Published online Jul 18, 2018. doi: 10.5312/wjo.v9.i7.100
Peer-review started: May 5, 2018
First decision: June 6, 2018
Revised: June 15, 2018
Accepted: June 28, 2018
Article in press: June 28, 2018
Published online: July 18, 2018
Processing time: 75 Days and 13 Hours
Anterior transolecranon dislocation of the elbow is rarely observed in children, reported in only a small series. The present case involves an anterior transolecranon dislocation of the left elbow joint in a 7-year-old child, which was surgically treated. Two attempts of closed reduction failed because the radial head had buttonholed via the joint capsule. After its release, open reduction was easily performed; osteosynthesis of the olecranon was not performed. Remarkably, good result was obtained, despite a mild flexion deformity at the last follow-up. This case report aims to highlight this treatment method, which may be considered for such an uncommon injury.
Core tip: Anterior transolecranon dislocation is rarely observed in children and rarely reported in the literature. This case shows that the management of this injury can be difficult, requiring surgery with or without osteosynthesis of the olecranon.
- Citation: Bouaziz W, Guidara AR, Trabelsi A, Bardaa T, Hammami M, Ellouz Z, Keskes H. Anterior transolecranon dislocation of the elbow in a child: A case report and review of literature. World J Orthop 2018; 9(7): 100-104
- URL: https://www.wjgnet.com/2218-5836/full/v9/i7/100.htm
- DOI: https://dx.doi.org/10.5312/wjo.v9.i7.100
Although anterior transolecranon dislocation of the elbow is not uncommon in adults, it is rarely seen in children[1]. Limited published recommendations for the management of these lesions in children are available. Closed reduction is possible in most elbow dislocations. We report a rare case of irreducible anterior transolecranon fracture dislocation of the left elbow joint in a 7-year-old child who was surgically treated.
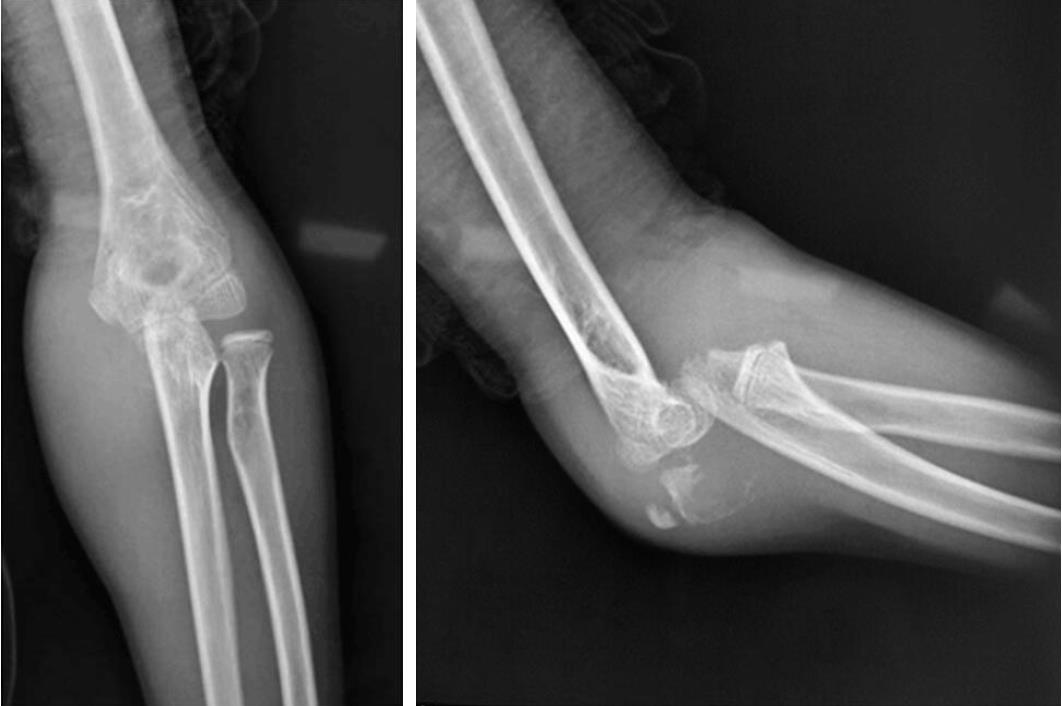
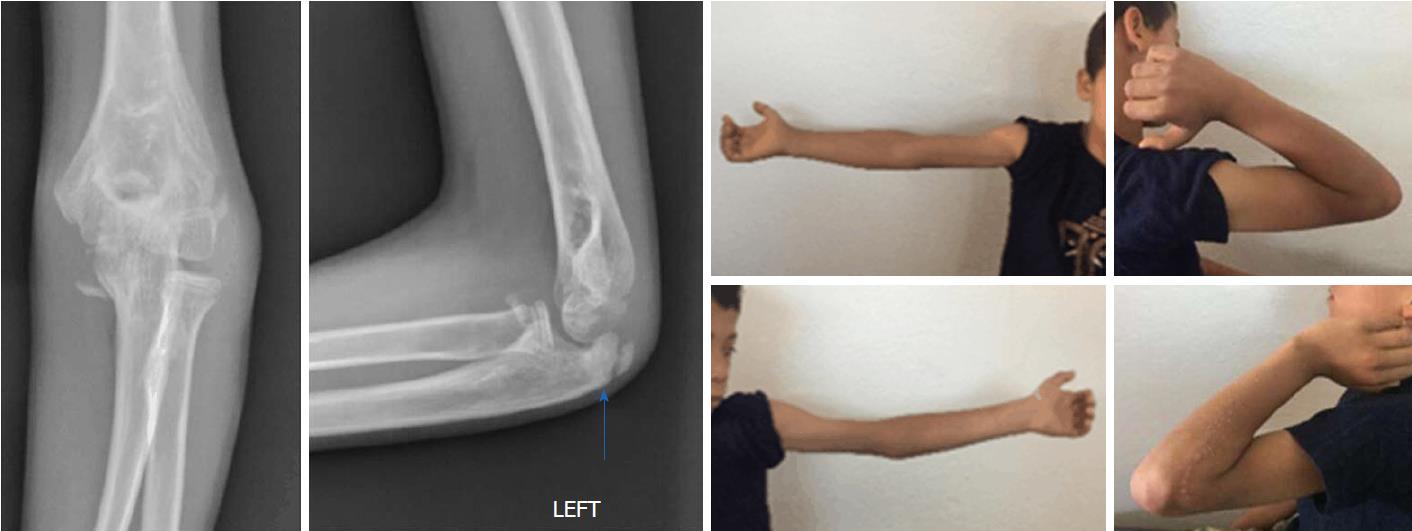
A 7-year-old boy was admitted to the emergency department of the Habib Bourguiba University Hospital, Tunisia, for direct left elbow trauma sustained in a fall 2 h earlier while playing with his friends on the street. The patient presented with severe pain, swelling, and deformity of the elbow, with functional disability of the left upper limb. The neurovascular status of the limb was intact, range of motion was restricted by pain, and the fingers were mobile and sensitive. In addition, the radial pulse was palpable and equal to that of the contralateral side. X-rays of the elbow revealed anterior and lateral transolecranon dislocation (Figure 1). The child was transferred to the operating room and placed in the decubitus position, with his arm on a hand table. Closed reduction was attempted twice under general anesthesia and using an X-ray image intensifier. Maneuver was conducted as recommended in a previous report by Winslow[2]; however, both attempts were unsuccessful. Therefore, the patient was surgically treated.
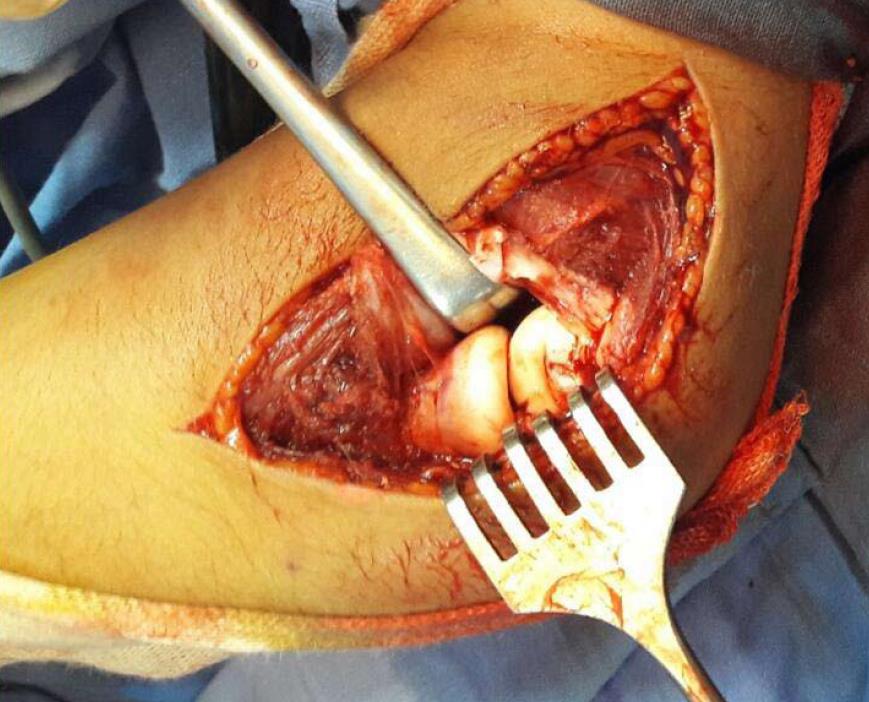
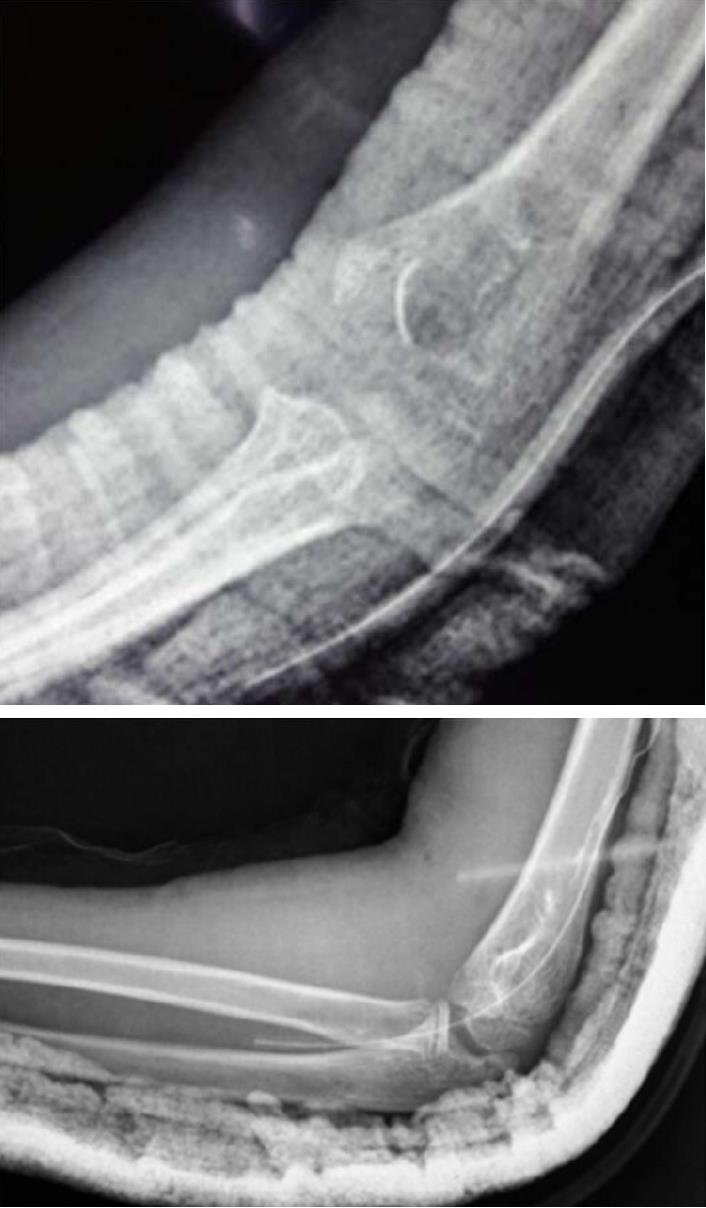
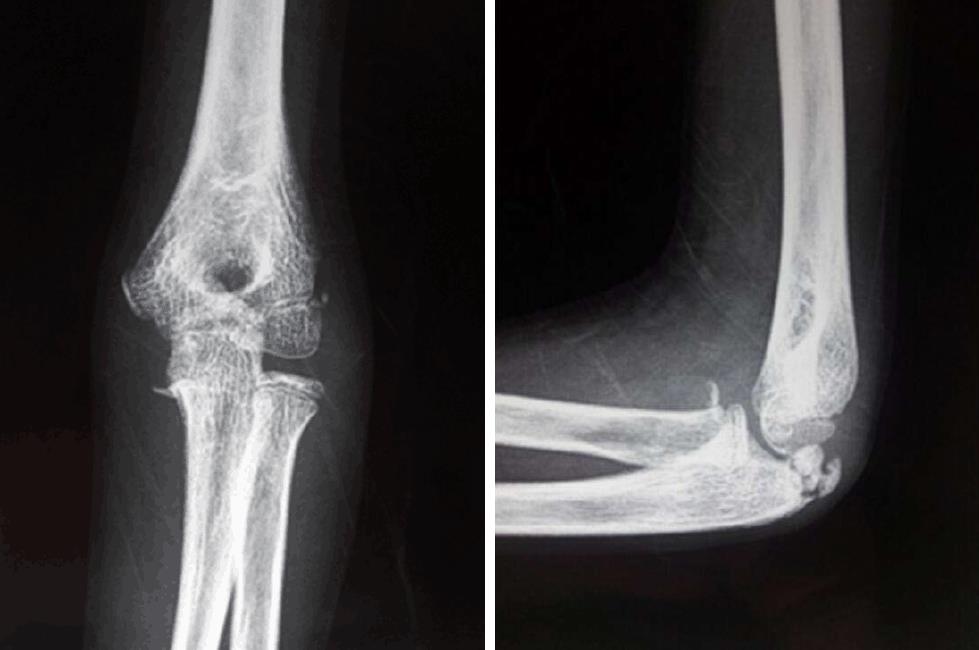
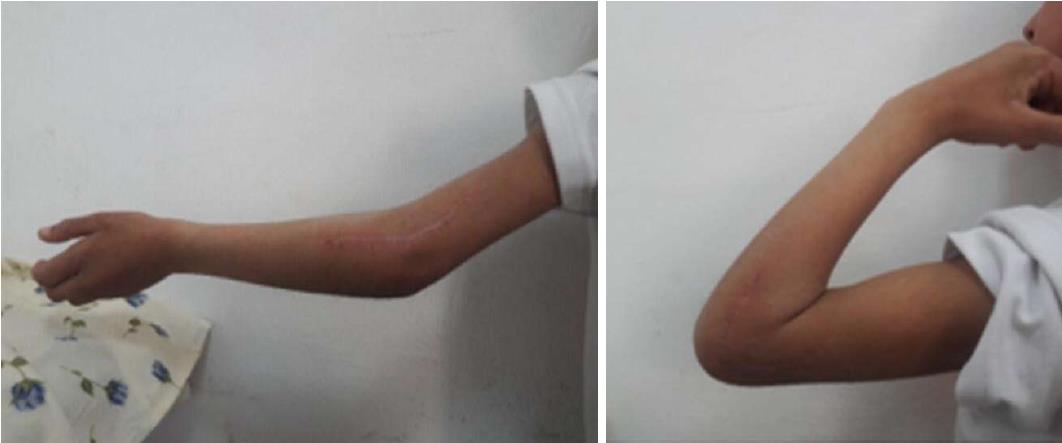
A lateral approach to expose the elbow joint found that the olecranon and radial head were anteriorly dislocated, and the annular ligament was torn. The closed reduction attempts failed because the radial head was buttonholed through the torn anterior capsule of the elbow joint. Subsequently, the radial head was released, and the joint was reduced under direct vision (Figure 2). Reduction was perfect, as verified by an X-ray image intensifier. Because the joint was found to be stable following reduction, internal fixation of the olecranon fracture was not performed. Using a splint, the reduced joint was externally immobilized for four weeks (Figure 3). Recovery was uncomplicated. Eventually, the patient was discharged after wound inspection on the third postoperative day. The splint was removed a month later, with the initiation of healing of the olecranon revealed on X-ray by incomplete densification of the fracture (Figure 4). Although the patient had complete flexion of the elbow joint, extension was incomplete (Figure 5). He was referred for rehabilitation and assisted active range of motion exercises. After three months, the patient recovered good range of motion. He showed only 10° of sequellar extension lag, complete range of pronation, and supination movements, and was able to perform all daily activities. His quickDASH score was 4.54. Plain radiographs indicated healing of the olecranon fracture (Figure 6).
By far, posterior elbow dislocations are the most common dislocations among children, and these are an effect of indirect forces transmitted to the elbow following a fall on the outstretched hand[3,4]. Till date, a few number of anterior transolecranon dislocations of the elbow has been reported[5].
Anterior dislocations of the elbow among children were often associated with fractures around the elbow, and some cases included neurovascular injury[6,7]. Closed reduction has commonly been performed, except in cases involving soft-tissue interposition or buttonholing of the radial head through the capsule that have prevented it[8,9]. Closed reduction was attempted in this case, but it failed because of buttonholing of the radial head through the capsule of the joint, which was discovered during surgery, along with a torn annular ligament. Similar cases of close reduction failure because of buttonholing of the anterior capsule have been reported in Japan by Takase et al[8] and in the United States by Aversano et al[10]. The anatomic pathology of anterior transolecranon fracture dislocation described by Tiemdjo et al[11] and as shown in Table 1, includes 4 types, each with a proposed treatment. This classification has prognostic and therapeutic values.
| Classification | Description | Treatment |
| Type 1 | Epiphyseal splinting or proximal fracture of the olecranon If the periosteum is intact | Reduction + Tension-band Wiring Reduction + Plaster |
| Type 2 | Transverse fracture | Reduction + Tension-band Wiring |
| Type 3 | Oblique fracture | Reduction + Screwed plate |
| Type 4 | Olecranon fracture + associated injury (radius, humerus) | Reduction + Osteosynthesis of the olecranon fracture and the associated injury |
No clear conclusions regarding the surgical approach and technique to reduce and stabilize the dislocated elbow joint can be drawn from the available published reports. We selected the lateral approach for better visualization of the articular surface of the joint and chiefly for direct control of the radial head. Reduction of the dislocated joint was easy to perform following the release of the buttonholed radial head. In most reports, surgical reduction was followed by osteosynthesis of the olecranon. We selected simple immobilization of the elbow until consolidation because stable reduction of the olecranon was achieved. Contrary to what was recommended Tiemdjo et al[11], we did not perform osteosynthesis to limit damages of the growth plate and avoid clutter by the material, which may probably perturb the range of motion later. In addition, no other further intervention was required to remove the osteosynthesis material. Postoperative stability was maintained by a splint with a 75°-80° flexed elbow to obtain less tension of the olecranon. The result was considered good, despite the sequellar mild flexion deformity. An enhanced reduction is associated with better result. Osteosynthesis of the olecranon could improve results only if a perfect reduction was achieved. The reduction in this patient was good and stable. Therefore, immobilization did not allow immediate rehabilitation. This explains the mild flexion deformity at the last follow-up. Accordingly, accelerated functional treatment and rehabilitation following surgery are recommended, as long periods of immobilization are not beneficial[12]. In this patient, splint removal after only four weeks following the surgery allowed relatively early mobilization.
In conclusion, this uncommon case of anterior transolecranon dislocation could not be successfully managed using simple closed reduction. Open reduction without osteosynthesis of the olecranon had an excellent result at the last follow-up. This indicates that perfect reduction must be the main goal of any approach and that osteosynthesis is not the only way to recover anterior function of the elbow.
Anterior transolecranon dislocation of the elbow is rarely observed in children and is reported in only a small series of cases. This case report aimed to highlight that osteosynthesis is not essential in such an uncommon injury.
Anterior transolecranon dislocation.
Simple elbow dislocation.
Plain radiographs revealed anterior dislocated elbow with olecranon fracture.
Open reduction without osteosynthesis.
Only few cases of anterior transolecranon dislocation in children have been reported in the literature. We think that our case may be the first one reported in the African continent.
This case will contribute to improvements in our understanding of the management of anterior transolecranon dislocation in children. The main lesson learned was that osteosynthesis is not essential for the management of such fractures.
We thank the boy’s parents for allowing us to share his details and thank Dr. Wajdi Bouaziz for advice and for performing the surgery.
CARE Checklist (2013) statement: The authors have read the CARE Checklist (2013), and the manuscript was prepared and revised according to the CARE Checklist (2013).
Manuscript source: Unsolicited manuscript
Specialty type: Orthopedics
Country of origin: Tunisia
Peer-review report classification
Grade A (Excellent): 0
Grade B (Very good): 0
Grade C (Good): C
Grade D (Fair): D
Grade E (Poor): 0
P- Reviewer: Canavese F, Massoud EIE S- Editor: Ji FF L- Editor: A E- Editor: Tan WW
| 1. | Guitton TG, Albers RG, Ring D. Anterior olecranon fracture-dislocations of the elbow in children. A report of four cases. J Bone Joint Surg Am. 2009;91:1487-1490. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 19] [Cited by in F6Publishing: 19] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 2. | Winslow R. A case of complete anterior dislocation of both bones of the forearm at the elbow. Surg Gynecol Obstet. 1913;16:570-571. [Cited in This Article: ] |
| 3. | Altuntas AO, Balakumar J, Howells RJ, Graham HK. Posterior divergent dislocation of the elbow in children and adolescents: a report of three cases and review of the literature. J Pediatr Orthop. 2005;25:317-321. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 33] [Cited by in F6Publishing: 34] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 4. | Kaziz H, Naouar N, Osman W, Ayeche M. Outcomes of Paediatric Elbow Dislocations. Malays Orthop J. 2016;10:44-49. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 12] [Cited by in F6Publishing: 12] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 5. | Ring D, Jupiter JB, Sanders RW, Mast J, Simpson NS. Transolecranon fracture-dislocation of the elbow. J Orthop Trauma. 1997;11:545-550. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 161] [Cited by in F6Publishing: 161] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 6. | Lasanianos N, Garnavos C. An unusual case of elbow dislocation. Orthopedics. 2008;31:806. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 6] [Cited by in F6Publishing: 6] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 7. | Fadili M, Wichou M, Haddoun AR, Harfaoui A, Dkhissi M, Zryouil B. [Anterior luxation of the elbow. A case report]. Tunis Med. 2001;79:251-252. [PubMed] [Cited in This Article: ] |
| 8. | Takase K, Mizuochi J. Irreducible dislocation of the radial head with undisplaced olecranon fracture in a child: a case report. J Pediatr Orthop B. 2011;20:345-348. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 12] [Cited by in F6Publishing: 12] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 9. | Takami H, Takahashi S, Ando M. Irreducible isolated dislocation of the radial head. Clin Orthop Relat Res. 1997;345:168-170. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 15] [Cited by in F6Publishing: 15] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 10. | Aversano F, Kepler CK, Blanco JS, Green DW. Rare cause of block to reduction after radial head dislocation in children. J Orthop Trauma. 2011;25:e38-e41. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 11] [Cited by in F6Publishing: 11] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 11. | Tiemdjo H, Kinkpe C, Coulibaly NF, Sane A, Ndiaye A, Seye SI. [Anterior transolecranon fracture-dislocations of the elbow in children: A case report and review of the literature]. Arch Pediatr. 2015;22:737-740. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 9] [Cited by in F6Publishing: 10] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 12. | Riel KA, Bernett P. [Simple elbow dislocation. Comparison of long-term results after immobilization and functional treatment]. Unfallchirurg. 1993;96:529-533. [PubMed] [Cited in This Article: ] |