Published online Jun 1, 2004. doi: 10.3748/wjg.v10.i11.1639
Revised: October 4, 2003
Accepted: October 22, 2003
Published online: June 1, 2004
AIM: To assess CT, MR manifestations and their diagnostic value in hepatic tuberculosis.
METHODS: CT findings in 12 cases and MR findings in 4 cases of hepatic tuberculosis proved by surgery or biopsy were retrospectively analyzed.
RESULTS: (1) CT findings: One case of serohepatic type of hepatic tuberculosis had multiple-nodular lesions in the subcapsule of liver. Parenchymal type was found in 10 cases, including multiple, miliary, micronodular and low-density lesions with miliary calcifications in 2 cases; singular, low-density mass with multiple flecked calcifications in 3 cases; multiple cystic lesions in 1 case; multiple micronodular and low-density lesions fusing into multiloculated cystic mass or “cluser” sign in 3 cases; and singular, macronodular and low-density lesion with multiple miliary calcifications in 1 case. One case of tuberculous cholangitis showed marked dilated intrahepatic ducts with multiple flecked calcifications in the porta hepatis. (2) MR findings in 4 cases were hypointense on both T1-weighted imagings and T2-weighted imagings in one case, hypointense on T1-weighted imagings and hyperintense on T2-weighted imagings in 3 cases. Enhanced MR in 3 cases was slightly shown peripheral enhancement or with multilocular enhancement.
CONCLUSION: Various types of hepatic tuberculosis have different imaging findings, and typical CT and MR findings can suggest the diagnosis.
- Citation: Yu RS, Zhang SZ, Wu JJ, Li RF. Imaging diagnosis of 12 patients with hepatic tuberculosis. World J Gastroenterol 2004; 10(11): 1639-1642
- URL: https://www.wjgnet.com/1007-9327/full/v10/i11/1639.htm
- DOI: https://dx.doi.org/10.3748/wjg.v10.i11.1639
During the second half of the twentieth century, as a result of improved nutrition, reduced crowding, public health measures, and effective chemotherapy, a dramatic decrease in the incidence of tuberculosis was seen in the world[1]. But in recent years, increased incidence of tuberculosis has been attributed to several causes, including AIDS epidemic, iv drug abuse and increase in the number of immunocompromised patients[2,3]. Hepatic tuberculosis is the most common manifestation of upper abdominal parenchymatous organ tuberculosis and its incidence has also been increasing.
Imaging features of hepatic tuberculosis have been described by several researchers at computed tomography (CT) and magnetic resonance imaging (MRI), the imaging appearance of these lesions is considered as nonspecific and, a histopathological or bacteriological confirmation is often required[4-7].
The CT and MRI features of 12 patients with pathologically proven hepatic tuberculosis examined between 1984 and 1999 were analyzed retrospectively to improve the imaging diagnotic accuracy and differentiation of hepatic tuberculosis.
Of the 12 hepatic tuberculosis patients, 7 were male and 5 female, aged from 18 to 69 years (mean, 38.2 years). The diagnosis was proved by surgery (8 cases), liver biopsy (3 cases) and abdominoscopy (1 case). The duration of symptoms ranged from 1 to 18 mo. The most frequent clinical symptoms and signs were right upper abdominal pain (n = 10), upper abdominal tenderness (n = 8), low-grade fever (n = 8), night sweat (n = 6), weight-loss and fatigue (n = 5), abdominal mass (n = 1), hepatomegly (n = 4) and jaundice (n = 2). Among the 12 cases, 4 were accompanied by extra-hepatic tuberculosis. Laboratory test showed anemia (n = 10), raised erythrocyte sedimentation rate (n = 9) and abnormal liver function (n = 7). Tuberculin test was positive in 4 out of 5 patients tested. Eight patients were examined with ultrasound, but only 2 were correctly diagnosed. All the 12 patients had chest x-ray, and evidences of pulmonary tuberculosis were found in 2.
CT was performed with Siemens Somatom DR3 and HiQ units for the patients in routine fasting state. Some patients were given 500 mL of diluted iodinated contrast medium (10 g/L meglumine diatrizoate) orally 30 min before scanning. Scan scope ranged from the dome of diaphragm to the last plane of liver. All patients were examined with plain scanning at first and then using 600 g/L meglumine diatrizoate 60-80 mL for enhanced scanning with section thickness of 8-10 mm and internal of 10 mm.
MR was performed with a superconducting unit (Impact; Siemens, Germany) operating at a field strength of 1.0 T by using a body coil. The matrix size for data acquisition was 256 × 128, and a 6-10-mm section thickness with a section gap of 0-4-mm. Conventional fast spin-echo (TSE) included T1-weighted images (700/12 ms, TR/TE) and T2-weighted images (2600-5000/128-165 ms, TR/TE). If necessary, FLASH T1-weighted images with transverse angle of 70-75° were added. Post-contrasted MRI was obtained on FLASH T1-weighted images and TSE T1-weighted images after 0.2 mmol/kg GD-DTPA. Some patients were examined by using T1-weighted imaging fat suppression.
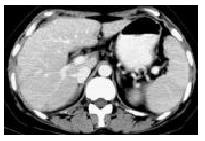
Serohepatic type One case of serohepatic type of hepatic tuberculosis had multiple-nodular hypodense lesions with slightly peripheral enhancement in the subcapsule of liver and thickened subcapsule of quadratus lobe on CT (Figure 1).
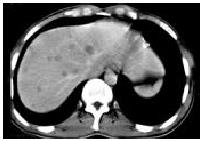
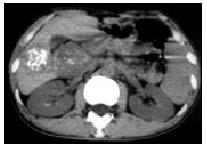
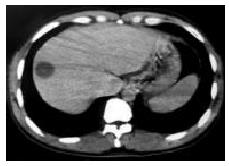
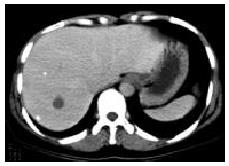
Parenchymal type Ten cases of parenchymal type of hepatic tuberculosis were divided into 3 subtypes: (1) Miliary tuberculosis (n = 2) : CT showed multiple, miliary, micronodular and low-density lesions with size ranging from 0.6 cm to 1.8 cm and no marked enhancement (Figure 2). Multiple miliary calcifications were found in 1 case. (2) Nodular tuberculosis (n = 7) : Nodule was more than 2.0 cm in diameter. Singular, slightly low-density (ranging from 34-42 Hu) lesions in liver were seen in 3 cases with multiple flecked calcifications in 2 cases (Figure 3), and with slightly peripheral enhancement in 2 cases, no marked enhancement in 1 case. Multi-nodular lesions were in 4 cases. One case of scattered multi-nodular lesions was two isolated cystic masses, with 23 Hu and 29 Hu respectively, and had no marked enhancement (Figure 4). Gathered multiple masses were found in the other 3 cases. CT revealed multiple micronodular and low-density lesions fusing into multiloculated cystic mass or “cluser” sign with multiloculated enhancement. (3) Mixed tuberculosis (n = 1) : CT demonstrated singular, macronodular and low-density lesion with slightly enhanced rim and multiple miliary calcifications (Figure 5).
Tuberculous cholangitis One case of tuberculous cholangitis showed slightly diffuse hepatomegly, marked- dilated intrahepatic ducts, multiple calcificated lymph nodes in the porta hepatis and other regional distribution of lymph nodes in abdomen, and a large amount of hyperdense ascites. It was proved by surgery and pathology that tuberculosis of common hepatic duct involved left and right intrahepatic ducts and secondary marked dilated distant ducts. Lymph node tuberculosis and tuberculous peritonitis were also diagnosed pathologically.
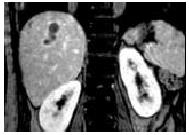
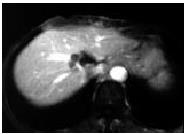
MR was performed in 4 patients. One case of serohepatic type of hepatic tuberculosis diagnosed on CT was reexamined with MR after therapy, showing multiple-nodular lesions with hypointense on T1-weighted images and hyperintense on T2-weighted images in the subcapsule of liver. The lesions had slightly peripheral enhancement after contrast administration. The other 3 cases were classified as parenchymal type of hepatic tuberculosis on CT, including miliary tuberculosis, mixed tuberculosis and nodular tuberculosis. Miliary tuberculosis showed multiple, miliary, micronodular lesions with hypointense on T1-weighted images and hyperintense on T2-weighted images. Mixed tuberculosis showed singular, macronodular lesion presented as a hypointense mass on both T1-weighted images and T2-weighted images (Figure 6) with peripheral enhancement. In this case, the lesion presented round-like on axial plane but irregular strip with multilocular enhancement on coronary and sagittal planes (Figure 7). Nodular tuberculosis revealed multiple micronodular lesions fusing into multiloculated cystic mass, which was hypointense on T1-weighted images and marked hyperintense on T2-weighted images, with multiloculated enhancement (Figure 8).
Among the 12 cases, 4 had lymph node tuberculosis, showing enlarged lymph nodes, with ringed peripheral enhancement or calcifications in 2 cases respectively (Figure 3). Pancreatic tuberculosis, adrenal tuberculosis and tuberculous peritonitis were found in 1 case.
Hepatic tuberculosis is considered to be a rare clinical entity. Unless there was a high index of suspicion, the diagnosis was often overlooked[1,4]. Hepatic tuberculosis can be manifested by relatively nonspecific clinical presentation. The most frequent clinical symptoms and signs were right upper abdominal pain, upper abdominal tenderness, low-grade fever, night sweat, weight-loss and fatigue, abdominal mass, hepatomegly and jaundice[4,8,9]. Anemia, raised ESR, abnormal hepatic function and positive tuberculin test could be found in laboratory examinations.
Classification of hepatic tuberculosis has remained in dispute by now[8-10]. The authors of this article considered it comprehensive and reasonable to classify hepatic tuberculosis into serohepatic type, parenchyma type and tuberculous cholangitis. In a sense, we do not agree that tuberculous cholangitis belonged to parenchymal type of hepatic tuberculosis[8]. The parenchymal type is the most common one among the 3 types, which can be further divided into 3 subtypes, i.e. miliary tuberculosis, nodular tuberculosis and mixed tuberculosis.
Parenchyma type Miliary tuberculosis: This subtype is the most common form of hepatic tuberculosis and was found in 80-100% of autopsied patients with disseminated pulmonary tuberculosis[11]. It is depicted as multiple or diffuse miliary micronodular lesions (≤ 2.0 cm in diameter on CT), often as a part of tuberculosis in the whole body. So clinically it was not difficult to diagnose correctly[9,12]. Radiographic examination could detect hepatomegly and micronodular lesions, but it was extremely difficult to find noncalcificated lesions with less than 0.5 cm in diameter with CT[12-17]. In this series, CT revealed multiple, miliary, micronodular, hypodense lesions (> 0.5 cm in diameter) scattered in liver in 2 cases with miliary calcifications in one case.
Nodular tuberculosis: The lesion, with a diameter > 2 cm, is less common and has been found to be fused by miliary lesions or micronodular lesions[4]. Because nodular lesion is apt to be found by CT and MRI, most reported hepatic tuberculosis belongs to nodular tuberculosis[10,12-15,17-28]. Pathological features of this subtype are more complex than those of other subtypes. If tuberculous granuloma had no evident caseating necrosis or had a large amount of fibrous tissue existed, CT revealed a hypodense mass with slightly peripheral enhancement and no features on imaging findings could be found, it was difficult to diagnose it correctly[13]. In tuberculous granuloma, when calcium deposited calcificans punctata or even “powdery” calcificans, it might appear in the hypodense lesion that could be detected on CT and is therefore helpful to the diagnosis[6,13,24-26]. Two cases in this study were found to have calcificans punctata in the lesion center. When marked caseation or liquefaction necrosis emerged in the center of tuberculous granuloma, it means tuberculous abscess was formed and CT manifestation would be a cystic lesion with slightly or no enhanced rim[12,17,18]. In this study there were two isolated cystic masses with no marked enhancement. Compared with liver cyst, the CT findings of the isolated cystic masses were higher than those of liver cyst and the wall of isolated cystic was more blurring. When multiple micronodular lesions fused into macronodular mass, CT present as a “clunter” sign or a mutilotulated cystic mass with mutilobulated enhancement[13,19], which could be considered as a special CT feature but small pyogenic hepatic abscesses needed to be ruled out firstly[29]. Such manifestation was characterized by a less marked enhancement and a shorter duration, being different from bacterial hepatic abscess. Three cases in this study were found.
Mixed tuberculosis (or miliary macronodular tuberculosis) : One case showed multiple miliary calcifications with singular hypodense lesion. We considered that one of the typical CT features of hepatic tuberculosis might be multiple, various-dense lesions, indicating that there are lesions developed in different pathologic stage coexisting in hepatic tuberculosis, including tuberculous granuloma, liquefaction necrosis, fibrosis or calcification.
Tuberculous cholangitis Tuberculous cholangitis is rare and occurs mainly in children. Obstructive jaundice is the most common in clinic. Pathology revealed regional or diffuse duct dilation with duct wall thickening and stiffening[8]. Imaging findings showed irregular dilated intrahepatic ducts or diffuse miliary calcifications along the course of the bile ducts. The latter was considered as a typical feature of tuberculous cholangitis[13,30]. In our case, CT demonstrated mild diffuse hepatomelgy, marked dilated intrahepatic ducts and multiple flecked calcifications in the porta hepatis, complicated with tuberculous peritonitis.
Serohepatic type Serohepatic type of hepatic tuberculosis is the most uncommon one in the 3 types and was depicted as miliary tuberculous lesions in the subcapsule of liver or “frosted liver”, formed by thickened subcapsule[8]. To our knowledge, the imaging findings of this type have not been reported. In our case, CT revealed multi-nodular hypodense lesions in the subcapsule of liver and thickened subcapsule of quadratus lobe. On MRI, multi-nodular lesions appeared as hypointense areas on T1-weighted imagings and as hyperintense areas on T2-weighted imagings, with slightly peripheral enhancement after contrast administration. The features of CT and MRI were consistent with pathological features.
MRI of hepatic tuberculosis showed a hypointense nodule with a hypointense rim on T1-weighted imagings, and hypointense, isointense or hyperintense with a less intense rim on T2-weighted imagings, and peripheral enhancement or internal septal enhancement on post-contrasted MRI [20,21,24,31]. MR findings were related to different pathological stages of tuberculosis[20,24,31]. At the early and medium stages of granuloma with or without caseation or liquefaction necrosis, the lesion showed a low signal intensity on T1-weighted imagings and a high signal intensity on T2-weighted imagings. Similar lesions with hypointense on T1-weighted imaging and hypo- and iso-intense on T2-weighted imagings were corresponding to fibrous stage of tuberculosis and may have slightly or no peripheral enhancement. Tuberculous granuloma at early or medium stage and fibro-proliferous lesions all depicted as a low-density area on CT but as various signal intensities on T2-weighted imaging, which is the main advantage of MRI in the diagnosis of hepatic tuberculosis. In addition, 3D-MR imaging is helpful to distinguish the pattern of lesions and diagnose the disease. But MRI is limited to detect calcification. MR findings in 4 cases of this study were hypointense on T1-weighted imaging, hypointense in one case and hyperintense on T2-weighted imaging in 3 cases. Calcificated lesions on CT showed no signal intensity on MRI. In 2 cases in our study, lesions with hyperintense on T2-weighted imaging were pathologically proved by surgery to be a caseation necrosis in tuberculous granuloma and hypointense, and were proved to be a complete fibrosis. In short, CT and MRI have some characteristic manifestations valuable for the qualitative diagnosis of hepatic tuberculosis.
| 1. | Hassan I, Brilakis ES, Thompson RL, Que FG. Surgical management of abdominal tuberculosis. J Gastrointest Surg. 2002;6:862-867. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 22] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 2. | Yilmaz T, Sever A, Gür S, Killi RM, Elmas N. CT findings of abdominal tuberculosis in 12 patients. Comput Med Imaging Graph. 2002;26:321-325. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 32] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 3. | Yang ZG, Min PQ, Sone S, He ZY, Liao ZY, Zhou XP, Yang GQ, Silverman PM. Tuberculosis versus lymphomas in the abdominal lymph nodes: evaluation with contrast-enhanced CT. AJR Am J Roentgenol. 1999;172:619-623. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 65] [Cited by in RCA: 57] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 4. | Fang SG, Yang JZ. Diagnosis of hepatic tuberculosis. Shijie Huaren Xiaohua Zazhi. 1999;7:412-413. |
| 5. | Suri R, Gupta S, Gupta SK, Singh K, Suri S. Ultrasound guided fine needle aspiration cytology in abdominal tuberculosis. Br J Radiol. 1998;71:723-727. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 40] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 6. | Tan TC, Cheung AY, Wan WY, Chen TC. Tuberculoma of the liver presenting as a hyperechoic mass on ultrasound. Br J Radiol. 1997;70:1293-1295. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 26] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 7. | Xing X, Xia S. Diagnosis and treatment of hepatic tuberculoma. Chin J Tuberc Respir Dis. 1997;20:169-171. |
| 8. | Wu JP, Qiu FZ. Huang Jiasi Surgery. 5th ed. Beijing: People‘s hygiene publisher. 1992;1324-1325. |
| 9. | Li YH, Chi J. Clinical and pathological features of hepatospleic tuberculosis. J Chin Med Univ. 1996;25:193-194. |
| 10. | Levine C. Primary macronodular hepatic tuberculosis: US and CT appearances. Gastrointest Radiol. 1990;15:307-309. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 81] [Cited by in RCA: 86] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 11. | Thoeni RF, Margulis AR. Gastrointestinal tuberculosis. Semin Roentgenol. 1979;14:283-294. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 78] [Cited by in RCA: 83] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 12. | Xie R, Zhou X, Chen J. [CT in diagnosis of tuberculosis of liver and spleen]. Zhonghua Jiehe He Huxi Zazhi. 1999;22:237-238. [PubMed] |
| 13. | Hou MH, Xue YS, Gen SQ, Liu QW, Huang H, Wang J, Gou LX, Jian ZJ, Ju CQ. CT manifestation of hepatic tuberculosis. Chin J Radiol. 1996;30:151-154. |
| 14. | Suri S, Gupta S, Suri R. Computed tomography in abdominal tuberculosis. Br J Radiol. 1999;72:92-98. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 100] [Cited by in RCA: 87] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 15. | Leder RA, Low VH. Tuberculosis of the abdomen. Radiol Clin North Am. 1995;33:691-705. [PubMed] |
| 16. | Jadvar H, Mindelzun RE, Olcott EW, Levitt DB. Still the great mimicker: abdominal tuberculosis. AJR Am J Roentgenol. 1997;168:1455-1460. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 102] [Cited by in RCA: 107] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 17. | Oto A, Akhan O, Ozmen M. Focal inflammatory diseases of the liver. Eur J Radiol. 1999;32:61-75. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 26] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 18. | Reed DH, Nash AF, Valabhji P. Radiological diagnosis and management of a solitary tuberculous hepatic abscess. Br J Radiol. 1990;63:902-904. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 47] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 19. | Malde HM, Chadha D. The "cluster" sign in macronodular hepatic tuberculosis: CT features. J Comput Assist Tomogr. 1993;17:159-161. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 14] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 20. | Kawamori Y, Matsui O, Kitagawa K, Kadoya M, Takashima T, Yamahana T. Macronodular tuberculoma of the liver: CT and MR findings. AJR Am J Roentgenol. 1992;158:311-313. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 56] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 21. | Fan ZM, Zeng QY, Huo JW, Bai L, Liu ZS, Luo LF, Yang JC, Zhou XH. Macronodular multi-organs tuberculoma: CT and MR appearances. J Gastroenterol. 1998;33:285-288. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 33] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 22. | Varela M, Fernández J, Navasa M, Bruix J. Pseudotumoral hepatic tuberculosis. J Hepatol. 2003;39:654. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 9] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 23. | Lupatkin H, Bräu N, Flomenberg P, Simberkoff MS. Tuberculous abscesses in patients with AIDS. Clin Infect Dis. 1992;14:1040-1044. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 56] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 24. | Maeda N, Tanaka S, Andachi H, Osaki M, Horie Y, Suou T, Kawasaki H. Solitary hepatic tuberculoma with chronic hepa-titis C diagnosed by polymerase chain reaction using paraffin-embedded resected specimen. Hepatol Res. 1999;15:80-89. [RCA] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 25. | Kok KY, Yapp SK. Isolated hepatic tuberculosis: report of five cases and review of the literature. J Hepatobiliary Pancreat Surg. 1999;6:195-198. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 35] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 26. | Stoupis C, Taylor HM, Paley MR, Buetow PC, Marre S, Baer HU, Vock P, Ros PR. The Rocky liver: radiologic-pathologic correlation of calcified hepatic masses. Radiographics. 1998;18:675-85; quiz 726. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 75] [Cited by in RCA: 50] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 27. | Hickey N, McNulty JG, Osborne H, Finucane J. Acute hepatobiliary tuberculosis: a report of two cases and a review of the literature. Eur Radiol. 1999;9:886-889. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 31] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 28. | Andronikou S, Welman CJ, Kader E. The CT features of abdominal tuberculosis in children. Pediatr Radiol. 2002;32:75-81. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 44] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 29. | Jeffrey RB, Tolentino CS, Chang FC, Federle MP. CT of small pyogenic hepatic abscesses: the cluster sign. AJR Am J Roentgenol. 1988;151:487-489. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 97] [Cited by in RCA: 95] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 30. | Abascal J, Martin F, Abreu L, Pereira F, Herrera J, Ratia T, Menendez J. Atypical hepatic tuberculosis presenting as obstructive jaundice. Am J Gastroenterol. 1988;83:1183-1186. [PubMed] |
| 31. | Yan FH, Zeng MS, Cheng WZ, Liu R, Zhou KR, Fang J, Ji Y. MRI findings of hepatic tuberculosis. Linchuang Fangshexue Zazhi. 2002;21:439-442. |