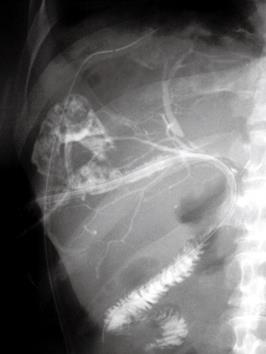
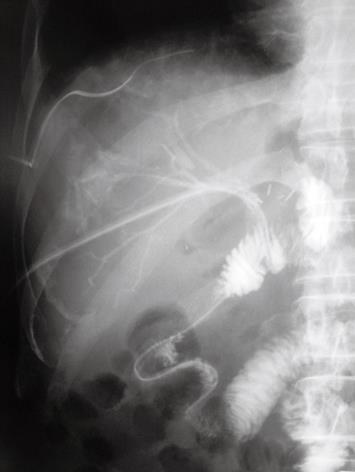
Forty days after discharge, the patient was readmitted because of severe pyrexia. Upon admission, computed tomography demonstrated two low-density areas associated with dilatation of the intrahepatic bile ducts in the anterior segment. Hepatic abscesses caused by stenosis of the hepaticojejunostomy were diagnosed. Percutaneous drainage catheters were inserted into each abscess, and pus was discharged. Abscessography demonstrated communications between the dilated intrahepatic bile ducts of the anterior branch and each of the abscesses (Figure 1). Pyrexia improved, and discharge of clear bile from one of the drainage catheters continued. One week after insertion of the drainage catheters, abscessography was repeated. It was difficult to insert the catheter from the abscess into the intrahepatic bile duct. Another percutaneous transhepatic biliary drainage catheter was inserted directly into the intrahepatic bile duct under ultrasonographic guidance. An 11-Fr tube (11 Fr PTCS tube; Sumitomo Bakelite) with several side holes was placed in the jejunal limb through the intrahepatic bile duct, and passed through the stenosis of the hepaticojejunostomy (Figure 2). Bile juice was discharged from the 11-Fr tube, and discharge from the drainage catheters of the abscess decreased. One of the catheters was removed from the abscess because pus discharge stopped. One week after initial insertion of the 11-Fr tube, cholangiography was performed via the tube. A 10-Fr BLAKE Silicone Drain is flexible, which made one-step insertion difficult. After insertion of a 0.035-inch guide wire, the 11-Fr tube was switched to a 10-Fr BLAKE Silicone Drain (Figure 3). The drain was connected to a J-VAC Suction Reservoir, and continued low-pressure suction was applied. The remaining catheter was removed from the abscess. The patient was discharged 5 d after switching the 11-Fr tube to a 10-Fr BLAKE Silicone Drain connected to the J-VAC Suction Reservoir. After 4 mo, the patient was readmitted because of liver failure. The portal vein was obstructed by recurrent carcinoma. Three weeks after readmission, the patient died. The 10-Fr Blake Silicone Drain was not occluded.
Diagnostic techniques for hepatobiliary disease have improved recently, but advanced hepatic hilum malignancy is still encountered frequently[5-7]. Palliative treatment with a biliary stent is carried out in patients with inoperable malignancy in order to relieve symptoms related to obstructive jaundice[8]. In patients undergoing hepatectomy for advanced hepatic hilum malignancy, aggressive dissection may compromise the ductal blood supply. Peripheral branches of blood vessels, with small diameters and a poor blood supply, may be damaged along with the bile duct, which increases the risk of biliary leakage[1]. The use of stents has been recommended to decompress the bile duct, reduce the risk of bile leakage, and decrease fibrotic narrowing of the anastomosis during early healing[9-12]. However, the risk of biliary complications such as leakage or stenosis is increased by the presence of small several bilioenteric anastomoses[1].
We performed placement of a percutaneous transhepatic biliary stent using a 10-Fr BLAKE Silicone Drain connected to a J-VAC Suction Reservoir for the treatment of stenotic hepaticojejunostomy. BLAKE Silicone Drains promote efficient drainage: a larger area is in contact with tissue as compared with perforated drains, which facilitates the effective removal of fluid by capillaries. These drains contain no plasticizing agents, which are considered to have deleterious effects in humans. The channels do not interfere with removal, and the drains can be removed easily, safely and securely. These drains also provide a high flow rate when connected to a closed suction device (J-VAC Suction Reservoir). The suction pressure of the J-VAC Suction Reservoir is lower than that with other portable low-pressure continuous suction devices. As a result of low suction pressure, the J-VAC Suction Reservoir does not damage tissue; therefore, we used this drainage system in the lumen of the bile duct and jejunum.
We have evaluated previously the efficacy of a BLAKE Silicone Drain connected to a J-VAC Suction Reservoir for the management of pancreatic fistula. In basic experiments, no collections of fluid were detected around the BLAKE Silicone Drain. When leakage occurred, it did not cause an abdominal abscess, and a “drain canal” linking the anastomosis with the extracorporeal orifice was formed all along the drainage route[2].
In the patient described in this report, 5-Fr silicon drains were used as a stent for the bilioenteric anastomosis. Stenosis of the anastomosis occurred after leakage. We used a 10-Fr BLAKE Silicone Drain as an external stent for bilioenteric anastomosis after major hepatectomy with pancreatoduodenectomy. The drain is placed within the hepaticojejunostomy via the stump of the jejunal limb. It is then connected to the J-VAC Suction Reservoir. Bile and pancreatic juice can be drained by a single drain. Even if bilioenteric anastomosis leaks, a 10-Fr intraluminal diameter of the anastomosis is maintained[3].
The treatment of stenotic bilioenteric anastomosis requires the long-term placement of a stent in the anastomosis. The BLAKE Silicone Drain is flexible and contains no plasticizing agents. It has four continuous channels instead of holes along the sides, and prevents obstruction of small biliary branches. The BLAKE Silicone Drain is therefore suited for long-term placement. The input port of the J-VAC Suction Reservoir has an anti-reflux valve, which reduces the risks of the reverse flow of fluid into the body and of retrograde infection. This valve enables the patient to use the reservoir without having to worry about the level of the drainage bag during position changes and ambulation. The J-VAC Suction Reservoir is portable and convenient in size, which enables the patient to carry it around in a specially designed pochette on the shoulder. A BLAKE Silicone Drain connected to a J-VAC Suction Reservoir usually remains free of occlusion for about 6 mo.
In conclusion, placement of a percutaneous transhepatic biliary stent using a 10-Fr BLAKE Silicone Drain connected to a J-VAC Suction Reservoir was useful for the treatment of stenotic hepaticojejunostomy.
| 1. | de Castro SM, Kuhlmann KF, Busch OR, van Delden OM, Laméris JS, van Gulik TM, Obertop H, Gouma DJ. Incidence and management of biliary leakage after hepaticojejunostomy. J Gastrointest Surg. 2005;9:1163-1171; discussion 1171-1173. |
| 2. | Aimoto T, Uchida E, Nakamura Y, Matsushita A, Katsuno A, Chou K, Kawamoto M, Taniai N, Yoshida H, Tajiri T. Efficacy of a Blake drainR on pancreatic fistula after pancreaticoduodenectomy. Hepatogastroenterology. 2008;55:1796-1800. |
| 3. | Yoshida H, Mamada Y, Taniai N, Mizuguchi Y, Nanbu K, Mizutani S, Satoh S, Shioya T, Tokunaga A, Tajiri T. Low-pressure continuous suction of bile and pancreatic juice from the hepatic duct and jejunal limb after major hepatectomy with pancreatoduodenectomy. Surg Today. 2008;38:285-288. |
| 4. | Yoshida H, Mamada Y, Taniai N, Mizuguchi Y, Shimizu T, Kakinuma D, Ishikawa Y, Kanda T, Matsumoto S, Yokomuro S. Fixation of the greater omentum for prevention of delayed gastric emptying after left hepatectomy with lymphadenectomy for cholangiocarcinoma. J Hepatobiliary Pancreat Surg. 2007;14:392-396. |
| 5. | Unno M, Okumoto T, Katayose Y, Rikiyama T, Sato A, Motoi F, Oikawa M, Egawa S, Ishibashi T. Preoperative assessment of hilar cholangiocarcinoma by multidetector row computed tomography. J Hepatobiliary Pancreat Surg. 2007;14:434-440. |
| 6. | Miyazaki M, Kimura F, Shimizu H, Yoshidome H, Ohtsuka M, Kato A, Yoshitomi H, Nozawa S, Furukawa K, Mitsuhashi N. Recent advance in the treatment of hilar cholangiocarcinoma: hepatectomy with vascular resection. J Hepatobiliary Pancreat Surg. 2007;14:463-468. |
| 7. | Tajiri T, Yoshida H, Mamada Y, Taniai N, Yokomuro S, Mizuguchi Y. Diagnosis and initial management of cholangiocarcinoma with obstructive jaundice. World J Gastroenterol. 2008;14:3000-3005. |
| 8. | Yoshida H, Mamada Y, Taniai N, Mizuguchi Y, Shimizu T, Yokomuro S, Aimoto T, Nakamura Y, Uchida E, Arima Y. One-step palliative treatment method for obstructive jaundice caused by unresectable malignancies by percutaneous transhepatic insertion of an expandable metallic stent. World J Gastroenterol. 2006;12:2423-2426. |
| 9. | Cameron JL, Gayler BW, Zuidema GD. The use of silastic transhepatic stents in benign and malignant biliary strictures. Ann Surg. 1978;188:552-561. |
| 10. | Saypol GM, Kurian G. A technique of repair of stricture of the bile duct. Surg Gynecol Obstet. 1969;128:1071-1076. |