Peer-review started: September 29, 2016
First decision: October 31, 2016
Revised: February 22, 2017
Accepted: March 13, 2017
Article in press: March 13, 2017
Published online: June 28, 2017
Processing time: 271 Days and 8.2 Hours
Parkinson’s disease (PD) is an idiopathic progressive neurological disorder characterised by resting tremor, restrictions in mobility and muscular rigidity that can lead to problems in maintaining oral health. Here we report a case where crown lengthening surgeries were successfully performed in a PD patient for complete oral rehabilitation. Certain special considerations that are required before and during periodontal surgery in such patients are also elucidated. Often dentists and PD patients are reluctant to embark on complex dental procedures resulting in a compromised outcome. However, early intervention along with proper education and motivation of these patients can aid in achieving satisfactory results.
Core tip: Parkinson’s disease (PD) is a degenerative disorder of the central nervous system. Diagnosis of PD is often made after careful history taking, physical examination and observing a positive continued response to dopaminergic medications. Laboratory tests and imaging studies are not used routinely. The problems encountered during the dental treatment of a PD patient include the patient’s inability to keep his mouth open, uncontrolled movements of head and tongue and excessive salivation. This case report lays emphasis on various considerations that are required while doing periodontal surgery in these patients.
- Citation: Arora R, Sharma RK, Tewari S, Kapoor H. Periodontal surgery in a stage II Parkinson’s disease patient: Report of a case with special considerations. World J Neurol 2017; 7(2): 24-27
- URL: https://www.wjgnet.com/2218-6212/full/v7/i2/24.htm
- DOI: https://dx.doi.org/10.5316/wjn.v7.i2.24
Parkinson’s disease (PD) is an advanced neurodegenerative disorder in which patient experiences resting tremor, bradykinesia, constrained mobility and lack of postural stability which have deleterious effects on patient’s quality of life[1]. Patients with PD may require dental treatment for root caries, periodontitis, fractured or attrited teeth and complete oral rehabilitation. Due to the progressive nature of the disease, it is prudent to perform major dental procedures early in the course of the disease; a conservative approach is considered more appropriate in later stages of PD[2]. Restorations with well-defined margins may not be obtainable in the presence of subgingival decay, short clinical crowns, traumatic injury or endodontic perforation, which may hence require crown lengthening surgeries (CLS)[3].
The literature regarding intraoral surgical procedures in PD patients is very limited and mainly includes isolated reports of implant placement[4]. Periodontal surgery in such patients can be performed in routine practice if certain guidelines are followed at the time of surgery. Here we present a case of successful management of an early PD patient in which CLS were performed for oral rehabilitation.
A 68-year-old male patient was referred to the Department of Periodontics, Government Dental College, Rohtak for CLS on certain teeth. Patient gave a history of two years of PD and was taking medications for the same. His medical reports indicated that he was having early PD (stage 2 on Hoehn and Yahr scale)[5] with right side more affected. The patient was taking a combination of Levodopa (100 mg) and Carbidopa (10 mg) thrice daily for the past one year. Patient had a slightly stooped posture with bradykinesia and resting tremor. Parkinsonian tremors were also observed in lips. Past dental history included root canal treatment in 13, 23, 31, 32, 33, 41, 42 and 43; and extractions of 12, 14, 15, 25, 26 and 34.
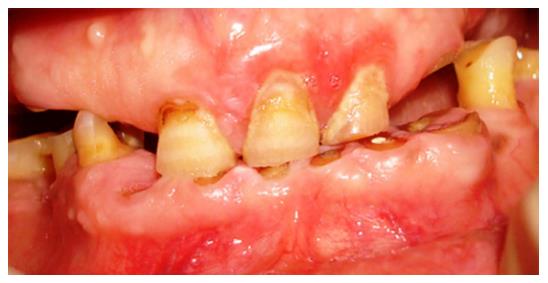
Intraoral examination revealed eleven teeth in mandibular and six in maxillary arch with an average gingival and plaque index score of two (Figure 1). The lower incisors were severely attrited. These along with upper and lower left canines exhibited insufficient supragingival sound tooth structure for crown margin preparation. An orthopantamograph and intra oral periapical radiographs were obtained. Crown lengthening surgery was planned in 13, 23 and 33. Mandibular incisors, due to their short clinical root lengths were not suitable for undergoing this procedure. However they were retained for prosthodontic reasons. Patient’s physician was consulted for evaluation of patient’s medical status before undergoing periodontal surgical procedure. A written informed consent was acquired from the patient after explaining him the procedure.
Beginning with oral prophylaxis, the patient was scheduled for an early morning appointment for CLS. He was asked to take his medication 60-90 min before the procedure so that peak effectiveness of the medication could be attained at the time of surgery. He was assisted in sitting on the dental chair and the chair was slowly raised to a 45° position to make him comfortable. After administration of local anaesthesia, internal bevel incisions along buccal and palatal aspects of 23 were given which continued as a distal wedge on the adjacent edentulous region. Full thickness buccal and palatal flaps were then reflected. Ostectomy and osteoplasty were carried out with hand and rotary instruments under copious irrigation. Vacuum suction was used throughout the procedure.
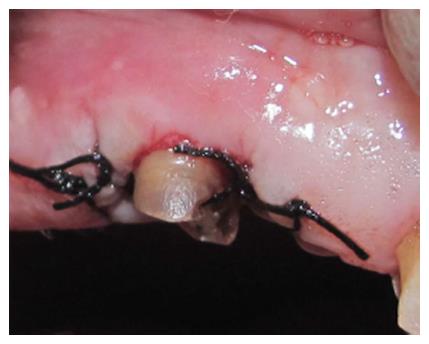
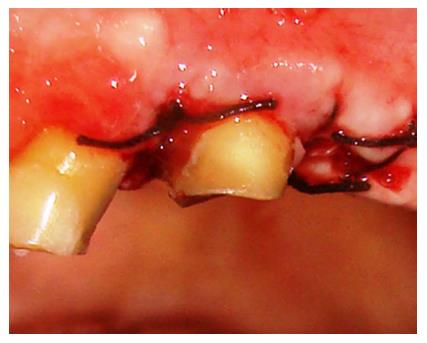
A periodontal probe was used to confirm the presence of at least 5 mm of sound tooth structure coronal to the crest of bone all around the tooth. The flaps were then adjusted and sutured (Figures 2 and 3). Post operative instructions were given and the patient was asked to report after a week for suture removal. Similar procedure was carried out for tooth numbers 13 and 33. Healing at the end of 1, 2 and 4 wk was found to be good and there were no post surgical concerns. Oral hygiene maintenance was reinforced at each visit. Oral rehabilitation was completed in another six weeks (Figure 4).
PD is a progressive disorder of the central nervous system which results from the degeneration of dopamine-containing cells in the substantia nigra, a region of the midbrain. Most people with PD first experience non motor symptoms like constipation, mood changes, anosmia and orthostatic hypotension which are then followed by motor symptoms. The initial symptoms in the course of the disease are movement-related, comprising shaking, rigidity, sluggishness of movement and difficulty in walking. In due course of time, cognitive and behavioural complications may arise. Dementia has also been seen to occur in the later stages of the disease.
A diagnosis of PD is often made after careful history taking, physical examination and observing a positive continued response to dopaminergic medications. Laboratory tests and imaging studies are not used routinely. The problems encountered during the dental treatment of a PD patient include the patient’s inability to keep his mouth open, uncontrolled movements of head and tongue and excessive salivation. Weakened ability to swallow can increase the risk of aspiration. PD patients who have been on medications like levodopa may begin to develop dyskinesias after several years, which can affect the jaw as well as lead to teeth grinding. The present patient had sufficient mouth opening, not requiring a mouth prop or bite block, minimal orofacial tremors and normal salivary flow inspite of levodopa medication. Tremor and rigour of the orofacial muscles may bring pain, temporomandibular joint discomfort and attrition[6].
Restoration of oral health is best completed as early as possible in PD, as was done in the present case. Treatment plan for these patients should be devised taking care of patient’s long term dental needs. Retaining teeth can be a means of preserving bone when planning a partial or complete tooth supported overdenture. Teeth, which are periodontally compromised or decayed may serve as overdenture abutments after root canal treatment and/or CLS. PD patients often have difficulty in retaining their dentures due to tremors, rigidity and drooling saliva[7]. Overdentures can provide better masticatory efficiency as compared to conventional complete dentures and were therefore planned for this patient.
As PD is commonly associated with urinary urgency and incontinence, these patients should be asked to empty their bladders before beginning with any dental procedure[8]. The dental chair should be raised slowly, allowing the patient to adjust to the upright sitting position to accommodate PD-associated autonomic dysfunction[9]. Depending on the patient’s physical disability, intravenous sedation, local or general anesthesia can be administered. Appointments should be kept short, not longer than 45 min and should begin about one to one and half hour after administration of PD medication[6]. The periodontist needs to be extremely patient while giving incisions or performing osseous reduction which require utmost precision. PD patients require certain special instructions as they may face difficulty in maintaining oral hygiene[10]. Use of toothbrush with specially designed handle for better grasp or an electric toothbrush is recommended as was done in the present case. Mouthwashes are generally not advised for people with PD because they present the risk of choking, but in cases where they are required, it is best to prescribe those which are non-alcohol based.
This report demonstrates that CLS with osseous resection can be successfully performed in a PD patient and PD is no contraindication to periodontal surgery as is generally believed.
A 68-year-old male patient having difficulty in chewing was referred for crown lengthening surgeries (CLS) in certain teeth.
Patient had severely attrited maxillary and mandibular teeth which required crown lengthening for the placement of an overdenture. Patient was found to have stage II Parkinson’s disease (PD).
Complete blood counts were within normal limits.
Insufficient crown lengths in maxillary and mandibular teeth and stage II PD.
CLS with special considerations were performed.
Often dentists and PD patients are reluctant to embark on complex dental procedures resulting in a compromised outcome. However, early intervention along with proper education and motivation of PD patients can aid in achieving satisfactory results.
Arora et al report periodontal surgery in a patient with PD and discuss potential Parkinson-specific problems, obstacles and caveats when performing dental procedures. The manuscript is concise and well-written.
Manuscript source: Unsolicited manuscript
Specialty type: Clinical neurology
Country of origin: India
Peer-review report classification
Grade A (Excellent): A
Grade B (Very good): B
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P- Reviewer: Orlacchio A, Unger M, Xu PY S- Editor: Ji FF L- Editor: A E- Editor: Li D
| 1. | Bhat V, Weiner WJ. Parkinson’s disease. Diagnosis and the initiation of therapy. Minerva Med. 2005;96:145-154. [PubMed] |
| 2. | Lobbezoo F, Naeije M. Dental implications of some common movement disorders: a concise review. Arch Oral Biol. 2007;52:395-398. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 21] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 3. | Arora R, Narula SC, Sharma RK, Tewari S. Evaluation of supracrestal gingival tissue after surgical crown lengthening: a 6-month clinical study. J Periodontol. 2013;84:934-940. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 50] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 4. | Packer M, Nikitin V, Coward T, Davis DM, Fiske J. The potential benefits of dental implants on the oral health quality of life of people with Parkinson’s disease. Gerodontology. 2009;26:11-18. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 31] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 5. | Hoehn MM, Yahr MD. Parkinsonism: onset, progression, and mortality. 1967. Neurology. 1998;50:318 and 16 pages following. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 316] [Cited by in RCA: 341] [Article Influence: 12.6] [Reference Citation Analysis (0)] |
| 6. | Friedlander AH, Mahler M, Norman KM, Ettinger RL. Parkinson disease: systemic and orofacial manifestations, medical and dental management. J Am Dent Assoc. 2009;140:658-669. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 45] [Cited by in RCA: 45] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 8. | Winge K, Skau AM, Stimpel H, Nielsen KK, Werdelin L. Prevalence of bladder dysfunction in Parkinsons disease. Neurourol Urodyn. 2016;25:116–122. [RCA] [DOI] [Full Text] [Cited by in Crossref: 94] [Cited by in RCA: 79] [Article Influence: 4.2] [Reference Citation Analysis (1)] |
| 9. | Alexander RE, Gage TW. Parkinson’s disease: an update for dentists. Gen Dent. 2000;48:572-580; quiz 581-582. [PubMed] |
| 10. | Collins R. Special considerations for the dental patient with Parkinson’s disease. Tex Dent J. 1990;107:31-32. [PubMed] |