Published online Dec 25, 2023. doi: 10.5501/wjv.v12.i5.256
Peer-review started: September 1, 2023
First decision: September 14, 2023
Revised: September 22, 2023
Accepted: October 25, 2023
Article in press: October 25, 2023
Published online: December 25, 2023
Processing time: 115 Days and 11.3 Hours
The coronavirus disease 2019 (COVID-19) pandemic has put standard, routine childhood vaccinations at risk worldwide. The disruption in vaccine coverage has resulted in a negative impact on the health of children, with some races, ethnicities, age groups, areas of settlement, and parts of the world affected more than others. This literature review studied and examined the impact of COVID-19 on infant, child, and adolescent vaccinations. Retrospectively, the analysis showed a decline, delays, or interruptions in the coverage of vaccines during the pan-demic and a decline in some countries' pre-pandemic and post-pandemic eras. Necessary attempts and efforts should be made for these delayed and missed vaccinations, as failure to do so could put children's health at risk. Thus, priority should be directed at instituting catch-up programs to support vaccine uptake and decrease the probability of acquiring vaccine-preventable diseases.
Core Tip: Studies worldwide have reported a decline in vaccination rates among the pediatric population because of the coronavirus disease 2019 pandemic. The disruption in vaccine coverage has resulted in a negative impact on the health of children, with some races, ethnicities, age groups, areas of settlement, and parts of the world affected more than others. Government efforts should be directed towards reversing these missed vaccinations.
- Citation: Locke J, Marinkovic A, Hamdy K, Balendra V, Sanyaolu A. Routine pediatric vaccinations during the COVID-19 pandemic: A review of the global impact. World J Virol 2023; 12(5): 256-261
- URL: https://www.wjgnet.com/2220-3249/full/v12/i5/256.htm
- DOI: https://dx.doi.org/10.5501/wjv.v12.i5.256
The coronavirus disease 2019 (COVID-19) pandemic profoundly impacted the healthcare systems worldwide, resulting in significant and unintended consequences such as the disruption of routine health services, including immunization. A range of factors have contributed to these disruptions, such as travel restrictions, policies designed to reduce person-to-person contact, and concerns about viral exposure, resulting in the cancellation or postponement of patient visits. One result of these disruptions is a significant reduction in vaccine coverage, particularly in regions such as north Africa and the Middle East, south Asia, Latin America, and the Caribbean[1,2]. In the United States, data shows a decline in vaccination rates during the pandemic period, particularly during age-limited preventive care, and although vaccination rates rebounded during the expanded primary care period, they have yet to reach pre-pandemic levels[3]. To address this issue, China's Centers for Disease Control and Prevention (CDC) developed successful catch-up vaccination guidelines for children who missed or experienced delays in vaccination due to COVID-19[4]. Although sub-Saharan Africa experienced the lowest disruptions, data reveals a significant decline in vaccine coverage globally against vaccine-preventable diseases such as measles, diphtheria, tetanus, and whooping cough. Moreover, there are growing concerns on the heightened risk of outbreaks of other vaccine-preventable diseases such as polio[1]. Understanding the early impacts of the pandemic on vaccine coverage will help immunization programs determine how to continue to serve the health care needs of the population. Thus, this review aims to explore the impact of the COVID-19 pandemic on global immunization for other communicable diseases.
A mini-review was carried out to describe the epidemiological elements of the present global immunization decline in the pediatric population during the COVID-19 pandemic. An electronic literature review was conducted primarily using Google Scholar, MedLine Plus, and PubMed. The search for the assembled data was not limited to peer-reviewed studies published between December 2019 and September 2023. Grey literature sources were also visited to learn more about the decline in routine pediatric vaccinations during the pandemic. When selecting publications or manuscripts, keywords such as COVID-19 pandemic, immunizations of children, vaccinations, and disruption of vaccines were considered.
Prior to the pandemic, the United States ranked highest coverage of most recommended pediatric vaccines due to its vaccination guidelines for documentation of vaccines for daycares and schools[3]. In September 2020, routine infant, child, and adolescent weekly vaccinations, showed that it was lower than 2019. Vaccination coverage had major distinctions between race and ethnicity across all ages and periods. The lowest was in African American children, and although disparities were present pre-pandemic, COVID-19 made these differences more significant, especially in the 18-mo-old age group[3]. When comparing the age groups and race for up-to-date vaccinations, the African American pediatric population was low on the spectrum. In the age group of 7 mo, the highest vaccine receiving population was in Asian infants (88.0%) and the lowest in African American infants (61.0%); in the 6-year-old age group, the highest was among Hispanic children (79.0%), and lowest was in African American children (70.0%); in the adolescent age group the lowest vaccinated were among African American adolescents (51.0%) and Caucasian adolescents (51.0%)[3]. Another disparity was seen in children living in rural areas, having increased missed vaccination doses, compared to their peers living in urban areas (33.3% vs. 15.2% unvaccinated children)[5]. These findings make it imperative to ensure that all children are targeted for their required vaccinations no matter their living situation.
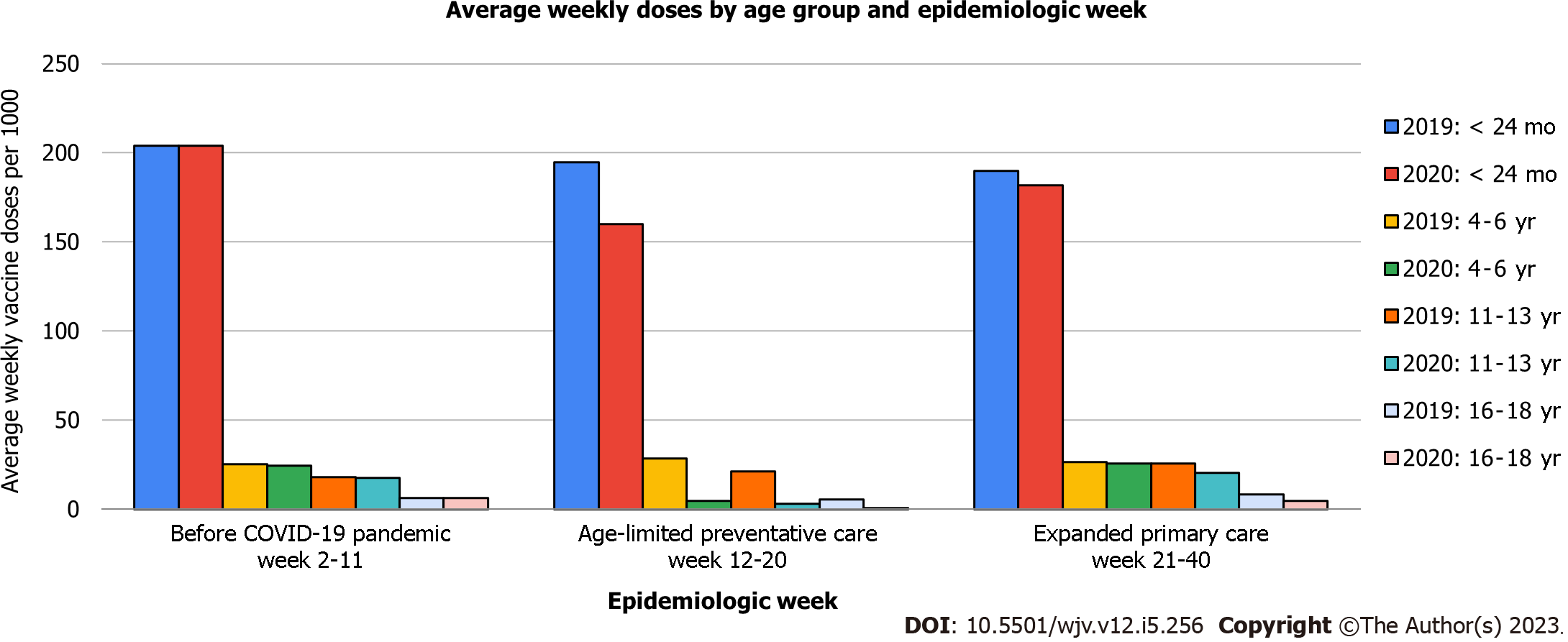
Figure 1 compared the average weekly vaccine doses in 2019 and 2020 among those < 24 mo, 4-6 years, 11-13 years, and 16-18 years in the United States. Before the COVID-19 pandemic months: 2019 = 01/06/19-03/16/19; 2020 = 01/05/20-03/14/20; age-limited preventative care months: 2019 = 03/17/19-05/18/19; 2020 = 03/15/20-05/16/20; expanded primary care months: 2019 = 05/19/19-10/05/19; 2020 = 05/17/20-10/03/20. The vaccines administered in the study were: Children < 24 mo-hepatitis B (HepB); rotavirus; diphtheria, tetanus, pertussis (DTaP); Haemophilus influenzae type B (Hib) conjugate; measles, mumps, rubella (MMR); inactivated polio; varicella-zoster; and 13-valent pneumococcal conjugate. Children 4-6 years-MMR, varicella-zoster, and inactivated polio. Children 11-13 years-human papillomavirus (HPV), Tetanus toxoid, reduced diphtheria toxoid, acellular pertussis vaccine, and quadrivalent meningococcal conjugate. Adolescents 16-18 years-HPV and quadrivalent meningococcal conjugate[3].
The weekly vaccination rates shown in Figure 1, were measured by age group, period, and year. The pre-pandemic period in 2020 across all age groups was comparable to that in 2019. The period that saw a decline across all age groups was the age-limited preventative care in 2020 compared to 2019. The expanded primary care, was the only time that showed increased vaccination rates amongst all age groups. These findings further demonstrated how the COVID-19 pandemic affected the pediatric population regarding immunizations and how much this vulnerable population recovered from diseases.
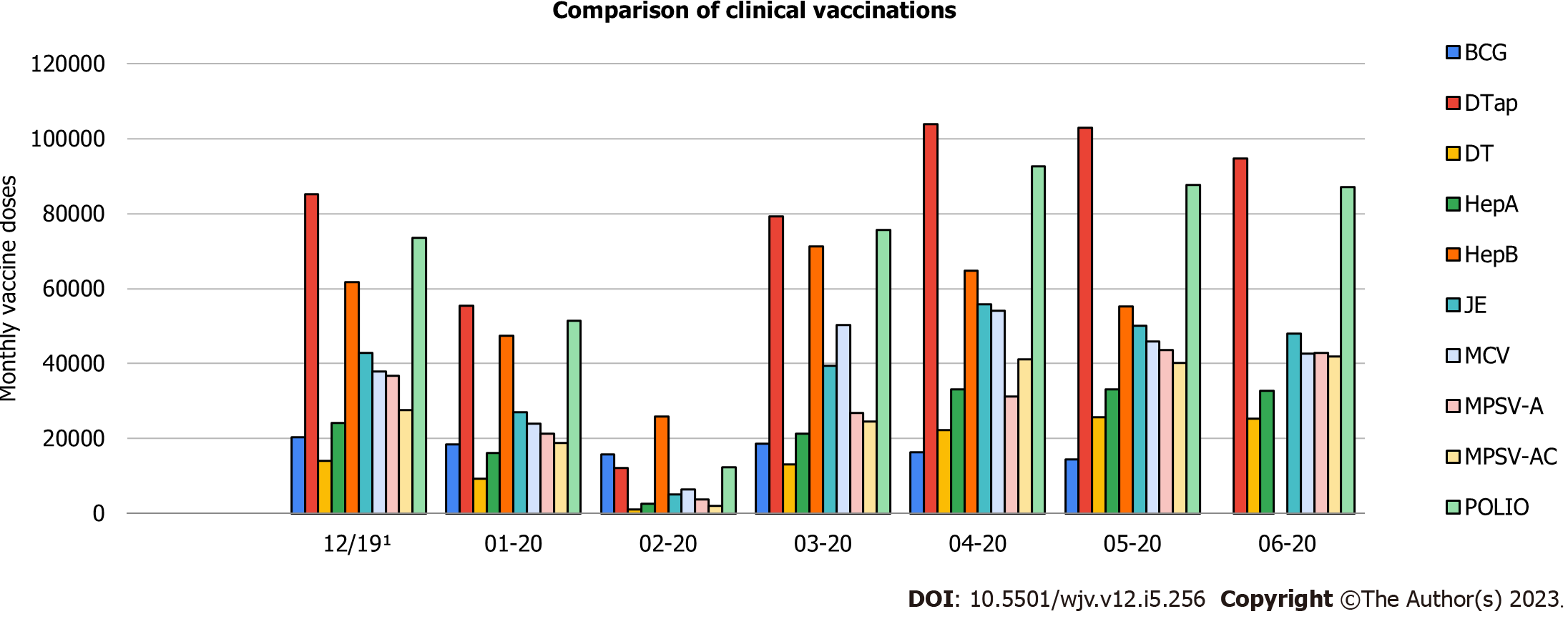
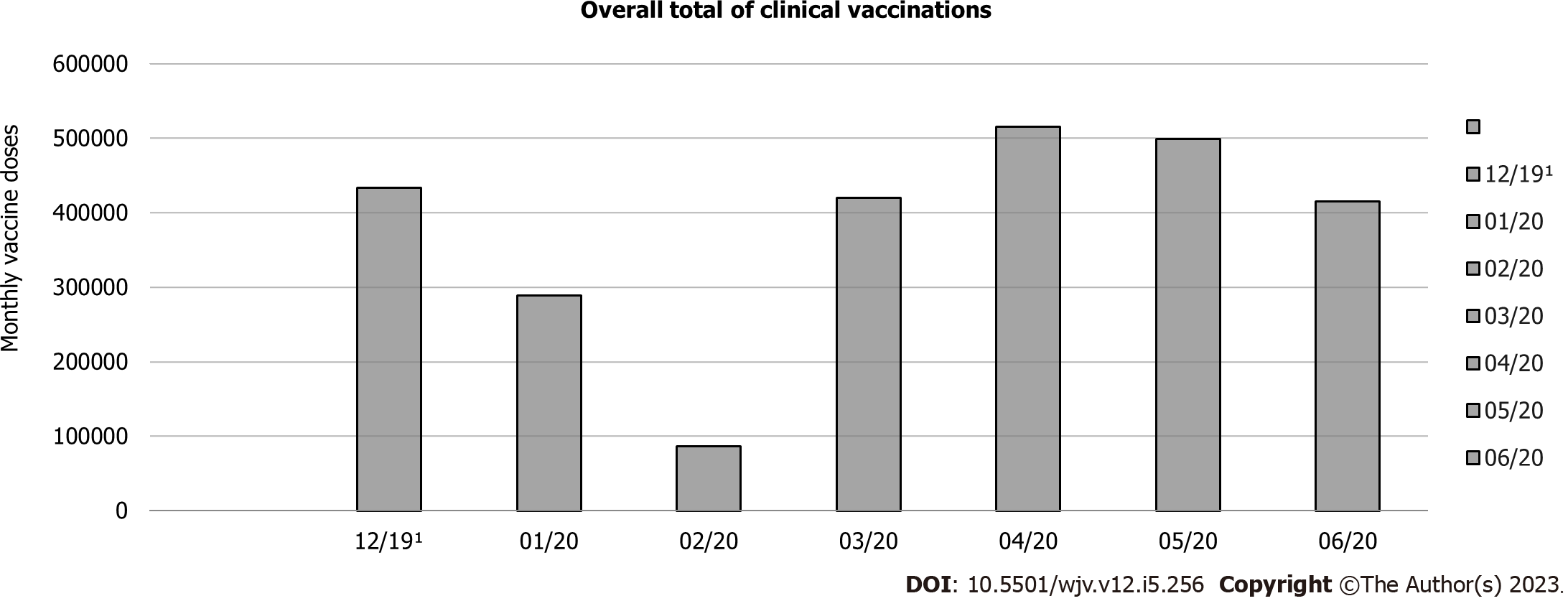
Figures 2 and 3 compared the monthly vaccine doses administered in vaccination clinics in the United States from January 2020 to June 2020 with the baseline doses administered in December 2019[4]. Vaccinations compared are Bacillus Calmette-Guerin (BCG) vaccine, DTaP vaccine, diphtheria and tetanus toxoid vaccine, hepatitis A vaccine, HepB vaccine, Japanese encephalitis vaccine, measles-containing vaccine (MCV) vaccine, group A meningococcal polysaccharide vaccine, group A and C meningococcal polysaccharide vaccine, polio vaccine, and total vaccines. As depicted in Figure 2, weekly vaccination doses declined from the baseline in December 2019, especially in February 2020; however, most vaccines took a positive step in the catch-up phase of delivery doses in the following six months. One possible reason for the increase in required vaccinations administered to the pediatric population, beginning in late March 2020, could be the strategies executed to promote childhood vaccinations and reaching out to patients that were past due by the vaccine safety datalink, a collaboration with the CDC[6].
The usual immunization schedule was significantly impacted by the COVID-19 pandemic, particularly in the pediatric population. Even after taking COVID-19 precautions and returning to regular activities, the gaps in vaccine coverage raise the risk of vaccine-preventable infections. According to studies, the disruptions in normal immunizations caused by the pandemic provided risk of a 10.0% increase in mortality from diseases that can be prevented by vaccination[2]. Diphtheria-tetanus-pertussis, third dose vaccine (DTP3), and MCV first dose (MCV1) coverage were estimated to have fallen by more than 7.0% worldwide compared to expected coverage in the absence of COVID-19. More than 8 million additional children missed the DTP3 and MCV1 beyond expected estimates of vaccination gaps for 2020[2]. The global vaccination rate against tuberculosis (BCG vaccine), poliomyelitis vaccine (polio 3), and HepB third dose (HepB3) also dropped in 2020[7,8]. Over half of the African countries recorded a reduction of vaccination rates with Tanzania (polio 3) and Djibouti (DTP, Hep3, 3 doses of Hib vaccine (Hib3), 3 doses of pneumococcus conjugate vaccine (PCV3), MCV1, and MCV2) mainly impacted. In Asia, the COVID-19 pandemic caused a decline in pediatric vaccination coverage for almost all vaccinations. Larger decline (7.0%) of the BCG vaccination was observed in India. DTP3 has the highest reduction in Nepal (9.0%). The most pronounced decline observed for MCV1 occurred in Indonesia (12.0%) while the largest reduction in polio 3 vaccination was recorded in the Democratic People's Republic of Korea. Significant reductions in Europe occurred in Bulgaria, Ukraine, and Montenegro with MCV1, MCV2, BCG, and HepB3. Reductions in routine vaccination rates also occurred in the Americas with BCG, MCV1, PCV3, and polio3. In Canada, report of the Childhood National Immunization Coverage Survey collected in 2021, during the COVID-19 pandemic, showed that in-school vaccination programs for adolescents experienced delays and interruptions which differed across jurisdictions; however, by March 2021, national vaccination coverage rates were similar to the pre-pandemic level[9]. In Oceania, reductions were noted in some countries, notably in Samoa for MCV1 and Kiribati for MCV2[7,8]. Although the first half of COVID-19 was the most severe and caused the biggest impact, the second half showed promise with the increased number of vaccinations being administered; but despite this increase, millions of doses were still not being delivered. Some regions have been on the rise in their attempts to recover from the impact of COVID-19, but there are some areas that are still under the average for vaccinations in the pediatric population[2]. Regions such as sub-Saharan Africa were already below the global target before the pandemic, therefore recovery would still leave the pediatric population vulnerable to preventable diseases and affecting the long-term health of the children in that area[2]. Addressing the pre-pandemic gaps in coverage of missed childhood vaccinations needs to be considered as well as ensuring that all children receive their necessary immunizations; whether it was missed pre-pandemic or post-pandemic[5].
Moreover, those over six months of age are recommended to get the COVID-19 vaccine, according to the CDC, for the best defense[10]; despite that, COVID-19 typically causes minor illness, low hospitalizations, and infrequent post-acute consequences in young children[11,12]. However, there has been a correlate with COVID-19 infection in children and adolescents developing new-onset type 1 diabetes (T1D) mellitus and potentially other post-acute sequelae[13]. Compared to pre-COVID-19 pandemic levels, the median glucose and hemoglobin A1C levels in newly diagnosed T1D children increased by 6.43% and 6.42%, respectively[14]. The pandemic of COVID-19 has increased the risk of juvenile new-onset T1D, diabetic ketoacidosis (DKA), and severe DKA worldwide[14]. During the early period of the B.1.1.529 (omicron) variant's predominance in the United States, the rate of COVID-19-associated hospitalization among children under five years of age peaked at 14.5 per 100000 in January 2022[11]. Roughly, this was five times the rate during the period of predominance of the B.1.617.2 (delta) variant in 2021[11]. It is worthy of note that 63.0% of infants and kids hospitalized in 2022 due to COVID-19 did not have any underlying medical issues[11]. It is of importance to encourage national pediatric associations to create national plans for integrating the COVID-19 vaccine into current immunization schedules, and according to the European Academy of Paediatrics campaign, "Vaccinate your child" should have support from national pediatric associations to reinstate postponed routine immunizations or vaccinate missed children[15].
Communities need to have a more inclusive system to provide opportunities for all children, no matter their living situation in order to receive their vaccinations. In 2019, it was found that coverage for the MCV1 vaccine which covers the first dose for measles was lower among children living in remote rural areas, compared to children living in urban areas[5]. Even a year after the COVID-19 pandemic started, challenges and gaps in the vaccines and immunizations system continued. Vaccinations systems are limited in tracking outside age groups with the current delay by notifying who and what vaccination is required for that given child. More strategic programming needs to be in place to reach the pediatric population who missed vaccinations. Regions around the world can begin to develop stronger and healthier communities with a more up-to-date immunization requirement system, but if vaccines are still delayed, COVID-19 will continue to impact the children's health now and the future generations.
Studies worldwide have reported a decline in vaccination rates among the pediatric population because of the COVID-19 pandemic. Government efforts should be directed toward reversing these missed vaccinations. Strategies need to be strictly followed during times of crisis to prioritize the maintenance and reduced delays in routine childhood vaccination programs. Initiatives include low-income countries obtaining their missed vaccines through an organized programs such as increasing vaccine availability in remote areas, decreasing the wait times to care, as well as increasing public health awareness. To address these vaccine deficiencies and to maintain children's health protection from preventable communicable illnesses like polio and measles, public health procedures must be strictly followed. These infections can have negative consequences, including mortality, for younger children. Thus, stringent protocols should be safeguarded to avoid the increase in risk of other fatal illnesses, and emphasize the importance of providing consistency in maintaining childhood vaccinations to ensure the health and protection of preventable diseases in children.
Provenance and peer review: Invited article; Externally peer reviewed.
Peer-review model: Single blind
Specialty type: Virology
Country/Territory of origin: Anguilla
Peer-review report’s scientific quality classification
Grade A (Excellent): A
Grade B (Very good): 0
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Rahmati M, Iran; Gao S, China S-Editor: Qu XL L-Editor: A P-Editor: Chen YX
| 1. | Buguzi S. Child vaccination rates fall to decade low amid pandemic. Sci Dev Net July 17, 2021. [cited 12 May 2023]. Available from: https://www.scidev.net/asia-pacific/news/child-vaccination-rates-fall-to-decade-low-amid-pandemic/. |
| 2. | Causey K, Fullman N, Sorensen RJD, Galles NC, Zheng P, Aravkin A, Danovaro-Holliday MC, Martinez-Piedra R, Sodha SV, Velandia-González MP, Gacic-Dobo M, Castro E, He J, Schipp M, Deen A, Hay SI, Lim SS, Mosser JF. Estimating global and regional disruptions to routine childhood vaccine coverage during the COVID-19 pandemic in 2020: a modelling study. Lancet. 2021;398:522-534. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 227] [Cited by in RCA: 232] [Article Influence: 58.0] [Reference Citation Analysis (0)] |
| 3. | DeSilva MB, Haapala J, Vazquez-Benitez G, Daley MF, Nordin JD, Klein NP, Henninger ML, Williams JTB, Hambidge SJ, Jackson ML, Donahue JG, Qian L, Lindley MC, Gee J, Weintraub ES, Kharbanda EO. Association of the COVID-19 Pandemic With Routine Childhood Vaccination Rates and Proportion Up to Date With Vaccinations Across 8 US Health Systems in the Vaccine Safety Datalink. JAMA Pediatr. 2022;176:68-77. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 95] [Article Influence: 31.7] [Reference Citation Analysis (0)] |
| 4. | Wu J, Yu W, Cao L, Rodewald L, Ye J, Song Y, Li L, Liu X, Wen N, Wang F, Hao L, Li Y, Zheng H, Li K, Ma C, Wu D, Liu Y, Zhang G, An Z, Wang H, Yin Z. Effectiveness of Catch-Up Vaccinations after COVID-19 Containment - China, 2020. China CDC Wkly. 2020;2:968-974. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 7] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 5. | Downey K. Progress in vaccinating children against measles has slowed in LMICs. Healio. December 17, 2020. [cited 4 May 2023]. Available from: https://www.healio.com/news/primary-care/20201217/progress-in-vaccinating-children-against-pediatric-measles-vaccination-rates-has-slowed-in-lmicslast. |
| 6. | Stephenson J. Sharp Drop in Routine Vaccinations for US Children Amid COVID-19 Pandemic. JAMA Health Forum. 2020;1:e200608. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 7. | Maltezou HC, Medic S, Cassimos DC, Effraimidou E, Poland GA. Decreasing routine vaccination rates in children in the COVID-19 era. Vaccine. 2022;40:2525-2527. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 32] [Article Influence: 10.7] [Reference Citation Analysis (0)] |
| 8. | Muhoza P, Danovaro-Holliday MC, Diallo MS, Murphy P, Sodha SV, Requejo JH, Wallace AS. Routine Vaccination Coverage - Worldwide, 2020. MMWR Morb Mortal Wkly Rep. 2021;70:1495-1500. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 24] [Cited by in RCA: 93] [Article Influence: 23.3] [Reference Citation Analysis (0)] |
| 9. | Statistics Canada. Childhood National Immunization Coverage Survey, 2021. [cited 23 June 2023]. Available from: https://www150.statcan.gc.ca/n1/daily-quotidien/230612/dq230612b-eng.htm?utm_campaign=statcan-statcan-cnics-encve-23-24&utm_medium=eml&utm_source=stakeholder230612. |
| 10. | CDC. COVID-19 vaccination for children. Centers for Disease Control and Prevention. [cited 18 September 2023]. Available from: https://www.cdc.gov/vaccines/covid-19/planning/children.html. |
| 11. | Muñoz FM, Sher LD, Sabharwal C, Gurtman A, Xu X, Kitchin N, Lockhart S, Riesenberg R, Sexter JM, Czajka H, Paulsen GC, Maldonado Y, Walter EB, Talaat KR, Englund JA, Sarwar UN, Hansen C, Iwamoto M, Webber C, Cunliffe L, Ukkonen B, Martínez SN, Pahud BA, Munjal I, Domachowske JB, Swanson KA, Ma H, Koury K, Mather S, Lu C, Zou J, Xie X, Shi PY, Cooper D, Türeci Ö, Şahin U, Jansen KU, Gruber WC; C4591007 Clinical Trial Group. Evaluation of BNT162b2 Covid-19 Vaccine in Children Younger than 5 Years of Age. N Engl J Med. 2023;388:621-634. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 56] [Article Influence: 28.0] [Reference Citation Analysis (0)] |
| 12. | CPS. COVID-19 vaccine for children and adolescents. Canadian Paediatric Society. Feb 4, 2022. [cited 18 September 2023]. Available from: https://cps.ca/en/documents/position/covid-19-vaccine-for-children-and-adolescents. |
| 13. | Rahmati M, Yon DK, Lee SW, Udeh R, McEVoy M, Kim MS, Gyasi RM, Oh H, López Sánchez GF, Jacob L, Li Y, Koyanagi A, Shin JI, Smith L. New-onset type 1 diabetes in children and adolescents as postacute sequelae of SARS-CoV-2 infection: A systematic review and meta-analysis of cohort studies. J Med Virol. 2023;95:e28833. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 24] [Reference Citation Analysis (0)] |
| 14. | Rahmati M, Keshvari M, Mirnasuri S, Yon DK, Lee SW, Il Shin J, Smith L. The global impact of COVID-19 pandemic on the incidence of pediatric new-onset type 1 diabetes and ketoacidosis: A systematic review and meta-analysis. J Med Virol. 2022;94:5112-5127. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 86] [Cited by in RCA: 98] [Article Influence: 32.7] [Reference Citation Analysis (2)] |
| 15. | Dembiński Ł, Vieira Martins M, Huss G, Grossman Z, Barak S, Magendie C, Del Torso S, Dornbusch HJ, Mazur A, Albrecht K, Hadjipanayis A. SARS-CoV-2 Vaccination in Children and Adolescents-A Joint Statement of the European Academy of Paediatrics and the European Confederation for Primary Care Paediatricians. Front Pediatr. 2021;9:721257. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 14] [Article Influence: 3.5] [Reference Citation Analysis (0)] |