Published online Dec 18, 2015. doi: 10.5312/wjo.v6.i11.867
Peer-review started: May 30, 2015
First decision: August 4, 2015
Revised: September 11, 2015
Accepted: October 12, 2015
Article in press: October 13, 2015
Published online: December 18, 2015
Processing time: 203 Days and 23.5 Hours
Coronal shear fractures of distal humerus involving the capitellum and the trochlea are rare injuries with articular complexity, and are technically challenging for management. With better understanding of the anatomy and imaging advancements, the complex nature of these fractures is well appreciated now. These fractures involve metaphysealcomminution of lateral column and associated intraarticular injuries are common. Previously, closed reduction and excision were the accepted treatment but now preference is for open reduction and internal fixation with an aim to provide stable and congruent joint with early range of motion of joint. Various approaches including extensile lateral, anterolateral and posterior approaches have been described depending on the fracture pattern and complexity. Good to excellent outcome have been reported with internal fixations and poor results are noted in articular comminution with associated articular injuries. Various implants including headleass compression screws, minifragment screws, bioabsorbable implants and column plating are advocated for reconstruction of these complex fractures. Inspite of articular fragments being free of soft tissue attachments the rate of osteonecrosis and osteoarthritis is reported very less after internal fixation. This article summarizes the diagnostic and treatment strategies for these rare fractures and recommendations for management.
Core tip: Coronal shear fractures of the distal humerus are rare, complex fractures. The radiographic evaluation and better understanding by computed tomography helps in the management of these technically challenging fractures. Open reduction and internal fixation by various approaches and implants is advocated. We aim to review the existing diagnostic and treatment protocols with our recommendations for management.
- Citation: Singh AP, Singh AP. Coronal shear fractures of distal humerus: Diagnostic and treatment protocols. World J Orthop 2015; 6(11): 867-876
- URL: https://www.wjgnet.com/2218-5836/full/v6/i11/867.htm
- DOI: https://dx.doi.org/10.5312/wjo.v6.i11.867
Coronal shear fractures of the distal humerus involving capitellum and trochlea account for less than 1% of elbow fractures[1,2]. These injuries result from axial loading of the capitello-trochlear area by the forces transmitted through the radial head and could be associated with more complex distal humeral fractures and dislocation with concomitant ligamentous injuries[1,3]. The complexity of these fractures in recent times has been better appreciated by digital imaging and computed tomographic scans[3-6]. Open reduction and internal fixation provides anatomical reduction, stability and early mobilisationand has become preferred treatment. Closed reduction, immobilisation and fragment excision are known to be associated with poor outcomes[7,8]. Failure of fixation or non-anatomic reduction leads to articular incongruity, posttraumatic arthrosis, stiffness and potential ulnohumeral instability[8-10]. The intraarticular and complex nature of these fractures makes optimal surgical exposure and implants debatable. The surgical approach and reconstruction of articular surfaces is technically challenging and several extensile approaches and fixation devices for reconstruction of articular surfaces are propagated in recent case series[3-5,8]. For articular surface reconstruction various implants including headless screws, miniscrews can be used. Despite several case series the management protocol is still not defined. In this article we review the existing literature regarding diagnostic advancements and treatment protocols for these complex fractures.
The capitellum is described as portion of spherical surface of distal humerus projecting anterior and inferior as a smooth, round hemispherical structure. Its articular surface does not extends posterior to the coronal plane of humerus[6]. The axis of flexion and extension of the elbow joint passes through the capitellum and range of flexion that develops from this centre is 0-140 degrees[11]. Intact radiocapitellar articulation is necessary for valgus and longitudinal stability of the elbow and forearm. Capitellar excision leads to coronal plane instability when medial structures are injured along with. Moreover ulnotrochlear disruption will lead to instability and arthritis over years. Valgus instability and painful distal radioulnar junction have been reported following excision[3].
The mechanism of injury in these fractures is fall on outstreched arm with complexity of fracture propotional to acting force. Often direct axial compression of radial head with capitellum is responsible for fracture pattern. Spontaneous reduction after elbow instability will also lead to injury pattern. The incidence is higher among women because of high rate of osteoporosis and carrying angle difference than men[5-7]. Usually the associated injuries are of lateral collateral ligament, trochlea, epicondyle, condylar and elbow dislocation[3-8]. Lateral collateral ligament injury is seen in 40% and radial head fracture is reported in 30% of the patients[2,8,9].
The most commonly used classification system is that of Bryan and Morrey with type IV fractures described by McKee et al[10] and Bryan et al[12]. In this system, type I fractures are complete capitellar fractures with little or no extension into the lateral trochlea, type II fractures are anterior osteochondral fractures with minimal subchondral bone; and type III fractures are comminuted or compression fractures of the capitellum. McKee et al[10] described type IV fractures in six patients with coronal shear fractures of capitellum that extended medially including most of the trochlea identified by the presence of the pathognomonic “double arc sign” on lateral radiographs.
As per Trauma Association (OTA)/AO classification system, capitellarfracturesare denoted 13B3-distal humerus, partial articular, and frontal plane- and are further subclassified as B3.1, indicating isolated capitellum fractures; B3.2, trochlea fractures; or B3.3, capitellum and trochlea fractures with a secondary fracture line in the sagittal plane. Capitellum and trochlea fractures may also be components of more complex, multifragmentaryintercondylar fractures (i.e., 13C3.3)[13].
Dubberley et al[8] recently proposed a treatment - and outcome-oriented classification of capitellum and trochlea fractures. Type I fractures involved the capitellum with or without the lateral trochlear ridge; type II injuries involved the capitellum and trochlea as a single piece and type III injuries consisted of fractures of both the capitellum and the trochlea as separate fragments. Each fracture type was additionally subclassified as A or B based on the presence of posterior condylar comminution, which was found to influence surgeon choice of fixation method and outcome.
Based on radiographs and intraoperative findings Ring et al[7] identified five articular segment injury patterns (types I to V) distal to the base of the olecranon fossa, representing progression of the severity of the articular injury beyond an isolated capitellum fracture. Most of the fractures required an extensile lateral approach to the elbow to reduce and reconstruct the articular surface with buried implants. An olecranon osteotomy was required when the articular fracture extended to the medial epicondyle (type V).
Careful history of injury mechanism should be done followed by evaluation of the elbow to identify open fractures and movement block. Elbow instability is best assessed under anaesthesia and is difficult in emergency due to pain and spasm. A thorough neurovascular and bony examination should be done. Clinically crepitus with elbow movements and painful limited range of motion or impingement is often present. Pain is mostly localized along lateral aspect of the elbow but can be diffuse due to ligamentous and associated injuries. Examination is often difficult due to pain and swelling. Associated injuries, wrist and shoulder joints, forearm compartments and secondary musculoskeletal survey are a must in these patients.
The anteroposterior view radiograph in most cases cannot show the fracture fragment and a lateral view is essential[1-3]. The oblique view also details more of the injury hence standard AP, lateral and radiocapitellar views should be done in every case.
On lateral view isolated capitellar fracture appears as half-moon shaped fragment lying free[12]. The capitello-trochlear fracture or type IV McKee[10] is typically described as double arc sign on lateral view but this sign is not pathognomonic of this type as it may not be present in all cases. A simple capitellar fracture on radiographs turns out to be a complex fracture intraoperatively with most of them having part of trochlea involved[1-4]. This sign thus may be misleading as isolated trochlea also present as half-moon or double arc sign[14]. In our previous series none of the six patients with type IV fractures show this sign. Three patients were associated with lateral condyle and in other three the fragment was internally rotated[15]. Imaging of the joints above and below the level of injuries will reveal bony injuries and soft tissues should be judged by clinical evaluation and magnetic resonance imaging. Plain radiographs have a 66% sensitivity and a negative predictive value of 63%-67% for fractures extending to trochlear region[1,2].
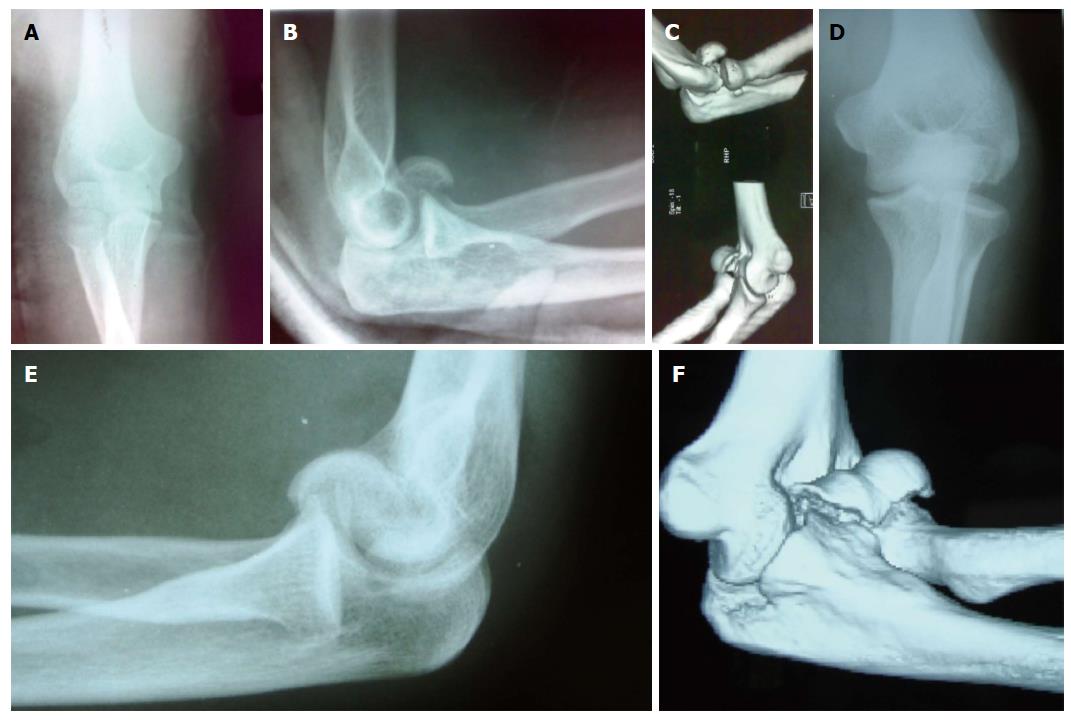
The inability to determine the extent, thickness and size of the fragment in standard radiographs has necessitated some authors to propose a two and three dimensional computed tomography (CT) scan in order to establish a better preoperative description of the injury and thorough analysis of anatomical features of the fracture[1-7]. This approach has a profound effect on implant choice and therapeutic strategy (Figure 1). Three-dimensional (3-D) scans are also useful when evaluating for concomitant injuries like transcondylar or intercondylar distal humerus fractures. On the CT scan, if the fracture extends into the medial epicondyle or if posterior involvement of the trochlea is indicated, the preferred surgical approach might be through an olecranon osteotomy[3,7]. Concomitant capitellar fractures and radial head fractures may be missed on plain radiographs, but diagnosed on CT scan[6]. Fractures of radial head, olecranon, lateral or medial epicondyle, lateral and medial columns, lateral collateral disruption and dislocation elbow are known concomitant injuries and should be taken into consideration.
Closed management has been reported in some series and is a reasonable option only if strict anatomic alignment can be obtained. Moreover reduction techniques are difficult in swollen elbows and later risk of displacement is there leading to complications[6]. Prolonged immobilization often leads to elbow stiffness. If comminution has occurred, the fracture fragments may act as loose bodies, and mechanically block elbow motion[2,3]. Intact radiocapitellar articulation is essential to both valgus and longitudinal stability of elbow and forearm. Capitellar excision creates instability in coronal plane when medial structures are disrupted. Poor clinical outcome were reported in more than 50% of patients at follow up after capitellar excision in various series[2,4]. Other complications are valgus instability and painful distal radioulnar joint. The non-operative treatment is reserved only for medically unfit patients.
In various series good to excellent outcomes have been reported with ORIF in majority of patients with these fractures. The superior results are attributed to anatomic reduction and stable fixation with early range of motion excercises[1,3,5-8,11,14,15].
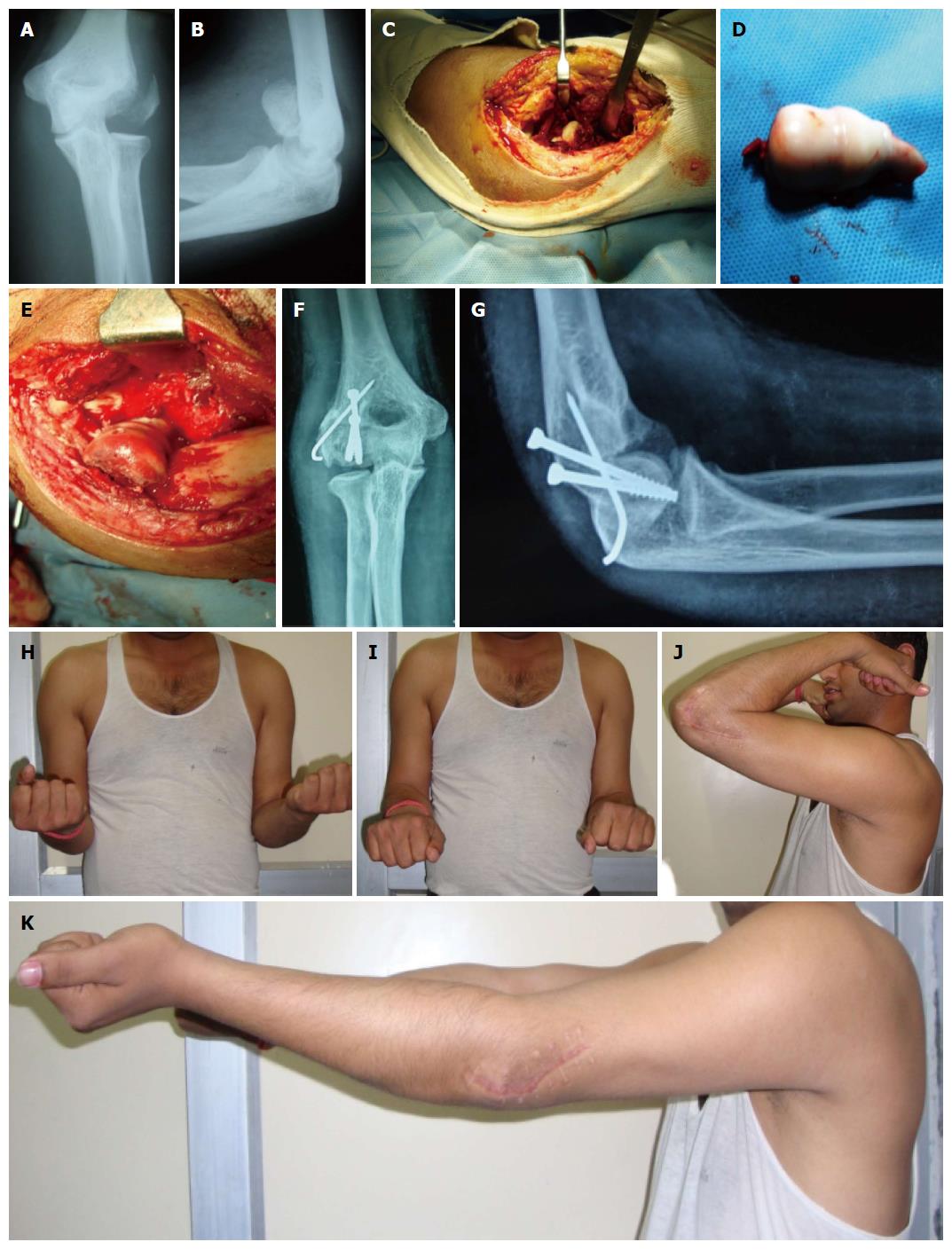
This is most commonly used approach for isolated capitellar and Type IV capitellum farctures[1,3,6,9,15,16]. Under regional/general anaesthesia the injured elbow is assessed clinically for ligamentous stability. It is done under tourniquet control. A skin incision is made centered over the lateral epicondyle extending from the anterior aspect of the lateral column of the distal end of the humerus to approximately 2 cm distal to the radial head (Figure 2). A continuous flap is raised by elevating the common extensor origin along with the anterior capsule and connected to the Kocher interval distally with forearm pronated. In patients with a lateral epicondylar fracture fragment, the epicondylar fragment with the lateral collateral ligamentous complex origin is reflected distally to enhance exposure. Fracture fragments are reduced and provisionally fixed with K-wires. The large articular fragments can be fixed by miniscrews on table. The proper position of the debrided fragment on the fracture bed should be located precisely by using K-wires as joy stick. The guide to correct positioning is the medial remaining trochlear fragment and trochlear ridge rather than lateral articular congruence. Two screws are used to fix the fracture and provide rotational control. Supplemental fixation with mini-fragment screws or Kirschner wires can be used to reconstruct complex fracture patterns. The radial wrist extensors are repaired to the soft-tissue cuff on the lateral supracondylar ridge, and the Kocher interval is closed in continuity with the proximal exposure. The remainder of the wound is closed in layers.
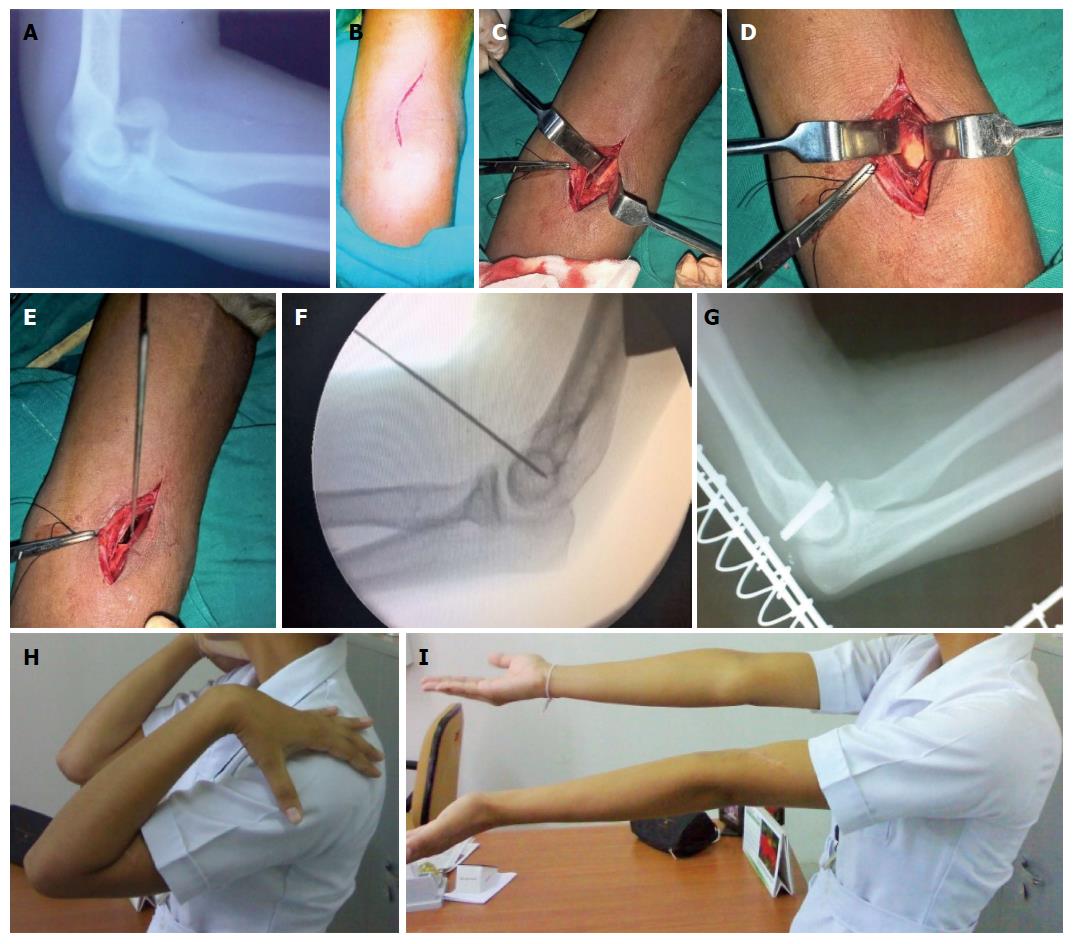
This approach has advantage that it approaches the capitellum and trochlea without disruption of LCL or an olecranon osteotomy[17,18]. The incision begins proximally overlying the lateral aspect of the biceps muscle. It is directed medially to cross the elbow joint obliquely and then directed back laterally over the proximal forearm (Figure 3). The surgical dissection continues between the biceps and brachioradialis origin. The lateral antebrachial nerve is protected. The radial nerve is identified on the deep surface of the brachioradialis and retracted laterally. The dissection continues distally to the biceps tendon. Brachialis is reflected medially off the distal humerus metaphysis and elevated distally to expose the capsule. The capsule is opened longitudinally directly over the displaced fracture fragment. The fragment is reduced under direct visualisation and provisionally K wire is fixed from anterior to posterior. Then wire can be exchanged for headless screws or bioabsorbable pin. The skin and subcutaneous tissue is closed with absorbable sutures and elbow is immobilized in back splint. We have found this approach suitable for capitellum fractures with excellent results.
When the medial extension of the fracture fragments is significant and there is significant posterior comminution the olecranon osteotomy approach provides better visualisation and fixation ease[7,8,19,20]. A posterior skin incision is used. Full thickness skin flaps are created medially and laterally. The ulnar nerve is mobilized and isolated. An apex distal chevron osteotomy is created at the midlevel of olecranon. The olecranon fragment and triceps are then reflected proximally. The fixation by this approach may utilise headless, cannulated screws in combination with reconstruction plates. The osteotomy may be repaired with tension band construct or cannulated screw system. In studies published till now the differences between the outcomes between extended lateral and the posterior midline approach are negligible[3,9,19,20].
There are very few reports on reduction and fixation by arthroscopic assisted methods and this is useful for excsion in very small fragments[21-23]. Moreover indications of fixation of complex fractures by this method are unclear and further studies are required to doucument any advantage over previous techniques.
Standard medial approach with medial epicondylectomy is performed[14]. The ulnarnerve is identified and secured. The trochlear fractureis exposed. The fragment is debrided of tissues and the fracture bed is prepared. Apposition is achieved and secured with a smooth K-wire. Two Headless screws can be used from anterior to posterior direction for definitive fixation. Articular congruency is restored and range of motion of the elbow is checked. Medial epicondyle is secured with mini screws and the wound is closed in layers.
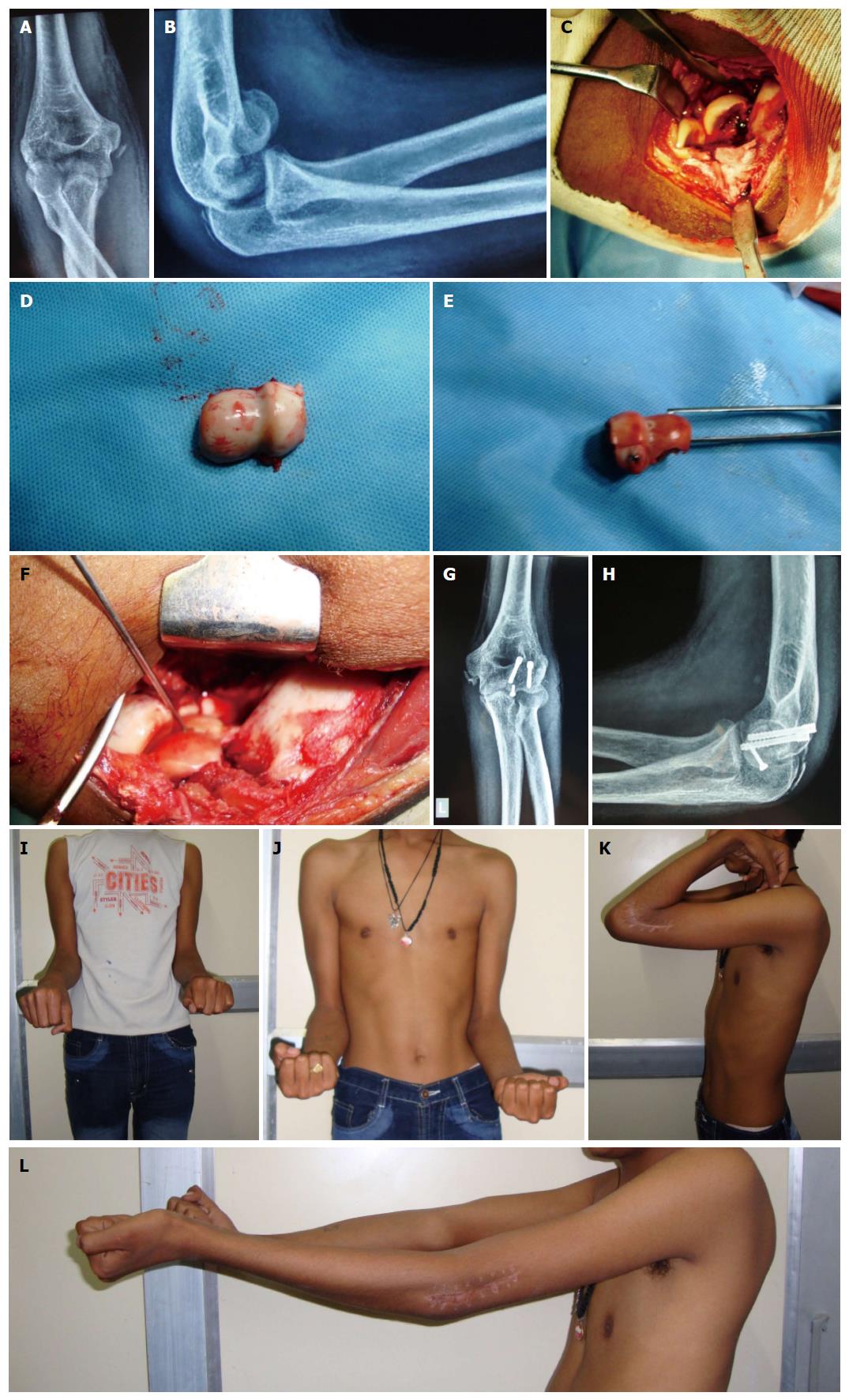
Supplemental bone graft may be required in impacted fragments after their elevation[24-26]. Small articular fragments not amenable to fixation by 3.5 mm screws should be fixed by 2.7 mm miniscrews and buried in subchondral bone[3,15,23] (Figure 4). The terminally threaded Herbert screws and fully threaded acutrack provide fracture site compression through variable thread pitch designs. Biomechanical data have demonstrated that acutrak screw fixation of capitellum fractures is superior to posteroanterior 4.0-mm cancellous lag screws and Herbert screws but in clinical series this has not been demonstrated[27,28]. Divergent fashion placement screws is recommended to ensure rotational control with sufficient spread of screws to avoid iatrogenic fracture of the capitellum[29,30]. Supplemental fixation is often required to reconstruct more complex fracture patterns with posteroinferior/lateral metaphyseal comminution and/or trochlear extension. Supplemental fixation options include minifragment screws, threaded K-wires, and bioabsorbable pins. When extensive posterolateral comminution is present, plating of the lateral column with pelvic reconstruction, precontoured, or locking plates may be required to buttress the lateral column[31]. Lateral collateral ligament may be repaired primarily to its origin using transosseous sutures passed through drill holes or suture anchors or using figure-of-8 tension-band wire technique in cases of avulsion or fractured parts[3]. Medial collateral ligament disruption may require primary repair or a hinge orthosis. Incomplex fractures with comminution authors had similar results in terms of complications, the need for removal of hardware, and poorer results occurred in the type 3 fractures[8,11]. This probably reflects difficulty in reconstructing small fragments using the devices available at present. The on table reconstruction of radial head fractures and capitellar fractures had been reported with excellent results[15,32]. Further development of devices that allow reconstruction of this specifically shaped articulation may improve the outcome further in the future.
The splint is removed in approximately 1 wk, and the patient is encouraged to do gentle active range of motion exercises. When extensive intra-articular comminution has occurred, the elbow may need to be immobilized for a longer period of time. Passive range of motion and strengthening is not started until bony healing is evident, at about 6 to 8 wk postoperatively. We advocate use of oral indomethacin (25 mg, three times daily), for 4 wk to minimize the possibility of heterotopic ossification in cases with elbow dislocation. With medial collateral ligament/associated injuries, the limb is placed into a functional brace. In the presence of concomitant ligamentous or functionally equivalent osseous injuries, a ligament-specific protocol is instituted, with mobilization in pronation (lateral-sided injury) or supination (medial-sided injury). Strengthening exercises are initiated on clinical and radiographic evidence of fracture union.
A number of series have reported on patient outcomes following ORIF of capitellum and trochlea fratures[2,8,9,11,15]. Only a few have attempted to correlate clinical and functional outcome with fracture subtype[3,8,11,15]. A functional arc of ulnohumeral motion is achieved in most of these patients despite a mean postoperative flexion contracture of 14.5° to 17.5°. In a cohort of 28 patients, Dubberley et al[8] reported significantly inferior functional elbow evaluation scores when there was medial trochlear extension and/or capitellum-trochlea comminution. Fracture subtypes differed significantly with respect to grip strength and flexion-extension power, but not with respect to elbow or forearm motion. In other series patients with type IV fractures patients had significantly reduced terminal flexion and net ulnohumeral arc and greater loss of terminal extension compared with patients with type I fractures[3]. Ashwood et al[11] validated the concept of posterior comminution and articular fragmentation as an important determinant of outcome after capitellar and trochlear fractures. The poorer results occurred in patients with severe injuries associated with posterior comminution of the humerus and who required more extensive reconstructive procedures[11]. The complications following surgical treatment include fixation failures, pain, instability, stiffness and neurologic complications. Hardware complications include impingement and subcutaneous positioning. Total elbow arthroplasty represent a salvage treatment for severe arthrosis, osteonecrosis, nonunion/malunion[33].
Coronal shear fractures involving the capitellum and trochlea are significant articular injuries and the changing trends in their management reflects better understanding of complex articular fracture pattern. The recommendations include use of CT, open reduction and internal fixation of all displaced fractures and selection of approach depending on fracture pattern. We recommend use of anterolateral approach for these fractures to prevent postoperative flexion contracture. With posterior comminution, olecranon osteotomy is the preferred approach. Early range of motion should be initiated following stable fixation. The implants of choice are headless cannulated screws and supplementation should be done by minifragment screws/pins/column plates. The counseling about postoperative flexion contracture and sequelae should be done in complex fracture patterns. The increased flexion contracture in these patients may be due to the increased severity of the injury and to the extended surgical dissection needed to facilitate exposure of the anterior articular segments. The severity of articular communition significantly reduces the functional outcome scores of elbow. Although earlier reports indicated no cases of osteonecrosis or collapse in the region of the fracture, these have been documented with longer follow-up. The on table reconstructions have been reported with success in these fractures and reconstruction should take precedence over excision to restore articular surfaces.
P- Reviewer: Cerchione C S- Editor: Ji FF L- Editor: A E- Editor: Jiao XK
| 1. | Yari SS, Bowers NL, Craig MA, Reichel LM. Management of distal humeral coronal shear fractures. World J Clin Cases. 2015;3:405-417. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 22] [Cited by in RCA: 20] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 2. | Lee JJ, Lawton JN. Coronal shear fractures of the distal humerus. J Hand Surg Am. 2012;37:2412-2417. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 25] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 3. | Ruchelsman DE, Tejwani NC, Kwon YW, Egol KA. Coronal plane partial articular fractures of the distal humerus: current concepts in management. J Am Acad Orthop Surg. 2008;16:716-728. [PubMed] |
| 4. | Watts AC, Morris A, Robinson CM. Fractures of the distal humeral articular surface. J Bone Joint Surg Br. 2007;89:510-515. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 50] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 5. | Guitton TG, Doornberg JN, Raaymakers EL, Ring D, Kloen P. Fractures of the capitellum and trochlea. J Bone Joint Surg Am. 2009;91:390-397. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 66] [Cited by in RCA: 55] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 7. | Ring D, Jupiter JB, Gulotta L. Articular fractures of the distal part of the humerus. J Bone Joint Surg Am. 2003;85-A:232-238. [PubMed] |
| 8. | Dubberley JH, Faber KJ, Macdermid JC, Patterson SD, King GJ. Outcome after open reduction and internal fixation of capitellar and trochlear fractures. J Bone Joint Surg Am. 2006;88:46-54. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 79] [Cited by in RCA: 106] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 9. | Mighell M, Virani NA, Shannon R, Echols EL, Badman BL, Keating CJ. Large coronal shear fractures of the capitellum and trochlea treated with headless compression screws. J Shoulder Elbow Surg. 2010;19:38-45. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 73] [Cited by in RCA: 72] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 10. | McKee MD, Jupiter JB, Bamberger HB. Coronal shear fractures of the distal end of the humerus. J Bone Joint Surg Am. 1996;78:49-54. [PubMed] |
| 11. | Ashwood N, Verma M, Hamlet M, Garlapati A, Fogg Q. Transarticular shear fractures of the distal humerus. J Shoulder Elbow Surg. 2010;19:46-52. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 52] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 12. | Bryan RS, Morrey BF. Fractures of the Distal Humerus. The Elbow and Its Disorders. 3rd ed. Philadelphia: WB Saunders 1985; 325-333. |
| 13. | Fracture and dislocation compendium. Orthopaedic Trauma Association Committee for Coding and Classification. J Orthop Trauma. 1996;10 Suppl 1:v-ix, 1-154. [PubMed] |
| 14. | Singh AP, Dhammi IK, Jain AK, Jain S. Neglected isolated fracture of the trochlea humeri. Chin J Traumatol. 2010;13:247-249. [PubMed] |
| 15. | Singh AP, Dhammi IK, Garg V, Singh AP. Outcome of surgical treatment of type IV capitellum fractures in adults. Chin J Traumatol. 2012;15:201-205. [PubMed] |
| 16. | Mehdian H, McKee MD. Fractures of capitellum and trochlea. Orthop Clin North Am. 2000;31:115-127. [PubMed] |
| 17. | Imatani J, Morito Y, Hashizume H, Inoue H. Internal fixation for coronal shear fracture of the distal end of the humerus by the anterolateral approach. J Shoulder Elbow Surg. 2001;10:554-556. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 48] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 18. | Malki AA, Salloom FM, Wong-Chung J, Ekri AI. Cannulated screw fixation of fractured capitellum: surgical technique through a limited approach. Injury. 2000;31:204-206. [PubMed] |
| 19. | Sano S, Rokkaku T, Saito S, Tokunaga S, Abe Y, Moriya H. Herbert screw fixation of capitellar fractures. J Shoulder Elbow Surg. 2005;14:307-311. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 61] [Cited by in RCA: 65] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 20. | Bilsel K, Atalar AC, Erdil M, Elmadag M, Sen C, Demirhan M. Coronal plane fractures of the distal humerus involving the capitellum and trochlea treated with open reduction internal fixation. Arch Orthop Trauma Surg. 2013;133:797-804. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 27] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 21. | Feldman MD. Arthroscopic excision of type II capitellar fractures. Arthroscopy. 1997;13:743-748. [PubMed] |
| 22. | Kuriyama K, Kawanishi Y, Yamamoto K. Arthroscopic-assisted reduction and percutaneous fixation for coronal shear fractures of the distal humerus: report of two cases. J Hand Surg Am. 2010;35:1506-1509. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 33] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 23. | Mitani M, Nabeshima Y, Ozaki A, Mori H, Issei N, Fujii H, Fujioka H, Doita M. Arthroscopic reduction and percutaneous cannulated screw fixation of a capitellar fracture of the humerus: a case report. J Shoulder Elbow Surg. 2009;18:e6-e9. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 26] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 24. | Singh AP, Singh AP, Vaishya R, Jain A, Gulati D. Fractures of capitellum: a review of 14 cases treated by open reduction and internal fixation with Herbert screws. Int Orthop. 2010;34:897-901. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 45] [Cited by in RCA: 53] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 25. | Giannicola G, Sacchetti FM, Greco A, Gregori G, Postacchini F. Open reduction and internal fixation combined with hinged elbow fixator in capitellum and trochlea fractures. Acta Orthop. 2010;81:228-233. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 30] [Cited by in RCA: 29] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 26. | Mighell MA, Harkins D, Klein D, Schneider S, Frankle M. Technique for internal fixation of capitellum and lateral trochlea fractures. J Orthop Trauma. 2006;20:699-704. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 41] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 27. | Elkowitz SJ, Polatsch DB, Egol KA, Kummer FJ, Koval KJ. Capitellum fractures: a biomechanical evaluation of three fixation methods. J Orthop Trauma. 2002;16:503-506. [PubMed] |
| 28. | Sen MK, Sama N, Helfet DL. Open reduction and internal fixation of coronal fractures of the capitellum. J Hand Surg Am. 2007;32:1462-1465. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 24] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 29. | Grantham SA, Norris TR, Bush DC. Isolated fracture of the humeral capitellum. Clin Orthop Relat Res. 1981;262-269. [PubMed] |
| 30. | Ring D. Open reduction and internal fixation of an apparent capitellar fracture using an extended lateral exposure. J Hand Surg Am. 2009;34:739-744. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 24] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 31. | Mahirogullari M, Kiral A, Solakoglu C, Pehlivan O, Akmaz I, Rodop O. Treatment of fractures of the humeral capitellum using herbert screws. J Hand Surg Br. 2006;31:320-325. [PubMed] |
| 32. | Businger A, Ruedi TP, Sommer C. On-table reconstruction of comminuted fractures of the radial head. Injury. 2010;41:583-588. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 34] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 33. | Brouwer KM, Jupiter JB, Ring D. Nonunion of operatively treated capitellum and trochlear fractures. J Hand Surg Am. 2011;36:804-807. [PubMed] |