Published online Mar 24, 2021. doi: 10.5306/wjco.v12.i3.144
Peer-review started: December 16, 2020
First decision: January 7, 2021
Revised: January 12, 2021
Accepted: February 12, 2021
Article in press: February 12, 2021
Published online: March 24, 2021
Processing time: 84 Days and 21.7 Hours
Although under-recognized, cancer survivors continue to be at an increased risk of death from cardiovascular complications post-remission or cure. This increased burden of cardiovascular disease results from the interplay of various factors. Adequate cardiovascular risk assessment and timely intervention through a multi-disciplinary approach in these patients plays a pivotal role in the prevention of cardiovascular morbidity and mortality. We discuss the shortcomings of using current risk prediction scores in cancer survivors and provide some insights into cardiovascular risk management relevant for primary care physicians, oncologists, and cardiologists alike.
Core Tip: Accurate assessment of cardiovascular risk in adult cancer survivors is important. Cancer survivors form a unique subset of a vulnerable population given their exposures to potential cardiotoxic therapies. The importance of common preventive cardiovascular strategies in the long-term outcomes of cancer survivors is understated in clinical practice.
- Citation: Mohammed T, Parekh T, Desai A. Cardiovascular risk management in cancer survivors: Are we doing it right? World J Clin Oncol 2021; 12(3): 144-149
- URL: https://www.wjgnet.com/2218-4333/full/v12/i3/144.htm
- DOI: https://dx.doi.org/10.5306/wjco.v12.i3.144
A 40-year-old African American female, with a past medical history of Hodgkin’s lymphoma, and hypertension, comes to your clinic for follow-up. At age 18, she was diagnosed with Hodgkin’s lymphoma and treated with doxorubicin, bleomycin, vincristine, etoposide, prednisone, and cyclophosphamide chemotherapy along with 24Gy radiation to the neck, mediastinum, and para-aortic nodes. Today, her blood pressure is well controlled with losartan. She has never smoked, does not have diabetes, and has a normal body mass index. Her last lipid profile revealed total cholesterol of 197 mg/dL, high-density lipoprotein cholesterol of 36 mg/dL, and low-density lipoprotein cholesterol of 156 mg/dL.
There are mainly two questions discussed here: How would you calculate her cardiovascular disease (CVD) risk? How can you reduce the risk of future cardiovascular events in her case?
According to the commonly used American Heart Association/American College of Cardiology (AHA/ACC) atherosclerotic cardiovascular disease (ASCVD) risk estimator, her 10-year risk of cardiovascular disease is 3.8%, putting her into the low-risk criteria[1]. However, this does not account for the increased risk of cardiovascular events from her exposure to potentially cardiotoxic chemotherapy and radiation, both known to increase cardiovascular (CV) morbidity and mortality in cancer survivors[2,3]. Here, we discuss the shortcomings of using ASCVD risk calculators in cancer survivors and provide some insights into cardiovascular risk management among cancer survivors relevant for primary care physicians, oncologists, and cardiologists alike.
As we know, advances in cancer medicine have resulted in long-term remission and even cure in some early-stage cancers. Although less recognized, cancer survivors continue to be at an increased risk of death from cardiovascular complications post-remission or cure[4]. Interestingly, cardiovascular disease is now one of the leading causes of death among long-term breast cancer survivors[5]. This increased burden of the cardiovascular disease results from the interplay of various factors such as chemotherapy (type, formulation, or cumulative dosage), exposure to radiation therapy or indirect factors (stress, deconditioning from cancer), or other pre-existing patient-related risk factors (increased age, obesity, hypertension, and diabetes). Also, demographic and socioeconomic disparities in cancer survivors could have an additive effect on outcomes[6]. Thus, adequate cardiovascular risk assessment and timely intervention through a multi-disciplinary approach in these patients play a pivotal role in the prevention of cardiovascular morbidity and mortality in this patient population.
For childhood cancer survivors, a risk prediction tool for heart failure, ischemic heart disease, and stroke (by age 50) currently exists[7]. The childhood cancer survivor study cardiovascular risk calculator includes parameters such as type and dose of chemotherapy, and dose and extent of radiation in addition to the conventional cardiovascular risk factors utilized by the ASCVD risk calculator (Table 1). Going back to our patient, the estimated probability of developing heart failure for her by 50 years of age is 13.7% (95%CI: 7.9%-19.5%) with a relative risk of 33 (95%CI: 18.0-60.7) for developing heart failure compared to a non-cancer sibling. This would put her at intermediate risk (7.5% to 19.9%) of future cardiovascular events. Thus, the ACC/AHA ASCVD risk calculator severely underestimates the risk of future cardiovascular events and its use is not sufficient in this special group of patients. A similar model was developed for predicting heart failure and cardiomyopathy in breast cancer patients, however, it was limited to trastuzumab exposure[8]. Currently, no validated risk prediction tools exist for accurate cardiovascular risk assessment in cancer survivors who have undergone cardiotoxic chemotherapy or radiation treatments for adult cancers. Thus, it is imperative for primary care providers to aggressively treat known risk factors in cancer survivors to reduce their cardiovascular disease burden.
| ASCVD risk calculator | CCSS cardiovascular risk calculator |
| Age | Age |
| Gender | Gender |
| Race | Age at diagnosis of cancer |
| Cholesterol-total cholesterol, HDL levels | Dyslipidemia medication use |
| Blood pressure-systolic, diastolic, medication use | Hypertension medication use |
| Diabetes | Diabetes Medication use |
| Smoking | Anthracycline chemotherapy exposure and dosage (if known) |
| Alkylating chemotherapy exposure | |
| Platinum agents chemotherapy exposure | |
| Radiation exposure to the brain, neck, and chest | |
| Chest radiation dose | |
| Heart-specific radiation dose |
Hypertension, hyperlipidemia, obesity, and diabetes are common comorbidities among cancer survivors, as with the general population[9]. Cancer therapeutics related cardiac dysfunction (CTRCD) [defined as a decline in ejection fraction (EF) from baseline > 10% to a value < 53%] is often diagnosed late as symptoms of heart failure appear. Anthracycline and trastuzumab are one of the most commonly used chemotherapeutic agents known to cause CTRCD. Anthracyclines lead to a dose-dependent irreversible structural damage to cardiomyocytes (Type I CTCRD) resulting in heart failure, whereas trastuzumab causes inhibition of signal transduction predominantly (reversible injury, type II) and has an additive effect to the cardiotoxicity from other modalities when used in a combinational anticancer treatment regimen[10]. Radiation-induced heart disease, from radiation treatment to prevent cancer recurrence is another cause for major cardiovascular events among long-term cancer survivors that need to be accounted for where assessing CVD risk among patients[11]. An area of active research is assessing the utility of various CV imaging techniques for the early detection of individuals at a higher risk of future CV events following cardiotoxic therapy. Myocardial strain assessment through echocardiography and cardiac magnetic resonance to detect myocardial fibrosis when other imaging techniques are nondiagnostic have been an important addition to the existing diagnostic tools to detect early myocardial injury and follow-up CTRCD[12]. However, early intervention and effective cardioprevention as guided by accurate risk assessment can delay the occurrence or possibly prevent CTRCD. Hence, aggressive risk factor reduction should be pursued in all cancer survivors as outlined below.
As we know, patients with uncontrolled hypertension are at an increased risk of heart failure[13]. Given the increased incidence of cardiotoxicity of numerous anticancer agents, cardio-oncology experts recommend a target BP below 140/90 mmHg in general and below 130/80 mmHg in patients who have diabetes mellitus or kidney disease for the maximal benefit[14]. However, this should change with the new AHA/ACC hypertension guidelines[15]. A meta-analysis evaluating the efficacy of neurohormonal blockade in preventing the decline of left ventricular EF after chemotherapy suggested that patients on beta-blockers and/or angiotensin-converting enzyme inhibitors or angiotensin receptor blockers had higher EF at 4 wk follow up compared to those on placebo with usual care[16]. Hence, these drug classes should be preferentially used as anti-hypertensives in patients with cancer for their added benefit in preventing cardiac dysfunction in cancer survivors.
Recent data suggest that diabetic risk reduction among cancer survivors was much lower compared to their non-cancer counterparts[17]. Uncontrolled diabetes, obesity, and hyperlipidemia have been shown to induce myocardial fibrosis which subsequently increases the incidence of symptomatic cancer treatment-related cardiotoxicity[18]. Hence, increased vigilance and multi-disciplinary collaborations between expert diabetic educator, a nutritionist and/or dietician, and primary care physicians are required for optimal diabetes management and maintaining the HbA1c goal of < 7% in most patients.
Up to 40% of cancer survivors develop obesity placing them at an increased risk of adverse cardiovascular outcomes and secondary cancers in the future. Growing evidence suggests the importance of adequate weight management in improving overall health and wellbeing especially cardiovascular health among survivors. In a study of breast cancer patients treated with anthracyclines and trastuzumab, obesity was found to be an independent risk factor associated with greater cardiotoxicity when compared to non-obese patients[19]. Given the high prevalence of obesity and associated inactivity in cancer survivors, energy balance interventions need to be incorporated in the treatment plan right from the time of the first diagnosis. A motivating diet plan- and exercise-induced weight management have led to clinically meaningful weight loss and subsequent control of risk factors related to cardiovascular health[20].
The role of nutrition and exercise is often underestimated despite robust evidence on its effects on cardiovascular morbidity and mortality among cancer survivors. It has been reported that adult survivors of pediatric cancers were found to have low cardio-respiratory reserve compared to age-matched healthy individuals[21]. Exercise training has been shown to significantly improve the decline in cardio-respiratory reserve after cancer therapy[22]. A large-scale study called TITAN is currently underway to evaluate the effect of a multidisciplinary approach to reduce the CTRCD. Exercise training is the cornerstone of the intervention arm in the study along with pharmacy, nutritional counseling, and cardiology team support[23]. A specific model for exercise and physical training for cancer patients and survivors, called cardio-oncology rehabilitation has also been proposed to effectively manage the CVD risk factors in this vulnerable population[24].
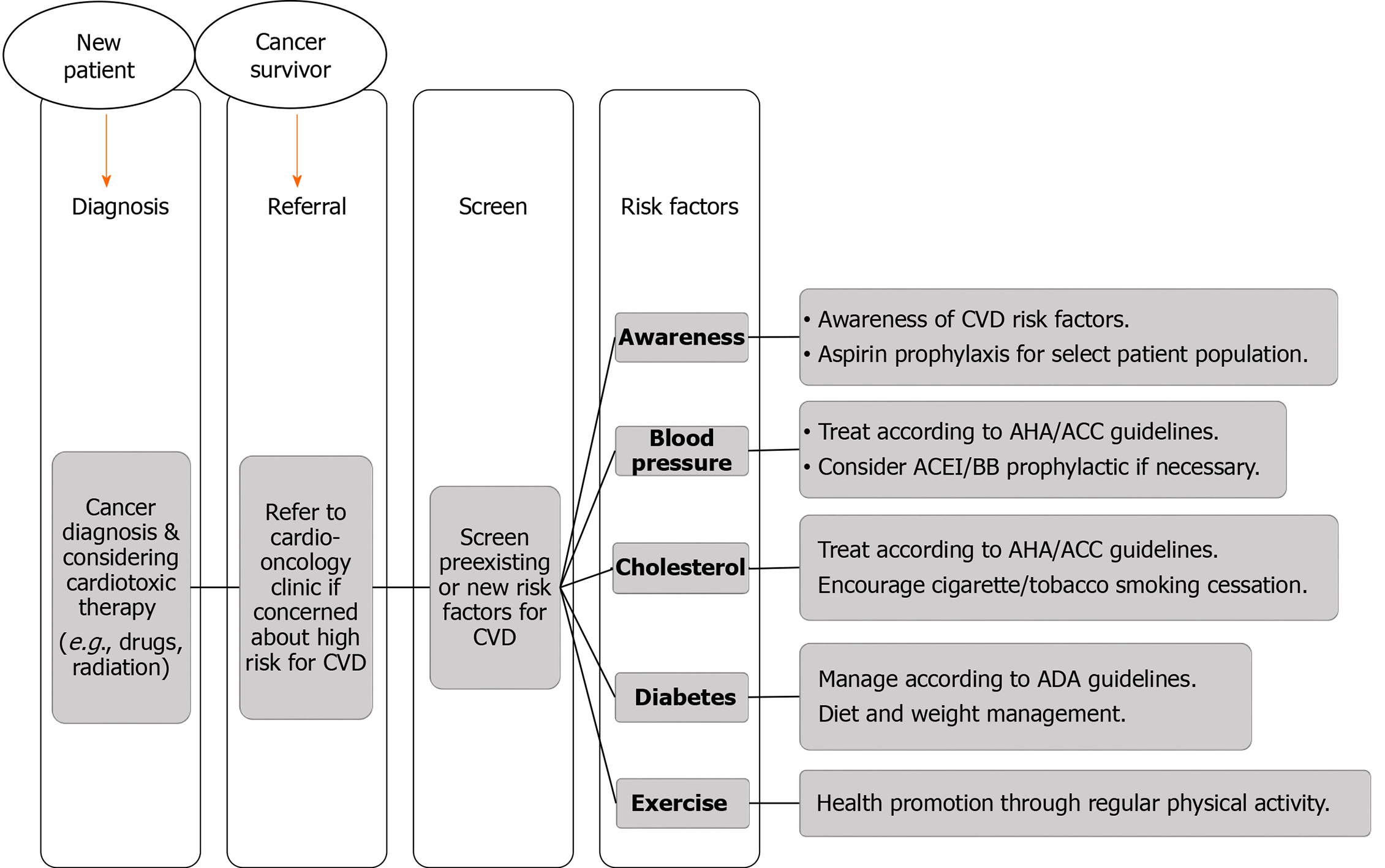
While researchers continue to develop a tool to estimate the cardiovascular risk among adult cancer survivors, the physician should focus on managing these patients by utilizing the ABCDE steps to prevent heart disease which has been largely applied to breast and prostate cancer survivors but can be adapted for all types of cancer survivors[25,26]. A: Being Awareness of risks of heart disease and symptoms associated with cardiovascular illness, and Aspirin prophylaxis for eligible patients; B: Maintaining Blood pressure below cutoffs; C: Controlling Cholesterol levels and promoting Cigarette/tobacco smoking cessation; D: Diet and Diabetes management; and E: Exercise (Figure 1).
In conclusion, cardio-oncologist care must be initiated right from the pre-treatment stage for identifying high-risk patients and mitigating the factors known to contribute to cardiotoxicity to after treatment phase where future cardiovascular risk is frequently assessed and appropriate measures are undertaken to maintain long-term cardiovascular health. Recent progress in terms of utilizing advanced imaging techniques and identifying the role of cardioprotective medications to prevent the progression of ventricular dysfunction has been a step in the right direction, and now the urgent need is to direct future studies with the focus to develop an accurate cardiovascular risk prediction and assessment tool for adult cancer survivors to continue to provide comprehensive cancer. In the meantime, physicians should work collaboratively and must strive to optimize and aggressively manage cardiovascular risk factors in cancer survivors since they form a unique subset of a vulnerable population given their exposures to potential cardiotoxic therapies.
Manuscript source: Invited manuscript
Specialty type: Oncology
Country/Territory of origin: United States
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): 0
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Sardesai S S-Editor: Zhang H L-Editor: A P-Editor: Wang LL
| 1. | Goff DC Jr, Lloyd-Jones DM, Bennett G, Coady S, D'Agostino RB, Gibbons R, Greenland P, Lackland DT, Levy D, O'Donnell CJ, Robinson JG, Schwartz JS, Shero ST, Smith SC Jr, Sorlie P, Stone NJ, Wilson PW, Jordan HS, Nevo L, Wnek J, Anderson JL, Halperin JL, Albert NM, Bozkurt B, Brindis RG, Curtis LH, DeMets D, Hochman JS, Kovacs RJ, Ohman EM, Pressler SJ, Sellke FW, Shen WK, Smith SC Jr, Tomaselli GF; American College of Cardiology/American Heart Association Task Force on Practice Guidelines. 2013 ACC/AHA guideline on the assessment of cardiovascular risk: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation. 2014;129:S49-S73. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1958] [Cited by in RCA: 2590] [Article Influence: 235.5] [Reference Citation Analysis (0)] |
| 2. | Desai R, Desai A, Abbas SA, Patel U, Bansod S, Damarlapally N, Doshi R, Savani S, Gangani K, Sachdeva R, Kumar G. National prevalence, trends and outcomes of takotsubo syndrome in hospitalizations with prior history of mediastinal/intrathoracic cancer and radiation therapy. Int J Cardiol. 2020;309:14-18. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 16] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 3. | Desai A, Noor A, Joshi S, Kim AS. Takotsubo cardiomyopathy in cancer patients. Cardiooncology. 2019;5:7. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 22] [Cited by in RCA: 35] [Article Influence: 5.8] [Reference Citation Analysis (0)] |
| 4. | Hanrahan EO, Gonzalez-Angulo AM, Giordano SH, Rouzier R, Broglio KR, Hortobagyi GN, Valero V. Overall survival and cause-specific mortality of patients with stage T1a,bN0M0 breast carcinoma. J Clin Oncol. 2007;25:4952-4960. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 214] [Cited by in RCA: 217] [Article Influence: 12.1] [Reference Citation Analysis (0)] |
| 5. | Bradshaw PT, Stevens J, Khankari N, Teitelbaum SL, Neugut AI, Gammon MD. Cardiovascular Disease Mortality Among Breast Cancer Survivors. Epidemiology. 2016;27:6-13. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 218] [Cited by in RCA: 324] [Article Influence: 36.0] [Reference Citation Analysis (0)] |
| 6. | Parekh T, Desai A. Demographic and Socioeconomic Disparities Among Cancer Survivors in Clinical Trials Participation, USA, 2016-2018. J Cancer Educ. 2020;. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 8] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 7. | Chen Y, Chow EJ, Oeffinger KC, Border WL, Leisenring WM, Meacham LR, Mulrooney DA, Sklar CA, Stovall M, Robison LL, Armstrong GT, Yasui Y. Traditional Cardiovascular Risk Factors and Individual Prediction of Cardiovascular Events in Childhood Cancer Survivors. J Natl Cancer Inst. 2020;112:256-265. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 79] [Article Influence: 15.8] [Reference Citation Analysis (0)] |
| 8. | Ezaz G, Long JB, Gross CP, Chen J. Risk prediction model for heart failure and cardiomyopathy after adjuvant trastuzumab therapy for breast cancer. J Am Heart Assoc. 2014;3:e000472. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 183] [Cited by in RCA: 209] [Article Influence: 19.0] [Reference Citation Analysis (0)] |
| 9. | Koene RJ, Prizment AE, Blaes A, Konety SH. Shared Risk Factors in Cardiovascular Disease and Cancer. Circulation. 2016;133:1104-1114. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 924] [Cited by in RCA: 1039] [Article Influence: 115.4] [Reference Citation Analysis (0)] |
| 10. | Nicolazzi MA, Carnicelli A, Fuorlo M, Scaldaferri A, Masetti R, Landolfi R, Favuzzi AMR. Anthracycline and trastuzumab-induced cardiotoxicity in breast cancer. Eur Rev Med Pharmacol Sci. 2018;22:2175-2185. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 34] [Reference Citation Analysis (0)] |
| 11. | Raghunathan D, Khilji MI, Hassan SA, Yusuf SW. Radiation-Induced Cardiovascular Disease. Curr Atheroscler Rep. 2017;19:22. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 74] [Article Influence: 9.3] [Reference Citation Analysis (0)] |
| 12. | Gilon D, Leibowitz D, Durst R, Iakobishvili Z. Imaging in Cardio-oncology: An Overview of an Emerging Medical Discipline. J Thorac Imaging. 2020;35:4-11. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 5] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 13. | Kuriakose RK, Kukreja RC, Xi L. Potential Therapeutic Strategies for Hypertension-Exacerbated Cardiotoxicity of Anticancer Drugs. Oxid Med Cell Longev. 2016;2016:8139861. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 16] [Cited by in RCA: 23] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 14. | Mouhayar E, Salahudeen A. Hypertension in cancer patients. Tex Heart Inst J. 2011;38:263-265. [PubMed] |
| 15. | Whelton PK, Carey RM, Aronow WS, Casey DE Jr, Collins KJ, Dennison Himmelfarb C, DePalma SM, Gidding S, Jamerson KA, Jones DW, MacLaughlin EJ, Muntner P, Ovbiagele B, Smith SC Jr, Spencer CC, Stafford RS, Taler SJ, Thomas RJ, Williams KA Sr, Williamson JD, Wright JT Jr. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Hypertension. 2018;71:1269-1324. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2649] [Cited by in RCA: 2532] [Article Influence: 361.7] [Reference Citation Analysis (0)] |
| 16. | Vaduganathan M, Hirji SA, Qamar A, Bajaj N, Gupta A, Zaha V, Chandra A, Haykowsky M, Ky B, Moslehi J, Nohria A, Butler J, Pandey A. Efficacy of Neurohormonal Therapies in Preventing Cardiotoxicity in Patients with Cancer Undergoing Chemotherapy. JACC CardioOncol. 2019;1:54-65. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 45] [Cited by in RCA: 87] [Article Influence: 14.5] [Reference Citation Analysis (0)] |
| 17. | Hwangbo Y, Kang D, Kang M, Kim S, Lee EK, Kim YA, Chang YJ, Choi KS, Jung SY, Woo SM, Ahn JS, Sim SH, Hong YS, Pastor-Barriuso R, Guallar E, Lee ES, Kong SY, Cho J. Incidence of Diabetes After Cancer Development: A Korean National Cohort Study. JAMA Oncol. 2018;4:1099-1105. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 62] [Cited by in RCA: 119] [Article Influence: 19.8] [Reference Citation Analysis (0)] |
| 18. | Kosalka P, Johnson C, Turek M, Sulpher J, Law A, Botros J, Dent S, Aseyev O. Effect of obesity, dyslipidemia, and diabetes on trastuzumab-related cardiotoxicity in breast cancer. Curr Oncol. 2019;26:e314-e321. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 27] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 19. | Guenancia C, Lefebvre A, Cardinale D, Yu AF, Ladoire S, Ghiringhelli F, Zeller M, Rochette L, Cottin Y, Vergely C. Obesity As a Risk Factor for Anthracyclines and Trastuzumab Cardiotoxicity in Breast Cancer: A Systematic Review and Meta-Analysis. J Clin Oncol. 2016;34:3157-3165. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 169] [Cited by in RCA: 159] [Article Influence: 17.7] [Reference Citation Analysis (0)] |
| 20. | Rock CL, Flatt SW, Byers TE, Colditz GA, Demark-Wahnefried W, Ganz PA, Wolin KY, Elias A, Krontiras H, Liu J, Naughton M, Pakiz B, Parker BA, Sedjo RL, Wyatt H. Results of the Exercise and Nutrition to Enhance Recovery and Good Health for You (ENERGY) Trial: A Behavioral Weight Loss Intervention in Overweight or Obese Breast Cancer Survivors. J Clin Oncol. 2015;33:3169-3176. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 137] [Cited by in RCA: 158] [Article Influence: 15.8] [Reference Citation Analysis (0)] |
| 21. | Miller AM, Lopez-Mitnik G, Somarriba G, Lipsitz SR, Hinkle AS, Constine LS, Lipshultz SE, Miller TL. Exercise capacity in long-term survivors of pediatric cancer: an analysis from the Cardiac Risk Factors in Childhood Cancer Survivors Study. Pediatr Blood Cancer. 2013;60:663-668. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 66] [Cited by in RCA: 63] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 22. | Scott JM, Zabor EC, Schwitzer E, Koelwyn GJ, Adams SC, Nilsen TS, Moskowitz CS, Matsoukas K, Iyengar NM, Dang CT, Jones LW. Efficacy of Exercise Therapy on Cardiorespiratory Fitness in Patients With Cancer: A Systematic Review and Meta-Analysis. J Clin Oncol. 2018;36:2297-2305. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 140] [Cited by in RCA: 225] [Article Influence: 32.1] [Reference Citation Analysis (0)] |
| 23. | Pituskin E, Haykowsky M, McNeely M, Mackey J, Chua N, Paterson I. Rationale and design of the multidisciplinary team IntervenTion in cArdio-oNcology study (TITAN). BMC Cancer. 2016;16:733. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 27] [Cited by in RCA: 32] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 24. | Gilchrist SC, Barac A, Ades PA, Alfano CM, Franklin BA, Jones LW, La Gerche A, Ligibel JA, Lopez G, Madan K, Oeffinger KC, Salamone J, Scott JM, Squires RW, Thomas RJ, Treat-Jacobson DJ, Wright JS; American Heart Association Exercise; Cardiac Rehabilitation; and Secondary Prevention Committee of the Council on Clinical Cardiology; Council on Cardiovascular and Stroke Nursing; and Council on Peripheral Vascular Disease. Cardio-Oncology Rehabilitation to Manage Cardiovascular Outcomes in Cancer Patients and Survivors: A Scientific Statement From the American Heart Association. Circulation. 2019;139:e997-e1012. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 149] [Cited by in RCA: 299] [Article Influence: 59.8] [Reference Citation Analysis (0)] |
| 25. | Bhatia N, Santos M, Jones LW, Beckman JA, Penson DF, Morgans AK, Moslehi J. Cardiovascular Effects of Androgen Deprivation Therapy for the Treatment of Prostate Cancer: ABCDE Steps to Reduce Cardiovascular Disease in Patients With Prostate Cancer. Circulation. 2016;133:537-541. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 81] [Cited by in RCA: 119] [Article Influence: 13.2] [Reference Citation Analysis (0)] |
| 26. | Montazeri K, Unitt C, Foody JM, Harris JR, Partridge AH, Moslehi J. ABCDE steps to prevent heart disease in breast cancer survivors. Circulation. 2014;130:e157-e159. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 34] [Article Influence: 3.1] [Reference Citation Analysis (0)] |