Published online Feb 8, 2016. doi: 10.5409/wjcp.v5.i1.136
Peer-review started: August 22, 2015
First decision: October 13, 2015
Revised: November 17, 2015
Accepted: December 17, 2015
Article in press: December 18, 2015
Published online: February 8, 2016
Processing time: 161 Days and 15.4 Hours
Acute lobar nephritis (ALN) is a localized non-liquefactive inflammatory renal bacterial infection, which typically involves one or more lobes. ALN is considered to be a midpoint in the spectrum of upper urinary tract infection, a spectrum ranging from uncomplicated pyelonephritis to intrarenal abscess. This condition may be difficult to recognize due to the lack of specific symptoms and laboratory findings. Therefore the disease is probably underdiagnosed. Computed tomography scanning represents the diagnostic gold standard for ALN, but magnetic resonance imagine could be considered in order to limit irradiation. The diagnosis is relevant since initial intravenous antibiotic therapy and overall length of treatment should not be shorter than 3 wk. We review the literature and analyze the ALN clinical presentation starting from four cases with the aim to give to the clinicians the elements to suspect and recognize the ALN in children.
Core tip: Acute lobar nephritis (ALN) is a renal bacterial infection presenting difficult diagnosis due to the lack of specific symptoms and laboratory findings. Suspecting ALN in children with septic fever with or without clinical signs should be part of the diagnostic tool of clinicians. The diagnosis is relevant both to prefer intravenous antibiotic therapy and suggest an overall length of antibiotic treatment not shorter than 3 wk. We review the literature and analyze the ALN clinical presentation, with the aim to give to the clinician the elements to suspect, diagnose and accurately treat ALN in children.
- Citation: Bibalo C, Apicella A, Guastalla V, Marzuillo P, Zennaro F, Tringali C, Taddio A, Germani C, Barbi E. Acute lobar nephritis in children: Not so easy to recognize and manage. World J Clin Pediatr 2016; 5(1): 136-142
- URL: https://www.wjgnet.com/2219-2808/full/v5/i1/136.htm
- DOI: https://dx.doi.org/10.5409/wjcp.v5.i1.136
Acute lobar nephritis (ALN), also known as acute focal bacterial nephritis, is a localized non-liquefactive inflammatory renal bacterial infection, which typically involves one or more lobes[1,2]. It presents as an inflammatory mass without frank abscess formation[3]. ALN is considered to be a midpoint in the spectrum of upper urinary tract infection (UTI), a spectrum ranging from uncomplicated pyelonephritis to intrarenal abscess[4]. According to some authors[5], this spectrum lacks a dynamic progressive nature and two patterns, based on computed tomography (CT) findings, are described: Simple ALN, which represents progression of acute pyelonephritis (APN), and complicated ALN, which may progress into renal abscess without or even with treatment[6]. The typical presentation of ALN shares some common clinical and laboratory features with both renal abscess and APN including septic fever, flank pain, sick appearance, nausea or vomiting, elevation of inflammatory markers, pyuria and bacteriuria[1,7]. According to a recent study patients with ALN are febrile for longer after hospitalization and have more nausea/vomiting symptoms than those with APN[8]. A timely diagnosis is relevant because under-diagnosis may result in late renal scarring, and/or evolution in renal abscess, which in turn may lead to hypertension or renal failure[9].
A 4-year-old girl was admitted with a 2 d history of high fever and abdominal pain. Fever persisted despite an oral amoxicillin-clavulanate treatment prescribed by her family physician.
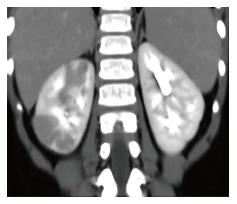
The patient’s medical history was remarkable for an episode of APN 2 years before, successfully treated with oral antibiotics. At admission she was febrile and looked sick with an unremarkable physical examination. White blood cell count (WBC) was 24.600/mm3, C-reactive protein (CRP) 24.52 mg/dL (normal range 0-5 mg/dL) and erythrocyte sedimentation rate (ESR) 97 mm/h (normal range 0-20 mm/h). Urinalysis revealed leukocyturia (200 WBC/mm3 at standard optical microscopy) without bacteriuria. Urine cultures were repeatedly negative as was chest X-ray. Abdominal ultrasonography (US) showed a nonspecific diffuse increased echogenicity of the right kidney, which appeared smaller than the left; no focal masses were detected on both kidneys. A CT scan showed multiple lesions with irregular margins and variable size in the right kidney, which appeared hypodense after contrast medium administration (Figure 1). ALN was diagnosed and a three weeks intravenous antimicrobial therapy with ciprofloxacin and tobramycin was started with clinical improvement. Voiding cystourethrography (VCUG) and dimercaptosuccinic acid (DMSA) renal scintigraphy performed 6 mo later showed a reflux with associated renal scarring nephropathy.
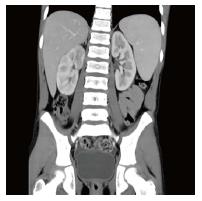
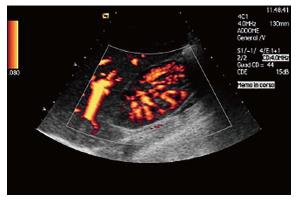
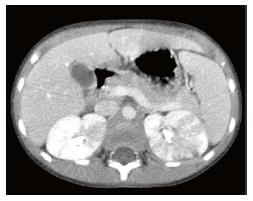
A 13-year-old boy was admitted after 3 episodes of high fever in the last 2 mo, without an obvious focus. During the first episode, the boy was confused and agitated; CT and magnetic resonance imagine (MRI) of the brain, cerebrospinal fluid (CSF) examination, electroencephalography (EEG), chest X-rays, urinalysis with standard optical microscopy, urine culture were normal; blood test showed increased CRP (10.8 mg/dL). Empirical therapy with acyclovir and ceftriaxone was started with clinical success, maintained for 5 d and switched to oral treatment for 5 more days. The boy was discharged with a diagnosis of suspected encephalitis. After 2 wk of wellness, the patient presented fever, vomiting and drowsiness. MRI of the brain was normal. Chest X-ray and echocardiogram were also normal. CRP was 13.9 mg/dL. Abdominal US was negative. Empirical treatment with ceftriaxone was started with rapid improvement. The boy was discharged after 5 d of intravenous therapy; at home he continued with 3 d oral amoxicillin-clavulanate. Four days after the end of treatment, he was admitted for the third time with fever and vomiting. On examination, he was in good clinical condition. The abdomen was soft, slightly painful in the right flank. CRP was 10.4 mg/dL. Urinalysis with optical microscopy, chest X-rays and abdominal US were negative. An abdominal CT scan was performed. The scan (Figure 2) revealed multiple poorly defined hypodense areas after contrast medium administration in the right kidney, compatible with ALN. One of these areas presented a 5 mm colliquative part in the middle, attributable to an abscess. An abdominal US was repeated (Figure 3) with power-doppler analysis showing at least two hypoperfused areas at the right kidney. The patient’s medical history was unremarkable; no previous UTIs were reported. Intravenous antimicrobial therapy with tobramycin and teicoplanin was started and maintained for 3 wk, followed by oral amoxicillin-clavulanate for other 3 wk.
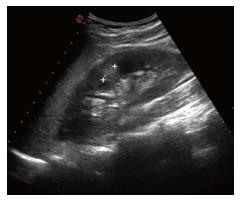
A 17-year-old girl was admitted with a 2 d history of high fever, chills and pain on the left flank. On physical examination, she looked sick; the abdomen was soft and painful in the left flank. WBC count was normal (8340/mm3), while there was a marked increase of both CRP (25.33 mg/dL) and ESR (62 mm/h). Urinalysis revealed leukocyturia (50 WBC/mm3 at standard optical microscopy) but no bacteriuria. Urine and blood cultures were repeatedly negative. Abdominal US (Figure 4) showed an increased volume of the left kidney with a small hyperechoic mass (1 cm diameter), consistent with ALN. Intravenous therapy with ceftriaxone and tobramycin was started; after 48 h the patient was still febrile and sick, therefore treatment was switched to intravenous ciprofloxacin, teicoplanin and cefotaxime. There was a slow and gradual clinical improvement and after 72 h, the fever disappeared. Intravenous antimicrobial therapy was maintained for three weeks.
A 6-year-old girl presented with a 24 h history of high fever, vomiting and abdominal pain on the left iliac fossa without diarrhea. Physical examination was unremarkable except for an abdominal evoked pain in the left iliac fossa. WBC was 21.190/mm3, CRP 34 mg/dL. Urinalysis with standard optical microscopy was negative and therefore urine cultures were not performed. Chest X-ray was normal. Abdominal US showed an increased volume of both kidneys; CT scan was then performed revealing multiple wedge-shaped cortical hypodense lesions in both kidneys, more represented in the left one (Figure 5). Intravenous therapy with ceftriaxone was started; after 48 h, the patient was still febrile and sick, so intravenous netilmicin was added with clinical improvement. The therapy was continued for 10 d, then switched to oral ciprofloxacin, for additional 2 wk.
ALN may be difficult to recognize due to the frequent absence of specific signs and symptoms and the wide differential diagnosis (Table 1). Specific symptoms as flank pain or laboratory findings (positive urinalysis and bacteriuria) may be absent. Therefore the disease is probably underdiagnosed[10]. Nevertheless, fever with septic features (sick appearance, malaise, chills, and nausea or vomiting), increased inflammatory indexes and/or abdominal pain, should suggest a deep bacterial infection. The diagnosis of this condition is relevant due to the need of a specific therapeutic approach.
| Clinical and laboratoristic ALN differential diagnosis | |
| APN | Leukocyturia and bacteriuria |
| Appendicitis[26] | Mc Burney, Blumberg and Rovsing’s sign, right iliac fossa pain, typical age |
| Gastroenteritis[27] | Diarrhea, dehydration’s signs |
| Infected urachal cyst[28] | Belly button discharge |
| Nephrolithiasis[29] | Colic pain, familiarity, previous episode, micro/macrohematuria, Giordano’s sign |
| Pancreatitis[30] | Typical pain, serum amylase and lipase elevated |
| Pelvic inflammatory disease[31] | Sexually active female, irregular periods, vaginal discharge, dyspareunia, lower abdomen pain |
| Pneumonia[32] | Dyspnea, cough, typical auscultation, Sat O2 < 96% |
| Sickle cell disease[33] | Anemia, decreased haptoglobin, sickle cell, ethnicity |
Sonographically, ALN presents as focal hypoperfused lesions with poorly defined irregular margins disrupting cortico-medullary differentiation. Masses can be respectively hyper-, iso-, or hypo-echogenic depending on the temporal sequence of the lesions and resolution of the disease[11,12]. Renal pole swelling has also been reported[11,13,14]. Although renal US is an effective diagnostic method, there may be false positive and false negative results[13,15], and often a false negative US is frequently reported. A study[16] demonstrated that isolated severe nephromegaly (defined as renal length of greater than mean +3 SD for age) has a diagnostic sensitivity of 90%; the finding of a focal renal mass increases the sensitivity to 95% (compared with the gold standard CT), with a specificity of 86.4%. The diagnostic gold standard for ALN is CT scanning[11,13,15,17]. CT images of the involved areas are usually normal in non-enhanced scans but appear as wedge-shaped, poorly defined regions of decreased nephrogenic density after contrast medium administration[11,13]. With the aim to avoid radiation exposure, MRI should be strongly considered[18]; in fact CT scan results in a small but not negligible increased lifetime risk for cancer[19,20]. Enhanced ultrasound in the near future could replace CT scan because of comparable sensitivity and specificity. Unfortunately second-generation contrast agents are off-label in children, even if there are no adverse events documented in literature[21]. Static scintigraphy with DMSA, the gold standard to identify renal involvement in UTI, has no application in the differential diagnosis of this condition showing only focal uptake defects with the means of a hypoactive area in the renal parenchyma. In the literature, positive urine culture rate has a wide variability; the bias probably depends on the ability of different centers to diagnose ALN, particularly when urinalysis and urine are negative. When positive, results are not different from other forms of UTI: The most represented urinary pathogen is Escherichia coli in 40%-75% of the cases, while other gram negative germs are less frequent; gram positive germs infection is unusual[8,10,22].
Treatment is based on antibiotic therapy. Empiric approach, before antibiogram response when available, should be targeted at gram negative germs. Intravenous administration is recommended at least until 2 to 3 d after defervescence with a possible switch to oral treatment. A study suggested that a 3 wk antimicrobial therapy protocol should constitute the treatment of choice for all radiographically documented patients with ALN[22]. Surgical intervention is needed in the 25% of the cases where the lesion turns to renal abscess[23].
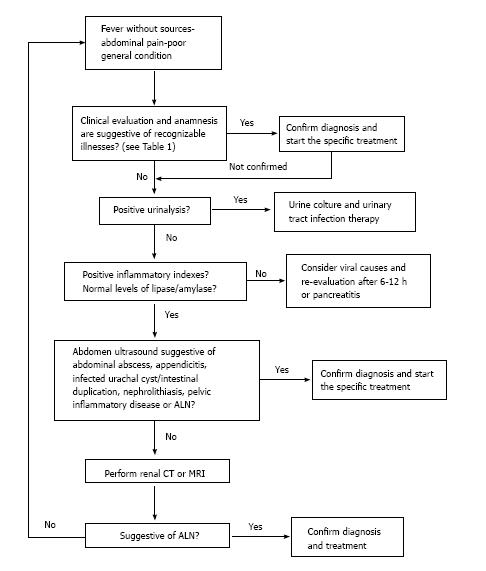
These 4 cases presented with high fever, toxic appearance and abdominal pain. Only 1 case presented with flank pain, a specific UTI symptom not reliable before age of 6-8 years. Furthermore, as a confounding factor, urinalysis showed leukocyturia only in 2 cases, both with no bacteriuria at microscopy and negative urine cultures (one of these children started antibiotic treatment prior to admission). The other 2 patients presented negative microscopic and dip stix urinalysis. In case 4, urine culture was reported not performed because of the negative urinalysis. Our findings are in line with previous published reports. Evaluating data of 25 children diagnosed with ALN, some authors[10] showed that the main clinical presentation was represented by septic temperatures and rapid deterioration of clinical condition, characteristics that were present in all the children. Only the older children (10 out of 25), with a mean age of 8 years, suffered from specific symptoms such as flank pain, whereas younger children presented with unspecific symptoms such as vomiting, lethargy, abdominal pain or poor feeding. Laboratory findings showed always an elevation of CRP, ESR and WBC. Leukocyturia and bacteriuria were not found in all of the children but in 18/25 and 20/25 respectively. Positive urine cultures were found in 20/25 children; however 4 of 5 children with negative urine cultures had been pretreated with oral antibiotics prior to admission. In our experience, CT scan was performed in 3 cases. In case 3, US images were so typical (enlargement of the kidney and presence of a mass) that we decided not to obtain CT scans, in order to avoid irradiation of the patient. Case 2 is noteworthy because CT revealed multiple lesions, one of these with a 5 mm colliquation area, probably an ALN evolution in abscess. US power Doppler, performed the day after, identified upper UTI compatible lesions. According to some authors, ALN should be considered as complicated UTI. Further radiological examination as VCUG is thus considered mandatory for the detection of urinary tract anomalies, known as the main underlying predisposing factors of ALN in children[24,25]. This series highlights the lack of specific clinical presentation of ALN. This condition should be suspected in front of a child with high fever, poor general condition and elevation of inflammatory markers, without an apparent infective focus even in presence of negative abdominal ultrasound, urinalysis and microscopy. Alternatively ALN should be suspected in patients with APN not responsive to antibiotic treatment. We suggest avoiding CT scan when sonographic criteria of severe nephromegaly and focal mass are present and to perform MRI instead of CT in the other cases, in order to minimize radiation exposure. We present a diagnostic algorithm that could be used to suspect and then recognize ALN in children (Figure 6).
Clinicians often take on challenge with septic fever without clear clinical signs; the authors report four cases presenting with acute lobar nephritis (ALN), an underestimated condition, with the aim to give to the clinicians the instruments to suspect and diagnose ALN. A timely diagnosis is relevant because under-diagnosis may result in late renal scarring, and/or evolution in renal abscess, which in turn may lead to hypertension or renal failure.
Important areas of research could be evaluate the sensitivity and specificity of both magnetic resonance and intravenously enhanced ultrasound in diagnosing ALN with the aim to avoid computed tomography and then to spare radiations.
In literature there is lack of data about ALN in childhood. The authors report of four cases of pediatric ALN, rising diagnostic and therapeutic issues. Furthermore the authors describe their experience about MR or enhanced ultrasound study of kidney in diagnosing ALN. These techniques are not mentioned elsewhere in the ALN diagnosis.
All children with septic fever with or without abdominal pain should raise in the clinicians the suspect of deep bacterial infection. For a correct diagnosis it is essential both performing urinalysis before antibiotic therapy and abdominal imaging.
Enhanced ultrasound is a free radiation imaging technique consisting in instillation of microbubble in bladder or vein emphasizing structures. Unfortunately, its use in children is still off-label.
This is a series of 4 cases with acute lobar nephritis in children discussing the clinical presentation, radiological features, treatment and management issues.
P- Reviewer: Bhimma R, Mubarak M S- Editor: Ji FF L- Editor: A E- Editor: Lu YJ
| 1. | Zaontz MR, Pahira JJ, Wolfman M, Gargurevich AJ, Zeman RK. Acute focal bacterial nephritis: a systematic approach to diagnosis and treatment. J Urol. 1985;133:752-757. [PubMed] |
| 2. | Kline MW, Kaplan SL, Baker CJ. Acute focal bacterial nephritis: diverse clinical presentations in pediatric patients. Pediatr Infect Dis J. 1988;7:346-349. [PubMed] |
| 3. | Rosenfield AT, Glickman MG, Taylor KJ, Crade M, Hodson J. Acute focal bacterial nephritis (acute lobar nephronia). Radiology. 1979;132:553-561. [PubMed] |
| 4. | Sheu JN. Acute lobar nephronia in children. Pediatr Neonatol. 2015;56:141-142. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 5] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 5. | Cheng CH, Tsau YK, Lin TY. Is acute lobar nephronia the midpoint in the spectrum of upper urinary tract infections between acute pyelonephritis and renal abscess? J Pediatr. 2010;156:82-86. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 30] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 6. | Shimizu M, Katayama K, Kato E, Miyayama S, Sugata T, Ohta K. Evolution of acute focal bacterial nephritis into a renal abscess. Pediatr Nephrol. 2005;20:93-95. [PubMed] |
| 7. | Soulen MC, Fishman EK, Goldman SM, Gatewood OM. Bacterial renal infection: role of CT. Radiology. 1989;171:703-707. [PubMed] |
| 8. | Chen WL, Huang IF, Wang JL, Hung CH, Huang JS, Chen YS, Lee SS, Hsieh KS, Tang CW, Chien JH. Comparison of acute lobar nephronia and acute pyelonephritis in children: a single-center clinical analysis in southern taiwan. Pediatr Neonatol. 2015;56:176-182. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 11] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 9. | Williams G, Fletcher JT, Alexander SI, Craig JC. Vesicoureteral reflux. J Am Soc Nephrol. 2008;19:847-862. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 133] [Cited by in RCA: 112] [Article Influence: 6.6] [Reference Citation Analysis (0)] |
| 10. | Seidel T, Kuwertz-Bröking E, Kaczmarek S, Kirschstein M, Frosch M, Bulla M, Harms E. Acute focal bacterial nephritis in 25 children. Pediatr Nephrol. 2007;22:1897-1901. [PubMed] |
| 11. | Rathore MH, Barton LL, Luisiri A. Acute lobar nephronia: a review. Pediatrics. 1991;87:728-734. [PubMed] |
| 12. | Boam WD, Miser WF. Acute focal bacterial pyelonephritis. Am Fam Physician. 1995;52:919-924. [PubMed] |
| 13. | Rauschkolb EN, Sandler CM, Patel S, Childs TL. Computed tomography of renal inflammatory disease. J Comput Assist Tomogr. 1982;6:502-506. [PubMed] |
| 14. | Loberant N, Jerushalmi J, Camal S, Gaitini D, Greif Z, Noi I. Acute focal bacterial nephritis: emphasis on imaging. Child Nephrol Urol. 1990;10:150-153. [PubMed] |
| 15. | Klar A, Hurvitz H, Berkun Y, Nadjari M, Blinder G, Israeli T, Halamish A, Katz A, Shazberg G, Branski D. Focal bacterial nephritis (lobar nephronia) in children. J Pediatr. 1996;128:850-853. [PubMed] |
| 16. | Cheng CH, Tsau YK, Hsu SY, Lee TL. Effective ultrasonographic predictor for the diagnosis of acute lobar nephronia. Pediatr Infect Dis J. 2004;23:11-14. [PubMed] |
| 17. | Yang CC, Shao PL, Lu CY, Tsau YK, Tsai IJ, Lee PI, Chang LY, Huang LM. Comparison of acute lobar nephronia and uncomplicated urinary tract infection in children. J Microbiol Immunol Infect. 2010;43:207-214. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 14] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 18. | Yılmaz K, Koç G, Yel S, Dursun İ, Doğanay S. Acute lobar nephronia: value of unique magnetic resonance imaging findings in diagnosis and management. Turk J Pediatr. 2015;57:105-108. [PubMed] |
| 19. | Chodick G, Ronckers CM, Shalev V, Ron E. Excess lifetime cancer mortality risk attributable to radiation exposure from computed tomography examinations in children. Isr Med Assoc J. 2007;9:584-587. [PubMed] |
| 20. | Brenner D, Elliston C, Hall E, Berdon W. Estimated risks of radiation-induced fatal cancer from pediatric CT. AJR Am J Roentgenol. 2001;176:289-296. [PubMed] |
| 21. | Mitterberger M, Pinggera GM, Colleselli D, Bartsch G, Strasser H, Steppan I, Pallwein L, Friedrich A, Gradl J, Frauscher F. Acute pyelonephritis: comparison of diagnosis with computed tomography and contrast-enhanced ultrasonography. BJU Int. 2008;101:341-344. [PubMed] |
| 22. | Cheng CH, Tsau YK, Lin TY. Effective duration of antimicrobial therapy for the treatment of acute lobar nephronia. Pediatrics. 2006;117:e84-e89. [PubMed] |
| 23. | Bachur R. Nonresponders: prolonged fever among infants with urinary tract infections. Pediatrics. 2000;105:E59. [PubMed] |
| 24. | Uehling DT, Hahnfeld LE, Scanlan KA. Urinary tract abnormalities in children with acute focal bacterial nephritis. BJU Int. 2000;85:885-888. [PubMed] |
| 25. | Ammenti A, Cataldi L, Chimenz R, Fanos V, La Manna A, Marra G, Materassi M, Pecile P, Pennesi M, Pisanello L. Febrile urinary tract infections in young children: recommendations for the diagnosis, treatment and follow-up. Acta Paediatr. 2012;101:451-457. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 114] [Cited by in RCA: 108] [Article Influence: 8.3] [Reference Citation Analysis (0)] |
| 26. | Marzuillo P, Germani C, Krauss BS, Barbi E. Appendicitis in children less than five years old: A challenge for the general practitioner. World J Clin Pediatr. 2015;4:19-24. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 81] [Cited by in RCA: 74] [Article Influence: 7.4] [Reference Citation Analysis (1)] |
| 27. | Whyte LA, Al-Araji RA, McLoughlin LM. Guidelines for the management of acute gastroenteritis in children in Europe. Arch Dis Child Educ Pract Ed. 2015;100:308-312. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 16] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 28. | Allen JW, Song J, Velcek FT. Acute presentation of infected urachal cysts: case report and review of diagnosis and therapeutic interventions. Pediatr Emerg Care. 2004;20:108-111. [PubMed] |
| 29. | Polito C, Apicella A, Marte A, Signoriello G, La Manna A. Clinical presentation and metabolic features of overt and occult urolithiasis. Pediatr Nephrol. 2012;27:101-107. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 7] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 30. | Suzuki M, Sai JK, Shimizu T. Acute pancreatitis in children and adolescents. World J Gastrointest Pathophysiol. 2014;5:416-426. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 68] [Cited by in RCA: 64] [Article Influence: 5.8] [Reference Citation Analysis (2)] |
| 31. | Greydanus DE, Dodich C. Pelvic inflammatory disease in the adolescent: a poignant, perplexing, potentially preventable problem for patients and physicians. Curr Opin Pediatr. 2015;27:92-99. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 13] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 32. | Wallihan R, Ramilo O. Community-acquired pneumonia in children: current challenges and future directions. J Infect. 2014;69 Suppl 1:S87-S90. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 26] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 33. | Chakravorty S, Williams TN. Sickle cell disease: a neglected chronic disease of increasing global health importance. Arch Dis Child. 2015;100:48-53. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 101] [Cited by in RCA: 121] [Article Influence: 12.1] [Reference Citation Analysis (0)] |