Published online Dec 18, 2018. doi: 10.5312/wjo.v9.i12.300
Peer-review started: October 2, 2018
First decision: November 16, 2018
Revised: November 22, 2018
Accepted: December 13, 2018
Article in press: December 13, 2018
Published online: December 18, 2018
Processing time: 78 Days and 0.4 Hours
Metallosis describes the build-up of metal debris in the soft tissues after a period of metal on metal articulation. This debris can be asymptomatic or lead to catastrophic implant failure, which can present acutely, as in this case, or over a period of time. This report highlights how a metal clip used to hold the polyethylene liner to the tibial base plate broke 5 years after implantation, dislodged from its original position and went on to cause post-operative knee metallosis.
We present a case of a 63 year old lady admitted to our unit with an acute onset of right knee pain on top of a previous right total knee replacement. There was no associated trauma and examination revealed an erythematous, swollen and tender right knee. Blood investigations went on to display significantly raised inflammatory markers, raising the suspicion of a septic joint. This patient was taken to theatre for a knee arthrotomy and lavage of what was thought to be a septic joint when she was found to have extensive knee metallosis. On further inspection the metal clip, normally used to secure the polyethylene insert to the tibial base plate, had broken, dislodged, and had triggered this response. After the initial washout, this lady went back to theatre, once the appropriate implants were in stock, for an exchange of liner and metal clip.
This case highlights this very rare complication which has never been reported in the literature and the success of this patient’s management.
Core tip: Metallosis describes the build-up of metal debris in the soft tissues after a period of metal on metal articulation. This can present acutely, as in this case, or gradually. This case report highlights how a metal clip used to hold the polyethylene liner to the tibial base plate broke 5 years after implantation, dislodged from its original position and went on to cause post-operative knee metallosis. The success to this patient’s management came from thorough debridement, and replacement of the components involved.
- Citation: Saad AI, Shahban SA, Fernandes R. Metallosis following a clip breakage in a total knee arthroplasty implant: A case report. World J Orthop 2018; 9(12): 300-303
- URL: https://www.wjgnet.com/2218-5836/full/v9/i12/300.htm
- DOI: https://dx.doi.org/10.5312/wjo.v9.i12.300
Metallosis is a rare condition that has been recognised to affect both knee and hip arthroplasties. The most common cause leading to this malady is abrasive wear of the polyethylene component, inadvertently allowing two or more of the metal components to come into contact. This subsequently leads to a serious and debilitating synovial reaction.
Though the majority of cases documented in the literature of metallosis involve the wear of the polyethylene component; we present a rare and interesting case of metallosis in the knee following breakage of the metal clip used to hold the polyethylene insert of a Vanguard® implant in place. This consequently allowed the femoral and tibial components to come into contact leading to the acute metal induced synovitis.
A 63 years old lady had a right total knee replacement (TKR) in 2013 using the Vanguard® knee system - Biomet implant. She was admitted into hospital in March 2018 - approximately five years following her initial TKR. She presented with an insidious and acute onset of worsening right knee pain and swelling, not associated with any trauma. The pain was affecting her mobility, limiting her ability to weight bear on that joint.
On clinical assessment, she had an erythematous and fluctuant right knee with a moderate joint effusion. Along with this, she had a tender joint line with a limited range of movement. There was no evidence of wound breakdown, equally in 2013 following her primary procedure, she had an uncomplicated recovery period. She had a core body temperature of 37.3 °C, with no accompanying fevers or rigors, and the rest of her physiological markers were unremarkable.
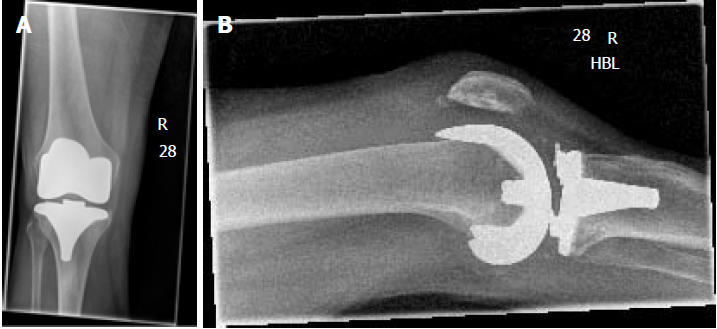
Her initial blood investigations revealed significantly raised inflammatory markers with a white cell count (WCC) of 20.27 × 109/L, neutrophils of 16.68 × 109/L and C - reactive protein (CRP) of 186 mg/L, suggesting an acute infection. Radiographs of the knee showed a relatively well positioned in-situ TKR, with no evidence of loosening, with the possibility of a joint effusion (Figure 1A and B).
Given this patients history, examination and biochemical findings, a right knee septic arthritis could not be excluded, and as such she was taken to theatre for a knee arthrotomy with a view to debride the joint, and potentially replacement of the polyethylene liner.
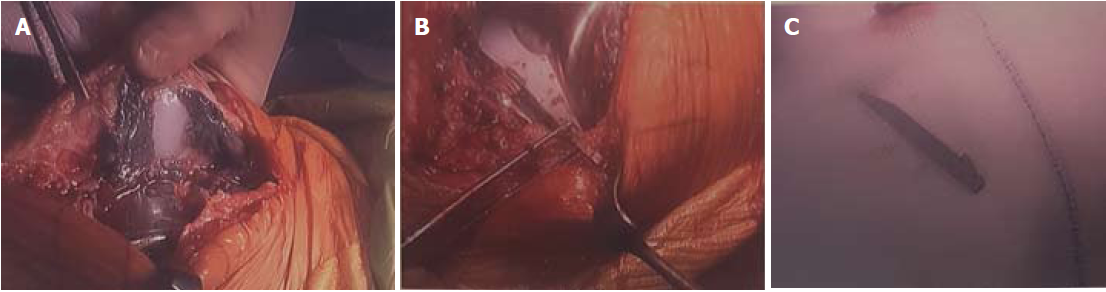
After the initial arthrotomy was made, significant purulent, dark coloured fluid extruded from the joint. The knee joint was formally opened and at this point no pus was seen, however there was a significant amount of metallosis debris deeply embedded into the soft tissues surrounding the knee prostheses (Figure 2A). On further inspection, it was clear that the metal clip which is normally used to secure the polyethylene insert to the tibial base plate had broken and dislodged (Figures 2B and C). Despite this broken metal clip, the polyethylene liner was still in its original position, and on further examination the femoral, tibial and patella implants were all well fixed with no evidence of loosening. There was also no evidence of significant macroscopic wear of the femoral and tibial components.
The broken metal clip was retrieved successfully and in whole (part being dislodged and part being well fixed in the polyethylene liner). The Vanguard® TKR system is no longer used in our trust, and consequently we were unable to replace the liner and metal clip. This lady therefore went on to have a thorough soft tissue debridement of her metallosis and lavage with copious normal saline solution. She later had a second staged procedure (after a total of 18 d) at which point we were able to obtain the correct implants, and thus provide her with a new polyethylene liner and metal clip to secure it in place. In the interim, between stages, she was prescribed a course of two grams of intravenous flucloxacillin antibiotics (to complete a six week course) and was restricted with her weight bearing, to prevent polyethylene liner displacement.
Superficial and deep tissue samples from the time of her 1st procedure did not grow any organisms. The histology report demonstrated areas of black necrosis with reactive fibrosis, a giant cell foreign body reaction triggered by black, irregular metallic particles, confirming the diagnosis of metallosis.
Post-operatively, the patient’s inflammatory markers started to improve with a fall in the CRP to 52 mg/L and WCC of 12 × 109. There was also marked improvement in her symptoms, pain and range of movement of the knee. She was later discharged whilst being able to fully weight bear and with a much improved knee. At the six week stage, in the outpatient clinic, she had complete resolution of her symptoms and was happily discharged from clinic.
Metallosis is an uncommon synovial reaction that can lead to serious complications and almost always requires revision surgery. It is therefore critical to understand the causes that lead to this condition. Avoidance of this essentially comes down to trying to ensure that the individual metal components of any part of the prosthetic joint are not allowed to come into contact and abrade against each other. Most case reports in the literature document the development of metallosis following significant wear of the interposed polyethylene component[1]. In this report we found no significant wear of the polyethylene insert, but rather, ensuing metallosis which was allowed to occur due a metal clip which had broken and dislodged, allowing for metal-on-metal (MOM) abrasion of the components.
As the inflammation progresses, often over a prolonged period of time, patients with knee metallosis usually present with gradual worsening knee pain and, occasionally, a noticeable rash (indicating necrosis). Prosthetic dislocation is often a late sign and demonstrates significant polyethylene wear[2]. This almost always goes on to require revision surgical intervention.
Different companies have different ways in which one can secure the polyethylene liner to the tibial base plate. In the case of the Vanguard® TKR system, one is required to slide the metal clip through both the liner and tibial component, thus allowing for a secure hold of the two. Clip breakage is not a recognised complication of TKR, and very rarely occurs. One would expect that when the clip breaks, this disrupts the position of the polyethylene component, which would ultimately lead to displacement or even dislocation of the knee joint. In our case, though we found the insert to be stable, we concluded that the broken and loose part of metal clip was abrading the metal back components of the joint, and thus triggering the metallosis inflammatory reaction.
When there is a suspicion of post-operative knee metallosis, imaging may help in coming to this diagnosis. Described in the literature are the metal-line sign and the cloud sign which occasionally can be seen on plain radiographs[2,3].
With regards to the pre-operative radiographic images (Figures 1A and B) it was not immediately recognised that the clip had broken and moved out of position. In retrospect, there is a suspicion that the broken metal clip is visible in the initial set of radiographs. Whether or not pre-operative recognition would have aided in planning is debatable, as the decision to debride the joint was made on clinical grounds of a possible diagnosis of septic arthritis. Liner exchange could not be carried out at the first instance due to non-availability of the insert and clip as these components were no longer used by the trust - something which, with more detailed pre-operative imaging, potentially could have been planned for and potentially could have allowed her to have a single staged procedure.
Metallosis is most commonly caused by wear of the polyethylene insert, leading to a chronic inflammatory process with signs that may or may not be easily identifiable on plain radiographs. Septic arthritis is potentially fatal and thus requires a thorough work up. Once septic arthritis is excluded, early diagnosis of metallosis is key and often requires revision surgery in terms of debridement with or without implant exchange. We present a rare case of metallosis from what was thought to be a robust mechanism of polyethylene liner stabilisation. We urge all clinicians to bear this in mind when dealing with prostheses which have the potential to allow any form of MOM interaction(s).
Manuscript source: Unsolicited manuscript
Specialty type: Orthopedics
Country of origin: United Kingdom
Peer-review report classification
Grade A (Excellent): 0
Grade B (Very good): 0
Grade C (Good): C, C
Grade D (Fair): 0
Grade E (Poor): 0
P- Reviewer: Drosos GI, Erkan S S- Editor: Ma YJ L- Editor: A E- Editor: Bian YN
| 1. | Argenson JN, Parratte S. The unicompartmental knee: design and technical considerations in minimizing wear. Clin Orthop Relat Res. 2006;452:137-142. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 67] [Cited by in F6Publishing: 61] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 2. | Romesburg JW, Wasserman PL, Schoppe CH. Metallosis and Metal-Induced Synovitis Following Total Knee Arthroplasty: Review of Radiographic and CT Findings. J Radiol Case Rep. 2010;4:7-17. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 17] [Cited by in F6Publishing: 21] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 3. | Paydar A, Chew FS, Manner PA. Severe Periprosthetic Metallosis and Polyethylene Liner Failure Complicating Total Hip Replacement: The Cloud Sign. Radiol Case Rep. 2015;2:115. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 12] [Cited by in F6Publishing: 16] [Article Influence: 1.8] [Reference Citation Analysis (0)] |